Abstract
Background
Healthcare providers experience a significant rate of nonfatal occupational injuries associated with their occupational duties and characteristics.
Objective
This study aimed to gauge occupational and physical therapists’ exposure to physical risk factors and pain levels related to patient handling in outpatient rehabilitation settings.
Methods
For this observational, descriptive, and cross-sectional study design, the Workplace Ergonomics Risk Assessment (WERA) tool was used to collect real-time data, and a self-administered numeric pain intensity scale was utilized to rate pain levels.
Results
The study included ninety-eight participants. The WERA overall final score showed that participants were exposed to moderate physical risk factors associated with Work-Related Musculoskeletal Disorders (WMSDs). Postures and repetitions of the anatomical areas were positively correlated with the use of force, vibration tools, contact stress tools, and task duration. Pain ratings showed that most of the participants experienced moderate to severe physical pain immediately after therapy sessions. A Kruskal-Wallis H test revealed a statistically significant difference in the exposure to physical risk factors in outpatient rehabilitation settings.
Conclusion
Participants were exposed to moderate levels of physical risk factors and moderate to severe pain that may lead to WMSDs. Participants working in pediatric settings experienced the most significant exposure to physical risk factors. Results from this observational study were consistent with those from self-reported studies involving WMSDs from different geographical regions worldwide.
Keywords
Introduction
Although slight incremental decreases in rates of nonfatal occupational injuries have been recorded over the past five years, improvements vary by industry, and overall levels remain high. 1 In 2022, the healthcare and social assistance industry recorded the second most significant distribution of nonfatal occupational injuries. 1 Various studies have highlighted that healthcare staff who are directly involved with patient handling are at higher risk of experiencing nonfatal occupational injuries.2–7 These workers include Occupational Therapists (OTs) and Physical Therapists (PTs), who may spend most of their working hours in contact with patients.
Occupational and physical therapy requires constant interaction with patients with injuries, illnesses, or disabilities. OTs and PTs are likely to spend most of the workday on their feet, helping patients recover or improve their health condition.8,9 Growing demand for therapeutic services exacerbates an already high workload. The daily duties of OTs and PTs typically involve considerable physical and mental exertion. Moreover, OTs and PTs regularly treat clients/patients with severe physical disabilities from all age groups, and their treatments usually require substantial physical effort.3,10
The physical activities required of OTs and PTs can involve manually lifting and transferring patients and equipment and treatment sessions that consist of repetitive motions and maintaining static postures for extended periods.3,8,9,11 Repetitive motions can include numerous body parts during therapeutic modalities, mobility techniques, and joint mobilizations. Other activities include lifting, transferring, bending, twisting, kneeling, squatting, and maintaining prolonged postures. These activities were identified as the leading factor associated with work-related musculoskeletal disorders (WMSDs) among OTs and PTs.3,11,12,13 Studies on WMSDs have shown a mixed prevalence of injuries, from 8% to 86% among OTs10,11,14,15 and 17% to 96% among PTs.3,12,16,17 Several factors might cause a wide range of injuries prevalence among OTs and PTs, including workload, number of patients, years of practice, and use of safe patient handling and mobility equipment. The most common anatomical areas of WMSDs were the lower back (35%), followed by the upper back (18%), neck (14%), and shoulders (10%). 17
Studies on WMSDs among occupational and physical therapists are mainly self-reported using questionnaires or online surveys.4,10,11,18 Still, workers’ compensation injury data also determine the prevalence, risk factors, and anatomical features associated with injuries.2–4,10–12,14–17,19 However, the literature lacks knowledge of the postures, repetitions, and tools that may lead to injury among these professionals.
In this study, we hypothesized that OTs and PTs would be exposed to significant physical risk factors during therapeutic sessions, contributing to increased reported pain levels. Furthermore, the magnitude of these exposures and associated pain levels varies across outpatient rehabilitation settings, including pediatric, neurology, and orthopedic specialties. Thus, our research questions were: what were the real-time physical risk factors OTs and PTs were exposed to during therapeutic sessions, and how were these exposures associated with reported pain levels? How do these exposures and pain levels differ across outpatient rehabilitation settings, including pediatric, neurology, and orthopedic specialties? Therefore, this study aimed to observe real-time exposure to physical risk factors among OTs and PTs during therapeutic sessions and to assess the associated pain levels resulting from this activity. A secondary aim was to examine these outcomes specifically within outpatient rehabilitation settings, including pediatric, neurology, and orthopedics. To the best of our knowledge, no study has directly observed OTs and PTs, including workflow, task demands, or WMSDs.
Methods
Study design
This study utilized an observational, descriptive, and cross-sectional design to assess the physical risk factors associated with work tasks among OTs and PTs. Variables related to physical risks included posture, repetitious movement of body regions, use of force, vibration tools, contact stress tools, and task duration. Other examination variables were related to pain and included pain rating and anatomical areas of pain. Variables were measured on an ordinal scale.
