Abstract
Doctors are the first to fight COVID-19 and their mental health is at risk. This article aimed to investigate the psychological experiences of physicians recovered from COVID-19 disease. Phenomenological method was carried out to analyze the obtained data. Participants were 16 physicians recovered from COVID-19 disease in Yazd City from January 20th to March 1st, 2020. Samples were selected via purposive sampling and the subjects participated in-depth semi-structured interviews. Twelve main themes and 48 sub-themes were extracted, including 1- Adaptive emotional reactions, 2- Adaptive cognitive reactions, 3- Adaptive behavioral reactions, 4- Adaptive communicative reactions, 5- Adaptive spiritual reactions, 6- Adaptive copings, 7- Maladaptive Emotional reactions, 8- Maladaptive Cognitive reactions, 9- Maladaptive Behavioral reactions, 10- Maladaptive Communicative reactions, 11- Maladaptive spiritual reactions, and 12- Maladaptive Copings. According to the findings, adaptive psychological reactions and maladaptive psychological reactions can affect the psychological well-being of physicians.
Background
The COVID-19 crisis has been able to change the living conditions and social behaviors in this relatively short period of time and create new concerns in today's society, so it requires careful deliberation and measurement (Dong & Bouey, 2020). In Iran, by the end of December, the total number of patients with Covid-19 disease was 6,170,979. Also in Iran, the medical staff has gone through 5 waves of corona pandemics so far. During the Coronavirus epidemic, the individual, family, and social structures of lives are disrupted. Disruption of individual structures means reduction in individual control power and the predictability of life flow (Rubin & Wessely, 2020). Research showed that behavioral, cognitive, and emotional responses in the Coronavirus hypertensive conditions depend on psychological readiness and obtained social support (Malta et al., 2020).
Also in Iran, the study showed that getting a new and unknown disease of COVID-19 in addition to physical health risks, leads to difficult and different psychological experiences due to the nature and specific characteristics of the disease (Rahmatinejad et al., 2020). The health sector as the driving force of public health, due to the nature of activities related to its role in the treatment and rehabilitation of disease and control of the health situation of the community, is a vital and strategic sector in dealing with the crisis induced by Corona (Peters et al., 2020).
The confrontation of the medical staff with a wave of Corona-related referrals is important and needs to be investigated due to health risks and occupational exhaustion. Despite health considerations while dealing with patients, physicians and nurses are infected in hospital settings and other dangerous social environments, and frequent exposure to the virus prepares them to get infected with the disease (Ghinai et al., 2020). Findings of a study show that the infection rate of medical care staff is equal to 3.8% during the outbreak of the COVID-19 (Wu & McGoogan, 2020). It is natural that the effects of (Kang et al., 2020). In a cross-sectional study on medical staff in China during the outbreak of COVID-19, the results show that the staff who are in direct contact with patients infected with COVID-19 have a higher anxiety index than those who are not in direct contact with these patients (Liu et al., 2020a) and also physicians at the risk of the COVID-19 virus are experiencing minor mental health (Kang et al., 2020). Also, in relation to the medical community, research conducted in Iran showed that on the one hand, this group was involved in emotion regulation and on the other hand, they were affected by negative emotions such as anxiety (Bahonar et al., 2020). Therefore, the health system must deal with the complications of this disease in a multidimensional and purposeful way. Thus, the empowerment of health workers as one of the main functions of management and supervision of the health system has a significant contribution to dealing with this disease (Meskarpour-Amiri et al., 2020). Some studies show that patients have various psychological reactions in addition to physical symptoms which can act as an obstacle in the process of recovering from a disease and increase their suffering during the disease. Thus, apart from their performance, their reactions, and the extent and the manner of controlling reactions are important (Willgoss et al., 2012).
