Abstract
Background
Current literature suggests young outdoor workers experience a higher risk for workplace exposures including elevated risk of sun related health risks for outdoor workers.
Objective
This study aimed to assess young workers’ understanding of sun-related hazards and associated sun safety practices in the workplace.
Methods
A survey targeted young workers ages 18 −25 years in Canada and the United Kingdom either currently or previously employed. The full survey was on a variety of workplace hazards, and we report here on the subset of respondents who reported working outdoors for at least part of their typical day, for which a sun safety-related module was also asked. A sample of survey respondents were also invited to participate in a focus group.
Results
Nearly all (97%) of the 760 outdoor workers reported knowledge of skin cancer being a risk of sun exposure, but few workers (13.9%) reported receiving sun or heat safety training. Over half (65%) reported little concern about workplace sun exposure. Self-reporting of sun safe practices among respondents, such as often wearing UVR protective clothing (7.5%) was poor.
Conclusions
Findings suggest that young workers have moderate awareness of workplace sun safety, but generally reported poor adherence with sun-safe practices at work.
Introduction
Solar ultraviolet radiation (UVR) is classified as a human carcinogen by the International Agency of Cancer Research and is the main cause of skin cancer. 1 Outdoor workers are exposed to a higher amount of solar UVR, increasing risks associated with exposure,2–4 with levels often exceeding the solar UVR occupational exposure limits set by the International Commission on Non-Ionizing Radiation Protection (ICNIRP), 5 although occupational exposure limits may differ by location and exposures can vary with work hours and season. In addition to skin cancer, solar UVR exposure increases risk of solar keratosis, cataracts, ocular melanoma, pterygium, and macular degeneration. 6
Adverse health effects can also occur from heat exposure, which is commonly experienced by outdoor workers in the warmer months of the year. 7 Heat-related illnesses include cramps, heat stroke, fatigue, heat exhaustion, heat shock, and heat stroke. 8 Jackson and Rosenberg (2010) suggest heat stress is associated with occupational injuries due to physical discomfort, altered behaviour, and fatigue. Sun exposure is often accompanied by heat exposure, and therefore investigating the exposures together assists in the broader picture of occupational health and safety. Young workers, who often fill seasonal roles, may experience higher levels of heat exposure through seasonal work, such as agricultural/farm work. 9
Due to less work experience and lower education levels, young workers often obtain jobs in industries associated with high risk of hazardous exposures, including exposure to heat and solar UVR.10,11 Exposures at this age are particularly important because young workers may be more biologically vulnerable and because they have potentially more years of hazardous exposure and years during which long latency diseases, such as cancer, can develop. 12 Evidence shows that young workers are at higher risk of occupational injury.13–15 The factors that contribute to increased injury among young workers can also contribute to increased hazardous exposures (e.g., inadequate training and personal protective equipment use16,17). 11
While there may be misconception about the risks of heat stress and negative impacts of solar UVR in Canada and the United Kingdom compared to other countries closer to the equator, these risks are increasing with a changing climate and there is no region of either country that is without risk of exposure.18,19 For example, elevated mortality risks have been observed during events of extreme heat in Canada, both for non-accidental and respiratory causes. 18 In Canada, an estimated 4500 non-melanoma skin cancer cases each year have been attributed to workplace solar UVR exposure. 20 The high diagnosis rates, high health care expenses suggest significant concern to address this highly preventable cancer.21,22
Public risk perception of skin cancer remains relatively low, and the lack of understanding of risk associated with unprotected exposure to UVR is crucial in reducing incidence.23,24 Existing literature suggests that adolescent understanding of skin cancer risk remains low, and the risk of sun exposure is often downplayed. 25
Solar UVR and associated heat is not a hazard that can be eliminated for outdoor workers. However, effective protective behaviours to limit solar UVR and heat exposure exist, including seeking shade, avoiding peak UVR hours of the day, wearing protective clothing including sunglasses and wide-brimmed hats, applying, and reapplying sunscreen, staying hydrated, and checking the UV index when planning outdoor activities.2,26 To our knowledge, a study examining young workers’ understanding of occupational sun safety, specifically, has not been conducted in Canada nor the UK.
The aim of the overall study of which the present analysis is a part was to assess young peoples’ awareness and self-reported practices about hazardous exposures in the workplace in Canada and the United Kingdom. 27 We were primarily interested in young workers in Canada, but the survey platform we used had a relatively small number of prospective young people available to respond, so we added the UK to increase participation from a country with a similar climate and demographic profile to Canada. We also asked a series of sun safety-related questions of only those respondents who reported working outdoors on an average workday; the present paper focuses on this subset of the respondents, from both Canada and the UK. We also invited a randomly selected group of those survey respondents from Canada (for ease of scheduling) who answered the outdoor worker sun safety questions to participate in a focus group to further explore their experiences with sun safety at work. The present study aimed to assess young workers’ understanding of sun-related hazards and associated sun safety practices in the workplace, using responses from the survey and focus group discussions.
Methods
Data source #1: Survey
In October 2021, we conducted a survey on young workers’ understanding of hazardous exposures in their workplace. The survey developed for the purposes of this study used a variety of previous study instruments, including questions about personal protective equipment use for sun safety and beliefs about hazards like carcinogens, along with a review of studies that have sought to understand the barriers and facilitators for workplace health and safety among young workers.11,28–31 The survey was administered through the Prolific platform,32,33 which offers surveys to respondents through their online platform. Participants were pre-screened for residence (Canada or the United Kingdom), age (18–25 years), and employment status (either currently hold or previously held a full or part-time job. A sex-balanced sample was sought, an approach offered within the Prolific platform at the time of survey administration. With this approach, the survey was run once among females and once among males, run within two days of one another. Once participants provided informed consent, they were prompted to complete the survey on the Qualtrics platform, 34 a copy of which is included in Appendix 1. The study was approved by the Health Research Ethics Board of Alberta's Cancer Committee (HREBA.CC-19-0462).
