Abstract
Objectives:
Research has identified adults born with cleft lip and/or palate (CL/P) to be at risk of poorer psychological outcomes compared to the general population. This study investigated factors that may contribute to positive and negative adjustment in adults born with CL/P.
Design:
A survey was designed and distributed by the Cleft Lip and Palate Association in collaboration with the Centre for Appearance Research CAR at the University of the West of England (UWE). There were 207 eligible responses (95% completed online) received between July and October 2018. Dependent variables included the Body Esteem Scale for Adolescents and Adults, Harter’s Self Perception Profile for Adults (Global Self-Worth, Social Competence, and Intimacy subscales), the Fear of Negative Appearance Evaluation Scale, and the Revised Adult Attachment Scale. Independent variables were the Revised Life Orientation Test, biodemographic data, and self-reported single-item questions.
Results:
Factors associated with positive adjustment included reports of a happy childhood, talking about CL/P with family, close friendships, comfort in public spaces, satisfaction with appearance, and a positive life orientation. Psychological distress was associated with a desire for further surgery to improve appearance and/or function.
Conclusions:
Several factors were identified that may influence psychological adjustment in adults with CL/P. Throughout childhood, family-centered practice to support family cohesion and an open dialogue about CL/P is indicated, as is support for young people to develop social confidence. For adults returning to the cleft service, treatment options for appearance and/or functional concerns should be explored, with access to psychological support when indicated. Interventions to increase optimism, resilience, and self-acceptance may also be warranted throughout the life span.
Introduction
Cleft lip and/or palate (CL/P) is a congenital craniofacial condition requiring multidisciplinary treatment from the point of diagnosis (Berkowitz, 2013). Following the identification of CL/P in their child, parents often experience a range of emotions and may feel daunted by the treatment pathway ahead (Nelson et al., 2012). Depending upon the resources of the family to cope, parental well-being and family functioning may be affected (Crerand et al., 2015). As the child grows older, they may become aware of having a “different” appearance and/or speech, and social experiences and emotional well-being may be impacted (Havstam et al., 2011; Rumsey & Harcourt, 2012). Academic achievement may also be affected, particularly if the diagnosis is associated with an additional condition or syndrome (Wehby et al., 2014).
In recent years, recognition of CL/P as a lifelong condition has been steadily increasing (Stock & Feragen, 2016). This is largely due to recent efforts to examine the impact of CL/P in adulthood. This research has indicated poor self-esteem (Berk et al., 2001; Cheung et al., 2007; Ardouin et al., 2020), appearance-related distress, and a marked impact on social life (Marcusson et al., 2001; Ardouin et al., 2020, 2021) in adults with CL/P. Educational and/or vocational opportunities may also be impacted, as well as the desire to start a family, due to recurrence risk (Ramstad et al., 1995). Although care is now typically delivered by multidisciplinary teams, this has only become the norm over the past 2 decades. As such, the majority of today’s adults would not have benefited from the same standard of care while growing up. Consequently, research has called for information, treatment, and support to be made available into and throughout adulthood (Stock et al., 2015), as well as for ongoing support for families and young people to prevent difficulties persisting into adult life (Ardouin et al., 2020) and to promote overall adjustment.
