Abstract
Background
Although many studies explore surface electromyography (sEMG) in static postures, research on muscle activation during dynamic tasks in chronic non-specific neck pain (CNNP) is limited.
Objectives
To compare trapezius and sternocleidomastoid (SCM) activation and functional capacity during five upper limb tasks between individuals with CNNP and asymptomatic controls.
Methods
This was a cross-sectional comparative observational study. Twenty-seven individuals with CNNP and 25 asymptomatic controls completed five tasks: repetitive reaching (RRT), sustained overhead work (OW), waist-to-overhead lift (OL), fingertip dexterity (FD), and hand–forearm dexterity (HFD). sEMG recorded upper (UT), middle (MT), and lower trapezius (LT), and SCM activity. Functional capacity was assessed using selected WorkWell Systems Functional Capacity Evaluation (WWS-FCE) tasks.
Results
CNNP individuals showed greater UT activation across all tasks (p < 0.01, d = 0.78–1.67) and significant MT differences in most conditions (p < 0.01, d = 0.84–1.44). LT showed smaller but significant differences (p < 0.05, d = 0.47–0.84). SCM activity increased during OL (p < 0.01, d = 0.73–1.08) and in one RRT subtask (p = 0.011, d = 0.73). CNNP performed worse than controls in RRT (p < 0.001, d = –1.32 to −1.61), OW (p < 0.001, d = –2.17), OL (p = 0.006–<0.001, d = –0.80 to −1.26), and HFD (p < 0.001, d = –1.06 to −1.36), with no significant FD differences (p > 0.05).
Conclusion
Muscle activation profiles in chronic non-specific neck pain change with tasks, highlighting the importance of evaluating functional activities beyond static-posture assessments.
Keywords
Introduction
Although neck pain is not the most common musculoskeletal disorder, it remains a significant public health concern due to its multifactorial nature. 1 Chronic non-specific neck pain (CNNP), defined as pain persisting for at least three months without identifiable pathology, is highly prevalent. It is frequently associated with postural overload and myofascial dysfunction.2–4 Even with mild neck pain and few comorbidities, patients may nevertheless have functional restrictions 5 and reduced quality of life and work capacity, 6 highlighting the need to better understand the neuromuscular mechanisms underlying CNNP.
Postural loads, such as prolonged forward head posture, are associated with distinct biomechanical consequences; for instance, a craniovertebral angle below 50° is associated with increased pain and disability, 7 and 30° of head flexion increases cervical disc loading up to fourfold compared with a neutral posture. 8 Such loads may contribute to the development of chronic pain, which is known to affect muscle control strategies. 9 Overall, individuals with chronic neck pain demonstrate altered activation patterns in superficial cervical muscles, particularly the upper trapezius (UT) and sternocleidomastoid (SCM), which is commonly interpreted as a compensatory motor control strategy associated with impaired deep cervical muscle function. 10 Such adaptations may initially be protective but can become maladaptive over time, leading to a redistribution of muscle activity. 11 Beyond these activation changes, neuromuscular alterations are reflected in reduced upper limb strength and coordination, indicating measurable limitations in tasks requiring sustained performance. 12 Furthermore, pain has been shown to affect both fine and gross motor functions adversely, hindering essential daily activities such as writing, lifting, and reaching. 13 These functional impairments, resulting from pain-induced changes in muscle activation, reduce efficiency and significantly diminish quality of life. 14 However, most studies on cervical muscle activation have been conducted under controlled and static conditions15,16 while evidence regarding their behavior during dynamic and real-life tasks that require endurance, coordination, and postural control remains limited. 17 To meaningfully investigate neuromuscular behavior during such tasks, it is necessary to select individuals with clinically relevant neck pain who retain sufficient functional capacity to perform functionally demanding and standardized upper limb tasks. The Neck Disability Index (NDI) is a validated tool for classifying disability severity, and moderate disability (NDI 30–48%) was therefore selected to achieve this balance. 19 While foundational studies have established altered muscle activation patterns during specific tasks, 10 there is a lack of evidence regarding how these patterns vary across a broad spectrum of functional demands and how they can be interpreted alongside objective performance measures. Unlike previous studies focusing on single or highly constrained tasks, the present study simultaneously examines muscle activation and functional performance across multiple upper limb tasks with graded physical and sensorimotor demands, providing a more comprehensive and clinically relevant evaluation of task-dependent motor control alterations in CNNP.
This study aims to compare individuals with CNNP and asymptomatic controls in terms of activation of the UT, middle trapezius (MT), lower trapezius (LT), and SCM muscles, as well as functional capacity, during five upper limbs tasks using surface electromyography (sEMG). By analyzing neuromuscular responses and task performance together, the study seeks to identify potential alterations in motor control strategies associated with CNNP. Specifically, the study investigates differences in muscle activation patterns between individuals with CNNP and asymptomatic controls, and differences in functional capacity between the two groups.
Methods
Study design
This cross-sectional observational study was approved by the institutional ethics committee, and written informed consent was obtained from all participants prior to data collection. The study was conducted between May 2023 and May 2024 in a quiet, climate-controlled laboratory at the university, designed to minimize environmental distractions. All assessments, including participant positioning, electrode placement, and EMG recordings, were conducted by the same researcher, a physiotherapist trained and experienced in sEMG, to ensure consistency.
Participants
A total of 27 individuals with CNNP and 25 asymptomatic controls were included in the study. To minimize potential confounding factors, the groups were matched for age, sex, height, and body mass index (BMI). Participants in the CNNP group were recruited from patients presenting to (blinded) Hospital. Eligibility was determined through a detailed medical history, comprehensive physical examination, and evaluation of cervical spine radiographs and magnetic resonance images. After confirming the diagnosis of CNNP, the inclusion criteria were defined as being between 18 and 55 years of age, being right-hand dominant, having neck pain persisting for at least three months, having a Visual Analog Scale (VAS) score of ≥4 to indicate clinically meaningful pain,
18
and obtaining a score of 30–48% on the NDI, corresponding to moderate disability according to established NDI interpretation guidelines.