35–37Section one of the survey inquired about general understanding of hazardous exposures in the individual's current position (or if unemployed, their previous job). Section two of the survey was only asked of those who reported working outside (i.e., they reported anything but 0 h outdoors on a typical workday). We had no exclusion criteria for length of time spent in an outdoor job; anyone with any outdoor work time was asked the sun-related questions. The third section of the survey collected brief demographic information from each participant. Personal risk factors for skin cancer, including lighter eye, hair and skin colour, were assessed in demographic questions in the survey, since these may influence people's understanding of their own risk of skin cancer.35–37 For privacy reasons, no unnecessary information from the participants was collected or kept by the research team, including any personal identification in the survey system.
Data on individual sun and heat protection practices were collected via Likert-scale answers (never, rarely, sometimes, often, always practiced) and later converted to a five-point ordinal variable ranging from 0 (never using the protective practice) to 4 (always using the protective practice), based on methods used in previous studies from our team.29,38 Sun and heat protection practice scores were calculated by averaging the five-point scores across answers to the sun and heat questions, leading to scores in the range of 0 to 4. Sun Protection Practice Scores I (or, sun scores) were calculated from answers to questions on wearing sunscreen, a sleeved shirt, a wide-brimmed hat, sunglasses, and seeking shade. Extra questions on UV protective clothing and solar UV index were added to Sun Protection Practice Scores I questions to compute Sun Protection Practice Scores II (or, sun score II). Answers to questions on taking rest breaks and seeking air-conditioned rest areas, scheduling most strenuous work to cooler times of the day, minimizing overheating activities, and checking humidex ratings were used to calculate Heat Protection Practice Scores (or, heat scores).
Data source #2: Focus group
From the survey participants who indicated at least some outdoor work, a sub-set of participants were invited to participate in focus groups. This was limited to Canadian participants due to scheduling logistics. When respondents participated in the survey, they had the option to indicate they were open to being contacted for follow up. A call for participants, including focus group dates and times, was posted to the survey respondents’ subgroup on Prolific, and closed when it reached 20 participants. In the virtual focus group, after being reminded of the purpose and consenting to participate and be recorded, participants were asked to answer a series of open-ended questions for qualitative content analysis 39 . Audio was recorded and transcribed by Zoom. Transcriptions were reviewed by MD, RD, and EQ to ensure accuracy.
Data analysis
Descriptive analysis such as means, standard deviations, and percentages were used to summarize participants’ demographic, and job experience variables from the survey. Industry (sector) and occupation were classified according to the 2012 North American Industry Classification System (NAICS), and 2016 National Occupation Classification (NOC), respectively. Some of the classifications were combined into similar groups because of smaller group sizes.
Differences in sun and heat protection practice scores among outdoor workers (>0–1 h vs 2 + hrs), industries, and occupations were tested using Analysis of Variance (ANOVA) test. Two-sided p-value less than 0.05 was considered statistically significant. Chi-square analysis was used when grouping Likert scale responses. Multiple linear regression was used to model the predictors of sun and heat protection practice scores. The following explanatory variables: age, gender, country of residence, skin type, hair and eye colour, job status, years on job, tanning time, hours worked outside, and job and industry titles were considered in the initial model. Backward stepwise selection was used to arrive at the final model, leaving those variables in the model where p-values were below 0.2. All analyses were conducted using STATA 14.2 software (33).
Qualitative content analysis, a method used widely in health research, was used to better understand young workers’ perspectives about outdoor occupational exposures gathered from the focus group discussion, focused on solar ultraviolet radiation 39 While some anticipated themes were developed a priori, this approach also permitted themes to emerge throughout analysis. Our analysis team (RD, EQ) independently identified themes developed a priori (Supplementary Figure 1). Coding conflicts were resolved in a coding meeting, and any unresolved content was resolved by a third reviewer (CP). Unique comments deemed valuable in the context of the interviews were recorded separately and evaluated by coders.
Coding categories of comments made by focus group participants were tabulated for percent of coverage in responses. Themes were assessed for frequency across responses and nodes per interview question. Unique statements were recorded to include in the discussion of the paper.
