Abstract
Preoperative anxiety and pain can adversely affect recovery and satisfaction. Music is a safe, low-cost, non-pharmacological intervention that may enhance perioperative outcomes. This study evaluated the effects of patient-preferred music on anxiety, recovery, pain, satisfaction, and hemodynamics during unilateral knee arthroplasty under spinal anesthesia. In this prospective, randomized, controlled, single-blind trial, 80 patients were assigned to either a music group (Group M) or a control group (Group C). Group M listened to preferred music via headphones before and during surgery, while Group C received standard care. Anxiety (State-Trait Anxiety Inventory; state: STAI-S, trait: STAI-T), recovery (Quality of Recovery-15 [QoR-15]), pain (Numeric Rating Scale [NRS]), satisfaction, and hemodynamic parameters were measured. Minimal clinically important difference (MCID) analyses were used to assess clinical significance. Sixty-five patients (Group M: 32; Group C: 33) were analyzed. Postoperative STAI-S scores were significantly lower in Group M (p = .001), with a 6.18-point difference exceeding the MCID by 283%. QoR-15 scores were higher in Group M (p = .007), surpassing the MCID by 123%. Group M also showed lower systolic blood pressure at several perioperative points (p < .05), lower NRS pain scores at the 12th postoperative hour (p = .001), and reduced need for rescue analgesia (p = .035). Satisfaction was significantly greater in Group M (p = .001). No significant differences were found in heart rate (p > .05). Patient-preferred music significantly improved anxiety, pain, recovery quality, hemodynamic stability, and satisfaction. MCID analysis confirmed clinical relevance. Music may serve as an effective and feasible adjunct in perioperative care.
Keywords
Introduction
Total knee arthroplasty is among the most frequently performed surgical interventions today, aimed at enhancing patients’ quality of life by alleviating pain and functional limitations (White et al., 2025). Spinal anesthesia is commonly favored in such procedures because of its superior pain control, more rapid postoperative recovery, hemodynamic stability, and lower risk profile compared with general anesthesia (Calkins et al., 2024). Despite its advantages, spinal anesthesia presents several challenges for both anesthesiologists and patients. One of the most significant concerns is that patients remain awake and are exposed to visual and auditory stimuli in the operating room, which may induce anxiety. In particular, the orthopedic instruments used during knee arthroplasty generate noise levels high enough to potentially cause hearing impairment (Belyad et al., 2024).
Perioperative anxiety may activate the sympathetic nervous system, leading to adverse hemodynamic responses such as elevated blood pressure and heart rate. It is also associated with increased postoperative pain, higher incidence of sleep disturbances, delayed wound healing, elevated risk of infection, prolonged postoperative recovery, and delayed hospital discharge (Deng et al., 2023; Raghavan et al., 2019). Pharmacological agents such as benzodiazepines and opioids are commonly employed to alleviate perioperative anxiety. However, their use is associated with adverse effects, including drowsiness, respiratory depression, nausea, vomiting, and potential interactions with anesthetic agents, necessitating close monitoring (Brooke et al., 2024; Kowark et al., 2024). Moreover, the administration of high-dose sedative agents has been linked to an increased risk of postoperative delirium and cognitive dysfunction (Erel et al., 2024). Consequently, interest has grown in the use of non-pharmacological interventions as anxiolytic alternatives.
Music is one of the most widely utilized non-pharmacological interventions because of its safety, low cost, and non-invasive nature. Music therapy is considered a safe and effective method for reducing anxiety, primarily through its modulation of the limbic system and its ability to elicit pleasurable emotional responses (Sharkiya, 2024). Music facilitates emotional and physical comfort by alleviating feelings of alienation, enabling patients to shift their focus away from current concerns and thereby reducing anxiety. The use of headphones to deliver music further enhances this effect by masking external noise in both the surgical waiting area and the operating room.
In our previous study involving various surgical procedures, listening to a preferred music track prior to the induction of general anesthesia reduced postoperative anxiety and enhanced recovery quality (Akelma et al., 2024). Clinically, it also demonstrated improvements in hemodynamic parameters and patient satisfaction. However, the need for a more objective assessment in terms of clinical significance was identified. Based on these findings, we hypothesized that listening to preferred music during the pre-intraoperative period would improve the quality of recovery—measured by the minimal clinically important difference (MCID)—in patients undergoing elective orthopedic surgery under spinal anesthesia. The primary objective of the present study was to assess the effect of listening to favorite music on perioperative anxiety in patients undergoing knee arthroplasty under spinal anesthesia. Secondary outcomes include recovery quality as assessed by the Quality of Recovery-15 (QoR-15) questionnaire, postoperative pain, patient satisfaction, hemodynamic parameters, and the attainment of MCID thresholds.
Materials and Methods
Trial Design
This prospective, randomized, controlled, single-blind study was conducted in the orthopedic operating room of Ankara Bilkent City Hospital between January 9 and March 3, 2025.
