Abstract
Objective
Ultrasound visual biofeedback has the potential to be a useful tool in cleft palate ± lip care but there is little research on its effectiveness, nor on clinicians’ views on using it in research and practice. This study reports on cleft-specialist speech and language therapists’ (SLTs) views on the acceptability of the technique in clinical practice and on their readiness to contribute to future clinical trials of its effectiveness.
Design
A qualitative design comprising semi-structured focus groups/interviews.
Setting
Clinicians reflected on how easy it would be to use ultrasound in their regional cleft services.
Participants
Clinicians were recruited via invitation to a UK-wide list of cleft-specialist SLTs. Eleven participants took part over 2 focus groups and 2 interviews.
Analysis
Focus groups/interviews were recorded, transcribed verbatim, and an inductive thematic analysis was undertaken. Once complete, a deductive analysis using the theoretical framework of acceptability was conducted to summarise the findings.
Results
Four themes emerged: (1) value of ultrasound as an approach; (2) intrinsic drawbacks of acquiring and utilising ultrasound; (3) competence in effective performance within a clinical trial; and (4) incentives for clinicians and patients in participation in research.
Conclusions
Participants were positive about the benefits of ultrasound for visualising the articulators and improving patient outcomes. Barriers to adoption included the cost of the equipment and the time to travel to appointments. Across clinical and research uses of ultrasound the need for high-quality training and networking within a community of practice was highlighted.
Introduction
People with cleft palate ± cleft lip (CP ± L) can have ongoing difficulty with speech. Often these errors are described as “active” (learned) errors. 1 That is, speakers may mis-learn an articulatory placement to compensate for anatomical differences, even when these differences have been surgically corrected. These errors contrast with “obligatory” (passive) errors, such as hypernasality, which are not stimulable for speech intervention and may require further surgeries. Speech and language therapy for active errors can be effective, but there is no single intervention recommended. 2 Historically, intervention has focussed on articulatory placement: teaching speakers how to change erroneous articulations and then using the principles of motor learning to practice and then stabilise new articulations. This can be challenging because a common active error in CP ± L is backing of anterior consonants to more posterior places of articulation and this is difficult to describe and visualise. For example, /t/ may be realised at a velar or uvular place of articulation, but the main articulator, the tongue, is hidden from view and it is difficult for speech and language therapists (SLTs) to describe these invisible articulatory movements. One solution is using articulatory instrumentation to visualise the articulators in real time and use this for biofeedback. 3 Over the last 6 decades many small studies have used electropalatography (EPG) effectively to visualise tongue–palate contact for biofeedback. However, despite the longevity of this technique, robust evidence for its effectiveness remains limited to 1 small parallel design study meeting the inclusion criteria for a Cochrane Review. 4 In 2007 the CLEFTNET project 5 aimed to support all cleft centres in the UK to offer EPG for children and young people with persistent active articulation errors. Despite this initiative, EPG has not become a standard intervention across the UK; further research studies have remained at the case study level of evidence (see e.g. Patrick et al. 6 ) and many centres in the UK no longer offer this treatment.
Reasons for the slow adoption and lack of more robust research studies are not well explored, but Cleland 7 suggests that this might be because EPG requires expensive bespoke equipment and individualised hardware; it can only be used when children have stable dentition and no planned surgeries; and SLTs who use it need to be trained in the technique. Instead, a different biofeedback technique: ultrasound visual biofeedback (U-VBF) is suggested as a cheaper, more accessible alternative. With this technique a standard medical ultrasound probe is positioned under the chin, showing a real-time mid-sagittal view of tongue movements. Ultrasound has very little ongoing costs, and it does not rely on speakers having stable dentition. It also shows promise as an effective tool with children with other types of speech sound disorders 8 and has been used in randomised controlled trials (RCTs) with children with childhood apraxia of speech. 9 There have been recent advancements in portability, software development, and a framework for using ultrasound in practice has been endorsed by the UK Royal College of Speech and Language Therapists.9,10
Moreover, a small number of case studies using U-VBF with children with CP ± L have demonstrated improvements in accuracy of targeted consonants.11–13 Other studies have used ultrasound as an assessment tool with larger numbers of people with CP ± L and have shown that it can detect specific speech errors.14–16 There is clear potential for U-VBF to become a useful tool for establishing articulatory placement in speakers with CP ± L, but for this to be realised there are 3 key hurdles that need to be overcome. Firstly, we need to determine the acceptability of this technique to people with CP ± L; secondly, more robust clinical trials are required; and finally, we need to understand the barriers and enablers to SLT services for adopting the technology and taking part in clinical trials. These factors are interlinked. A recent feasibility RCT 17 has shown that it is possible to recruit and retain families to an RCT comparing U-VBF to articulation therapy and that U-VBF can be delivered with good fidelity. 18 A linked study looking at families’ perspectives on U-VBF and taking part in the same clinical trial showed that families find randomisation and the burden of extra assessments acceptable. 19 Moreover, those that received U-VBF highlighted how enjoyable the intervention was, with being able to see their tongue movements being particularly enlightening. U-VBF therefore shows promise as not just being acceptable to patients, but indeed a desirable technique in terms of patient satisfaction.
