Abstract
Objectives
To investigate the interdental arch relationship outcomes of 5-year-old children with unilateral cleft lip and palate (UCLP) before and after centralization of cleft services in the United Kingdom (UK) using the modified Huddart-Bodenham index (MHBI) and to investigate any differences in MHBI by cleft laterality.
Design
Retrospective cross-sectional study.
Setting
Evaluation of three-dimensional study models of children with a complete UCLP.
Participants
All available 5-year-old orthodontic study models of participants with UCLP from the precentralization Clinical Standard Advisory Group (CSAG n = 107) and postcentralization cleft care UK (CCUK n = 195) studies. The models were also grouped by cleft laterality (left and right sided).
Outcome measures
Differences between the interdental arch relationship outcomes were assessed using the MHBI. This index scored the buccal/palatal or labial/palatal relationships of 8 maxillary deciduous teeth with the opposing mandibular dentition. The anterior segment, buccal cleft segment, and noncleft segment scores were calculated and combined to calculate the MBHI total arch scores.
Results
Inter and intraexaminer reliability demonstrated high levels of agreement. Statistically significant differences in the anterior segment, buccal noncleft segment, and total arch MHBI scores were found, with postcentralization CCUK performing better. Right-sided UCLP had statistically significantly better buccal cleft segments, but no differences were found for the other MBHI segments or total arch scores.
Conclusions
There were improved interdental arch relationships postcentralization of cleft services in the United Kingdom. Cleft laterality differences were limited to the buccal cleft segment with right-sided UCLP having better MBHI scores.
Introduction
Orofacial clefts (OFCs) are the most common craniofacial anomaly in the United Kingdom (UK), with an estimated prevalence of 13 per 10 000 live births. 1 Internationally, the incidence varies widely across regions and ethnicities, being highest among Amerindian populations and lowest among African populations. 2
In the United Kingdom, cleft palate is the most common phenotype, followed by cleft lip (CL), unilateral CL and palate (UCLP), and bilateral CL and palate (BCLP). A cleft palate occurs more often in females, while CL and palate are more common in males. Unilateral clefts on the left side are twice as common as on the right, irrespective of sex, ethnicity, or severity. 3 Although landmark outcome studies of patients with UCLP have commonly pooled the left and right UCLP study samples,4–7 a recent study has found anatomical differences associated with cleft laterality. 8 There is an increasing interest in laterality and some studies have reported poorer outcomes for patients with right-sided UCLP.9–11 However, other studies have found either weak associations or no differences in laterality outcomes.12,13
Children with OFC often experience restricted maxillary growth following surgical repair, particularly if the cleft involves the lip, alveolus, and palate. This restriction can occur in vertical, anteroposterior (AP), and transverse maxillary dimensions and often becomes more apparent with continued facial growth. Restricted transverse buccal and anterior maxillary dimensions can lead to constricted and distorted maxillary dental arch forms and unfavorable interdental arch relationships. These unfavorable interdental arch relationships often result in anterior and/or posterior segment crossbites as well as anterior/posterior open bites. The incidence of buccal crossbites in patients with a UCLP has been reported to be as high as 96%. 14 These unfavorable interdental arch relationships can present challenges for orthodontic and/or orthognathic surgical correction as well as subsequent retention and stability of the occlusal corrections.
The use of interdental arch relationship outcome measures at age 5 years offers an opportunity to assess the occlusion following the primary surgical repair and continued facial growth, but prior to the transition to permanent dentition and any orthodontic treatment. 15
Cleft care in the United Kingdom underwent a fundamental reorganization following the recommendations of the 1998 Clinical Standards Advisory Group (CSAG). The CSAG findings highlighted the relatively poor outcomes when compared to other European cleft centers, where the number of surgical repairs undertaken per surgeon was considerably higher. 4 As a result, cleft care in the United Kingdom was centralized, and surgical services were restricted to 16 sites. 4 A key purpose of centralization was to ensure higher volumes of surgical repairs were carried out by each surgeon. Improved outcomes from the centralized service were reported in the follow-up cleft care UK (CCUK) investigation in 2013. 16
Previous outcome studies comparing pre-CSAG and post-CCUK cleft care centralization have reported significant improvements in the CCUK data including those assessing dental models using the 5-year-old index. 17 The 5-year-old index essentially assesses the AP dental arch relationship for children with UCLP. 15 In addition, improvements in the maxillary arch width dimensions and arch form were also noted for the CCUK group, although the actual arch width dimension improvements recorded from the CCUK models were relatively small and no assessment of the opposing mandibular dental arch was undertaken. 18
To date, no studies have investigated the transverse buccal and anterior interdental relationship outcomes from the CSAG and CCUK studies using the Modified Huddart-Bodenham Index (MHBI). The MHBI is an index that assesses the severity and frequency of crossbites in the sagittal and transverse dimensions to evaluate the amount of constriction within the maxillary dentition relative to the mandibular dentition. In addition, no studies to date have investigated cleft laterality outcomes for the CSAG and CCUK dental models.