On the other hand, since most studies in this area are quantitative studies and the contribution of qualitative research as the way which conveys the lived and immediate experience of individuals from a particular situation is fewer, we were determined to obtain a more accurate understanding of the lived experiences of the recovered people from this disease by using a qualitative research. Overall, it appears that doing research is essential to help identify the provoked psychological reactions and can help to explore ways to develop effective interventions in improving the psychological situation and the quality of the medical staffs’ life, especially physicians and community health.
Because qualitative research is a way to discover the lived and deep experiences of people from a particular situation, we were determined to obtain a more accurate understanding of the lived experiences of the recovered people from this disease by using a qualitative research. Overall, it appears that doing research is essential to help identify the provoked psychological reactions and can help to explore ways to develop effective interventions in improving the psychological situation and the quality of the medical staffs’ life, especially physicians and community health.
Methods
Participants
Participants were recruited via massage invitations on WhatsApp. Considering the research objective, a sample of physicians recovered from COVID-19 disease in Yazd City from January 20th to March 1st, 2020. Participants were recruited through purposive sampling. Sixteen physicians who recovered from COVID-19 were selected as the sample. Inclusion criteria were as follows: (1) tendency and consent to participate in the study; (2) being a physician; (3) being based in Yazd; (4) lack of previous cases of severe mental or physical diseases; (5) experience of working at hospital at least for one year, and (6) experience of being infected with COVID-19. The exclusion criteria were the inability to conduct during the study period. All participants provided informed consent. This research lacks a code of ethics because it was conducted during the outbreak of the coronavirus and many training centers and sessions were not held. However, as described in the method, written informed consent was obtained from the participants and all ethical principles were observed.
Data Gathering
In individual interviews, which is a common method to collect data in qualitative studies, viewpoints, incentives, and experiences of participants are explored. Thirty to forty-minute in- depth semi-structured interviews were held through telephone due to epidemic conditions. After introducing themselves and expressing their intentions, the interviewer asked the interviewees to record their talks. The interview started with this open-ended question: “What was your personal experience recovered from COVID-19 disease?”
With respect to the expressions made by interviewees, deepening and developing questions were asked. They were then asked: “What feelings, thoughts and behaviors did you have during the disease?
Analysis of Data
Colaizzi's phenomenological method was used in the current study to qualitatively analyze the psychological experience of physicians recovered from COVID-19. First, all the collected data was read to obtain a degree of immersion and sense of the whole. The data was read accurately to extract codes by spotlighting the text's exact words, which seemed to stand for pivotal concepts and views. Analysis proceeded by coding interviewees’ expressions and classifying them by two skilled psychiatrists, who were supposed to read them a couple of times to categorize codes, themes, and categories. After 16 interviews, data saturation was reached, and no new code was added.
Validation
To evaluate the validity and accuracy of the research data, four judgment criteria including validity, transferability, reliability and verification proposed by (Guba & Lincoln, 1994) were used. To ensure reliability, there was constant involvement with the subject and research data. The expertize poll was used in connection with the interview process and associated analysis. Expertize poll was also used to check the validity of the data and the transcripts of the interviews were provided to the experts for a more detailed review of the coding. To achieve the principle of transferability, physicians at different occupational, social and cultural levels were used. In addition, in order to ensure verification, researchers tried not to interfere with their judgments and biases as much as possible, and by recording all stages of work and the resulting data and preserving documents in all stages of research to ensure the validity of this research.