19
These thresholds were selected to ensure the inclusion of individuals with clinically meaningful pain and a moderate level of disability while preserving sufficient functional capacity to perform standardized upper-limb tasks. In contrast, a history of trauma (e.g., whiplash injury), vertebral fracture, tumor, previous surgery, psychological disorders, or any neurological, orthopedic, or systemic condition affecting upper limb function
Outcomes
Pain intensity and disability were assessed to determine eligibility for group assignment using the VAS and the NDI. Pain intensity was evaluated using the VAS, a 10 cm horizontal line anchored by “no pain” and “worst imaginable pain” with higher scores indicating greater pain intensity. 21 The NDI is a widely used questionnaire developed to assess pain and disability in individuals with neck pain. It consists of 10 items addressing both symptoms (e.g., pain, headache, concentration, sleep) and daily activities (e.g., personal care, lifting, reading, work, driving, recreation). The total score (0–50) indicates disability level; when expressed as a percentage (raw/50 × 100), categories correspond to none (0–8%), mild (10–28%), moderate (30–48%), severe (50–68%), and complete (≥70%). The Turkish version of the NDI is valid and reliable.19,22
Electromyographic data collection
sEMG signals from the UT, MT, LT, and SCM were recorded using an eight-channel EMG system (Noraxon Ultium, USA). Bipolar Ag/AgCl electrodes (Noraxon, USA Inc.) were placed 2 cm apart after standardized skin preparation involving shaving and alcohol cleaning, following the Surface ElectroMyoGraphy for the Non-Invasive Assessment of Muscles (SENIAM) guidelines. EMG signals were sampled at 1500 Hz and synchronized with a 50-fps video (Webcam C500, Logitech) to assist with timing. Electrodes were placed at specific points for each muscle: the midpoint between the acromion and C7 for UT; the medial border of the scapula and T3 for MT; two-thirds from the trigonum spinae to T8 for LT; and below the midpoint between the mastoid and sternal notch for SCM. 23 After electrode placement, maximal voluntary isometric contractions (MVICs) were evaluated using standardized manual testing positions before functional tasks. 10 For UT, participants sat unsupported with their arms abducted to 90° while resistance was applied at the elbow. For MT, measurements were taken in a prone position with 90° of horizontal abduction and external rotation. For LT, participants performed diagonal elevation in the prone position, aligned with the LT fibers’ orientation. SCM MVICs were recorded with participants lying on their backs, hips and knees flexed at 90°, performing contralateral neck rotation against resistance. 24 Each MVIC included one familiarization trial and three 5-s maximal efforts, separated by one-minute rests. 25 All were conducted by the same researcher with standardized verbal encouragement. A 5-min rest preceded functional activities. Analyses of EMG signals were performed using Noraxon MyoResearch 3.20 software (Noraxon, Scottsdale, USA). The signals were filtered using a band-pass filter (20 Hz–450 Hz). Cardiac artifacts were reduced, and the signals were smoothed using the RMS method with a 100-ms window. The peak value from a 5-s MVIC trial was recorded, and the average of three trials was utilized to normalize the EMG data from the exercises. During the Overhead Lift task, electromyographic recordings were obtained only during the standardized 5-kg lifting condition, which was performed by all participants under identical conditions. Higher lifting loads were used exclusively for functional capacity assessment and were not included in EMG analyses. For each trial, the mean EMG amplitude was calculated over the entire execution window, from movement onset to the end identified in the synchronized video. This value was then normalized to the average peak root mean square (RMS) from the three MVIC trials to yield % MVIC. The mean of the three trials was used for statistical analysis.
Functional capacity evaluation
