Abstract
Background
High-quality healthcare relies on competent and prepared nursing professionals. Final-year nursing students play a key role in preventing medical errors, thus ensuring patient safety.
Objective
This study aimed to examine the professional competencies of final-year nursing students, medical error tendency, and the relationship between these variables.
Methods
A descriptive-correlational design was used. Data were collected using the Personal Information Form, Medical Error Tendency Scale in Nursing, and Competency Inventory of Nursing Students. Higher competency scores indicate higher professional competence, while higher scores on the Medical Error Tendency Scale indicate a lower medical error tendency.
Results
Students showed high professional competence (M = 6.22, SD = 0.63) and low medical error tendency (M = 4.52, SD = 0.39). The highest score on the Medical Error Tendency Scale sub-dimensions was in Medication and Transfusion Practices (M = 4.68, SD = 0.34), and the lowest in Patient Monitoring and Equipment Safety (M = 4.29, SD = 0.53). Students scored highest in ethics and accountability (M = 6.43, SD = 0.61) and lowest in clinical biomedical science (M = 5.83, SD = 0.93). A significant positive correlation was found between professional competence and medical error tendency (r = .713, p < .01). Since high scores indicate a lower medical error tendency, it was concluded that as nursing students’ professional competence increases, their medical error tendency decreases. General clinical skills, critical thinking, and ethics significantly predicted medical error tendency.
Conclusions
The study highlights the importance of professional competence in reducing medical error tendencies among nursing students. Enhancing competencies, particularly in clinical skills, critical thinking, and ethics, through competency-based and simulation-supported education can contribute to improved patient safety outcomes.
Keywords
Introduction
Nursing education aims to equip students with the necessary professional competencies before they enter the profession by combining theoretical knowledge with clinical practice to ensure comprehensive preparation. 1 Various competency domains have been identified for nursing students; including communication and interpersonal skills, cognitive knowledge, nursing assessment and quality improvement, professional development, leadership, management and teamwork, and research utilization. 2 The World Health Organization (WHO) emphasizes the importance of all graduating nurse acquiring these competencies and defines clinical competence as the “gold standard” of nursing. 3
Professional competence is crucial not only for individual development but also for ensuring patient safety and improving health outcomes. 4 Therefore, nursing education should aim to prepare professionals capable of delivering safe and high-quality care in increasingly complex healthcare environments. 5 Although some studies report that nursing students perceive their competencies as high prior to graduation,6,7 these self-assessments may decline over time, particularly during the transition to professional practice. 2 Several studies have shown that newly graduated nurses often struggle to apply these competencies effectively in real clinical settings. 8 The literature highlights that nursing students exhibit deficiencies not only in technical skills but also in areas such as critical thinking, communication, teamwork, supportive roles, and professionalism. 9 Moreover, it is emphasized that the ability of of newly graduated nurses to provide high-quality and safe care are not at a satisfactory level. 10 As the largest group of healthcare professionals, nurses spend more time with patients than any other health worker 11 and meet the patient's care needs by taking part in various stages of the treatment process. Therefore, it is evident that professional competence is not merely a matter of individual achievement, but a critical factor that directly influences the quality and effectiveness of healthcare services.
Medical errors remain a global challenge, contributing significantly to morbidity and mortality. According to WHO (2019), millions of patients are affected each year. 12 The WHO's Global Patient Safety Action Plan 2021–2030 (2021) aims to eliminate avoidable harm in healthcare, envisioning a world where every patient receives safe and respectful care at all times and places. 13 Medical errors not only compromise safety but also give rise to ethical and legal issues. 14 In this context, understanding the competency levels of nursing students during the transition to professional practice, -as well as the relationship between these competencies and medical error tendency- is of critical importance for educational institutions and healthcare organizations. Nurses, who hold significant responsibilities for patient safety and well-being, are at high risk for committing medical errors. 15 Competence plays a crucial role in preventing such errors and contributes to enhanced patient safety and satisfaction in healthcare settings. 16 Nursing competence is essential not only for reducing medical errors but also for improving the overall quality of care.17,18 Nurses are essential members of the healthcare team; they must exhibit a high level of competence in performing their tasks and responsibilities to reduce the number of medical errors.16,19 Conversely, negligence and malpractice may be seen indicators of insufficient or inadequate competence.
Previous studies have shown a correlation between a nurse's level of competence and their medical error tendency. 19 Especially final-year undergraduate nursing students stand out as a group that should be focused on this issue because they are at the last stage of their education and are about to begin professional practice. 20
Furthermore, the transition from school to clinical practice presents certain challenges that may increase medical error tendency. According to the research findings, newly graduated nurses frequently lack the critical thinking skills required to provide expected care, resulting in limited competences that may compromise patient safety.21,22 In contrast, some studies have also reported that nursing students exhibit low medical error tendency,23,24 highlighting the need to further investigation into the the relationship between professional competence and medical error tendecy.
Although previous studies have examined the relationship between sociodemographic variables and professional competence among pre-graduation nursing students, 6 the issue of medical errors committed by senior nursing students remains insufficiently explored. However, high-quality healthcare directly depends on the competenc level of final-year students who are preparing for professional clinical practice. The way are students are prepared during this critical stage is a key factor influencing patient safety outcomes and the prevention of medical errors.25,26
This study aims to determine the relationship between professional competence and medical error tendency among final-year nursing students. By identifying which professional competencies are associated with medical error tendency, educational institutions and healthcare organizations can tailor their training programs to better develop these critical skills.