Results
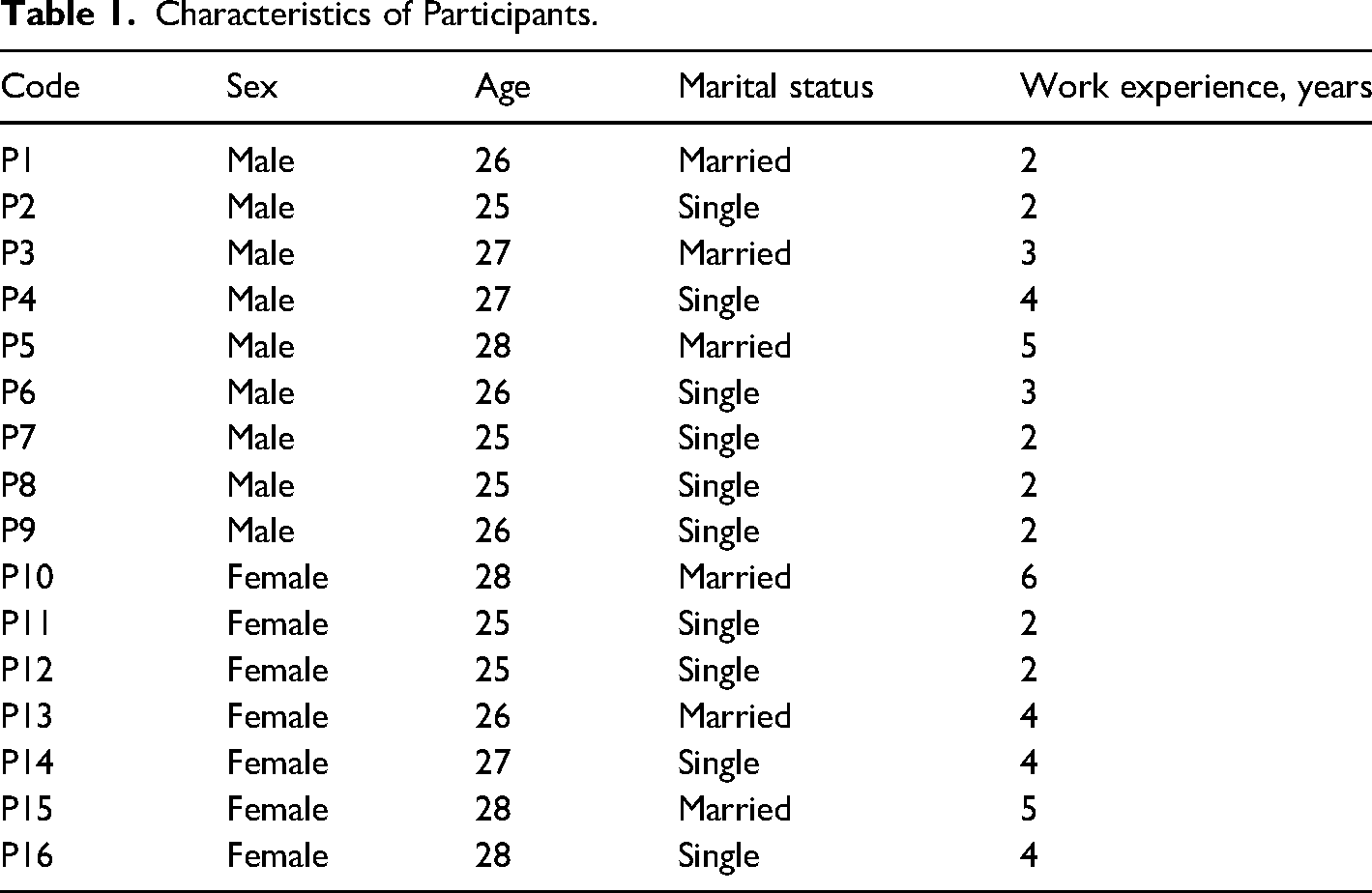
Table 1 shows the demographic information of the participants.
Characteristics of Participants.