Functional capacity was assessed using five tasks from the WorkWell Systems Functional Capacity Evaluation (WWS-FCE). WWS-FCE, a standardized tool widely utilized in rehabilitation and occupational health, has demonstrated established reliability and validity for both healthy adults and individuals with chronic low back pain.26,27 The selected tasks targeted upper limb functional performance and included the Repetitive Reaching Task (RRT), Sustained Overhead Work (OW), Waist to Overhead Lift (OL), Fingertip Dexterity Task (FD), and Hand and Forearm Dexterity Task (HFD) (Figure 1).
28
In the RRT, participants transferred 30 marbles between two bowls positioned below elbow height, using both their right and left hands in both directions. Each subtask was performed three times, and the average completion time was recorded
29
(Figure 1(a) and (b)). The FD employed the Purdue Pegboard Test, in which participants inserted pegs into holes using their right hand, left hand, or both hands within a designated time. Each trial was conducted three times, and the average score was calculated
30
(Figure 1(c)). The HFD was assessed using the Minnesota Manual Dexterity Test, which recorded the completion time for both the Dominant Hand Placement Test, where participants sequentially placed disks into holes, and the Turning Test, in which participants sequentially flipped the disks with both hands
31
(Figure 1(d)). In the Overhead Lift (OL) task, lifting commenced with a starting load of 5 kg. The load was progressively increased in increments of 2.5 kg or 5 kg, depending on the participant's performance. Participants were instructed to lift the load from waist level to a height of 80 cm above the table. The test was terminated when the participant reached their maximum lifting capacity
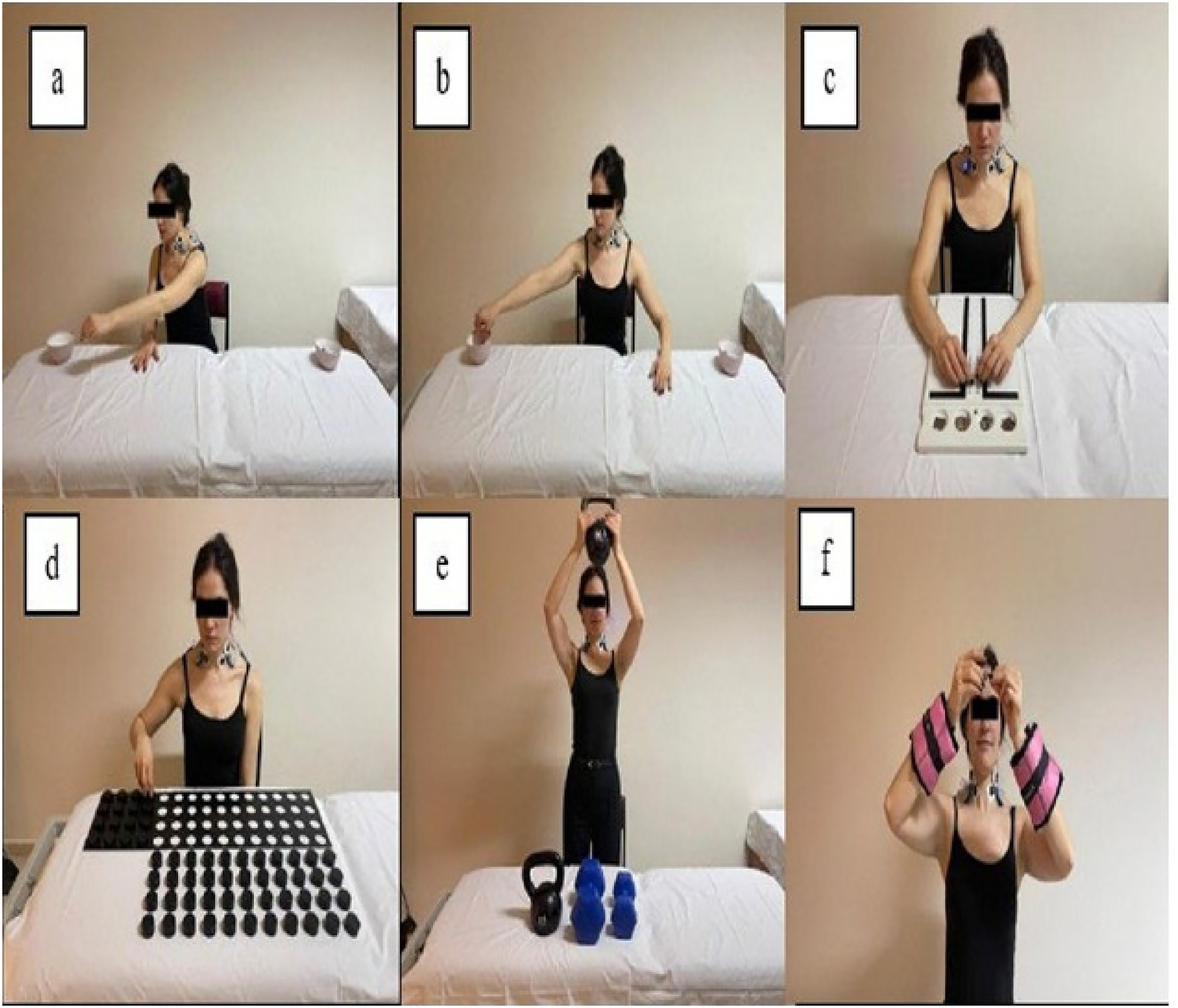
Upper limb functional tasks based on the WorkWell Systems FCE protocol
Sample size
Before data collection, an a priori power analysis was performed using G*Power v3.1 (independent-samples t test, two-tailed; α = 0.05; power = 0.90). The effect size (Cohen's d = 0.947) was derived from a previous study with a similar design. 33 This analysis confirmed that a sample size of at least 25 participants per group would be sufficient.
Statistical analysis
Statistical analyses were performed using IBM SPSS Statistics version 27.0. Mean and standard deviation (SD) values of the normalized EMG data and functional capacity measures were calculated for each functional task. The normality of data distribution was assessed using the Shapiro-Wilk test. Independent samples t-tests were conducted to determine differences between the two groups. In addition, effect sizes (Cohen's d) and 95% confidence intervals were calculated for each comparison. A significance level of p < 0.05 was considered statistically significant. Muscle activation data were additionally analyzed using a repeated-measures analysis of variance (ANOVA), with Task as the within-subject factor and Group as the between-subject factor. When the assumption of sphericity was violated (Mauchly's test, p < 0.05), Greenhouse–Geisser correction was applied. Effect sizes were reported as partial eta squared (ηp2).
Results
A total of 45 individuals with CNNP and 35 asymptomatic controls were assessed for eligibility. After applying exclusion criteria, 27 individuals with CNNP and 25 asymptomatic controls were included in the study. Electromyographic measurements were conducted with these participants. The flow of participants through each stage of the study, including eligibility screening and final analysis, is summarized in Figure 2. The sociodemographic characteristics of the participants are summarized in Table 1. There were no statistically significant differences between the groups in terms of sex, age, height, weight, or BMI (p > 0.05). VAS and NDI scores for both groups are presented in Table 1.
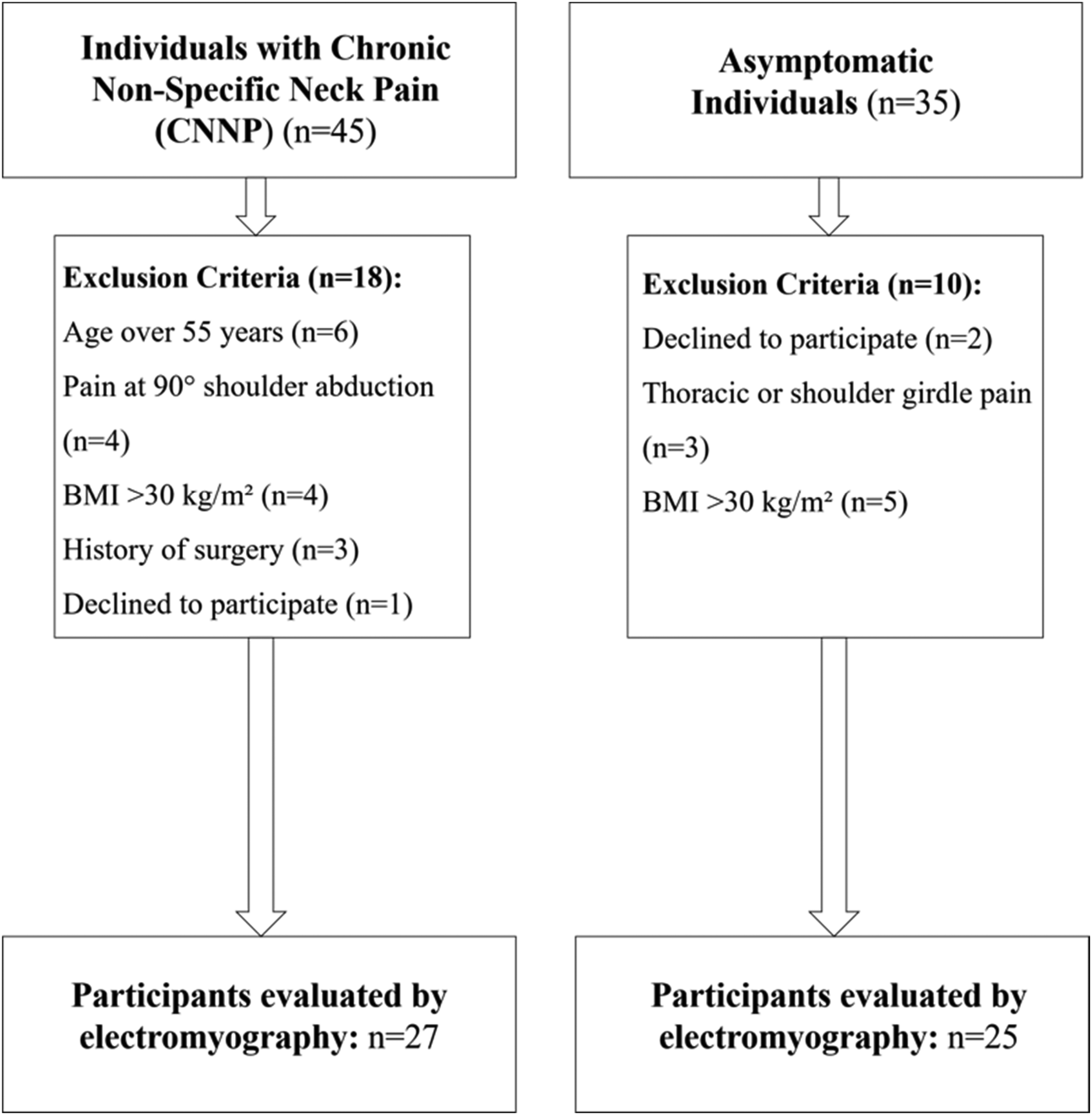
Flow diagram of participant recruitment and eligibility screening. Abbreviations: CNNP = chronic non-specific neck pain; BMI = body mass index; EMG = electromyography.