For this purpose, the following research questions were addressed:
What is the level of professional competence of final-year nursing students? What is level of medical error tendency of final-year nursing students? Is there a relationship between the sociodemographic characteristics of final-year nursing students and their level of professional competence? Is there a relationship between the sociodemographic characteristics of final-year nursing students and their medical error tendency? Is there a relationship between the level of professional competence and medical error tendency among final-year nursing students?
Methods
Design, setting and participants
This was a descriptive-correlational study, with the sample comprising all final-year nursing students (n = 155) enrolled at a university in western Turkey during the 2023–2024 academic year. The sample included 125 students who met the inclusion criteria of the study. The study's inclusion criteria were: (a) voluntary participation; (b) enrollment in a senior internship course; and (c) completion of all data collection forms. A descriptive-correlational design was chosen because it allows the researchers to both describe the current levels of professional competence and medical error tendency among final-year nursing students and examine the associations between these variables and selected sociodemographic factors. This non-experimental design was deemed appropriate for identifying relationships without manipulating variables.
The nursing internship program included 24 h weekly clinical training across various wards during the fall and spring semesters of the fourth year (a total of 28 weeks). Students provided patient care under supervision of nurses, developed care plans, and discussed them with clinic lecturers. Weekly audits and group discussions were conducted in each ward.
Data collection tools
The data were collected using the Personal Information Form, Medical Error Tendency Scale in Nursing (METSN), and The Competency Inventory of Nursing Students (CINS).
Personal information form
The Personal Information Form included questions on age, academic average, gender, experiences with medical errors (encountered or made), clinical practice area, satisfaction with studying in the nursing department, and self-perceived competence.
Medical error tendency scale in nursing
The scale, created by Özata and Altunkan (2010), is designed to evaluate nurses’ tendencies toward medical errors. 27 It consists of 49 items across 5 sub-dimensions: medication and transfusion administrations (18 items), hospital infections (12 items), falls (5 items), communication (5 items), and patient monitoring and equipment safety (9 items). The scale uses 5-point Likert format, and each item receives a score between 1-never and 5-always. The mean score is used to evaluate responses. The total possible score ranges from 49 to 245. Higher scores indicate a lower medical error tendency, while lower scores indicate a higher tendency. The scale does not include reverse-scored items. Özata and Altunkan 27 reported a Cronbach alpha of .95 for the original scale, and the same internal consistency coefficient (.95) was obtained.
The competency inventory of nursing students
This 7-point Likert-type scale was developed by Hsu and Hsieh (2013) and includes 43 items organized into six sub-dimensions: clinical biomedical science, general clinical skills, critical thinking and reasoning, caring, ethics and accountability, and lifelong learning. Higher scores indicate greater competence; with total scores ranging from 43 to 301. 28 The Turkish adaptation by Ülker and Korkmaz (2022) demonstrated high reliability (Cronbach's α = 0.978). 29
Data collection
Data were collected via a questionnaire between April and June 2024, following the approval of the ethics committee and relevant institutional permissions. The study was explained to the students during breaks between courses and assesment and those who volunteered to take part in the study gave their written consent. Participants were informed that the data collected would be used solely for scientific research purposes and that their identities would remain confidential. Students were given the data collection tools, and their completed forms were cellected. Completing the questionnaires took approximately ten minutes.
Statistical methods
SPSS 24.0 (Statistical Package for Social Science; Chicago, IL, USA) program was used for data analysis. The Kolmogorov-Smirnov test and 95% confidence intervals were used to assess the normality of data distribution. Descriptive statistics were presented as frequencies and percentages. To ascertain whether the sociodemographic traits and total scale scores differed in any manner, a one-way multivariate analysis of variance (MANOVA) was performed. Normality, linearity, the detection of univariate and multivariate outliers, the homogeneity of variance-covariance matrices, and the lack of multicollinearity were all confirmed before doing MANOVA. No significant violations were identified in these assumptions. The relationships between total scale scores and subscale scores were analyzed by Pearson correlation analysis and stepwise regression analysis. A significance level of p < 0.05 was accepted.
Ethical considerations
The University's Non-Interventional Research Ethics Committee granted ethical approval (E-60116787-020-523666, dated 30.04.2024 and numbered 08). Participant's consent was obtained prior to data collection, and written explanations of the study's purpose and methodology were provided. This study adhered to the guiding principles of the Declaration of Helsinki.
Results
Fourteen students provided incomplete responses to the data collection tools, while sixteen students refused to participate. The participation rate was 80.64%.
Most participants were female (78.4%), with a mean age of 22.50 ± 0.93 years. It was found that 82.4% of the students had academic achievement levels between B1 and B3 (grade point average is between 2.75–3.49 out of 4.00). Over the half of the students reported being satisfied with studying in the nursing department (53.6%). Among the students surveyed, 8.8% reported not perceiving themselves as competent nurses, while 17.6% expressed a lack of confidence in their nursing skills. While 50.4% of the students stated that they had encountered medical errors during clinical practice, 29.6% admitted to having made medical errors (Table 1).
Descriptive characteristics of nursing students (n = 125).