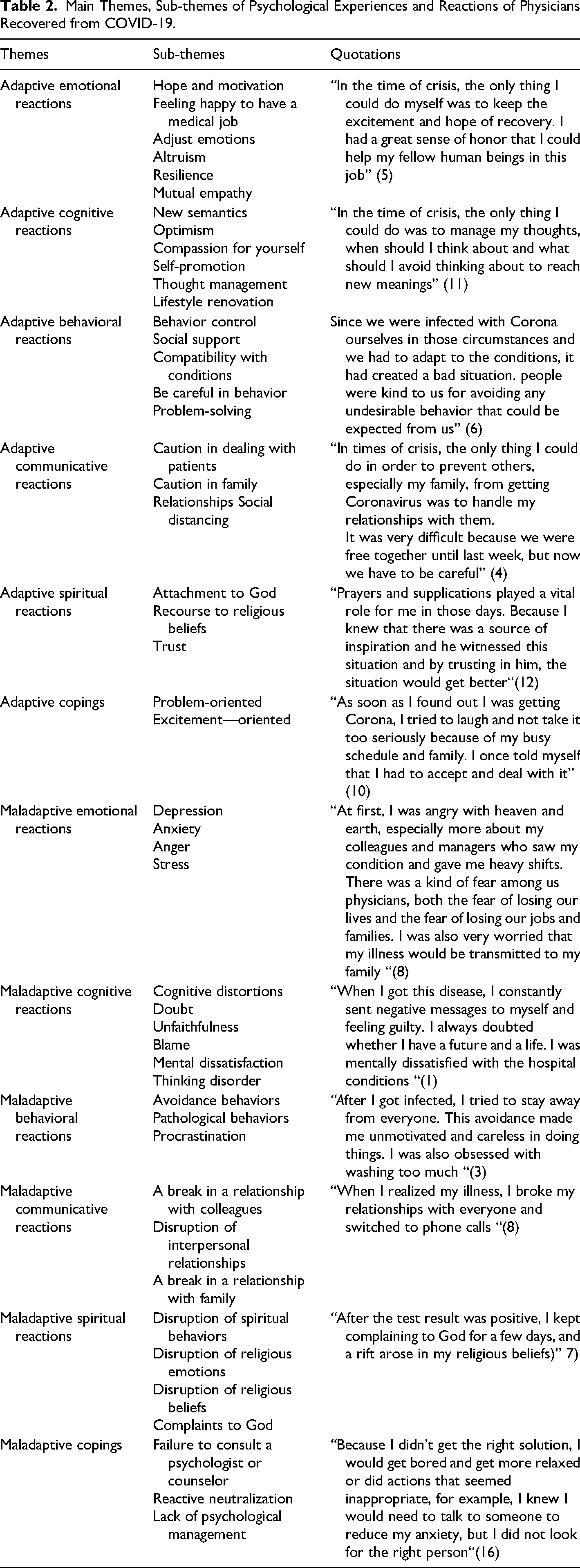
As can be seen in Table 2, data analysis resulted in the production of 12 main themes, 48 sub- themes.
Main Themes, Sub-themes of Psychological Experiences and Reactions of Physicians Recovered from COVID-19.
Discussion
Data analysis led to the identification of 12 main themes, 48 sub-themes. 12 main themes consist of 1- Adaptive emotional reactions, 2- Adaptive cognitive reactions, 3- Adaptive behavioral reactions, 4- Adaptive communicative reactions, 5- Adaptive spiritual reactions, 6- Adaptive copings, 7- Maladaptive Emotional reactions, 8- Maladaptive Cognitive reactions, 9- Maladaptive Behavioral reactions, 10- Maladaptive Communicative reactions, 11- Maladaptive spiritual reactions, and 12- Maladaptive Copings. In these circumstances, maintaining the mental health status of individuals is essential because people in different parts of society may experience stressful stimuli during the spread of COVID-19 (Shahyad & Mohammadi, 2020).
Considering the fact that nurses and physicians are working in environments where the death and life and the health of patients are paramount, their well-being and hope can help them with the health of themselves and their patients (Zadhasan et al., 2017). In the field of emotion regulation and resilience, (Gross, 2001) defined emotion regulation as the application of conscious and unconscious strategies to reduce, maintain, or increase positive or negative feelings. Emotion regulation plays an important role in the adaptation of physicians and nurses to stressful life events (Sun et al., 2020). In this study, some physicians infected with COVID-19 were trying to strengthen hope, empathy and resilience so that they could continue their personal and professional life more hopefully and happily.
