Abstract
Background
Adult patients in oncological palliative care often do not readily express their concerns to physicians or nurses, leading to the oversight of needs that remain unexplored and require additional support. These needs that remain unaddressed are classified as unmet needs.
Aim
This study aimed to construct a conceptual framework of the unmet needs of cancer patients in palliative care settings. Method: Charmaz’s constructivist grounded theory approach was adopted. Semi-structured interviews were conducted with eligible patients until theoretical saturation was reached, as outlined by the methodology. The interviews were transcribed and analyzed through two coding cycles: line-by-line coding and focused coding, using NVIVO 14 software.
Setting/participants
A total of 29 patients were recruited from home palliative care, hospice, and outpatient settings at the Istituto Nazionale dei Tumori of Milan’s Palliative Care - Hospice, Pain Therapy, and Rehabilitation Complex Unit.
Results
This process led to the identification of five categories: Seeking Empowerment Through Daily Support, Need to Contain the Risk of Losing Dignity, Support in Managing the Progression of the Disease, Understanding and Openness to the Future, and Seeking Existential Support, along with a core category defined as the Need for Acknowledgment. The core category encompasses patients’ need to express their most intimate needs, emphasizing how crucial it is for them to be seen and understood not only as individuals facing illness but as people with unique, complex life stories.
Conclusions
The conceptual model developed enabled the identification of these hidden needs, providing a deeper understanding of the emotional and psychological dimensions that shape the experience of advanced illness.
Background
Today, cancer poses significant demands on health care systems, 1 with an estimated 20 million new cases and 9.7 million deaths reported worldwide in 2022. 2 As survival extends for those with incurable cancer, the growing population of chronic cancer patients 3 introduces increasing challenges due to treatment complexity and toxicity.4,5
Cancer patients experience various physical symptoms, influenced by cancer type, stage, treatments, and comorbidities 6 along with significant social, emotional, and psychological challenges,7,8 highlighting the need for specialized multidisciplinary care. 9 Indeed, integrating a palliative approach is essential to manage complex care needs of advanced cancer patients. 10
Palliative care optimizes symptom management and enhances the quality of life for patients and caregivers by addressing preparation for death and quality of dying.11-14 Defining a good death is complex and individual, but common themes include freedom from suffering, maintained autonomy and avoiding inappropriate prolongation of dying.15,16 It is essential to explore patients’ goals and expectations, create a plan, and communicate end-of-life care wishes with health care providers, while normalizing and demystifying this topic,17,18 and empowering informed choices, such as deciding where to spend the end of life.19-22
Terminal cancer confronts individuals with loneliness and stigma, compounded by role changes, family and financial issues, deepening their need to avoid isolation and not feel excluded from the healthy world.19-21,23
However, many patients hesitate to voice their concerns to health care providers, leading to the oversight of unaddressed needs; these needs that remain unaddressed and require additional support are classified as unmet needs,22,24,25 that lead to high symptom distress, anxiety, and reduced quality of life,26,27 often influenced by cultural differences. 28
A recent review of qualitative studies on unmet needs in palliative oncology care, highlights essential aspects that impact patient well-being like a secure and dignified end-of-life, continuity of care, validation of suffering, and time for personalized support that embrace the totality of the person, from the most obvious physical aspects, to the deepest aspects of the soul intimacy. 25 Patients need to feel valued as individuals, with their unique needs prioritized, in a patient-centered care environment. 29
Assessing unmet needs in individuals facing advanced cancer is essential,27,30 as these needs evolve over time, offering a valuable opportunity to improve overall health outcomes.27,31
Nevertheless, there is a significant gap in understanding the full range of patient experiences and needs. The complex and multifaceted challenges faced during this stage of cancer give rise to a broad spectrum of patient needs. 32 Insufficient attention to these aspects may result in fragmented care that fails to align with patients’ values and preferences. 25 In-depth studies are necessary to explore these needs from the patient’s perspective, uncovering nuanced and deeply personal aspects of care that are often overlooked. 25
As a result, this study sought out to address this gap by developing a theory to explain the processes underlying unmet needs among patients living with terminal cancer.
