Abstract
Improving breastfeeding rates is a global goal. To achieve it, actions targeting modifiable factors that influence the breastfeeding experience, such as maternal self-efficacy, could be a promising path, especially with preterm infants’ mothers. Considering the current ubiquitous technology, we developed a mobile application for mothers of preterm infants to constitute a breastfeeding information and support platform. The study was developed in three phases: a survey to determine characteristics and preferences of preterm infants’ mothers; the app development by an interdisciplinary team, following the principles of Disciplined Agile Delivery; and the face and content validation by 10 professionals. The app contains 80 screens and 11 strategies to address prematurity, lactation, breastfeeding, peer support, maternal emotions, resilience, and motivation. Nurses can apply their expertise by designing mHealth-based interventions, employing scientific evidence, and considering the interests and preferences of the target population. Future studies will assess the user experience, the effect on breastfeeding self-efficacy, and breastfeeding rates, and develop a culturally adapted English version of the app for women in Canada.
Introduction
In this study, we report an applied research experience in a developing country, creating a mHealth resource to support mothers of preterm infants in breastfeeding. The occurrence of preterm birth, defined as before the 37th gestational week, can increase the likelihood of challenges with successful breastfeeding (Brockway et al., 2017). It is believed that swallowing-breathing-sucking coordination in premature infants does not exist until the age of 33 to 34 weeks (Orovou et al., 2022), requiring mothers to pump breast milk for some time. Additionally, these women experience feelings of maternal stress and anxiety, inadequacy, guilt, and failure (Palmér & Ericson, 2019). These factors imply that preterm infant mothers usually present reduced breastfeeding self-efficacy rates (Fernández Medina et al., 2019; Merlinda et al., 2017) since it is based both in the result of the performance also in conditional factors such as the intricacy of the task the woman is faced with, and the effort required to perform this task (Dennis, 1999).
Access to quality information and peer support are important aspects for women to decide on breastfeeding and persist in this decision. Online technologies have gained increasing popularity in women’s preference as a source of guidance and support (Demirci et al., 2016; Skelton et al., 2018). However, most apps do not use scientific research. Recent studies have revealed that online resources as websites (Dol & Richardson, 2019), and apps (Richardson et al., 2019) aimed at parents of Neonatal Intensive Care Unit (NICU) infants “are lacking and of concern in terms of quality and credibility” (Richardson et al., 2019, p. 2). We are unaware of any mobile app designed to specifically help mothers of preterm infants establish and maintain breastfeeding (Campana et al., 2022). Considering this gap, our aim is to develop and perform face and content validation of a mobile app to provide breastfeeding support to mothers of preterm infants.
Method
The app was based on the Breastfeeding Self-Efficacy Theory (Dennis, 1999) and positive psychology aspects (Kobau et al., 2011; Van Zyl et al., 2020). The Breastfeeding Self-Efficacy Theory states that self-efficacy expectations can influence women’s judgments regarding their ability to initiate, persist in, and continue breastfeeding, and positive psychology is the study of people’s positive attributes, psychological assets, and strengths. We conducted the study remotely over 15 months (2019–2021), involving researchers and evaluators from Brazil’s South, Southeast, and North regions, and from a province in Canada. The study consisted of three stages: 1. Initial exploratory stage, 2. App development, and 3. Appearance and content validation by a panel of experts. It was approved by the Research Ethics Committee (opinion 3.852.898, Certificate of Presentation of Ethical Appreciation 27703419.8.0000.5231), and all participants provided written informed consent.
App Development
We surveyed a convenience sample of 11 preterm infants’ mothers in a tertiary hospital in southern Brazil. Mothers who reported a desire to breastfeed answered questions about sociodemographic and clinical data, information about mobile device access, internet use, and preferences about apps and media/resources. Women who had a premature birth gave their opinions about the subjects and types of resources they expected to find in an app aimed at helping them to breastfeed their preterm babies.