According to the conducted studies, the cognitive responses of people infected with Coronavirus 2019 depend on the degree of psychological readiness and personal growth of each individual (Jiang et al., 2020). Also researchers concluded that in an outbreak of the COVID-19 crisis, those who had cognitive regulation and mastery over their own thoughts were capable of coping and better management of the disease (Chen et al., 2020). In Iran, research as “The Changes of Attitudes, Beliefs and Values at Individual and Cultural Levels and the COVID-19 pandemic” concluded that the formation of new attitudes and beliefs is expected in the Corona circumstances and thereafter (Farahani, 2020). Considering that the participants had a high level of education and highly educated people have relatively good cognitive abilities, the formation of reactions based on cognitive ability is expected.
The behavior control, social support, adaptation to the situation, caution in behavior, and problem-solving were among the thematic components of the adaptive behavioral reaction. Supportive behaviors are behaviors in which a person as being in a position of power uses the opinions of others while minimizing the use of pressure and command, and by considering their feelings, provides appropriate information and selection opportunities for them (Mageau & Vallerand, 2003). In line with this concept, (Bandura, 1977) in behaviorism theory has put behavior control and adaptation in the form of social cognitive theory and defined the regulation of environmental attractions, the creation of cognitive support and the production of results for their actions and controlling on behavior. The control and caution strategies help to construct workplace environment and enhance employee's self-motivation and facilitate the behaviors that satisfy the fulfillment of performance standards (Hart, 1995). Physicians are also key agents of the health system and require competencies beyond clinical skills, including self-management (Nicol, 2012). In the study by (Liu et al., 2020b), they examined the experiences of nurses and physicians in the fight against COVID-19 disease and they came to the conclusion that self-management is a way to cope with the condition of Coronavirus condition which one can transcend from this experience. In a study examined the experiences of nurses and physicians in the fight against COVID-19 disease and they came to the conclusion that self-management is a way to cope with the condition of Coronavirus condition which one can transcend from this experience (Liu et al., 2020b).
Among the adaptive and effective psychological responses of recovered physicians with COVID-19 was “Relations Management.” Researches have described in their research one of the reactions of the Iranian health system to deal with the Corona pandemic as relations management (Afrashteh et al., 2020; Meskarpour-Amiri et al., 2020). They also represented that the policy of successful countries in managing the Corona epidemic has been focused on reducing contact and increasing physical distance between individuals. These cases were also emphasized in the physicians’ reports. In this study, participants made decisions from the experience of this event such as physical distance, caution in relation to patients, and maintaining communication with family.
In the realm of adaptive psychological reactions, one can mention the spiritual dimension with the sub-categories of attachment to God, reliance on religious beliefs and trust. Religion causes the mental health of the individual and the society through various mechanisms. (Ano & Vasconcelles, 2005) confirmed the finding that religious coping strategies and devotion to God act as a protective and adaptive function for the individual against traumatic events. Some participants had a stronger attachment and connection to God. They were seeking attachment to God with an effort to approach to God. Some of them comforted themselves by praying and some by praying and reciting the Qur’an. Many believers consider God as a safe haven to which they turn in the time of stress and various threats to calm down; they also consider God as a safe base that provides them with courage and audacity to cope with problems (Ghobari & Haddadi Koohsar, 2011).