Methods
Charmaz’s constructivist grounded theory approach was used for this qualitative, single-center study. 33 This methodology is appropriate when there is limited knowledge about a phenomenon. 34 It uses an inductive-abductive logic, involving an iterative process where researchers move back and forth between data. Researchers make inferences from the data (inductive) and then verify them using theoretical sampling and additional data (abductive). Researchers are not separate from the research; knowledge is co-created with participants, 35 making the findings a co-construction of the researcher’s interpretations and the participants’ experiences. 36
The Consolidated criteria for reporting qualitative studies (COREQ) checklist was followed for reporting. 37
Setting
The research was conducted at the Istituto Nazionale dei Tumori of Milan’s Palliative Care - Hospice, Pain Therapy, and Rehabilitation Complex Unit, which offers a range of services, including home palliative care, inpatient Hospice, and outpatient palliative care service. Home care provides personalized support in the patient’s familiar environment, while inpatient Hospice offers more intensive care. Outpatient palliative care services allow patients to receive daytime care and return home in the evenings. This diverse setting enabled an in-depth exploration of unmet needs among terminal cancer patients across various palliative care contexts.
Sample
Participants were recruited using purposive sampling, to ensure variability in perspectives and experiences, with the sample size determined by theoretical saturation. 38
Patients included in this study were over 18 years old, receiving home palliative care services or admitted to the Hospice or Outpatient palliative care service at the Istituto Nazionale dei Tumori of Milan’s Palliative Care – Hospice, Pain Therapy, and Rehabilitation Complex Unit. They had a diagnosis of advanced-stage cancer (stage III/IV) and/or were in the end-of-life phase. Participants were recruited through referrals from health care providers within their respective settings to the research team, which identified eligible individuals according to the study’s inclusion criteriaAs the analysis progressed, theoretical sampling was used to seek additional data that could refine and elaborate the emerging categories, enrolling new participants who could provide deeper insights into specific aspects of the developing theory. Theoretical saturation was determined when gathering new data did not provide any new insights into the emerging categories. 38
Data Collection
Data were collected through in-depth, semi-structured face-to-face interviews. Charmaz emphasizes using intensive interviewing to closely attend to participants’ stories and construct theories. 39 All interviews were audio recorded and conducted by IB with the support of psychologist, SZ. Each patient was interviewed once in the environment they were in so either at home, hospice or outpatient palliative care service. For outpatients, an appointment was scheduled with the researcher to conduct the interview, to coincide with their next clinical visit. For hospice and home care patients, the researcher contacted them by telephone to arrange a suitable date and time for the interview. Both IB and SZ obtained written informed consent from all participants. They both have a clinical background in palliative care and qualitative research and professional relationships within research site. The interview guide was developed based on literature and research group discussions. After the initial interviews, it became apparent that there were important lines of inquiry; therefore, additional questions related to these topics were included. The initial interview guide is provided in the Supplement Material.
Demographic and clinical data for each patient, including age, gender, diagnosis, Karnofsky Performance Status (KPS), and level of awareness regarding their prognosis and diagnosis, were collected from medical records. The Karnofsky Performance Status (KPS) scale is a widely utilized tool for assessing the functional status of cancer patients, providing a standardized measure of their ability to perform daily activities. 40
Data analysis
Data collection and analysis were conducted concurrently, in line with grounded theory methodology. Interviews were audio recorded, transcribed verbatim by AB. The transcriptions were checked for accuracy 41 by LC, a PhD with a background in palliative care research. The data were analyzed by IL and LC using NVIVO 14 software through Charmaz’s method four steps: (1) initial line‐by‐line coding, (2) focused coding, (3) categorization of focused codes and (4) theoretical coding. Codes and emerging categories were discussed and agreed on by the research team. Preliminary categories were constructed from the coding process and were constantly compared with codes, and emerging categories to reveal new insights. This iterative process ensured that the emerging theory was firmly grounded in the data.36,42
Memo-writing during data collection and analysis, that documented emerging thoughts and insights, was used to develop ideas and explore relationships between codes and categories.
Rigor
The rigor was ensured by following Charmaz’s criteria for grounded theory33,36: credibility, originality, resonance, and usefulness. 36
Credibility was ensured through the accurate transcription of interviews, detailed field notes, constant comparisons, and collaborative review of the analyzed data by researchers to achieve consensus and mitigate potential bias.
Originality and resonance of the findings were achieved through ongoing interviews until data saturation and the use of the constant comparative method to validate emerging information.
Usefulness refers to the study’s contribution to knowledge that may be used by researchers.
Ethical Considerations
Ethical approval for this study was obtained from Comitato Etico Territoriale Lombardia 4 with the protocol number INT 127/23. Participants’ data were securely stored and encrypted to prevent unauthorized access. All electronic files were password-protected, and hard copies kept in a locked, secure location.