The final hurdle, cleft-care clinicians’ perspectives on using the technology both clinically and in research studies, is not well explored. Dugan and colleagues 20 interviewed 7 SLTs about their experiences of using U-VBF with children with other types of speech sound disorder (SSD). All of the participants in this study had gained experience with the technique via university research, rather than in community or hospital settings. The biggest barrier was a difficulty accessing the equipment and the most frequently mentioned benefit was the ability to visualise articulations, in line with the key benefit cited by families. 21 Some SLTs found the U-VBF easy to use, while others found that the images could be blurry and difficult to interpret. Solutions to this included modifying the ultrasound equipment to enable SLTs to draw the desired tongue shape on the screen or adding animations to the image (note, the software used in Cleland et al. 17 has this feature, videos can be viewed at www.speechstar.ac.uk). All SLTs thought that to use U-VBF additional high-quality training was necessary. The North American SLTs in this study thought that a key barrier for patients was the cost, since intervention delivered in universities was often not covered by insurance. Moreover, there were costs involved in travelling to the clinic since U-VBF cannot easily be delivered remotely. The burden of travel was also a top barrier for families in the above feasibility study with children with CP ± L, 21 although costs of the treatment were not an issue since in the UK speech and language therapy is provided free at the point of access.
For services to adopt a new intervention there should be robust evidence of improved outcomes for patients. Ideally any clinical trial which aims to measure the outcomes of U-VBF would involve the clinicians who will eventually deliver the intervention in their services, to ensure that its delivery is practical and achievable. Finch and colleagues 22 suggest that there is low confidence amongst SLTs to undertake research tasks and that overcoming this is crucial. Moreover, time to undertake research is limited. This, coupled with the lack of confidence of using a new technology such as ultrasound needs to be explored. Several studies have looked at how SLTs feel about adopting technology into their practice. For the most part SLTs adopt technology when it is convenient, easy to use, and recommended by others, 23 with empirical support for the technology being less important. However, previous studies have tended to look at the adoption of low-cost apps, which often have limited evidence base, but may be used to provide, for example, games and activities in intervention. Clearly the use of a medical imaging modality such as ultrasound encompasses learning to use a new technology (e.g. the software); becoming skilled in using a medical imaging technique; and becoming skilled in delivering a new intervention. SLTs’ perspectives on using U-VBF are therefore likely influenced by all 3 of these factors. While the use of medical imaging is scarce in management of most childhood speech disorders, SLTs who work with children with CP ± L may have previous experience using EPG for working on articulation and videofluoroscopy or nasendoscopy for evaluating velopharyngeal function. This group of clinicians may therefore have prior experience in learning to use medical imaging techniques compared to community paediatric SLTs. Given the complexity of the issues surrounding the perspectives of SLTs of using U-VBF in research and practice, this study took a qualitative approach to gain as wide a variety of views as possible.
Aims
