Abstract
Background
Implicit bias pervades health care, decreases quality of care, and disproportionately affects health outcomes for persons of color. Little is known about the use of biased language in the care of seriously ill children as documented in the electronic health record (EHR).
Objective
To describe the use of biased language in the EHR of critically ill pediatric patients and to assess if there is a difference based on patient demographics and clinical characteristics.
Setting/Participants
A retrospective review of EHRs was conducted on patients admitted to a Pediatric Intensive Care Unit (PICU) with a palliative care consult at a large, urban academic center in the United States in 2019.
Measurements
Demographics and clinical characteristics were compared between patients with and without biased language in their EHR in univariate and multivariate analyses. Frequencies of descriptor usage and health care team members using the descriptor were recorded. Exemplar quotes using biased language were recorded.
Results
In 63 patients, no differences were found in demographic or clinical characteristics between patients with and without positively and negatively biased language. In adjusted analysis, there was no effect of demographics or clinical characteristics on the odds of having at least 1 instance of negatively biased language. Physicians and social workers used more biased language than other health care team members.
Conclusion
Despite no statistically significant difference noted in this pilot study, linguistic biases exist in the EHR of seriously ill children, which may lead to testimonial injustice. Efforts to combat bias and racism in pediatric health care documentation may focus on revising note templates and educating across disciplines.
Introduction
The American health care system provides disparate care to persons of color1,2 leading to disproportionately poor health outcomes.3-5 Implicit bias, an unconsciously held prejudice against an individual or social group, has been extensively documented as occurring within health care settings4,6 and affects patient-provider interactions, patient adherence, treatment choices, influences outcomes, and perpetuates disparity.7-12
Biased language in the electronic health record (EHR) of patients can be stigmatizing, considered a linguistic microaggression, and can introduce testimonial injustice into the patient narrative.6,13,14 Testimonial injustice is defined as that which occurs when a speaker receives an unfair deficit of credibility due to prejudice on the part of the hearer. In the case of the medical record, one might introduce prejudice in the way the patient’s narrative is documented. Documentation that includes stigmatizing language may perpetuate downstream effects that negatively impact treatment recommendations as well as overall patient outcomes. 13
Specific themes associated with negatively biased or stigmatizing language in the EHR include questioning patient credibility, expressing disapproval, stereotyping, portraying patients as difficult, and emphasizing physician authority over patients. Themes associated with positive language bias may include direct compliments, expressions of approval, disclosure of positive feelings toward patients, minimization of blame, personalization, and highlighting patient authority. 15
Stigmatizing language in the EHR is well-established in adult health care and has been found to be more prevalent in the EHR of Black patients.6,16 Stigmatizing language in pediatric patients’ charts has been associated with poor outcomes in the setting of chronic diseases including obesity, diabetes, and sickle cell disease.17-19 The use of stigmatizing language has been shown to negatively impact treatment choices and recommendations as well as propagate bias in Black pediatric patients. 20
As experts in communication, palliative care teams are uniquely positioned to play a key role in confronting bias and doing anti-racist work. We sought to describe the use of biased language in critically ill children with a palliative consult at a single, large, urban tertiary care pediatric hospital
Methods
The Baylor College of Medicine Institutional Review Board reviewed and approved this study (Protocol H-50904).
Setting
Texas Children’s Hospital (TCH) is a quaternary care center with 3 campuses in metropolitan Houston, TX that reported 34,777 hospital admissions and 4,798,028 total patient encounters from all 50 states and from more than 70 countries in 2021.21,22 During the study period, the palliative care team included 5.4 full-time equivalent physicians, 4 nurse practitioners, 2 social workers, 1 chaplain, a part-time pharmacist, 1 nurse, a grief and bereavement team, learners, as well as administrative and research staff. The palliative care team at TCH is named the Pediatric Advanced Care Team (PACT).
Study Population
We conducted a retrospective electronic health record review of patients admitted to the TCH general Pediatric Intensive Care Unit (PICU) with a new palliative care consult from January 1, 2019 through December 31, 2019.
Data Collection Instrument
The data abstraction form was designed using the Research Electronic Data Capture (REDCap) database, a secure web-based application designed to support data capture research studies23,24 and included patient age at PACT consultation, sex, race, ethnicity, primary language, religion, insurance, and clinical characteristics.