Informed consent was obtained from all participants before interviews, covering both consent for participation and access to their medical records. Participants were fully informed about the study’s purpose, procedures, data use, anonymity, and their right to withdraw without consequences.
Additionally, data management practices complied with the General Data Protection Regulation (GDPR) and institutional guidelines on data protection and ethical research.
Results
Twenty-nine patients were interviewed from February to September 2024, sufficient to reach theoretical saturation, including 5 patients at home, 13 in hospice, and 11 as outpatients. The mean age of participants was 65 years, with 15 males and 14 females. Most patients were diagnosed with metastatic lung cancer. The KPS score was 60, reflecting moderate functional impairment. In terms of awareness, 19 patients had full knowledge of their diagnosis, but only 10 were fully aware of their prognosis. The interviews lasted an average of 14.06 minutes.
Participants’ Characteristics.
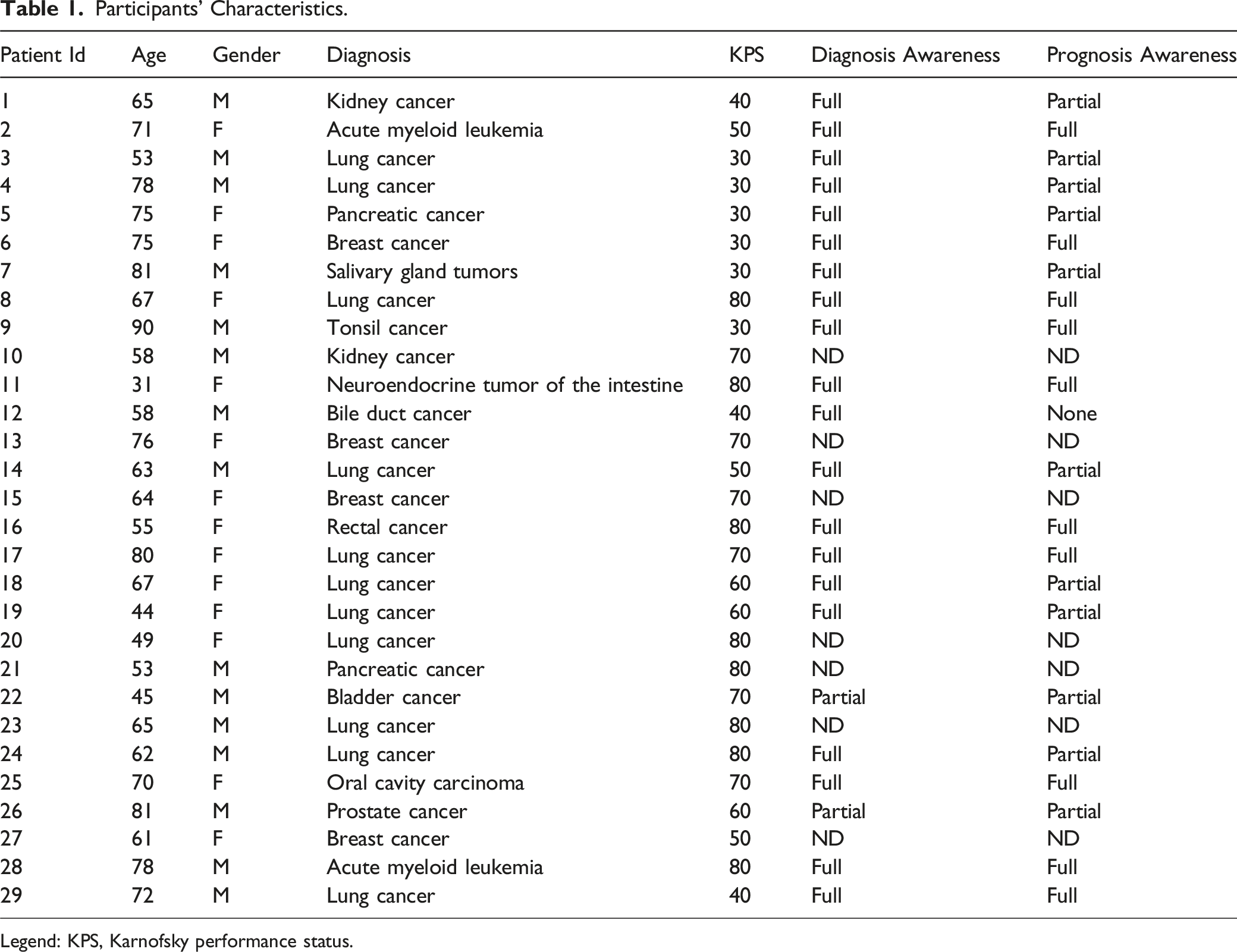
Legend: KPS, Karnofsky performance status.
