Abstract
Background
Numerous interventions exist for neck pain in all age groups, but novel manual approaches warrant further investigation to assess their applicability in pediatric populations.
Objective
This study aimed to determine and compare the immediate effects of instrument-assisted soft tissue mobilization (IASTM) and classical massage (CM) in children aged 10–11 years with chronic neck pain.
Methods
IASTM or CM were applied to the neck regions of a total of 52 children with chronic neck pain. Visual Analogue Scale (VAS), universal goniometer, and digital pressure algometer were used to evaluate pain severity, Range of Motion (ROM), and pressure pain threshold (PPT).
Results
Significant within-group improvements were observed in VAS scores and cervical ROM post-treatment (p < .001). Additionally, a significant difference was found only in the PPT value of the left cervical region in the CM group (W = –2.237; p = .025). Between-group differences at each time showed that significant differences were found in cervical flexion (U = 2.630, p = .009) and PPT left cervical (U = –2.326; p = .020) before treatment and also, significant differences were obtained in the PPT right cervical (U = –2.555; p = .011), PPT right upper trapezius (U = –2.545; p = .011), and PPT left upper trapezius (U = –1.968; p = .049), after treatment.
Conclusion
Both IASTM and CM were equally effective in reducing pain severity, the study's primary outcome. When adjusted for time, differences emerged only in cervical lateral flexion, with region-specific variations. However, long-term outcomes remain unknown, and future trials should include follow-up periods, larger and more diverse samples, and control or placebo groups to clarify clinical effect.
Keywords
Introduction
Pain is one of the most significant health problems affecting the musculoskeletal system in children. 1 Many factors, such as poor sitting posture, carrying heavy backpacks, and excessive homework, contribute to musculoskeletal pain. 2 Although the epidemiology and treatment of musculoskeletal pain in adults have been extensively investigated, only a limited number of studies have addressed this issue in children. 3
The prevalence of musculoskeletal symptoms in children ranges from 16% to 86% in developed countries and from 46.3% to 88.8% in developing countries. 1 Pain is mostly seen in the neck region of school children. 4 Considering the annual prevalence of neck pain in children, it appears to vary between 28 and 40%. 5
Although various manual therapy methods have been developed for musculoskeletal pain, these are usually applied and studied in adults.6,7 Their effectiveness has been demonstrated either alone or as an adjunct to traditional treatment approaches.6,7 However, research on manual therapy techniques in pediatric populations is limited. Dice et al. 8 reported that neuromuscular techniques, joint mobilizations (grades I–IV), visceral manipulation, and craniosacral therapy have been used in preadolescent children. Nevertheless, the authors emphasized several barriers, including insufficient evidence, lack of knowledge, fear of litigation, and concerns about patient safety. 8 A systematic review also indicated that studies on the treatment of pediatric neck pain are insufficient, and researchers have been urged to develop more effective treatment procedures. 9
Massage is commonly applied to infants and children for purposes such as promoting physical growth, supporting motor development, and managing pain. 10 Classical massage (CM) is a traditional approach in pediatric clinics, primarily based on the gate control theory of pain reduction.11,12 Instrument-assisted soft tissue mobilization (IASTM), which is known as ‘strigil’ in ancient Greece and Rome and as ‘gua sha’ in traditional Chinese medicine—originates from practices aimed at treating musculoskeletal pain. 11 The pain management mechanism of IASTM resembles James Cyriax's cross friction massage as it creates an irritation effect and inhibits pain through postsynaptic mechanisms rather than the gate control theory.11,13,14 The primary purpose of IASTM is to induce microtrauma, thereby facilitating a local inflammatory response and remodeling connective tissue. Consequently, IASTM aims to reduce pain, enhance soft tissue mobility, and improve ROM and function within a shorter duration and with less therapist effort.13,14
In the United States and United Kingdom, researchers showed substantial direct and indirect annual costs associated with treating chronic musculoskeletal pain in children, highlighting the urgent need to strengthen the evidence base and establish manual therapy guidelines for pediatric populations. 8 Thus, this study was designed to investigate effects of IASTM on children whom has not been applied before and to compare its effectiveness with CM, which is widely used in treating pediatric musculoskeletal disorders. Although both manual therapies reduce pain through different mechanisms, the primary aim of these interventions is pain management. Therefore, we hypothesized that IASTM will lead to greater immediate reductions in neck pain and improved cervical range of motion compared to classical massage. Since the main complaint was pain, the primary objective was to find better intervention to reduce pain level.
Materials and methods
Study design
The study is a single-blinded, randomized clinical trial.