Results
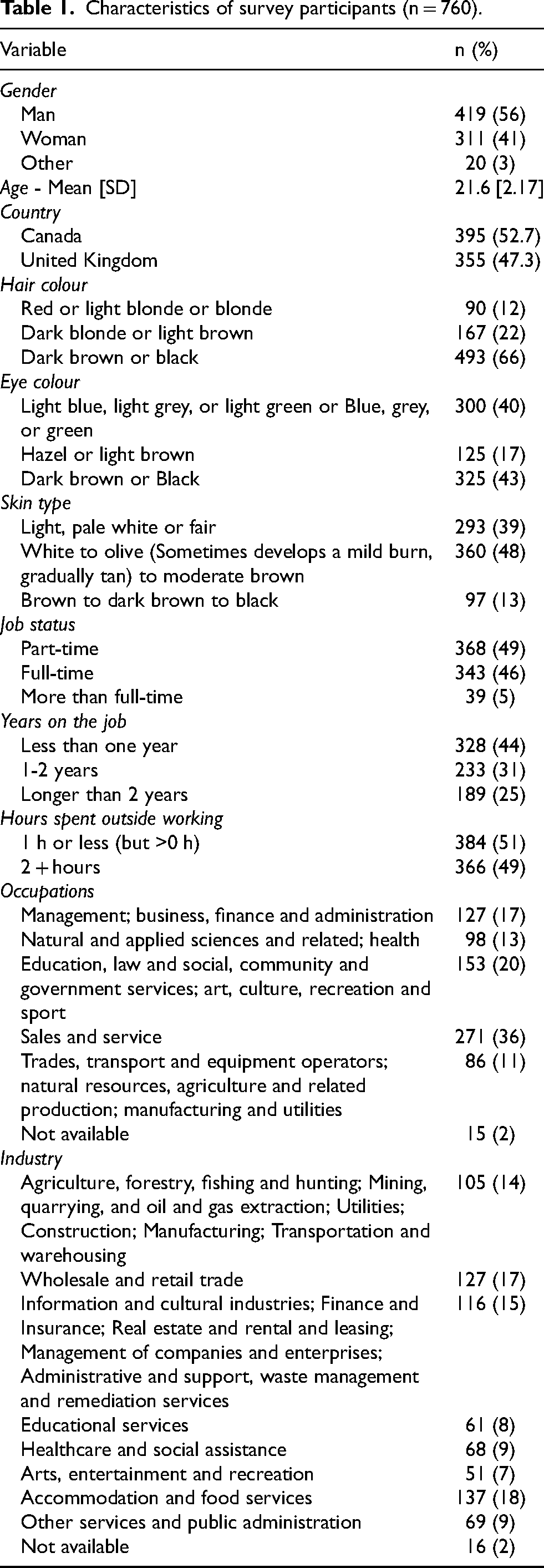
Among survey respondents (n = 1839), 760 reported working outside (i.e., they chose anything but 0 h per day outdoors for that survey question) and had complete data, of which 366 reported working outside for two hours or more (Table 1). The average age of respondents who worked outdoors was 21.6 years. Respondents equally reporting having blue/green/grey eyes and dark brown or black eyes. They primarily had dark brown or black hair (66%), white to olive skin (48%), and were working less than one year on the job (44%). The main industries of employment were accommodation and food services (18%), followed by wholesale and retail trade (17%). Respondents primarily held sales and service occupations (36%) followed by occupations in education, law and social, community and government services; and art, culture, recreation, and sport (20%).
Characteristics of survey participants (n = 760).

Personal protective equipment (PPE) and other protective measures provided by employers varied, 639 of the 750 respondents (85%) reported provision of drinking water at work, followed by air-conditioned rest areas (57%), and canopies or shade structures (41%) (Figure 1). Of note, the most frequently employer-provided measures were primarily preventive for heat illnesses, rather than solar UVR exposure reduction. The least commonly provided PPE were neck flap or brim attachments for hats (7%), wide-brimmed hats (13%), and sunscreen (21%). Almost a third of respondents reported that employers provided the option to reschedule work to cooler times of day (Figure 1).
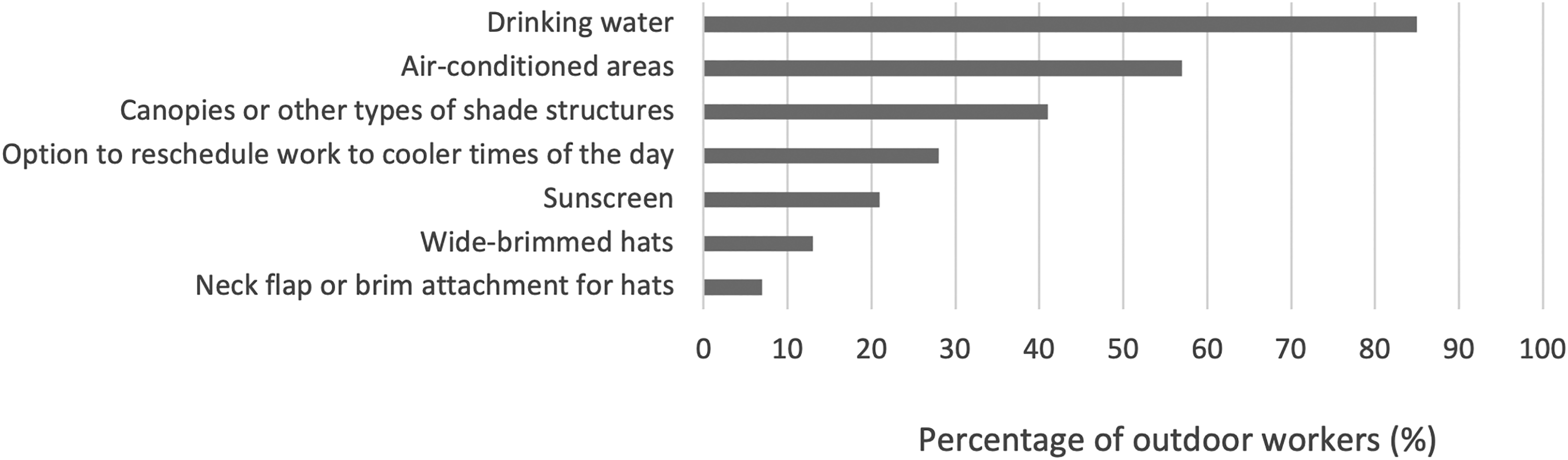
Percentage of outdoor workers (n = 760) by type of personal protective equipment or other protective measures provided by employers.