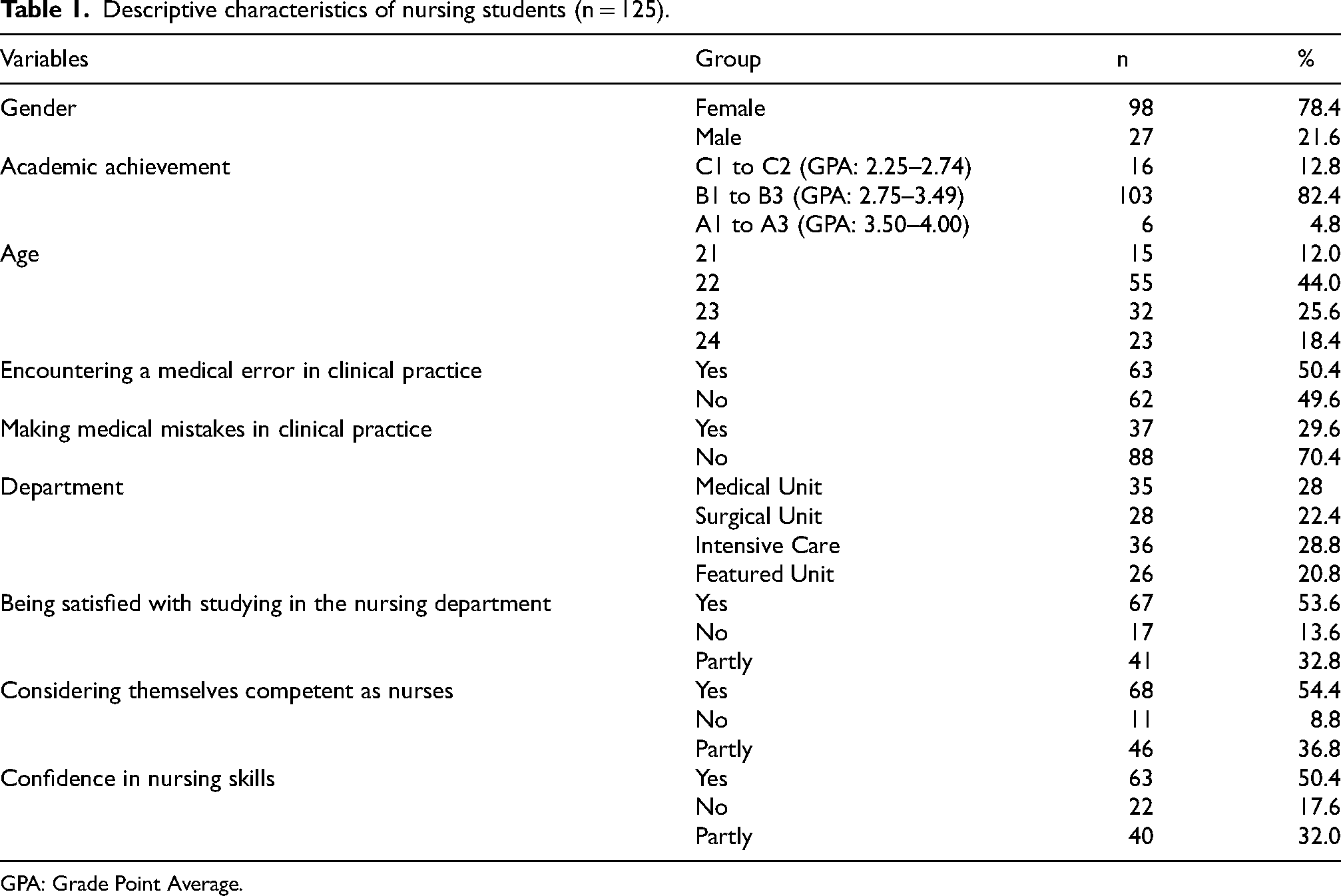

GPA: Grade Point Average.
The mean total score of the participants in the CINS was 6.22 ± 0.63, indicating a high level of competency. Among the sub-dimensions, ethics and accountability had the highest mean score (6.43 ± 0.61), while the clinical biomedical science had the lowest (5.83 ± 0.93). The total mean score of the METSN was 4.52 ± 0.39, indicating a low medical error tendency among nursing students. The Patient Monitoring and Equipment Safety sub-dimension had the lowest mean score (4.29 ± 0.53), whereas the Medication and Transfusion Administrations sub-dimension had the highest (4.68 ± 0.34) (Table 2).
Nursing students’ mean scores on medical error tendency scale in nursing and the competency inventory of nursing students (n = 125).