The aims of the study were to compare the transverse and AP interdental arch relationships of children with a complete UCLP, before and after centralization of the cleft care pathways in the United Kingdom using the MHBI, and to determine any differences in MBHI outcomes by cleft laterality.
The study's null hypotheses were that there are no differences in MBHI outcomes for 5-year-old children with complete UCLP-treated pre and postcentralization of cleft services in the United Kingdom and that there are no differences in MBHI outcomes by cleft laterality.
Material and Methods
To assess the interdental arch relationship outcomes, the MBHI was used. The index divided the maxillary arch into 2 buccal segments (the cleft and noncleft buccal segments) and an anterior (labial) segment (Figure 1). Each buccal segment consisted of the deciduous canine and first and second primary molars, whereas the anterior segment comprised the deciduous central incisors only. The maxillary deciduous lateral incisors were not included due to their frequent absence. A numerical score was determined for each maxillary tooth relative to the opposing mandibular tooth with the models in occlusion (Figure 2).
19
The modified version of the index as proposed by Dobbyn et al
20
was used and took into consideration the following:
If a central incisor was missing, then the other central incisor was used to score it. If a deciduous molar was missing, then it was scored based on the neighboring deciduous molar. If both were missing, then the score was given based on the relationship between the midpoint of the missing deciduous molar ridge and the opposing tooth.
