Abstract
Accidental falls are the second most prevalent adverse event within hospital settings, including U.S.’s Veterans Health Administration (VHA), often resulting in injury and prolonging patient recovery. The Morse Fall Scale (MFS) is widely used to assess fall risk within patient settings. Despite its known limitations, it remains a key tool for determining which patients are at risk for falls across healthcare institutions. Veterans with a completed MFS, Care Assessment Need (CAN), and Charlson Comorbidity Index (CCI), admitted to a VHA hospital from July 1, 2020, to June 30, 2022, were included in this retrospective analysis. MFS total scores were captured using electronic health record data from the VHA’s national Corporate Data Warehouse. Veterans were identified as having a documented fall through clinical notes. Logistic regression models were used to evaluate the tool’s performance at predicting falls. Among 440,771 Veterans, 14,458 (3.3%) had a documented fall during their inpatient stay. On average, those who experienced a fall had higher MFS scores. However, despite this trend, this tool exhibited poor discrimination in the likelihood of falls. Although incorporating patient demographics, the CAN, and CCI into the model improved performance, the model still performed poorly when assessing fall risk. Although the MFS is a required component of clinical workflow in many hospital systems, including VHA, its suboptimal discrimination of fall risk undermines its practical utility. Improved risk models are needed to assess fall risk and from which appropriate fall prevention measures can be initiated.
Introduction
Accidental falls are the second most prevalent adverse event in hospital care settings (Bouldin et al., 2013; Oliver et al., 2010; Quigley et al., 2006). A hospital fall can result in severe patient injury, lead to additional complications, and prolong patient recovery. Estimates suggest that approximately 25% to 50% of all hospital falls result in injury, with nearly 10% ending in serious harm (e.g. fractures and death) (Oliver et al., 2010; Quigley et al., 2006). Furthermore, the overall cost of falls within the United States is estimated at over $50 billion per year (Cost of Older Adult Falls | Fall Prevention | Injury Center | CDC, n.d.), with an inpatient fall costing on average $62,521 per event (Dykes et al., 2023).
Background
Designed specifically to evaluate the risk of falls among hospitalized patients, the Morse Fall Scale (MFS; Morse et al., 1989b) is one of the most common fall-risk assessment tools across U.S. healthcare systems, including the largest integrated system – Veteran’s Health Administration (VHA; Jewell et al., 2020; Quigley et al., 2006). Typically administered by nursing staff, fall-risk mitigating interventions are implemented based upon the resulting total score (U.S. Department of Veterans Affairs, 2004). The VHA provides numerous healthcare and social support services to eligible U.S. Veterans and several fall prevention programs to proactively reduce hospital falls. Since 1999, the MFS has been consistently collected and documented within the VHA (Quigley et al., 2006) and remains the primary tool for assessing fall risk across all VHA inpatient settings.
A thorough evaluation of the MFS’s ability to accurately assess fall risk in the VHA and other healthcare system settings is warranted. Prior studies outside the VHA have identified several key limitations in MFS’s ability to accurately assess fall risk. These include a substantial false positive rate for documented hospital falls (O’Connell & Myers, 2002) and worse accuracy and precision than other fall-risk assessment tools, such as John Hopkins Fall Risk Assessment Tool (Kim et al., 2022) and Hendrich II Fall Risk Model (Nassar et al., 2014). Suspected reasons have included that the MFS does not account for pertinent acute modifiable conditions (e.g. changes in medication, care equipment) (Kim et al., 2022; Nassar et al., 2014), overemphasis on history of previous falls, and insufficient accounting of critical dynamic factors such as changes in diagnoses and treatments, which result in performance degradation over time (Ghahramani et al., 2016).
We aimed to evaluate whether accounting for such factors in established risk indices of comorbidity and mortality might augment MFS’s fall risk prediction performance for hospitalized patients. Originally intended to assess patient morbidity and mortality risk, the Care Assessment Need (CAN) score and the Charlson Comorbidity Index (CCI) have been repurposed to assess frailty and other patient outcomes, including after surgery and after cancer diagnosis (Hasan et al., 2020; Kuo et al., 2021; Osborne et al., 2020a, 2020b; Ruiz et al., 2018; Soerensen et al., 2021; Tuty Kuswardhani et al., 2020).
Aim
This assessment evaluated (a) the performance of the MFS in predicting hospital falls in VHA and (b) whether other established risk indices of morbidity and mortality (CAN and CCI), enhances the MFS’s prediction accuracy.
Methods
Assessment Design
Retrospective cross-sectional case-control analysis using VHA’s national electronic health record (EHR) data.
Data Source and Patient Cohort
EHR data from across VHA is centralized in a relational database, the Corporate Data Warehouse (CDW). In CDW, we identified patients from ages 18 to 105 years, who were admitted to an acute care VHA setting between July 1, 2020, and June 30, 2022. We excluded patients with no MFS documented during admissions or those with an incomplete CAN or CCI score, which indicates that they were not actively part of a care team or actively involved in the VHA healthcare system within the last 2 years (Fihn et al., 2013; Figure 1).