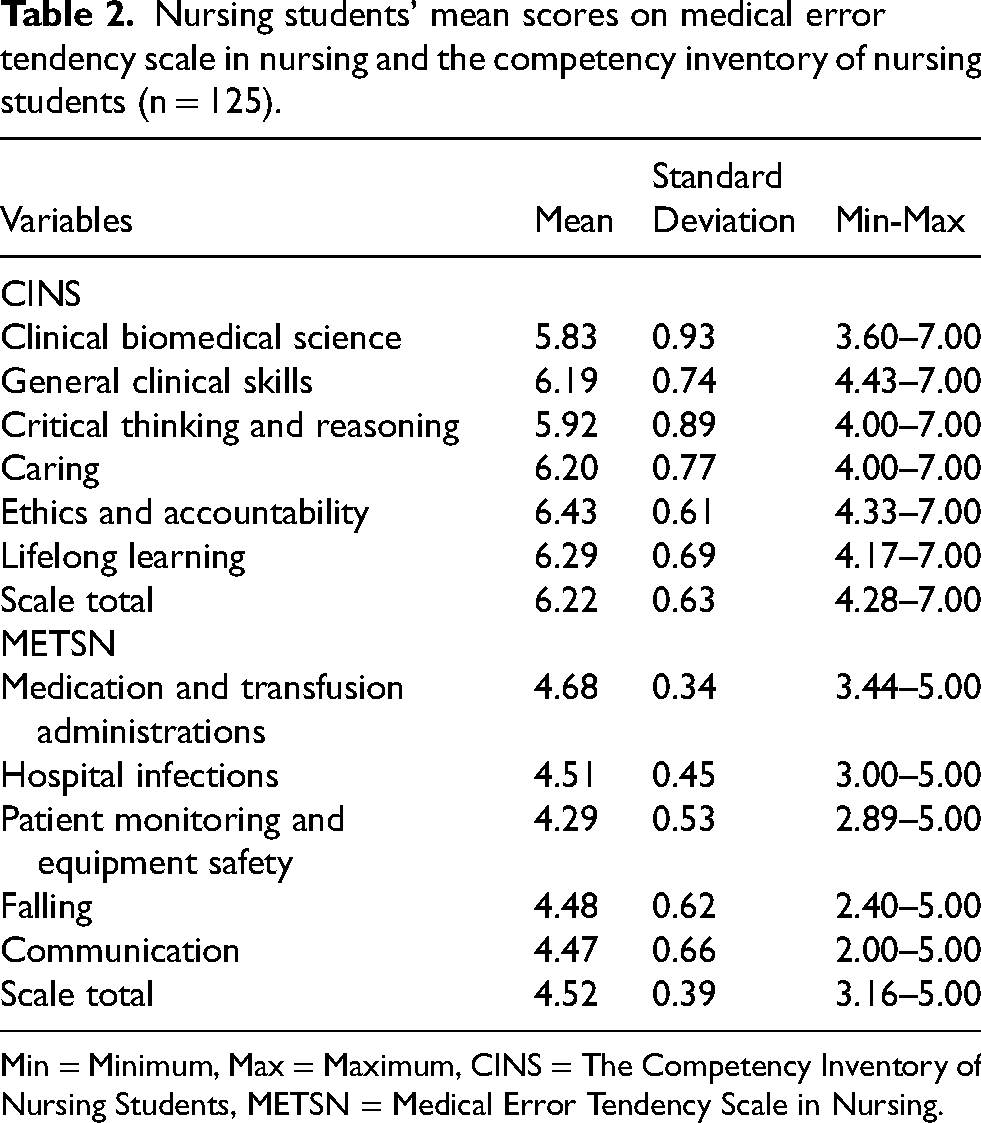
Min = Minimum, Max = Maximum, CINS = The Competency Inventory of Nursing Students, METSN = Medical Error Tendency Scale in Nursing.
The examination of core competency, and medical error tendency scores by the students’ demographic characteristics using MANOVA was presented in Table 3.
MANOVA analysis of the competency inventory of nursing students and medical error tendency scale in nursing according to nursing students’ descriptive characteristics (n = 125).
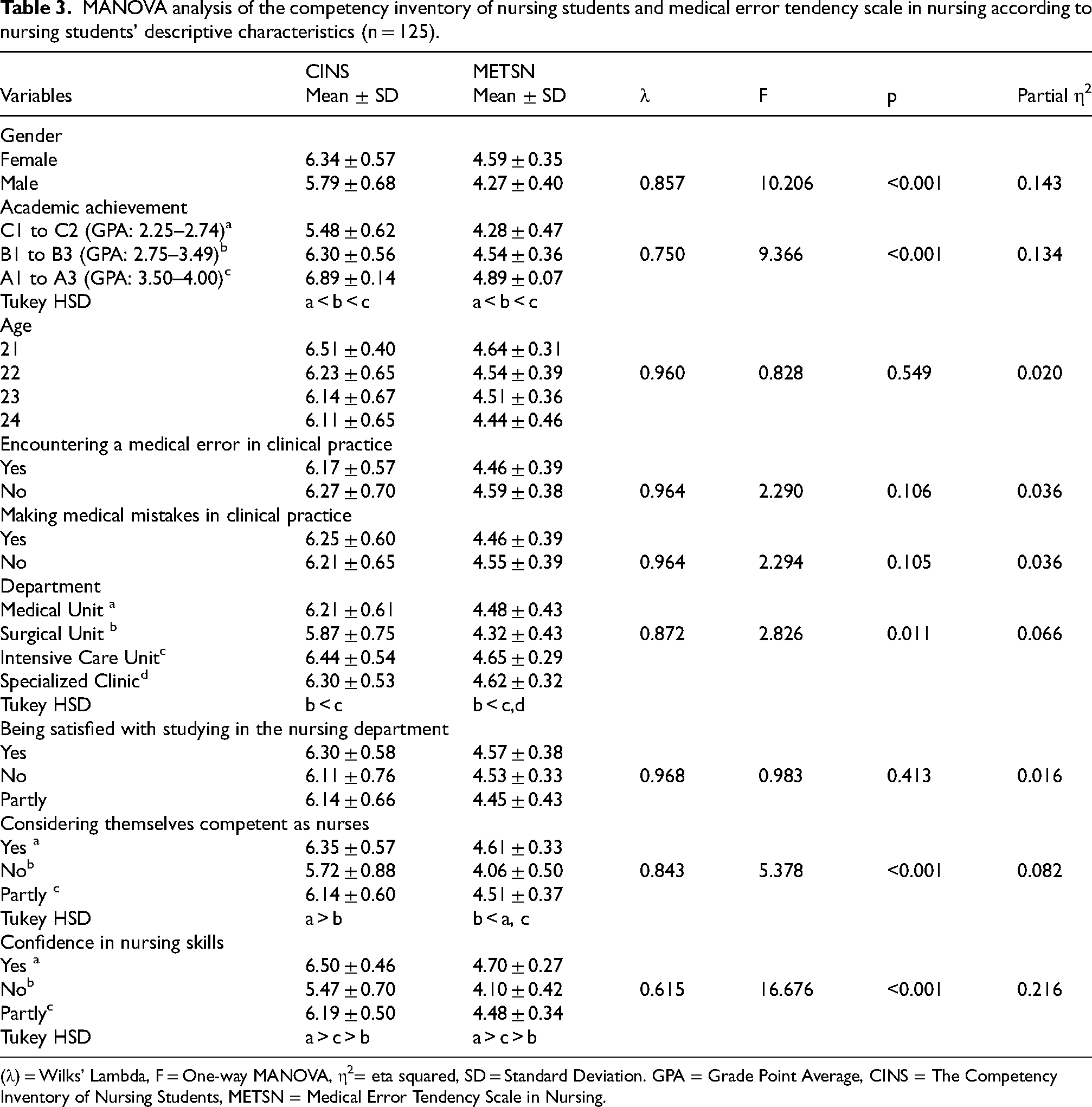
(λ) = Wilks’ Lambda, F = One-way MANOVA, η2= eta squared, SD = Standard Deviation. GPA = Grade Point Average, CINS = The Competency Inventory of Nursing Students, METSN = Medical Error Tendency Scale in Nursing.