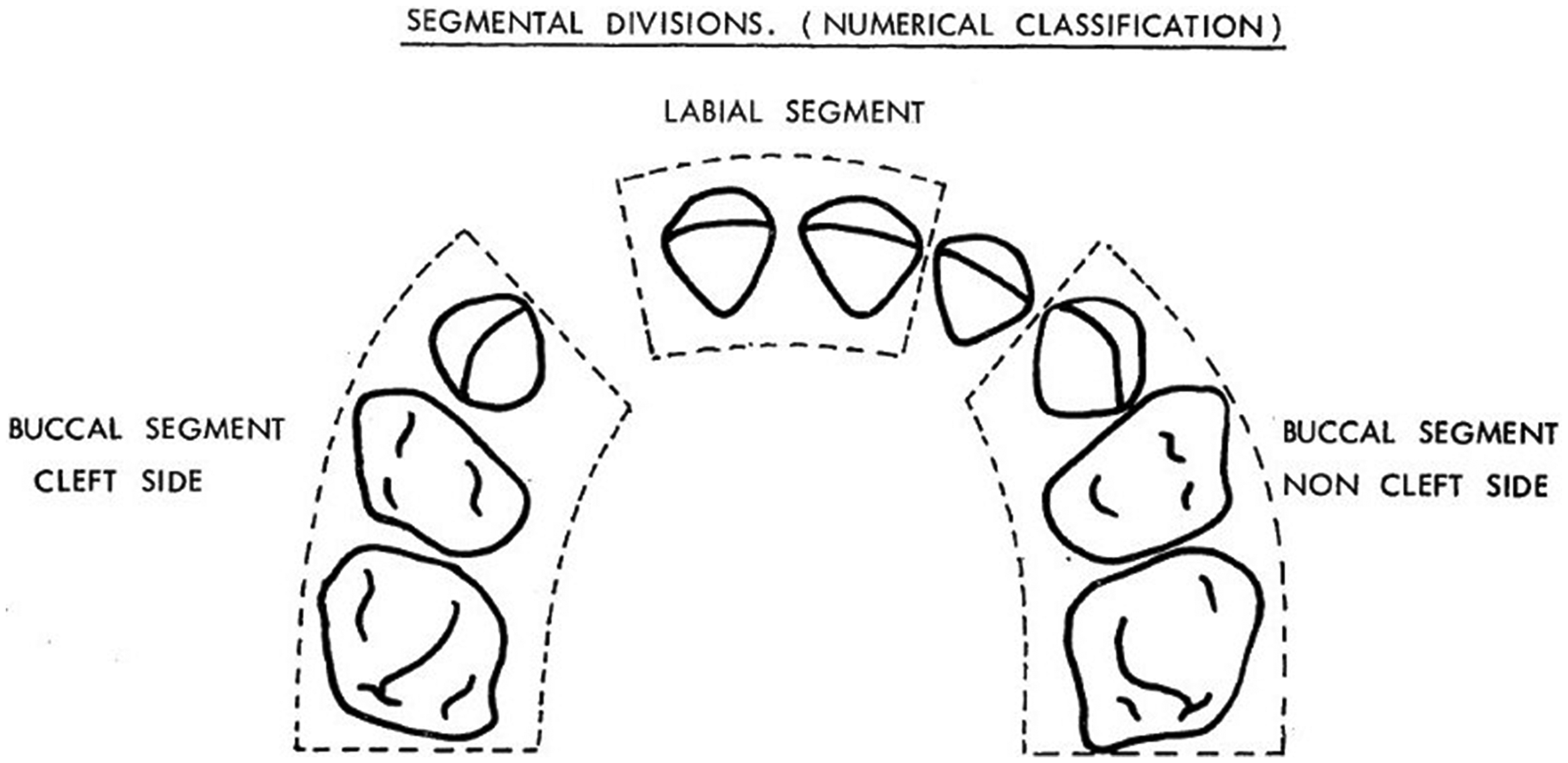
Huddart and Bodenham index segments. 19
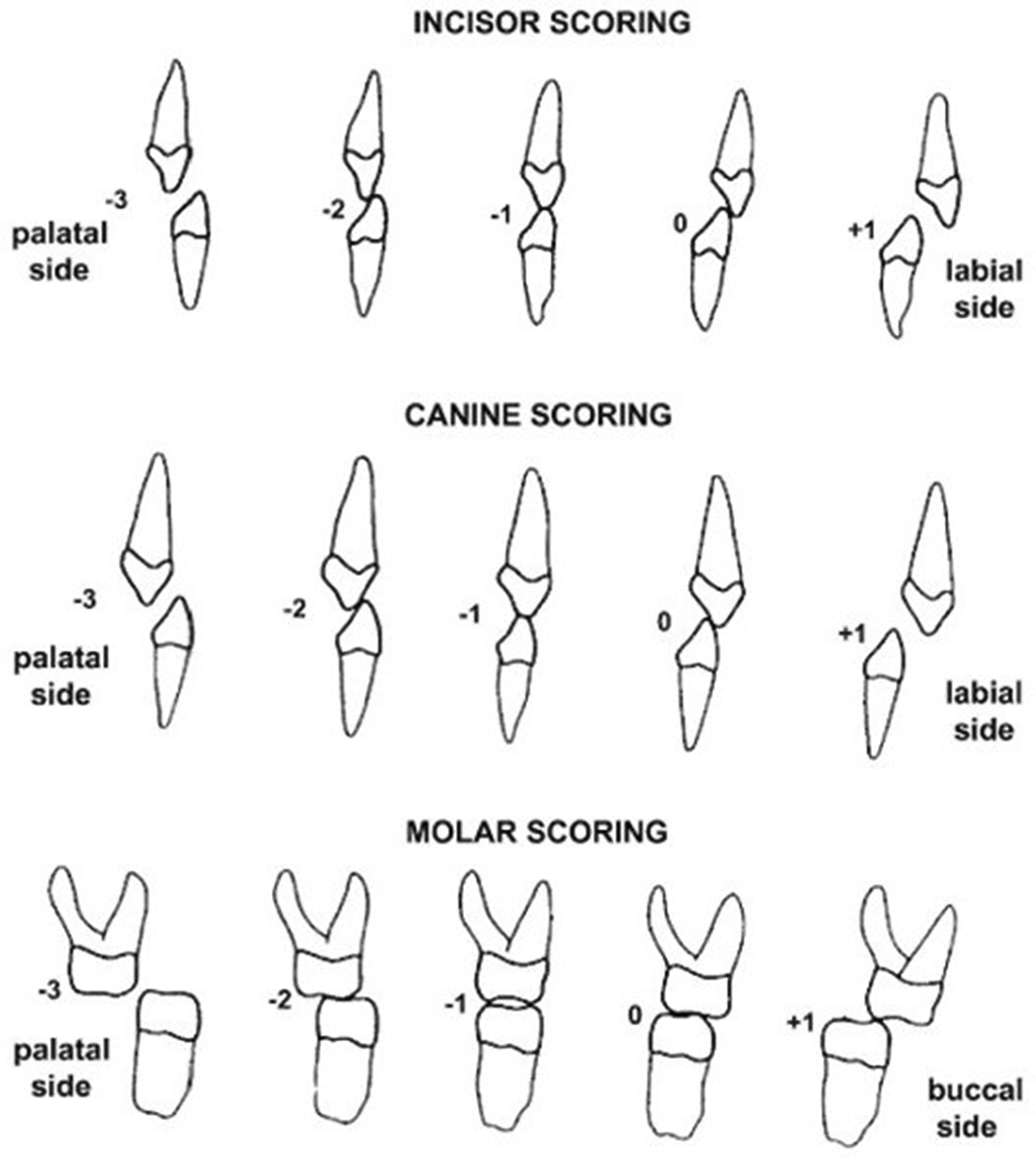
The modified Huddart and Bodenham index (MBHI) scoring guide. 20
Each model had a potential maximum total arch MHBI score ranging from −24 to +8, with a more negative score representing a more severe transverse and AP interdental arch relationship. Using this index, normal occlusal relationships were scored 0; an edge-to-edge occlusion was scored −1: a crossbite with contact was scored −2; a crossbite without contact was scored −3; while an increased overjet or buccal occlusion with no contact scored +1 (Figure 2). Separate segment scores were obtained for the anterior, buccal noncleft side, and buccal cleft side, with a total arch MHBI score derived from combining the segment scores.
Data Sources
Maxillary and mandibular plaster orthodontic study models of 5-year-old nonsyndromic patients with complete UCLP (including a soft tissue band of < 5 mm) were identified from the CCUK and CSAG models archives held at the University of Bristol Dental School. All participants were previously given a unique identifier number specific to each study (CSAG and CCUK) to protect and anonymize patient information. These unique identifier numbers were then used to link new study reference numbers for blinding the assessors to the origin of the models and to allow for sample randomization.