Focused Coding, Categories and Core Category.
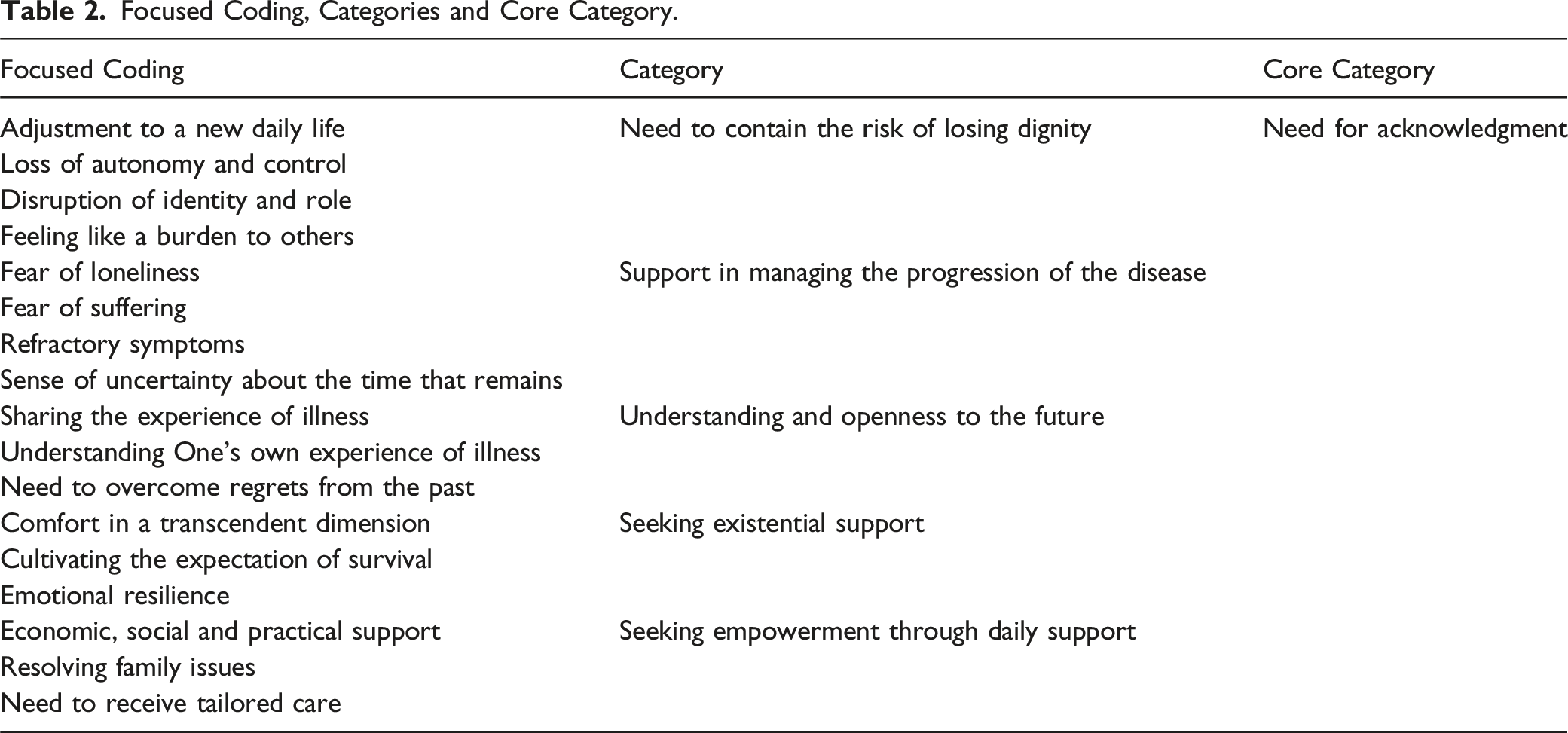

The core category is Need for Acknowledgment, reflecting the patients’ need for others to recognize and validate their deepest needs, hidden vulnerabilities, available resources, and those that need encouraging, in order to live the best possible life.
