Abstract
Background
There are known sex and racial/ethnic differences in colorectal cancer care. The purpose of this study is to investigate these differences in end-of-life health care utilization, advance care planning, and associated outcomes among Texan Medicare colorectal cancer decedents.
Methods
In this retrospective case control study, we used the Texas Cancer Registry linked with Medicare data for patients (n = 5757) aged ≥66 years who died 6 months to 5 years after receiving a diagnosis of primary colorectal cancer from 2010-2018. We used chi-square tests, t-tests, or ANOVA as appropriate for outcomes in the last 30 days of life to assess sex and racial/ethnic differences. Multivariable logistic regression models were used to assess differences in the odds of inpatient admission and hospice enrollment.
Results
Significantly more female decedents were hospice enrolled. Non-Hispanic Black decedents, and to a lesser extent Hispanic decedents, had greater health care utilization, including inpatient stays, and less hospice enrollment compared to non-Hispanic White decedents. Advance care planning was low (≤2.2%) across all groups, with no significant differences. Multivariable logistic regression models showed that female decedents had greater odds of hospice enrollment compared to male decedents, and non-Hispanic Black decedents had greater odds of inpatient stays and decreased odds of hospice enrollment compared to non-Hispanic White decedents.
Conclusion
Sex and racial/ethnic disparities in care highlight opportunities for process and quality improvement and suggest a need for practice changes to improve access to quality end-of-life care. More work is needed to incorporate advance care planning and billing into regular workflows.
Background
Colorectal cancer is a leading cause of death in Texas and the United States.1,2 Racial and ethnic disparities have been observed in colorectal cancer care, including in screening, 3 treatment, and outcomes, 4 with non-Hispanic Black patients experiencing the highest mortality rates. 1 In Texas, non-Hispanic Black adults have the highest colorectal cancer incidence 2 and the highest rates of late-stage colorectal cancer diagnosis. 5 Compared to women, men are more often diagnosed with this cancer and have higher mortality rates in both the United States 1 and Texas. 2 A prior study assessing health care utilization and expenditures in the last year of life among colorectal cancer decedents from 1996-1999 found that women not only used hospice care more than men, but also had greater use of inpatient services, skilled nursing facility services, and home health, which was mostly attributed to older age and less social support among women. 6
Colorectal cancer is a leading cause of cancer-related death, making it essential to assess disparities in end-of-life care received, including palliative care, 7 advance care planning (ACP),8,9 and hospice use, 10 which can significantly impact quality of life for patients with colorectal cancer. Nationally, disparities in end-of-life care have been observed, 11 with racial and ethnic minority patients reporting less ACP, 12 lower hospice enrollment,13,14 and more burdensome end-of-life care15,16 compared to non-Hispanic White patients. Although men have higher colorectal cancer mortality rates 1 and a shorter life expectancy compared to women, 17 women are more likely to report ACP and enroll in hospice, perhaps influenced by factors such as more life years with disability, lived experiences, and lower socioeconomic status. 18
The purpose of this study is to investigate sex and racial/ethnic differences in the care received in the last 30 days of life by Texan colorectal cancer decedents. We hypothesize that female decedents receive more ACP and hospice care, while minoritized decedents have higher levels of health care utilization.
Methods
Study Cohort
We used data from the Texas Cancer Registry (TCR) – Medicare, a linkage of a population-based cancer registry from Texas with administrative Medicare claims data. TCR files are linked to Medicare claims using probabilistic linkage methods that ensure the protection of individual patient privacy. This study was reviewed by our institutional review board and deemed exempt.
In this study, we included patients diagnosed with primary colorectal cancer between 2010 and 2018 who died 6 months to 5 years after diagnosis, with death occurring between 2010 and 2019. Patients were excluded if they were under 66 years of age at the time of death, if the colorectal cancer diagnosis occurred at autopsy, if they had less than 12 months of continuous Part A and B (no HMO) enrollment prior to death, or if they had unknown race or ethnicity information.
Demographic Data
We collected information on patient demographics, including age at death, sex, race and ethnicity (categorized as Hispanic, Non-Hispanic White, or Non-Hispanic Black), and marital status. United States county data were used to report rural or urban residence and border county status. Zip code data were used to report the percentage of residents without a high school education and living below the poverty level, expressed as quartiles (first quartile representing higher rates of high school completion and less poverty, and fourth quartile representing less high school completion and more poverty). We also included information on dual insurance eligibility and original Medicare entitlement reason. Colorectal cancer stage, provided through the TCR and National Cancer Institute (NCI) Charlson Comorbidity Index (CCI), 19 based on inpatient and outpatient claims in the last 12 months of life, are reported.