A single researcher (BA) scanned and digitally articulated all study models over a 4-week period. Models were scanned randomly using 3 Shape R750™ desktop laboratory laser scanner. All the original plaster models were articulated and bases trimmed to the wax bite taken at the time of the record collection. The scanned models were then checked for correct orientations and accuracy of articulation with the original plaster models. Five of the scanned models had to be rescanned using the 3 Shape TRIOS™ intraoral scanner due to the inability to accurately capture the correct articulation of the plaster models within the 3 Shape R750™ scanner. Both scanners were calibrated as per manufacturer guidelines prior to scanning.
Once scanned, a dental data manager, who otherwise took no further part in the study, assigned random study identification numbers to the digital files using a random number generator (https://www.randomcodegenerator.com/en/generate-codes). These files were uploaded into the OrthoAnalyzer™ software program to aid model viewing and scoring.
Prior to scoring, both assessors (BA/PF) undertook a calibration exercise using 15 digital study models of patients with UCLP unrelated to the CCUK and CSAG samples. The assessment was carried out independently using the same MHBI assessment instruction and scoring sheet. Once completed, both assessors compared their MHBI scores and where differences were noted, each assessor discussed their interpretation of the scoring criteria to reach a consensus for future scoring.
A customized MS Excel (Microsoft Corp. Redmond, WA) sheet was formulated with all the scanned models randomized by their study reference number for the entry of the MHBI scoring. Scores were recorded into the MS Excel sheet for each maxillary tooth within each of the anterior, buccal cleft, and nonbuccal cleft side segments. Automatic summation of the segments and total arch MHBI score was carried out within MS Excel. Both assessors carried out their assessments independently, viewing the digital models on the same laptop and using the same digital viewing software (OrthoAnalyzer™) settings. The software allowed for 3D manipulation of the models, magnification, and viewing of the maxillary and mandibular occlusal surfaces for tooth identification.
Reproducibility
Thirty models were randomly chosen for repeat scoring 4 weeks following the first assessment. Furthermore, since 2 different scanners were used, one a laboratory bench top scanner (3 Shape R750™) and the other a handheld intraoral scanner (3 Shape TRIOS™), a reproducibility assessment within and across the 2 scanning methods was also carried out. This was achieved by hand scanning 29 randomized plaster models using 3 Shape TRIOS™ intraoral scanner. The repeat assessment was carried out 2 weeks after the initial assessment by one assessor (BA).
A sample size calculation indicated that a total sample size of 140 participants (70 per group) would give a power of 80% with a 5% significance level to detect a true difference in transverse dental arch relationship total arch MHBI scores > 1.58. This was determined by ClinCalc.com using total MHB arch score differences reported by Mikoya et al 21 who investigated 2 groups of 5-year-old Japanese children with UCLP who had different palatal surgery protocols.
Participant demographic data (sex and date of birth) was obtained from the original CSAG and CCUK studies. Cleft laterality was determined by the main author (BA) from the scanned study models and was confirmed by an experienced orthodontic consultant (PF).
Statistical Analysis
The data were analyzed using Stata version 16 (Stata Corp, College Station, Texas, USA) with a predetermined level of significance set at α = 0.5. Intraclass correlation coefficients (ICCs) were used to assess the levels of inter and intraassessor agreements. In addition, it was used to assess the agreement when the models were hand-scanned versus laboratory-scanned. Ordered logistic regression was used to test if there was statistical evidence of differences in outcomes between the CCUK and CSAG samples, as well as for cleft laterality and sex. The comparison was undertaken for each of the segment scores (anterior, buccal cleft, and buccal noncleft) as well as the total arch MHBI score.
Ethics
This study conformed with the Declaration of Helsinki and was deemed by the University of Bristol's Research and Ethics Committee as a project that required no ethical approval. The research ethics committee required no ethical approval when the CSAG study was carried out as it was considered an audit project. Data collected by the CCUK study was carried out with ethical approval (REC reference number: 10/H0107/33, Southwest 5 REC). Patient/parent consent was obtained prior to the original data collection for both the CSAG and CCUK studies.
Results
A total of 344 orthodontic models of 5-year-olds with UCLP were retrieved from the CCUK/CSAG record archive. Due to incomplete or unidentified data, 302 models were ultimately assessed, with 195 from the CCUK cohort and 107 from the CSAG cohort. Both cohorts had similar gender distributions, although the CSAG cohort had a slightly higher mean age (6.5 years vs 5.6 years), while the CCUK group had a slightly higher prevalence of left-sided UCLP (71.3% vs 62.6%). The CCUK data had missing information for sex (4 cases) and age (6 cases), while the CSAG data had missing age information for 5 cases (Table 1).
Demographic Characteristics of the 5-Year-Old Patients With Unilateral Cleft Lip and Palate.