Participants
Children aged 10–11 years with physician-diagnosed chronic neck pain were recruited between March 2021 and August 2021 at the Pediatric Physiotherapy Unit of the Faculty of Health Sciences, Eastern Mediterranean University University.
All children (n = 925) with 10–11 ages registered in Famagusta primary schools were invited to the study through parental invitation letters, which explained the purpose of the study. The parents of 74 children responded, and after screening based on inclusion and exclusion criteria, 22 children were excluded from the study after the assessor (fourth author) made the measurements (such as pain severity, pain duration, neck motions). The children's participation flow was shoen in the Figure 1.
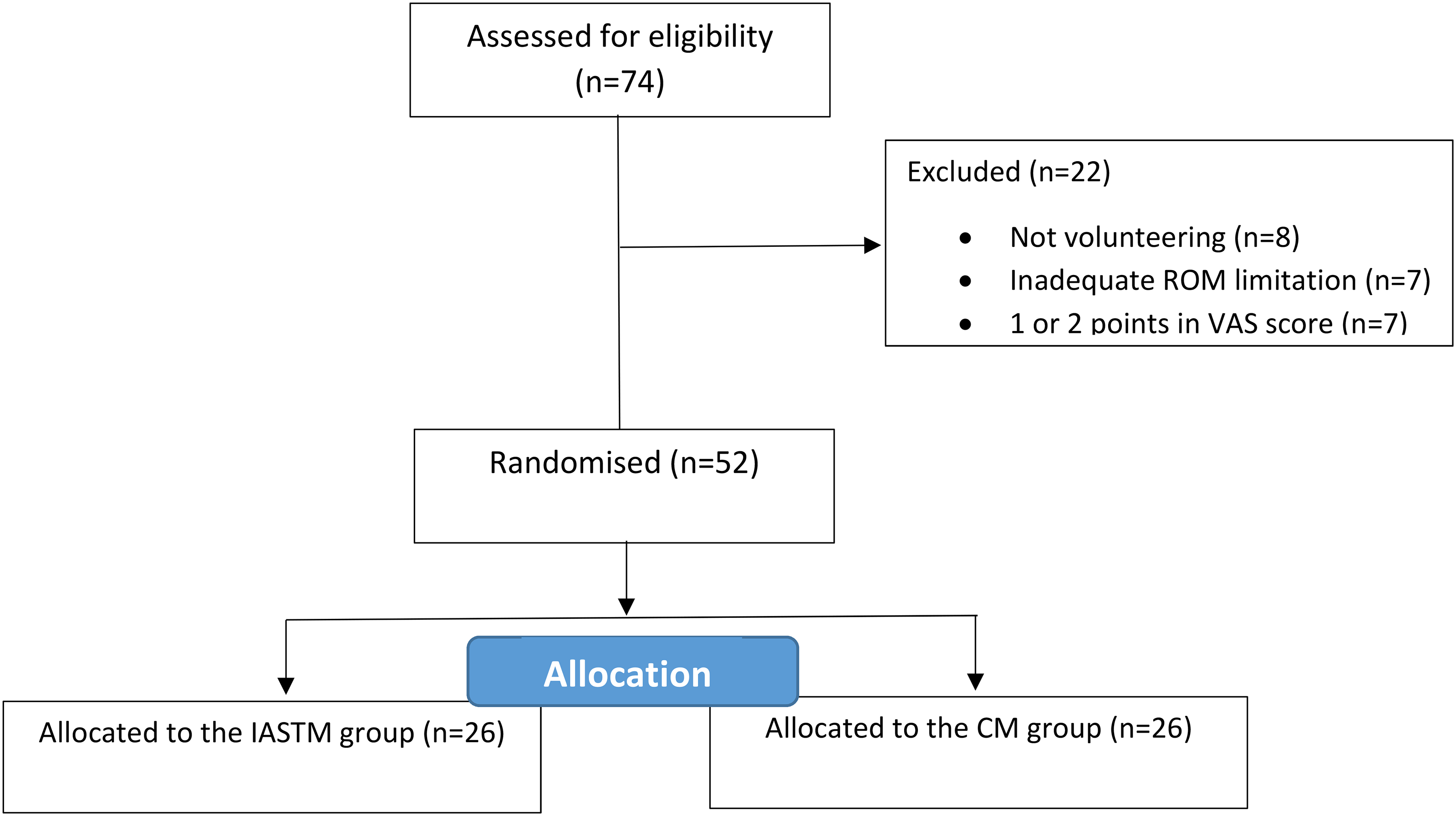
CONSORT flow diagram of the study. IASTM: Instrument Assisted Soft Tissue Mobilization, CM: Classic Massage, ROM: Range of Motion, VAS: Visual Analogue Scale.