Participants
Recruitment of the study population took place in 2022 and included OTs and PTs working in outpatient rehabilitation settings within three public governmental hospitals of the same healthcare system in Kuwait. Inclusion criteria included therapists who had worked for at least one year in pediatric, orthopedic, and neurological rehabilitation clinics and specialized in these areas. The inclusion criteria only focused on these rehabilitation settings because OTs and PTs predominantly worked in these settings in this geographical location and mainly provided direct patient contact. The exclusion criteria included therapists with pre-existing musculoskeletal injuries, therapists currently holding an administrative position, and therapists with no direct patient handling or who only treated a small number of patients (≤ 3 patients per day).
A priori power analysis was conducted using G*Power version 3.1.9.7 20 to determine the minimum sample size required to test the study hypothesis. Results indicated the required sample size to achieve 80% power for detecting a medium effect, at a significance criterion of α = 0.05, was N = 159 for the Kruskal-Wallis U Test, and N = 84 for the Spearman Correlation test. However, due to time and resource constraints associated with individually observing each participant during a therapeutic session, only 98 participants were recruited.
This study included 98 participants (42 OTs; 56 PTs). Of these, 57 were female (30 OTs; 27 PTs), and 41 were male (12 OTs; 29 PTs). Table 1 shows the mean and standard deviations for age, years of experience, daily work hours, and the number of patients per day. Participants’ areas of practice included orthopedics (n = 26), neurology (n = 33), and pediatrics (n = 39).
Mean and standard deviation values for participants’ variables.
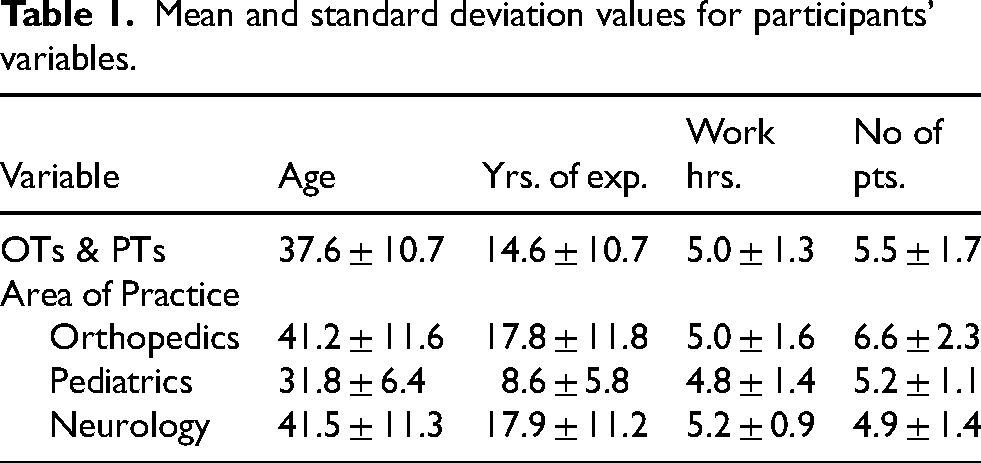
Assessment tools
The Workplace Ergonomics Risk Assessment (WERA; Appendix 1) is a standardized observational tool designed to screen work tasks for exposure to physical risk factors associated with WMSDs. 21 WERA targets four main upper body regions (shoulder, wrist, back, and neck) and the legs of the lower body. Also, WERA examines six physical risk factors, including posture, repetition, forceful, vibration, contact stress, and task duration. Including task duration as an exposure risk factor is essential to WERA due to the relationship between time and the risk of developing WMSDs. Veerasammy et al. 22 highlight that multi-tasks and duration increase MSD risk due to mechanical exposure or muscle fatigue accumulation that decreases tissue tolerance or physical effort. Moreover, Fan et al. 23 concluded that increased task duration may likely increase the physical workload and the risk of MSD. The WERA is a valid and reliable tool with well-established psychometric properties. 24 Usability testing demonstrated a high mean agreement between raters on the tool's items.21,24 Cohen's Kappa coefficient was 72.1 total agreement, indicating good inter-observer reliability. Validation tests showed a strong association between WERA results and reported pain, discomfort, or aches. Although a pilot test was not conducted before administration, the instrument's validity and reliability have been established.
The WERA scoring system and action levels guide the degree of physical risk factors (posture, repetition, forceful, vibration, contact stress, and task duration) and five body regions (shoulder, wrist, back, neck, and leg). The six physical factors and the five body regions are combined to make two parts (Part A and Part B) with nine overall items of physical risk factors.