Outcomes
We used Common Procedural Terminology (CPT) codes and International Classification of Diseases (ICD) versions 9 and 10 codes from Medicare claims files to assess emergency department (ED) visits, invasive mechanical ventilation use, intensive care unit (ICU) admission, inpatient admission, inpatient days, ACP, palliative care consultation, use of home health services, hospice enrollment, and days in hospice during the last 30 days of life (Appendix Table 1).
Statistical Analysis
Patient demographics and outcomes are reported by sex and race/ethnicity and presented as number (proportion) or mean (standard deviation [SD]), as appropriate. Chi-square tests, t-tests, or ANOVA were used as appropriate for categorical or linear variables to assess statistically significant differences between groups. Multivariable logistic regression models were used to assess sex and racial/ethnic differences in the odds of inpatient admission or hospice enrollment in the last 30 days of life, adjusting for age, marital status, colorectal cancer stage, rural/urban residence, border county status, dual eligibility, original entitlement, percentage of residents without a high school education based on zip code data, and the NCI CCI. 18 All analyses were conducted using SAS 9.4. All P-values are two-sided, and an alpha level of 0.05 was considered statistically significant.
Results
Patient Demographics
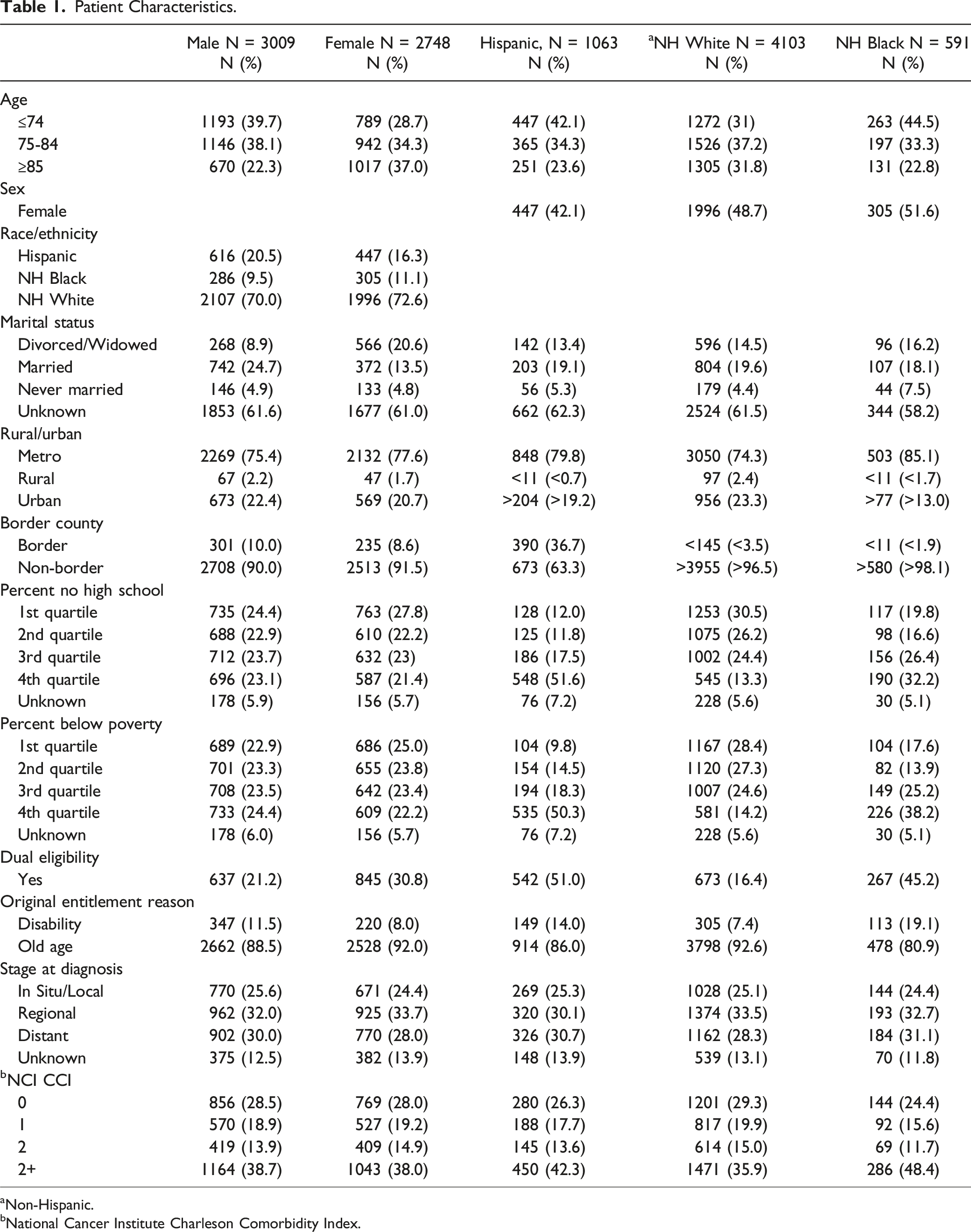
In total, 5757 Texan Medicare colorectal cancer decedents met inclusion criteria (Figure 1). Of these, 3009 (52.3%) were male and 2748 (47.7%) were female, while 1063 (18.5%) were Hispanic, 4103 (71.3%) were non-Hispanic White, and 591 (10.3%) were non-Hispanic Black (Table 1). Male decedents were slightly younger, most aged ≤74 years (40%) or 75-84 years (38%), compared to female decedents, most aged 75-84 years (34%) or ≥85 years (37%). More Hispanic (42%) and non-Hispanic Black (45%) decedents were aged ≤74 years compared to non-Hispanic White decedents (31%). More non-Hispanic White (49%) and non-Hispanic Black (52%) decedents were female compared to Hispanic decedents (42%). More