For the purpose of this study, “adjustment” was conceptualized as the process of the relative adaptation of an individual to the demands of their environmental context (see Seaton, 2009). Five key domains of adjustment were utilized, according to conceptual CL/P framework of Stock et al. (2016, 2020; Table 1): Emotional Wellbeing, Social Functioning, World View, Appearance Satisfaction, Vocational Milestones, and Condition-Specific Factors.
A Conceptual Framework of Psychological Adjustment to Cleft Lip and/or Palate.
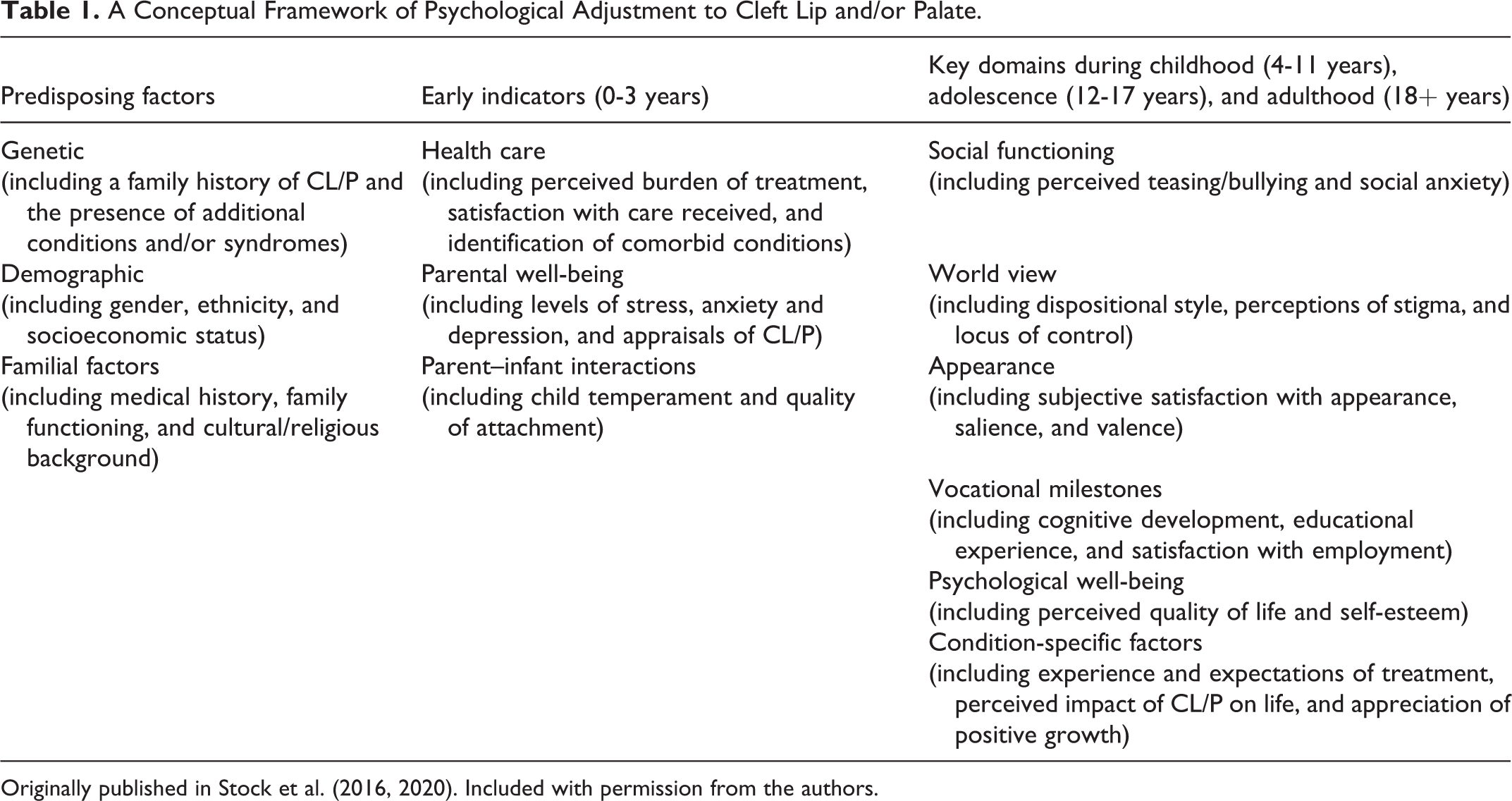
Originally published in Stock et al. (2016, 2020). Included with permission from the authors.
A key part of developing support for those affected by CL/P is an understanding of the factors, which may contribute to adjustment. Although a handful of quantitative studies have explored possible factors associated with psychological adjustment in parents of children born with CL/P (Stock et al., 2020), and in children and adolescents with CL/P (Berger & Dalton, 2011; Feragen et al., 2015; Feragen & Stock, 2016), investigations of contributing factors to adjustment in adulthood have been scarce. However, 3 recent qualitative studies explored adults’ narratives of growing up with CL/P and identified a range of self-reported influential factors, including support from family and friends, satisfaction with treatment outcomes, social experiences with peers and members of the public, satisfaction with appearance, and optimism (Stock et al., 2016; Nicholls et al., 2018; Kappen et al., 2019).
The aim of the present study was to build upon recent qualitative work in this area to quantitatively examine potential factors associated with psychological adjustment in adulthood.
Method
Design
A survey was designed by the Cleft Lip and Palate Association (CLAPA) in collaboration with the Centre for Appearance Research (CAR) at the University of the West of England (UWE). The CLAPA is a dedicated UK-based charity supporting those affected by CL/P. The online survey platform SurveyMonkey was used to collect both quantitative and qualitative data. The survey was also made available in paper format contained within a 54-page booklet. The survey consisted of 220 questions split across 12 sections.
The survey was conducted as part of a larger program of work aimed at improving the support available to adults born with CL/P in the United Kingdom (the CLAPA Adult Services Programme). This broader program of work was launched in recognition of the limited support resources available and varied treatment experiences of UK adults with CL/P. The program involved extensive engagement with the CL/P community via a UK-wide workshop tour, the survey, and the development and evaluation of three community-based interventions: an Adults Conference, a Panel Discussion series broadcast in podcast and video format, and a “Leaver’s Pack” of information for adults who have left/are about to leave routine CL/P care. More information about the CLAPA Adult Services Programme can be found online (CLAPA, 2021). Given the volume of data collected from the survey, findings are reported across a series of papers, including the current paper (Ardouin, Davis et al., 2020; Ardouin, Drake, et al., 2020; Ardouin, Hare, et al., 2020; Ardouin et al., 2021).
Materials
The survey was designed using current literature (eg, Stock & Feragen, 2016) and the varied expertise of the research team. Standardized measures were used wherever possible. Where topics of interest were not covered by standardized measures, single-item questions were developed.
The draft survey was reviewed by the CLAPA Adult Voices Council (AVC), a group of 8 adults born with CL/P. The AVC examined all proposed questions to ensure readability and that the results could be interpreted in a way which would answer the question that the researchers sought to determine. Questions that were unclear were either removed or amended with input from the AVC. The final version was later reviewed again with an additional 6 self-selecting volunteers (all adults living in the United Kingdom who were born with CL/P). These volunteers received no tangible incentive for their participation; however, travel expenses to attend the meeting were reimbursed.