This study had 2 key aims. Firstly, to determine the acceptability of U-VBF to SLTs with experience of working with people with CP ± L. Secondly, to determine the barriers and enablers to SLTs taking part in a future randomised clinical trial of U-VBF compared to treatment as usual. In this study we aimed to gain the views of SLTs who had limited experience of U-VBF, in both research and practice, in order to inform future implementation of U-VBF research and practice in cleft centres.
Method
The study used a qualitative design comprising semi-structured focus groups and interviews with SLTs. A topic guide for the focus groups was developed from 2 sources. First, the topics regarding acceptability of U-VBF were developed based on the theoretical framework of acceptability (TFA) by Sekhon et al., 24 these topics were discussed first. This framework comprises 7 constructs: affective attitude, burden, perceived effectiveness, ethicality, intervention coherence, opportunity costs, and self-efficacy. These constructs determine how a clinician perceives an intervention's appropriateness and acceptability. For example, the construct “burden”, is defined as “the amount of effort required to participate in the intervention”, and might encompass areas such as the dosage of the intervention. Definitions for all constructs are given in Table 1.
Deductive Coding into the Theoretical Framework of Acceptability.
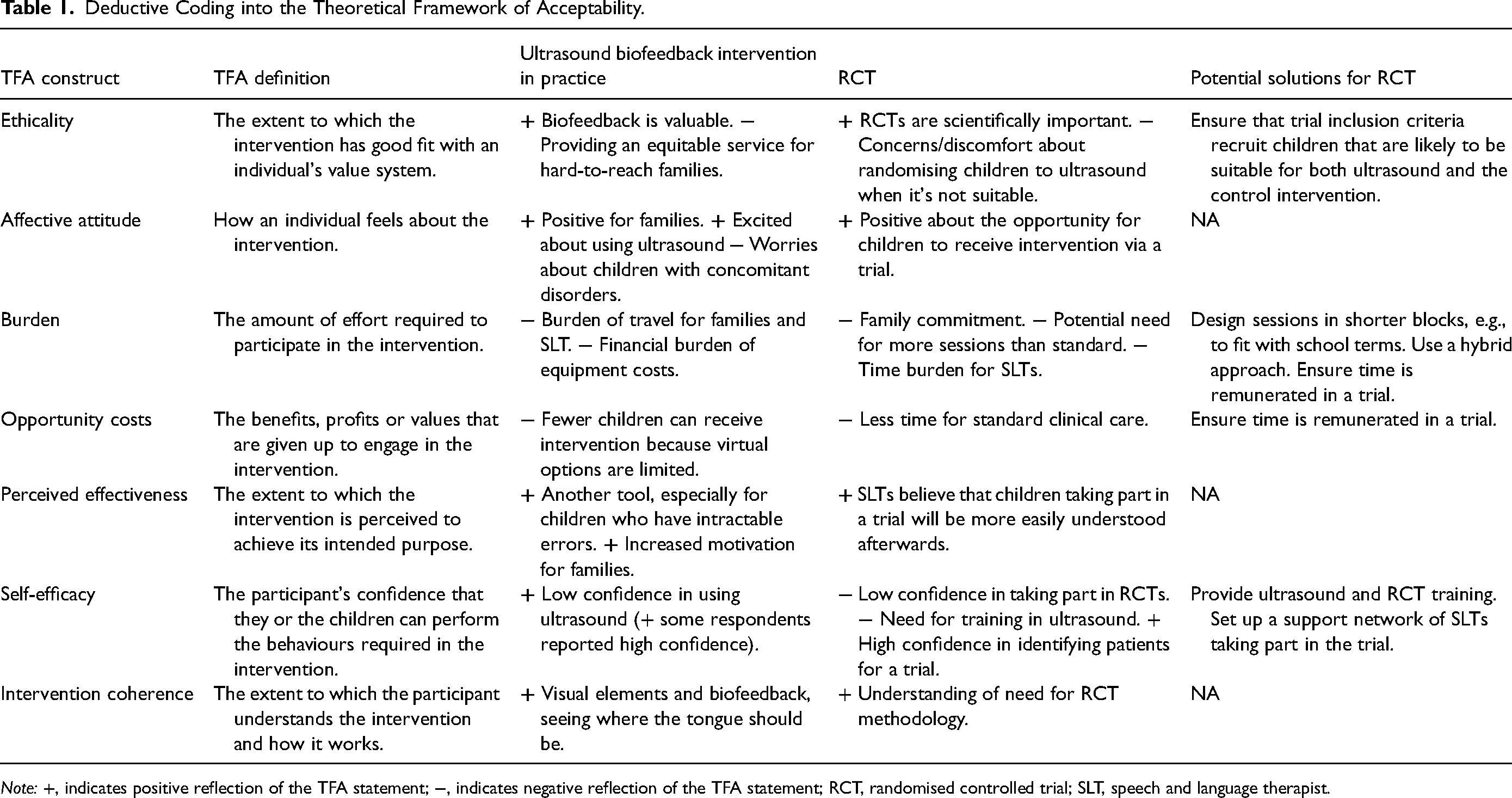
Note: +, indicates positive reflection of the TFA statement; −, indicates negative reflection of the TFA statement; RCT, randomised controlled trial; SLT, speech and language therapist.
Second, topics about the barriers and enablers to participating in a clinical trial comparing U-VBF with standard care were adapted from a study about healthcare professionals recruiting to trials. 25 The topic guides are available on the OSF (https://osf.io/a7vgt/). Topics were specific to the use of U-VBF in practice and in a clinical trial, though participants were free to compare the intervention to others they had experience of, such as articulation intervention or EPG.
This study was approved by the Department of Psychological Sciences and Health, University of Strathclyde Ethics Committee. All participants consented to taking part.
Participants
Participants were recruited via email to the UK Cleft and Craniofacial Clinical Excellence Network. We requested that specialist cleft SLTs who were interested in taking part in a focus group to contact the qualitative researcher (second author). We specifically stated that we would like to have a balance of people who have some experience with ultrasound, those who don’t yet have experience but would like to, and those that can’t envisage their service providing ultrasound at any time in the near future to gain a diverse range of perspectives.
Fourteen participants contacted the researcher to express interest and 11 took part across 2 focus groups and 2 interviews, see Table 2 for participant details. Groups and interviews were scheduled according to the availability of participants.
Participant Details.
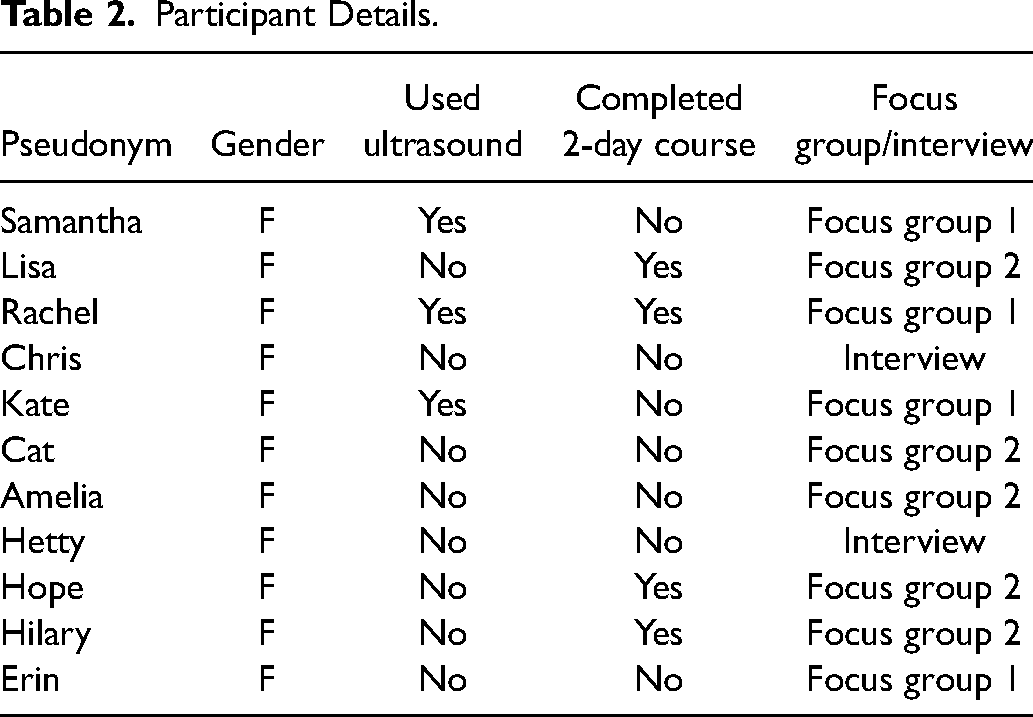
Participant's Prior Experience with Ultrasound in Research and Practice
Of the 11 participants, 3 had prior experience using U-VBF in their workplace, although this experience was relatively new. One year prior to the current study, the first and third authors had invited a representative from each of the 16 cleft centres in the UK to a 2-day training course on U-VBF. These SLTs were not excluded from the current study, but the authors who provided the training were not involved in the focus groups or interviews. Lisa, Rachel, Hope, and Hilary had taken part in the training (see Table 2). No participants in the current study had collaborated on prior ultrasound research with the study team; however some participants had taken part in a trial evaluating the timing of primary surgery. 26 Involvement in this trial was constrained to recording participants’ speech at specific time points, rather than providing speech interventions.
