Abstract
Introduction
Palliative care (PC) is delivered in both hospital and outpatient settings to provide an integrated approach to quality of life for patients with life-limiting illnesses and their families.1-3
PC delivery has changed over time, particularly in how hospital-based PC services operate. Initially, in-hospital PC services were aimed towards patients with cancer and terminal care, but increasingly, there is a focus on providing equitable access to those with non-malignant conditions.4-6 There is also a paradigm shift from equating palliative care with end-of-life care, towards provision of PC concurrently with disease-targeted therapies, 7 as PC has proven effective at preventing and relieving suffering through early assessment and symptom management. 8 As demand for PC in the hospital setting has increased, many hospitals employ PC staff to provide care either through specialist consults or in designated PC units. Despite these changes, hospitals continue to find it challenging to integrate inpatient PC with curative care or disease-targeted treatment. 9
Early access to PC is also critical for reducing burden on healthcare systems, particularly as the population ages and faces increased burden from chronic diseases. 2 Additionally, early access to PC has been shown to decrease healthcare expenditures by reducing medically unnecessary hospital presentations and investigations, the length of inpatient admissions, and the utilization of intensive care services. 1
Despite this, early integration of PC in a patient’s disease journey is seldom seen in practice.9-11 Even when PC services are readily available, physicians delay referral despite patients meeting referral criteria. 12 PC is frequently poorly integrated and called for too late during an illness, and though this issue has long been recognized, it remains a persistent challenge.10,11,13 To improve the timely provision of PC, it is necessary to characterize barriers and facilitators to its early integration. Much of the contemporary work has been undertaken within the American context. In contrast to the American model of health care, Australia adopts a hybrid model whereby the Government provides basic-level insurance (universal healthcare) known as Medicare, and individuals can choose to supplement this by purchasing additional private health insurance. Medicare provides palliative care and inpatient or hospice care in a public facility free of charge. However, patients may also utilize private insurance to cover additional or alternative private services and may incur out-of-pocket costs or ‘gap-fees’ for certain medicines or specialist appointments that are not fully covered by Medicare. 14 Factors impacting on the provision and timing of PC in an Australian context have been minimally explored.
Aim and Objectives
The aim of this study was to identify multi-disciplinary facilitators and barriers to inpatient PC in Australian hospitals through a scoping literature review.
Methods
This scoping review was undertaken in accordance with the methods described by Arksey and O’Malley 15 and Levac et al 16 and reported according to the Preferred Reporting Items for Systematic Reviews and Meta-Analysis (PRISMA) statement. Consistent with these methods, thematic domains identifying key types of barriers and facilitators were generated through exploration of the data to help generate hypotheses regarding which key factors are most likely to impact PC provision in hospitals.
Search Methodology
We searched 3 databases (CINAHL Plus, MEDLINE and Embase) from 2000 up to April 2024 to focus on more current models of palliative care. The search strategy used medical subject headings (MeSH) as well as key terms related to ‘inpatient,’ ‘palliative care,’ ‘Australia’ (inclusive of state names as well) and ‘hospital.’ The search strategy as implemented in CINAHL is contained in our supplementary materials. Titles, abstracts, and full texts were independently screened by 2 researchers against the inclusion and exclusion criteria. We pre-specified our methods in an unpublished protocol.
Study Selection
Eligible articles included those (1) written in English, (2) published from January 2000 through April 2024, (3) focused on the hospital setting and based in Australia, (4) limited to an adult population (18+ years), (5) related to palliative care in hospital, (6) referring to collaboration with non-palliative care clinicians, and (7) including palliative care professionals. Studies were excluded for the following reasons: (1) in home-based hospice or sub-acute settings; (2) focused solely on patient outcomes; (3) focused on paediatric care; (4) did not include any palliative care expert or team involvement (for example, a rejected study focused on the difficulties faced by renal nurses in end-of-life care); (5) did not address carer-specific issues (for example, studies that looked exclusively at patient outcomes for palliative care). Conference abstracts and letters to the editors were also excluded. We extracted the following information: study design, study duration, study setting, study population, data collection methods, study aim, and barriers and facilitators to PC practice.