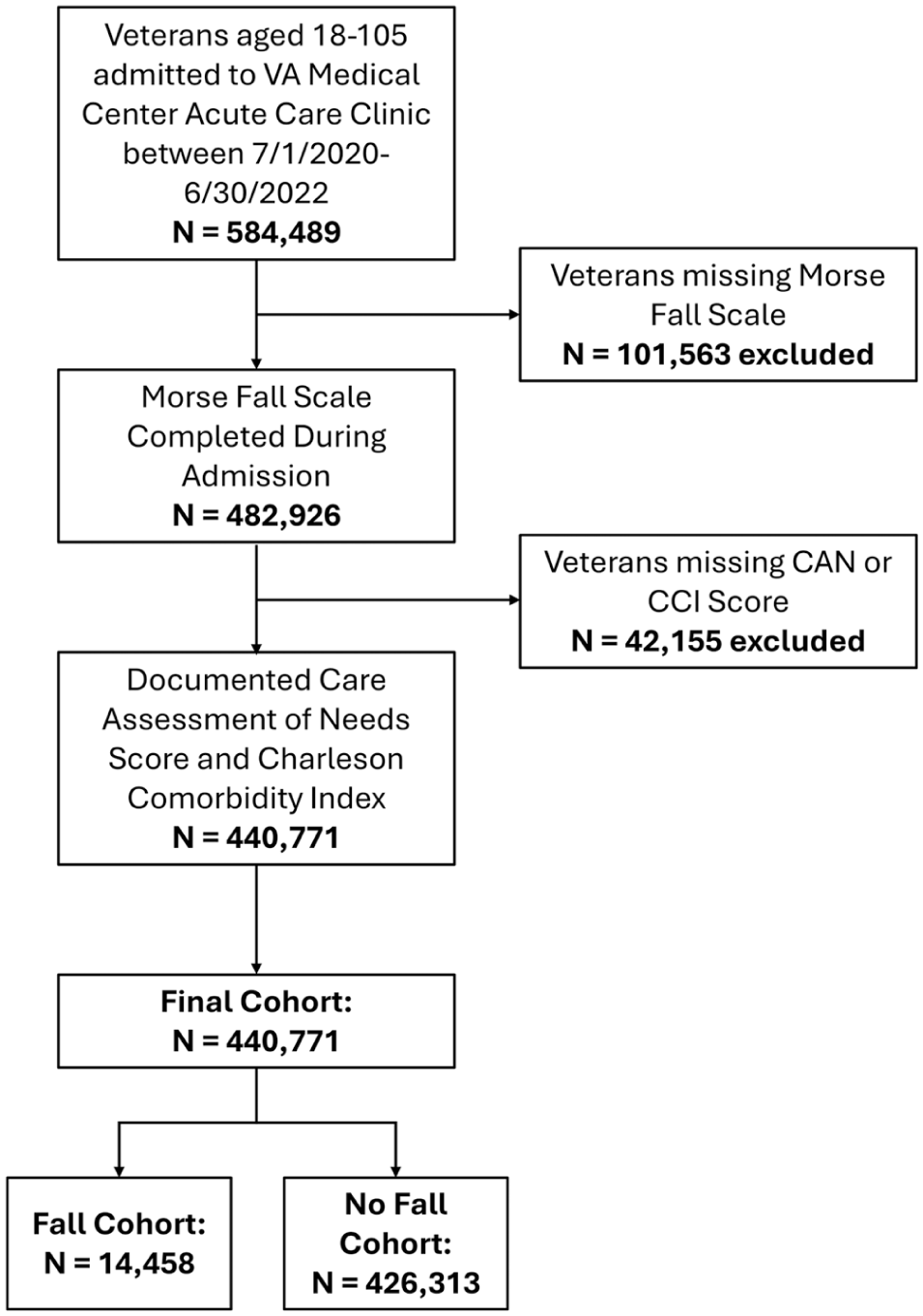
Flowchart depicting the selection of the assessment cohort.
Model Variables
Patient Characteristics
Demographic information was extracted from the CDW. These characteristics included the patients’ age at admission, sex (male, female), race (American Indian/Alaskan Native, Asian, Black or African American, Native Hawaiian or Other Pacific Islander, White, Missing/Unknown), and ethnicity (Hispanic or Latino, Not Hispanic or Latino, Missing/Unknown).
Morse Fall Scale
The MFS includes six variables in its assessment of fall risk (Morse et al., 1989b). Supplemental Table 1 details each risk factor and the associated response score. All items are added together to obtain a total score, which ranges from 0 to 125. Higher scores indicate a greater fall risk (Morse et al., 1989a). Within the VHA, MFS total scores are categorized into risk groups (i.e. Low [0–24], Moderate [25–44], High [45–125]). Based upon VHA policy, the MFS is completed by nursing staff upon the patient’s admission and at any change in status (e.g. change in location or mobility assisted device). Fall-risk mitigating interventions are implemented both based upon the resulting risk groups and specific item responses. These results are then recorded and incorporated into the patient’s EHR note templates (About VHA – Veterans Health Administration, n.d.; U.S. Department of Veterans Affairs, 2004). Throughout a patient’s inpatient stay, multiple MFS may be completed. Among those who did not experience a fall, the MFS closest to their admission date was extracted. For those with a documented fall, the MFS closest to, but not following, the fall event was obtained.
Care Assessment Need
The VHA’s CAN 1-Year Mortality model utilizes 38 structured EHR variables to assess a patient’s risk of mortality within the following year (Fihn et al., 2013). Calculated weekly, the model produces a probability of mortality for each patient, expressed as a percentile from 0 to 99, with a higher number indicating a higher risk. As the CAN risk-assessment model is automatically calculated weekly, the score closest to the patient’s admission date was extracted and used for this assessment.
Charlson Comorbidity Index
Developed in 1987, the CCI is intended to evaluate the 10-year survival outlook for patients with multiple comorbidities (Charlson et al., 1987, 2022). The CCI applies varying weights to 17 different disease categories and has been reliably leveraged to evaluate and predict patient prognosis. For this assessment, the CDW was used to obtain all diagnosis codes available prior to a patient’s admission date to retrospectively calculate the CCI.
Falls Definition
The VHA National Center for Patient Safety defines a fall as a loss of upright position that results in the patient landing on the floor, or on an object (U.S. Department of Veterans Affairs, 2004) and excludes falls resulting from violent blows or other purposeful actions (Young-Xu et al., 2020). Clinicians use this definition to identify and document incidence of falls within the VHA’s EHR (U.S. Department of Veterans Affairs, 2004). We classified patients into two cohorts during the assessment period: (a) those with any documented fall during their stay, and (b) those with no documented fall. Specific clinical progress note titles and definitions were used to identify patients with documented falls. Supplemental Table 2 outlines the inclusion/exclusion criteria for identifying falls through EHR progress notes.
Data Analysis
Descriptive statistics were used to summarize and compare patient characteristics among those with and without a documented fall. Significance testing (i.e. Student’s T-test, χ2 test) was used to evaluate differences among the two cohorts. Logistic regressions, with the inclusion of orthogonal polynomial terms, were used to assess the tool’s ability at evaluating the likelihood of falls in VHA acute care settings. Orthogonal polynomials were leveraged to account for collinearity among polynomial terms. Likelihood-ratio tests were utilized to assist with model selection and the evaluation of polynomial terms. To identify optimal thresholds and calculate model specificity and sensitivity, the Youden Index was leveraged. Because this assessment utilized a fixed, large dataset of all eligible Veterans, an a priori power analysis was not conducted. Instead, the full available sample was utilized, enabling the detection of small to moderate effect sizes in observational assessments (Cohen, 2013).
Finally, since the CAN and CCI scores have been successfully repurposed to assess patient outcomes (Hasan et al., 2020; Kuo et al., 2021; Osborne et al., 2020a, 2020b; Ruiz et al., 2018; Soerensen et al., 2021; Tuty Kuswardhani et al., 2020), and patient demographics are known factors in fall risk (Ghahramani et al., 2016; Jewell et al., 2020; Quigley et al., 2006), a logistic regression model including these variables was performed.
All data analysis was conducted using R Statistical Software v4.1.2. This quality improvement and evaluation project received a Determination of Non-Research from Stanford IRB #72805 (Stanford University, Stanford, CA, USA).
Results
Sample Characteristics
Of the 584,489 Veterans admitted to an acute care setting during the assessment period, a total of 440,771 patients comprised the analytic sample (Figure 1). The sample was predominantly male (92.6%), with an average (Standard deviation [SD]) age of 66.9 (14). The majority self-identified as White (67.8%), followed by Black or African American (23.8%), and identified as not Hispanic or Latino ethnicity (88.5%). Evaluating clinical characteristics, the average (SD) total score for the CAN score was 65.5 (SD = 28.6), while the average CCI score was 3.9 (SD = 3). Among this sample, 14,458 (3.3%) had a documented fall during their hospital stay (Table 1).