Data Collection and Analysis
Focus groups/interviews were conducted online using Microsoft Teams by the same qualitative researcher (second author) who had previously interviewed families about their views on taking part in a clinical trial of U-VBF. 21 This researcher is a clinical psychologist with no experience of speech and language therapy or CP ± L. The groups/interviews were semi-structured with open-ended questions. They were recorded in Microsoft Teams, transcribed verbatim, identifying information removed, and analysed by the same qualitative researcher using inductive thematic analysis, in line with our previous study with families. 21
Once the inductive thematic analysis was complete, the first author used the theoretical framework of acceptability 24 to deductively code into the 7 intervention acceptability constructs. We present these as a summary in Table 1.
Reflexivity and Trustworthiness
To enhance trustworthiness a researcher who was not familiar with U-VBF or cleft care conducted the focus groups/interviews and performed the inductive analysis. Given that some participants had taken part in a training course provided by the first and third authors, there was a risk that participants may have felt coerced to respond positively. To mitigate this, we employed a researcher from outside the field and email invitations made it clear we were seeking positive and negative views. Nevertheless, we acknowledge that those who volunteered may have had prior positive views about U-VBF. All the authors critically examined the interpretations and conclusions drawn from the data. No changes were made to the thematic analysis by any of the other authors. To enhance transferability, we include a detailed description of the data collection processes and make available the topic guide.
Member Checking
A draft of this manuscript, including the thematic analysis below, was sent to all participants to check their views were represented accurately. Participants were given 1 week to respond or suggest changes. Four participants responded. One noticed an error in the pseudonymisation, this was rectified. One requested a statement that they felt could identify their workplace be removed, this was therefore removed. One asked that we change a statement about “SLTs being underconfident in research” to “some respondents were underconfident.” All responded that this paper, with these revisions, is a fair and accurate account of their views.
Results
Inductive Thematic Analysis
Four main themes were developed: (1) perceptions of the value of U-VBF as an approach (biofeedback, transportable, understanding, less invasive); (2) intrinsic drawbacks of acquiring and utilising U-VBF for practitioner and patient (financial, confidence, child-related difficulties, travel/accessibility); (3) fundamental perspectives on undergoing an RCT and competence in effective performance within the trial (feelings about RCT, recruitment, skills/resources needed to execute, sessions/dosage); and (4) incentives for SLTs and patients in recruitment and participation in research.
Theme 1: Perceptions of the Value of Ultrasound as an Approach (Biofeedback, Transportable, Understanding, Less Invasive) in Practice
SLTs showed their want and excitement for new approaches, especially the use of U-VBF. Evident amongst the SLTs was optimism in the use of U-VBF giving them “Another tool in the toolbox” (Chris, 5) and “adding another string to the bow” (Amelia, 912). All participants agreed in the positive use of U-VBF creating “another option” (Hope, 19), with SLTs being “very keen to get my hands on ultrasound” (Kate, 24). Visual components to U-VBF were prevalent throughout the discussion, with it being a unique addition compared to standard therapies. This was seen as a helpful element for patients and SLTs, allowing SLTs to show patients what is being asked of them. Samantha describes the importance of seeing what is happening inside the mouth: You can explain until you're blue in the face about what a child needs to do with their tongue, but because they can't see it as easily, I don't think that they always get it. So adding that visual component so you can talk about what's on the screen and what's happening and what they are doing … So having that visual component I think is just, you know, obviously the really important thing with and then the thing that makes it different from other approaches that we use. (Samantha, 394–401)
Moreover, U-VBF helps in understanding in what is expected within therapy It might help that kind of biofeedback in the child, really think about what they're doing, and the parent also see what their (child's) tongue is doing, and what it needs to be doing. So I think for lots of families, it's going to be a positive thing to kind of understand a bit more about what we're trying to achieve. (Hope, 605–609)
Understanding articulation is highly important to the SLTs “for them to understand, really understand visually where their tongue is and where it should be” (Cat, 674–675).
Many SLTs compared U-VBF to EPG. The lack of portability of the EPG was given as a downfall in comparison to ultrasound: it is more portable than EPG. So I guess you know you could offer that ultrasound a lot more easily out in the community because it's transportable. (Kate, 223–225)
The SLTs “love that the ultrasound is so portable” (Rachel, 322) allowing it to be a better approach within the community being “something that we could use” (Hetty, 45–46), as well as the portability issue, EPG requires “dental plates” (Hetty, 23). In comparison U-VBF was agreed to be “not invasive” (Hetty, 87): it's not invasive, but it is a little bit more invasive than just looking at pictures and saying words. (Cat, 713–714)
The positive impact of having another “tool” to use during therapy sessions shows the high value of U-VBF especially for children with more intractable cleft speech characteristics, “there are some children where you get really stuck and you think, oh, I wish I could ultrasound them” (Chris, 8–9). Perceptions of U-VBF are “hopeful” and “excited” to see where this technique leads.