Demographic characteristics of the participants.
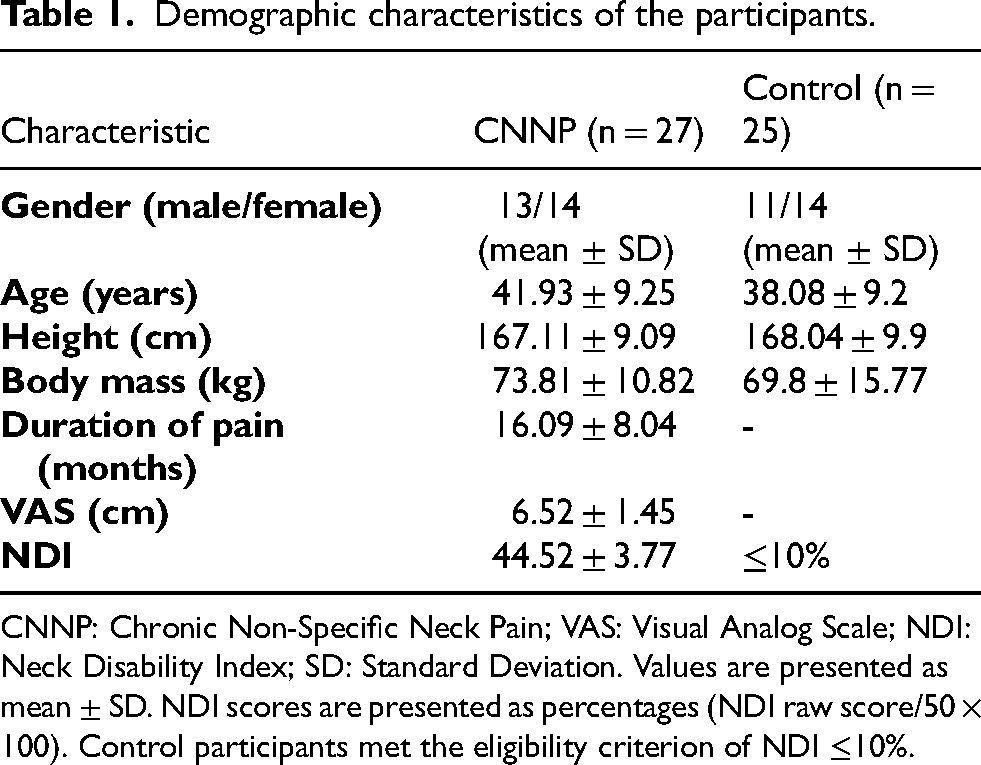
CNNP: Chronic Non-Specific Neck Pain; VAS: Visual Analog Scale; NDI: Neck Disability Index; SD: Standard Deviation. Values are presented as mean ± SD. NDI scores are presented as percentages (NDI raw score/50 × 100). Control participants met the eligibility criterion of NDI ≤10%.
During the RRT, UT activation was consistently higher in the CNNP group than in controls across all subtasks (p = 0.007–<0.001, d = 0.78–1.67). MT exhibited significant differences in the right-hand subtasks and the left-hand R→L condition (p = 0.004–<0.001, d = 0.84–1.07), while LT showed smaller but significant differences in the right-hand subtasks (p = 0.019–0.043, d = 0.47–0.68). SCM differed significantly only in the right-hand R→L subtask (p = 0.011, d = 0.73), with no significant group differences in the remaining subtasks (p = 0.095–0.300) (Table 2). During the OW task, UT, MT, and LT activations were significantly higher in the CNNP group compared with controls (UT: p < 0.001, d = 1.59; MT: p < 0.001, d = 1.06; LT: p = 0.004, d = 0.84), whereas SCM showed no significant group difference (p = 0.303, d = 0.29) (Table 3). In the OL task, the CNNP group showed significantly greater activation across all muscles than controls. The most considerable differences were observed in UT (p < 0.001, d = 1.54), MT (p < 0.001, d = 1.34), and SCM (p < 0.001, d = 1.08), while LT showed a smaller but still significant difference (p = 0.008, d = 0.77) (Table 3). In the FD task, UT and MT activations were significantly higher in the CNNP group than in controls across all subtasks (UT: p < 0.001, d = 1.11–1.68; MT: p < 0.001, d = 1.14–1.32). LT did not differ significantly in the right-hand subtask (p = 0.180, d = 0.38) but was significantly greater in the left-hand, both-hands, and assembly subtasks (p = 0.002–<0.001, d = 0.70–1.44). SCM showed no significant group differences in any subtask (p = 0.121–0.380, d = 0.25–0.44) (Table 4). In the HFD task, UT and MT activations were significantly higher in the CNNP group than in controls in both placement and turning subtasks (UT: p < 0.001, d = 1.44–1.51; MT: p < 0.001, d = 1.07–1.44). LT presented smaller but significant differences in both subtasks (p = 0.007–0.023, d = 0.65–0.78), whereas SCM showed no significant group differences (p = 0.059–0.069, d = 0.52–0.54) (Table 5). In addition, repeated-measures ANOVA revealed significant main effects of Task for all examined muscles. Significant Task × Group interactions were observed for UT, MT, and SCM, whereas no significant interaction effect was found for LT. Detailed ANOVA results are provided in Supplemental Table S1.
Comparison of muscle activation during functional tasks in individuals With chronic non-specific neck pain and asymptomatic controls.