Ethical Principles
The study was approved by the Ankara Bilkent City Hospital Ethics Committee (approval no: E2-23-4704, 27/09/2023) and registered at ClinicalTrials.gov (identifier: NCT06764407). Institutional permission was obtained from Ankara Bilkent City Hospital as part of the ethics committee submission prior to patient recruitment. Written and verbal consent was obtained from the individuals involved in the study.
Patient Selection and Randomization
Patients aged between 18 and 70 years, classified as American Society of Anesthesiologists (ASA) physical status I–II, literate, fluent in Turkish, and scheduled to undergo unilateral total knee arthroplasty under spinal anesthesia were considered eligible for inclusion in the study. Patients were excluded if they had severe hearing or visual impairment, a history of narcotic drug use or alcohol dependence, dementia, regular use of antidepressants, no preferred music selection, any contraindication to spinal anesthesia, or were scheduled for revision knee arthroplasty. Written and verbal informed consent was obtained from all participants in accordance with the Declaration of Helsinki.
We performed a priori sample size calculation, based on pilot data obtained from postoperative State-Trait Anxiety Inventory–State (STAI-S) scores, using G*Power version 3.1.9.2 (Franz Faul, Universität Kiel, Germany). A preliminary pilot study indicated that 31 patients per group were required to achieve 80% power with 5% types I error rate, based on the STAI-S score. Accounting for a potential dropout rate of 25%, the final required sample size was calculated as 80 patients.
Out of 145 eligible patients, 47 were excluded for not meeting the inclusion criteria, 11 declined to participate, and 7 were excluded due to inadequate communication. Consequently, a total of 80 patients were enrolled and randomized into the music group (Group M) and the control group (Group C). After randomization, 15 patients were excluded from the final analysis because of the need for sedation (n = 3), inadequate spinal anesthesia (n = 5), failure to complete the postoperative questionnaire (n = 4), or loss to follow-up during the postoperative period (n = 3). Thus, 65 patients were included in the final analysis (Group M, n = 32; Group C, n = 33). (Figure 1 shows the Consolidated Standards of Reporting Trials (CONSORT) flow chart).
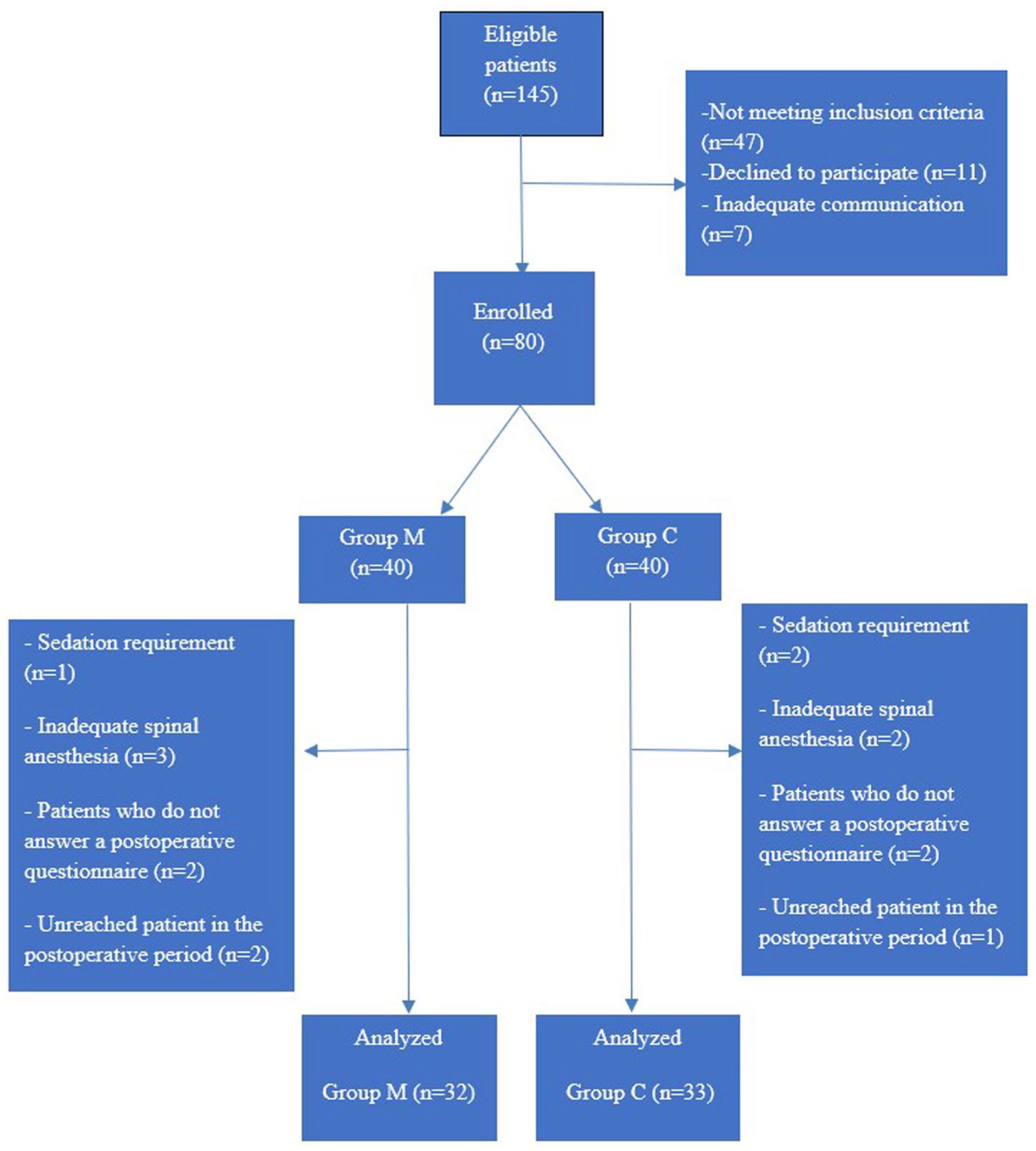
CONSORT flow diagram.