Figure 1 illustrates how the categories derived from the data analysis converge into the core category. Representation of the categories and core category of the theory.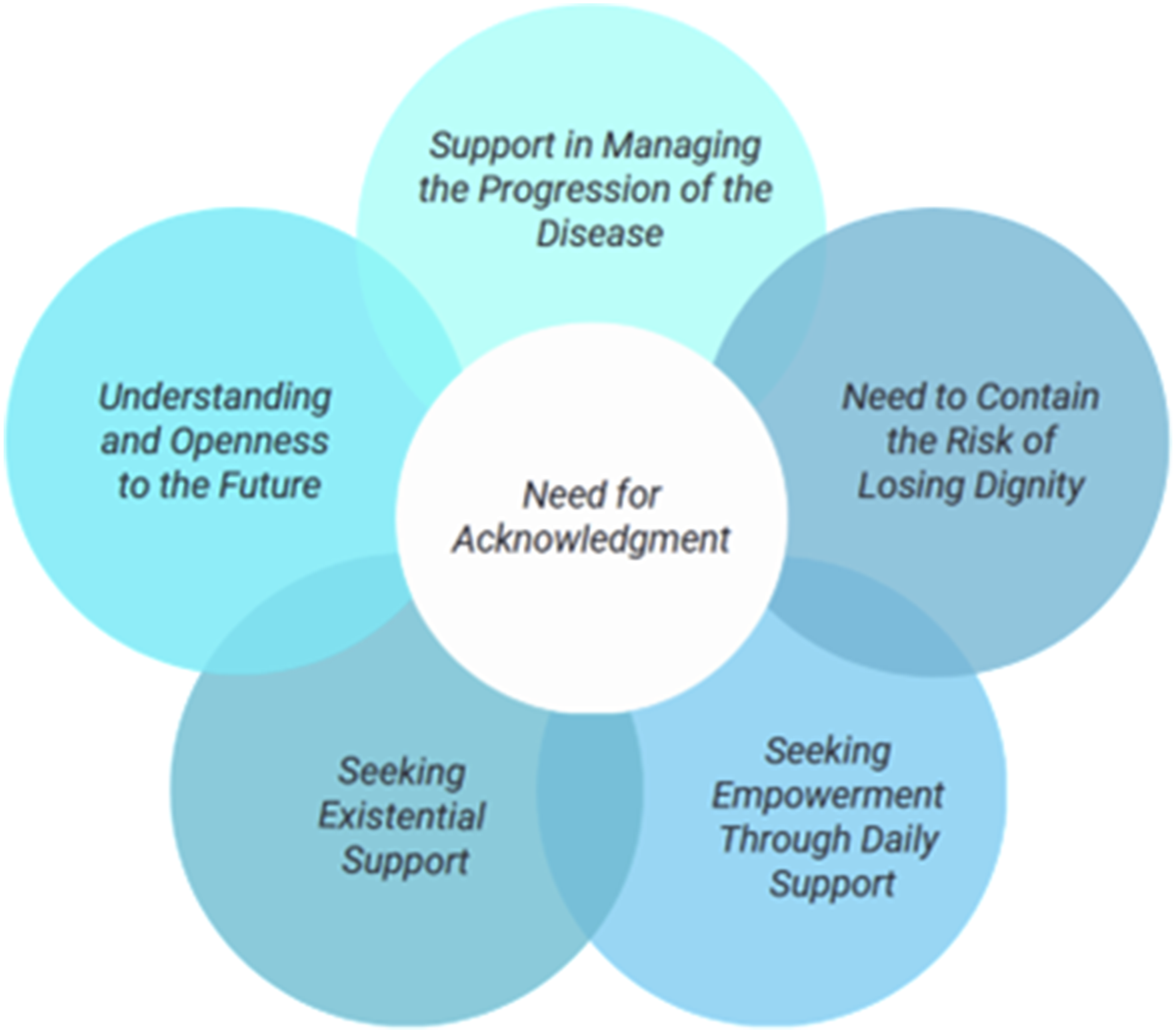
Seeking Empowerment Through Daily Support
Patients in palliative care often feel that the health care system is unresponsive to their vulnerabilities. They experience long waiting times, travel difficulties, postponed appointments, and conflicting opinions from professionals, resulting in feelings of disorientation and mistrust due to a lack of understanding and support.