The results of the one-way MANOVA revealed a significant difference in core competency, and medical error tendency based on gender (Wilks’ Lambda (λ) = 0.857; F = 10.206; p < 0.001; Partial η2=0.143). Female students were found to have higher scores in both core competency, and medical error tendency (p < 0.001) (Table 3).
The one-way MANOVA test results showed a significant difference in core competency, and medical error tendency scores based on academic achievement (Wilks’ Lambda (λ) = 0.750; F = 9.366; p < 0.001; Partial η2=0.134). According to the Tukey Honestly Significant Difference (HSD) test results, students with high academic achievement (A1 to A3) had significantly higher scores in both core competency, and medical error tendency than those with lower academic achievement (p < 0.001) (Table 3).
Significant differences were found in core competency and medical error tendency scores based on the clinical practice department (λ=0.872, F = 2.826, p = 0.011, Partial η2=0.066). Students in the Surgical Unit (M = 5.87, SD = 0.75) had lower scores than those in the Intensive Care Unit (M = 6.44, SD = 0.54) on the Nursing Students’ Competency Scale. According to post hoc Tukey HSD tests, students in the Surgical Unit (M = 4.32, SD = 0.43) also scored lower on the METSN than those in the Intensive Care Unit (M = 4.65, SD = 0.29) and in specialized clinics (M = 4.62, SD = 0.32) (Table 3).
Significant differences were determined in levels of core competency and medical error tendency based on students’ self-perceived competence as a nurse and nursing skills. Students who perceived themselves as competent as nurses (Wilks’ Lambda (λ) = 0.843; F = 5.378; p < 0.001; Partial η2=0.082) and rated their nursing skills as competent (Wilks’ Lambda (λ) = 0.615; F = 16.676; p < 0.001; Partial η2=0.216) had significantly higher scores in both core competency and medical error tendency (Table 3).
The results of Pearson correlation analysis between the CINS and METSN are presented in Table 4. A significant positive correlation was found between professional competence and medical error tendency (r = .713, p < 0.01). As higher scores on the Medical Error Tendency Scale reflect a lower likelihood of making medical errors, this finding suggests that an increase in professional competence is associated with a decrease in the tendency to make medical errors.
Correlation analysis of the competency inventory of nursing students and medical error tendency scale in nursing (n = 125).
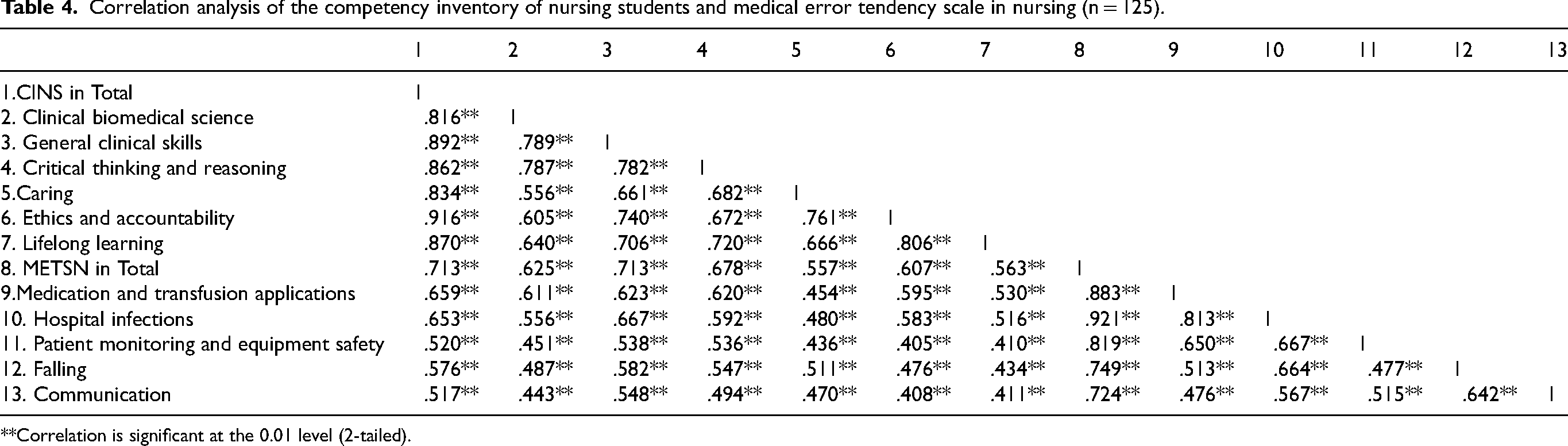
**Correlation is significant at the 0.01 level (2-tailed).
Significant positive correlations were also found between the total professional competence scores and all sub-dimensions of the Medical Error Tendency Scale. Specifically, higher competence levels were associated with higher scores in medication and transfusion practices (r = .659), hospital infections (r = .653), patient monitoring and equipment safety (r = .520), falls (r = .576), and communication (r = .517) (p < 0.01 for all). These findings reinforce the idea that greater professional competence is linked to a reduced tendency to make medical errors (Table 4).