A total of 52 children with chronic neck pain were divided into two groups: IASTM (n = 26) and CM (n = 26) using the Random Allocation Software. 15 To ensure blinding, assessments were performed by an independent evaluator in a separate room, who remained unaware of group allocation. Randomization was also concealed by an independent statistician.
All children in the study and their parents were informed both verbally and written informed consent was obtained from all parents prior to participation.
According to the inclusion criteria, children who had a minimum 10-degree limitation in at least one direction of active neck movements, had neck pain above 3 on the Visual Analog Scale (VAS), had neck pain for at least 3 months, and were diagnosed with chronic neck pain by the physician were included in the study.
Children with neurological pain (neuropatic pain, cerebral palsy, muscle disease) and/or musculoskeletal pain next to the neck region (shoulder pain, toracal pain), serious medical conditions (cancer, vertebral fractures, inflammatory diseases) and with open wounds in the neck region that could affect the manual therapy approaches were excluded from the study.
Ethics
The study was conducted in accordance with the Declaration of Helsinki and approved by the Ethical Review Board of the Eastern Mediterranean University (17.11.2020, ETK00-2020-0038). Additional approval was obtained from the Ministry of Education (01.12.2020, İÖD/E6727).
Interventions
The first author, a certificated IASTM practitioner and experienced physiotherapist, delivered both interventions. Prior to the study, a few trial sessions were conducted to assess feasibility and acceptance by children. The force and speed of the interventions were adapted to the children's age and developmental level. 14 Participants were instructed to avoid analgesics or additional treatments for neck pain on the study day.
The children were randomly divided into two groups. All children were evaluated before and after one-session intervention, either IASTM or CM, and their immediate effects were examined. The children were asked to go to the assessment room again after either intervention and have a rest for 5 min. Following this resting period, final assessments were conducted. The children were informed that they should not state the type of their intervention to the assessor. Any unpleasant feeling during/after the interventions and/or any side effect which caused withdraw of children from the study were recorded by the therapist (first author).
Due to the covid-19 pandemic conditions, both therapist (first author) and assessor (fourth author) used masks. Additionally, instruments for IASTM group were disinfected between uses.
Instrument assisted soft tissue mobilization
The total treatment time was 15–20 min.13,16 The Graston Technique as an IASTM technique was applied with appropriately sized stainless steel instruments. 8 Appropriate types of were chosen depending on the body structures of the children. Large instrument was used for large surface areas and small instrument was used for small surface areas and fibrocytic-scar structures. Vaseline was used as an intermediate to reduce friction. Instruments were positioned at a 30–60° angle to the skin and strokes were then applied parallel to muscle fibers at tolerable pressure, bilaterally. Target muscles included upper and middle trapezius, levator scapulae and erector spinae. 16
The children were informed that the IASTM would be applied to their neck regions. The instruments were introduced to them and the aims of this manual therapy were explained. Prior to treatment, the therapist demonstrated the technique on her arm to reduce anxiety. Then, children were seated with their arms supported on a table and forehead resting on hands.
Classical massage
The total treatment time was 20–25 min. The Swedish Technique which is a CM technique and was used, characterized by long strokes, kneading, and friction as needed. 17 Baby oil was used as an intermediate to facilitate smooth movements. Target muscles were the upper and middle trapezius, levator scapulae and erector spinae.18,19
The children were informed that a classical massage would be applied to their neck regions. As soon as the aims of CM were explained to them, Children were seated with neck and arms supported by pillows, arms abducted at 90° with elbows flexed.
Data collection
Baseline demograpic information including children's age, sex, height, weight, hand dominance, exercise habits, sitting posture duration, and injury history (previous sports injuries or accidents) was obtained. Outcomes included pain severity, range of motion, pressure pain threshold, and treatment satisfaction.