Sample Characteristics Among Veterans With a Documented Fall Compared to Those Without Using χ2 and t-Test.
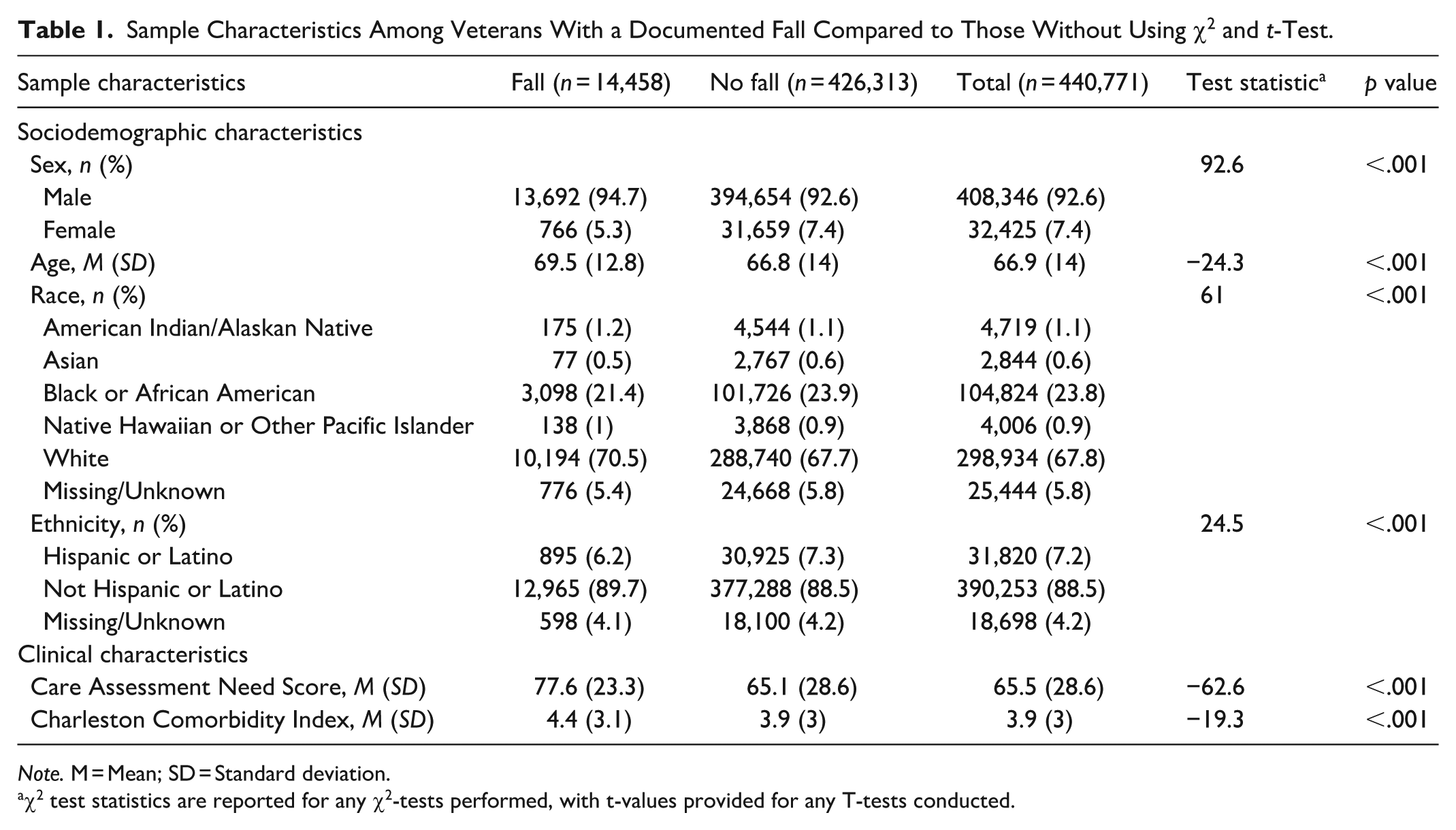
Note. M = Mean; SD = Standard deviation.
χ2 test statistics are reported for any χ2-tests performed, with t-values provided for any T-tests conducted.
Student’s T-test and χ2 tests revealed significant differences in demographics between those with and without a documented fall (Table 1). Those with a documented fall were slightly older (69.5 [SD = 12.8] vs. 66.8 [SD = 14), p < .001) and represent a greater proportion of males (94.7% vs. 92.6%, p < .001). Black or African American Veterans represent a greater proportion of the no fall group (23.9%) compared to those with a documented fall (21.4%). Conversely, White Veterans represented a greater proportion of the fall group (70.5%) compared to those without a documented fall (67.7%). In addition, a greater proportion of those who identified as Not Hispanic or Latino represented the fall group (89.7%) compared to those without a documented fall (88.5%).
When comparing clinical characteristics, individuals who experienced a fall had, on average, higher total scores. Patients with a documented fall exhibited a significantly higher CAN score (77.6 [23.3] vs. 65.1 [28.6], p < .001) as well as significantly higher CCI scores compared to those without a fall (4.4 [3.1] vs. 3.9 [3], p < .001).
MFS Results
Among the entire sample population, the average (SD) total score for the MFS was 45.5 (23.3), with those who experienced a fall having significantly higher average total MFS scores compared to those who did not experience a fall (57.8 [26.4] vs. 45.1 [23.1]; p < .001) (Table 2). Despite this difference, Figure 2 depicts an overlap in the distribution of total scores observed among the two populations, with minimal discernable patterns. It should be noted that the substantial outliers observed within this figure show that 68.5% of the sample population exhibited an MFS score of 35.
Morse Fall Scale Risk Classification by Incidence of Fall.