Part A (items 1−5) assesses the exposure to posture and repetition of the shoulder, wrist, back, and neck, while evaluating the exposure to posture only for the leg. Depending on movement and posture, body regions are rated for risk levels as low, medium, or high according to rating descriptions. For example, the shoulder is considered a medium risk level for posture when the shoulder is bent upward (≤ 90 °). In contrast, the shoulder is regarded as a high-risk level in repetition when the shoulder moves with no rest. Subsequently, a risk matrix (low, medium, and high) based on posture and repetition (posture and duration for the rating of the leg only) is used for scoring. Part B (items 6−9) assesses exposure to force with the shoulder posture of Part A, vibration and contact stress with the wrist posture of Part A, and task duration with force. Force is estimated based on lifting patients, objects, or equipment and their weight; vibration is estimated based on the duration of using such tools; and using tool handles is estimated based on the shape of the handle. Initially, the four physical risk factors of Part B are rated for risk level as low, medium, or high according to rating descriptions. The forceful risk factor matrix is scored based on the force and shoulder posture, whereas the vibration risk factor is assessed based on vibration and wrist posture. The contact stress risk factor matrix is scored based on contact stress and wrist posture. The task duration risk factor matrix is scored based on the task duration of the participant's daily schedule of similar tasks and the amount of force. The assumptions of postures, repetitions, and duration are detailed on the WERA scoring sheet (Appendix 1).
The final total score is determined by summing the scores from the nine items and is composed of discrete data ranging from 18 to 54. A low-risk level has a final score of 18−27, where the task is considered acceptable; a medium-risk level has a final score of 28−44 with a recommendation of additional assessment and modification; and a high-risk level has a final score of 45−54, with which the task is considered unacceptable and requires immediate modification.
A self-reported numeric pain intensity scale was used to rate the degree of pain after completing therapy sessions. The pain scale ranged from 0 to 10 (0 = no pain, 1−3 = mild pain, 4−6 = moderate pain, and 7−10 = severe pain). 25 The interclass correlation coefficient was 0.95, indicating high agreement. 26 The participants used a figure of the human body with identified body segments to pinpoint the region with the most pain. Although a pilot test was not conducted prior to administration, the validity and reliability of the pain scale have been well established in previous studies.
Procedure
Ethical approval was obtained from the Institutional Review Boards of Kuwait University - Health Science Center and the Kuwait Ministry of Health (Ref-0025-119). The OT and PT departments were contacted to obtain lists of their therapists. A simple random sampling approach was used to select participants. All participants were informed about the study, signed an informed consent form, and completed a demographic questionnaire. Before conducting the study, two observers were trained in applying the WERA and demonstrated good inter-observer reliability in using the assessment tool. The observers received training from an ergonomics expert with 19 years of experience in work-related musculoskeletal disorders. The training lasted one week and began with an explanation of the study's objective, the observation method, and the specific tasks involved in observation. The observers were provided with detailed instructions on the procedure. Training included role-play and video therapy sessions to practice the observational technique. Recorded observations were compared and evaluated by the research team and the trainee. In addition, the research team provided the trainees with ongoing feedback on their performance.
In the therapy room or gym, the two trained observers sat separately to assess the participants’ exposure to the physical risk factors and completed a WERA sheet for each participant. Observation and assessment were conducted for at least 30 min during a single therapy session, which typically ranges from 30 to 45 min. Observers recorded, counted, and timed on separate sheets, then documented each part and final results on the WERA scoring sheet. Observers recorded the most frequently occurring angles and repetitions of the shoulder and wrist, as well as the alignment, bending, and repetition of the back and neck, and the position of the leg. Observers also recorded whether participants were involved in lifting loads (patients and equipment) and noted the weight of the loads. Moreover, observers documented whether participants used vibration tools and tool handles. In addition, observers recorded task duration based on participants’ daily schedules with similar tasks. Finally, immediately after the session, the observers provided the participant with a self-reporting pain scale rating sheet. This research protocol complied with the tenets of the Declaration of Helsinki.
Study analysis
The Statistical Package for the Social Sciences (SPSS) version 27 was used for analysis. Descriptive statistics summarized the demographics and frequencies of the physical risk factors. The Kruskal-Wallis H test was applied to determine exposure to physical risk factors and pain ratings across different areas of clinical practice. Additionally, the Bonferroni correction was applied to multiple comparisons between the different clinical practice groups. The Spearman's Correlation test was applied to determine the association between WERA Part A and Part B, as well as between the pain rating and WERA.