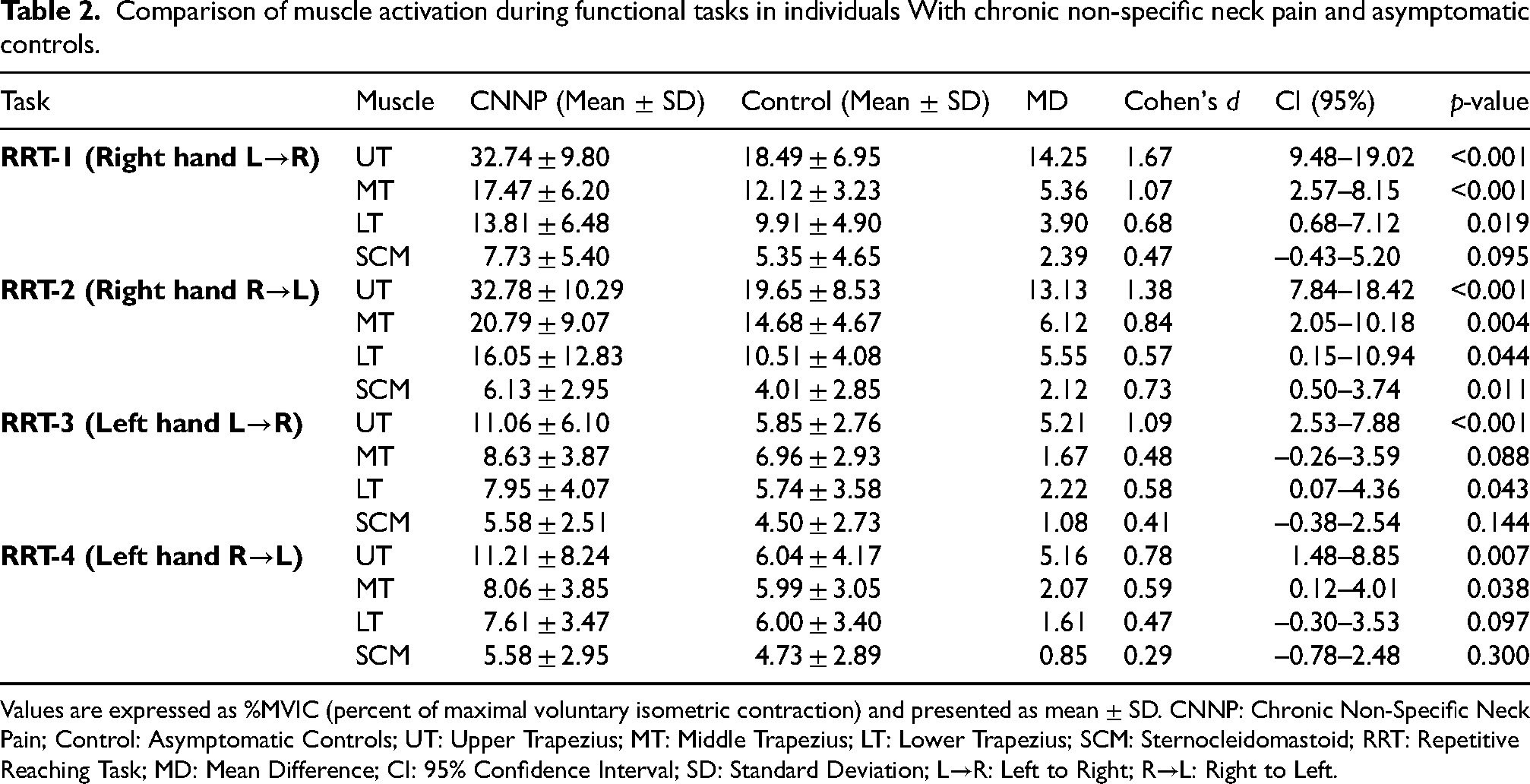
Values are expressed as %MVIC (percent of maximal voluntary isometric contraction) and presented as mean ± SD. CNNP: Chronic Non-Specific Neck Pain; Control: Asymptomatic Controls; UT: Upper Trapezius; MT: Middle Trapezius; LT: Lower Trapezius; SCM: Sternocleidomastoid; RRT: Repetitive Reaching Task; MD: Mean Difference; CI: 95% Confidence Interval; SD: Standard Deviation; L→R: Left to Right; R→L: Right to Left.
Comparison of muscle activation during functional tasks in individuals With chronic non-specific neck pain and asymptomatic controls.
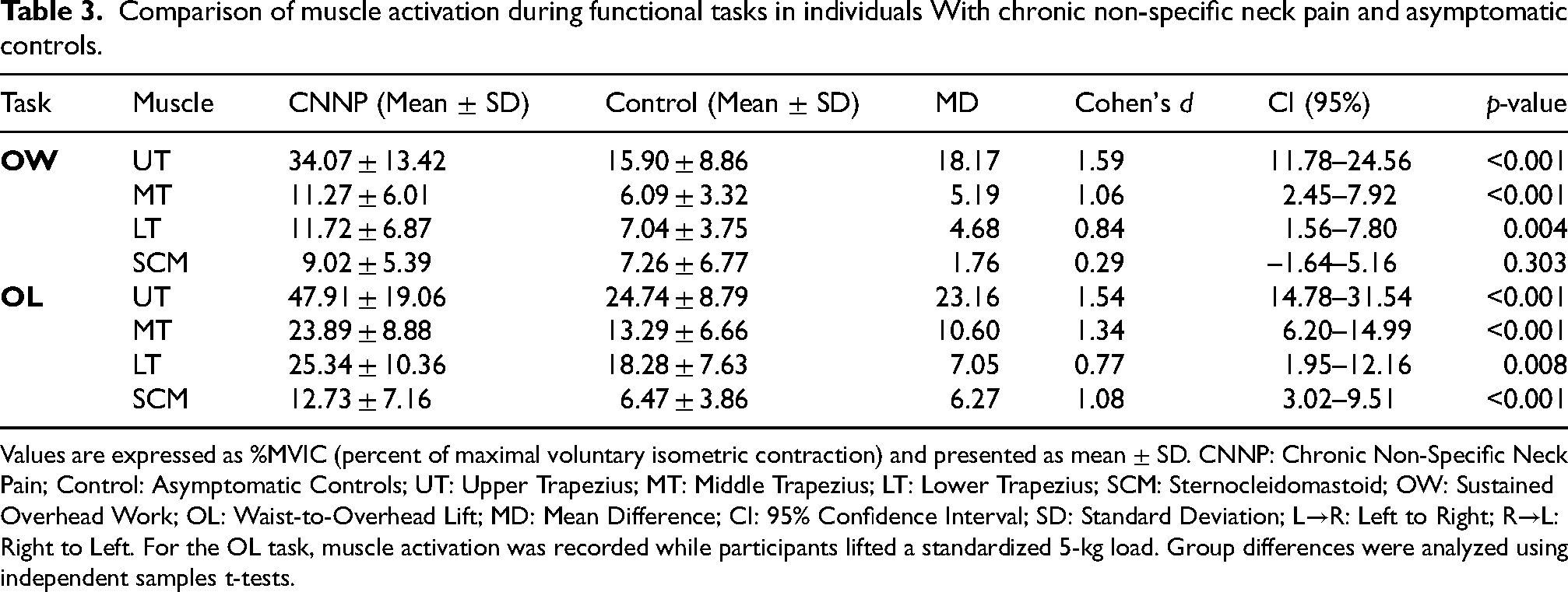
Values are expressed as %MVIC (percent of maximal voluntary isometric contraction) and presented as mean ± SD. CNNP: Chronic Non-Specific Neck Pain; Control: Asymptomatic Controls; UT: Upper Trapezius; MT: Middle Trapezius; LT: Lower Trapezius; SCM: Sternocleidomastoid; OW: Sustained Overhead Work; OL: Waist-to-Overhead Lift; MD: Mean Difference; CI: 95% Confidence Interval; SD: Standard Deviation; L→R: Left to Right; R→L: Right to Left. For the OL task, muscle activation was recorded while participants lifted a standardized 5-kg load. Group differences were analyzed using independent samples t-tests.