Theme 2: Intrinsic Drawbacks of Acquiring and Utilising Ultrasound Therapy in Practice for Practitioner and Patient (Financial, Confidence, Child-Related Difficulties, Travel/Accessibility)
SLTs discussed practical struggles in acquiring and using U-VBF. Although participants were overall positive towards using ultrasound, obtaining the machine financially was seen as a “hurdle” (Hetty, 605). Financial was the biggest struggle in beginning U-VBF with SLTs still trying to procure machines or not yet able to use them. Budgeting for the services was a large issue with Amelia stating it would be “very difficult because of finances and potentially governance” (Amelia, 112–113). Hetty explains the budget provided to SLTs and why this cost is such a problem for the new technique: it's frustrating because it's such a tiny amount within the NHS budget. We're talking a few thousand pounds. It's peanuts. But for a speech therapy budget, when to maybe buy a handbook of resources is £50 or something like that to say well actually, I want £5000 for an ultrasound machine and the software that goes with it, or whatever that would seem as being a massive amount when actually it isn't really. (Hetty, 75–80)
Conversely, Hope states The way that I'm thinking about it is that it's a one-off payment. So compared to EPG that is per patient an additional cost” (Hope, 456–457). “It's the funding I think getting the equipment is the big one, especially in the NHS. (Chris, 22–23)
A further barrier was SLTs’ low confidence in using ultrasound. Only 2 SLTs felt “reasonably confident” (Samantha, 538) in its use with Rachel stating, “therapy wise, yes, happy, confident” (517) though said she has not used this technique in assessment yet. All other participants found themselves struggling with their confidence due to issues such as lack of practice, understanding, and training: So if ten is like the most confident I can do it, and I'm Joanne Cleland (the first author) and a zero is, I can't do it at all. I think I'm probably like a five to six at the moment in that I think I've done all the reading and done the training. I've looked at all the things I can look at and I think until I actually do it now I'm, like, you kinda learn most by doing. (Chris, 94–97)
Chris commented on the lack of practical learning after doing all the “reading” and “training” this is echoed by other participants who state the importance of the training to be competent. Lisa comments on the positive boost in her confidence after the training with the first and third author: I read a few things and I just thought this this is something I will not be able to do. It was all just blurry lines, but after Joanne Cleland's (the first author) session I thought actually, yeah, it does make sense and it seemed a lot more sort of user friendly than electropalatography. (Lisa, 753–736)
Lisa goes from no confidence and feeling like this is a therapy she will “not be able to do” to understanding ultrasound and stating it as “a lot more user friendly”. Although participants’ confidence was low, their belief in learning is high, being happy to “just give it a go” (Hope, 725) and feeling confident to “know how to get that support” (Hilary, 735).
Participants also discussed child-specific worries including concomitant disorders and sensory issues that might affect application of ultrasound, though they felt “so used to being adaptable and thinking about individualising the choice of what therapy we're doing” (Hilary, 258–259). Concomitant disorders which could affect U-VBF were discussed as the main drawback: I just wondered about the children with bone anchored hearing aids or the cochlear implant if there is that. I think we did discuss that, but I can't remember what Joanne said. But that that was the only thing really that I wondered if the headset might not suit them and if it kind of it does it exclude that group. (Lisa, 281–284)
The headset (note, using a probe holding headset is optional, but its use is standard in the UK) was also commented on regarding the sensory elements that children may struggle with: the only obstacle that I've slightly come across was a child with autism who didn't like the gel or the headset particularly being on. (Kate, 233–235)
Amelia also named the “cold gel” as a sensory factor. With this the adaptability of the SLTs showed again commenting that “That sort of applies to any intervention, doesn't it?” (Amelia, 248) regarding sensory issues in therapy, showing their ability to “individualise” therapy for the child.
There were also barriers regarding patients’ ability to travel to clinics. SLTs reviewed the issues some of their patients have regarding “cost” of travel and “parking”: I know that for some families they have to rely on public transport to get here and therefore it might cost them quite a bit or it, you know, some of the clinics you've got to pay for parking. (Hetty, 682–684)
Hetty points out the fact that not all parents own a car which can be a struggle in offering an “equitable service” (Lisa, 169). Cat discussed the extremes families go to gain therapy for their child: “we've had patients fly in from the Isle of Man to receive speech therapy fortnightly because they weren't getting anything” (Cat, 835–837). Cat states the alternative to not travelling is not “getting anything” where distance is again a factor, “lots of our rural children have less options for speech therapy with a specialist within the cleft team. So then it tends to be virtual so they can have input” (Rachel, 214–216). The use of virtual input is problematic for U-VBF: I will not be able to justify coming out of clinic for a session to see one patient in the school. But I could see three patients and three different schools in a morning quite easily online. (Amelia, 1177–1179)
Theme 3: Fundamental Perspectives on Undergoing an RCT and Competence in Effective Performance of Trial (Feelings About RCT, Recruitment, Skills/Resources Needed to Execute, Sessions)
SLTs discussed participating in an RCT comparing U-VBF and articulation intervention citing “worry” and “uncomfortable” feelings regarding randomising the children into either Ultrasound or Articulation therapy groups: I think not 100% comfortable, but I don't know. I just can't imagine how we would be able to do that because with some of the younger ones, if they couldn't cope with the ultrasound and if you randomise them to ultrasound, then …it would be the wrong therapy for them. (Cat, 1231–1234) if it was randomised then obviously then you can control certain criteria and I would worry that certain children might not be able to cope with the equipment. (Samantha, 849–851)
Coping with group allocation was a main issue in randomising participants, especially towards the U-VBF, worrying about the ability to cope with the equipment “we might be just setting them up to fail if they were in an ultrasound group and they couldn't cope with it” (Rachel, 840–841). Amelia brought up the factor of “harm” where she would be “more comfortable randomising a group of patients where I was fairly confident in either approach would be would not cause harm” (Amelia, 1256–1257). This was balanced by other SLTs who supported the use of RCT methodology: I don't have a problem with it because I know that it strengthens the methodology of research, so for the greater good. I think. (Chris, 242–243)
Chris shows their willingness to use the RCT method as it “strengthens” research providing “proof” which Hetty states “one of the difficulties with speech therapy is a lot of what we do hasn't got the exact scientific basis” (Hetty, 455–456). Although their perspectives on randomisation were varied and hesitant, this was contrasted by their comfort in identifying patients for a trial which was a resounding “yes” and recruiting to a trial with “plenty of families” (Rachel, 720), and “In terms of confidence to like identify appropriate children, I'd say a ten” (Chris, 204–205). The discussions showed the SLTs were confident and comfortable in their ability to recruit children especially due to the high volume of patients they have with “children coming out of our ears” (Amelia, 1109). Kate states: From our services’ point of view, the Cleft services I don't think recruitment would be a problem… There are plenty of families I think that would be happy to participate. (Kate, 745–747)
Emphasised is the fact there are “plenty” of families due to the demand for therapy and growing waiting lists, “I think they're such a demand for speech therapy that parents would probably bite our hand off if you were offering this package” (Samantha, 725–726). The only worry focused on was the family's ability for “commitment” to the hypothetical trial.