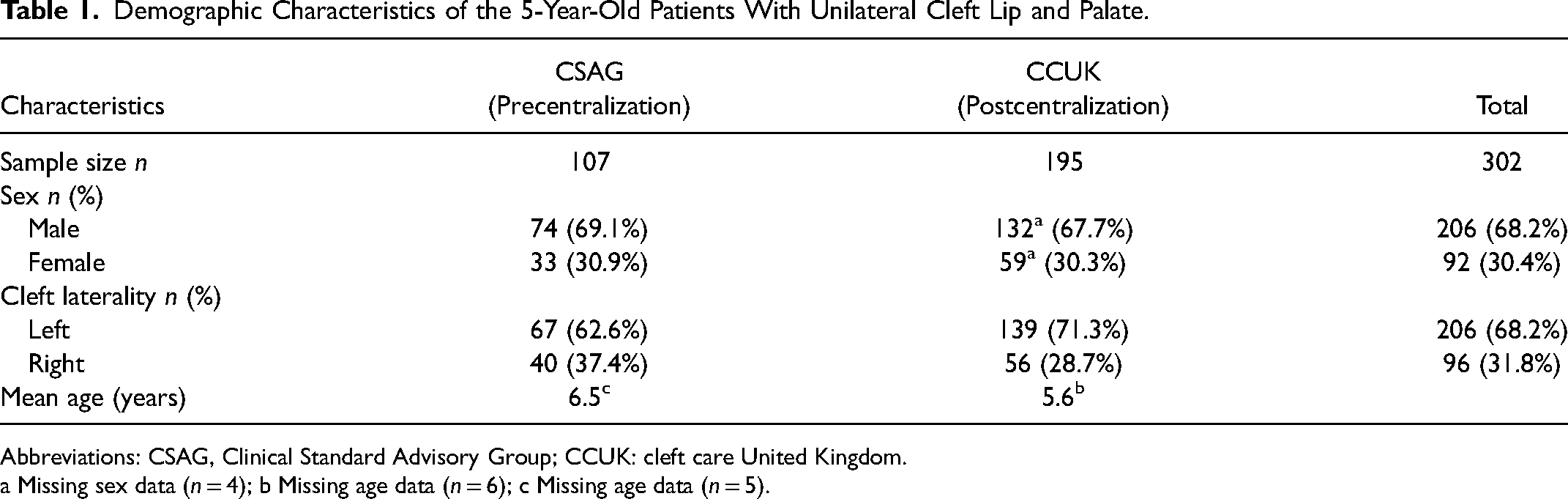

Abbreviations: CSAG, Clinical Standard Advisory Group; CCUK: cleft care United Kingdom.
a Missing sex data (n = 4); b Missing age data (n = 6); c Missing age data (n = 5).
Intra and Interrater Reliability for the MHB Index
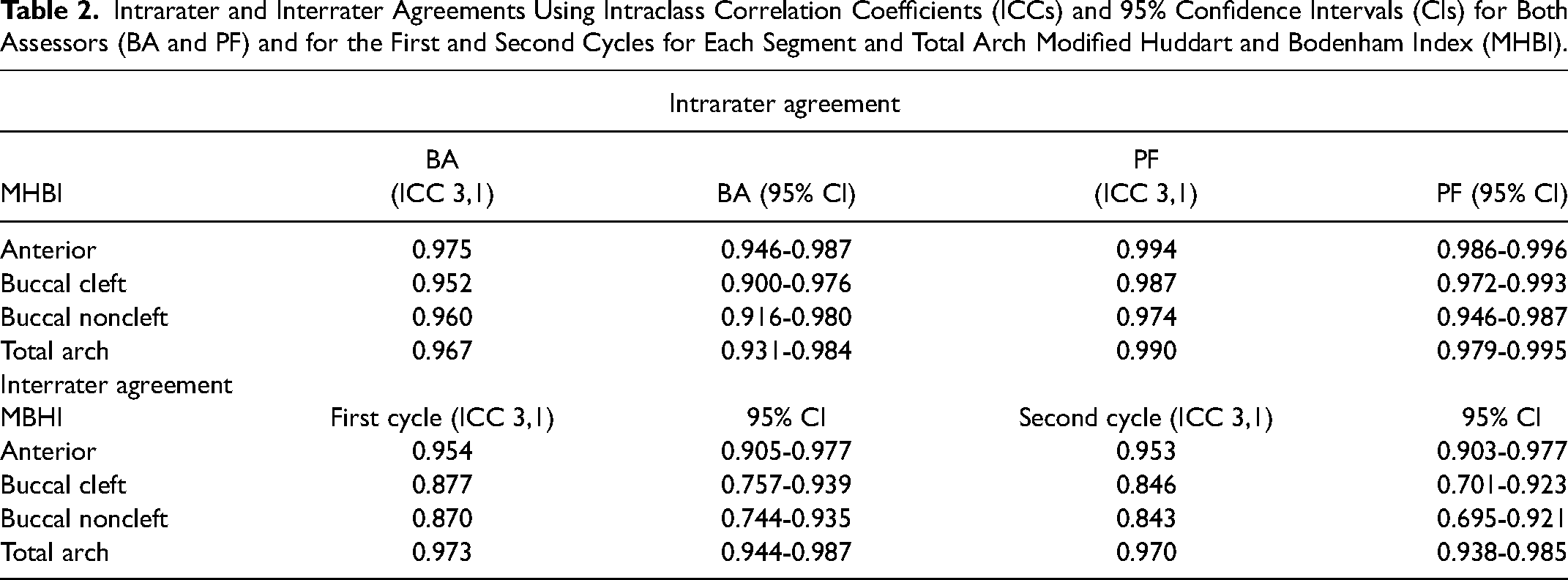
High intrarater agreements were achieved for MHBI scores of all segments for both assessors (Table 2). High interrater agreements were achieved for MBHI scores between 2 examiners across 2 cycles for all segments and the total arch MHBI scores (Table 2). High intrarater agreements (ICC 0.999-0.996) were also achieved for assessor BA for MHBI scores obtained for handheld and laboratory scanned models.