Few respondents received any form of sun safety training at their current job, both among those working one hour or less outdoors (n = 28, 7.3%) and those working two hours or more outdoors (n = 78, 21.3%).
Sun safety awareness: True/false questions and fact checks
Encouragingly, most participants responded ‘false’ to the question about exposure to solar UVR having only short-term consequences (n = 707, 94%). Nearly all (n = 736, 97%) participants knew that solar UVR can cause cancer, and 727 (97%) knew that skin cancer can be fatal. Participants also correctly understood that solar UVR is still a concern on days that are not sunny (n = 670, 89%). A majority (n = 638, 85%) of participants knew that that sunscreen needs to be applied multiple times over the day.
For the most part, participants were aware that the sun can cause skin cancer (n = 710, 95%), sunburn (n = 707, 94%), sunspots (n = 597, 80%), skin wrinkling (n = 564, 75%), suntan (n = 479, 64%), eye damage leading to impaired vision (n = 465, 62%), freckles (n = 409, 55%), and cancer in or around the eyes (n = 372, 50%), but knowledge of cataracts being a result of sun exposure was only correctly identified by 253 (34%) of participants.
When asked about the most effective skin cancer prevention method, few participants selected the correct answer seeking shade, (n = 134, 18%). Others selected wearing sunglasses (n = 5, 1%), wearing protective clothing (n = 146, 19%), applying sunscreen (n = 199, 27%), and the idea that all options provide the same degree of protection (n = 266, 35%). When asked about hours of the day most at risk of a sunburn, 479 (64%) of participants selected the correct answer for Canada and the UK (11 a.m. to 3 p.m.), followed by the selection of 2 p.m. to 6 p.m. (n = 216, 29%). Few participants selected the other options; 8 a.m. to 12 p.m. (39, 5%) or none of the above (16, 2%). Nearly all participants (697, 93%) correctly identified the definition of UV index (a measure of the strength of the sun's UV rays).
Sun safety practices in respondents’ workplaces
Respondents reported their degree of agreement with statements about sun safety practices at their own workplaces (Figure 2). A majority (n = 481, 64%) strongly disagreed or disagreed that they received the information they needed to protect themselves from solar UVR at work. Furthermore, 64% reported not being concerned about sun exposure at work. The majority (54%) of respondents did not believe that their workplace sun exposure will increase their risk of cancer, although most (62%) agreed that “the right equipment and supplies” reduces solar UVR exposures at work. A strong belief that applying sunscreen adequately protects against harmful solar UVR exposure (76%) was reported among respondents, though approximately half (50%) agreed that they enjoy looking tanned.
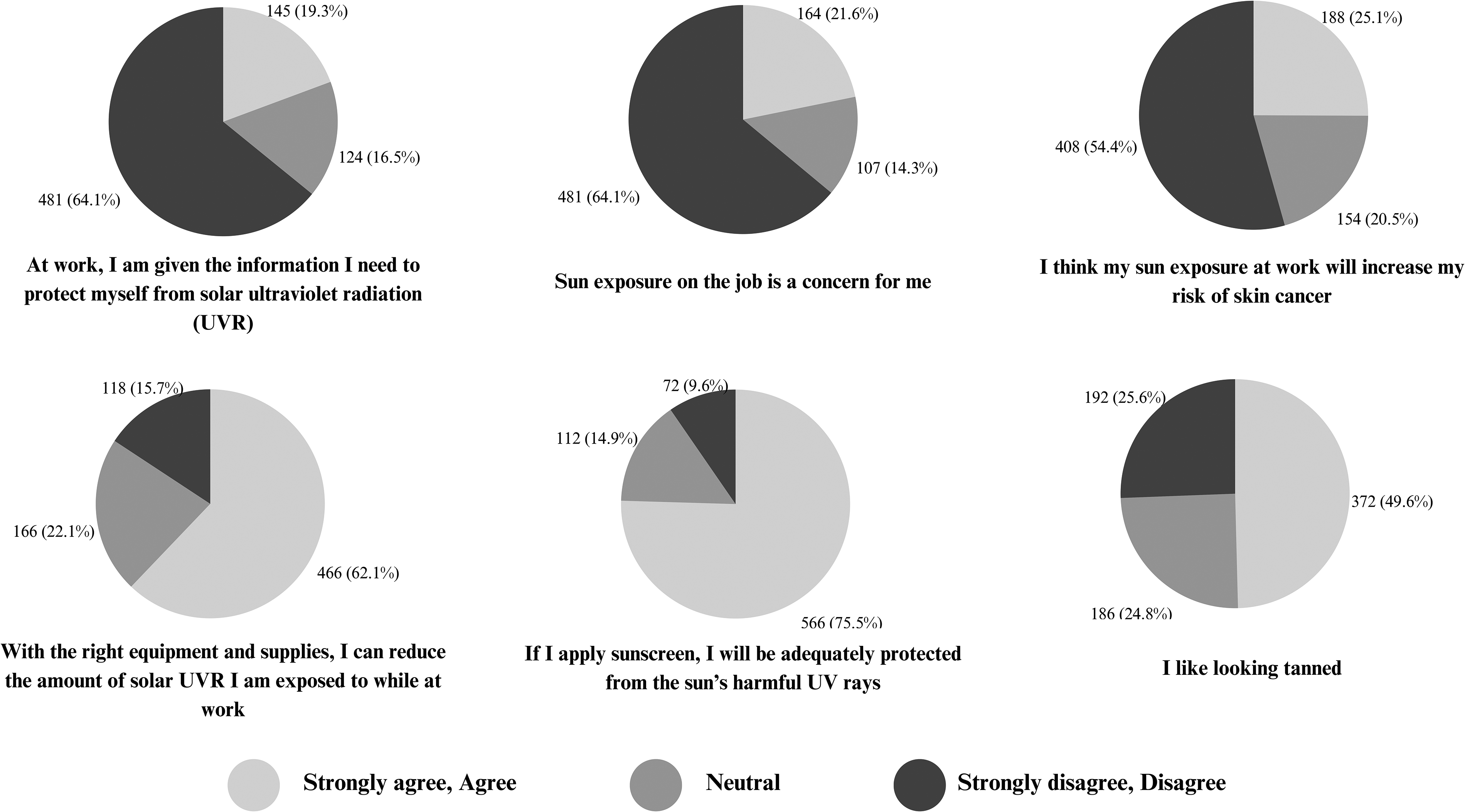
Agreement with statements capturing sun safety attitudes (n = 760).