Two authors experienced in supporting breastfeeding of preterm infants, one neonatal nurse and one lactation consultant, started the app development. The app’s content was based on scientific evidence about managing preterm infant breastfeeding (Brockway et al., 2017; World Health Organization [WHO], & United Nations Children’s Fund [UNICEF], 2020). The theoretical frameworks adopted (Dennis, 1999; Van Zyl et al., 2020) provided the app’s motivational content focused on promoting maternal self-confidence. After creating the content scripts, the authors designed an initial prototype with a descriptive proposal for navigation flow and interactivity with the user.
A multidisciplinary team was assembled, comprised of two nursing professors, four computer science undergraduate students, and one software developer. Working remotely, with weekly meetings via Google Meet, our team started discussing the feasibility and prepared a technical list of requirements for the initial prototype, ordered by priority, following the Agile Development Principles (Alyahya et al., 2013). We used the Figma vector on the app prototyping graphic; React Native to create declarative interfaces through native components written in JavaScript; Typescript as a programming language, and Android as the operating system. To manage the project version, we adopted Git, a software that simplifies the participation of several developers in the same database. To store the application code, we used a repository on GitHub.
Across 5 months, undergraduate students developed a part of the app’s requirements, which were presented and discussed at each weekly meeting, so the app prototype was viewed via Figma and examined. A new Android Application Pack (.apk) was released and tested by the team throughout the week, in successive cycles, until the completion of the application development (Alyahya et al., 2013).
A panel of experts evaluated the app’s face and content validity. Experts were selected according to the criteria: 1 – master’s degree or PhD and at least 2 years of clinical or research experience in breastfeeding preterm infants, OR 2 – graduation in Psychology/Coach Certification and a minimum of 2 years of professional experience. Experts received a questionnaire by e-mail for characterization and a tool to evaluate screenshots of the app.