Definitions
Age, sex, race, ethnicity, primary language, religion, and insurance were self-reported by the patient or parent at the time of registration at TCH. Patients were asked if they consider themselves to be American Indian/Alaska Native, Asian, Black, Native Hawaiian/Pacific Islander, and/or White. They were then asked if they consider themselves to be Hispanic or Latino, what language they prefer, and what, if any, religious preference they have. Due to the small sample size, the language and religion variables were dichotomized into English and Non-English and Christian and Non-Christian, respectively. “Medicaid” included any Medicaid insurance plan, “Public” included the Children’s Health Insurance Program (CHIP) and any military or other government- funded insurance plans, “Private” included any private insurance plans, and “Not Insured” included patients without any form of insurance coverage.
Clinical Characteristics
Patient’s problem lists were reviewed at the time of their initial PACT encounter during the study period, the number of active problems were recorded, and they were assigned 1 or more complex chronic condition (CCC) categories. 25
Data Extraction
Charts were reviewed from the time of initial PACT consult moving forward throughout the patient’s hospitalization until hospital discharge, death, or through the end of calendar year 2020. The instances of positive and negative descriptors in patient care notes were counted by entering the terms “lovely,” “engaging,” “compliant,” “pleasant,” “kind,” “difficult,” “challenging,” “non-compliant,” “angry,” and “claims” into the EHR search function. These specific descriptors were selected from a list based on a primary literature review of biased language within health records 16 and a survey of the 30 interdisciplinary health care providers from our palliative care team. Some permutations of these words were accepted such as “loving” and “challenged.” Selected quotes using descriptors were recorded to provide context and examples of descriptor usage.
Health care team members using the descriptor were also documented and were categorized as physicians, nurse practitioners, physician assistants, nurses, social workers, child life specialists, chaplains, psychologists, respiratory therapists, occupational therapists, or physical therapists.