Results
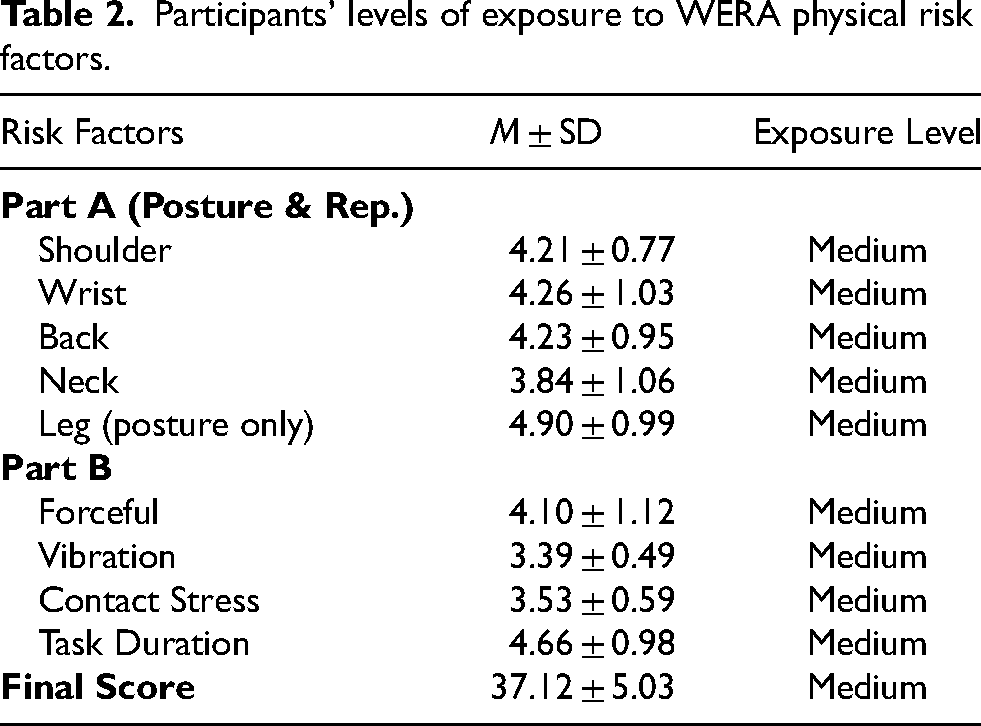
The WERA overall final score (M = 37.12, SD = ± 5.03 with CI (95%) = 36.12–38.12) showed that most participants experienced moderate exposure (n = 91, 93%) to physical risk factors associated with WMSDs, in addition to low (n = 1, 1%) and high (n = 6, 6%) exposures. Analysis of WERA Part A revealed that the wrist had the highest risk of exposure to posture and repetition (M = 4.26, SD = ± 1.03 with CI (95%) = 4.06–4.46). Moreover, WERA Part B showed that exposure to task duration scored highest compared to the other physical risk factors for WMSDs (M = 4.66, SD = ± 0.98 with CI (95%) = 4.47–4.85) (Table 2).
Participants’ levels of exposure to WERA physical risk factors.
A Spearman's Correlation test showed a large correlation of physical risk exposure between the wrist's posture and repetition and the use of vibration tools (rs (96) = .541, p ˂ .001) and the use of contact stress tools (rs (96) = .533, p ˂ .001). Also, Spearman's Correlation test showed a medium correlation of physical risk exposure between the wrist's posture and repetition and the use of force (rs (96) = .307, p ˂ .002), and a small correlation between the wrist's posture and repetition and the task duration (rs (96) = .275, p ˂ .006). Moreover, Spearman's Correlation test showed a large correlation of physical risk exposure between the back's posture and repetition and the use of force (rs (96) = .710, p ˂ .001) and the task duration (rs (96) = .542, p ˂ .001) (Table 3).
Spearman's correlation between the WERA physical risk factors of parts A and part B.

*Significant at p ≤ .05; ** Significant at p ≤ .0001.
Exposure to physical risk factors in outpatient rehabilitation settings
Participants in the pediatrics in outpatient rehabilitation setting showed a greater mean of exposure to repetition and faulty posture in the back (M = 4.46 ± 0.82 with CI (95%) = 4.29–4.62) and legs (M = 5.46 ± 0.72 with CI (95%) = 5.31–5.60), as well as a greater mean of exposure to the use of force (M = 4.36 ± 1.06 with CI (95%) = 4.15–4.57) than participants in the orthopedics and neurology outpatient settings. However, Participants in the neurology outpatient rehabilitation setting showed a greater mean of exposure to repetition and faulty posture in the shoulder (M = 4.39 ± 0.86 with CI (95%) = 4.22–4.56), as well as a greater mean of exposure to the task duration (M = 4.91 ± 1.16 with CI (95%) = 4.68–5.14) than participants in the orthopedics and pediatrics (Figure 1). In addition, Participants in the pediatric outpatient setting had a greater final score mean of exposure to physical risk factors (M = 38.33 ± 4.71 with CI (95%) = 37.39–39.26) than participants in the orthopedics (M = 35.00 ± 3.38 with CI (95%) = 34.33–35.66) and neurology (M = 37.36 ± 6.01 with CI (95%) = 36.17–38.55). Moreover, a Kruskal-Wallis H test revealed a statistically significant difference in multiple risk factors between Part A and Part B. For example, the Kruskal-Wallis H test showed a statistically significant difference in the back region's exposure to posture and repetition risk factors between the different outpatient rehabilitation settings (H (2) = 10.206, p = .006), with a mean rank WERA final score of 56.41 for pediatrics, 52.64 for neurology, and 35.15 for orthopedics. Multiple comparison adjustments using the Bonferroni correction revealed significant differences between neurology and orthopedic settings (adjusted p = .042) and between pediatric and orthopedic outpatient rehabilitation settings (adjusted p = .006) (Table 4).