For the first evaluation round, the experts evaluated the app’s objectives, structure/presentation, and relevance using a Likert-type scale of 1 = “strongly disagree” to 5 = “strongly agree.” Twenty-three items were related to breastfeeding experts, and 12 items were related to Psychology/Coaching specialists. They should suggest app improvement for items assigned by responses 1 and 2.
We calculated the content validity coefficient (CVC), an objective method for quantitatively measuring content validity, when a select panel of content experts evaluates an instrument and rates item relevance to the domain of content, responding to a Likert-type rating scale. The proportion of experts who are in agreement about item relevance provides a quantitative measure of content validity, the CVC. We reviewed and modified aspects of the app related to items with a CVC < 0.7 or which we deemed pertinent, even if the item had reached the desired CVC (Coluci et al., 2015; Polit & Beck, 2018). For the second evaluation round, we reduced the assessment tool to six items for which CVC was <0.7 in the first round. Experts reassessed only the screens that had undergone modifications.
Results
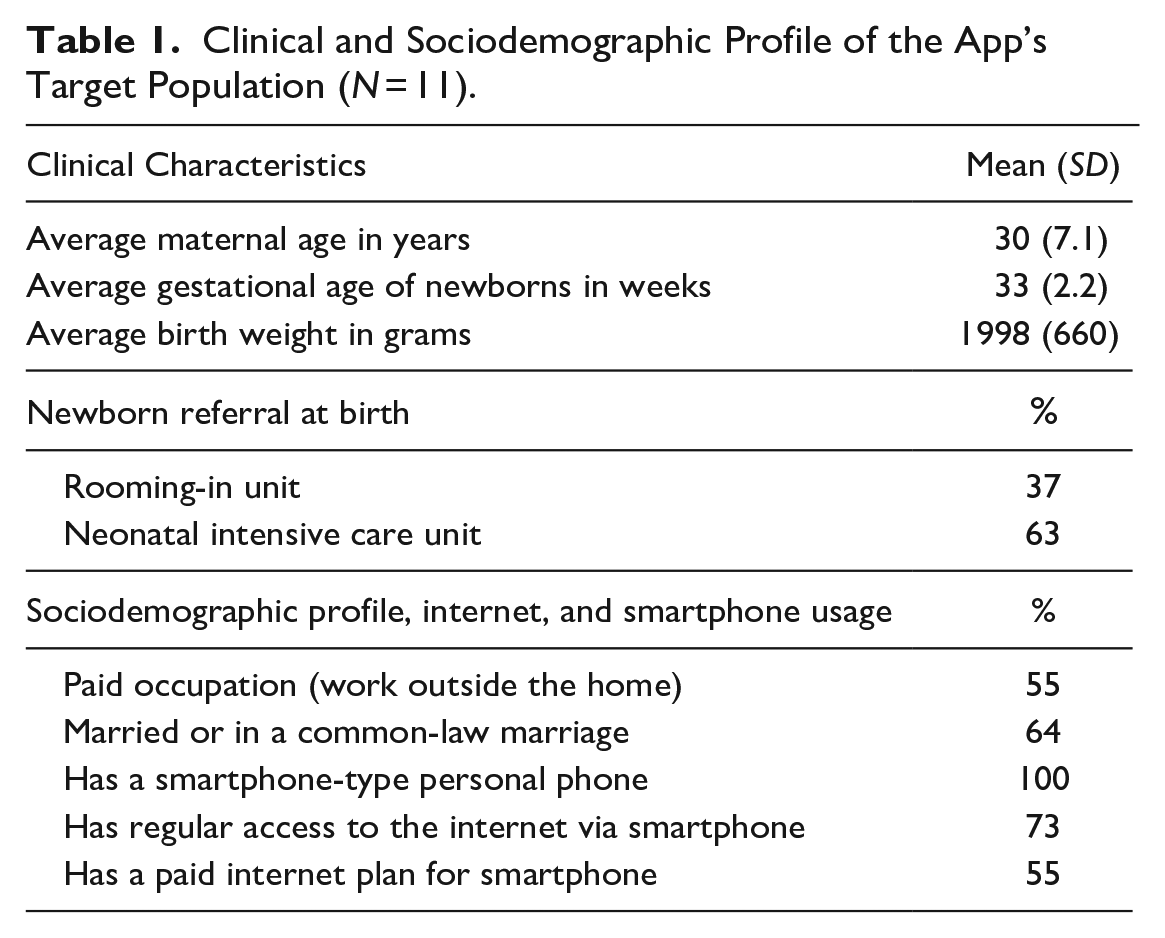
Table 1 shows the clinical and sociodemographic characteristics of participant mothers. Mothers suggested including some content in the app: “How to pump breast milk,” “Explain why it takes so long to start breastfeeding a preterm baby,” and “Talk about the NICU.”
Clinical and Sociodemographic Profile of the App’s Target Population (N = 11).

The AmamentaCoach app (“The Breastfeeding Coach” app) consists of dozens of screens with texts, infographics, videos, polls, the Mother’s Diary, music playlists, photo upload spaces, and motivational notifications, among other resources. The Mother’s Diary allows recording of the newborn’s information, pumping, peer support, the mother’s emotional states, goals, and performance reports. We conditioned the contents for users on the personal data recorded in the initial registration, including demographical and clinical questions. Thus, part of the content is exclusive to mothers of infants who stay in a rooming-in, another for mothers of infants admitted to the NICU, and a third part is common to all. Figure 1 shows some screens of the AmamentaCoach app, and Table 2 details the app’s content and features.