Quality and Risk of Bias Assessment
The quality of eligible articles was evaluated by 2 independent reviewers using Joanna Briggs Institute’s (JBI) critical appraisal tools. 17 Checklist scores were converted to percentages to compare quality across study design, and a percentage less than 30% was defined as unacceptable, although no studies fell below that threshold.
Data extraction from articles identified the process by which PC staff worked with or integrated into usual medical care in the inpatient setting and identified potential barriers and facilitators to PC referral and use. From the extracted data and in consultation with palliative care specialists, barriers and facilitators were categorized into 7 domains: (1) Patient concerns, (2) Family concerns, (3) Clinician knowledge, education, and experience in palliative care use, (4) Recognition and acceptance of prognosis when a patient was dying or needing end of life treatment, (5) Reconciliation of individual and professional values around PC, (6) Clinician access to resources for PC in the hospital, and (7) Communication between the PC team and hospital ward clinicians. These domains were developed to fit the specific issues of the use of PC services in hospitals but were adapted to this context from The Theoretical Domains Framework, which applies psychological theory to healthcare implementation. 17 We charted data in a table to visually convey which studies informed each of the theoretical domains. 18
Results
Our search returned 1029 studies, 34 of which met inclusion criteria. A PRISMA diagram in Figure 1 summarizes this process. PRISMA diagram of the study selection process.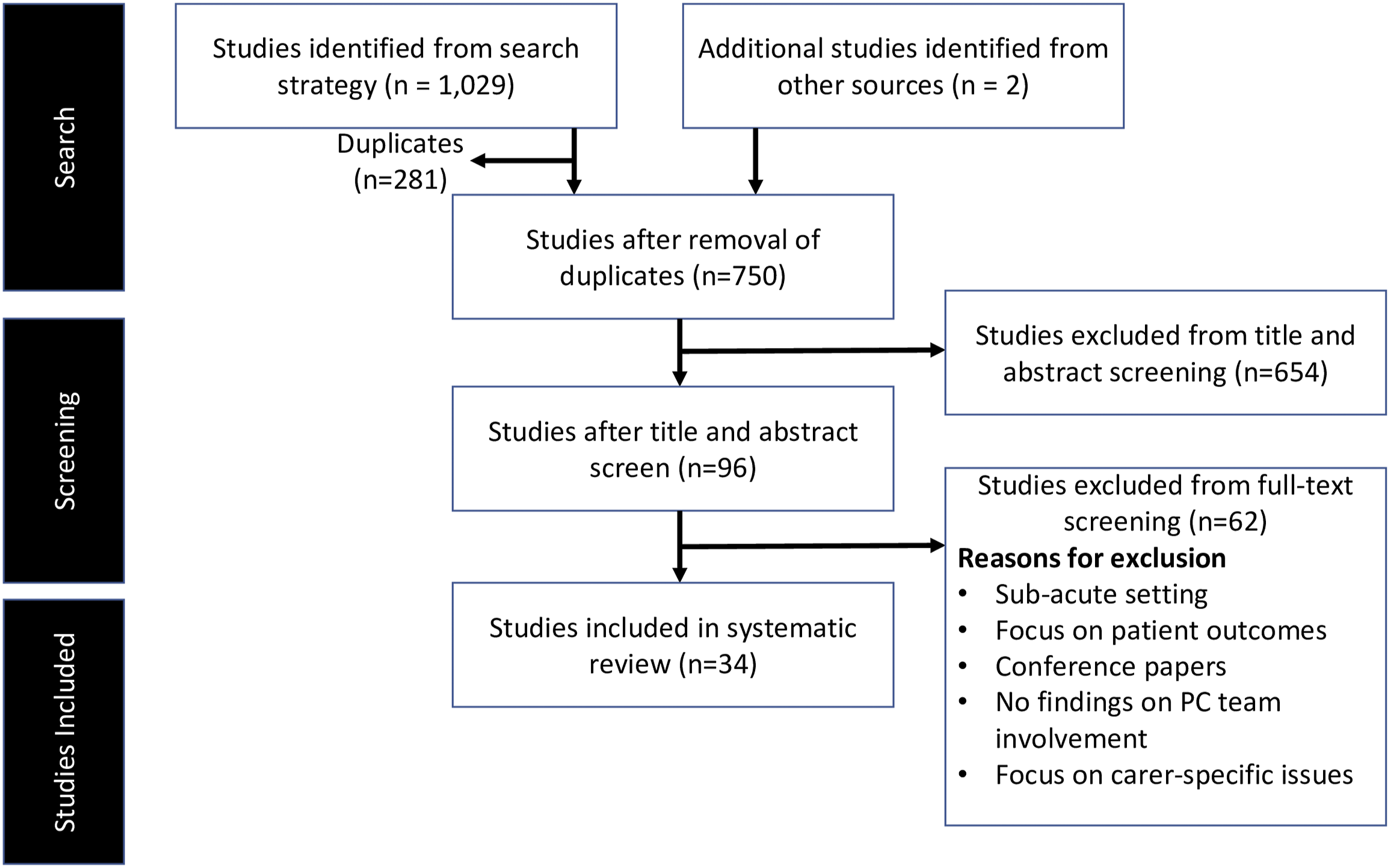
Study Characteristics
Most studies collected data in Australia’s 3 most populous states, with eleven from Victoria,6,13,19-26 8 from New South Wales,27-34 and 6 from Queensland.35-40 Two studies were completed in Western Australia,41,42 2 in South Australia,43,44 and 1 in the Australian Capital Territory. 45 Two studies used data from national surveys of clinical professionals but did not report how these professionals were distributed across the country.46,47 The locations of the hospitals involved in the 2 remaining studies were not reported.10,12
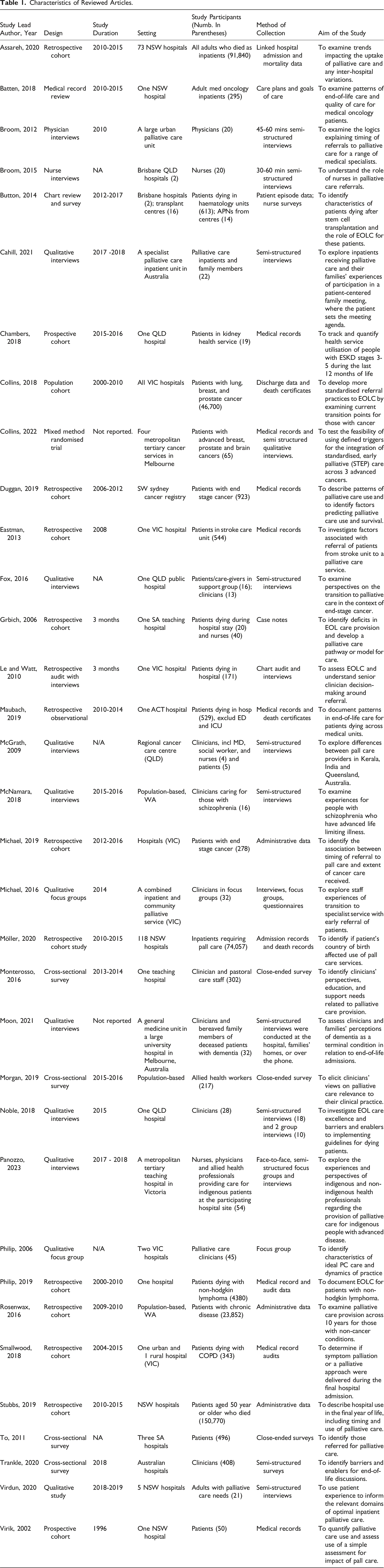
Characteristics of Reviewed Articles.
Facilitators and Barriers
In reviewing the barriers and facilitators to PC service use, we developed 7 domains to define types of barriers and facilitators: (1) Patient concerns, (2) Family concerns, (3) Clinician knowledge, education, and experience on palliative care use, (4) Recognition and acceptance of prognosis when a patient is dying and end of life treatment is needed, (5) Reconciliation of individual and professional values around PC, (6) Clinician access to resources in the hospital, and (7) Communication between PC and clinicians.