Music Intervention
Patients in the music group were provided with a personalized playlist comprising songs they enjoyed, regardless of artist or genre, with a total duration of 1 hr. If the duration of surgery exceeded this period, the playlist was repeated. All patients were equipped with headphones (MDR-ZX110/B, Sony, Brazil) designed to block ambient noise that could contribute to anxiety or distract from the intervention. The volume was adjusted by the investigator based on patient preference, but was limited to a maximum of 60 dB (Azi et al., 2021). Patients were informed that they could remove the headphones at any time; however, doing so would result in exclusion from the study.
Preoperative Period
Demographic data, including age, sex, height, weight, history of previous elective and/or emergency surgery, educational level, and marital status, were recorded during the preoperative evaluation period. The preoperative STAI (state anxiety [STAI-S] and trait anxiety [STAI-T]), in which patients self-reported their current (state) and general (trait) levels of anxiety, and the QoR-15 questionnaire, which assesses postoperative recovery quality, were administered. In both groups, intravenous midazolam was administered at a dose of 0.02 mg/kg in the preoperative unit. Patients in the music group were provided with over-ear headphones for 15 min to enhance isolation from environmental stimuli. During the same period, patients in the control group were not permitted to listen to music. In both Group M and Group C, heart rate (HR) and systolic and diastolic blood pressure (SBP and DBP, respectively) were measured upon entry into the preoperative waiting room and again 15 min later. In Group M, this 15-min period involved listening to music through over-ear headphones, whereas patients in Group C did not receive any auditory intervention. After these measurements, all patients were transferred to the operating room.
Intraoperative Period
HR, SBP, DBP, mean arterial pressure, and peripheral oxygen saturation (SpO₂) were monitored and recorded in the operating room using non-invasive methods. Following the recording of baseline monitoring data, all patients received spinal anesthesia with 2.2 ± 0.2 mL of 0.5% hyperbaric bupivacaine. The level of sensory block was assessed, and cases of inadequate spinal anesthesia were converted to general anesthesia and excluded from the study. As patient communication was necessary during the administration of spinal anesthesia, music playback was temporarily discontinued. Following confirmation of an adequate block level, headphones were reapplied to patients in Group M, and their personalized playlists were resumed. Patients in Group C did not wear headphones or listen to music at any stage.
All patients received oxygen via a Venturi face mask adjusted to deliver a 40% fraction of inspired oxygen (FiO₂). Pulse rate, blood pressure, respiratory rate, and oxygen saturation were recorded intraoperatively at regular intervals. Any side effects or adverse events were documented. Headphones were removed at the end of the surgical procedure.
Postoperative Period
All patients received an adductor canal block with 20 mL of 0.25% bupivacaine under ultrasound guidance in the post-anesthesia care unit, once the spinal anesthesia had regressed to the T12 sensory level. All patients received a standardized postoperative multimodal analgesic regimen consisting of acetaminophen 650 mg every 6 hr. In cases where the Numeric Rating Scale (NRS) pain score was 4 or higher, 50 mg of intravenous tramadol was administered.
Outcome Measures
The primary outcome was anxiety assessed using the STAI. All patients completed STAI-S and STAI-T in their hospital rooms 1 hr preoperatively, and STAI-S was repeated 4 to 6 hr postoperatively. The STAI, developed by Spielberger et al. (1983) and adapted into Turkish by Oner and Le Compte (1985), is a self-report instrument consisting of 40 items rated on a 4-point Likert scale (Oner & Le Compte, 1985; Spielberger et al., 1983). It comprises 2 subscales: 20 items assess STAI-S, and 20 items assess STAI-T. Total scores range from 20 to 80, with higher scores indicating greater anxiety. Internal consistency has been reported as Cronbach’s α = .94 (state) and .91 (trait) for the Turkish version (Evren et al., 2011). Cronbach’s alpha could not be calculated in the present study because item-level responses were not retained; only total scores were recorded.
