Abstract
Patient care needs in ambulatory care (AC) settings continue to grow and evolve in the United States, with commensurate growth of nursing responsibilities in AC. Conducting research on the nursing workforce and nursing practice is essential to understanding and meeting the needs of nurses and patients in this setting. However, the structures and characteristics of AC settings pose challenges for conducting research on AC nursing practice. This article explains unique barriers to participation in research for nurses in AC, describes recruitment challenges for nurse researchers in AC, and provides strategies to increase recruitment of nurses for AC research. Researchers in AC must find ways to recruit representative participant samples, be clear and precise in defining terms, and report robust demographic information about participants and their practice settings.
Background
Aging populations and the growing prevalence of multiple chronic conditions are contributing to higher demands on healthcare systems around the world. Additionally, increasing global attention placed on addressing determinants of health (including social, economic, and environmental factors) highlight the need to focus on non-hospital settings (World Health Organization and the United Nations Children’s Fund, 2018). In the United States, these aspects of the population are not the only critical influences on the country’s healthcare needs. In 2010, the enactment of the Affordable Care Act (ACA) began a movement toward payment models that focus on prevention (Shrank et al., 2021), care shifting to outpatient or community-based settings (Peikes et al., 2020), and expanded access to health insurance coverage (Shrank et al., 2021). As a result, American healthcare systems are experiencing increased growth in patient care visits and services in ambulatory care (AC) settings. AC refers to care provided in outpatient settings such as medical offices, hospital outpatient clinics, ambulatory surgery centers, and dialysis centers (Agency for Healthcare, Research and Quality, 2018).
As healthcare continues to evolve in AC, so does the work of healthcare teams, including Registered Nurses (RNs). Research to further understand what makes high functioning AC teams and ensure the highest quality of patient care is necessary. Nursing responsibilities in AC settings are shifting and RNs are moving into new domains where they are increasingly practicing to the top of their licensure, such as providing wellness and preventive care once considered the domain of providers (Bauer & Bodenheimer, 2017). Additionally, exploration of AC nurses’ role identity has highlighted that the functions of their role and their partnership and collaboration with other team members and patients result in an identity and practice distinct from other nursing roles (Brzozowski et al., 2023; Ashley et al., 2018).
RNs in AC have a distinct work environment and practice, highlighting the need for the advancement of knowledge in this nursing population to support patient outcomes. For example, individual and work setting characteristics such as education, experience, location of clinic, and behaviors of supervisors influence nurses’ perceptions of environmental factors including in AC settings (Brzozowski et al., 2022; Olu-Abiodun & Abiodun, 2017; Specchia et al., 2021). Likewise, AC settings have physical structures, staffing approaches, patient care models, and logistical characteristics different from other healthcare settings that influence nursing practice and ultimately, patient care (Fritz et al., 2022). Given the specialized work environment, practice, and identity of AC nurses, it is essential that further research is conducted to better understand the needs of AC nurses, and empower them to meet the expanding needs of their patients.
Furthermore, quantitatively testing validated tools and nursing workforce models drawn from hospital settings in AC has highlighted variability between settings (Brzozowski et al., 2022). This variability indicates it may not be feasible or appropriate to directly translate or apply research from one setting to another. Additional research and testing of validated instruments and models within AC settings is necessary to create resources that match the unique needs of nurses and patients in AC. However, given the structures and characteristics of this setting, conducting research with AC nurses poses challenges.
The authors have conducted research studies spanning a range of designs (i.e., interviews, surveys), samples (local to nationwide), and methodologies (qualitative, quantitative, and mixed methods). Through this work, we have experienced unique challenges related to recruitment of nurses in the AC setting. This article is intended to share what we have learned and highlight opportunities for other researchers conducting studies involving nurses in AC.