Domain 1: Patient Concerns
Patient reluctance to engage with palliative care was a commonly identified theme, and studies highlighted several reasons for this.25,38,39 McGrath et al 38 noted that feelings of pride and independence and the stigma associated with dying, in addition to preferences to stay home rather than enter hospice or inpatient PC, made patients reluctant to seek palliative care support. Michael et al 25 and Fox et al 40 also reported that patients had strong negative connotations regarding palliative care. Fox et al 40 reported that clinicians heard negative views of palliative care from patients, which subsequently led clinicians to be reluctant in making referrals.
Negative views of palliative care sometimes arose from misperceptions, which were discussed in articles by Fox et al, 40 Monterosso et al, 12 and Stubbs et al 31 Fox et al 40 found that patients often believed that PC focused only on physical symptom control and ignored or neglected psychosocial and spiritual dimensions of care. They also found that patients believed PC were appropriate solely for terminal or near terminal care and that a referral to PC meant that no further formal medical treatment was available for their disease. In other words, patients associated PC with the end stages in life journeys, 40 which was further supported in the research by Stubbs et al. 31
Patient or family resistance to palliative care services sometimes led clinical staff to delay PC referral. For example, Broom et al
35
found that medical oncologists felt that family or patient resistance prevented referral even when the oncology team was prepared to refer. Age of the patient had some impact on decisions to refer to PC, although there was conflicting evidence on the direction of effect. Duggan et al
29
reported a 20% increase in the likelihood of receiving early PC referral among those aged 85 and over as compared to people aged between 75 and 84 (RR1.2, 1.07-1.35,
Domain 2: Family Concerns
Family resistance to PC, particularly if they associated PC with a terminal prognosis, was noted in multiple studies, including Broom et al 35 and McNamara et al 41 Phillip and Komesaroff 23 also found that healthcare staff were reluctant to discuss palliative care if families discouraged discussion of prognosis or diagnosis. In some instances, family resistance arose from cultural beliefs that dying persons should not be told they were dying; McGrath et al 38 found such beliefs present among some ethnic groups from India, for example. McGrath et al also found these cultural values were occasionally present in the Australian context as well, although norms for clinical care in Australia support providing patients with transparent prognostic information. Finally, Grbich and colleagues 44 discussed how unique family dynamics could lead to reluctance to use PC services. For example, in 1 case, a daughter expressed concern that PC could not accommodate her wish to take her mother home. More generally across families, Grbich et al 44 noted several caregiver factors contributing to concern about PC, including distress or concerns regarding prognosis, the impact of medications on drowsiness, and dissatisfaction with the quality of care received by their loved ones. Family concerns could also be disease specific – Moon et al 7 found that families of patients with dementia were often unaware of its status as a life-limiting illness, which could lead to the continuation of futile life-prolonging treatments if this misunderstanding was not appropriately rectified by clinicians.
On the other hand, family members were also sometimes facilitators of PC use. McNamara et al 41 noted that family members played important roles as advocates of PC services. Similarly, Virdun and colleagues 33 reported that patients stressed the importance of family member engagement in PC. It was noted that when patients were cognitively impacted by their medical treatment, family members were indispensable for assisting the patient to engage in treatment discussions. Further, patients mentioned several ways in which hospitals can facilitate family caregivers taking on advocacy roles, including flexible visiting hours and regular ward round times, so that family members could balance visits alongside external commitments. Cahill et al 34 described formalized family meetings with an interdisciplinary team, which provided a forum for family concerns to be shared and addressed. These meetings sometimes facilitated greater acceptance of PC involvement.
Domain 3: Clinician Knowledge, Education, and Experience
The knowledge, education, and experience of the clinicians treating the patient was also influential. Broom et al, 10 McGrath et al, 38 and Monterosso et al 12 interviewed clinicians who emphasized that a lack of knowledge, experience, or inclination from clinical staff can delay or prevent PC referral. Stubbs et al 31 likewise found that shortcomings in the clinical judgement of doctors and nurses led to late PC referral. Michael et al 25 noted that poor clinician knowledge can result from insufficient training on what patients need with regards to palliative care, including uncertainty about how the principles of comfort care integrate with standard care, which is more often characterized as curative. On a related note, Panozzo et al 26 found that a lack of knowledge of indigenous cultural values sometimes resulted in sub-optimal relationships between PCS and indigenous Australians, which could complicate their access to care.