Authors TMK and EK performed chart review to abstract demographics, clinical characteristics, positive and negative descriptor count, quotes, and health care team member using descriptors. To ensure accuracy of these counts and study team concordance in interpretation of descriptor usage, authors audited each other’s work on every seventh chart.
Statistical Methods
The primary research question was to describe the relationship between the use of biased language in health care records and patients’ demographics. The secondary research question that emerged was to describe how this biased language was used and by whom.
To ascertain if there was a difference in the prevalence of having 1 or more positive or negative biased words in an individual’s charts, differences between categories were assessed using the Kruskal-Wallis test for numeric variables when comparing multiple groups, Fisher’s exact test for categorical variables with small, expected frequencies, and the Chi-squared test for categorical variables otherwise. Multivariable logistic regression adjusting for demographic and clinical factors was performed for the probability of having 1 or more negative words for an individual. All analyses were performed using R software version 4.3.0 (R Core Team, Vienna, Austria). P-value <0.05 was considered statistically significant.
Results
Demographics and Clinical Characteristics
Patient Characteristics and Comparison Between Groups With and Without Biased Language.
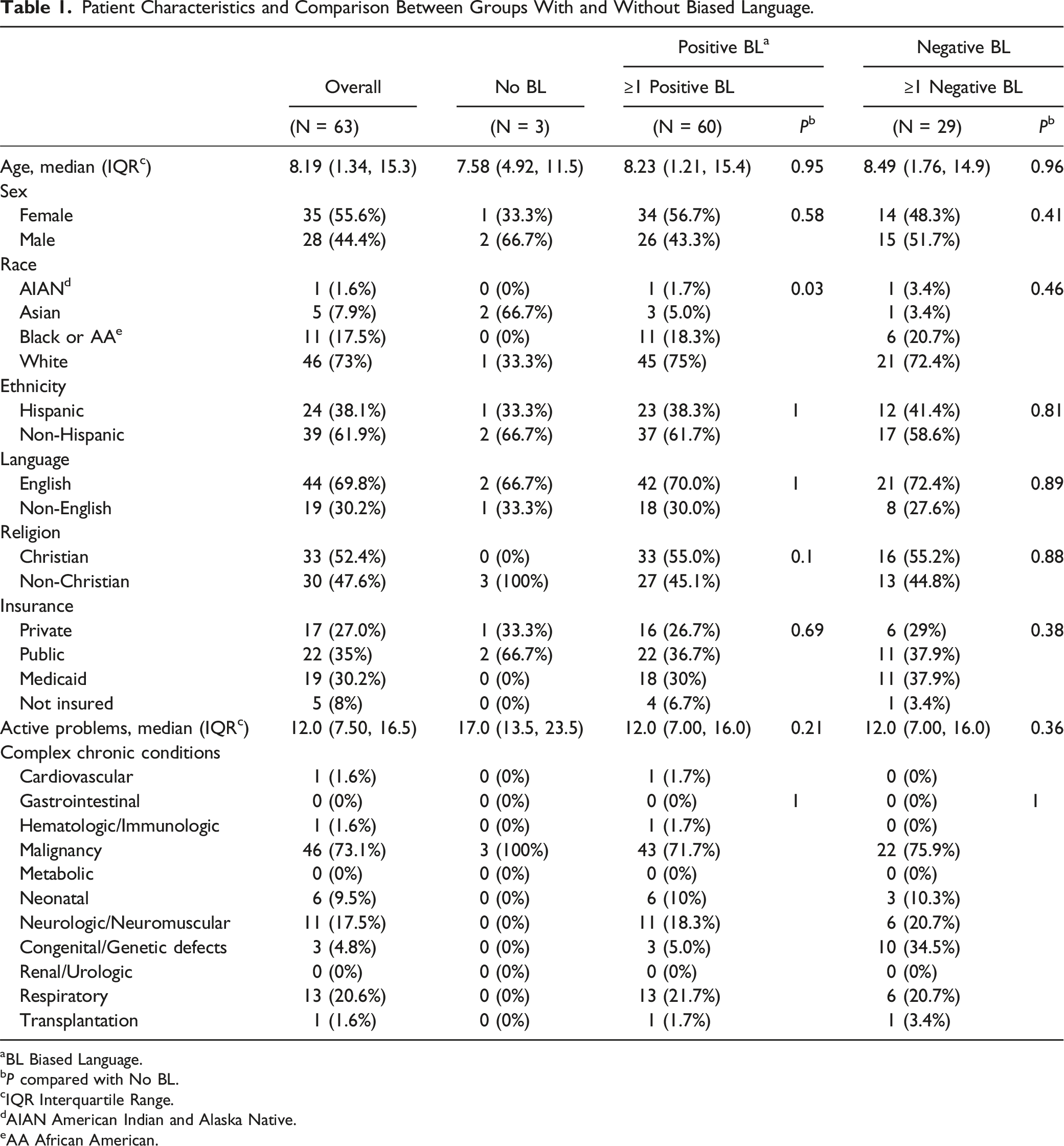
aBL Biased Language.
bP compared with No BL.
cIQR Interquartile Range.
dAIAN American Indian and Alaska Native.
eAA African American.
There were no significant demographic or clinical differences between those with and without negative biased language (P > 0.05). Similarly, the number of active problems and complex chronic conditions did not differ significantly between groups with either type of biased language (P > 0.05).
Odds of Negative Biased Language
Odds of Negative Biased Language by Patient Characteristics.
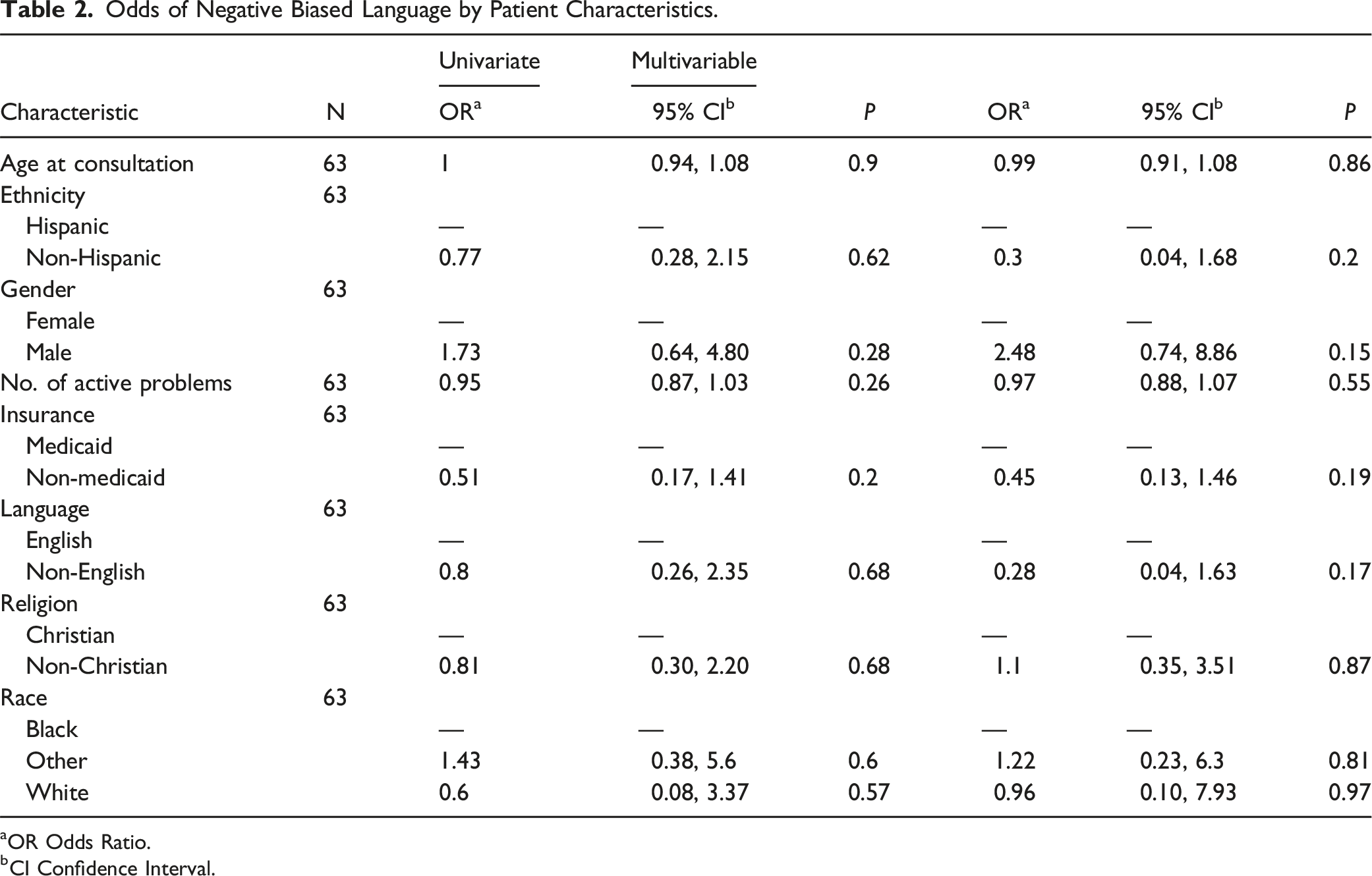
aOR Odds Ratio.
bCI Confidence Interval.
Number of Charts by Counts of Words