Intrarater and Interrater Agreements Using Intraclass Correlation Coefficients (ICCs) and 95% Confidence Intervals (CIs) for Both Assessors (BA and PF) and for the First and Second Cycles for Each Segment and Total Arch Modified Huddart and Bodenham Index (MHBI).
The distribution of the CCUK and CSAG segment scores and total arch MBHI scores were nonnormal and for comparative purposes, the medians and interquartile range (IQR) were calculated for the anterior segment, buccal cleft segment, buccal noncleft segment, and total arch MHBI scores for both CCUK and CSAG cohorts (Table 3).
Modified Huddart and Bodenham Index (MBHI) Median Scores and Interquartile Ranges for the Clinical Standards Advisory Group (CSAG) and Cleft Care UK (CCUK) 5-Year-Olds Cohorts for Anterior Segment, Buccal Cleft Segment, Buccal Noncleft Segment and Total Arch Scores.

CSAG Versus CCUK MHBI Outcomes
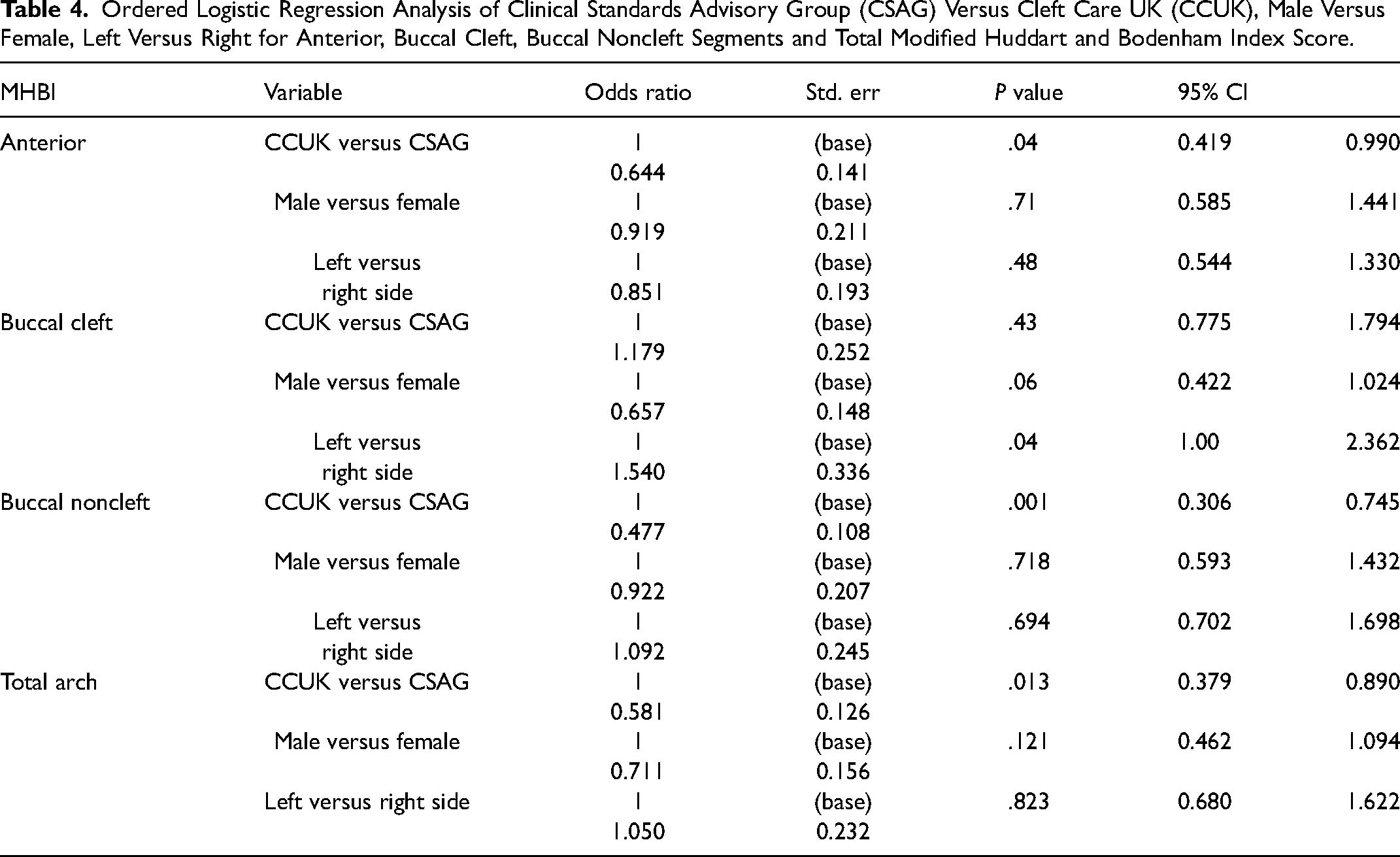
Anterior segment: Significant differences in MHBI scores for the anterior segment between CCUK and CSAG cohorts were noted (Table 4), with CCUK having better outcomes. It was observed that a higher number of patients in the CCUK cohort had near-normal occlusion, with an MHBI anterior segment score of 0 to +1 (normal occlusion).