Procedure
Institutional ethical approval was obtained from the faculty ethics committee at UWE. The survey was advertised between July and October 2018 via direct e-newsletters to CLAPA members, interviews in national and local media, posters and leaflets, and CLAPA’s social media between July and October 2018. Prior to survey completion, potential participants were made aware that their contribution to the survey was voluntary, that their data would be kept confidential, that they would not be personally identified during dissemination of the findings, and that they could withdraw their data from the study at any time prior to publication. Participants were asked to indicate their consent for their data to be used for research purposes. According to participant preference, surveys were completed either online (via the platform SurveyMonkey) or in paper format contained within a 54-page booklet. Further information about measures included in this analyses can be found in Table 2.
Measures Included in Analyses.

a Categorical response of 1 (0 friends) to 5 (4 or more friends).
b Categorical response of 1 (strongly disagree) to 5 (strongly agree).
c Categorical response of 1 (poor) to 4 (excellent).
d Categorical response of 1 (very unhappy) to 5 (very happy).
e Further information for standardized measures reported in manuscript.
Dependent Variables
The Appearance Evaluation subscale of the Body Esteem Scale for Adolescents and Adults (BES-AA; Mendelson et al., 2001) was used to evaluate subjective satisfaction with overall appearance. This subscale is made up of 10 items, rated on a 5-point Likert scale (0 = not at all; 4 = always). A higher score indicates higher body esteem. All subscales of the Body Esteem Scale have high internal consistency and reliability and correlate well with the broader concept of self-esteem (Mendelson et al., 2001).
Three subscales of the Harter Self-Perception Profile for Adults (SSP-Ad; Messer & Harter, 1986) were used to evaluate self-perceived Global Self-Worth, Social Competence, and Intimacy. The Norwegian-style scoring of the scale was used, which is considered more straightforward, valid, and reliable than the original scale (Wichstrøm, 1995). Respondents indicated, on a 4-point Likert scale (1 = describes me very poorly; 4 = describes me very well), the degree to which they identify with different statements. All subscales have 6 items. Higher scores indicate a more favorable self-judgment. Good content and criterion validity, and internal and external reliability of this measure have been reported (Wichstrøm, 1995).
The Fear of Negative Appearance Evaluation Scale (FNAES; Lundgren et al., 2004) was used to evaluate participants’ degree of concern that others would evaluate them negatively as a result of their appearance. Respondents indicated, on a 5-point Likert scale (1 = not at all; 5 = extremely), to what extent they identify with 6 statements. A higher score indicates higher levels of fear. The FNAES has been shown to consist of a strong single factor and to have good internal consistency and reliability. The measure correlates well with related measures of body image and psychological well-being, yet also accounts for unique variance (Lundgren et al., 2004).
The Revised Adult Attachment Scale (R-AAS; Collins, 1996) was used to assess participants’ attachment styles in adult relationships. The R-AAS contains 3 subscales, each composed of 6 items. The “Close”’ subscale examines the extent to which an individual feels comfortable with closeness and intimacy. The “Depend” subscale examines the extent to which an individual feels comfortable in depending on others for support. The “Anxiety” subscale examines how much an individual worries about being rejected or unloved. Respondents answered all 18 questions of the 3 subscales using a 5-point Likert scale (1 = not at all characteristic of me; 5 = very characteristic of me). Higher scores on the “Close” dimension characterize individuals who find intimacy with others easy. Higher scores on the “Depend” subscale characterize individuals who feel that others are trustworthy and dependable. Higher scores on the “Anxiety” subscale characterize individuals who worry about being rejected or unloved. The R-AAS has strong validity and reliability and correlates well with related concepts, such as psychological distress, self-esteem, and satisfaction in romantic relationships (Ravitz et al., 2010).
Independent Variables
One standardized measure was utilized in the present study as a potential independent variable (IV) impacting psychological adjustment. The Revised Life Orientation Test (LOT-R; Scheier et al., 1994) is a 10-item measure of optimism and pessimism. Items are rated on a 5-point Likert scale (0 = strongly disagree; 4 = strongly agree). A higher score indicates a more positive life orientation. Results can also be interpreted as follows: 19 to 24 high optimism; 14 to 18 moderate optimism; and 0 to 13 low optimism. The LOT-R has demonstrated a clear factor structure, content validity, and internal and external reliability (Herzberg et al., 2006).
The remaining IVs included biodemographic data (such as cleft type) and self-reported single-item questions (see below).
Analysis
A review, verification, and validation of the database was undertaken prior to analyses. A missing values analysis in the form of the Little’s Missing Completely at Random (MCAR) Test was performed on all variables. The MCAR test showed that data were missing at random, χ2 (53) = 49.234, P = .622, and would not affect conclusions. Skewness and kurtosis were also checked for all dependent variables (DVs). All DVs were found to fall within acceptable range (<3) with the exception of the FNAES (3.487). Finally, univariate outliers were examined (ie, cases that sit at the extreme upper or lower tails of the distribution of a single variable) and there were no unduly large or strongly influential observations in the sample. Taking these findings together, it was concluded that there were no excessively influential observations in the sample and analyses proceeded as planned.