Primary outcome measure
Pain severity
The Visual Analogue Scale (VAS) is a method consisting of a 10 cm scale from 0 to 10. A line showing the lowest score with (0 cm) and highest score with (10 cm) are defined as no pain and worst pain. Children were asked to sign their pain levels on this line. 20
Secondary outcome measure
Range of motion (ROM)
Universal goniometer was used to measure active ROMs. 21 Children were asked to perform cervical flexion, extension, right-left lateral flexion and right-left rotation movements in the sitting position. Each measurement was repeated 3 times and the mean result was recorded in degrees. 21
Pressure pain threshold (PPT)
The Wagner Force One Model FDIX 50TM, Wagner Instruments, Greenwich, Conn digital pressure algometer was used to measure PPT.22,23 The cylindrical end of the device consists of a 1 cm2 pressure application surface and records the result as Newton (N).24,25 Pressure pain thresholds of neck were measured at the regions of 3 cm lateral to the C1, C3-4 and C7 spinous processes, 3 cm lateral to the trapezius region (muscle belly), 3 cm medial to the acromion, the midpoint of the trapezius muscle and 3 cm lateral to the T7 spinous process with a suitable pen for the skin. 22
While pressure was applied vertically to the neck and upper back area of the children with the algometer, they were asked to say “stop” as soon as they felt pain. The test was repeated 3 times for each region, with a 30-s break between the measurements. Numerical data were recorded by taking the averages of the regions where the measurements were made. 26
Satisfaction with treatments
VAS was used to determine the level of satisfaction from the IASTM and CM interventions. The children determined their satisfaction levels on a 10 cm scale. A value of “0” indicates that they are not at all satisfied, and a value of “10” indicates that they are satisfied. 27
Statistical analysis
The population were 925 children aged 10–11 registered to the Ministry of Education from Northern Cyprus. As sample size calculation, a power analysis was performed using the G*Power 3.1.9.2 software while α=0.05, β=0.20, and large effect size (d = 0.80) in two-group design. A minimum of 52 participants was required.