Buccal cleft segment: No significant differences in MBHI scores for the buccal cleft segment between the CSAG and the CCUK were observed (Table 4).
Buccal noncleft segment: Significant differences in the MBHI buccal noncleft segments were noted between the CSAG and the CCUK, with the CCUK having better outcome scores (Table 4).
Total arch scores: Significant differences in the MBHI total arch between the CSAG and CCUK were noted with the CCUK having better outcomes (Table 4).
Cleft laterality (left vs right) and sex MBHI outcomes: Significant differences in the MBHI outcomes were noted for right-sided clefts, but these findings were limited to the buccal cleft segment only. No significant differences were noted for the anterior, buccal noncleft, and total MHBI scores (Table 4). No significant differences for sex were noted in the MBHI segment and total arch scores (Table 4).
Discussion
Key Findings
Using the MHBI, this study assessed the interdental arch relationship outcomes in 5-year-old children with complete UCLP treated before and after the centralization of UK cleft services. The findings noted that the postcentralization group (CCUK) had significantly better MHBI scores in the anterior segment, buccal noncleft segment, and total arch compared to the precentralization group (CSAG), although the scores for the buccal cleft segment were similar. Right-sided UCLP had better buccal cleft segment scores than left-sided ULCP, but there were no significant differences in other MBHI segment scores or total arch scores. There were no significant differences in the MHBI segment and total arch scores by sex.
Ordered Logistic Regression Analysis of Clinical Standards Advisory Group (CSAG) Versus Cleft Care UK (CCUK), Male Versus Female, Left Versus Right for Anterior, Buccal Cleft, Buccal Noncleft Segments and Total Modified Huddart and Bodenham Index Score.
Reliability of Measurement
The MHBI demonstrates high inter and intraexaminer reliability, with ICC values of 0.967 and 0.973, respectively. These results align with findings by Salazar et al 22 and Martin et al, 23 which noted similarly high reliability when using the MHBI on digital study models. The use of digital models, whether captured by handheld or laboratory scanners likely contributed to the high reliability, as the 3D manipulation and stable articulation of digital models reduced potential errors compared to handheld plaster models.
Study Sample Demographics
Both the CSAG and CCUK studies included 5-year-old children with nonsyndromic complete UCLP ± a soft tissue band under 5 mm. The demographics of the CSAG and CCUK groups had comparable gender distribution (male: CCUK 67.7% and CSAG 69.1%) while the CSAG group had a slightly older mean age (CCUK 5.6 years and CSAG 6.5 years). The difference in age reflected the differing recruitment protocols used by these 2 studies, with the CSAG, conducted as a retrospective national audit whereas the CCUK was undertaken as a cross-sectional national study where data was collected at designated audit clinics. This age difference may potentially affect the interpretation of this study's findings due to the implications of differences in facial growth and dental development. Both groups had a higher prevalence of left-sided clefts (CCUK 71.3% and CSAG 62.6%), consistent with previous studies.1,2,24,25
Anterior Segment Scores
Unilateral CL and palate affects the anterior segment interdental arch relationship, posing correction challenges. This study found that the CCUK cohort had significantly better MHBI anterior segment scores than the CSAG cohort, with more CCUK patients showing near-normal occlusion (scores of 0 to +1). This aligns with the findings of Al-Ghatam et al 17 using the 5-year-old index, who found only 30% were rated as “good” or “excellent” in the CSAG group, but where over 50% rated as “good” or “very good” in the CCUK cohort. This further supports evidence that centralization of cleft services has resulted in improved outcomes in the anterior segment interdental arch relationship. Additionally, the CCUK cohort MBHI anterior segment scores were similar to those in other recent studies, while the CSAG scores were again less favorable.22,26
Buccal Cleft Segment Scores and Buccal Noncleft Segment Scores
In the buccal segment, no significant differences were found between CCUK and CSAG on the cleft side, but CCUK performed significantly better on the noncleft side. Possible explanations of these findings may include differences in surgical palatal repair protocols, surgeon training, and case volumes. Cleft surgeons in the United Kingdom use a range of different primary surgical timings and sequences. They do not all consistently use the same protocols. 27 The original CSAG recommendations on centralization were not prescriptive as to timings or techniques for surgery. However, through the process of centralization timings, and admission times as well as surgical training pathways became more similar. 27 A shortcoming of this study was that we were unable to access historical surgical repair data on an individual basis and could not carry out a multiple regression model to investigate surgical confounders. However, the CSAG cohort commonly received the Veau and Wardill-Kilner pushback technique with releasing incisions on both the cleft and noncleft sides of the hard palate, a procedure that can lead to greater maxillary arch collapse. 28 Whilst the CCUK cohort commonly included a vomer flap repair often removing the requirement for releasing dissection on the noncleft side of the hard palate. The vomer flap procedure has been reported to have reduced interference with maxillary growth. 29 The effect of changes to the surgical training and case volumes could not be assessed by this study.