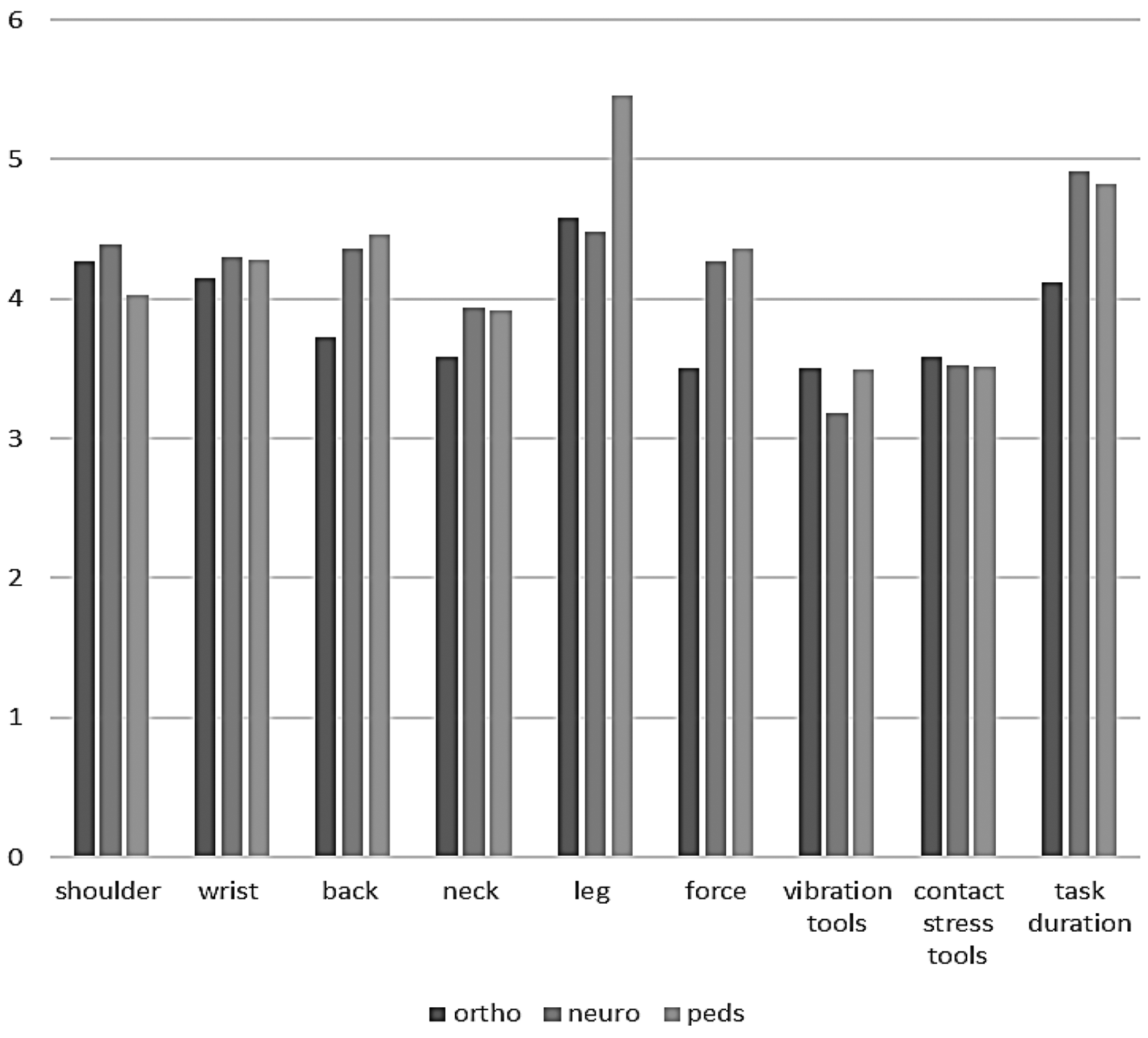
The mean exposure to the physical risk factors in outpatient rehabilitation settings.
Kruskal-Wallis H Test between the outpatient rehabilitation settings and the WERA physical risk factors of Part A, Part B, and the final score.