For standardized measures, items were reversed as appropriate, (sub)scale totals were calculated, and descriptive statistics were generated. These results can be found in the other papers from this series (Ardouin, Davis et al., 2020; Ardouin, Drake, et al., 2020; Ardouin, Hare, et al., 2020; Ardouin et al., 2021). Regression modeling was used to identify factors that may influence psychological adjustment in adults with CL/P. In order to determine which variables to include in the model, all IVs were explored through a set of exploratory data analyses (EDA). The EDA involved Pearson correlation (when both the DVs and the IV were continuous), one-way analysis of variance (when the DV was continuous and the IV was categorical with more than 2 categories), or independent samples t test (when the DV was continuous and the IV was categorical with only 2 categories). Based on the outcome of the EDA, IVs were included in the regression models if they met the following criteria; the IV was associated with 2 or more DV; and the inclusion of the variable did not cause multicollinearity problems (ie, all variance inflation factors are less than 4). Finally, Pearson correlation was used to assess the relationship between DVs as well as the IVs included in the regression models. For statistically significant correlations, r values of approximately 0.1 in magnitude are considered to represent a small effect, 0.3 to represent a medium effect, and 0.5 to represent a large effect (Cohen, 1988).
Results
Participants
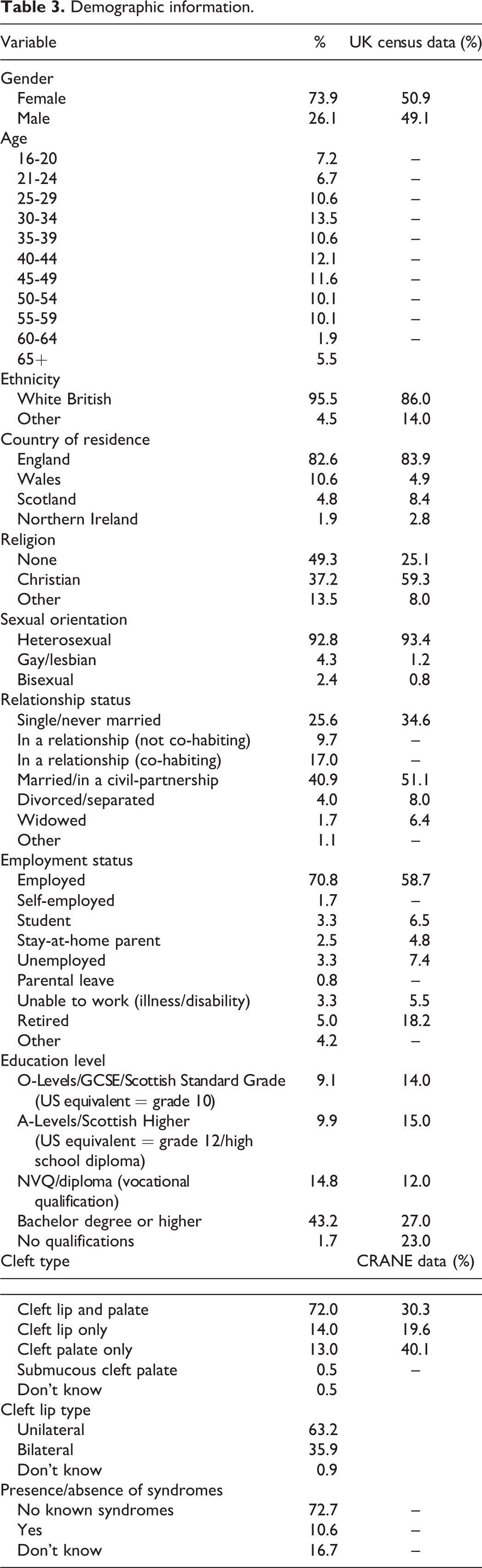
A total of 224 survey responses were received. Seventeen participants were excluded as they had been born outside the United Kingdom (7.6%). Of the remaining 207 eligible responses, 94.7% were completed online. A further 5.3% returned paper versions via post. These were entered into SurveyMonkey by a student intern, and all surveys were checked by the second author. The most commonly reported recruitment method was a CLAPA email campaign (44.4%). Other successful recruitment methods included social media (32.8%), direct contact with CLAPA staff (8.9%), word of mouth (3.9%), a leaflet or poster (3.3%), or the CLAPA website (2.8%). A total of 207 eligible responses were analyzed in the present study. Participant demographics are provided in Table 3 alongside national census data for comparison where available (Cleft Registry and Audit Network, 2018; Office for National Statistics, 2018).
Demographic information.
Regression Models
Following the outcome of the EDA, the following variables were included in the final regression model: life orientation (measured by the LOT-R), as well as the following 1-item questions: happy childhood, ability to rely on family, ability to enjoy time with family, ability to talk about cleft with family, number of close friends, perceived quality of close friendships, satisfaction with speech, satisfaction with appearance, satisfaction with surgical outcomes, satisfaction with psychological support, desire for further surgery for functional reasons, desire for further surgery for appearance reasons, feelings of comfort in public spaces, and perception of being treated with the same dignity and respect as others.
The following variables were analyzed (EDA) but did not meet the criteria for inclusion in the regression models: gender, age, cleft type, unilateral/bilateral, the presence of syndrome, country of residence, religion, sexual orientation, ethnicity, employment status, education level, satisfaction with romantic relationships, satisfaction with general practitioner (GP), satisfaction with dental treatment, satisfaction with speech and language therapy, satisfaction with hearing, perceived discrimination in home/neighborhood, perceived discrimination in workplace/study environment, perceived discrimination in public transport, perceived discrimination by police and justice system, and perceived discrimination by government.
Summaries of the final regression models are shown in Table 4. Only statistically significant variables are included in the presentation of each model below.
Regression Models.