Hispanic (51%) and non-Hispanic Black (45%) decedents had dual eligibility compared to non-Hispanic White decedents (16%). Additionally, more Hispanic (14%) and non-Hispanic Black (19%) decedents were disabled compared to non-Hispanic White decedents (7%). Approximately 24%–26% of decedents had in situ/local disease, and 28%–31% had distant disease at diagnosis across groups. Hispanic (42%) and non-Hispanic Black (48%) decedents were more likely to have NCI CCI scores >2 compared to non-Hispanic White decedents (36%). Criteria for inclusion and exclusion using Texas Cancer Registry-Medicare data. Patient Characteristics. aNon-Hispanic. bNational Cancer Institute Charleson Comorbidity Index.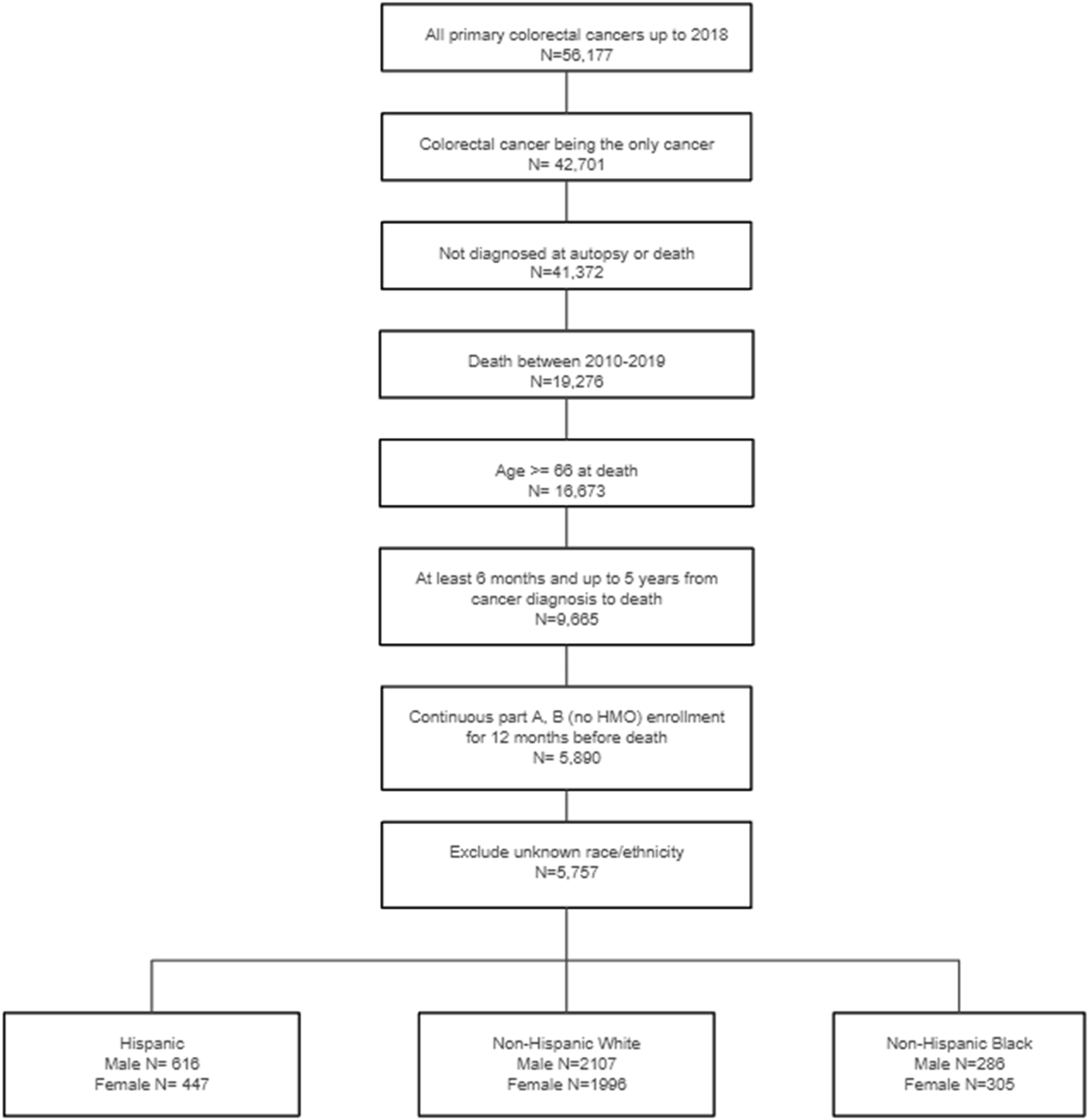
Patient Outcomes
Patient Outcomes in the Last 30 days of Life.
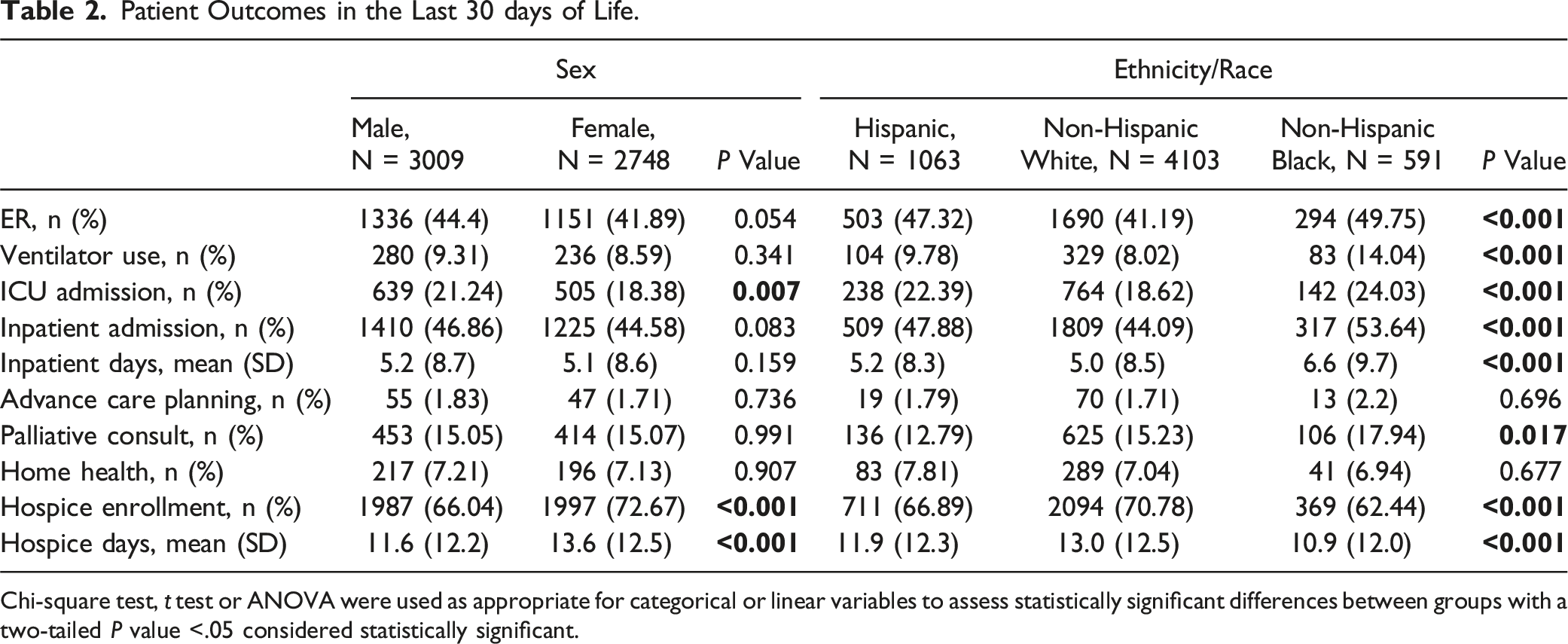
Chi-square test, t test or ANOVA were used as appropriate for categorical or linear variables to assess statistically significant differences between groups with a two-tailed P value <.05 considered statistically significant.