The most reported reasons for not using sun protection were forgetting to use PPE (66%), it being too hot or uncomfortable to wear long sleeves (43%), not minding getting a tan (31%), and not liking the sticky consistency of sunscreen (27%) (Figure 3). Results by job type showed workers in natural and applied sciences; health; education, law and social, community and government services; and art, culture, recreation, and sport were most likely to report forgetting to wear PPE (approximately 65%) (Table S.1). When examined by industry (NAICS), workers in healthcare and social assistance and arts, entertainment and recreation had the highest rates of forgetting to wear PPE (75%) (Table S.2).
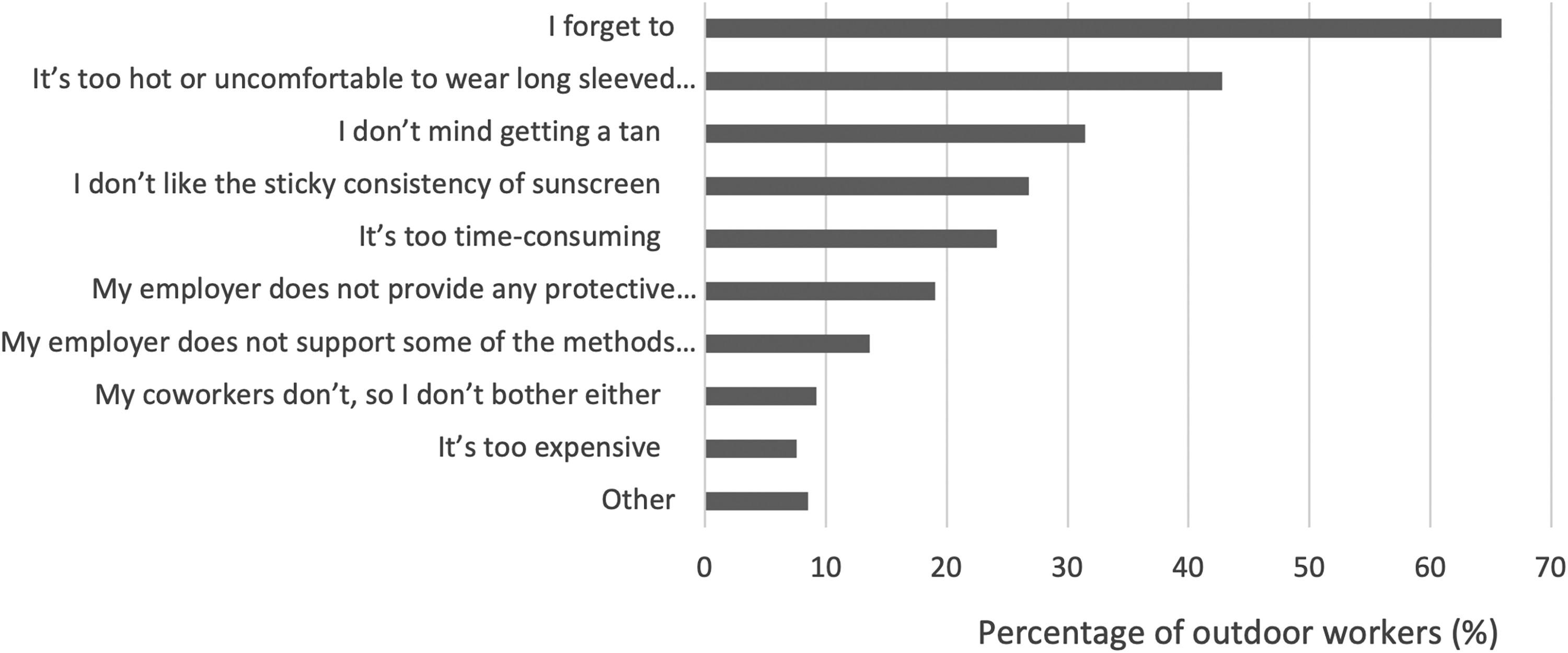
Percentage of outdoor workers (n = 760) by reason for not using sun safety measures.
Sun safety practices: Individual sun protection choices
More people reported never, rarely, or sometimes to wearing UVR protective clothing (92.5%), a wide brimmed hat (90.3%), sunglasses (66.9%), or sunscreen (66.9%); checking the humidex ratings (88.5%); checking the solar UVR index (88.0%); spending time in direct sunlight trying to get tanned (86.7%); scheduling strenuous activity for cooler times of the day (73.3%); minimizing activity in the heat (68.0%); or, seeking shade or air conditioning (61.1%) compared to often or always. When asked about sun-protective practices on a warm sunny day, other questions received a significant proportion of respondents who reported often or always wearing a shirt that covers their shoulders (70.1%). Responses when asked about staying in the shade to avoid sun exposure were split between often/always seeking shade and never/rarely/sometimes seeking shade.