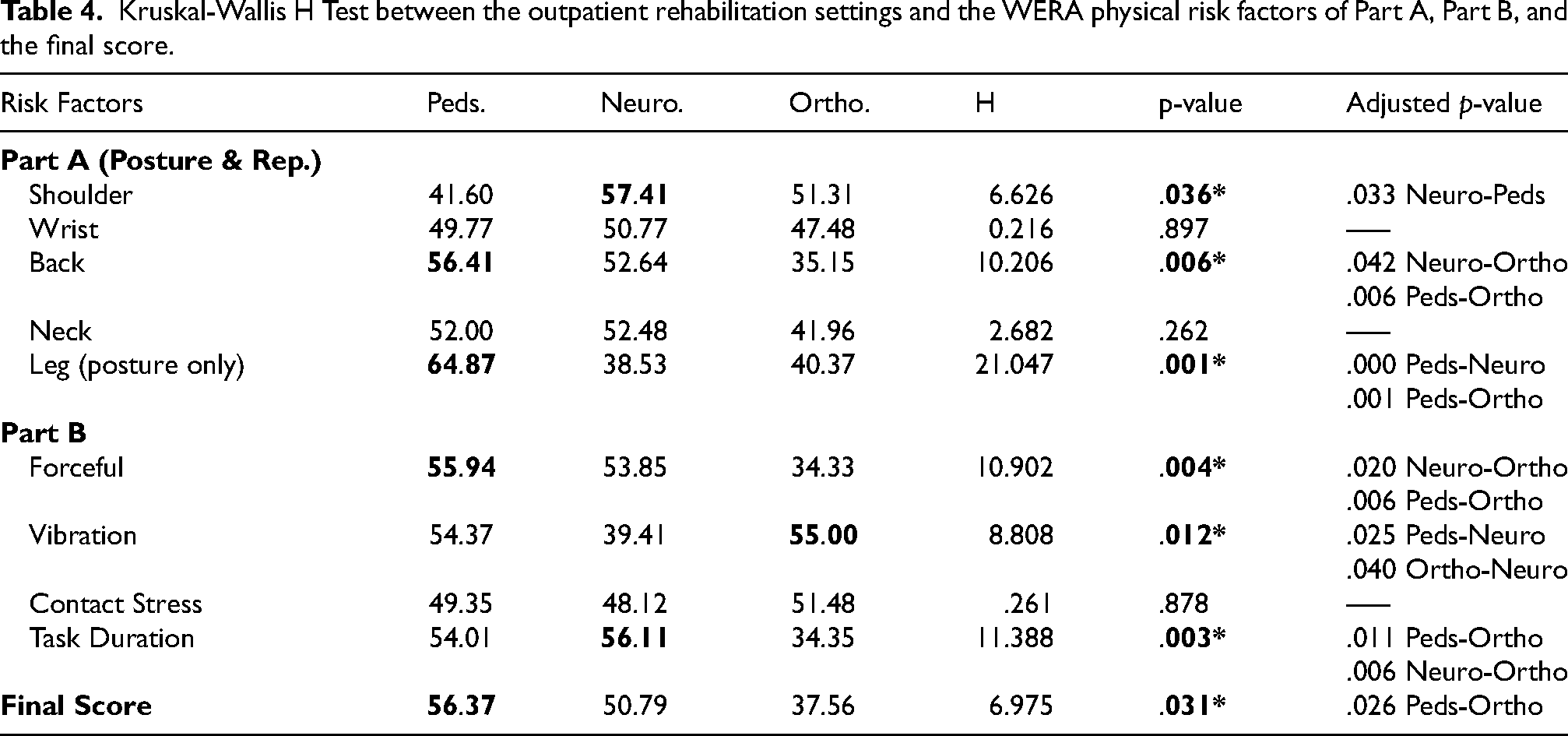
A Kruskal-Wallis H test showed a statistically significant difference in the final score of the exposure of the physical risk factors between the different outpatient rehabilitation settings (H (2) = 6.975, p = 0.031), with a mean rank WERA final score of 56.37 for pediatrics, 50.79 for neurology, and 37.56 for orthopedics. Multiple comparison adjustments using the Bonferroni correction showed a significant difference between the pediatric and orthopedic outpatient rehabilitation settings (adjusted p = .026) (Table 4).
Levels and anatomical areas of pain
Our results showed that 91% (n = 89) of the participants reported experiencing pain immediately after their therapy sessions, with 65% (n = 64) experiencing moderate to severe physical pain (M = 4.33, SD = ± 2.23). The data ranged from no pain (n = 9, 9%), mild (n = 25, 26%), moderate (n = 50, 51%), and severe (n = 14, 14%) pain. The anatomical regions with most pain were the lower back (n = 49, 50%; M = 4.84, SD = ± 1.78), shoulder (n = 18, 18%; M = 4.89, SD = ±2.14), neck (n = 9, 9%; M = 4.44, SD = ± 2.07), and wrist (n = 6, 6%; M = 4.00, SD = ± 1.55).
A Spearman's Correlation showed no statistical significance between pain ratings and WERA physical risk factors (rs (96) = −.064, p = .533). A Kruskal-Wallis H test revealed no statistically significant difference in pain ratings across the different outpatient rehabilitation settings (H(2) = 2.161, p = .339), with mean ranks of 52.06 for pediatrics, 43.67 for neurology, and 53.06 for orthopedics.
Discussion
In the current study, participants from local occupational and physical therapy healthcare departments were assessed for exposure to physical risk factors during patient treatment and subsequently queried about pain levels associated with their work activities, movements, and postures. WERA results indicated that participants were exposed to medium levels of physical risk factors, and most participants experienced moderate to severe levels of pain immediately after performing a therapy session, suggesting the need for further investigation and task modification.