A facilitator for PC service integration was improvements in knowledge and experience around end-of-life discussions. Trankle et al 47 found that improvements in training and experience around end-of-life discussions could facilitate PC referral and could be gained through either job or life experience. They suggest such experience could be facilitated through peer mentoring, staff workshops, and role play.
Domain 4: Recognition of Dying
Multiple studies also identified clinicians’ failure to accurately recognize dying as a barrier to PC referral and as a cause of unnecessary interventions in the last days of life. Stubbs et al 31 compared the proportion of hospital decedents who received PC with the proportion who could have benefited from PC referral, and found that many dying patients were not appropriately identified as such. Stubbs et al hypothesized that an associated barrier was clinicians’ tendency to rely on their subjective clinical judgement of prognosis over objective diagnostic tools to identify eligible patients. Grbich et al 44 further found that recognition and documentation of the terminal phase occurred in only approximately 1 out of every 2 studied deaths. Maubach et al 45 found that rates of recognition of dying varied across specialties, with oncologists most likely to recognize dying and provide and communicate accurate forecasts.
Good documentation of advance care plans and comfort care plans was a facilitator for PC referral. Maubach et al 45 reported that documentation of comfort care plans was significantly higher in oncology wards compared to respiratory and cardiology wards. This study identified that the presence of goals of care documentation decreased use of active medical management, such as “dialysis, intubation and [Medical Emergency Team] calls” in the final 48 h of life. 45
Domain 5: Reconciliation of Individual and Professional Values Around PC
Clinicians’ professional values were frequently described as barriers to PC referral.35,40,47 Fox et al 40 found that oncologists delayed referral to PC if they saw themselves as effectively managing all patient needs. Broom et al 35 found that healthcare professionals would sometimes take on personal crusades against diseases or perceive an urgent need to treat in the case of some cancers, which then created a barrier to timely PC referral. Similarly, Trankle et al 47 found that clinicians perceived avoiding death as paramount, while Le and Watt 21 found that clinicians often became emotional about a patient’s dying. Consequences of this barrier could be significant.39,40 Noble et al 39 found that clinicians often focused too much on futile attempts at prolonging life, which led to delaying end-of-life discussions and/or PC involvement until too late in a patient’s illness.
Individual values or perceptions about PC also created barriers.21,31,35,40 Broom et al 35 reported that clinicians would delay PC referral to avoid the task of explaining PC to the patient. Stubbs et al 31 echoed this point, indicating that clinicians had difficulty initiating conversations about death, while a clinician interviewed by Fox et al 40 described not wanting to scare patients with a PC referral. And, finally, Philips and Komesaroff 23 described 1 GP who preferred to consider his patient as a friend, which ultimately resulted in failing to provide the patient with optimal medical care.
Domain 6: Access to Services and Resources
Access to PC services and resources was a key facilitator for providing PC referrals. For example, in studies by both Broom et al 10 and Assareh et al, 9 results indicated that the lack of onsite palliative care services at the hospital was a major barrier. When PC is present, Noble et al 39 found that hospital staff could still experience difficulty navigating the bureaucracy around PC referrals. In both qualitative interviews and focus groups, this study found that staff were confused about when to appropriately make palliative care referrals.
Several studies found that geographic location could be a barrier to receiving PC9,38,42 Assareh et al 9 found that patients from non-major urban areas received less PC and experienced delays in PC engagement compared to their urban counterparts. Similarly, Rosenwax et al.’s retrospective cohort study 42 found a statistically significant decrease in referrals to specialist palliative care for patients living in more remote areas and for patients living in aged care facilities. In McGrath et al.’s qualitative study, 38 patients indicated that financial costs of travel were a barrier to receiving PC.
Likewise, hospital resource availability could also be a significant barrier to receiving PC. Grbich et al 44 quoted a nurse who felt that the hospital staff could not provide sufficient staff to sit with dying patients as would have been needed to help provide dignified care for those at the end of life. Further, Fox et al 40 identified time constraints as key to providing clinical care, while in qualitative interviews with patients, Virdun et al 33 identified the lack of private rooms and available nursing staff trained in palliative care to sit with patients long enough to sufficiently assess needs as important barriers. In Noble et al.’s study, 39 interviewed subjects reinforced the need for more available palliative care clinicians.