Comparison of muscle activation during functional tasks in individuals With chronic non-specific neck pain and asymptomatic controls.
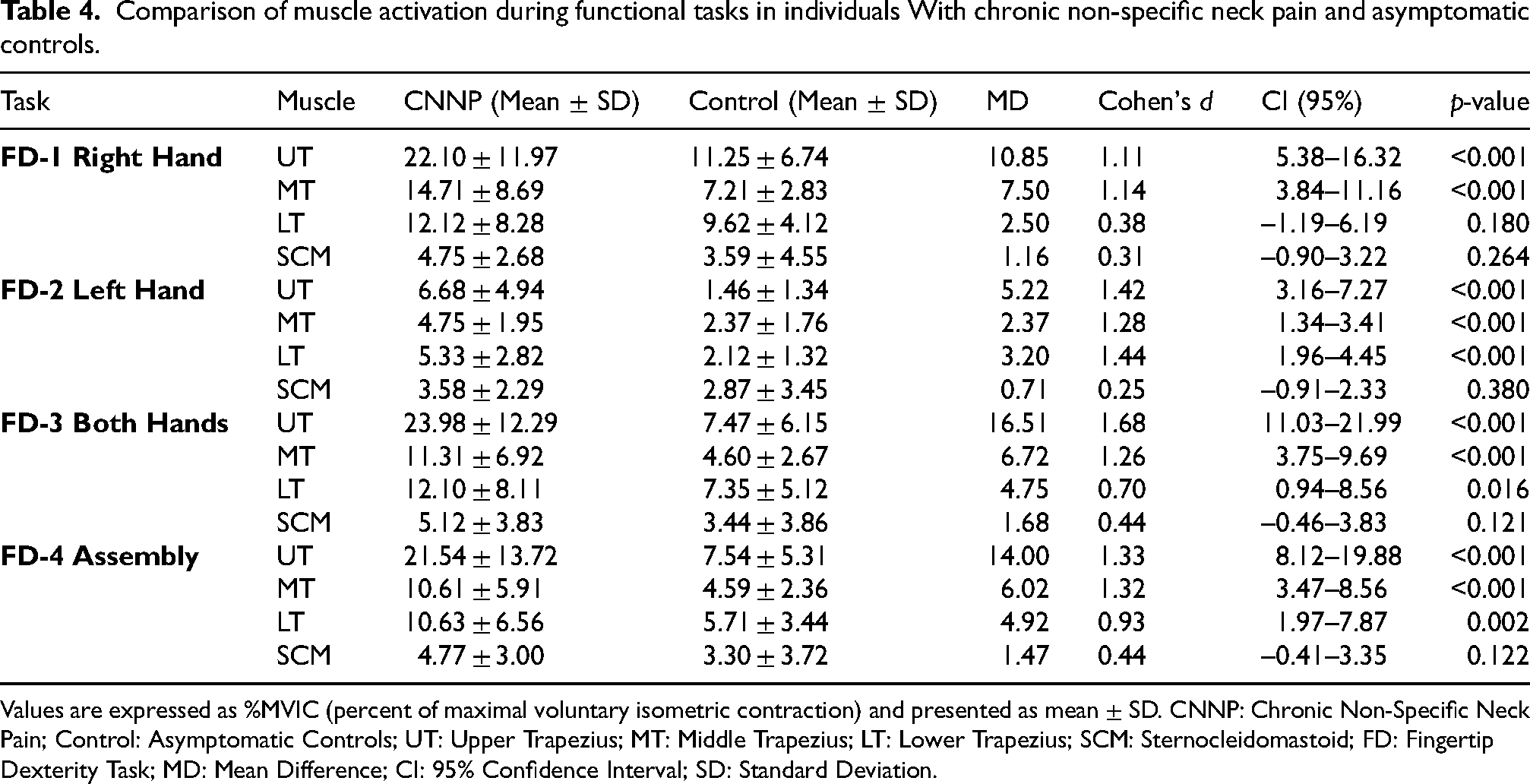
Values are expressed as %MVIC (percent of maximal voluntary isometric contraction) and presented as mean ± SD. CNNP: Chronic Non-Specific Neck Pain; Control: Asymptomatic Controls; UT: Upper Trapezius; MT: Middle Trapezius; LT: Lower Trapezius; SCM: Sternocleidomastoid; FD: Fingertip Dexterity Task; MD: Mean Difference; CI: 95% Confidence Interval; SD: Standard Deviation.
Comparison of muscle activation during functional tasks in individuals With chronic non-specific neck pain and asymptomatic controls.