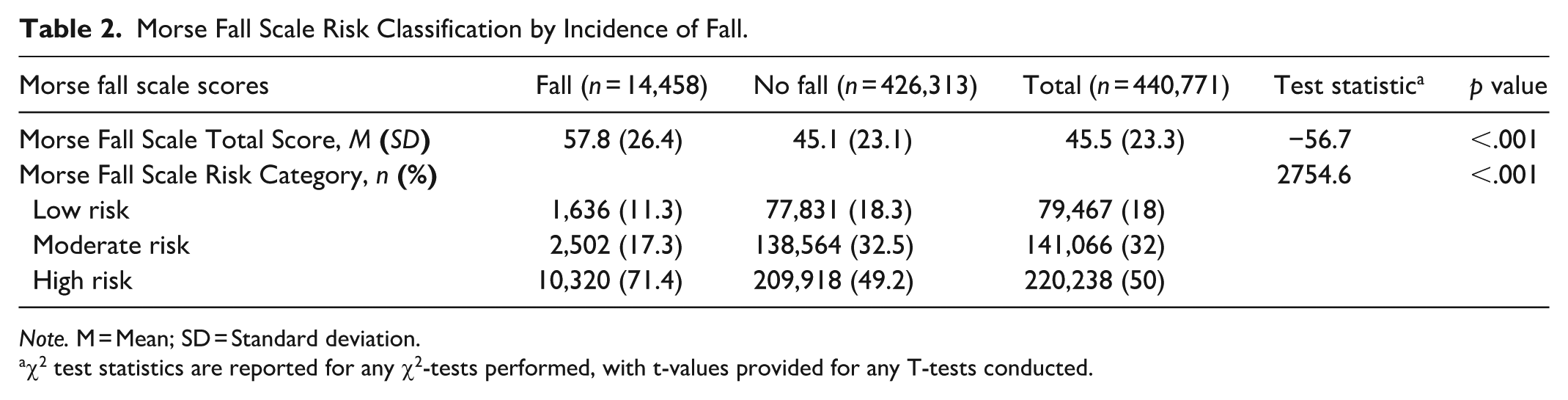
Note. M = Mean; SD = Standard deviation.
χ2 test statistics are reported for any χ2-tests performed, with t-values provided for any T-tests conducted.
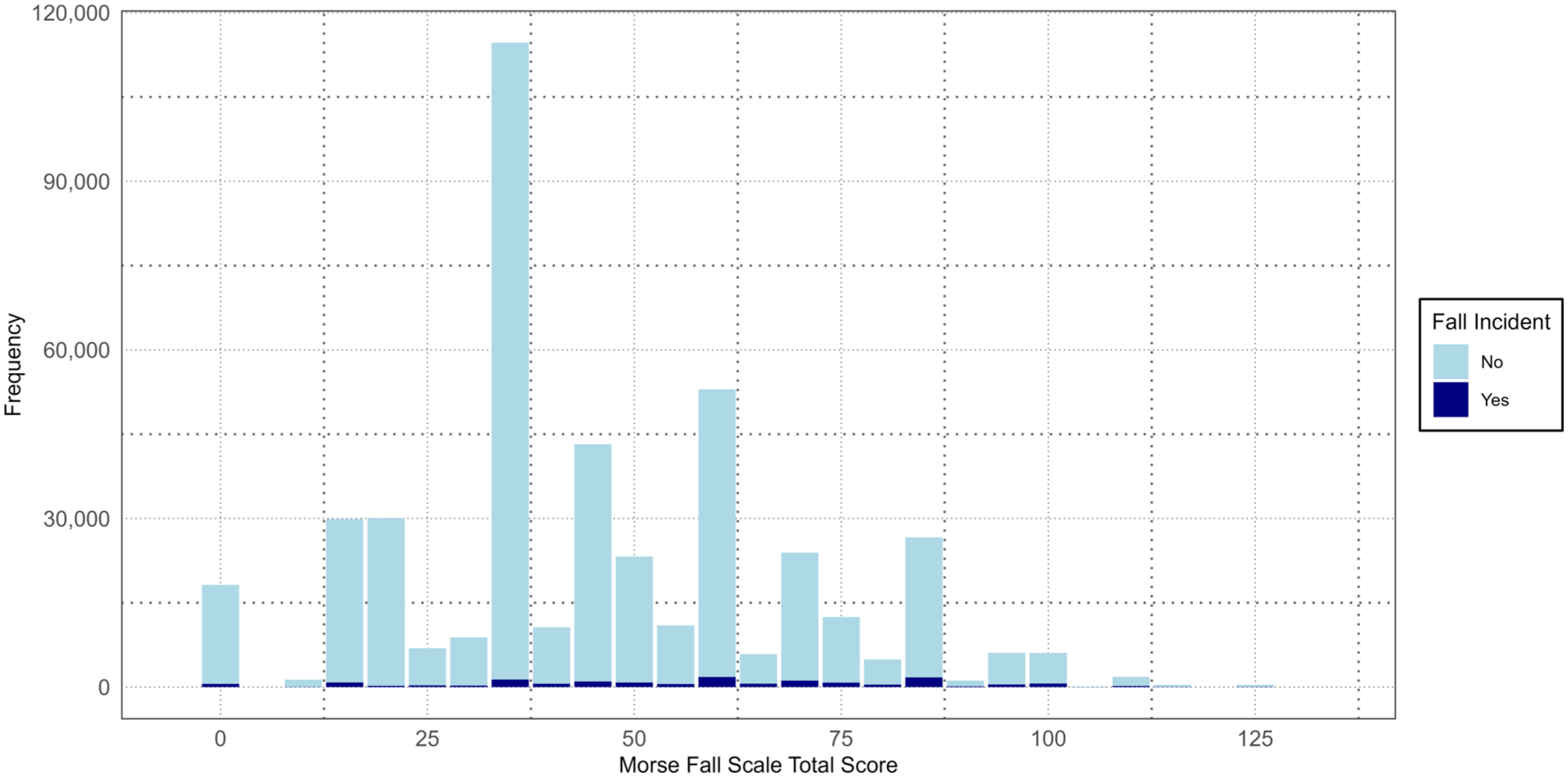
Distribution of Morse Fall Scale total scores by fall incident status.
Evaluating the resulting risk categories based upon MFS total score, 18% of the sample population were considered “Low Risk,” 32% were classified as “Moderate Risk,” and 50% as “High Risk” (Table 2). When examining the distribution of risk group classifications, significant differences were observed among the fall and no fall cohorts (χ2 statistic = 2,754.6, p < .001). Among those with a documented fall, 71.4% were classified as “High Risk,” while 11.3% were classified as “Low Risk.” Similarly, among those who did not experience a fall, 49.2% were classified as “High Risk,” while 18.3% were classified as “Low Risk.” When considering the proportion of fall incidence by risk category, 2.1% of those classified as “Low Risk” experienced a fall, while 1.8% of those classified as “Moderate Risk” had a documented fall. Among the “High Risk” cohort, 4.7% of patients experienced a fall.
Among the individual responses of the MFS questions, 82.7% of the sample population had a secondary diagnosis (i.e. ≥2 medical diagnoses in chart) while 80.1% had documented “IV or IV access” (Table 3). “IV or IV access” refers to the presence of an intermittent-use or continuous-use intravenous fluid therapy. When comparing those with and without a documented fall, significant differences were observed among each question. The greatest difference between groups was from MFS question regarding the patients’ history of falls. Among those who experienced a fall, 48.8% had a documented history of falling, while only 22.8% of those who did not experience a fall had a history of falling. Although significant, minimal differences were observed among the MFS question regarding a secondary diagnosis. Among those who fell, 87% had a documented secondary diagnosis, compared to 82.5% among those who did not experience a fall. Additionally, among those patients with a documented fall, 69.7% had documented “IV or IV access” compared to 80.4% without a fall.