One participant described the frustration of facing these challenges: “I was there for four hours waiting for them to call me. In fact, I said, 'I'm leaving because I'm just wasting my time here.”
Interview 1
To strengthen their empowerment, patients believe it would be helpful to bring closure to unfinished matters in their lives, particularly those related to their family, to prevent future difficulties for those who remain after they are gone.
Ensuring the well-being of loved ones becomes a key concern, as illustrated by one participant: “My thoughts are always about my son, about his family, the thought of not leaving him in situations, in a situation that then makes him, have to tribulate too much later when I'm not there.”
Interview 2
However, not everyone has the strength to navigate daily life independently, sometimes, external assistance is necessary for even the simplest tasks. Economic and social challenges can become overwhelming, intensifying existing stress and making it increasingly difficult to prioritize personal well-being. This is perceptible in the participants’ own words: “I pay a person to help me around the house because I can't, even if maybe I'm at home however I see that I don't have the energy even the mental energy to say this thing I'll put it here, this I'll put it there... instead sometimes I accumulate because mental fatigue creates all this confusion for me, so I accumulate things.”
Interview 25
Need to Contain the Risk of Losing Dignity
The central concern for patients is their identity in the eyes of others; they seek to be recognized beyond their illness and to maintain the image of who they were before becoming sick, preserving the roles they have built throughout their lives and to which they have always aspired.
As one participant pointed out, self-acceptance is a gradual and challenging process, requiring adaptation to new limits and changing needs: “In my opinion, a very significant need is that of self-acceptance, because it is not something taken for granted. When you find yourself having lived your life one way and then everything changes, you have to readjust to a new version of yourself. You must gradually accept all these things; it is not easy to come to terms with the new limits and the new needs you have.”
Interview 5
A sense of loss of control over their lives emerges in the words of the participants, thinking back to the life they had before, while simultaneously expressing a strong desire to regain that control. Even among those who claim to still maintain a certain level of control, there is a fear of losing that ability and the necessity of having to delegate.
This aspect is strongly evident in the interviews; notably, one participant characterizes the fear of losing control as a profound threat to their autonomy and self-determination. “It makes me feel vulnerable to know that I don't have control; I have always had control over everything in my life.”
Interview 26
Patients feel profound sadness and nostalgia for their former lives, emphasizing the gap between their expectations and current reality. Each new limitation diminishes their sense of identity and independence; activities like going to the movies or outings with friends shift from being ordinary to extraordinary desires. The focus changes from normalizing their condition to learning to live with it, finding a new balance, and reassessing priorities.
This change is reflected in the words of one participant, who highlighted the desire for normalcy rather than extraordinary experiences: “In everyday life, the nonsense, the hogwash – these are the reasons why I need to... have... I don’t want anything extraordinary, just what is normal.”
Interview 27
This journey extends beyond the individual, as the loss of normalcy can evoke feelings of being a burden to others rather than a contributor. Such sentiments can significantly alter the dynamics of relationships with friends and family, impacting the quality of interactions.
As one participant painfully acknowledged, the perception of being a burden weighs heavily on their well-being: “I got it into my head that I am a burden towards some people, some family members, because I create a bad life for them as well basically, because this is a terrible life”
Interview 21
Support in Managing the Progression of the Disease
The uncertainty regarding the course of the illness and the manner of the end of life leads patients to hope for a gentle passing, characterized by minimal physical and emotional suffering, wishing to face this moment with serenity.
The desire to avoid suffering is further underscored by one participant, who expressed a profound fear of confronting the moment of death: “The fears…the fears are there, the fears are there, I mean I would like, I would like if it happens that I don't understand, because if I understand I go crazy”
Interview 21
The most frightening thing, beyond the pain itself, is facing everything without human closeness. When alone, the mind wanders, inevitably returning to the thought that the end is near. The presence of someone else can offer not only moments of distraction and lightheartedness but also a sense of security, shared experience and relief.
One participant reflected on the comfort offered by companionship during such vulnerable moments: “There are always maybe times when I'm maybe more alone, I have more time to think, that then maybe I have some weak moments”
Interview 12
The uncertain waiting these patients experience creates a deep sense of precariousness, both in their current situation and in how to fill their remaining time. This uncertainty leads them to question their future, often leaving them without the answers they seek.
One participant vividly described the intensity of these thoughts, especially during the night, when they are most overwhelming: “When I can’t sleep, I start to think about how it will end, how it won’t end, how much time I have, how much time I still have... and then it’s... it’s at night that all these thoughts come to you, right before you sleep.”