Postoperative recovery quality was assessed using the QoR-15, a patient-reported outcome measure derived from the original QoR-40 (Myles et al., 1999). The QoR-15 consists of 15 items covering 5 domains: physical comfort, physical independence, emotional state, psychological support, and pain. Total scores range from 0 to 150, with higher scores reflecting better recovery quality (Stark et al., 2013). The QoR-15 has been validated in Turkiye. Internal consistency has been reported as Cronbach’s α = .75 for the Turkish QoR-15 (Aslanlar et al., 2024). Cronbach’s alpha could not be calculated in the present study because item-level responses were not retained; only total scores were recorded.
Hemodynamic variables were evaluated in the music group before and after the music intervention, and in the control group before entering and after leaving the preoperative waiting room.
Postoperative pain was assessed using the NRS (0 = no pain, 10 = worst pain imaginable) at 1, 4, 12, and 24 hr postoperatively. Patient satisfaction was evaluated using a single-item Likert-type scale (1–10), in which patients rated their overall satisfaction with the perioperative experience.
All assessments were administered by a researcher who was blinded to group allocation. All potential side effects—including nausea, vomiting, dizziness, headache, hypotension, bradycardia, desaturation, and apnea—as well as the need for additional sedative administration, were recorded.
Statistical Analysis
All statistical analyses were performed using SPSS software (version 25.0, IBM Corp., Armonk, NY, USA). Continuous variables were expressed as mean ± standard deviation (SD) or median (interquartile range, IQR), depending on the distribution of the data. Categorical variables were presented as frequencies and percentages. Normality was assessed using the Shapiro–Wilk tests.