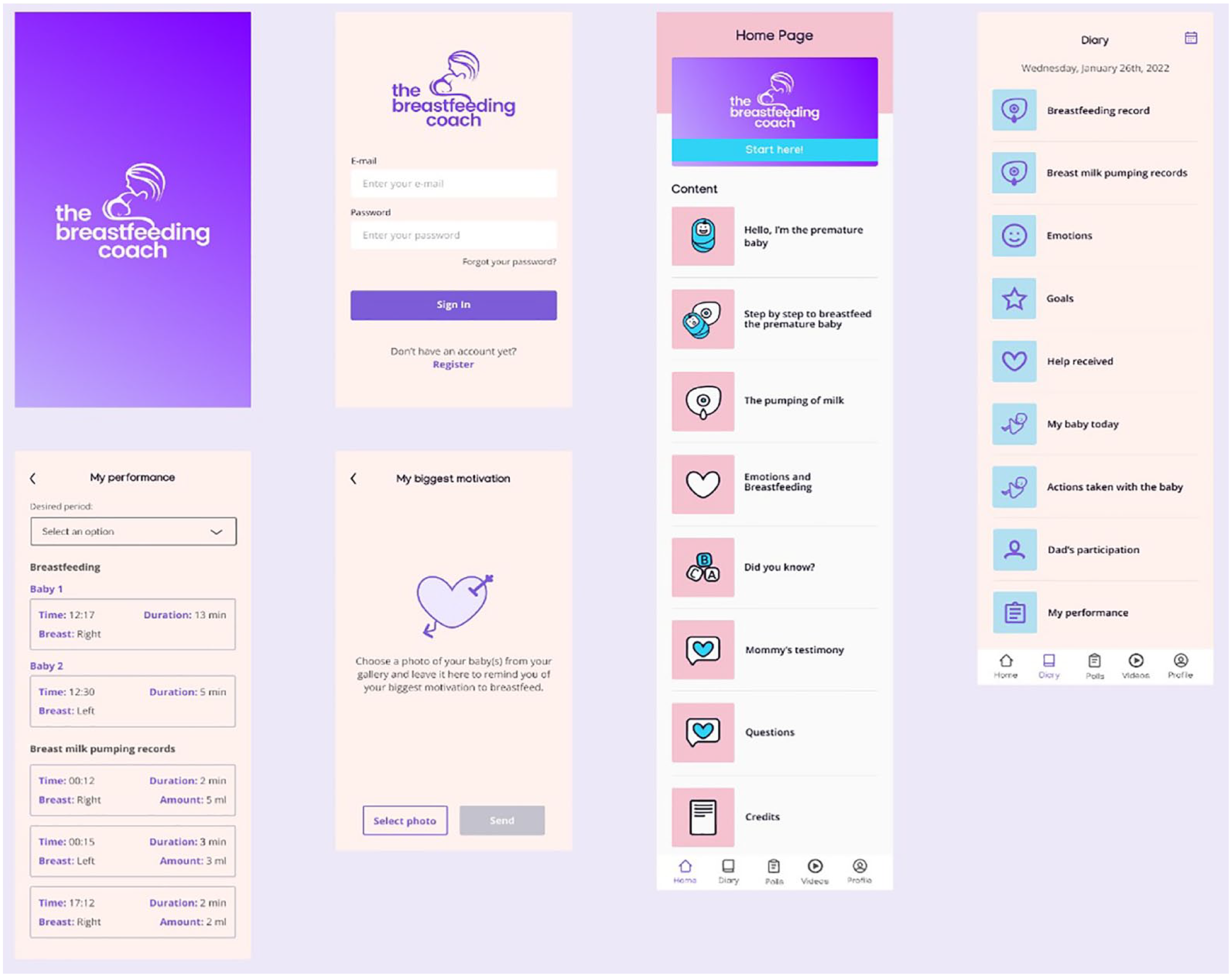
Some screens of the AmamentaCoach app.
Contents, Topics Covered, and Presentation Strategies Adopted in the AmamentaCoach App.