Continuous variables were shown as mean ± standard deviation (x ± ss), and categorical variables as number (n) and percentage (%). Due to group sizes (<30), Mann–Whitney U and Wilcoxon signed-rank tests were used for between- and within-group comparisons (age, BMI, sitting durations, PPT, ROM, and VAS). Chi-Square tests were applied for categorical data (sex, dominant hand, exercise habit, and injury history). Quade's non-parametric analysis of covariance (ANCOVA) was used to adjust baseline differences. Considering the error level (= α) as .05, p values below or equal to this value (p ≤ .05) was considered statistically significant. The data obtained in the study were analyzed using the IBM SPSS Statistics 26.0 (Demo version).
Results
Sociodemographic information of 52 children included in the study is shown in Table 1. There was no statistically significant difference between the groups for age, height, weight, BMI and sitting durations of the participants (p > 0.05). A total of 37 (71.15%) boys and 15 (28.85%) girls participated in the study (χ2 = 2.342; p > 0.05). While there was no difference in hand dominancy (χ2 = .000; p > 0.05), there was a significant difference in terms of exercise habit (χ2 = 3.900; p < 0.05) and injury history (χ2 = 4.457; p < 0.05) (Table 1).
Sociodemographic variables of the children.
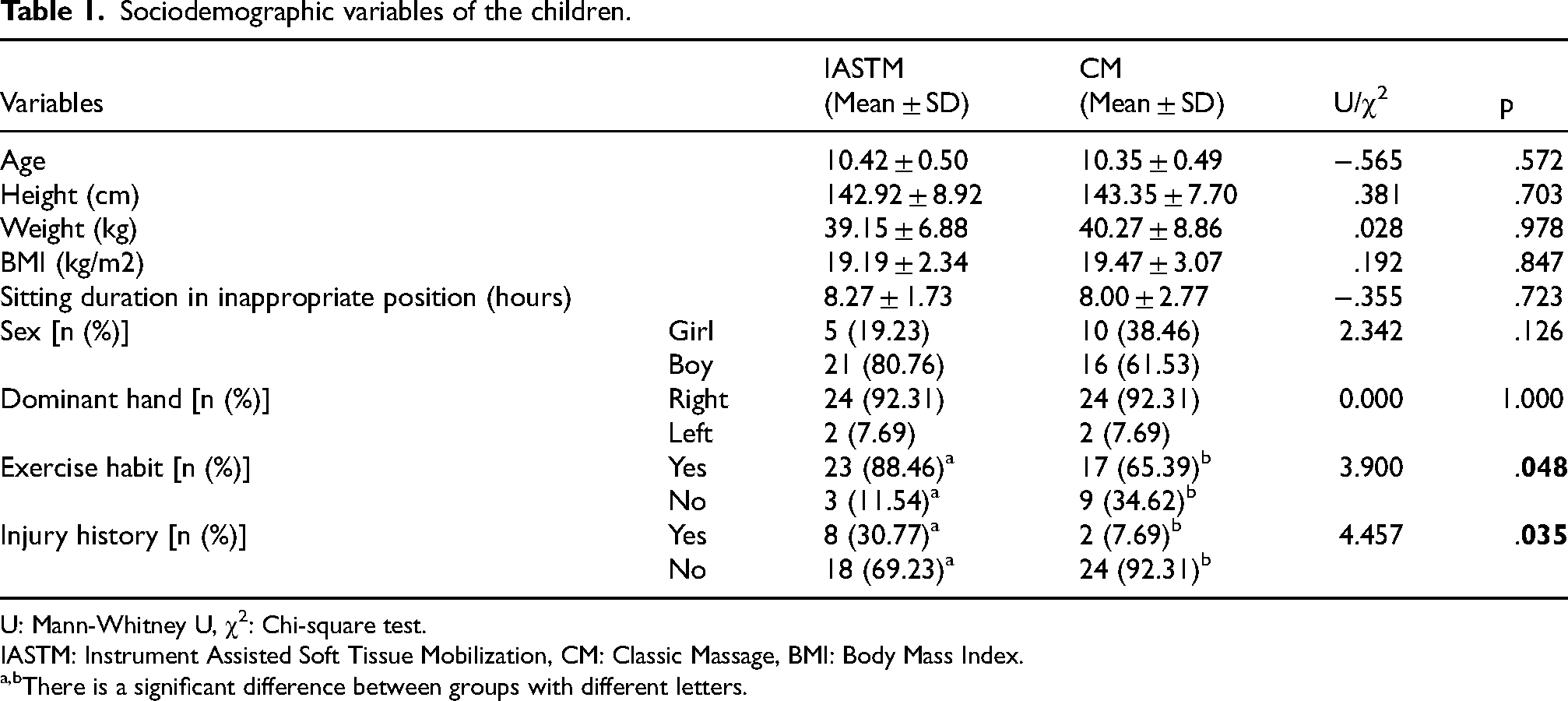
U: Mann-Whitney U, χ2: Chi-square test.
IASTM: Instrument Assisted Soft Tissue Mobilization, CM: Classic Massage, BMI: Body Mass Index.
There is a significant difference between groups with different letters.
In Table 2, the results were reported according to the group, time, and adjusted baseline separately.
Comparisons of the pain severity, range of motion, and pressure pain threshold before and after treatment within and between IASTM and CM group.
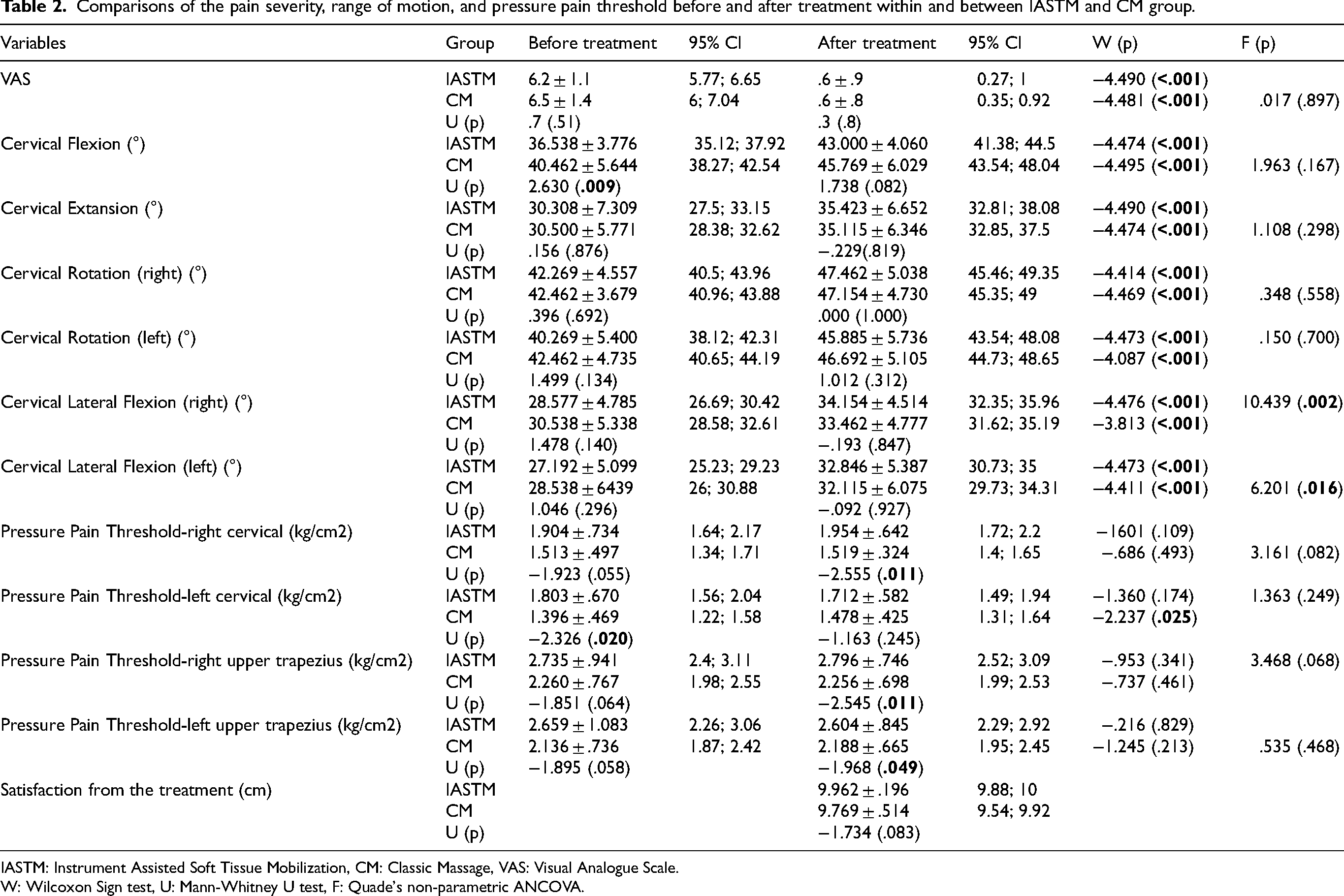
IASTM: Instrument Assisted Soft Tissue Mobilization, CM: Classic Massage, VAS: Visual Analogue Scale.
W: Wilcoxon Sign test, U: Mann-Whitney U test, F: Quade's non-parametric ANCOVA.
Pain severity as the primary outcome measure