The expertise to carry out the therapy after recruitment with skills and resources were discussed which contributed to the SLTs’ feelings of competency. Gaining access to the equipment to perform a trial with Erin stating, “an Ultrasound” (Erin, 1059) when asked about resources. The lack of equipment within the services was evident: An ultrasound machine, if we're going to be doing the interventions like locally, then yes, we don't currently have an ultrasound machine here. (Chris, 337–339)
Skill in being able to work the Ultrasound effectively was stated as “essential” in performing a trial effectively: I think it would be essential, surely, to have at least a baseline level of skill in use of ultrasound in order to make it a level playing field. If you're comparing ultrasound with other therapy approaches. (Amelia, 1060–1063) I think they would need ultrasound training … I want to say basic, but I don't actually think it would be basic. I think they'd have to be fairly competent or quite competent in just general kind of speech sound work. (Chris, 187–190)
There is need for “training” and “skill” to perform U-VBF effectively within a trial setting to “make it a level playing field”. SLTs stated they “wouldn't feel skilled to do it” (Erin, 680) regarding U-VBF without training. Citing the 2-day course, certain participants had participated in in the past, they said that this made them feel more “confident to give it a go” (Samantha, 670). Having the time to undertake research was also important with participants showing their struggle to find time within their: Like at therapy, time is a resource, isn't it? So most of clinical time really. (Lisa, 1398–1399)
Given that research studies often employ dosages higher than those used in clinical practice, we asked SLTs to reflect on the ability to provide up to 20 intervention sessions. Their time was limited due to factors such as “capacity” (Chris), “maximum standard” (Chris), “annual leave” (Amelia), “people get sick” (Kate) and “holidays” (Rachel) which all caused hesitation for more intense trial dosage. Hetty states that “20 weeks would be difficult to offer” (Hetty, 625) with it being “challenging as a clinician to make sure that I'm around for 20 weeks in a row” (Samantha, 1105–1106). Although 20 weeks in a row is “difficult” (Erin, 1093) Rachel states: majority of my cleft kids will have … closer to 20 than they will to 6 purely for the progress tends to be slower initially while they're getting the hang of finding that alveolar position. (Rachel, 1082–1087)
With 20 weeks being more possible with “flexibility” (Kate, 1114) and “consecutively weekly sessions” (Samantha, 1100) being possible in blocks of 10 rather than 20: I think that's always been the case that it kind of like 10 sessions over a term is quite useful way of seeing things. But I think if you're going to do 20 kind of every week that would be difficult for families. (Erin, 1092–1094)
With 10 sessions over a term being feasible “a couple of blocks of 10” (Samantha, 1106) is a useful way to see things focusing on working to a “termly basis” (Hetty, 622).
Theme 4: Incentives for Therapists and Patients in Recruitment and Participation in Research
SLTs discussed positive incentives to take part in a trial and for patients to participate in research, mentioning multiple factors that were rewarding. Many therapists talked about the networking benefits of research, being able to discuss and bounce off fellow therapists asking questions such as “how are you using it (the ultrasound)? What have you found?” (Hetty, 316) which would not normally be possible for most especially within the community and the prevalence of solo work: therapists like being involved with research projects because it allows them to network with other therapists and in terms of kind of professional development it can be enormously beneficial. (Kate, 1170–1173)
Kate specifically states that research projects “allows” networking benefiting their “professional development”. Samantha cites the focus group as reference to what could be helpful for clinicians: having access to a group of clinicians who are doing the same thing like we’re sort of doing a little bit today if you had like meetings with the other therapists involved in collecting the data then I think that would be really helpful. (Samantha, 1182–1184)
Incentive of networking contribution was positively addressed by SLTs after usually working “autonomously” (Lisa, 1332), being able to discuss in small groups was a positive incentive for trial participation and further learning. Having “access” to research also gives ability to learn new skills which SLTs were keen to do: I think the idea of being able to develop your skills and technique would be motivating. (Kate, 1169–1170)
Participants discussed the incentive for learning “an additional set of skills” (Lisa, 1528) regarding U-VBF, “just not necessarily to have ultrasound funded, but have the therapy skills” (Lisa, 1530–1531) the incentive for research being based in long-term knowledge of ultrasound skills.