Practice scores for heat and sun protection were low overall, and no differences were detected between outdoor workers working up to one hour, and those working two hours or more, except that those working longer hours outside had higher heat protection scores (score of 1.72, compared to 1.57 in those with up to an hour of outdoor work per day (p = 0.01) (data not shown). When examining sun and heat protection scores by job title (Table S.3), the highest scores were reported by those working in education, law, and arts and culture, as well as those in management and business. Results by industry for the heat and sun protection scores were similar to those by occupation.
Lower scores were found among some hair colour groups (dark brown or black, dark blonde or light brown, compared to red, light blonde, or blonde) (Table 2), which may reflect fairer people taking more precautions due to higher personal risk. Gender, country, and working two or more hours in the sun were found to be predictors of sun and heat protection scores. For model 1 (Heat Protection Practice Score), women and gender-non-conforming people had higher scores than men (beta values were positive, indicating these groups had higher scores). Young workers in the UK had lower heat protection scores than those in Canada, and those working two or more hours outside had higher scores than those working fewer hours outdoors. Model 2 (Sun Protection Practice Score I) also found women to have higher scores than men, lower scores for the UK, and higher scores for those working more hours outdoors. The third model (Sun Protection Practice Score II) found higher scores among women, lower in the UK, and higher scores among those working more hours outdoors, however, these scores were smaller than those of Model 2 (Sun Protection Practice Scores I).
Multiple linear regression results for modeling heat and sun (I and II) protection practice scores.
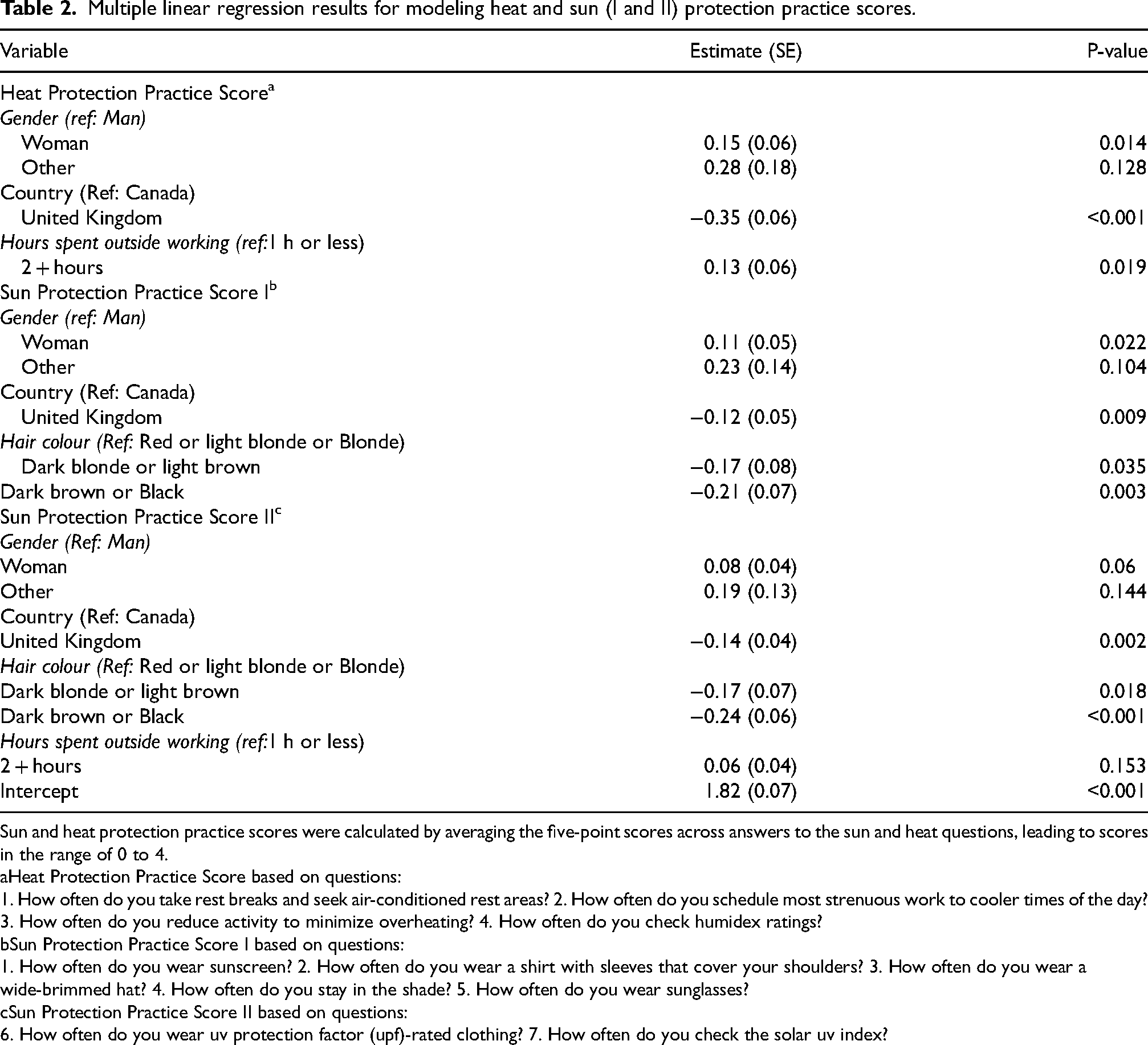

Sun and heat protection practice scores were calculated by averaging the five-point scores across answers to the sun and heat questions, leading to scores in the range of 0 to 4.