More non-Hispanic Black and, to a lesser extent, Hispanic decedents had significantly more health care utilization compared to non-Hispanic Whites decedents (Table 2). Non-Hispanic Black decedents were more likely to have an ER visit (50% vs 41%, P < 0.001), use mechanical ventilation (8% vs 4%, P < 0.001), be admitted to the ICU (24% vs 19%, P < 0.001), and be admitted as inpatients (54% vs 44%, P < 0.001) compared to non-Hispanic White decedents. Non-Hispanic Black decedents also experienced longer inpatient lengths of stay (LOS) (mean 6.6 [SD 9.7] vs 5.0 [SD 8.5] days, P < 0.001). While there was no statistically significant difference between groups in ACP, the proportion of decedents with ACP was low overall, with only 1.7%–2.2% of decedents having had a billed ACP encounter. Non-Hispanic Black decedents were more likely to receive palliative consults (18% vs 15%, P = 0.017) in the last 30 days of life compared to non-Hispanic White decedents; however, they were less likely to be hospice enrolled (62% vs 71%, P < 0.001) and had shorter hospice LOS (mean 10.9 [SD 12.0] vs 13.0 [SD 12.5] days, P < 0.001). No significant difference in home health was observed across groups.
Multivariable Logistic Regression Models for Inpatient Stay and Hospice Enrollment.
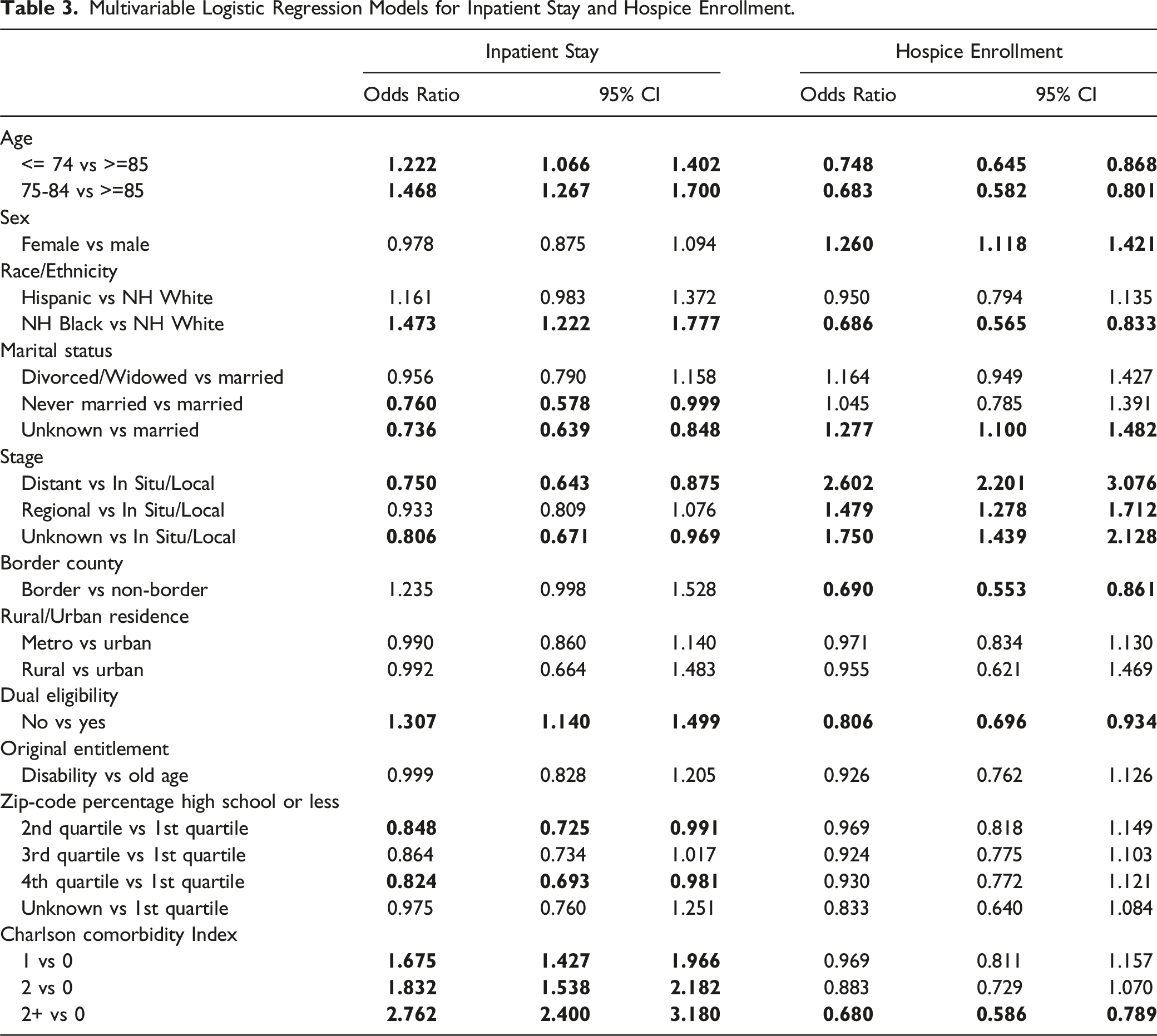
Non-Hispanic Black decedents had higher odds of inpatient admission compared to non-Hispanic White decedents (OR 1.513, 95% CI 1.259-1.818) but decreased odds of hospice enrollment (OR 0.669, 95% CI 0.552-0.812) (Table 3). There was no statistically significant difference in the odds of inpatient admission or hospice enrollment between Hispanic and non-Hispanic White decedents.
Discussion
In this retrospective cohort study, we assessed sex and racial/ethnic differences in health care utilization, ACP, palliative care consultation, and hospice enrollment among 5757 Medicare colorectal cancer decedents in the last 30 days of life. Female decedents were less likely to experience an ICU admission and more likely to be enrolled in hospice, with more days in hospice compared to male decedents. Further analysis using a multivariable logistic regression model found no significant sex difference in the odds of inpatient admission but confirmed that females had higher odds of hospice enrollment than males. Non-Hispanic Black and, to a lesser extent, Hispanic decedents had more health care utilization, including ER visits, ventilator use, ICU admissions, inpatient admissions, and more inpatient days compared to non-Hispanic White decedents. Although a higher proportion of non-Hispanic Black decedents had a palliative care consultation in the last 30 days of life, they were less likely to be enrolled in hospice and had fewer days in hospice compared to non-Hispanic White decedents. Rates for ACP were low across all groups. Adjusted models found that non-Hispanic Black decedents had higher odds of inpatient stay and lower odds of hospice enrollment compared to non-Hispanic White decedents. No significant differences in these outcomes were found between Hispanic and non-Hispanic White decedents.