Willcoxon signed rank test by separating to the groups was used to see the within-group changes in time in Table 2. When VAS measures were compared, statistically significant decreases were found before and after both IASTM (W = –4.490; p < 0.001) and CM (W = –4.481; p < 0.001) group. Between-group differences at each time were examined by Mann-Whitney U test (Table 2). There was no significant difference in VAS levels between groups both before and after the treatment (p > 0.05).
Other outcome measures: ROM, PPT, satisfaction from treatment
Willcoxon signed rank test by separating to the groups was used to see the within-group changes in time (Table 2). In respect to ROM measures, it was observed that there was a statistically significant increase in all neck motion directions before and after treatment both IASTM and CM groups (p < 0.001). When PPT measures were compared, it was determined that there was no statistically significant difference between the pressure pain thresholds before and after treatment in both IASTM and CM groups (p > 0.05) except for left cervical in CM group (W = –2.237; p < 0.05) (Table 2).
Between-group differences at each time were examined by Mann-Whitney U test in Table 2. According to the results before treatment, it was found statistically significant increased in cervical flexion (U = 2.630; p < 0.05) and statistically significant decreased in the PPT left cervical (U = –2.326; p < 0.05) in CM group. According to the results after treatment, it was found statistically significant difference in the PPT results of right cervical (U = –2.555; p < 0.05), right upper trapezius (U = –2.545; p < 0.05), and right upper trapezius (U = –1.968; p < 0.05) in CM group (Table 2). These results showed that PPT results varied greatly depending on the applied area.
Looking at the subjective findings of the IASTM recorded by the first author, no side/adverse effect was reported during or after the study. When the perceived satisfaction levels from the interventions were examined, it was seen that both groups satisfied from the intervention similarly with high values (U = –1.734; p > 0.05).
Finally, we adjusted to the baseline and then we computed as ANCOVA in Table 2, we found that cervical lateral flexion on both sides were different (F = 10.439; p < 0.05 on right and F = 6.201; p < 0.05 on left). The mean change of the measurement according to the group and time were demonstrated by Figure 2.