Total Arch MHBI Scores
The odds ratios and median total arch MHBI scores revealed that interdental arch relationships improved significantly following the centralization of cleft services. While the CCUK median scores aligned with recent studies, the CSAG scores showed a higher incidence of maxillary arch constriction, with anterior and buccal crossbites.21,26 This improvement in total arch MBHI scores supports the work of Al-Ghatam et al 17 who reported that 53% of the CCUK cohort had good to excellent dental relationships, compared to only 29% in CSAG when measured using the 5-year-old index. The improved interdental arch relationships found in CCUK potentially reduce orthodontic treatment need and lessen the requirement for future orthognathic surgery. They may also allow for improved occlusal stability with a lower risk of relapse following orthodontic correction. 9
Cleft Laterality and Sex
Better MBHI scores were noted for right-sided clefts, but this was only significant for the buccal cleft segment, while no differences were found in the anterior, buccal noncleft, or total MHBI scores. This finding is difficult to explain, although Staudt et al 9 reported that 65% of patients with left-sided clefts required orthognathic surgery compared to just 20% with right-sided clefts, which supports the findings of better outcomes for right-sided UCLP. However, this is contrary to the findings of Chong et al 8 who reported better outcomes for left-sided clefts, possibly due to anatomical differences. Differences in cleft laterality outcomes remain inconclusive and warrant further investigation. Sex did not impact the MHBI segment and total arch scores, a finding that is in agreement with Siegenthaler et al, 30 who reported no sex differences in MHBI scores when assessing UCLP outcomes following early and late secondary alveolar bone grafting.
The present study had several limitations, which need to be considered when interpretating the findings, namely:
Sample selection and data loss: Both the original CSAG and CCUK studies faced constraints due to their retrospective designs, respectively, recruiting ∼73% and 74% of patients with UCLP. The unavailability of archived data from both original studies due to loss and/or damage was disappointing and represented ∼29% from CCUK and 55% from CSAG. However, the similarity in gender distribution and mean ages with respect to the original studies suggested that the data used in this study were representative of the original samples, and data loss was random. Model artifacts: Seven archived models were excluded due to artifacts (eg, gauze on occlusal surfaces and damaged models), and 35 archived models were omitted due to unclear coding, which further contributed to the data loss. Lack of potential confounding data: Important confounding factors, such as surgical protocols, surgeon experience, and the use of presurgical devices, were not assessed. Without this information, it remains uncertain what specific elements of the centralization process led to improved outcomes, such as changes in the quality of surgical training, surgical volumes, or techniques.
Implications of the Study and Future Work
The study findings confirm that changes implemented following the CSAG recommendations have positively impacted dental arch outcomes for children with complete UCLP. The implied benefits of improved transverse and anterior-posterior dental arch outcomes in 5-year-olds not only include the reduced burden and complexity of orthodontic and/or orthognathic treatment, but also potentially facilitating more stable corrections post-treatment. Additionally, a digital record of the archived CSAG and CCUK plaster models has now been established, offering a more durable and accessible resource, avoiding the risk of further damage and/or loss of the original CSAG/CCUK models. Future research should explore potential confounding factors, such as surgical protocols, surgeon experience, and presurgical interventions on occlusal outcomes, as well as an investigation into the causes and outcome implications relating to cleft laterality.
Conclusions
The null hypotheses of no difference in MBHI outcome scores for 5-year-old children with complete UCLP treated pre and postcentralization of cleft services in the United Kingdom, and no difference in outcomes by cleft laterality, were both rejected. Significant differences were found in MHBI scores, with the postcentralization group (CCUK) scoring higher than the precentralization group (CSAG) in the anterior segment, buccal noncleft segment, and total arch MHBI scores. This indicates that following centralization of cleft care in the United Kingdom an improvement of both the transverse and AP interdental arch relationships occurred in patients with UCLP. Cleft laterality differences were found for the MBHI buccal cleft segment, with improved outcomes for right-sided clefts, but not for the MBHI buccal noncleft, anterior segments, and total arch scores.
Footnotes
Acknowledgments
We wish to acknowledge that Prof Martyn Sheriff provided valuable guidance and direction with the statistics and Mr Chris Kettle's model scanning guidance.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