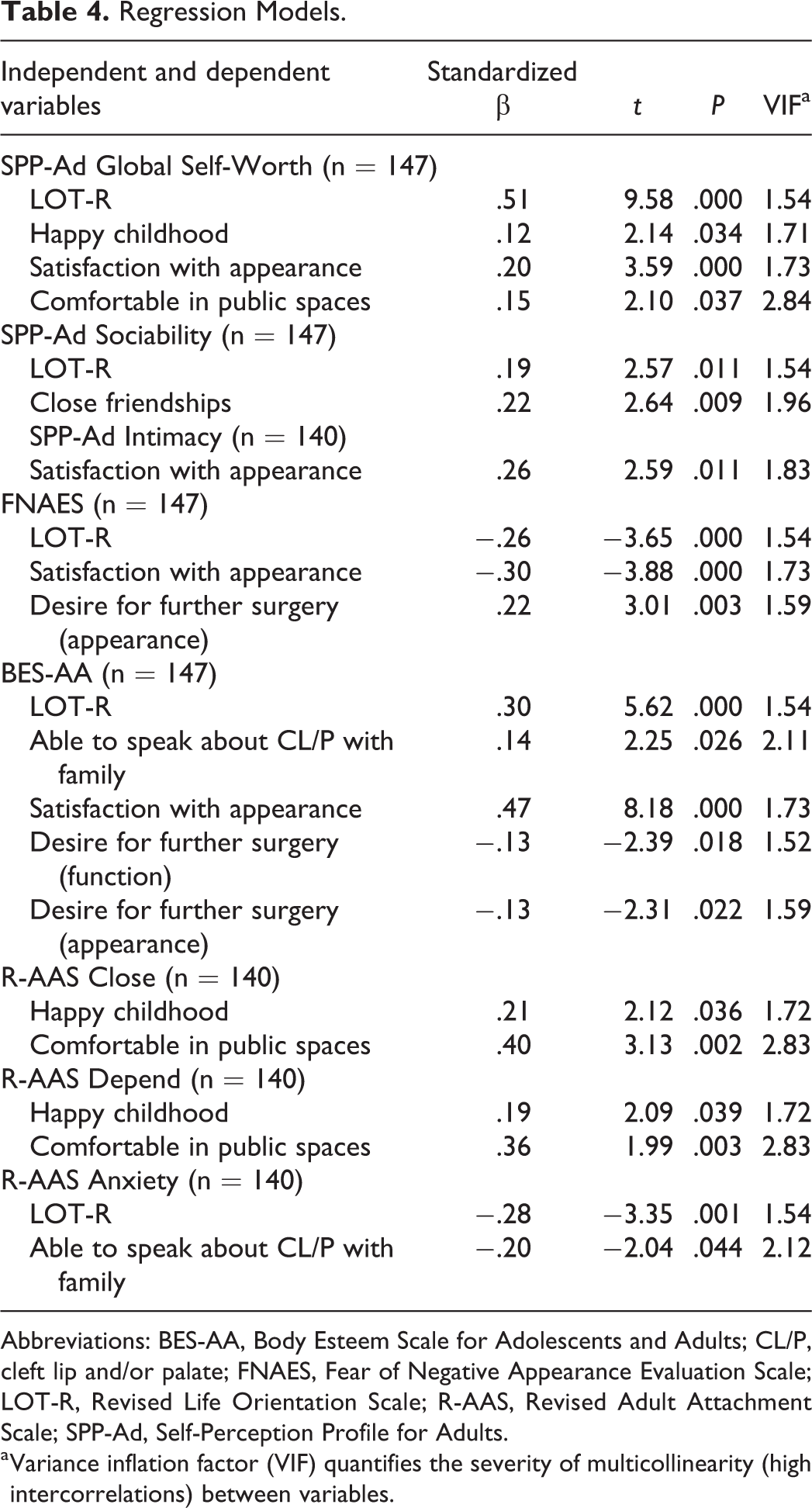
Abbreviations: BES-AA, Body Esteem Scale for Adolescents and Adults; CL/P, cleft lip and/or palate; FNAES, Fear of Negative Appearance Evaluation Scale; LOT-R, Revised Life Orientation Scale; R-AAS, Revised Adult Attachment Scale; SPP-Ad, Self-Perception Profile for Adults.
a Variance inflation factor (VIF) quantifies the severity of multicollinearity (high intercorrelations) between variables.
Self-Perception Profile for Adults Global Self-Worth
The fitted model accounted for 73.2% of the variance and comprised 4 statistically significant variables, adjusted R 2 = 0.732, F(15, 131) = 27.618, P < .001. A positive life orientation, a happy childhood, satisfaction with appearance, and comfort in public spaces were positively associated with higher self-perceived global self-worth.
Self-Perception Profile for Adults Sociability
The fitted model accounted for 47.4% of the variance and comprised 2 statistically significant variables, adjusted R 2 = 0.474, F(15, 131) = 9.768, P < .001. A positive life orientation and close friendships were positively associated with higher self-perceived social competence.
Self-Perception Profile for Adults Intimacy
The fitted model accounted for 25.6% of the variance and comprised 1 statistically significant variable, adjusted R 2 = 0.256, F(15, 124) = 4.190, P < .001. A greater satisfaction with appearance was positively associated with higher self-perceived competence in intimate relationships.