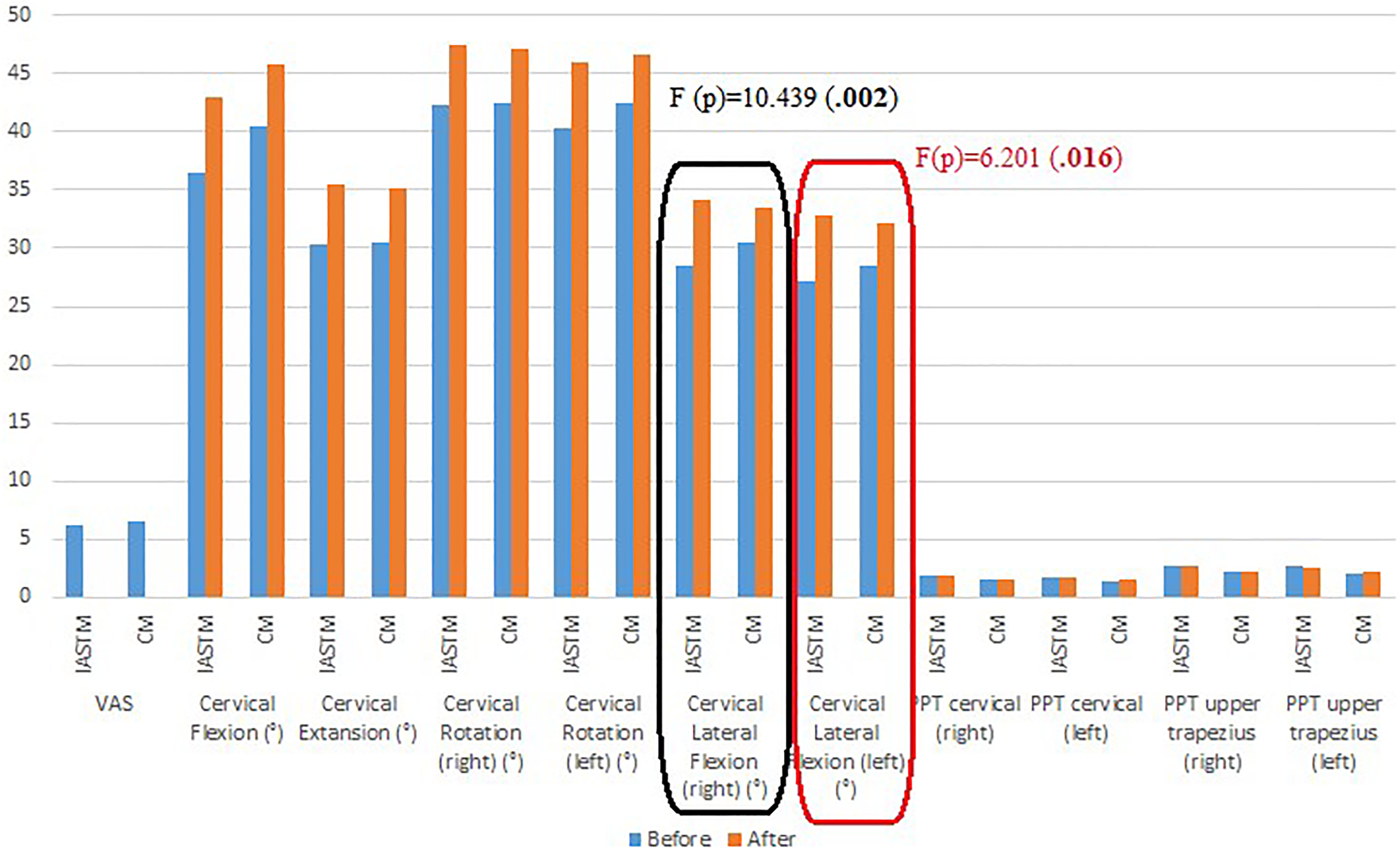
The mean values of outcome measures in the groups. IASTM: Instrument Assisted Soft Tissue Mobilization, CM: Classic Massage, VAS: Visual Analogue Scale, PPT: Pressure Pain Threshold.
Discussion
The findings of this study demonstrated that both IASTM and CM produced comparable positive effects on pain reduction and cervical range of motion in children with chronic neck pain. Neither technique was consistently effective in improving pressure pain thresholds, with the exception of the left cervical region in the CM group. When outcomes were compared between the groups, no significant differences were observed in VAS or ROM, whereas PPT values varied by anatomical region. Notably, differences in cervical flexion and PPT of the left cervical region were present at baseline but were no longer significant after treatment. After adjusting for baseline, cervical lateral flexion was significantly greater in the IASTM group compared to the CM group. Importantly, although both interventions significantly reduced pain—the primary outcome—no between-group differences were observed. Since these results represent the effects of a single session, further studies are required to evaluate the long-term benefits and to clarify the relative advantages of each intervention.
Lauche et al. 28 applied IASTM to 39 people aged between 18–75 with chronic neck and low back pain with a VAS value of 4 and above. In the study, the IASTM was applied to the cervical and lumbar regions for 15 min and the immediate effect was investigated before and seven days after a treatment session. These authors found significant immediate reductions in pain severity. Although their study differed in age group and follow-up time, our findings similarly support the immediate analgesic effect of a single IASTM session. Thus, this study extends evidence to children, suggesting that IASTM may be a safe and effective option for pediatric neck pain.