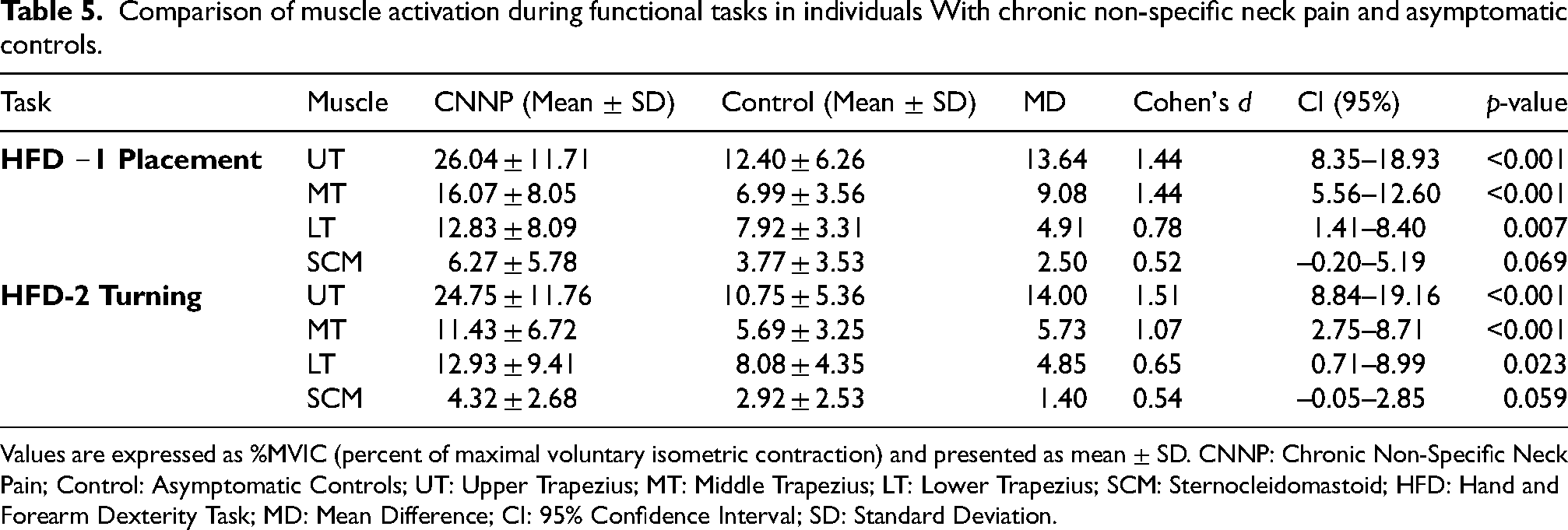
Values are expressed as %MVIC (percent of maximal voluntary isometric contraction) and presented as mean ± SD. CNNP: Chronic Non-Specific Neck Pain; Control: Asymptomatic Controls; UT: Upper Trapezius; MT: Middle Trapezius; LT: Lower Trapezius; SCM: Sternocleidomastoid; HFD: Hand and Forearm Dexterity Task; MD: Mean Difference; CI: 95% Confidence Interval; SD: Standard Deviation.
Regarding functional capacity outcomes, individuals with CNNP performed significantly worse than asymptomatic controls across all RRT subtasks (p < 0.001, d = 1.32–1.61). In the OL task, the CNNP group exhibited markedly lower success rates in the 7.5 kg (p = 0.006, d=–0.80), 10 kg (p < 0.001, d=–1.26), and 15 kg lifts (p < 0.001, d=–1.16). In the OW task, performance was substantially lower in the CNNP group (p < 0.001, d=–2.17). In the FD task, no significant differences were observed in the right-hand, left-hand, or both-hands subtasks (p = 0.66–0.89, d = -0.12 to 0.04), whereas the assembly subtask showed a trend toward lower performance in the CNNP group (p = 0.07, d = –0.51). In the HFD task, both placement and turning subtasks demonstrated significantly reduced performance in the CNNP group compared with controls (p < 0.001, d = 1.06–1.36) (Table 6).
Comparison of functional capacity measures between individuals with chronic non-specific neck pain and asymptomatic controls during different functional tasks.
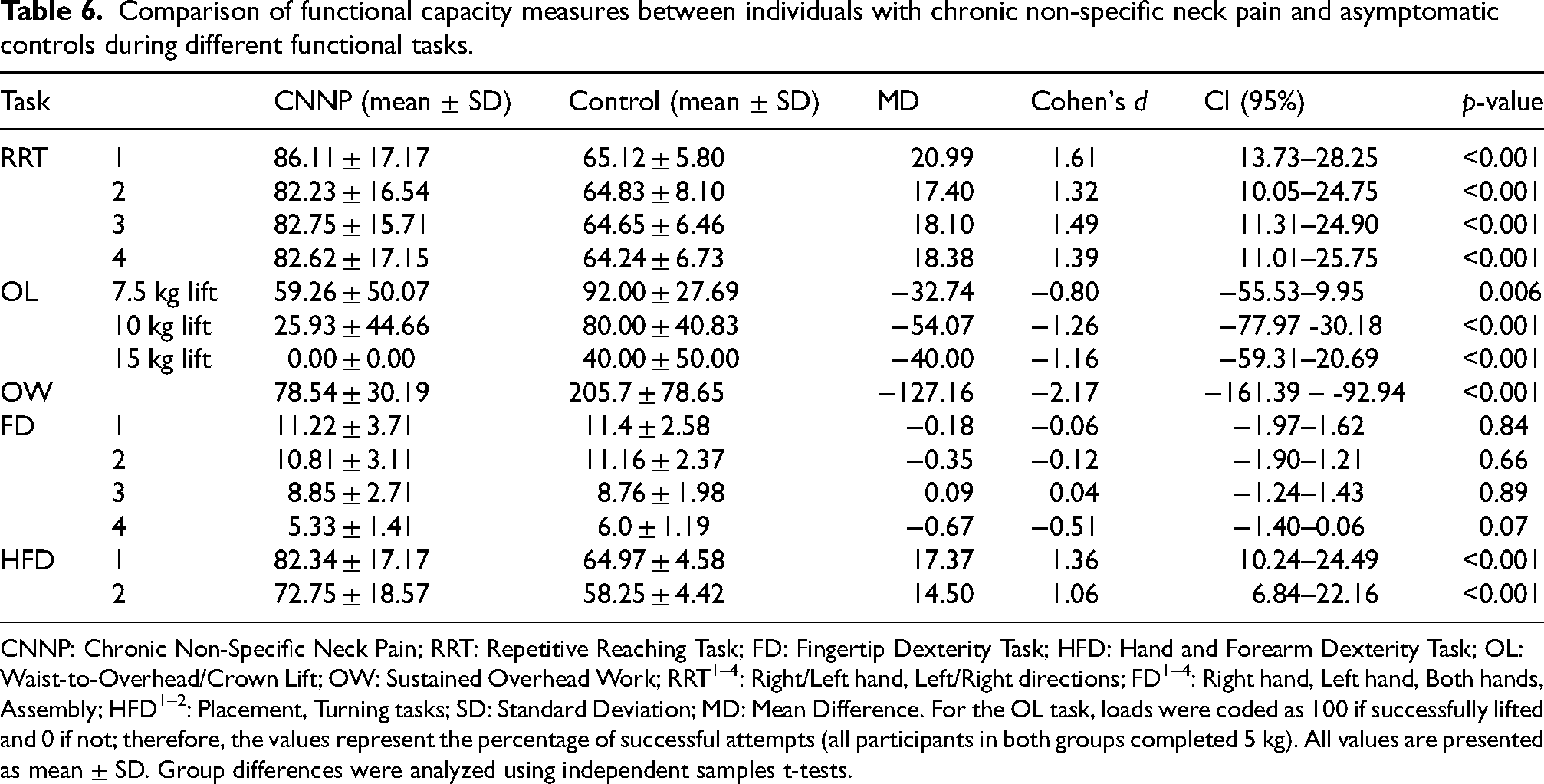
CNNP: Chronic Non-Specific Neck Pain; RRT: Repetitive Reaching Task; FD: Fingertip Dexterity Task; HFD: Hand and Forearm Dexterity Task; OL: Waist-to-Overhead/Crown Lift; OW: Sustained Overhead Work; RRT1–4: Right/Left hand, Left/Right directions; FD1–4: Right hand, Left hand, Both hands, Assembly; HFD1–2: Placement, Turning tasks; SD: Standard Deviation; MD: Mean Difference. For the OL task, loads were coded as 100 if successfully lifted and 0 if not; therefore, the values represent the percentage of successful attempts (all participants in both groups completed 5 kg). All values are presented as mean ± SD. Group differences were analyzed using independent samples t-tests.