Most charts contained some positive biased language (at least 1 positive word in the chart) while there were many charts that did not contain any negative biased language. There was significantly more variation in number of positive words per chart than negative words (Figure 1). Percentage of patients with varying numbers of positive and negative words in chart (P < 0.01).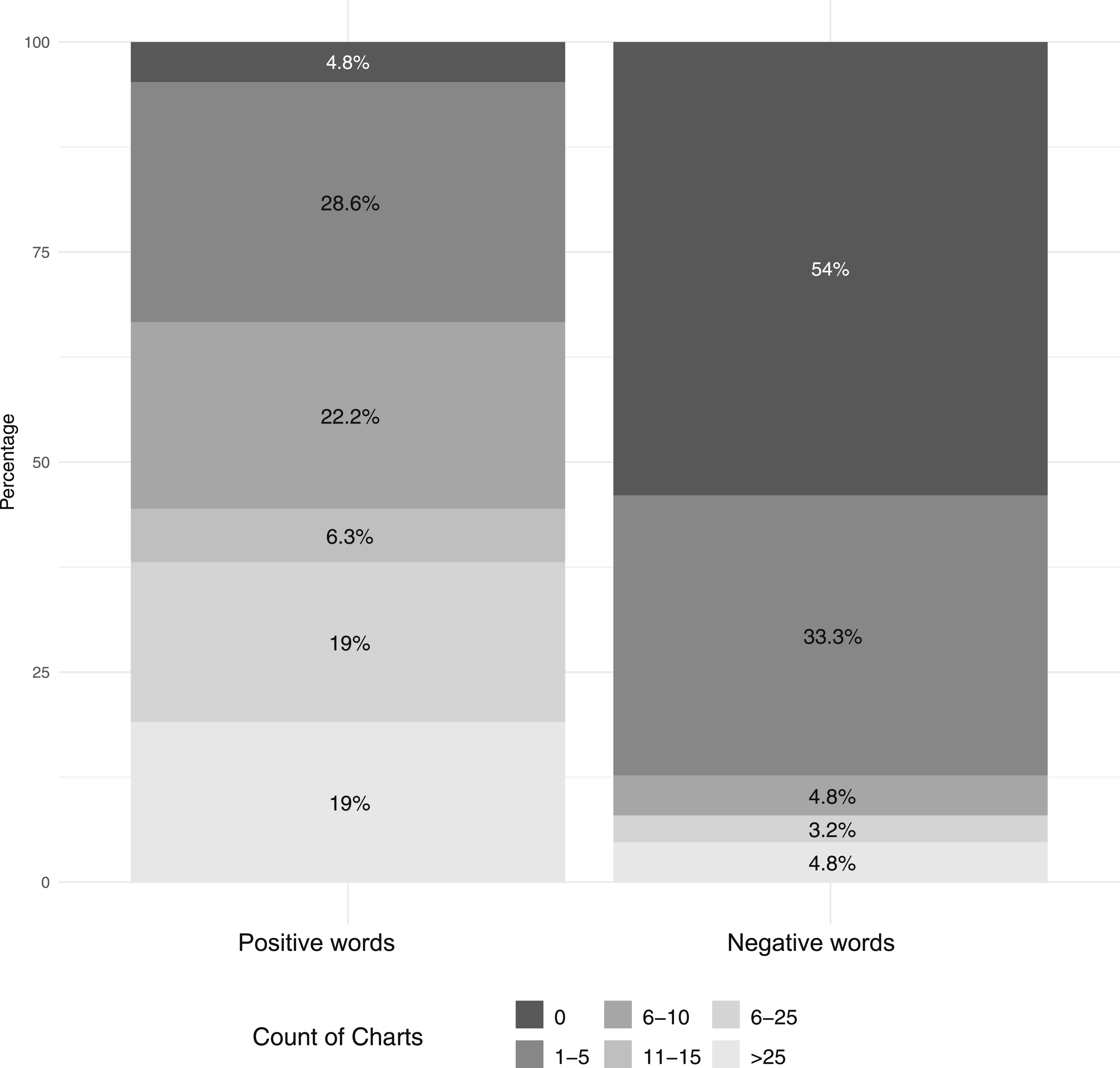
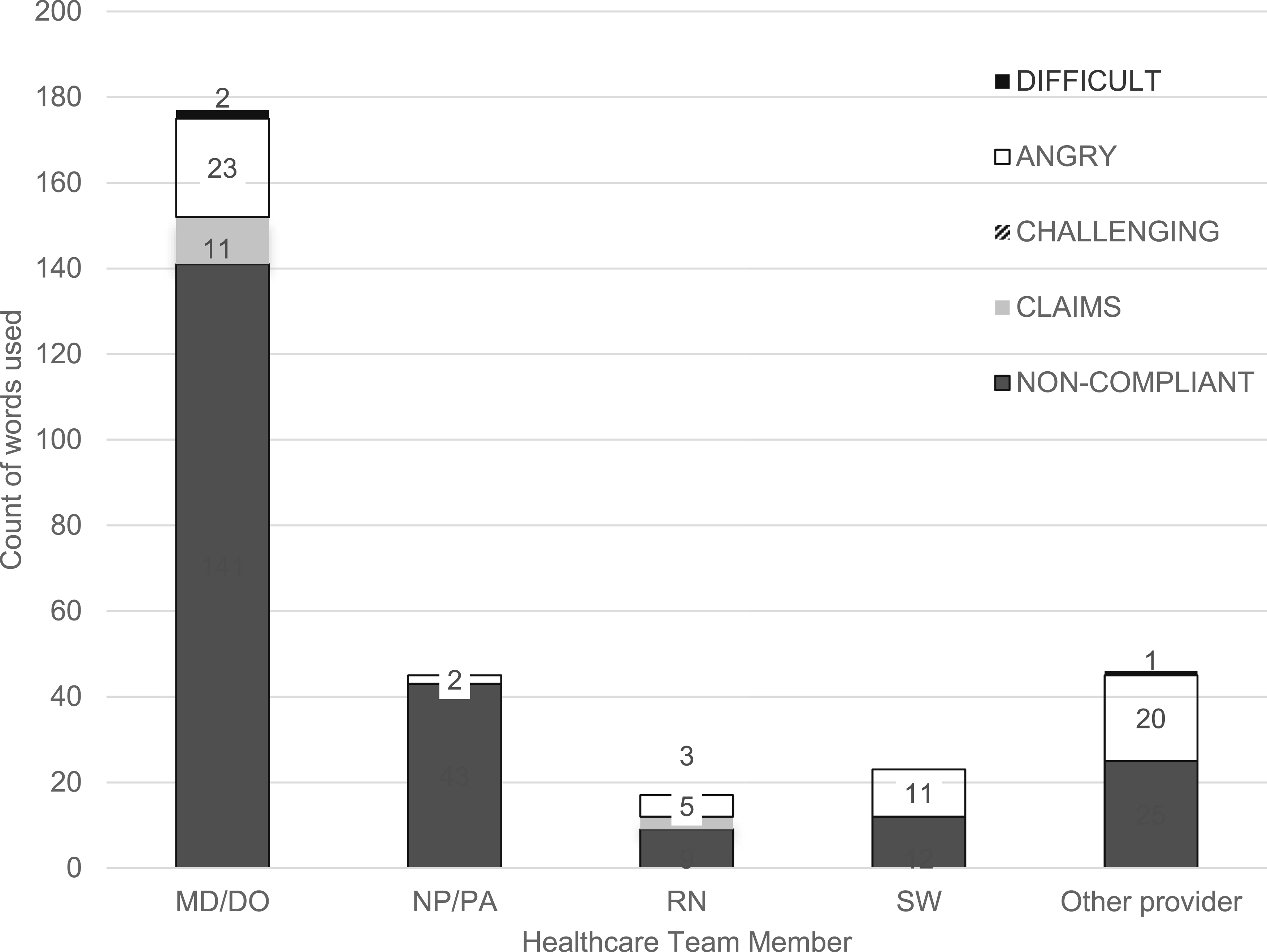
Use of Biased Language by Health care Team Member
All ten descriptors (5 positive, 5 negative) were identified in chart review. Physicians and social workers used more positive biased language compared to other health care providers, with physicians also using the most negative biased language (P < 0.01 for both) (Figures 2 and 3). Use of positive biased language by health care team member. P < 0.01. Other: Dietitian, pharmacist, technician, diet technician SLP, RD (dietitian). Use of negative biased language by health care team member. P < 0.01. Other: Care coordinator, scribe, pharmacist, optometrist.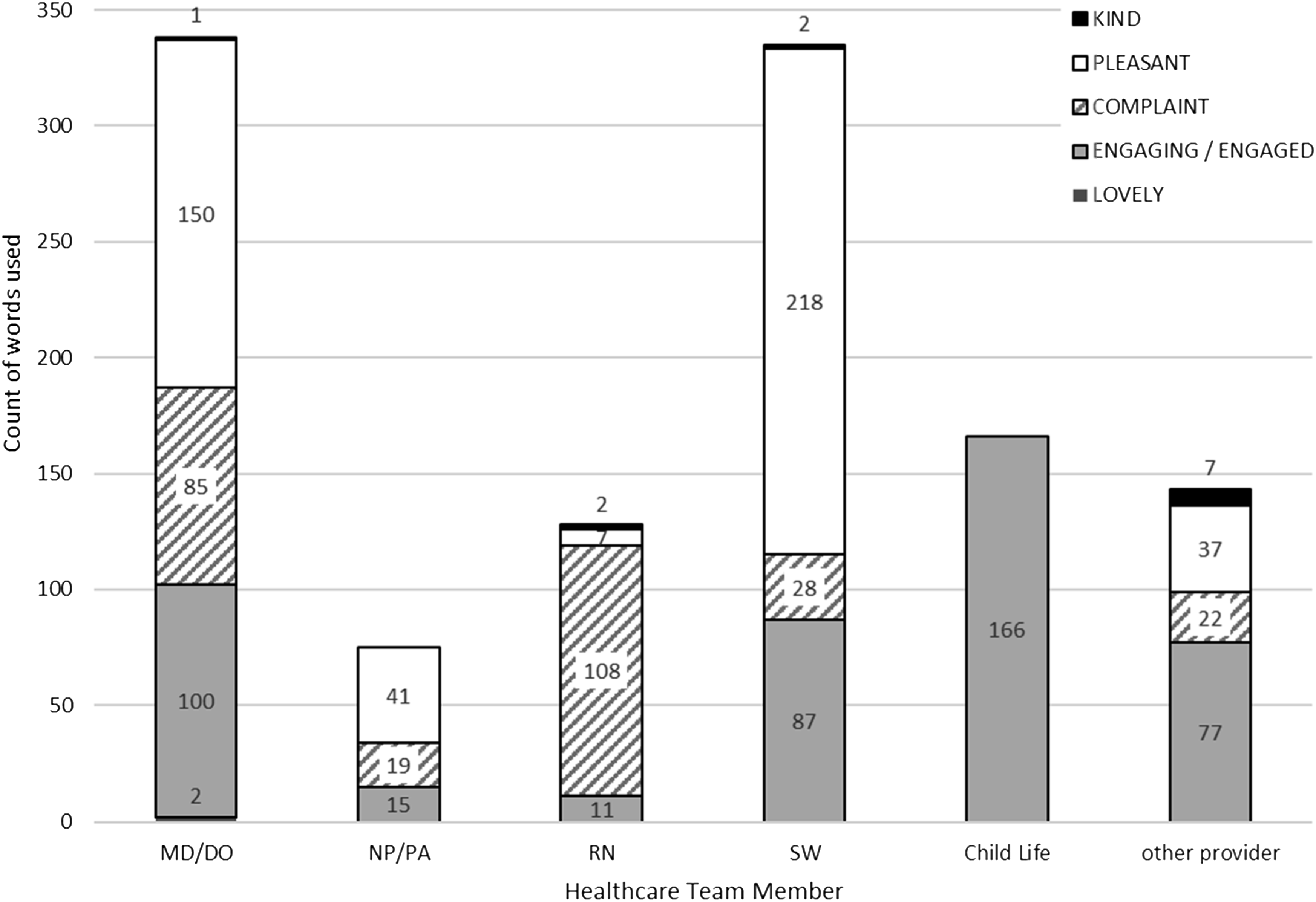
Exemplary Use of Biased Language
Quotes From Patient Charts Exemplifying Usage of Positive and Negative Biased Language and Health care Team Member Quoted.