Finance was a consistent issue for the therapists with discussions of incentivisation surrounding the financial burden to be aided. Hilary states: be paid for the separate time (i.e. the additional time for research activities should be costed) rather than have that taken away from my clinical time that would be an incentive. (Hilary, 1520–1521)
Protected time to complete the trial and not take away from general clinical practice were essential. Compensation for “travel costs and clinical time” (Lisa, 1537) were an incentive to the SLTs but also the trusts (services) they work within “I think finances to actually recruit or allocate dedicated sessions I think would be an incentive to certainly the trusts” (Amelia, 1523–1524).
SLTs believed the main incentive for families was the ability to get more therapy and overall improved speech “I mean the main incentive is that they’re going to get therapy isn’t it?” (Kate, 1167–1168). Along with getting therapy being “seen faster” (Chris, 419) due to having access to a trial whilst also getting more therapy than usually offered as Hetty stated “you're getting more therapy than you would otherwise have had” (Hetty, 772–773). The incentive of more therapy, getting therapy, and being seen faster, were the main incentives echoed by all practitioners: what would it look like if your child was understood? (Hetty, 713–714)
Hetty resonates the therapist's main objective to benefit their patients and overall incentive to improve speech.
SLT's Perspectives Within the Theoretical Framework of Acceptability: Deductive Analysis of Focus Groups/Interviews
To summarise the SLTs’ perspectives on the acceptability of U-VBF and of taking part in a trial, we performed deductive coding in line with the theoretical framework of acceptability. 24 This was applied once the inductive thematic analysis detailed above was complete. Results are presented in Table 1, with positive and negative comments indicated in each of the constructs. Columns 3 and 4 detail whether these comments relate to the use of U-VBF in practice, or to its use in a trial. This analysis revealed that there were more positive than negative themes regarding acceptability of U-VBF, but more negative themes regarding taking part in a trial. We therefore give potential solutions in column 5 where possible. These are explored further in the discussion.
Discussion
This study sought the views of SLTs working with people with CP ± L on the acceptability of using U-VBF in research and practice. Previous studies have determined that patients and carers find U-VBF an acceptable and indeed enjoyable intervention technique. 19 Moreover, they report that taking part in a pilot RCT is both acceptable and feasible for families. 19 Families cite the visual element of U-VBF as being transformative in their understanding of articulation and in their child's progress in acquiring new articulations. However, U-VBF is not yet integrated into routine care 7 and research looking at the barriers to adoption of this technology from the perspectives of clinicians has been limited to a small study of North American clinicians providing U-VBF via university research clinics. In this study, we sought the views of SLTs working in community/hospital locations with people with CP ± L. The clinicians in our study work within the publicly funded National Health Service where intervention is provided free at the point of access. We included both those with some prior experience of U-VBF and those new to the technique; none of the participants had taken part in research using U-VBF. Crucially, we expanded the research area to incorporate perspectives on contributing to future clinical trials with this technique. This is important, because currently the evidence for U-VBF with patients with CP ± L is weak, so while our results show enthusiasm for adoption of this technology, enthusiasm for taking part in empirical trials of the technique was more reserved. Below we explore the acceptability of U-VBF in research and practice and make recommendations for ensuring future clinical trials are acceptable to clinicians.
Using U-VBF in Practice
In line with Dugan et al. 20 clinicians were consistently positive about the potential benefits of U-VBF to visualise the articulators. Children with CP ± L often have difficulty with the acquisition phase of motor-based interventions, with backing patterns of articulation common. Using ultrasound, clinicians could see a clear benefit to being able to work on achieving these often-intractable speech errors. The benefits of visualisation chimed with the views of carers of children with CP ± L who also cited this as a key benefit. 19 Articulatory biofeedback techniques therefore have high intervention coherence 24 (Table 1) to both carers and clinicians: that is, it is clear to both the patient and the SLT how and why U-VBF intervention works, this in turn results in high affective attitude towards the intervention.
Many of the clinicians in this study compared U-VBF to EPG. Cleft care in the UK is in a unique position in that there is a history of EPG being offered to patients with particularly intractable articulation disorder, 5 although more recently EPG has been discontinued in some centres. The theoretical underpinnings of the intervention are the same, 3 although the actual equipment is very different. In line with previous expert opinion that EPG has not become standard care in the UK due to practical issues, 7 clinicians thought that U-VBF was more portable than EPG and that although the initial equipment is expensive, there are less ongoing costs. While EPG requires stable dentition, the SLTs in our study highlighted other child-specific factors, such as sensory issues which may hinder the use of U-VBF, particularly if it is used with a probe-stabilising headset. Nevertheless, the clinicians did highlight that an individualised approach is always necessary with this group of patients.
Self-Efficacy, Confidence, and Training
Self-efficacy (Table 1) was a particular concern, with confidence and training needs a barrier that spanned using U-VBF in both research and practice. Dugan et al. 20 found that clinicians believed that they need specialised, high-quality training in order to use U-VBF, and our respondents made very similar reflections. This is not surprising. While undergraduate courses include teaching on understanding articulation, this often does not incorporate using medical imaging. The Royal College of Speech and Language Therapists identify using ultrasound as “extended scope of practice”, 10 and therefore training and hands on experience are necessary. The SLTs in our group who had received such training reflected on it positively and believed that once they had undertaken training then with practice and support from other colleagues, they could become skilled in the technique.