Morse Fall Scale Question Responses Among Patients with a Documented Fall Compared to Those Without Using χ2 -Test a .
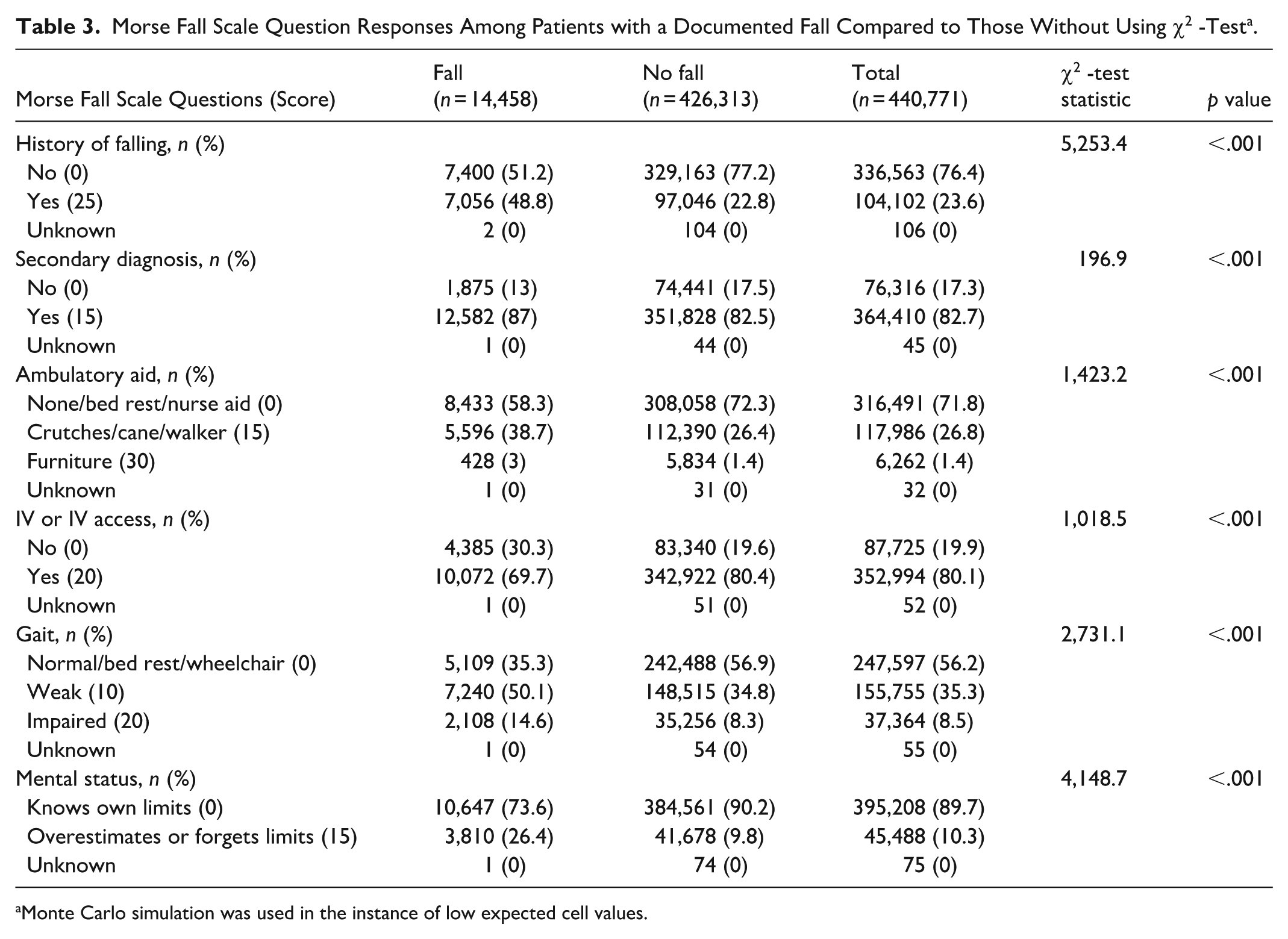
Monte Carlo simulation was used in the instance of low expected cell values.
MFS Model Results
Several statistical models were utilized to assess the performance of the MFS (Table 4). The logistic regression model with a linear term (Model 1) suggested that an increase in the MFS total score is associated with increased odds of a documented fall. However, this base model resulted in an area under the curve (AUC) of 0.65, suggesting poor discrimination in the MFS ability to predict a fall for an individual. The inclusion of a quadratic term (Model 2) resulted in a significant polynomial term and an improvement in model fit over the base model (likelihood ratio test [LRT]: χ2 (1) = 214.6, p < .001). However, this model did not provide an improvement in discrimination of a documented fall (AUC: 0.65). Finally, a cubic term was included in the model (Model 3), resulting in significant polynomial terms and an improvement in model fit over the quadratic polynomial model (LRT: χ2 (1) = 559.9, p < .001). The curvilinear fit of this model suggested a slight increase in the likelihood of a documented fall at MFS total scores near zero and a slight decrease in likelihood at total scores near 125. Figure 3 provides a depiction of the proportion of MFS total scores by fall incident fitted with the curvilinear model. However, like the other models, this model also resulted in poor discrimination (AUC: 0.66). Leveraging the Youden Index, we identified an optimal threshold at 0.026 which provided a sensitivity of 0.68 and a specificity of 0.57.
Model Coefficients and Standard Errors Comparing Assessment Tool Scores and the Incidence of Fall Using Polynomial Logistic Regressions.