Similarly, the immediate effects of massage therapy were investigated in a study which included 116 adults with chronic pain and a significant decrease was found in pain values after a single session. 29 In line with those results, our findings confirm that CM is beneficial for children with chronic neck pain. Taken together, evidence suggests that both IASTM and CM are effective for short-term pain relief across age groups. However, the present study is the first to directly compare these two interventions in a pediatric population, and no superiority was found in terms of immediate pain management. Future research should examine long-term outcomes and different clinical contexts.
With regard to ROM, Lee et al. 30 compared IASTM and roller stick massage in young adults aged 20–25 years with hamstring muscle shortness and found both to be effective immediately and after 48 h. Similarly, our study demonstrated significant improvements in most cervical ROMs in both groups. While CM is more accessible and requires fewer resources, IASTM may provide greater gains in specific motions such as cervical lateral flexion, which warrants further investigation.
Contrary to previous findings in adults by Lauche et al. and Bakar et al.,27,28 our study did not reveal significant effects of IASTM or CM on PPT in most regions. The only significant increase was seen in the PPT value of left cervical region within the CM group. According to the comparisons between the CM and IASTM interventions, the values of pain threshold showed significant differences. The PPT of some regions had a tendency to increase, whereas a decrease was seen in others. Regarding the other group comparisons, IASTM was more successful to increase right PPT values, whereas left side values had a tendency to decrease.
Although, change in threshold is not adequately known for childhood, Hogeweg et al. 31 showed that children's pain threshold increased with age for the paraspinal regions so our results also confirm that PPT may not present a clinically significant result with a session. Differences between right and left side thresholds may reflect variability in children's painful regions or age-related sensitivity to pain pressure. Given that PPT in children is known to increase with age, these results suggest that PPT changes following a single treatment may not be clinically meaningful in pediatric populations. Future studies should explore age-specific responses and use larger sample sizes to better understand PPT outcomes.
Another important finding was related to children's acceptance of interventions. While CM was readily accepted due to its familiarity, additional explanation and demonstration was required. Some children initially showed hesitation toward the instruments, which was mitigated through this explanation and demonstration. Future studies could investigate how to enhance pediatric comfort with unfamiliar therapeutic tools.
To our knowledge, no prior studies have evaluated pediatric satisfaction with manual therapy. Both groups in this study reported high and comparable satisfaction, and no adverse effect was observed. This suggests that both interventions are well-tolerated by children.
Further studies should focus on the long-term effects of manual approaches in pediatric population. These approaches are used as an adjunctive method in the treatments of chronic musculoskeletal system disorders so they can be added to exercise and other traditional interventions in order to investigate and compare their further effects. Moreover, since exercise habits and injury states of the groups were different, these variables should be considered while designing studies.
Limitations
The same therapist applied both interventions and this could cause – consciously or unconsciously- bias. Secondly, regarding the design of study, there is no control/placebo group and follow-up periods. Control/placebo group would have shown whether some other causes like any kind of touching to painful areas or Hawthorne effect would have caused change in this sample. Follow-up periods would be important to show whether these effects would last for a while. Thirdly, although groups were homogen in many important factors, they were not homogen in terms of exercise habit and injury history, so they may cause confounding effects on results. Moreover, since the power analysis was conducted for the minimum number, sample size was small. Lastly, the country where the study was carried out had lockdown in the study duration since the positive cases had a gradual increase. Thus, covid-19 pandemic conditions prevented to use more objective measurements for ROM while planning the study as the same electrodes could have been a worry in terms of hygen. These limitations should be taken into account while planning further research.
Conclusion
This single-blind randomized study found that both IASTM and classical massage produced immediate effects on pain and range of motion in children with chronic neck pain. While these preliminary results are encouraging, they are limited by the short-term nature of the intervention and the lack of a control/placebo group. Further research is needed to confirm these findings and assess long-term outcomes.
Footnotes
Abbreviations
Acknowledgements
We want to thank for all children and their parents to participate in our study, even in covid-19 pandemic conditions.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
The recommendations of the Declaration of Helsinki and the Ethical Review Board of the Eastern Mediterranean University (dated 17.11.2020 and numbered ETK00-2020-0038) were used. All children in the study and their parents were informed both verbally and in writing before the study, and a voluntary informed consent form was signed by the parents.
Author contributions
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
The datasets collected during and/or analyzed during the current study are available from the corresponding author upon reasonable request.
Clinical trial registration number
The study was registered at the US National Institutes of Health (ClinicalTrials.gov) NCT04817384.