Fear of Negative Appearance Evaluation Scale
The fitted model accounted for 50.6% of the variance and comprised 3 statistically significant variables, adjusted R 2 = 0.506, F(15, 131) = 10.964, P < .001. A positive life orientation and satisfaction with appearance were negatively associated with fear of negative appearance evaluation, while a greater desire to seek further surgery to improve appearance was positively associated with fear of negative evaluation.
Body Esteem Scale for Adolescents and Adults
The fitted model accounted for 72.3% of the variance and comprised 5 statistically significant variables, adjusted R 2 = 0.723, F(15, 131) = 26.425, P < .001. A positive life orientation, the ability to speak about CL/P with family, and satisfaction with appearance were positively associated with body esteem, while the desire for further surgery to improve appearance and/or function was negatively associated with body esteem.
Revised Adult Attachment Scale Close
The fitted model accounted for 21.2% of the variance and comprised 2 statistically significant variables, (adjusted R 2 = 0.212, F(15, 124) = 3.495, P < .001. A happy childhood and comfort in public spaces were positively associated with closeness and intimacy in adult relationships.
Revised Adult Attachment Scale Depend
The fitted model accounted for 29.8% of the variance and comprised 2 statistically significant variables, adjusted R 2 = 0.298, F(15, 124) = 4.942, P < .001. A happy childhood and comfort in public spaces were positively associated with an ability to depend on others for support.
Revised Adult Attachment Scale Anxiety
The fitted model accounted for 39.1% of the variance and comprised 2 statistically significant variables, adjusted R 2 = 0.391, F(15, 124) = 6.943, P < .001. A positive life orientation and the ability to speak about CL/P with family were negatively associated with worries about being rejected or unloved.
Associations Between Variables
Pearson correlation analyses found that most variables were correlated to varying degrees, displaying small to large coefficient (r) values (r = 0.11-0.85; see Table 5).
Pearson Correlations Between Study Variables.
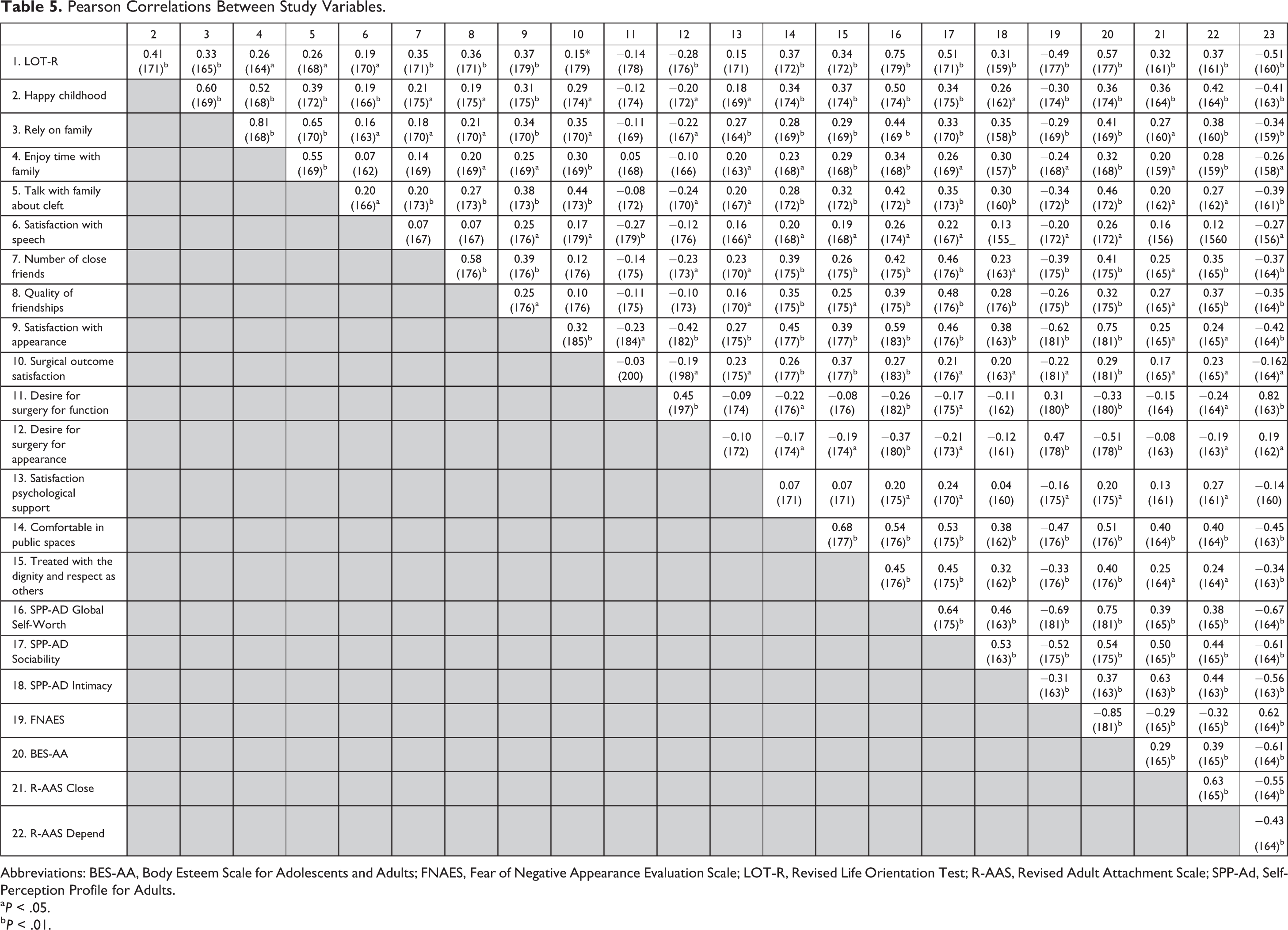
Abbreviations: BES-AA, Body Esteem Scale for Adolescents and Adults; FNAES, Fear of Negative Appearance Evaluation Scale; LOT-R, Revised Life Orientation Test; R-AAS, Revised Adult Attachment Scale; SPP-Ad, Self-Perception Profile for Adults.
a P < .05.
b P < .01.