Hospitals where palliative care specialists worked alongside other healthcare professionals, sometimes in multidisciplinary teams, were found to have improved facilitation of PC referrals in several studies. For example, Duggan et al 29 found that access to integrated centers with both oncology and PC services facilitated PC use. Michael et al 25 reported that access to a PC consultative service led to earlier access to palliative care as needed for symptom management. Finally, Noble et al 39 found that involvement of palliative-care trained nursing staff in multidisciplinary team meetings facilitated PC referral and access.
Domain 7: Communication Between PC and Clinicians
Dysfunctional relationships between PC and other healthcare professionals were commonly cited as a barrier to timely PC integration.10,23,35 Both Broom et al 10 and Philip and Komesaroff 23 identified the lack of working relationships between hospital clinicians and palliative care specialists as a barrier to effective PC to the extent that the clinical judgement of specialists was undermined, and patients perceived the lack of collegial relationships. In some cases, hospital clinicians felt that their care was criticized and were less likely to refer to PC, although Philip and Komesaroff noted that such issues were generally minor.
Multidisciplinary discussion between PC staff and other hospital clinicians was widely found to be a facilitator for PC integration.29,33,41,47 Duggan et al 29 found that multidisciplinary team discussion meetings were significantly associated with early PC usage. Multidisciplinary team meetings were found to improve visibility of the PC team and facilitate working relationships and referral pathways with hospital staff. Virdun et al 33 reported that patient perceptions of greater communication between PC and other hospital clinicians facilitated better integration of care. McNamara et al 41 found that involvement of general (family) practitioners, PC staff, and mental health workers in case conferencing and the sharing of lead roles across these parties facilitated improved referral and use of PC for patients with schizophrenia. Le and Watt 21 found that allowing nursing staff and allied health to communicate directly with the PC staff facilitated care. In addition, good working relationships with PC also facilitated improvement of PC competencies among non-palliative care specialists. For example, Le and Watt 21 noted that PC staff helped junior medical staff communicate with families and patients. Finally, Collins et al 13 found that formalized trigger points which mandated a referral to PCS could be an effective method of overcoming psychological communication barriers that might otherwise prevent these referrals being made.
Discussion
While early integration of PC with disease-targeted management has been linked to improved patient outcomes, PC remains underutilized. This is not surprising given the number of barriers identified in studies of Australian hospitals, which indicate significant issues in providing timely and needs-based PC in this context. Given the complexity of potential issues with implementation, additional training and education for clinicians alone will not suffice to facilitate implementation. Instead, hospitals need to be attentive to how to address patient and family concerns, how to provide greater resources for ongoing PC service use, and finally, how to influence clinician perceptions regarding the use of PC. Only by identifying and understanding the full set of barriers and facilitators, as we have attempted in this study, can we begin to move towards solution generation.
We identified perceptions among Australian patients (and to a lesser extent clinicians) that palliative care was either appropriate only for terminal care or was incompatible with standard or curative medical treatment. In the international literature, a distinction is made between palliative care, which manages the needs of patients with a serious or life limiting illness at any stage of their illness, and hospice care, which is explicitly reserved for patients nearing the end of life. 48 Both terms represent an approach to care and can be provided at home as well as in a facility. Conversely, the term hospice in an Australian context usually refers to a dedicated inpatient facility that delivers palliative care. 49 To members of the public, the terms are likely synonymous, which may contribute to the confusion and barrier to engagement that we identified in our review.