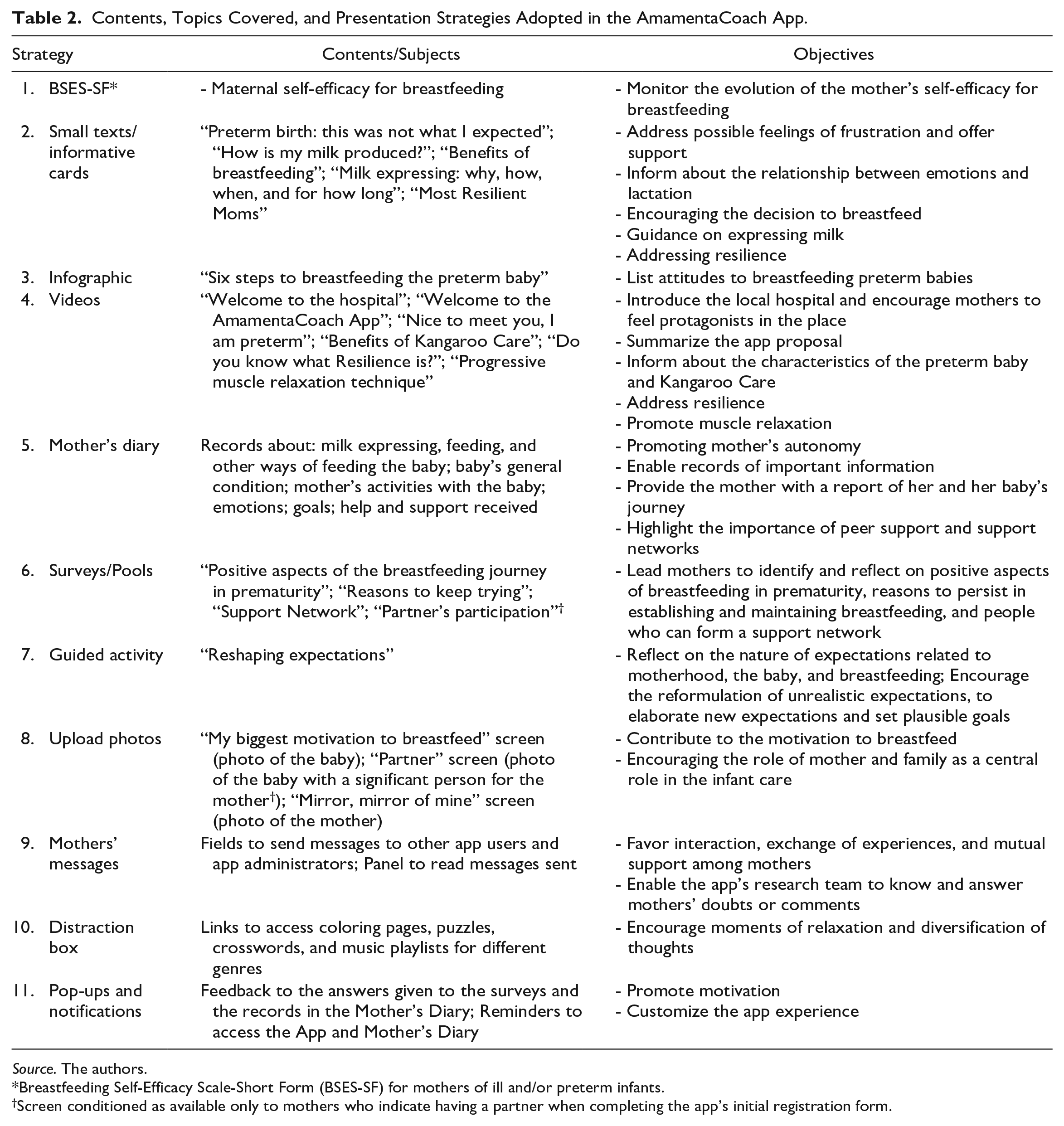
Source. The authors.
Breastfeeding Self-Efficacy Scale-Short Form (BSES-SF) for mothers of ill and/or preterm infants.
Screen conditioned as available only to mothers who indicate having a partner when completing the app’s initial registration form.
Nine of the 40 specialists invited to perform the app face and content validation accepted the invitation. Among the eight postgraduate evaluators, two were specialists, two had a master’s degree, and four had a PhD. We also included a design professional. Their average age was 42, and 70% had more than 5 years of experience.
We modified all screens with CVC-I < 0.7 in the first round and four screens with CVC-I > 0.7, but whose expert’s comments had indicated a need for improvement and returned them to the experts for a second evaluation. Table 3 shows the concordance coefficients in each domain in the first (n = 10) and second round of app evaluation (n = 9). Several experts’ notes referred to the app’s figures, indicating that they could be less abstract, more interesting, more frequent, and include women from different ethnicities. One of the experts did not understand the app logo. Three experts suggested more vibrant or cheerful colors. There were also some comments about the content. The suggestions included simplifying the language, including some breastfeeding myths content and mother’s progress reports based on the records made in the app. Our team improved the app, including proofreading, changing images, figures, and color patterns, and creating a new logo. We included a function to present the mother’s progress with the records made in the app.