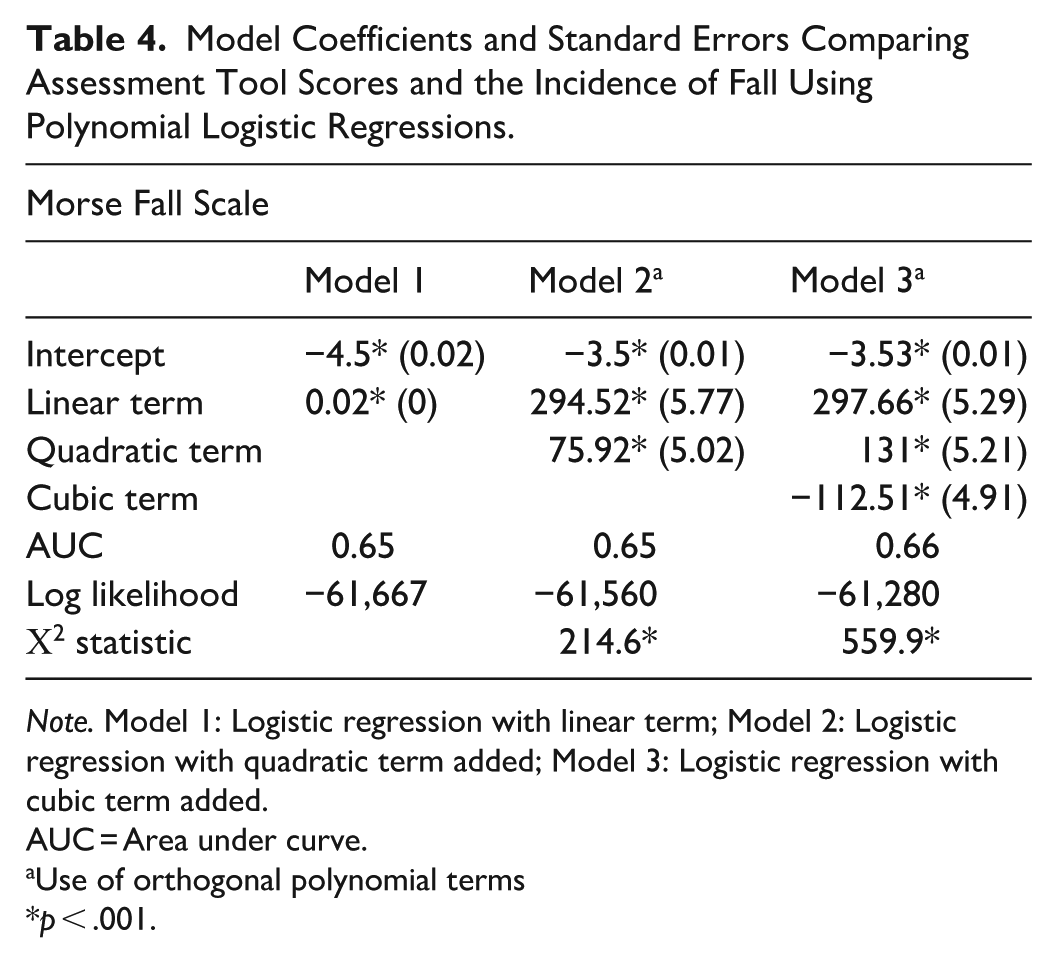
Note. Model 1: Logistic regression with linear term; Model 2: Logistic regression with quadratic term added; Model 3: Logistic regression with cubic term added.
AUC = Area under curve.
Use of orthogonal polynomial terms
p < .001.
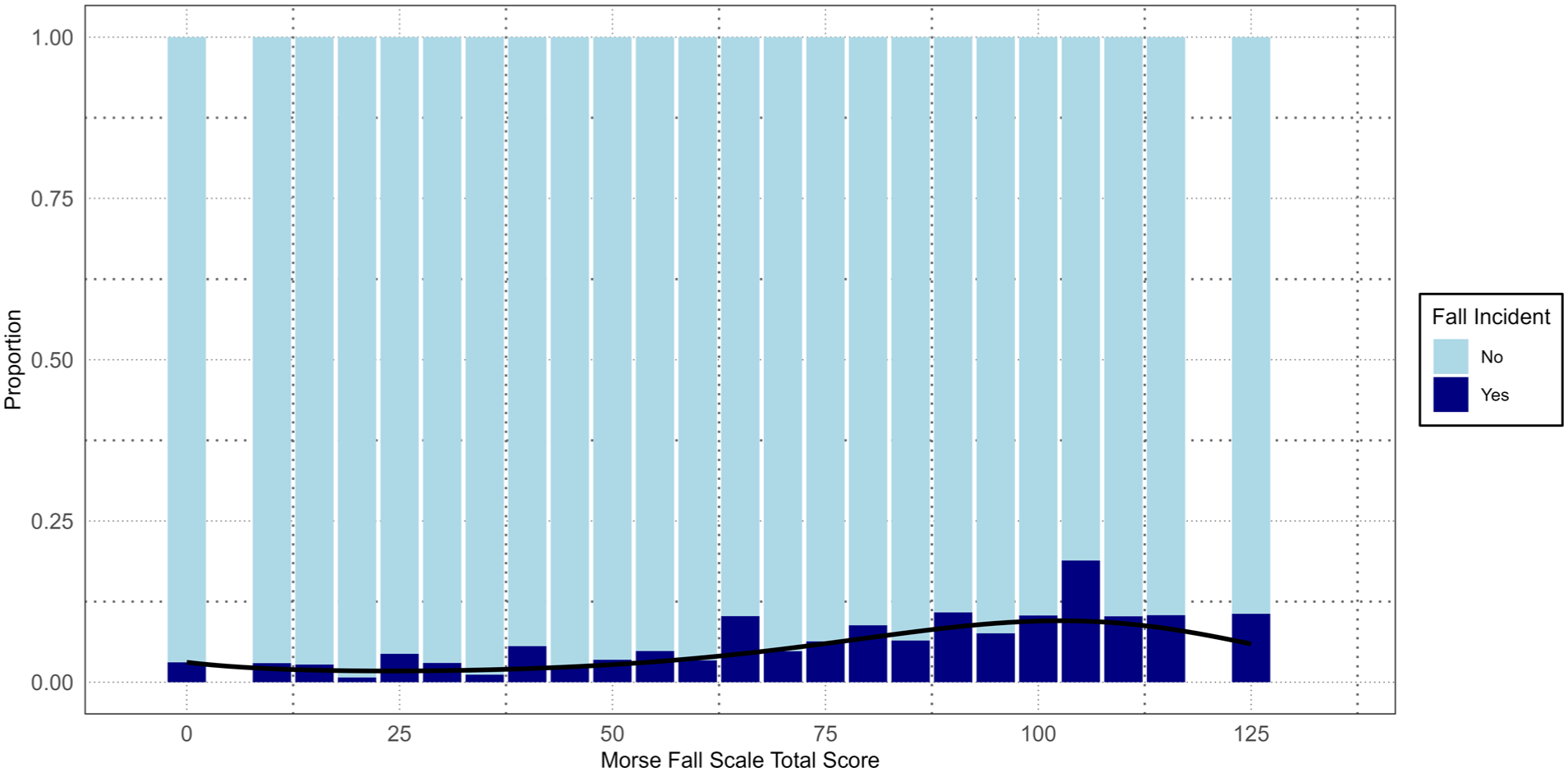
Proportion of Morse Fall Scale total scores by fall incident status with fitted cubic polynomial logistic regression model.
Final Model Results
To determine if patient and clinical characteristics improve model performance, the CAN, CCI, and patient demographics (i.e. age, sex, race, and ethnicity) were included within our model. When comparing the AUC, the inclusion of these additional variables appeared to improve model performance. We obtained an AUC of 0.7, compared to the 0.66 of our cubic polynomial model. With an optimal threshold of 0.032, Figure 4 further depicts the confusion matrix comparing the predicted and actual fall incident status of the cohort. Among the 14,458 patients with a documented fall, 64% (n = 9,274) were predicted to experience a fall. Similarly, among those who did not experience a fall (n = 426,313), 64% (n = 274,509) were accurately predicted. Despite these improvements over the original model, this model exhibited poor precision at 5.8%. The model coefficients are provided within Supplemental Table 3. Although slight collinearity was present within this model, Supplemental Table 4, correlation among variables does not impact predictive performance.