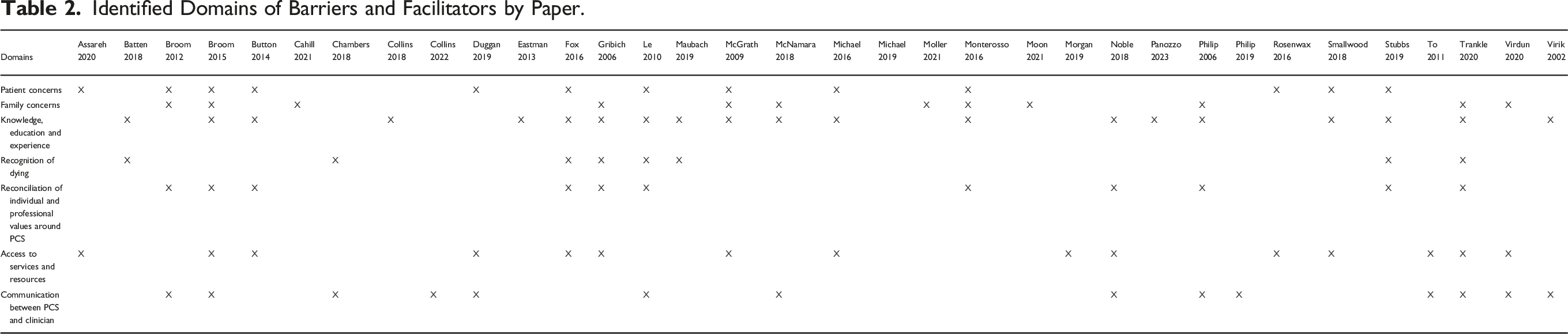
Identified Domains of Barriers and Facilitators by Paper.
Many of the studies that examined a range of barriers and facilitators drew heavily on qualitative analyses. For example, Broom et al 35 used semi structured interviews with 20 ward nurses to identify barriers to transitioning patients to palliative care. The qualitative studies we found examined multi-disciplinary factors but were limited by their specialized contexts. These studies also frequently lacked attention to deficits in local resources. In contrast, the included quantitative studies focused frequently on timing of referrals to palliative care and patients’ demographic variables associated with referral timing, but they lacked insight into the complexity of multi-disciplinary factors influencing PC referral. Monterosso et al 12 developed and used a survey tool that produced quantitative findings, but those study results were not directly relevant to interactions with the PC team. Trankle et al 47 provide the most comprehensive survey results on barriers to referrals using a survey of almost 400 clinicians, but their study was limited to clinicians’ communication around end-of-life issues. In summary, while the qualitative studies provided insight into the barriers and facilitators to PC delivery, there is limited understanding of the relative prevalence of these barriers and facilitators in Australian hospitals.
From this scoping review we intend to utilize the identified domains to develop a survey tool to collect data on facilitators and barriers to PC integration in Australian hospitals. This standardized survey could be applied across multiple sites and allow for future consistent identification in the literature of multidisciplinary barriers and enablers to palliative care referral. This would allow for comparisons between hospitals which cannot yet be made based on the studies in this review given they used unique question sets. It is hoped that this survey tool could contribute to filling the literature gaps identified in this review by producing estimates of the prevalence of specific barriers and facilitators to palliative care integration in Australian hospitals. Prevalence estimates will allow prioritization of future research. The survey and our initial findings will be reported in a subsequent paper.
Conclusion
This scoping review identified 7 domains of barriers and enablers to the early integration of palliative care services into patient care. Further efforts should be made to estimate their prevalence, in order to prioritize and design interventions to address barriers, and to leverage enablers to improve patient outcomes.
Supplemental Material
Supplemental Material - A Scoping Review of the Barriers and Facilitators to Clinician Engagement in Hospital-Based Palliative Care in Australian Hospitals
Supplemental Material for A Scoping Review of the Barriers and Facilitators to Clinician Engagement in Hospital-Based Palliative Care in Australian Hospitals by Edward Meehan, Catriona Parker, Darshini Ayton, Naomi Katz, Michelle Gold, Yufei Wang, Dasuni Ralapanawa, Xin Kwok, and Jane Banaszak-Holl in American Journal of Hospice and Palliative Medicine®.
Footnotes
Author Contributions
EM and CP contributed equally to the conduct of the literature review and the writing of this work and are joint first authors. EM, CP, and JBH carried out title and abstract screening, full text review, and data extraction. EM and CP drafted the manuscript. All authors contributed during the review and revision of the manuscript, and all authors approved the final version of the article, including the authorship list.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Data Availability Statement
This scoping review relied on published papers which are available to researchers through the relevant journals. We retain copies of the original data extraction spreadsheets, and we can provide these to researchers upon reasonable request.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