Between-group comparisons of continuous variables were conducted using the independent samples t-test for normally distributed data and the Mann–Whitney U test for non-normally distributed data. Paired samples t-test or Wilcoxon signed-rank test was used to analyze within-group differences. Categorical variables were compared using chi-square or Fisher’s exact tests, as appropriate. The primary outcome was the postoperative STAI-S score. The MCID was calculated for STAI-S change and QoR-15 scores to evaluate the clinical relevance of statistically significant results. The percentage by which the observed between-group difference exceeded the MCID was also computed to aid interpretation. A p-value of <.05 was considered statistically significant.
Results
The groups were comparable in terms of demographic and clinical characteristics, including age, sex, body mass index, educational status, ASA classification, marital status, comorbidities, and anesthetic history. In addition, the prevalence of previous surgical history was similar between the groups (p > .05) (Table 1).
Demographic and Clinical Characteristics of the Study Population.
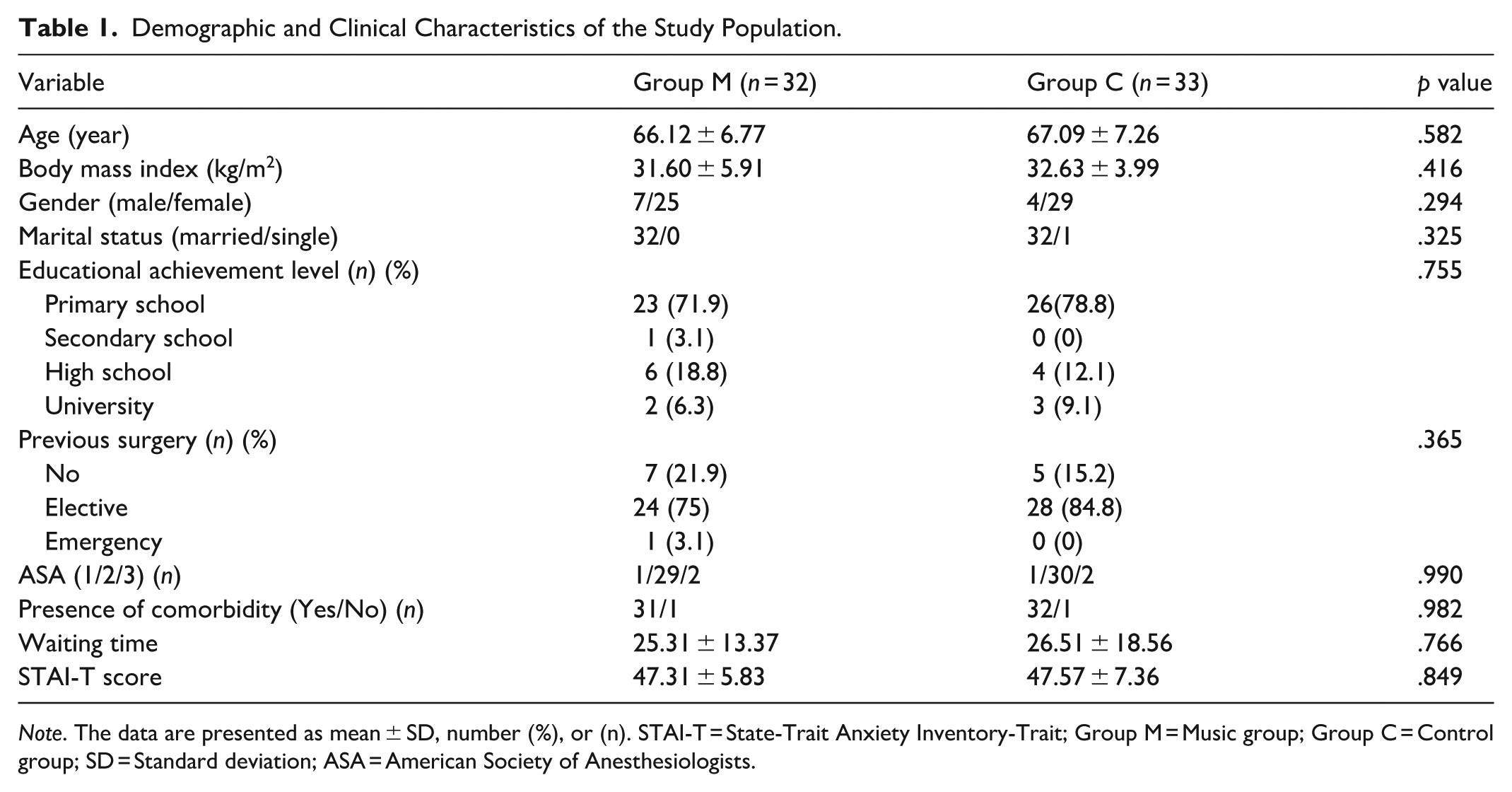
Note. The data are presented as mean ± SD, number (%), or (n). STAI-T = State-Trait Anxiety Inventory-Trait; Group M = Music group; Group C = Control group; SD = Standard deviation; ASA = American Society of Anesthesiologists.
The mean preoperative STAI-S and baseline STAI-T scores were similar for both groups (p > .05) (Tables 2 and 1, respectively). There was no significant between-group difference in baseline STAI-T scores (p > .05) (Table 1). In our study, the mean postoperative STAI-S score was 36.09 ± 4.36 in Group M and 42.27 ± 6.21 in Group C. The between-group difference of 6.18 points was statistically significant (p = .001) (Table 2). The MCID was calculated as 2.18. The observed difference between the two groups exceeded the MCID by 283.49%, indicating a clinically meaningful improvement in anxiety levels. In addition, analysis of the change in STAI-S scores revealed a mean reduction of 10.43 ± 6.74 points in Group M and 6.51 ± 8.76 points in Group C. The between-group difference of 3.92 points was statistically significant (p = .038). The MCID for change in STAI-S scores was calculated to be 3.37. The observed between-group difference exceeded this threshold by 116.32%, indicating a clinically meaningful change.