Interview 1
Understanding and Openness to the Future
The emotional burden of a terminal diagnosis can be overwhelming, but sharing it with a confidant, often a family member or close friend, can lighten the load. Indeed, patients emphasized the importance of having someone to share their evolving experiences and emotions.
One participant described the comfort of receiving such support and the relief of the possibility share the burden of what they were experiencing: “Help from others, even simply as a shoulder, helps me to vent, to declare what I have, to not be afraid to have what I have, to be open.”
Interview 13
Physical presence does not always guarantee deep understanding, and the strain of suffering can lead even close friends to distance themselves. This often results in a shift in interpersonal relationships, leaving patients feeling misunderstood, even by those who have previously been supportive.
As one participant explained, the societal tendency to deny or push away the realities of illness and death often contributes to this emotional distance: “Because in my opinion many people are not able to accept the disease even if it is not, it is not their own. There is a society in my opinion for heaven's sake eh... where a little bit pain and illness, death (is moved) are a little bit denied, pushed away. […] ”
Interview 23
In order to look to the future, there remains a need to look back and reflect on one’s past. Some regrets may surface over missed opportunities or things left undone, yet there is also a strong desire to move forward and rise above them.
One participant critically reflected on this complex emotional experience, expressing a sense of regret while simultaneously acknowledging the inherent limitations of retrospective analysis: “Especially in the beginning maybe checks done earlier eh maybe wouldn't have changed anything, no one has a crystal ball we can't know, eh however... neglecting symptoms here on that yes a little bit of regret I have.”
Interview 29
Seeking Existential Support
The mind often succumbs to persistent thoughts about death and the unknown, leading to feelings of overwhelm. In these moments, cultivating emotional resilience becomes essential, not by denying reality but by confronting it. Developing strategies to address these emotions allows individuals to find serenity and clarity, enabling them to better manage their fears and uncertainties.
One participant described how they sometimes found the strength to momentarily set aside their fears, using courage to manage the intensity of their emotions: “It takes on a whole other, let's say another flavor, that is, another point of view and ... sometimes you manage to, to let's say you have courage and you put it in the corner for a moment this fixed thought that's there, other times you get overwhelmed.”
Interview 15
Between reality and hope, patients experience moments of overwhelm, followed by instances in which the hope for recovery and a return to well-being arises. This hope, although at times irrational, serves as an emotional refuge, allowing them to imagine a better future, even if only temporarily.
One participant emphasized the fluctuating nature of hope as a significant source of emotional comfort: “The hope would be to get well, live four or five more years peacefully quietly, continue to ... to live.”
Interview 19
Therefore, patients develop personal strategies to navigate between these extremes, often finding comfort in transcendence. Through the connection to a higher dimension, patients gain the strength to accept the finiteness of earthly existence, leading to a profound sense of inner tranquility. As one participant pointed out, this approach contributed to the emotional coping, stating:“In fact I from the very beginning told the doctors you continue with your therapy I go on my way, in the sense, I try to pray, I have people praying for me, this is very important.”
Interview 25
Discussion
This study explored the unmet needs of cancer patients within palliative care. In spite of the heterogeneous sample, the central category Need for Acknowledgment, managed to gather and unite their perspectives on their deepest needs. In their quest to be fully recognized, first and foremost as a person, then as a patient facing terminal illness, patients express a deep need for acknowledgment of their needs, desires, and expectations. It is not merely about receiving practical assistance; rather, it is about feeling truly heard and understood, so that their journey is not reduced to a mere clinical course but is acknowledged in its full human, emotional, and identity-related complexity.
As highlighted by previous studies, 25 hidden needs cover a wide range of areas, reaching deeper dimensions of the individual as terminality progresses. The results of our study contribute to this understanding by providing an explanatory model for these evolving needs.
Practical support and assistance with daily activities have emerged as some of the most immediate and tangible unmet needs, leaving patients increasingly dependent on others. In this vulnerable state, relationships with family members and caregivers are crucial for maintaining an acceptable quality of life. However, for individuals without a family support network and relying solely on their financial resources, this dependence becomes especially complex, highlighting not only financial challenges but also a profound loneliness that require urgent attention.19,20,23
The loss of control over life has also emerged in previous literature, 25 but from the words of the patients in this study, this concept is closely tied to the preservation of dignity. Regaining control over practical and material aspects is essential not only for maintaining autonomy but also as a pathway to reclaim empowerment and a sense of security.