Likewise, some SLTs felt underconfident in taking part in research. Previous studies 22 have suggested that there is low confidence amongst SLTs to undertake research and that overcoming this is crucial. While low confidence in research is not specific to trails of U-VBF, in this study low confidence was confounded by a lack of confidence in using the ultrasound. However, the clinicians were enthusiastic about the prospect of receiving ultrasound training, joining a community of practice, and the upskilling opportunities that taking part in a research project provides. They were also very positive about their ability to recruit patients to a trial comparing U-VBF and articulation intervention. This coupled with previous positive perspectives of families 19 suggests that there is appetite for further clinical trials in this area if high quality training can be provided.
Burden of U-VBF in Research and Practice
Financial considerations are a significant burden (Table 1), both for adopting U-VBF in practice and for a clinical trial. These concerns were both from the viewpoint of the health service (cost of equipment) and the patient (travel costs to the clinic). The burden of travel was a key concern in previous research,19,27 both in terms of time and financial costs. While other types of intervention, such as articulation therapy may also require travel to clinics, intervention which does not involve instrumentation may be more amenable to provision via telehealth. In the previous qualitative study of USA-based clinicians 20 there were concerns that U-VBF would not be covered by medical insurance. While that is not a concern in the UK, the National Health Service in the UK is generally considered to be underfunded (https://www.bma.org.uk/advice-and-support/nhs-delivery-and-workforce/funding/health-funding-data-analysis) and SLT funding typically does not include large equipment budgets. The solution to this is to provide more robust empirical evidence that U-VBF is both effective and efficient so SLTs can make a case for purchasing equipment. Previous studies of EPG 28 have shown that instrumental techniques can reduce the time needed in intervention and further research looking at the health economics case for U-VBF is needed. Further concerns were voiced about the time commitment to take part in a research trial, including being able to offer an adequate dosage of U-VBF. Again, these concerns are budgetary and would apply to any intervention trial. Clinical trials of U-VBF should therefore be adequately resourced.
The SLTs in our study were aware that RCTs are the gold standard for measuring the effectiveness of an intervention, indeed some SLTs had been part of a previous trial looking at the timing of primary surgery. 26 They were confident about recruiting to a trial of U-VBF, but there was general unease, or ethicality concerns (Table 1), about the randomisation process, particularly if children were randomised to an intervention that the SLT believed would be unsuitable. In a pilot RCT comparing U-VBF to standard treatment, patients and families expressed no such anxiety about randomisation and participants in both arms of the trial were positive about their experiences. 19 This is perhaps because in that trial, the inclusion criteria were designed by clinicians experienced in using U-VBF to ensure that children would benefit from either U-VBF or the control intervention. Although SLTs were aware of the necessity for robust clinical trials, they did express conflict between this and their duty of care towards individual patients to ensure they receive the right intervention for them. Again, the solution to this is to carefully design the inclusion criteria for a trial and ensure adequate training for those recruiting families to ensure the experience is positive for both clinicians and patients.
Limitations
A key limitation of this study is sample size. We purposely limited our sample to UK clinicians working with CP ± L, but caution should be taken in applying our results to other cultures or with other client groups given these clinicians may have had prior experience using articulatory biofeedback such as EPG. Moreover, clinicians working with this client group may be more familiar with RCTs as this design is commonly used in the multi-disciplinary teams they are part of, for example some of our clinicians had experience of providing audio recordings as part of an RCT looking at the timing of primary surgery. 26 A further important limitation is that it was difficult to determine if the SLTs who took part in our focus groups were pre-disposed to being positive about U-VBF. Indeed, our respondents were very positive about the intervention: negative responses tended to focus on factors such as costs and practicalities. One solution to this would be to employ mixed-methods, using a survey of a larger number of clinicians.
Conclusions
For U-VBF to be adopted into clinical practice there are three key hurdles: the acceptability of the technique to people with CP ± L; an understanding of the barriers and enablers to SLT services for adopting the technology and taking part in clinical trials; and finally robust evidence from these trials is needed. Previous research has shown that the technique is indeed acceptable to people with CP ± L and their families. 19 This study showed that SLTs working with people with CP ± L are encouraged about the potential benefits of ultrasound for visualising the articulators and improving patient outcomes. However, to enable them to use this technology in research and practice they require access to the equipment, high-quality training, and support from a community of practice. There remains a need for robust clinical trials of U-VBF, but the findings here suggest these should be adequately resourced and inclusion criteria should be carefully designed to ensure clinical equipoise.
Supplemental Material
sj-docx-1-cpc-10.1177_10556656251322279 - Supplemental material for Clinicians’ Perspectives on Using Ultrasound Visual Biofeedback for Research and Practice with People with Cleft Palate ± Cleft Lip
Supplemental material, sj-docx-1-cpc-10.1177_10556656251322279 for Clinicians’ Perspectives on Using Ultrasound Visual Biofeedback for Research and Practice with People with Cleft Palate ± Cleft Lip by Joanne Cleland, Robyn McCluskey, Maria Cairney, Lisa Crampin and Linsay Campbell in The Cleft Palate Craniofacial Journal
Footnotes
Acknowledgements
Thank you to the speech and language therapists who took part in the study.
Data Availability
The data that support the findings of this study are available on request from the corresponding author. The data are not publicly available due to privacy or ethical restrictions.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Statement
Ethical approval for this study was granted by the University of Strathclyde. All participants gave signed consent.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The study was funded by the Chief Scientist Office of Scotland, Grant Number TCS/20/02.
Participant Consent Statement
This study was approved by the Department of Psychological Sciences and Health, University of Strathclyde Ethics Committee. All participants gave informed consent.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