Purpose
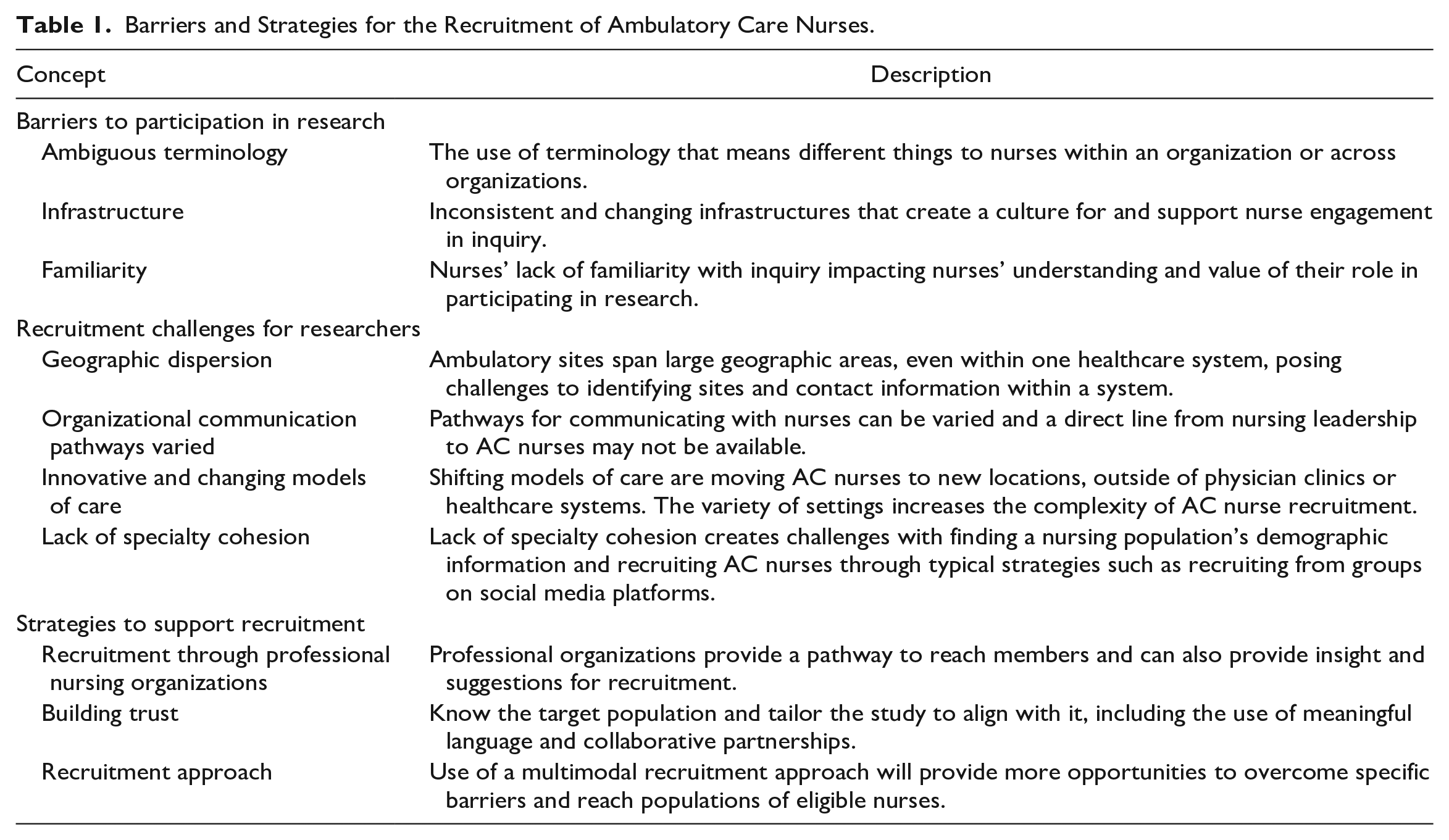
The purpose of this article is to describe barriers to participation in research for RNs in AC, describe recruitment challenges for nurse researchers in AC, and provide strategies to increase recruitment of nurses for AC research. Table 1 provides an overview of these concepts.
Barriers and Strategies for the Recruitment of Ambulatory Care Nurses.
Barriers to Participation in Research
RNs in AC may encounter several barriers to participating in research studies. These barriers include uncertainty about eligibility related to ambiguous terminology, a lack of familiarity with research, and a lack of infrastructure supporting nurse engagement in research. Barriers to participation will be discussed in this section.
Ambiguous Terminology
One challenge to recruitment and AC nurses’ participation in studies may be related to the use of ambiguous terminology, or terminology that means different things in different organizations or even within one organization. For example, in one organization, the same type of setting is referred to variously by employees as “clinic,” “office,” or “practice.” Some use “office” to refer to most primary and specialty care settings and “clinic” to refer to a subset of settings serving vulnerable populations. Others use “office” to refer to a specific department within the building (clinic). Some employees use “practice” to refer to a patient panel served by a single provider while others use it to mean either the entire department or the entire building, which may contain several departments. The ambiguity in terminology can make it difficult for potential participants to determine whether they meet eligibility criteria for a study.