Stepwise multiple regression analysis was conducted to identify predictors of medical error tendency, with the disposition to commit medical errors as the dependent variable and the six sub-dimensions of the competency scale as independent variables. The model explained 54% of the variance. General clinical skills (B = 0.401, p = 0.000), critical thinking and reasoning (B = 0.234, p = 0.014), and ethics and accountability (B = 0.187, p = 0.034) were identified as significant predictors. Multicollinearity diagnostics indicated acceptable tolerance and Variance Inflation Factor (VIF) values for all predictors (all VIFs <2), suggesting no serious multicollinearity concerns (Table 5).
Multiple regression analysis results of the medical error tendency scale in nursing (stepwise method.).
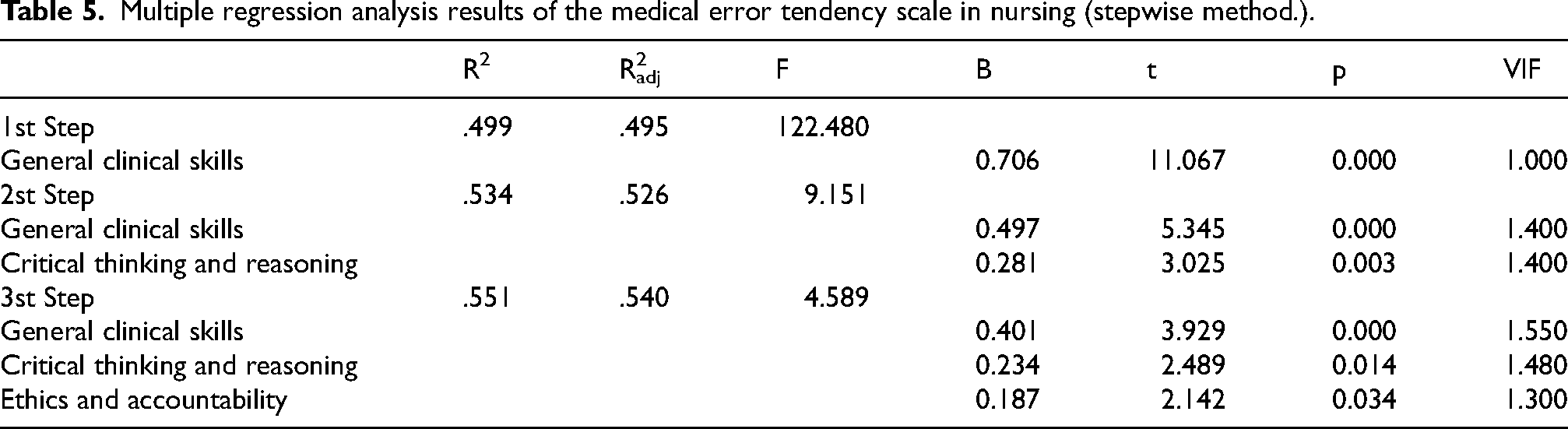
Discussion
The aim of this study was to explore the relationship between the professional competence levels of final-year nursing students—an important measure of the effectiveness of undergraduate education—and their medical error tendency.
The study found that the majority of final-year nursing students exhibited high levels of professional competence and viewed themselves as competent nurses. Notably, students scored highest in the ethics and accountability sub-dimension of the Competency in Nursing Students Scale, consistent with findings from other studies.28,29,30 Hsu and Hsieh (2013) emphasized that ethics and accountability are key factors contributing to nursing students’ over all competence. 28 In a similar vein, a scoping review examining the competencies expected of undergraduate nursing students, emphasized the significance of knowledge in health ethics, adherence to professional nursing ethical standards, and the integration of ethical values into clinical practice. 31 A novice nurse's ethical understanding and sense of accountability can be developed through clinical practice and by observing professional role models. 28 The emphasis on ethics in both coursework and clinical practice at the study instution likely contributed to the students’ high scores in the ethics and accountability sub-dimension. Conversely, students scored lowest in the clinical biomedical science sub-dimension, consistent with previous studies,28–30 indicating perceived inadequacy in areas such as anatomy, physiology, and clinical testing. This may stem from various factors including the limited application of biomedical knowledge in clinical practice, 32 the quality and consistency of support provided to students, limited learning opportunities, inconsistencies in how the prioritization of biomedical sciences during clinical placements, and the fact that mentors in these settings may not universally recognize the importance of this knowledge. 33 Furthermore, the predominance of care-centered roles in clinical practice may limit students’ focus on biomedical knowledge. Therefore, incorporating case-based formats into biomedical science curricula 34 and integrating these courses with clinical practice through methods such as simulation, may enhance nursing students’ biomedical science knowledge, thereby support the delivery of safe, evidence-based care.
In this study medical error tendency of final-year nursing students was low. In the literature, it is reported that nursing students23,24 and final-year nursing students14,35 generally exhibit low medical error tendency, and this is consistent with the findings of the present study. This situation may have been influenced by the sensitivity and meticulousness of final-year nursing students to ensure and maintain patient safety, 14 the number of patients they are responsible for is small, they do not keep shifts, and they usually receive support from instructors or clinical nurses during serious practices, 35 which may have affected this situation. Additionally, the continuation of students’ theoretical coursework during their education, which includes topics such as patient privacy, ethics, and the maintenance of a safe care environment, may have contributed to this outcome.