Among the other adaptive reactions that physicians infected with COVID-19 showed, were effective confrontations. Coping strategies are a continuous effort to adapt people to an unbalanced state. In emotion-based coping, the emotions are adjusted and the stress is removed (Dyrbye et al., 2005). This coping strategy, if used effectively, can enable management of internal and environmental stressors, and feelings of wellbeing and mental adaptation with the stressful situation are resulted (Barry & Farmer, 2020). (Rubin & Wessely, 2020) stated in their research that the disturbance of individual structures means a decrease in individual control power and in life flow expectancy occurring during the disease. Along with the occurrence of these items, the necessity of using coping strategies is more likely to be experienced especially for the medical staff due to the exposure to patients and more work pressure. In the following, a problem-oriented coping strategy involves the constructive actions of the individual in relation to stressful situations, and tries to eliminate or change the stressor. This confrontation can be directed either inward or outward (Gunnell, 2000). The researchers stated that coping skills, especially problem- oriented ones are an important factor in maintaining the mental health of individuals in stressful conditions of COVID-19 and if they fail to use coping strategies, they will face many problems in the field of mental health (Shigemura et al., 2020).
Among the psychological reactions, there were maladaptive emotional reactions such as anger, anxiety, depression, and guilt. Medical students and physicians with certain problems such as the large volume of practical activities, variety and breadth of content, severe and frequent stress due to dealing with critically ill patients, observation of deficiencies in hospital wards and its effects on the patient are more prone to despair, stress, and isolation (Eisenberg & Chung, 2012). Studies have shown that the incidence of respiratory diseases, including COVID-19, will cause anxiety and depression due to serious physical problems and reduced quality of patients’ life (Wu & McGoogan, 2020). According to the research by (To et al., 2020), anxiety can cause people to fail to recognize right and wrong information, weaken the immune system and create many physical problems including in individuals’ eating and sleeping. In the workplace of nurses and physicians, they experience long-lasting stress and immerse themselves in the problems of others (Liu et al., 2020a). Anger was reported as one of the most negative reactions of the recovered physicians. Not only does Coronavirus pandemic provide a risk of dying from infection to the virus, but also the psychological pressure causes anger and rage in individuals (Duan & Zhu, 2020). Gentili et al. (2020) showed in their research that reducing anger in these situations is especially useful for medical staff during a crisis.
According to the findings of the present study, one of the maladaptive reactions of recovered physicians from COVID-19 was cognitive reactions. A study has shown that many health care providers used cognitive distortions and defense mechanisms after their test result was positive and the infection was confirmed (Li et al., 2015). Therefore, the high level of anxiety in this group can activate cognitive distortions. On the other hand, doubt is a natural part of all the experiences of the disease and can be seen during the diagnosis, treatment and prognosis process (Mishel, 1990). According to the study suspicion of the chronic condition of COVID-19 disease, which is unpredictable and uncontrollable, leading to mental reactions in patients, including depression (18). Huang et al. (2020) also showed that coping strategies with psychological pressure on individuals infected with COVID-19 disease, physicians and nurses weaken their health and psychological well-being due to a reduction in confidence and trust, which was also reported in this study. In other studies, the epidemiological features of COVID-19 disease, including the period of the infection, the number of contacts, and the probability of transmission of the virus caused the isolation and quarantine of individuals which in turn led to the self-reprimand of individuals for nonconformity in the necessary precautions and dissatisfaction (Anderson et al., 2020), which was consistent with the findings of this study.
In this study, dysfunctional behaviors were described in the form of five domains, namely avoidant behaviors, pathological behaviors, and procrastination. The a study showed that there are higher levels of anxiety and stress among physicians due to employment in hospital and distance from the family in critical situations; for this reason, they often hide many events (Zhou et al., 2020). In the field of pathological behaviors, (Wester & Giesecke, 2019) showed that medical staff often suffer from obsessive-compulsive disorder due to being in a contaminated hospital environment and the threat of various diseases which has been multiplied by the outbreak of the Coronavirus and the requirement to comply with health protocols. This is because people may avoid situations where germs and pollutants are possible for the fear of microbial contamination and follow the obsessive methods focused on disease prevention (Lai et al., 2020). In another study on the effects of Coronavirus, it has been pointed out that Corona conditions and quarantine during this period have also caused a lot of mental damages such as the reduction of mood, apathy, and procrastination in individuals (Rubin & Wessely, 2020). Among the other issues in the field of psychological incompatibility, was the scope of communication with subdivisions of a break in a relationship with colleagues, disruption of interpersonal relationship and the severance of relationship with family. In fact, this separation of relationship can be attributed to the result of quarantine. Quarantine means separation and restriction of movement and commuting to reduce the spread of the disease and decrease the risk of infection to others (Kim, 2018). Most previous studies have been conducted on the psychological and physical effects of hospital quarantine on the medical staff, especially nurses. Since nurses and physicians are at the forefront of dealing with various crisis due to the nature of their work (Aghaei et al., 2020), they are also at the forefront in the face of Corona, and have a quarantine period due to the high probability of infection with the Corona. Cava et al. (2005) examined the experiences of individuals in quarantine, who were infected with SARS in Toronto and concluded that despite the individual differences of people, the important themes were extracted from the interviews included the feeling of insecure and uncertain about life, the feeling of isolation and coping problems dealing with psychological pressures and mental stresses.