Similarly, the first author noted confusion around the term “primary care” when recruiting participants. Some inpatient nurses responded to the call for primary care nurses, assuming they were eligible because they use the primary nursing care delivery model on their inpatient unit. Furthermore, AC nurses were not always certain whether their specialty practice was primary care. For example, an obstetrician-gynecologist clinic may be considered either primary care or specialty care, depending on how the organization defines the clinic. This created confusion among potential participants.
The authors have also heard the term “ambulatory care” used in hospitals to refer either to nurses who work in ambulatory surgery or the emergency department. Nurses from these hospital departments may self-select into studies recruiting “ambulatory care nurses,” even when the study is intended for nurses in outpatient clinics. Variability in how terms are understood can make it difficult to communicate inclusion and exclusion criteria effectively and concisely for AC nursing research.
Infrastructure
A second barrier to nurse participation is inconsistent and frequently changing infrastructure in AC. Start and Graystone (2021) noted that structures in AC have not traditionally promoted RN engagement in developing the science of AC nursing. Fritz et al. (2022) reported a lack of support and resources for nursing research in AC as compared with inpatient resources, even within the same healthcare system, as well as frequent fluctuations in infrastructure with acquisitions and mergers. In AC, many organizations lack structures such as library access, resources (e.g., nurse scientists), and explicit institutional support for nursing engagement in inquiry (Fritz et al., 2022). This lack of scholarly infrastructure provides challenges for facilitating a culture of nurses interested in participating in research. Nurses who would be interested in participating may be unaware of potential opportunities because internal organizational communication channels are unrefined. Without a research infrastructure, there may be no way for nurses to find opportunities to participate in research studies that have been presented to the organization.
Familiarity
Another potential barrier to AC nurse participation in research is a lack of familiarity with inquiry (research, evidence-based practice, and quality improvement), which may influence how nurses understand and value their role in research and evidence-based practice. Berlin et al., (2020) found AC nurses are older on average than other nursing populations, with 61% of AC nurses who responded to their survey being over 45 years old, compared with 36% of inpatient nurses. They also found AC nurses are less likely than inpatient nurses to have bachelor’s degrees or have completed a nurse residency. Without the exposure to inquiry commonly found in bachelor’s programs and new graduate nurse residencies, AC nurses may, on average, have less familiarity with research and evidence-based practice than their inpatient colleagues and, therefore, do not fully understand the underlying importance of participating or seek out opportunities to participate. Despite these barriers, the literature indicates AC nurses want to participate in moving science forward in their specialty (Brzozowski et al., 2023).
Recruitment Challenges for Researchers
Researchers may encounter challenges in recruiting AC nurses. These include the geographic dispersion of nurses, barriers related to organizational structure and culture, new or changing models of care, and difficulty in reaching nurses who fit inclusion criteria. These challenges will be explored in this section.
Geographic Dispersion
One common challenge to recruiting participants for research in AC is the geographic dispersion of potential participants across healthcare organizations. Even within a single healthcare system, AC sites can be numerous and span a wide area. It may be difficult to find contact information for each site. Fritz et al. (2022) noted this in their study on nursing professional development (NPD) in AC, in which NPD practitioners reported serving as many as 80 sites across multiple states. Several participants in this study reported frequent involvement in acquisitions and mergers. As AC sites are acquired by healthcare systems, it can be difficult to find and maintain accurate lists of sites and contact information within a system. This generates challenges for researchers seeking to recruit participants across sites.
Organizational Communication Pathways Varied
Pathways for communicating research opportunities can be varied and do not always involve a direct line from nursing leadership to AC staff nurses. Start and Graystone (2021) identified a need to help connect nurses from AC to opportunities for engagement in research efforts and noted reporting structures in AC can vary in ways that make it difficult to implement Magnet®-related processes like research. For example, a healthcare system may not have a distribution list that includes all AC RNs. Rather, distribution of a message must go through leaders who forward to staff, resulting in gaps in communication. The authors encountered these challenges in recruitment for their studies. They worked through leaders or attended meetings with sub-populations of the eligible nursing workforce to share the research study. It was often unclear how many eligible nurses actually received information about the study and the opportunity to participate. The lack of straightforward communication pathways for nurses in AC contributes to challenges in reaching the target population.