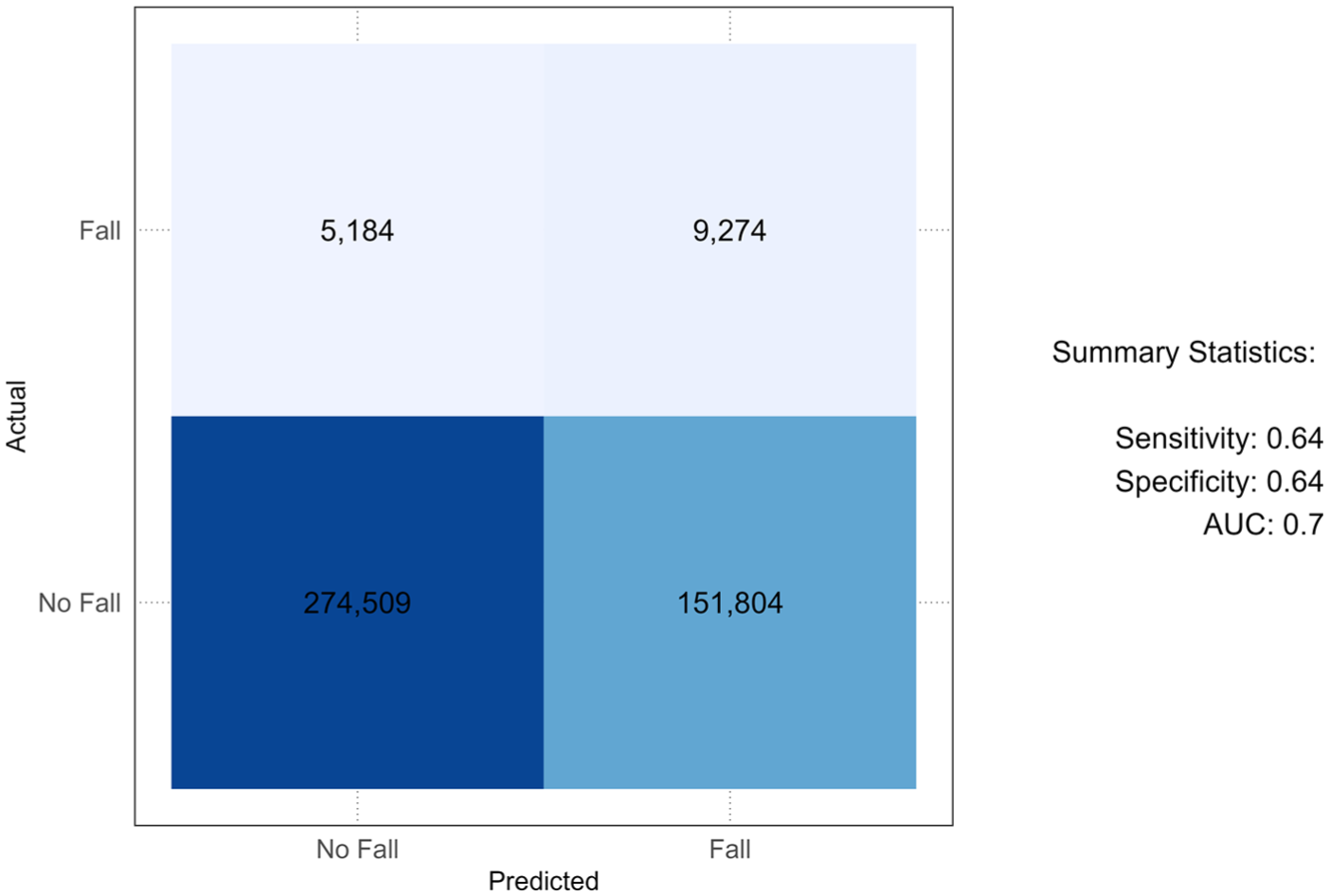
Total number of Veterans by actual and predicted fall incident status.
Discussion
Our results suggest the need for an improved fall-risk clinical assessment tool that enables healthcare providers to accurately identify inpatients at risk of falling and then initiate customized targeted interventions. We demonstrated that the MFS is insufficient to predict and discriminate the likelihood of a fall during an acute care stay within the VHA. Our best performing model resulted in a sensitivity of 68% and a specificity of 57%. As a result, this model, with poor discrimination, classified most patients into the no fall group. The ability to accurately determine which inpatients are at high risk for fall is critical for reducing falls and related injuries (U.S. Department of Veterans Affairs, 2004). Nursing staff are required to complete the MFS fall-risk assessment tool for all VHA inpatient admissions and during any inpatient status change (About VHA – Veterans Health Administration, n.d.; U.S. Department of Veterans Affairs, 2004). Yet, to our knowledge, this is the first assessment analyzing the efficacy of the MFS across all VHA acute care settings, which includes over 3,500 ward locations.
Studies that have assessed the MFS in the Veteran population have been sparse and limited in scope. While one study provided descriptive statistics on the MFS within the VHA, this work did not evaluate its validity nor consider the prevalence of fall events following assessment (Quigley et al., 2006). Moreover, this prior study primarily focused on a few select VHA medical centers. When compared to our findings, a smaller single-site study also observed similar unsatisfactory performance results, reporting a sensitivity of 83% and specificity of 29% for the MFS (O’Connell & Myers, 2002). Another study observed slightly better performance, with a sensitivity of 85.7% and specificity of 58.8% (Kim et al., 2022). Additionally, two international studies in Brazil and Lebanon found that the MFS sensitivity was 95.2% and 36.9%, and specificity was 64% and 53.9%, respectively (De Souza Urbanetto et al., 2016; Nassar et al., 2014).
Several potential intrinsic limitations of the MFS may contribute to these results in a healthcare setting. The MFS places disproportionate emphasis on a history of falls, as noted by the scoring weights (Ghahramani et al., 2016; Kim et al., 2022). In general, patients often may not have accurate documentation of prior falls or may not be able to accurately recall prior fall events (Ganz et al., 2005; Hale et al., 1993; Hoffman et al., 2018). This may lead to the misclassification among those patients without a documented history of falls (Ghahramani et al., 2016). Within our sample, while those who experienced a fall had a greater prevalence of prior falls, over 50% of those without a prior fall experienced a fall during hospital care. Appropriate interventions may not have been placed for these inpatients due to the lack of reliable historical fall reporting.