In this study, final-year nursing students had highest medical error tendency in the “Patient Monitoring and Equipment Safety” sub-dimension. Similarly, Türk et al. (2019) reported low scores in this sub-dimension, attributing it to interns’ limited knowledge and experience due to their pre-graduation status and lack of continuous hospital exposure. 14 Karaveli (2020) also noted that restricted practice hours contribute to this outcome. 24 Intern students provide patient care and follow-up alongside nurses. However, nurses are responsible for officially documenting and reporting these processes. Although students observe and assist, their lack of authority to sign or formally record procedures may have influenced the results. Despite their active involvement, equipment safety procedures are carried out by nurses at schedules intervals, depending on the nature of the equipment and device. In some cases, a specific nurse is assigned to manage a particular piece of equipment, further limiting students’ opportunities for hands-on experience. Given these findings, nursing curricula should consider integrating more structured and supervised hands-on training focused specifically on patient monitoring and equipment safety, in order to better prepare students for the technical competencies required in real clinical settings.
In this study, students demonstrated the lowest medical error tendency in the sub-dimension related to medication and transfusion practices. Medication and intravenous fluid constitute a significant portion of the care provided by nurses. Medication errors can cause a number of difficulties for patients, ranging from moderate pain to substantial morbidity, which may lead to increased hospitalization or death. 36 Therefore, medication and transfusion practices are among the topics that are carefully and meticulously emphasized by nurses and educators in theoretical education and clinical practice, and this may have led to this result, as it covers an important area in practice.
This study found that female students demonstrated higher levels of competency and a lower medical error tendecy compared to their male counterparts. Comparable findings have been observed in studies involving nursing students 14 and nurses, 37 which also identified a significantly lower likelihood of medical errors among females. This reduced medical error tendecy may be attributed to greater awareness of such errors among female students, 38 leading to increased caution and control in clinical practice. 39 The current findings regarding nursing students’ competency levels further support this conclusion. Ogunmuyiwa et al. (2025) reported that gender significantly predicted clinical competency, with female students exhibiting higher competency levels. 40 This is further reinforced by evidence indicating that compassionate behavior and critical thinking skills—key elements of clinical competence—are more frequently seen in female students. 41 Additionally, Nilsson et al. (2016) found that female nurses scored higher on items related to value-based nursing principles. 42 Thus, the higher competency levels seen among female nursing students may be influenced by both the inherent characteristics of the nursing profession and the gender roles shaped by societal expectations.
The study's results show that students who intern in the intensive care unit exhibit high levels of competence and a low medical errors tendency. In contrast, students interning in surgical clinics show lower competency and a higher medical error tendency. Similarly, the literature reports that nurses working in surgical clinics have higher rates of medical errors and greater medical error tendency.43,44 The high volüme of both planned and unplanned (like emergency situations) admissions and discharges, the diversity of cases, and the varying nursing care requirements in surgical clinics increase the workload and stress experienced by students, which can negatively affect their clinical performance. 45 Furthermore, high patient density and the insufficient educational opportunities for students may further exacerbate this negative impact. 46 On the other hand, internships in intensive care units provide students to develop the ability to make rapid and effective decisions through direct patient contact in real-life clinical situations; This experiences, prioritizes patient safety and significantly contributes to students’ professional development. Such internship experiences are crucial for improving students’ clinical skills and professional performance, while also boosting their self-confidence, independence, and professional commitment.47,48
Furthermore, those who trusted their professional skills demonsrated higher levels of core competence and a lower medical error tendency. Similar results were obtained in studies researching nursing student competence, and competence levels were found to be good.49,30 In our study, the fact that the students participated in internship practice for 24 h per week (including weekdays and weekends) throughout both academic terms of the fourth year may have influenced these results. Shahzeydi et al. (2022) investigated the internship experiences of nursing students, nurses, and educators, and found that ran increased number of nursing procedures, performing various practices during different shifts, and exposure to a diverse range of patients had a positive impact on the overall this experience. 47 However, it should be noted that students’ perceptions of their competence and medical error tendency were obtained through self-reporting measurements, which may introduce response bias. Additionally, the possible impact of the Dunning–Kruger Effect (DKE) should be taken into account. This cognitive bias suggests that individuals with lower levels of experience or competency are more likely to overestimate their abilities, while those with higher levels of experience may underestimate their own competency. 50
One of the most important findings of this study is that as nursing students’ competence level increases, their medical error tendency decreases. Students with higher competence, supported by strong theoretical knowledge, critical thinking skillss, and practical skills, are better able to anticipate risks, make informed decisions, and respond effectively in clinical situations. Patient safety is directly related to the competence of healthcare professionals, and quality care can only be provided when healthcare professionals have sufficient skills. 51 For instance, Gezer and Alemdar (2024) found that as pediatric nursing competence improves, the likelihood of making medical errors decreases, 52 while Zaitoun et al. (2023) reported a positive correlation between nursing competence and patient safety. 53 The results of this study which show a low medical error tendency among final-year nursing students and its association with professional competence, align with the WHO's emphasis on strengthening healthcare workforce competencies to improve patient safety outcomes. These findings indicate that nursing education should focus not only on theoretical knowledge but also systematic skill development, supervised clinical practice, and interaction with professional role models. Collaboration with clinical nurses, timely feedback, and the integration of case-based learning and simulation exercises can strengthen students’ decision-making abilities, thereby reducing the likelihood of medical errors and enhancing patient safety.