Discussion
To our knowledge, this is the first study to explore the use of biased language in pediatric palliative care patients with serious medical illness. There was no significant difference in most demographics or any clinical characteristics between the patients who had biased language in their chart compared to patients without biased language in their chart. In this small sample, there was more positive biased language in the EHR than negative biased language, and more doctors and social workers used biased language than other health care team members.
Link and Phelan define stigmatizing language in the medical record as containing elements of labeling, stereotyping, separating, status loss, and discrimination co-occurring in a power situation that allows these processes to unfold.26,27 Goddeau highlights 3 linguistic characteristics of such language: casting doubt about patients, portraying the patient negatively, and implying patients are uncooperative. 28 There was evidence of this in our study. Although there was no statistical significance in the findings from our primary research question, the fact remains that there was biased language documented. This finding coupled with notable differences among individual disciplines with respect to not only use of stigmatizing language but specific words being used and in what context, warrant a more in depth review of how these practices might impact interactions with parents of children with serious illness.
The mode and manner of documentation is dictated by language specific to each discipline and also by hospital policy related to the scope of practice and documentation requirements for billing. 29 The mode available for documentation increases the likelihood of capturing biased language used by some disciplines and decreases the likelihood of capturing similarly biased language from other disciplines. In our study, doctors and social workers appeared to use positively biased language more than other members of the health care team. This may be influenced by the free text charting utilized more often by physicians and social workers than other disciplines, for example bedside nurses, who commonly have templates or checkboxes for charting.
Some words seemed to be discipline-specific. Doctors, who used the most negatively biased words, often used “non-compliant” in reference to lung or chest wall movement as part of the physical exam or in reference to taking medications. Similar to the association of the term “pleasant” with child life specialists, it is likely that this is related to discipline-specific language and training. Given what the literature says about biased language in medical documentation, perhaps other words or phrases could be considered in these instances that may not convey judgement or unintended bias. The authors suggest that the health care team member be more objective in their documentation. For example, instead of the patient being described as “pleasant” by their child life therapist, the therapist may document the words or actions that the patient used to respond to their intervention. Likewise, rather than describing a patient as “non-compliant,” one might describe the occurrence as medicine non-compliance or provide reason for the non-compliance such as transportation barriers preventing ability to pick up prescriptions or financial barriers preventing purchasing medications.
One of the challenges with evaluating the medical record for the presence of stigmatizing language is the inability to ascribe context and intent to the way in which words are utilized to capture the patient narrative by the clinician. This is especially challenging with respect to the role of “cut and paste” in EHR and the ability to repeatedly carry forward potentially damaging patient narratives through linguistic bias. In our study, this was seen frequently in physician notes with respect to patients described as “non-compliant” in an initial admission history and physical and subsequently carried forward through multiple progress notes. A recent study by Wang et al found that in a typical note only 18% is manually entered, 46% copied, and 36% imported. 30 This suggests EHR copying can serve as a “bias amplifier” and further highlights the need to remove bias from the documentation.