While the MFS was developed for acute care units (Morse et al., 1989a, 1989b), it lacks sensitivity in assessing fall risk among Veterans in inpatient settings, who often have more comorbidities than the general population (Wong et al., 2016). In our sample, over 80% had a secondary diagnosis, and nearly 80% had a document “IV or IV Access,” a common intervention in acute care settings (Connolly, 2018). These factors, included in the MFS assessment, may inflate fall-risk scores, explaining the disproportionately high number of patients with an MFS score of 35. This artifact is consistent with previous VHA findings (Quigley et al., 2006). Of those scoring 35, 95.7% had a secondary diagnosis and IV or IV access, indicating that these elements skew the MFS score.
Based upon the MFS scoring criteria, and VHA’s falls policy, an MFS score greater than 44 is considered “High Risk” (Morse et al., 1989b; U.S. Department of Veterans Affairs, 2004). It is not surprising that 50% of patients were classified as “High Risk,” upon reviewing the responses to the MFS and the characteristics of the sample population. However, this broad classification of “High Risk” may diminish the ability to differentiate and prioritize patients who are truly at greatest risk of falling. Although fall prevention strategies are developed and implemented individually, more nuanced fall-risk classifications are needed to better prioritize Veterans within these settings.
There are several notable strengths of our work, including the significant size and scope of our cohort in the U.S.’s largest integrated healthcare system. By refining our assessment to acute care settings, where reporting falls is a required mandate (U.S. Department of Veterans Affairs, 2004), we optimized the accuracy and reliability of the falls data, which addresses a known limitation of prior work (Ganz et al., 2005; Hale et al., 1993; Hoffman et al., 2018; Quigley et al., 2006). In addition, by assessing the utility of the MFS across all acute care settings, we obtained a large national sample that allowed for statistically robust results. Moreover, because this assessment included both patients with and without a documented fall, we were able to compare the clinical and demographic characteristics of these cohorts based upon their fall incident status, which addresses a limitation of prior work within VHA (Quigley et al., 2006; Young-Xu et al., 2020).
This assessment has limitations to consider. This work was performed within VHA, which represents a primarily male and older population with more comorbidities than other patient populations (Joan Wang et al., 2021; Wong et al., 2016). These population characteristics present the opportunity to examine the efficacy of MFS for patients with complex health needs but may limit the generalizability of the results. Since the MFS is used widely among healthcare systems, our results convey that other healthcare systems and settings should evaluate the efficacy of these assessments on their own unique patient populations. As this was an assessment which utilized a fixed, large dataset of all eligible Veterans, a traditional prospective power analysis was not performed. However, the sample size of 440,771, exceeding the scale of prior evaluations of the MFS, is substantial and confers adequate power to detect meaningful effects (Cohen, 2013). This is supported by the significant results (e.g. <0.001) obtained from the Student’s T-test, χ2 test, and logistic regressions, demonstrating increased precisions in our estimates. From a retrospective analysis, our results may be confounded by uncontrolled factors, such as a provider’s awareness of the MFS results (Hale et al., 1993; Oliver et al., 2010). This awareness may bias the implementation of fall prevention strategies. And while universal fall precautions are implemented based upon the patients’ MFS risk classification, individualized fall prevention interventions (U.S. Department of Veterans Affairs, 2004) are neither captured nor documented consistently in a standardized way. These limitations make it challenging to fully evaluate the efficacy of the MFS. Nonetheless, the classification of 50% of our population as “High Risk” highlights the tool’s lack of sensitivity to discriminate patients most at risk. Furthermore, the CAN and CCI, while dynamically calculated, appear to miss pertinent factors when assessing fall risk within this population. When incorporated within the logistic model alongside the MFS, these indices provided only slight incremental improvement in discrimination of fall assessment and overall model fit. This suggests that although they might provide some insight as to who might be at greater fall risk, their contribution beyond the MFS is limited. Future work may benefit from more targeted predictors to meaningfully enhance fall-risk assessment.
These findings underscore the need for an improved fall-risk assessment tool that enables our healthcare providers to accurately identify patients at risk of falling and then initiate individualized targeted interventions. A more robust model that incorporates additional drivers of fall risk and rapidly adapts to a patient’s changing clinical presentation would be invaluable. Furthermore, embedding such a model directly into the EHR, with real-time clinician access to automated risk calculation, would ensure consistent and efficient risk assessment while reducing the burden on clinical staff.
Conclusion
While the MFS remains a popular fall-risk assessment tool among healthcare systems and a required component of VHA clinical workflows, the MFS demonstrated suboptimal performance in predicting falls in the VHA acute care setting, calling into question its practical utility. In our evaluation, we identified several shortcomings in the MFS that may inhibit MFS’ ability to accurately assess fall risk. As such, a critical need for improved fall-risk prediction models exists to ensure better clinical fall-risk assessment and prevention strategies for patients.
Supplemental Material
sj-docx-1-cnr-10.1177_10547738261429981 – Supplemental material for Predicting Falls With the Morse Fall Scale: A Retrospective Assessment at the Veterans Health Administration
Supplemental material, sj-docx-1-cnr-10.1177_10547738261429981 for Predicting Falls With the Morse Fall Scale: A Retrospective Assessment at the Veterans Health Administration by Peter J. Hoover, Terri L. Blumke, Anna D. Ware, Malvika Pillai, Amber L. Wake, Kiran Rai and Jennifer S. Lee in Clinical Nursing Research
Footnotes
Author Note
Malvika Pillai participated in the assessment during their employment with the U.S. Department of Veterans Affairs, but is no longer affiliated with the VA.
Ethical Considerations
This quality improvement and assessment project received a Determination of Non-Research from Stanford IRB #72805 (Stanford University, Stanford, CA, USA). The IRB determined that this project was conducted to assess, analyze, critique, and improve current processes in an institutional setting, involving data-guided activities designed to bring about prompt improvements. Therefore, it does not meet the definition of research nor clinical investigation, and thus participant consent is deemed unnecessary according to national regulations (45 CFR part 46). In addition, no specific human subjects were contacted during this work.
Author Contributions
P.J.H.: Data curation, Formal analysis, Methodology, Visualization, Writing – original draft, Writing – review & editing; T.L.B.: Data curation, Methodology, Validation, Writing – review & editing; A.D.W.: Methodology, Validation, Writing – review & editing; M.P.: Methodology, Validation, Writing – review & editing; A.L.W.: Writing – review & editing; K.R.: Writing – review & editing; J.S.L.: Conceptualization, Project administration, Resources, Supervision, Writing – review & editing. All authors read and approved the final manuscript.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
Due to US Department of Veterans Affairs (VA) regulations and ethics agreements, the data utilized for this assessment are not permitted to leave the VA firewall without a Data Use Agreement. However, VA data can be made available to researchers with an approved IRB and VA authorized study protocol. For more information, please visit ![]() or contact the VA Information Resource Center at VIReC@va.gov.
or contact the VA Information Resource Center at VIReC@va.gov.
Supplemental Material
Supplemental material for this article is available online.
Author Biographies
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