Comparison of Preoperative and Postoperative QoR-15, STAI-S, and Pain Scores.
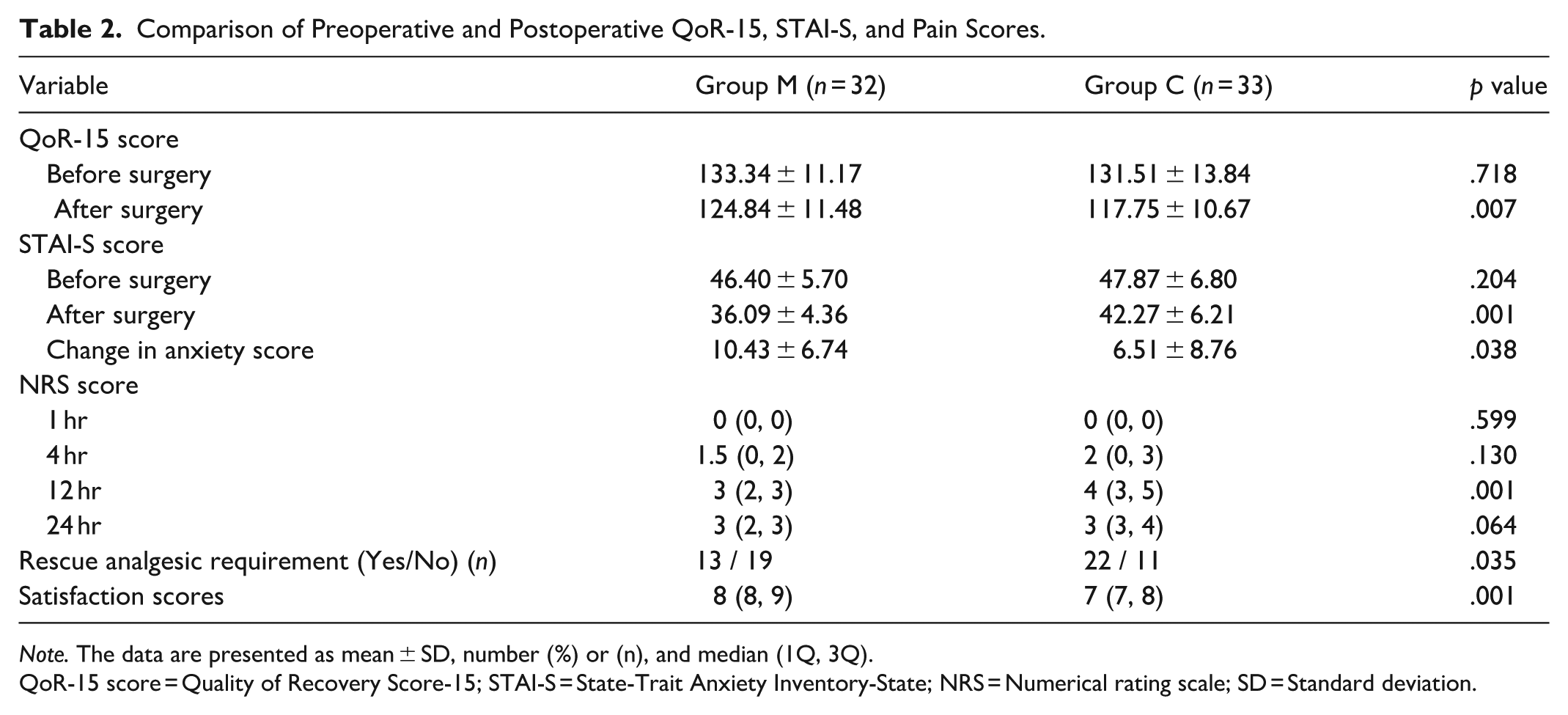
Note. The data are presented as mean ± SD, number (%) or (n), and median (1Q, 3Q).
QoR-15 score = Quality of Recovery Score-15; STAI-S = State-Trait Anxiety Inventory-State; NRS = Numerical rating scale; SD = Standard deviation.
The mean preoperative QoR-15 scores were comparable between Group M and Group C, with no statistically significant difference observed (p > .05) (Table 2). The postoperative QoR-15 score was significantly higher in Group M compared to Group C (Group M: 124.84 ± 11.48; Group C: 117.75 ± 10.67; p = .007) (Table 2). The MCID was determined as 5.74, and the observed between-group difference of 7.09 exceeded this threshold, indicating a clinically meaningful improvement. This corresponds to a 123.52% increase over the MCID, suggesting that the intervention in Group M achieved a clinically significant effect relative to Group C.
No significant differences were observed in NRS scores at 1, 4, and 24 hr between the groups. However, at the 12th postoperative hour, the NRS score was significantly higher in Group C than in Group M (p = .001), with median values of 4 (3–5) and 3 (2–3), respectively (Table 2). Satisfaction scores were significantly higher in Group M [median (IQR): 8 (8–9)] compared to Group C [7 (7–8)] (p = .001) (Table 2). In addition, the number of patients requiring rescue analgesia was significantly lower in Group M (n = 13) than in Group C (n = 22) (p = .035) (Table 2).
SBP values were significantly lower in Group M compared to Group C at several perioperative time points. Statistically significant differences were observed at 0 min (p = .015), 5 min (p = .010), 10 min (p = .012), 30 min (p = .044), 60 min (p = .018), and in the postoperative measurement (p = .028) (Figure 2). Similarly, DBP was significantly lower in Group M at 5 min (p = .016), 30 min (p = .044), 60 min (p < .001), and in the postoperative period (p = .004) (Figure 2). By contrast, no statistically significant differences in HR were observed between the groups at any measured time point.