Discussion
This study compared individuals with CNNP and asymptomatic controls in terms of muscle activation and functional performance during a range of upper limb tasks with varying demands. The findings indicate that between-group differences in muscle activation and performance were task-dependent and became more evident as task complexity and physical demand increased. In particular, tasks requiring sustained load, overhead activity, or higher sensorimotor control were associated with increased activation of superficial cervical and scapular muscles in the CNNP group, accompanied by reduced functional performance. In contrast, tasks with lower physical and postural demands revealed fewer or no group differences, highlighting the context-specific nature of neuromuscular alterations in CNNP. Furthermore, the significant interaction between group and task confirms that the altered muscle activation patterns in individuals with CNNP are not uniform but vary significantly depending on the functional task performed. From a motor control perspective, chronic neck pain is characterized by task-dependent adjustments rather than a uniform shift in muscle activation, a pattern supported by the present task-based surface EMG findings.11,34
Muscle activation patterns
During the RRT, individuals with CNNP showed greater involvement of superficial muscles, particularly the UT, with more limited differences in MT and LT and only task-specific differences in SCM. Increased activation of superficial cervical muscles during dynamic or low-load tasks has also been reported in neck pain populations.35,36 Increased UT co-activation during the low-load CCFT has been interpreted as a compensatory response to deep cervical flexor insufficiency. 4 One plausible explanation is reduced contribution of deep stabilizing muscles, which may promote compensatory recruitment of superficial muscles during functional tasks. 37 Consistent with this framework, altered deep muscle function has been reported during resisted cervical rotation in whiplash-associated pain, supporting the broader idea that impaired stabilizing function can modify task-related muscle strategies. 38 In line with contemporary pain–motor adaptation models, such compensatory patterns may have adverse secondary consequences by increasing reliance on superficial muscles during stabilization demands. 11 Task characteristics likely contributed to the differences observed across the remaining tasks. Overhead and sustained work are known to increase upper trapezius demands even over short durations, 39 and altered axioscapular/neck extensor behavior during shoulder exertions has been documented in nonspecific neck pain, suggesting that stabilization demands can amplify superficial muscle involvement. 40 In our data, OW was characterized by higher UT, MT, and LT activation in CNNP without a parallel change in SCM, whereas OL elicited higher activation across all muscles, likely reflecting the combined effect of external load and cervical stabilization requirements.
Evidence on fine-motor tasks is more limited, but available studies suggest that chronic neck pain is associated with altered motor strategies during prolonged or precision-demanding activities.41,42 For example, increased UT activity has been reported during prolonged writing and computer-based tasks have been associated with cervical muscle redistribution patterns suggestive of sustained low-threshold activation and challenges in recruiting stabilizing muscles.41,43 In this study, the CNNP group exhibited greater UT, MT, and LT activation during FD and HFD tasks
Functional performance
Individuals with chronic neck pain (CNP) have been shown to exhibit slower reaction times, impaired hand–eye coordination, reduced movement speed, and altered movement quality, partly related to restricted cervical mobility.46–48 In this context, including individuals with moderate NDI scores allowed the examination of clinically meaningful functional performance differences while ensuring safe and consistent task execution, thereby reducing potential floor effects associated with minimal disability and task intolerance in more severe cases. Consistent with this evidence, CNNP individuals in the present study completed RRT subtasks more slowly than controls, indicating impairments in movement speed and coordination. Pain-related proprioceptive deficits and protective motor strategies may restrict movement efficiency, while reduced cervical muscle endurance may contribute to early fatigue and postural adaptations during sustained or loaded tasks.49–51 Accordingly, CNNP individuals demonstrated lower performance in OL and OW, suggesting that functional capacity may decline earlier as task demands increase
Our study has some limitations. The relatively small sample size and recruitment from a single center with moderate disability levels limit the generalizability of the findings. In addition, sEMG signal quality may be affected by factors such as skin impedance, electrode placement, and movement artifacts. The absence of kinematic or postural monitoring during the functional tasks further limits the interpretation of EMG activity, as subtle compensatory movements may have influenced muscle activation.
This study provides evidence that altered motor control strategies and increased reliance on superficial muscles are associated with functional limitations during clinically meaningful upper limb tasks in individuals with CNNP. These findings highlight the importance of task-based assessments and support interpreting surface EMG results within a task-dependent motor control framework. Future studies incorporating larger samples and combined sEMG–kinematic analyses may further clarify the relationship between neuromuscular adaptations and functional performance. In addition, future research should explore the relationship between task-specific superficial muscle activation and corresponding functional performance outcomes to better understand how altered neuromuscular strategies contribute to functional limitations in individuals with CNNP.
Supplemental Material
sj-docx-1-bmr-10.1177_10538127261424303 - Supplemental material for Task-dependent muscle activation during functional upper-Limb tasks in adults with and without chronic non-specific neck pain: A cross-sectional study
Supplemental material, sj-docx-1-bmr-10.1177_10538127261424303 for Task-dependent muscle activation during functional upper-Limb tasks in adults with and without chronic non-specific neck pain: A cross-sectional study by Gizem Soylu and Özlem Ülger in Journal of Back and Musculoskeletal Rehabilitation
Footnotes
Acknowledgments
None.
Ethical considerations
This cross-sectional observational study received approval from an institutional ethics committee (committee name and approval number withheld for blinded review).
Author contributions (CRediT)
G.S. Conceptualization; Methodology; Investigation; Data curation; Formal analysis; Visualization; Writing – original draft; Writing – review & editing.
O.U. Validation; Resources; Supervision; Project administration; Funding acquisition; Writing – review & editing.
Consent to participate
All participants provided written informed consent before enrolment.
Consent for publication
Not applicable (no identifiable individual data, images, or videos are included).
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
The data supporting the findings of this study are available from the corresponding author upon reasonable request.
Supplemental material
Supplemental material for this article is available online.