The identification of general clinical skills, critical thinking and reasoning, ethics, and accountability as independent predictors of medical errors in this study offers significant insights for health education and practice. General clinical skills form the basis of patient care. Nurses’ mastery of these skills enables them to make accurate diagnosis and provide effective care. In the study conducted by Mohsenpour et al. (2021), the most common reasons for errors made by nursing students were determined as insufficient clinical skills and inadequate equipment. 54 In this context, the importance of comprehensive clinical skills training, such as orientation programs and simulation-based training, is growing in nursing education. These educational models enable new graduate nurses to be better prepared for complex and intensive care environments and can significantly reduce the risk of medical errors. 55 Zuriguel-Pérez et al. (2015) describe critical thinking as the ability to reflect on one's own reasoning to optimize positive outcomes and reduce errors in decision-making. 56 This process involves students integrating both theoretical knowledge and clinical skills to identify and address patients’ care needs. Zhang et al. (2024) found strong, statistically significant positive relationship between critical thinking skills and medication safety competence. 57 In a study by Bickel et al. (2020) on adverse events during nursing students’ clinical rotations, it was discovered that one of the most common causes of errors was a lack of critical judgment. 58 Nurses who lack clinical judgment skills can threaten the safety of patients. 59 Therefore, incorporating various active learning methods tailored to different learning styles in nursing education may support the development of critical thinking skills and reduce the medical error tendency.
Benner et al. (2010) emphasized the importance of developing clinical judgment, specialized skills, and ethical integrity in nursing students to enhance awareness of patient safety. 60 A nurse with a high level of professional competence is expected to possess ethical and moral values, clinical reasoning abilities, effective communication skills, and understanding of medical concepts related to nursing care practices. 61 It has been reported that nurses with strong ethical decision-making skills are better equipped to establish effective nurse–patient relationships and delivere high-quality care. 62
Although the regression model explained a substantial portion of the variance in medical error tendency (R2 = 54%), nearly half of the variance remains unexplained. This suggests that other factors, such as workload, stress levels, and the work environment, may also play significant roles in influencing medical error tendencies among nursing students.45,63,64,65
Future research should consider including these variables to gain a more comprehensive understanding of the factors affecting medical errors. Acknowledging these additional influences could enhance develop targeted interventions aimed at reducing medical errors in clinical settings.
Limitations
This study has several limitations that should be taken into account when interpreting the findings. First, the results have limited generalizability, as the sample consisted solely of final-year nursing students from a single university. Second, data were collected using self-report questionnaires, which may be prone to various response biases. Specifically, using a self-report measure to assess medical error tendency may have introduced social desirability bias, leading participants to underreport actual behaviors or inclinations. This bias could have influenced both the magnitude and direction of the observed correlations between professional competence and medical error tendency.
To mitigate this risk, anonymity and confidentiality were emphasized during the data collection process. Participants were explicitly informed that honest responses were critical and that there were no right or wrong answers, in order to reduce the pressure to respond in socially desirable ways. Future research should continue to adress social desirability biases, possibly by incorporating indirect questioning techniques, validity scales, or triangulating self-reported data with supervisor assessments or direct observation. Additionally, multi-center studies are recommended to enhance the generalizability of the results across diverse educational and clinical settings.
Conclusion
This study revealed that nursing interns exhibited high professional competence and a low medical error tendency. A significant positive correlation was determined between professional competence and medical error tendency, with medical error tendency decreasing as competence increased. Students scored highest in the ethics, and accountability sub-dimension of the professional competence scale and lowest in the clinical biomedical science sub-dimension. On the medical error tendency scale, the highest scores were found in medications and transfusion administration, while the lowest scores were in patient monitoring and equipment safety.
Moreover, general clinical skills, critical thinking and reasoning, ethics and accountability were determined as significant independent predictors of the medical error tendency. These findings suggest a need to strengthen the integration of theoretical knowledge with clinical training. For instance, field-specific ethics and law courses could be incorporated into the curriculum to further reinforce students’ strengths in ethics and accountability. Regular case discussions and information sessions on ethical dilemmas during clinical practice could also help enhance self-awareness, empathy, and professional development. Critical thinking and reasoning skills should ideally be fostered and assessed through simulations, laboratory practices, and clinical case studies, both in theoretical and practical settings. The relatively low scores in the biomedical science sub-dimension may indicate the necessity of linking biomedical science courses more directly to nursing care practices and ensuring their integration into clinical processes.
Additionally, students’ professional competence and medical error tendencies could be regularly monitored using scientifically validated tools, with individualized feedback potentially provided based on results. Nurses in clinical institutions may benefit from in-service training to effectively supervise and evaluate students during clinical practice. Finally, strong collaboration between nursing schools and clinical institutions could be established. Joint educational activities might be organized to enhance students’ competencies, curricula may be updated according to clinical needs, and clinical education processes could be further optimized.
Footnotes
Acknowledgements
We thank the students who participated in the study.
Ethical approval
The Pamukkale University's Non-Interventional Research Ethics Committee approval (E-60116787-020-523666 dated 30.04.2024 and numbered 08) and institutional permissions were obtained from the relevant University where the study was conducted. The study conformed to the principles of the Declaration of Helsinki.
Informed consent
Informed consent was obtained from all participants.
Author contributions
Conception or design of the work: SA.
Acquisition of the data: AŞZ, SA
Analysis and interpretation of the data: AŞZ, ÖF
Drafting the work: AŞZ, SA, ÖF
Revising it critically for important intellectual content: AŞZ, SA, ÖF
Final approval of the version to be published: AŞZ, SA, ÖF
Agreement to be accountable for all aspects of the work: AŞZ,SA, ÖF
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Conflict of interest
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