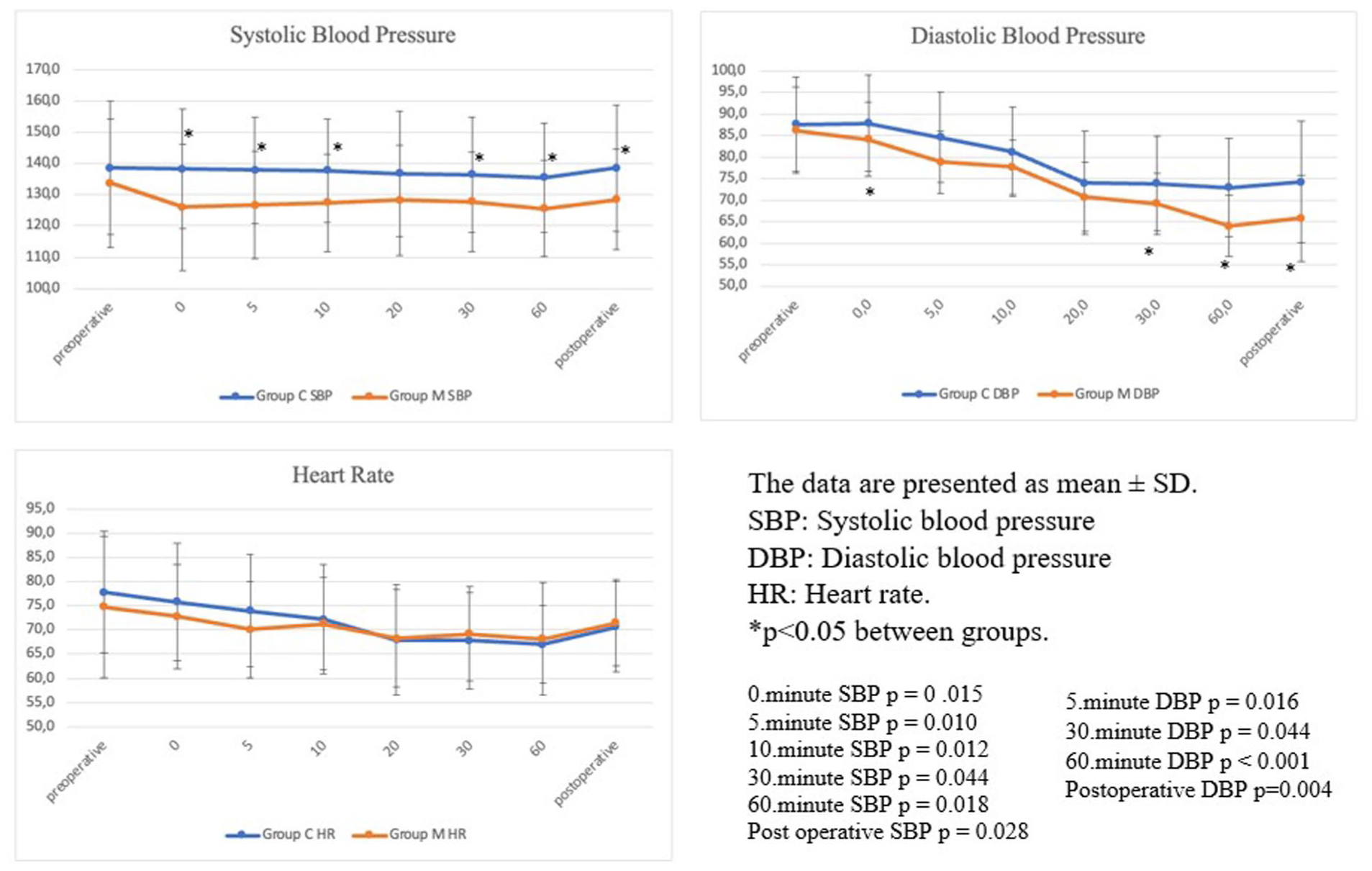
Hemodynamic changes between groups.
Discussion
In this study investigating the impact of listening to favorite music in patients undergoing unilateral knee arthroplasty under spinal anesthesia, we evaluated anxiety as the primary outcome, and quality of postoperative recovery, pain intensity, patient satisfaction, and hemodynamic parameters as secondary outcomes.
Anxiety is a physiological response characterized by feelings of fear, worry, restlessness, and nervousness, typically triggered by uncertainty or perceived threat (Egbert et al., 1963). Preoperative anxiety is highly prevalent, affecting approximately 25% to 80% of surgical patients (J. Wang et al., 2024). It has been associated with increased postoperative morbidity, including higher pain levels, greater analgesic requirements, delayed recovery, and prolonged hospital stays (Stamenkovic et al., 2018). These potential consequences underscore the importance of effective perioperative anxiety management strategies. Kakde et al. (2023) evaluated the effect of perioperative music listening on anxiety in patients undergoing elective cesarean section, while Kaur et al. (2022) investigated its impact in patients undergoing lower extremity surgery. Zhang et al. (2023) investigated the effect of music intervention on sedation in elderly patients undergoing transurethral prostate resection under spinal anesthesia and found that music was effective in inducing mild sedation. Various studies have implemented music interventions at different time points during surgical procedures; however, few have evaluated the clinical significance of their findings. In our study, patients in the music group had lower postoperative state anxiety scores than those in the control group, and the reduction in anxiety was more pronounced with patient-preferred music. Moreover, the between-group difference exceeded the MCID for state anxiety by a substantial margin, supporting that the observed effect was not only statistically detectable but also clinically meaningful.
The observed reduction in postoperative anxiety with patient-preferred music may be explained by several complementary mechanisms. First, music can act as a non-pharmacological distractor that shifts attention away from the operating room environment and postoperative discomfort. Second, allowing patients to listen to their preferred music may enhance perceived control and comfort, which are key determinants of perioperative anxiety. (Kühlmann et al., 2018) Finally, music has been associated with autonomic modulation, potentially attenuating the stress response during neuraxial anesthesia (Y. Wang et al., 2014). Clinically, these findings suggest that patient-preferred music is a simple, low-cost adjunct that may improve the perioperative experience without adding medication-related adverse effects.