Heat Protection Practice Score based on questions:
1. How often do you take rest breaks and seek air-conditioned rest areas? 2. How often do you schedule most strenuous work to cooler times of the day? 3. How often do you reduce activity to minimize overheating? 4. How often do you check humidex ratings?
Sun Protection Practice Score I based on questions:
1. How often do you wear sunscreen? 2. How often do you wear a shirt with sleeves that cover your shoulders? 3. How often do you wear a wide-brimmed hat? 4. How often do you stay in the shade? 5. How often do you wear sunglasses?
Sun Protection Practice Score II based on questions:
6. How often do you wear uv protection factor (upf)-rated clothing? 7. How often do you check the solar uv index?
Focus group
Between thematic coders (RD, EQ), the interrater reliability for themes coded was 94%. All conflicts were resolved without need for third party (CP). Only 13 of the 20 participants recruited for the focus group sessions attended. Only one participant reported being concerned about sun exposure when asked to list workplace exposures. However, when asked specifically about solar UVR concerns, the majority of participants expressed concern (75.0%). The two most common barriers to general PPE use at work were workplace culture and discomfort. Further, only one participant reported sun or heat exposure symptoms from work. Participants reported mostly seeking information about UVR from colleagues (66.7%), discussing solar UVR with employers (75.0%), and suggested better training for workplaces (33.3%). Concerning responses included: “if you get a tan, it's kind of just accepted”, “I was really just doing it for the money, so I don’t care to have conditions improved”, and “I don’t think I’ve ever considered solar exposure and its risks”.
Discussion
Our findings suggest young outdoor workers have moderate levels of understanding regarding workplace sun safety although overall hold negative opinions towards engaging in sun-safe protective practices. These results confirm concerns about young workers’ particular risk of the damaging health effects of occupational sun exposure.14,40 Outdoor workers have higher sun exposure and are at increased risk of harmful solar UVR-related health outcomes 3 ; thus, it is critical to address inadequate understanding of the risk, and the low rates of protective practices that young people are using.
Participants’ responses suggest an understanding of the UV index and some important sun-related health outcomes. Unfortunately, a relatively low proportion of workers were able to identify the highest risk hours for getting a sunburn (approximately two thirds), and awareness of prevention methods was insufficient, with only 18% selecting seeking shade as the most effective practice. Furthermore, awareness of eye-related risks was low, and was reflected in low rates of sunglass use in this sample. A study investigating adolescent knowledge of health risks found that no respondent mentioned avoiding solar UVR peak times. 41 Gaps in knowledge are likely influenced by the poor provision of sun safety information at work, and likely further contribute to inadequate protection measures. Similar findings of outdoor worker risk perception were found by Reeder et al. (2013), with limiting sun exposure being the least common method of protection and pro-suntan themes emerging among responses. 2 A survey study, similar to this one, conducted in Australia found similar results, 42 although reported a higher level of sun safety knowledge. The study also found forgetfulness to be a common barrier to using protection, such as forgetting to wear sunscreen or a long sleeve shirt.
The majority of the survey respondents were not concerned about sun exposure at work (65%), it was interesting to find that despite little personal concern for sun exposure, 62% of respondents indicated that with the right equipment, they can reduce their risk due to exposure at work, suggesting that intervention efforts have the potential to be effective if risks were better communicated to and prioritized among workers. Indeed, previous studies have found unrealistic optimism among youth regarding sun exposure, 41 including the notion that getting a tan is not very risky. 43 Some literature shows youth awareness of skin cancer risks, but little risk prevention action.43,44 A review found the most effective intervention methods of adolescents to move beyond health-based information and utilizing technology, such as the use of appearance-based apps or solar UVR index monitors. 45
Being knowledgeable about solar UVR and its associated risks may not be sufficient in promoting sun safety practices, as reflected in low adoption of sun-safety practices in this study sample. A previous study found that respondents were knowledgeable about the risks of sun exposure but swayed away from protective behaviours by desires supported by social media and attitudes in their peer groups. 46 However, our findings suggest that disagreement with sun safe concepts predicts not engaging in sun safe behaviours, which in turn suggests that shifting attitudes may increase the engagement in sun safe behaviours. Kao et al. 2018 found evidence that sun safe education can influence behaviours surrounding sun safety by route of changing attitudes, suggesting that sun safe behaviours could be shifted by exposure to sun safe education. 47
When asked about reasons for not engaging in sun safe practices, respondents mostly indicated that they forgot (67%), or that the side-effects of using PPE were undesirable (i.e., it's too hot out (43%), or they don’t like sunscreen consistency (27%)). Differences in reasons for not using sun safety practices differed between industries/occupations, which may be related to workplace culture and attitudes or individual worker roles and activities; however, there is minimal literature providing insight into the cause for these differences. Like the findings in our study, literature has shown desire for tanned skin is a barrier to engagement in sun safety practices.2,46 For example, a study assessing young people's attitudes towards tanning found that many respondents felt more attractive with a tan along with low reports of using sunscreen. 46 Acknowledging and addressing barriers, where possible, can be a useful strategy for encouraging sun safety use.