Participants were potentially at risk of developing WMSDs due to the nature of their work activities, which required spending much of their therapy sessions in direct contact with patients to demonstrate, prepare, and administer therapeutic interventions. Our observational findings were consistent with previous self-reported studies in East Asia, Western Europe, and the Middle East, which concluded that direct patient contact and handling were the main risk factors associated with WMSDs among OTs and PTs.3,7,11,27,28 In contrast to self-reported studies, our real-time observational study revealed the level of exposure and association with the risk factors. For example, the wrist was more exposed to faulty postures, high repetitions, and task duration than any other anatomical region. In addition, the posture and repetition of the wrist were associated with and exposed to all risk factors, including the use of force, vibration tools, contact stress tools, and task duration. Also, the use of force and task duration influenced the posture and repetitive back movements. The use of force was common during patient transfer and lifting, adjusting the patient's position, lifting and carrying weights, and performing soft tissue and myofascial release massage. The use of the vibration tool, such as the vibrator gun, was regular during muscle and scar tissue massage activities. In addition, observed contact stress tools included weights, physio balls, fine motor tools, activity of daily living tools, and physical agent modalities. A possible explanation for the various and vast exposure to the risk factors during the delivery of most therapeutic activities and techniques is the nature of OTs’ and PTs’ work.
Using real-time naturalistic observation, we found a medium risk in the WERA Part A (posture and repetition), coinciding with a medium pain rating in the participants’ lower back, shoulder, neck, and wrist. Similarly, other self-reported research studies from diverse geographical regions worldwide have consistently found that the most common WMSDs include pain in the lower back, shoulder, neck, and wrist.2–7,11,15,28,30–32 Our real-time observational results revealed more evidence and insight than the self-reported studies concerning posture and repetition. We estimated that the participants’ activities involved medium levels of repetitive movements and exposed them to risky postures that could lead to musculoskeletal disorders in their lower back, shoulders, neck, and wrists. Moreover, the shoulder was frequently flexed up to 90 degrees, the wrist was in flexion or extension positions, the back and neck were flexed up to 20 degrees, and the legs were flexed at the knee joint for sitting or squatting. Again, the nature of OTs’ and PTs’ work and patient handling was likely to elevate the risk of faulty postures and high repetitions. Likewise, Anyfantis and Biska 30 and Le et al. 7 reported that musculoskeletal injuries among the physical therapy respondents were likely due to performing repetitive tasks, exerting compromised body positions such as flexion and rotation of the spine and neck, and maintaining static postures for long periods.
Results showed positive low to high significant associations between the posture and repetition of the anatomical regions of WERA Part A and the use of force and task duration of WERA Part B. The finding may indicate the impact of risky use of force and task duration on the manipulation of postures and repetitions of the anatomical regions. In addition, a moderate level of pain was reported in these anatomical regions. Thus, the participants were likely at heightened risk of developing musculoskeletal disorders when the therapeutic activities involved physical force and lengthy task duration. Our results were consistent with those reported in previous studies. Gyer et al. 32 highlighted that wrist/hand injuries among PTs were related to highly repetitive tasks and muscle weakness. Forman et al. 33 concluded that wrist injuries are primarily related to the use of force and exertion caused by work and daily activities, which significantly influence the wrist joint's position and repetitive motion. Moreover, physical factors at work, such as high repetition, heavy lifting, pulling, squatting, sustained standing, and prolonged task duration, were predictive of pain in specific anatomical regions. Carneiro et al. 29 concluded that forearm and arm position in space and static postures were leading factors in the development of musculoskeletal disorders in the lower back. Meyers et al. 34 showed that the risk of shoulder injuries, such as rotator cuff syndrome, was greater with exposure to the elevation of upper extremities combined with forceful repetition. In addition, Nematimoez and Thomas 35 reported that maintaining the neck in a flexion position during lifting and lowering tasks increases the risk of lower back pain. Other researchers from different world geographical regions emphasized that OTs and PTs could develop musculoskeletal disorders by performing physical risk activities during therapy sessions, such as lifting, transferring, manual activities with force, and prolonged repetitive use of the wrist, shoulder, lower back, neck, and leg.3,7,11,16,19,28,30,32 Our observational work supported the relationship between musculoskeletal disorders and work activities, movements, and postures.
In this study, participants working in pediatric clinical settings were found to be at a greater risk of developing WMSDs than those working in orthopedics or neurology. The nature of their therapeutic activities, including static postures to maintain children's positions, the use of force to lift and transfer children, repetitive motions, and participation in floor-level activities, might explain their greater exposure to physical risk factors, particularly in the lower back and legs. Darragh et al. 36 identified lifting and transferring of children and equipment, operating playground equipment, applying manual therapy, performing floor work with children, and children's aggression toward therapists as the most common factors leading to injury in pediatric OTs and PTs. They reported that the lower back, neck, wrist, knee, and leg were the most injured anatomical regions. Understanding the diverse therapeutic activities involved in different clinical practices warrants further detailed investigation to determine their relationships with the risk of developing WMSDs.