Sex Differences
Female decedents were more likely to experience hospice enrollment and spent more days in hospice compared to male decedents. This finding aligns with a prior study on colorectal cancer decedents, which showed that women used hospice more frequently than men 6 and national studies showing that women are more frequently hospice enrolled.14,17 While a prior study showed that female colorectal cancer decedents receive more inpatient admissions, home health and other services compared to males, 6 in our study we found no statistically significant differences in health care utilization measures except for females having less ICU admissions. The data in our study aligns with national data in which females experience less health care utilization including inpatient and ICU admissions and more hospice due to a variety of factors including personal preferences shaped by experiences including caregiving, lower socioeconomic status and higher symptom burden.14,17,20,21
Ethnic and Racial Differences
Non-Hispanic Black decedents, followed by Hispanic decedents, had significantly more health care utilization compared to non-Hispanic White decedents. The higher health care intensity experienced by minoritized patients at the end of life is well described14-16,22,23 and is attributed to a variety of factors, including minoritized patients, especially non-Hispanic Black patients, being diagnosed with more advanced colorectal cancer and having higher mortality rates,1,2,24,25 as well as difficulties with health care access, 26 including barriers to needed screening 3 and treatment. 27
Non-Hispanic Black decedents were significantly more likely to receive a palliative care consultation. A previous study on palliative care consultation rates among inpatients with cancer found that Black patients have higher odds of receiving consultations,28,29 possibly due to higher rates of advanced colorectal cancer diagnosis, along with likely increased symptom burden, complications, and mortality.1,2,24 Additionally, disparities exist in the receipt of outpatient, timely palliative care. 30 The higher rates of palliative care in the inpatient setting among non-Hispanic Black decedents in our study might compensate for limited access to palliative care specialists in the outpatient setting. Hispanic decedents had the lowest rates of palliative care consultation. It is unclear whether language barriers, lower health literacy, or provider-related barriers may have contributed. 14 Non-Hispanic Black decedents, and to a lesser extent Hispanic decedents, received less hospice care compared to non-Hispanic White decedents, which aligns with prior literature.10,14 This finding could be due to the higher mortality at a younger age experienced by non-Hispanic Black colorectal cancer decedents, as hospice is more frequently used by older patients. 10 Lower rates of ACP 12 and less palliative care 30 earlier in the life course are other potential contributing factors.
Low Advance Care Planning Rates
Although no significant differences were observed between groups, the proportion of decedents who experienced ACP was 2.2% or less across all groups. While we examined ACP rates only in the last 30 days of life, national rates of timely ACP are low, 31 with noted disparities, 12 despite its known benefits, such as reducing the use of burdensome treatments, including chemotherapy in the last 14 days of life and inpatient and ICU admissions in the last 30 days of life. 32
Limitations
This study assessed colorectal cancer decedents in Texas and among patients ≥66 years old. This is an important limitation as recently, trends have pointed to rising colorectal cancer incidence in younger age groups with 20% of colorectal cancers in 2019 among patients 54 years or younger. 33 While we were able to report findings for non-Hispanic White, non-Hispanic Black, and Hispanic decedents, we were unable to include more granular data on other racial and ethnic minorities. Data were aggregated based on services billed to Medicare in the last 30 days of life and did not capture more detailed information such as patient or family preferences, which can be found in electronic health records or documented notes. Additionally, we used zip code data to assign patients their level of education and poverty level as a proxy for socioeconomic status.
Conclusion
Among Texan Medicare decedents with colorectal cancer, non-Hispanic Black and Hispanic decedents had higher health care utilization and less hospice care. Texan female decedents had less ICU admissions and used more hospice care compared to males. ACP rates were low across all groups marking an important opportunity for practice change to encourage more ACP completion, documentation and billing. Although more non-Hispanic Black decedents received palliative care consultation in the last 30 days of life, it remains unclear whether such consultations were provided earlier in the life course.
Footnotes
Author’s Note
Questions and queries regarding this study and associated data can be made to the corresponding author.
Acknowledgements
The collection of cancer incidence data used in this study was supported by the California Department of Public Health pursuant to California Health and Safety Code Section 103885; Centers for Disease Control and Prevention’s (CDC) National Program of Cancer Registries, under cooperative agreement 1NU58DP007156; the National Cancer Institute’s Surveillance, Epidemiology and End Results Program under contract HHSN261201800032I awarded to the University of California, San Francisco, contract HHSN261201800015I awarded to the University of Southern California, and contract HHSN261201800009I awarded to the Public Health Institute. The ideas and opinions expressed herein are those of the author(s) and do not necessarily reflect the opinions of the State of California, Department of Public Health, the National Cancer Institute, and the Centers for Disease Control and Prevention or their Contractors and Subcontractor.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by 2024 National Institute on Aging Sponsored Medical Student Training in Aging Research (MSTAR) program and the Data Management and Analysis Core for Comparative Effectiveness Research on Cancer in Texas (RP210130).