Content Validity Coefficients Attributed by the Experts: First and Second Evaluation Rounds.

CVC = content validity coefficient.
In the second round, we had a reduction of experts due to the impossibility of participation of one of them in the study period.
Discussion
The Brazilian AmamentaCoach app was elaborated consistently with a scientific basis, covering content related to prematurity, breastfeeding, and motivational aspects oriented toward the mothers’ engagement. An interdisciplinary collaboration between nursing and software development professionals was necessary to make its functionalities orbit around the target population’s needs and preferences. A diverse panel of experts validated the app, indicating their level of agreement regarding the appearance, language, and content of the app, and recording suggestions for improvement. In this way, the app achieved agreement rates of over 80% in both face and content after its second evaluation round.
This initiative aligns with the recognized global expansion of electronic and internet-based health promotion strategies (Almohanna et al., 2020). It is relevant not only due to the growing preference of mothers for e-resources but also considering the pandemic’s imminence, such as COVID-19, since mhealth strategies may enable the continuity of assistance and the promotion of breastfeeding without face-to-face interactions (Silva et al., 2021). The WHO Health Technical Evidence Review Group declares that mobile technologies have the potential to serve people who do not have access to health systems (Agarwal et al., 2016).
The survey revealed that the target population widely used apps for smartphones and expressed interest in information related to breastfeeding preterm infants. Women indicated that they also wanted emotional, technical, and advisory support about breastfeeding (Demirci et al., 2016) on eHealth resources. The AmamentaCoach app seeks to cover these aspects. A systematic review with results from eight countries concluded that combining educational activities with personalized, web-based support may be the most effective way to improve long-term breastfeeding outcomes (Almohanna et al., 2020).
Also, authors from this review highlighted that only three of the 16 studies employed a theoretical framework in their breastfeeding interventions employing e-technologies (Almohanna et al., 2020). We adopted the Breastfeeding Self-Efficacy Theory (Dennis, 1999) as a theoretical framework in addition to principles in positive psychology to support motivation, resilience, and optimism aspects (Kobau et al., 2011; Seligman, 2011; Van Zyl et al., 2020).
The intricacy of the task (Dennis, 1999) of establishing and maintaining breastfeeding for a preterm infant was recognized and addressed in the AmamentaCoach app, through the video “Nice to meet you: I am the preemie” and in the infographic “Six steps to breastfeeding the preterm baby.” However, we included strategies based on positive psychology principles, such as in the polls “Positive aspects of the breastfeeding journey in prematurity” and “Reasons to keep trying” to balance the perception of the challenge represented by this task. In addition, some functionalities highlighted some of the reasons why mothers tend to strive to breastfeed their babies: “My biggest motivation to breastfeed” app screen for baby photo upload, and information cards about the benefits of breastfeeding entitled “A period of struggle, a lifetime of results,” for example.
The effort demanded to breastfeed a preterm baby strongly relates to the difficulty in maintaining lactation through pumping or expressing breast milk (Dennis, 1999). Mothers may need to pump around six times a day to maintain lactation since these babies can take days, weeks, or even months to be able to breastfeed. Covering this theme, the app offers an infographic—"Six steps to breastfeeding the preterm baby,” and information cards on milk pumping.
Content aimed at maternal relaxation can indirectly contribute to lactation. Thus, a video with instructions on the Progressive Muscle Relaxation Technique (Karbandi et al., 2017) and the “Distraction box” were included in the app. In addition, we created a “Breastfeeding diary,” which has the potential to “fractionate” one large task into various smaller and simpler tasks (Leite et al., 2016). The “Breastfeeding diary” allows the mother to record the pumping or expressing of breast milk, the time spent with the baby in the kangaroo position, and the mother’s emotional state, which are essential elements related to breastfeeding in the preterm birth context.