Discussion
This study quantitatively explored IVs related to psychological adjustment in adults born with CL/P. The findings provide insight into a range of risk and protective factors that may influence long-term outcomes and are indicative of suggestions for practice, which may help to prevent the development of psychological distress in adulthood.
Associations Between Variables and Psychological Domains
Anxiety in adult relationships was strongly associated with almost all DVs, including low self-worth, low self-perceived competence in social and romantic relationships, increased fear of negative appearance evaluation, and poorer body esteem. The RAAS-Anxiety subscale examines the degree to which adults are concerned about being rejected or unloved. This seems to be a particularly important variable for future research to investigate and a potential target for psychological intervention.
For the purpose of interpreting results, DVs were categorized into 3 core domains of adjustment, based on the conceptual framework by Stock and colleagues (Stock et al., 2016, 2020): psychological well-being (Global Self-Worth), social (Sociability, Intimacy, RAAS), and appearance-related (BES-AA, FNAES).
Findings suggest a strong association between psychological well-being and appearance (Global Self-Worth, FNAES, and BES-AA) and between psychological well-being and social adjustment (Global Self-Worth, Sociability, and RAAS-Anxiety). Using this approach, there is also a strong association between appearance and social adjustment (FNAES, BES-AA, and RAAS-Anxiety). Taken together, this corroborates existing evidence that intervening in one domain may also indirectly improve adjustment in other domains (Clarke et al., 2013; Feragen et al., 2015). Further work is needed to confirm these associations and to assess the utility of this approach for psychological intervention.
Optimism
Broadly, the protective role of optimism in times of adversity has been well documented (Seligman, 2018) and has been associated with the use of productive coping strategies, positive social experiences, and an overall increase in well-being (Carver et al., 2010). Although under-researched in the craniofacial field, studies have begun to highlight dispositional style as a potentially influential factor for psychological adjustment in individuals and families affected by CL/P (Baker et al., 2009; Sischo et al., 2016; Stock, Costa et al., 2020). In the current study, a positive life orientation was found to be associated with reduced fear of negative appearance evaluation and decreased feelings of worry about being rejected or unloved in adult relationships. In addition, a higher degree of optimism was associated with higher global self-worth, greater self-perceived social competence, and higher body-esteem. In light of the view that optimism is a skill that can be learned (Seligman, 2018), the current study lends further support to the need for examination of interventions aimed at increasing optimism within the context of CL/P.
Family Cohesion
A wealth of CL/P research has demonstrated the potential impact of CL/P on parents and the wider family, both in the period following diagnosis and in the longer term (eg, Nelson et al., 2012; Stock et al., 2020). In the general population, models of intervention to improve child outcomes in times of adversity focus on the entire family unit, with the assumption that families who have the necessary supports and resources will raise healthy, competent, and well-adjusted children (Dunst & Trivett, 2009). The findings of the current study would seem to support this approach, whereby a self-reported happy childhood was associated with higher global self-worth, greater comfort with closeness and intimacy in adult relationships, and greater comfort with depending on others for support. Further, the ability to speak about CL/P with family was positively associated with greater body-esteem and found to be protective against feelings of worry about being rejected or unloved. Qualitative CL/P studies have also indicated that the ongoing opportunity to reflect openly about the condition, its impacts, and its treatment has a positive influence on self-acceptance and self-esteem in adulthood (Stock et al., 2016; Nicholls et al., 2018; Kappen et al., 2019). Such findings highlight the importance of providing psychological support for parents from the point of diagnosis onward to ensure individual parental well-being as well as stable and supportive familial relationships. As the child grows older, families may benefit from guidance regarding how to discuss challenging aspects of the condition, such as dealing with being “different” and treatment decision-making.
Social Experiences
Previous literature in both the craniofacial field and the wider field of “visible difference” (facial disfigurement) has demonstrated the potential impact of an altered appearance on individuals’ social experiences. Specifically, individuals may experience unwanted staring, questions, and comments from peers and/or members of the public, in addition to teasing, bullying, and social rejection (Rumsey & Harcourt, 2012). Such experiences, if interpreted as negative by the individual and if not appropriately addressed, can result in long-term psychological distress (Feragen & Stock, 2016). However, some studies have suggested that close friendships may moderate the harmful impact of negative social experiences, acting as a buffer to any distress (Feragen & Borge, 2010). The present study supports these findings, identifying a positive association between greater comfort in public spaces and higher global self-worth, greater comfort with closeness and intimacy in adult relationships, and greater comfort with depending on others for support. Correspondingly, the quality of close friendships was found to be predictive of self-perceived social competence. Such findings demonstrate the importance of positive social experiences for long-term psychological health and provide further evidence of the need for psychological intervention to target social confidence and social skills at key developmental points.