Implications
Preventing musculoskeletal disorders by reducing physical risk is essential for securing the safety of healthcare providers. 37 Therapists may potentially be at great risk for WMSDs due to risky postures and high repetitions coupled with the use of force, vibrational tools, contact stress, and extended task durations. Ultimately, exposure to physical risk factors may impact the physical health, career longevity, and overall well-being of OTs and PTs. Frustration, stress, and worry about their physical health, as well as concerns about taking time off work, may affect the delivery of rehabilitation services and increase healthcare costs.
Therefore, we suggest promoting knowledge in WMSDs, ergonomic principles of handling patients and therapeutic tools, and proper working postures. Keebler and colleagues 38 called for greater involvement of ergonomics in healthcare education and services, including equipment design, task design, patient safety, and the development of new healthcare technologies. Moghadam et al., 39 Sweeney et al., 40 Kopack, 41 and Sherman 42 concluded that increased awareness of ergonomics, the application of ergonomics interventions, and the utilization of ergonomics and workstation self-assessment checklists support the early identification of risks and encourage active participation in safety and self-protection. These strategies were also associated with reductions in musculoskeletal disorders, pain, and dysfunction, while simultaneously increasing performance and productivity. Healthcare organizations and educational programs should prioritize patient handling equipment and assistive devices for healthcare professionals and students to reduce the risk of WMSDs.43,44,45 Additionally, practice and safety guidelines, along with safe patient handling and mobility policies, are needed to support healthcare professionals and improve occupational health and safety.28,31,43–46 OTs and PTs should consider diverse approaches to treating patients, such as group therapy and teletherapy, where therapists may offer a variety of activities and therapeutic interventions. For example, the incorporation of virtual reality technology has been shown to improve enjoyment and participation in rehabilitation programs. 47
Limitations
This study has several limitations. The study was constrained by a relatively small sample size of 98 participants. This limited sample size may have affected the generalizability of the findings to broader populations. To achieve statistical power with a medium effect size of at least 80%, future research should consider increasing the sample size to 160 participants, thereby enhancing the robustness of the findings and improving the ability to detect meaningful results. Findings are limited to occupational and physical therapy practice in rehabilitation settings within the study's geographical location. Therefore, our results cannot be generalized to different populations, settings, or locations. In addition, this study did not compare exposure to physical risk factors or the level of pain between OTs and PTs. Future studies should consider examining these comparisons to identify potential differences. Neither the assessment time during the working day nor which working day (1st vs last) were controlled. Since assessing participants at the beginning of the working day may reveal different results because of cumulative stress at the end of the day, and similarly, cumulative fatigue throughout the working days, future studies should include these variables within the study design. Other potential confounding factors were not considered in this study. For example, unmeasured potential risk factors, such as general health, psychosocial factors, patients’ diagnoses and condition severity, patients’ weight, and organizational issues and policies, may provide a better understanding of the risk associated with the work of occupational and physical therapists. Moreover, WERA had its limitations, including that the assessment is limited to static and repetitive tasks, and subjective scoring may vary between evaluators. Additionally, the instrument and pain scale were not pilot tested prior to administration. Future studies should consider conducting pilot testing to further ensure its appropriateness for the target population. Finally, video recording and post-analysis may offer additional detailed data.
Conclusions
This study utilized real-time assessment of physical risk factors and pain among participants from OT and PT while conducting their professional duties. The general conclusion is that therapists recruited for this study were at moderate risk of developing WMSDs and moderate to severe pain, indicating that the tasks during therapeutic sessions require further investigation and changes. Moreover, the use of force during the therapeutic sessions was a main risk factor, altering the natural postures and increasing repetitive motions of the wrist and back. Due to the nature of the work and the handling of patients and tools, OT and PT pediatrics, as an outpatient rehabilitation setting, were the most exposed to and affected by the physical risk factors.
Future studies should consider investigating the outcomes of implementing prevention programs to reduce WMSDs among healthcare providers. Investigating the rationale behind females and males in selecting therapeutic activities may give insight into the relationship between gender, activity selection, and WMSDs. Research studies should further examine the availability and accessibility of safe patient handling and mobility equipment to improve workplace safety. Finally, as the healthcare environment is constantly progressing, ongoing development of safety strategies and policies is required.
Footnotes
Acknowledgment
Many thanks to the Heads of the Occupational Therapy and Physical Therapy Departments, as well as to all participating therapists, for their valuable support and contribution to this study.
Ethical considerations
This study was performed in line with the principles of the Declaration of Helsinki. Approval was granted by the Ethics Committee of Kuwait University – Health Sciences Center and the Kuwait Ministry of Health (Ref-0025-19).
Consent to participate
All participants provided written informed consent before participating.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
The data are available at: 10.6084/m9.figshare.23653380.
Appendix A