In this study, some participants experienced feelings of frustration and helplessness or were angry with God due to the high mental pressure caused by the Corona. The spiritual maladaptive reactions to the basic concepts of the rupture of spiritual behaviors, the rupture of religious emotions, the rupture of religious beliefs and complaining about God are among the other dysfunctional categories in this field. We are witnessing a reduction in the social role of religion with the pandemic of the Coronavirus and the closure of mass rituals. One of the negative coping patterns is having anger over God, due to being afflicted with a bad accident (Khodayari Fard & Abedini, 2018).
Maladaptive coping strategies included not seeing a psychologist or counselor, reactive neutralization, and lack of psychological management. According to the theory of reciprocal behavior analysis, temporal neutralization occurs when people move towards their draft, and see the world around as consistent with their early childhood decisions. They are likely to forget their awareness of some aspects of the real situation and at the same time, it's likely to magnify some other aspects of this-time this-place problem instead of taking action to solve the problem. Thus, ignoring and neutralizing are defined as “Unconscious Denial of Information Related to Problem-Solving” (Stewart & Jones, 2000). In the a study, the experiences of nurses and physicians in combating with COVID-19 disease were examined, and it was concluded that to maintain mental health, reinforcing systems such as professional psychological support have to be used in critical interventions (Liu et al., 2020b). In this study, a number of physicians by applying neutralization couldn't make it to a counselor or psychologist as well as proper psychological management.
Strengths
The data about the psychological experiences of the participants were gathered via multiple interviews at different times. Such interviewing scheme leads to a deep understanding of the patients’ work experiences, which in turn, leads to the collection of a comprehensive and authentic dataset. In contrast with many studies about the negative experiences during the outburst of stress during COVID-19, this study revealed that positive emotions, psychological adjustment and growth under pressure may coexist with the conventional negative emotions. We also discussed the impacts of such phenomena on physicians’ mental health.
Limitation
The results of this work is affected by several limitations. First, in line with other qualitative studies, the sample size was limited. Secondly, in order to prevent the infection of the experts, the research team could not conduct focus group interviews. Therefore, data was gathered through only one channel. Thirdly, due to the short-term nature of this study, long-term experiences of the research subjects were unable to be exposed. This can be a valuable source for future researches. Finally, the work pressure and the decreased motivation of working in groups, prevented our subjects, which were employed doctors, to be fully engaged with the research.
Conclusion
In connection with the explanation of these reactions, it can be said that the outbreak of Corona virus disease has raised several discussions on how to apply medical interventions, but what is overlooked in this issue is the need to address the appropriate psychological reactions in this crisis. In the present article, an attempt was made to examine and discuss the set of critical psychological reactions of physicians in these circumstances which can be examined by psychologists, mental health professionals, and health and medical services officials.
Footnotes
Acknowledgments
We would like to express our sincere gratitude to the physicians recovered from COVID-19 disease in Yazd City, who provided the necessary facilities for research, and also the participants of the present study.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