Précis
Texas Cancer Registry linked with Medicare data for patients aged 66 and older who died 6 months to 5 years after receiving a diagnosis of primary colorectal cancer from 2010-2018 was used to assess sex and racial/ethnic differences in health care utilization, advance care planning and associated outcomes in the last 30 days of life. More female patients were hospice enrolled compared to males while non-Hispanic Black patients had more health care utilization, and less hospice enrollment compared to non-Hispanic White patients.
Appendix
Definition of Outcomes.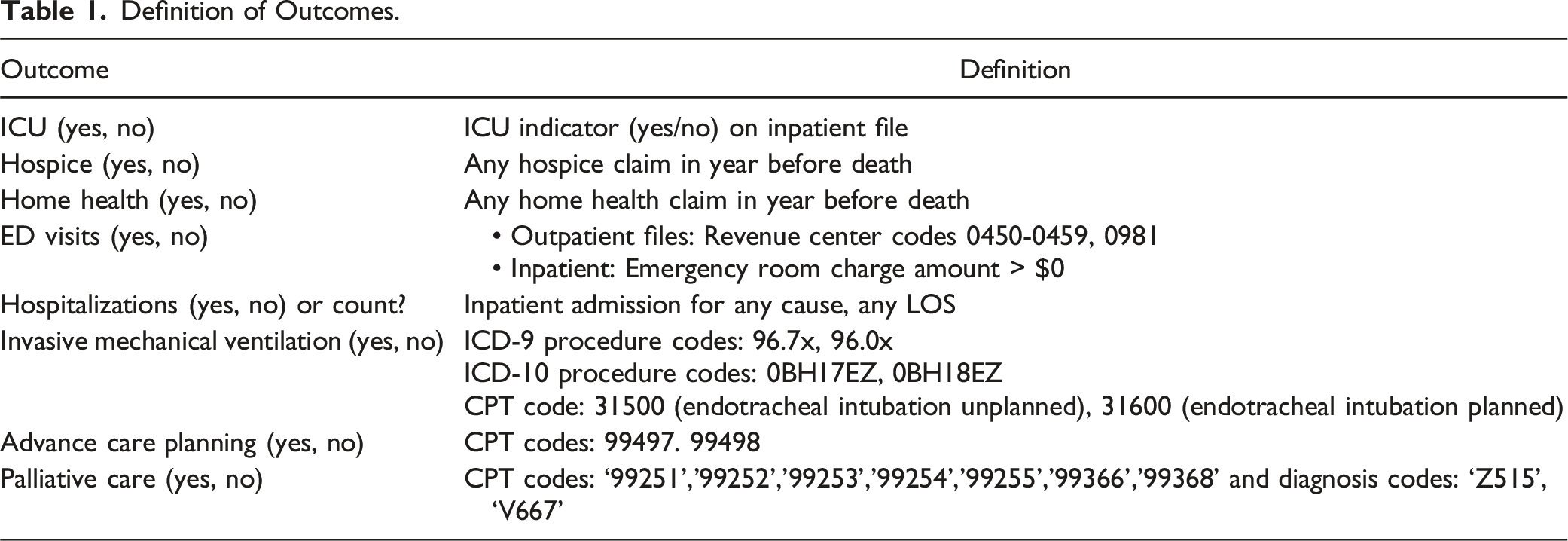
Outcome
Definition
ICU (yes, no)
ICU indicator (yes/no) on inpatient file
Hospice (yes, no)
Any hospice claim in year before death
Home health (yes, no)
Any home health claim in year before death
ED visits (yes, no)
• Outpatient files: Revenue center codes 0450-0459, 0981
• Inpatient: Emergency room charge amount > $0
Hospitalizations (yes, no) or count?
Inpatient admission for any cause, any LOS
Invasive mechanical ventilation (yes, no)
ICD-9 procedure codes: 96.7x, 96.0x
ICD-10 procedure codes: 0BH17EZ, 0BH18EZ
CPT code: 31500 (endotracheal intubation unplanned), 31600 (endotracheal intubation planned)
Advance care planning (yes, no)
CPT codes: 99497. 99498
Palliative care (yes, no)
CPT codes: ‘99251’,’99252’,’99253’,’99254’,’99255’,’99366’,’99368’ and diagnosis codes: ‘Z515’, ‘V667’