Innovative and Changing Models of Care
As recognized in the Future of Nursing 2020–2030 report, patient care models, delivery locations, and technology are all changing, which impacts how nurses care for patients in AC settings (Bauer & Bodenheimer, 2017; National Academies of Sciences, Engineering, and Medicine, 2021). AC nurses are not just caring for patients in physician clinics or healthcare systems. Innovative models of healthcare delivery are emerging. Walmart Health and Amazon have recently made significant moves into the healthcare industry through the establishment of retail medical clinics (Phares et al., 2021). Occupational health is projected to have a compounded annual growth rate of 3.8% from 2022 to 2027 (United States Occupational Health Market, n.d.), payers (e.g., insurance companies) and private equity are expected to continue acquiring AC services (Landi, 2022), and school-based healthcare centers continue to grow (Love et al., 2018). These shifting models of care increase the complexity of AC recruitment. Researchers must consider eligibility criteria carefully and recognize potentially eligible nurses may work in a variety of organizations and industries beyond traditional outpatient clinics.
Lack of Specialty Cohesion
Patient care around the world has occurred in non-hospital settings for decades (D’Antonio & Buhler-Wilkerson, 2022). In the United States, the ACA put new focus on this practice setting and the role of AC nurses (Cleveland et al., 2019). However, the lack of available demographic data about nurses in AC makes it difficult for researchers to know when they have succeeded in recruiting a sample representative of the larger population. For example, because demographic data about the larger specialty population was unknown, the second author was unable to determine whether a lack of racial and gender diversity in her dissertation research was representative of the broader population or indicated a need for additional recruitment efforts. Additionally, a shared identity of and within AC nursing is not as advanced as in other healthcare settings (Ashley et al., 2018; Brzozowski et al., 2023).
The lack of a shared unified identity contributes to challenges in recruitment, especially in the use of social media recruitment approaches. Although social media can be an effective recruitment strategy for targeted audiences and to support snowball sampling (Siegmund, 2018), it can pose challenges with obtaining a sufficient number of participants (Bethel et al., 2021). This challenge was a significant limitation of recruitment in the authors’ studies, as some populations of AC nurses, for example primary care RNs, do not have a strong social media presence in aligned Facebook groups or Twitter hashtags. Reaching this population of nurses using social media required the researchers to explore indirect approaches, such as working through Facebook groups intended for primary care Nurse Practitioners (NPs), or primary care physicians in hopes that members of the group (e.g., NPs or physicians) would share messages with eligible RN colleagues.
Strategies to Support Recruitment
This section includes strategies researchers may use to facilitate recruitment of study participants in AC. Strategies include recruitment through professional organizations, building trust with the AC nursing community, and adapting recruitment methods. Specific ways to engage these strategies are presented in the following paragraphs.
Recruitment Through Professional Nursing Organizations
Recruitment through professional organizations such as specialty practice organizations like the American Academy of Ambulatory Care Nursing, state boards of nursing, or existing research networks is a common strategy to reach nurses in AC. Leaders and members of the organization may have suggestions for recruiting the target population. Additionally, professional organizations may be leveraged to communicate study information to their members.
Although both authors have recruited participants through professional organizations, they found this strategy to be limited. Most professional organizations publish little demographic information about their members, which makes it difficult to determine exactly who will be reached using their distribution lists. For example, the geographic location of members, the patient populations they serve (e.g., primary care, specialty care, ambulatory surgery), and other demographic characteristics (e.g., age, gender, race/ethnicity) were not readily available. Additionally, it is common for these groups to charge a fee for use of their member lists. Researchers must weigh the potential value of recruiting through professional organizations with the resources needed to access these groups and the unknowns associated with the lack of demographic information and other characteristics of members. Further, the authors have observed many engaged members of professional organizations are in positions other than direct care (e.g., leaders or educators). Therefore, recruiting direct care nurses through professional organizations often depends on those who are members to see the recruitment notice and share it with others who may meet the inclusion criteria. Regardless of these challenges, professional nursing organizations remain a valuable component of the overall recruitment strategy for research on AC nursing.
Building Trust
Another strategy to improve recruitment in AC research is to build trust with the target population. This can be done through means such as tailoring the language on instruments and recruitment materials to the target population. For example, the first author replaced all references to “hospital” with “clinic” in a survey instrument and recruited subject matter experts to review the instrument for other language that might unintentionally communicate to participants that the study was not meaningful for AC (Brzozowski, 2020). The authors recommend pilot testing recruitment materials with members of the target population to identify avoidable misunderstandings. By adapting recruitment materials and instruments to match the language of AC settings, researchers may signal their trustworthiness as partners in scholarly endeavors in AC.
Collaborative partnerships with patients, community advisors, and nursing leaders can help build trust and rapport between researchers and the AC nursing community. Community advisors provide valuable insight on research design and strategies. In research related to AC, patient representatives and practice leaders may function as community advisors and offer feedback on the research needs of AC nurses and patient populations. Practice leaders may also facilitate connections with potential participants.