Satisfaction With Appearance
Subjective satisfaction with appearance, as measured by the single-item question “How happy are you with the whole of your appearance? (1 = very unhappy, 5 = very happy), was associated with increased body esteem and reduced fear of negative appearance evaluation. As could be expected, this finding is in line with previous literature suggesting that those who are less satisfied with their appearance are more likely to report social anxiety and avoidant behaviors (Versnel et al., 2012; Ardouin et al., 2020). Satisfaction with appearance was also associated with self-perceived competency in intimate relationships and higher levels of global self-worth. Broader literature has suggested that appearance could be regarded as central to attraction, and therefore any perceived differences could form a barrier to the initiation of social and romantic relationships (Sharratt et al., 2018). Consequently, fears of being negative judged or rejected may develop, and self-esteem may become affected (Sharratt et al., 2018). Conversely, positive experiences of friendships and romantic relationships may act as a buffer for appearance dissatisfaction (Feragen & Stock, 2016), once again highlighting the importance of positive social experiences and the need for psychological intervention to target these areas.
Desire for Further Surgery
It has been estimated that around 45% of adults with CL/P express a desire for further treatment (Marcusson et al., 2001; Sinko et al., 2005; Kappen et al., 2019). This desire has been linked to poorer psychological well-being, including appearance dissatisfaction, symptoms of anxiety and depression, and a higher degree of perceived stigmatization (Marcusson et al., 2001; Sinko et al., 2005; Chuo et al., 2008; Bemmels et al., 2013). The present study lends support to these findings, demonstrating an association between a desire for appearance-altering surgery and a greater degree of fear of negative appearance evaluation. Further, a desire for additional treatment, whether for appearance or functional reasons, was related to poorer body esteem.
Prior research has identified improvements in psychological well-being following surgical intervention (Hens et al., 2011; Byrne et al., 2014), suggesting that further treatment may be of benefit to some, especially given that treatment outcomes have improved since today’s adults were originally treated (Al-Ghatam et al., 2015; Smallridge et al., 2015). A recent related UK study found that 41% of surveyed adults were unaware of their entitlement to treatment as an adult, while others had struggled to access specialist care (Ardouin et al., 2020). This suggests that further work is needed to raise awareness among the CL/P population and nonspecialist health professionals (such as GPs) regarding the availability of UK-based CL/P treatment in later life. Nonetheless, adults’ motivations for further treatment, expected outcomes, and the anticipated burden of recovery should be discussed to ensure adults’ expectations of surgical outcomes are realistic and treatment decisions are supported (Stock, Marik et al., 2020). Wherever possible, psychologists should be integral to exploring and developing treatment options as part of routine cleft care.
Methodological Considerations
This study presents findings from a relatively large UK-wide survey of adults born with CL/P. Nonetheless, it cannot be assumed that this group, nor the self-selecting subgroup who responded to the survey, are representative of the adult CL/P population. In particular, adults with cleft palate only were under-represented in this study, as were men, and adults from minority groups. Further, the sample were highly educated as a whole, which may reflect the survey being less accessible to those with a lower level of education and/or an additional condition or syndrome. As such, further research is needed in order to engage and represent the experiences of more diverse populations of adults of CL/P. The authors chose to exclude non–UK-born adults from the analyses, given that health care systems vary considerably between countries. In future, international samples and comparison studies are needed to better understand cultural differences and variations in health care delivery. Further, participants in the current study were self-selecting, and questionnaires were not always completed in full, which may further raise issues of generalizability. Although demographic variables such as cleft type, age, and gender were explored at the EDA stage, they did not meet the criteria to be entered into the regression modeling, likely in part due to the limited sample size. These variables are known to have relevance in relation to adjustment to CL/P (Stock & Feragen, 2016). Previous studies have commented on the challenges of analyzing subsets of data even when the overall sample is relatively large (Feragen et al., 2015). Multicenter, interdisciplinary, and international work is, therefore, strongly encouraged to gain a more representative picture of the population and to move toward a better understanding of holistic outcomes in CL/P. Finally, although standardized measures were used where possible, most of the IVs were derived from single-item questions. The methodology of the study was also limited due to being cross sectional in nature. This limits the inferences that can be drawn from the results, including the direction of relationships. However, only items that were statistically robust were included in the final regression analyses. These analyses indicated a number of variables that are not typically investigated within the context of adjustment to CL/P, or currently addressed by known measures circulating in the field. The identification of these variables is supported by previous qualitative work and warrants further investigation in future.
Despite the acknowledged limitations, this comprehensive survey provides insight into a group, which has to date received relatively little attention in the context of CL/P. The findings will be used to inform future research in this area and are pertinent to the ways in which psychological support for adults with CL/P is delivered in clinical practice and in the community.
Conclusions
This study examined potential factors associated with psychological adjustment in the adult CL/P population. Throughout childhood, family-centered practice to support family cohesion and facilitate an open dialogue about CL/P is indicated, as is support for young people to develop social confidence. For adults returning to the cleft service, treatment options for appearance and/or functional concerns should be explored, with the involvement of a clinical psychologist where possible. Finally, interventions to increase optimism, resilience, and self-acceptance may also be warranted throughout the life span.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The CLAPA Adult Services Programme was funded by the VTCT Foundation (registered charity: 1155360).