Anxiety can influence pain perception and enhance sensitivity by acting on brain regions such as the prefrontal cortex, amygdala, and hippocampus (Vaegter et al., 2020). Music induces psychophysiological responses via the limbic system and is thought to modulate pain perception by promoting the release of enkephalins and endorphins (Nilsson, 2008). Studies investigating music therapy in the perioperative period have examined its effects not only on anxiety but also on pain levels, with numerous studies and meta-analyses demonstrating that music therapy can effectively reduce pain (Drzymalski et al., 2017; Shabanloei et al., 2010). However, some studies have reported no significant effect on pain despite observing reductions in anxiety levels (Drzymalski et al., 2017; Jacquier et al., 2022). These discrepancies are thought to result from differences in analgesic protocols and the timing of music therapy administration across studies. In our study, there was no significant difference in pain rating scores between the 2 groups at 1, 4, and 24 hr postoperatively; however, the pain rating score at 12 hr was significantly lower in Group M. In addition, the need for rescue analgesia was significantly lower in Group M compared to Group C. As part of the multimodal analgesia protocol, all patients received an adductor canal block, which likely contributed to effective analgesia in the early postoperative period, resulting in similarly low pain rating scores at the 1st and 4th hr. By the 12th hr, when the block’s effect was presumed to have diminished, pain perception appeared to be lower in the music group, suggesting a potential role of music in modulating late-phase postoperative pain.
Quality of recovery is widely recognized as a valid outcome measure in both clinical practice and research. It is a multidimensional construct encompassing physiological status, psychosocial well-being, and adverse events (Wu & Richman, 2004). High levels of postoperative pain have been associated with reduced recovery quality. Choi et al. (2023) demonstrated that intraoperative music interventions improved both postoperative recovery and pain in patients undergoing gynecologic laparoscopy. Similarly, Akelma et al. (2024) reported that patient-preferred preoperative music, compared to classical music, more effectively reduced anxiety and improved recovery quality in inguinal hernia surgery. In our study, preoperative QoR-15 scores were comparable between the groups, whereas postoperative QoR-15 scores were significantly higher in Group M. These findings support the notion that music contributes positively to postoperative recovery quality. Furthermore, when interpreted in terms of clinical significance, our results indicate not only a statistically significant difference but also a clinically meaningful improvement.
In modern healthcare, patient involvement in the decision-making process is increasingly emphasized. Patient satisfaction serves as a key indicator of an effective and efficiently functioning healthcare system (Heidegger et al., 2013). Satisfaction is also a critical parameter in evaluating perioperative care. Negative experiences during this period may adversely affect the postoperative recovery process and increase pain-related anxiety levels (Jaensson et al., 2019). In our study, patient satisfaction scores were significantly higher in Group M than in Group C, indicating that music listening markedly enhanced patient satisfaction. Music is believed to exert its effects by activating the parasympathetic nervous system, thereby attenuating physiological stress responses and contributing to hemodynamic stability (Biddiss et al., 2014; Pittman & Kridli, 2011; Zhang et al., 2023). Consistent with the existing literature, our study demonstrated that perioperative music contributed to improved hemodynamic stability at various time points throughout the perioperative period.
Limitations
Although clinical significance was assessed through MCID analyses, the generalizability of the findings may be limited by the single-center design and the inclusion of only a Turkish population. In our study, the music intervention was restricted to the preoperative and intraoperative periods; however, future studies could explore the effects of music applied during the postoperative period or at different perioperative time points. In addition, factors such as high intraoperative noise levels and patient movement during procedures such as joint arthroplasty may influence the efficacy of music interventions, suggesting that their effects could vary across different surgical populations.
Conclusion
This study demonstrated that perioperative administration of patient-preferred music had beneficial effects on anxiety, pain, hemodynamic parameters, quality of recovery, and patient satisfaction in individuals undergoing unilateral knee arthroplasty under spinal anesthesia. Unlike many previous studies, the inclusion of MCID analyses allowed for the evaluation of not only statistical but also clinical significance, thereby facilitating a more patient-centered interpretation of the findings. These results support the use of music as an effective, feasible, and low-cost non-pharmacological intervention in routine clinical practice. Patient-preferred music may be considered as a feasible adjunct in this setting; further multicenter studies could help confirm generalizability and optimize implementation.
Footnotes
Ethical Considerations
2nd Ethics Committee of Ankara Bilkent City Hospital
Authors Contributions
Surgical and Medical Practices: A.A, E.S., Concept: B.N., F.K.A., Design: B.N., F.K.A., Data Collection or Processing: A.A., E.S., Analysis or Interpretation: M.K., G.E., Literature Search: M.K., G.E., Writing: B.N., G.E., F.K.A.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The datasets generated and/or analyzed during the current study are not publicly available but are available from the corresponding author on reasonable request.*