The amount of help required or received (Dennis, 1999) was addressed in the pool on peer support and in the fields of “Breastfeeding diary” on professional and personal support networks. It can also be raised in the mothers’ “Message Board” and even in the content that highlights the participation of partners. Peer support is essential for developing a maternal role among mothers of very low birth weight babies (<1,500 g) (Rossman et al., 2015).
Attention to successful or improved performance aspects tends to increase self-efficacy perceptions, while attention to unsuccessful aspects of performance tends to decrease it (Bandura et al., 1977; Dennis, 1999). The AmamentaCoach app was programmed to send notifications with appreciative feedback for the different types of mothers’ responses on polls and the various records made in the “Breastfeeding diary,” always emphasizing the positive aspects of the mother’s journey.
The action options to be recorded in the “Breastfeeding diary” represent a range of favorable behaviors for successful breastfeeding of preterm infants, such as pumping, engaging in skin-to-skin contact, and relying on peer support. These favorable behaviors also make up goal options that mother can select both related to actions and regarding the management of emotions and thoughts.
Strategies aimed at raising mothers’ awareness of resilience and fostering this characteristic on the app also reinforce the assumptions of the theoretical frameworks adopted in the present study. Resilience is a predictor of positive coping in stressful situations (Secades et al., 2016), which should arouse the interest and attention of supporters of breastfeeding mothers of preterm infants. The strengthening of this characteristic has been the target of interactive technology interventions (Pusey et al., 2020).
Challenges and Prospects
The conception, development, and face and content validation of the AmamentaCoach app faced many challenges. Firstly, it was forming a multidisciplinary team to design and develop the software, considering the different kinds of expertise that was required due to its complexity. Secondly, it was a challenge balancing the expectation with achievability in developing an app that was as complete as possible in terms of content, creativity, and attractiveness of features and media, in the backdrop of limited human and financial resources. Lastly, the high workload that was expected of the panel of experts and the time it took to obtain judge’s responses were other constraints.
Some limitations of the study include the development of a single version available for smartphones with the Android operating system, in addition to not allowing real-time interactions. Regarding the validation stage, the low response rate of the invited professionals did not ensure the representativeness of all regions of the country. We only submitted the app’s screenshots for evaluation, which allowed us to evaluate the appearance and content, but not the usability, an important aspect that we are investigating with users of the application in another study. In addition, clinical validation of the app is needed to understand its effects on breastfeeding and self-efficacy outcomes.
This paper can help other nurses or health professionals who want to design health solutions based on eHealth. The detailed account of the steps taken provides a broad overview of our experience with the development of the AmamentaCoach app. In planning the content of eHealth-based interventions, it is pertinent to consider both the professional experience of the creators and the current research evidence, as well as the interests and preferences of the target population. In this way, it is expected to converge different sources of information to build a product with the potential to be well accepted by patients.
Recommendations
We strongly recommend establishing multidisciplinary groups to develop health promotion apps, and consider online work meetings at no cost, especially in countries with scarce resources. It is suggested that the AmamentaCoach app be translated and made available in English, as breastfeeding premature babies represents a global challenge.
Conclusion
Nurses can apply their expertise by designing mHealth-based interventions, employing scientific evidence, and considering the interests and preferences of the target population. In this experience, the AmamentaCoach app was completed with dozens of informative screens that provide support and motivation-oriented content for mothers of preterm infants, distributed into 11 different categories of strategies. With a panel of experts validating the app for face and content, it becomes possible to glimpse the potential to impact the breastfeeding experience of mothers of premature babies positively. It will be tested for usability and effectiveness in future studies, in addition to developing an English version culturally adapted for mothers in Canada, a country whose ethnic and cultural plurality can be interesting for the app’s user experience evaluation and whose demand for resources using mHealth for mothers of premature infants has already been identified in previous research.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Conselho Nacional de Desenvolvimento Científico e Tecnológico (CNPq), Call: CNPq/MCTI/FNDCT No. 18/2021—Range B—Consolidated Groups, process 421873/2021-3; and by CAPES Social Demand Program scholarship, process 88887.598013/2021-00.
Ethics Approval
Research Ethics Committee (opinion 3.852.898, Certificate of Presentation of Ethical Appreciation 27703419.8.0000.5231).