Practice scores suggest differential sun safety practices among our respondents, including by sex and gender. Literature supports this finding and indicates that men report poorer protective practices and are less likely to adopt protective behaviours through intervention. 48 Practice scores also suggest that those who work more hours outdoors reported higher rates of sun safety, similar to previous findings.29,49 Between Canadian and UK participant responses, UK respondents had statistically significantly lower sun and heat protection practice scores than Canadian young workers, especially for the heat protection practice score. This interesting finding may reflect cultural differences in understanding of sun-related risks, in addition to weather and latitude effects. For example, despite having comparable median latitude, Canada's southern border does extend to approximately 42°N, quite a bit further south than the UK's southern border at approximately 50°N. Canada also has more extreme temperatures and is colder in the winter but also hotter in the summer. 50
The culture in many outdoor workplaces does not support sun safe practices, including seeking shade, or wearing appropriate clothing or sunscreen. 2 Culture was listed as a barrier to engaging in sun safe practices at work among the focus group participants. A systematic review noted that among outdoor workers, there is a combination of characteristics that have been found to be associated with reluctance to use sun safety behaviours (e.g., being male, and of low education and adolescent age), which is reflective of our findings. 40 Additionally, young workers belong to a subgroup with its own culture, forming shared beliefs.51,52 These shared beliefs, workplace relationships and a sense of importance in the workplace have been found to influence safety related practices.51,52 Existing literature suggests that the effectiveness of interventions hinges on the attitudes of senior management in an organization. 47 Thus, many authors suggest targeting both individuals and employers to shift attitudes towards wanting to engage and support sun safety practices.
Minimal protective measures were provided by employers, aside from drinking water on site (85%) (which is for heat stress management, not skin cancer prevention), and this was reflected in a low prevalence of safety practices within this sample of young workers. Compared to a study of primarily adult outdoor workers in Alberta, the adherence to sun safety behaviours was lower among this sample of young workers. 29 These behaviours were easily forgotten, missed due to time constraints, or ignored due to reports of dislike or like of equipment. Many of the reported barriers to protection can be managed, for example, by increasing the protective equipment provided by employers, allotting time to apply or re-apply sunscreen and seek shade, and reminders to protect themselves, such as water breaks or watching for heat stress symptoms.
A few limitations of our study should be mentioned. While the survey was developed based on previously used surveys, the survey used for this study was not independently validated. The use of self-completed surveys is accompanied by potential response bias and recall bias, as well as incorrect answers based on understanding of the question. Further, recruitment via the Prolific platform raises the risk of introducing self-selection bias, which may limit the representativeness of the sample. For those who were unemployed at the time of survey completion, there is potential recall bias. Within occupational settings, response bias has been shown to be less likely, as compared to the general population. 53 Due to the method of administering this survey, there is a degree of selection bias given the nature of the individuals who may be drawn to a paying research website (Prolific). 32 Prolific participant recruitment was mainly done through social media platforms, thus excluding those who do not have access or choose to not engage online, though this is less likely to be a concern in our study due to the young age of our respondents. Another limitation of the study is that comparisons of individual location were not made, for example, the province in which an individual lives and is employed was not used as a factor of latitude UVR exposure (including daylength). Workplace culture was used broadly in this study, rather than investigating differences between workplace settings, limiting the extent to which culture could be understood in relation to sun safety knowledge, attitudes, and behaviour.
Another limitation in this study was that the regression models did not account for key confounders that may influence the results, such as detailed employer information and policies, as well as socioeconomic status of the survey participant.
Conclusions
Our study assessed young workers’ understanding of sun-related hazards and sun safety practices in the workplace using a survey and a focus group approach. Participant responses suggest that limited education influences worker attitudes, resulting in poor engagement in sun safe practices.
Future research building a body of evidence on barriers to worker safety may be referenced to support the implementation of workplace safety education, with emphasis on sun exposure for young outdoor workers. Building on the understanding of low engagement in training, risk perceptions, change in safety practices over a career or through aging, and investigating how risk perception may vary by phenotypic vulnerability are all valuable directions to pursue in future research. Further investigation into effective sun safety policies and workplace interventions would assist in identifying the most effective methods of changing sun protection practices among young outdoor workers.
Aligning with current sun safety recommendations, employers should provide reasonable access to PPE provisions in sizes to fit all employees, mandated breaks in shaded areas, and up-to-date improved training focused on sun and heat safety. Tailoring education programs and training initiatives to the gaps and trends among young workers, combined with psychological context, could increase adherence to sun safe practices. Additional research will assist in providing evidence for concrete policy recommendations for safety regulators and employers.
Supplemental Material
sj-docx-1-wor-10.1177_10519815261434382 - Supplemental material for Understanding young adults’ sun safety practices in the workplace
Supplemental material, sj-docx-1-wor-10.1177_10519815261434382 for Understanding young adults’ sun safety practices in the workplace by Emma K. Quinn, Ela Rydz, Anita Brobbey, Robert T. Duffy, Sajjad S. Fazel and Cheryl E. Peters in WORK
Footnotes
Acknowledgements
Not applicable.
Ethical approval and informed consent
The study was approved by the Health Research Ethics Board of Alberta's Cancer Committee (HREBA.CC-19-0462).
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This project was funded by the Derrick Thompson fund, as part of the O’Brien Institute for Public Health Catalyst Funds. Grant # 201907CTF_CPET_1.
Declaration of conflicting interests
The author declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Reporting guidelines
Not applicable.
Data availability
Anonymized data can be made available upon request.
Supplemental material
Supplemental material for this article is available online.