Recruitment Approach
Given the complexities associated with recruitment of AC nurses, the authors recommend a multimodal approach to overcome known barriers and challenges. Creativity may be needed to identify groups or channels that will reach specific populations of eligible nurses, whether directly or through a mediator. For example, researchers could work with healthcare systems and professional organizations to disseminate information about the study to their nurses while also leveraging social media. Although there are limitations to using social media to recruit AC nurses as noted above, social media platforms can provide the opportunity to quickly reach large numbers of individuals, including underrepresented populations (Bethel et al., 2021). Additionally, researchers should be aware of how to overcome other potential limitations of social media. Responses may be from bots, therefore closed groups are recommended and careful screening of data is necessary (Bethel et al., 2021). Researchers should also understand the ethical implications of social media recruitment (Bethel et al., 2021; Kamp et al., 2019).
The sampling approach is another area of opportunity researchers should consider when designing a study where AC nurses will be participants. For example, snowball sampling permits AC nurses to use their networks to further disseminate the study. In conjunction with social media recruitment strategies, snowball sampling has been shown to be effective in reaching specific populations (Siegmund, 2018). Raifman et al. (2022) suggest additional sampling approaches for hard-to-reach populations, including time-location sampling or respondent-driven sampling.
Another strategy to improve the quality of recruitment, particularly in qualitative studies, is to employ an additional layer of screening. Roehl and Harland (2022) recommend adding telephonic screening with potential interviewees who appear to meet inclusion criteria based on their responses to an initial online screening form. Both authors used a layered approach to screening. The first author conducted a second layer of screening through email communications after potential participants indicated interest through an online screening form. The second author implemented additional screening for a study after two interviewees who self-identified as having specific experiences on an online screening form divulged during interviews they did not have the required experience to participate in the study. Additional screening procedures may help identify ineligible participants before unusable data is collected.
Discussion
The lack of a shared understanding of common terms used in AC poses a serious barrier to recruitment for AC nursing research. In their article on the value of shared mental models in developing healthcare policy, Evans et al. (2019) described the importance of clear communication for creating a common understanding among stakeholders. To advance the science underlying patient care in AC, AC nurses and nurse scientists should advocate for clear, consistent operational and conceptual definitions of terms like “ambulatory care,” “primary care,” “clinic,” and “practice.”
The lack of published demographic data about nurses in AC settings creates challenges for researchers seeking to recruit representative samples. Researchers can facilitate improvements in AC nursing research by reporting robust participant demographics, such as individual and work setting characteristics. Professional organizations are encouraged to collect and report basic demographic information about their membership. As more scientists and organizations publish demographic information, relevant characteristics within specialties or subspecialties will become easier to identify and research results will become easier to interpret within the context of population norms.
Professional organizations are a key avenue for disseminating research opportunities and advancing science in their area of focus. They also build strong identities and networking opportunities among members. Professional organizations should recognize the need to advance AC nursing research and build structures and processes to support research in this area. Professional organizations that represent and draw nurses from different settings should create communities focused on AC to allow space for AC members to come together.
AC settings are composed of strong interprofessional teams. In AC research, nurses as well as non-nurses are doing research on patient care and nursing practice. For example, the Agency for Healthcare Research and Quality funded grants from 2000 to 2005 to drive the development of Primary Care Practice-Based Research Networks (PBRNs) resulting in over 150 PBRNs representing all 50 states (Agency for Healthcare Research and Quality, 2018b). Many PBRNs are still in existence today and often have a strong physician-centric approach to their work (Agency for Healthcare Research and Quality, 2018b). Although these networks are not necessarily nursing-focused, their work provides a strong network for researchers and advances the science in AC, which influences nursing practice and patient care in AC. Nurse researchers must leverage existing structures like these, while concurrently developing stronger research identities and research networks for nursing scholarship in AC.
Conclusion
As AC needs continue to evolve, additional nursing research will be needed on issues pertaining to AC patient needs and nursing practice. It is vital that researchers in AC find ways to recruit representative participant samples for this research and prevent contamination of research findings from participants who do not meet inclusion criteria. Researchers are encouraged to be clear and precise in defining terms, consider using enhanced screening techniques to ensure only participants who meet criteria are included in studies, and report robust demographic information about participants and their practice settings. Nursing must advance research in AC by developing a strong research identity, research presence, research network, and research infrastructure in the setting.
Footnotes
Acknowledgements
The authors would like to thank the ambulatory care nurses who participated in their doctoral research studies.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