This condition brings with it a sense of loss, not only of physical freedom but also of personal identity. Patients begin to see themselves as a burden to others, fearing that expressing their pain may weigh heavily on loved ones. Once active protagonists in their own lives, they now face a reality that no longer reflects their prior sense of normalcy, intensifying feelings of disconnection.
Although painful, this change leads to self-discovery, revealing new vulnerabilities as well as inner strengths. Through this process, patients strive to find a new balance between who they were and who they have become, a balance that will accompany them in the time they have left. They express a need to affirm their identity beyond the illness, resolutely seeking to maintain their roles and relationships, both socially and within the families they have built over their lives. Additionally, they yearn for security and reassurance in a reality increasingly dominated by unpredictability.
Existential support emerges as a cornerstone resource, one that patients heavily rely on and wish to see recognized as an integral part of their care. Turning to a transcendent or higher power appears as an internal strategy to give meaning to present and future events, providing purpose in a life trajectory marked by uncertainty.
A new need thus emerges: the need for emotional resilience, an inner strength to reinterpret suffering as an opportunity for personal growth. The hope for healing, more than ever, is seen as a driving force to face the time remaining. Even if the goal of recovery seems unattainable, the need to sustain hope is experienced as an integral part of their existential journey, underscoring the importance of acknowledging and supporting this personal outlook on the future.
All these elements, if properly recognized and addressed, contribute to defining a good death, facilitating a peaceful and dignified end-of-life experience.15,16
This study contributes to enriching the literature on oncological palliative care by proposing a new interpretative framework to understand the unmet needs of patients, with the emergence of the need for acknowledgment as a central category. The results highlight how this need is the deepest and most transversal, influencing and intertwining with all other needs, conditioning their expression and perception. The need for acknowledgment, therefore, represents the relational foundation upon which the entire course of illness is built. Recognizing and addressing this need appropriately can significantly improve the quality of the caregiving relationship, allow for the anticipation of latent needs, and promote truly person-centered care.
Strengths and Limitations of the Study
We developed a model of unmet needs in the context of oncological palliative care using a rigorous methodology that allowed us to elicit and focus on the patients’ perspectives, coming from different palliative care settings. However, this study has some limitations like the single-center nature of the study. The terminal stage of illness in the sample posed a significant challenge both in the participant recruitment phase and in the conduction of interviews. Further research could be conducted before clinical decline to overcome these limitations and enrich the range of unmet needs. Additionally, the use of heterogeneous data collection settings may have influenced the results, offering a broad view of experiences rather than addressing setting-specific needs. Finally, data were not returned to patients as their very short prognosis, limiting the ability to compare findings with them.
Conclusion
This study underscored the importance of exploring the unmet needs of the palliative care population, revealing a deep-seated need for recognition of often overlooked aspects of patients’ experiences. The conceptual model developed through grounded theory identified these needs, offering a deeper understanding of the emotional and psychological dimensions of patients in advanced illness stages. However, further research is needed to deepen and expand our understanding of these unmet needs in a manner specific to individual palliative care settings through the development of specific assessment tools to facilitate their identification and satisfaction.
Supplemental Material
Supplemental Material - Unmet Needs of Palliative Cancer Patients: A Grounded Theory Study
Supplemental Material for Unmet Needs of Palliative Cancer Patients: A Grounded Theory Study by Ilaria Basile, Letteria Consolo, Anita Bellani, Daniele Rusconi, Simonetta Zappata, Augusto Caraceni and Maura Lusignani in American Journal of Hospice and Palliative Medicine®.
Footnotes
Acknowledgments
The authors would like to express their gratitude to the patients who participated in this study, generously sharing their experiences and emotions while already navigating a challenging journey.
Author contributions
IB, LC, and ML conceptualized the research aim and developed the study methodology. IB and SZ conducted the interviews, while AB transcribed them verbatim, with LC verifying the accuracy of each transcription. IB, LC, SZ, and AB analyzed the collected data, following an inductive process to categorize the results, ultimately identifying the core category of this grounded theory. IB, LC, and DR contributed to the writing and editing of the final report. ML and AC provided critical revisions to the manuscript. All authors read and approved the final version.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical Statements
Informed Consent
All participants provided written informed consent before the interviews commenced. They were fully briefed on the study’s purpose, procedures, their right to withdraw at any time without consequences, and how their data would be protected and used.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