As a transdisciplinary patient- and family-centered specialty, palliative care teams are uniquely positioned to help health care systems reconsider how to sensitively document in the EHR. Our field has long modeled and educated on how to better communicate with patients and this may be an opportunity to bring that same focus to how we talk about patients (and document those communications). Navigating the right balance with respect to utilizing medical records to document patient care, provide adequate documentation for billing, and to carry forward the patient’s uniquely authentic voice is a skill that can be modeled and taught and may need to begin with focus on discipline-specific documentation and targeted educational efforts.31,32
There is limited data on how clinicians make or avoid moral judgments of patients, but the implications of labeling patients and families as good, bad, difficult, or lovely should be carefully considered because of the potential long-term impact on the provider-patient relationship, the disruption of medical trust, and the potential of adversely impacting treatment recommendations and health care outcomes. 33
With the passage of the Affordable Health Care Act in 2010 and the advent of OPEN Notes access for patients in 2021, more attention has been given to the impact of biased and stigmatizing language in the patient chart, more specifically its impact on patients and families. 34 Patients have reported concerns with the way their character is presented or how the history of their illness is perpetuated, which challenges health care teams to be intentional in how they carry forth patients’ stories. 35 There are several studies exploring the impact of bias in the EHR and the potential for perpetuating health care disparities in adults, while the growing body of literature for pediatrics is centered around racial disparities in treatment of pain in children with sickle cell or limb fractures.36,37
Palliative care, like many subspecialties in medicine, is notable for disparities in the number of patients from marginalized communities utilizing these services or being referred for these services. There are multifactorial barriers as to why these scenarios persist including the role of potential provider bias impacting consulting palliative care teams or approaching families who might benefit from additional services like palliative care. For pediatrics, this disparity in utilization of services seems profound.38,39
Strengths and Limitations
To our knowledge, this is the first study to look at the use of biased language in the charts of pediatric palliative care patients with serious medical illnesses. Strengths of this study include racial, ethnic, language, and socio-economic diversity of the patient population at the study site.
Multiple adult studies have demonstrated an increased likelihood of negative language used to characterize Black patients.6-10 As an example, Sun et al showed that Black patients had 2.54 times the odds of having at least 1 negative descriptor in the history and physical compared with White patients. Our findings raise concerns about stigmatizing language in the pediatric EHR and its potential to exacerbate racial and ethnic health care disparities. This pilot study looks not only at the occurrence of biased language, but further reports these occurrences by individual disciplines that comprise the health care team. Assessing bias through an interdisciplinary lens is novel and unique to the palliative care perspective.
There were several limitations to our study. Our sample size was small and from a single institution, limiting data analysis and study generalizability. Second, this project only measured word-use frequency, not context of word use, which limits what we can interpret from the data. Lack of context or semantic analysis could have potentially led to miscounted frequency of stigmatizing language or missed instances of descriptors used more complexly. Thirdly, this took place during the COVID-19 pandemic and in the years leading up to the implementation of the CURES Act. These 2 social contexts may have acted as confounders, changing how and what was documented in the EHR.
While this study had limited generalizability and its primary hypothesis was not statistically significant, it may generate questions for future research, specifically, why our center differed from other published studies that showed patterns of bias and disparate language use by note writers. One factor may be our highly diverse metropolitan area with a hospital workforce that represents the community it serves. Additionally, unlike much of the southern US, our children’s hospital was never segregated, even when it opened in the 1950s. Alternatively, given the greater social context of 2020, the murders of Breonna Taylor and George Floyd at the hands of police, and the Black Lives Matter movement, bias may have still occurred but providers self-censored their notes.
Next Steps
Future iterations of this work may include repeating this study with a more robust sample size and in other populations such as the Cardiovascular Intensive Care Unit and/or the Neonatal Intensive Care Unit. Future studies may also employ a dedicated and more robust qualitative methodology or software to elucidate the usage and context of biased language in pediatric patients with serious illness who are cared for by palliative care services at our site and others.
Conclusion
In our small pilot study, there was no statistically significant difference in the use of biased language based on patient demographics and clinical characteristics. Biased language was used by multiple team members and in varying contexts. Health care systems, teams, and individuals should consider removing biased language from documentation templates in the EHR. We encourage implicit bias education and anti-racism training across all health care disciplines and at every stage of training.
The ability to document and carry the patient’s voice is a part of our sacred duty as holders of their story and must be performed with respect to avoid linguistic bias and testimonial injustice. Careful consideration of word choice is necessary to ensure documentation that mitigates rather than contributes to health care disparities. There is testimonial power in our pen.
Footnotes
Acknowledgments
The writers would like to thank Britney Gomes for assistance with manuscript preparation, the Pediatric Palliative Care Research Network for its formative feedback when this was a work-in-progress, and, most importantly, the patients and families we serve for allowing us to be part of their narrative.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
