Abstract
Heart failure is a complex, progressive syndrome with significant impacts on quality of life and daily functioning. This study aimed to understand the self-care experiences of community-dwelling adults with heart failure in Australia while also portraying the context and impact of these experiences on participants. We focused on patients’ accounts of self-care, irrespective of their alignment with existing definitions or guidelines. A qualitative approach using in-depth interviews was chosen to capture the richness of lived experience. Nine participants with heart failure were recruited through advertisements distributed by community heart support organizations and social media to take part in a one-to-one online or telephone interview. Data were analyzed using reflexive thematic analysis informed by a critical realist perspective. Three themes were developed, offering insight into how participants experienced self-care: “self-care as balancing the visibility and invisibility of living with heart failure,” “self-care as developing understanding and being (mis)understood,” and “self-care as navigating relationships.” This study shows that people with heart failure use self-care in ways that differ from traditional clinical expectations. The findings suggest that current heart failure management approaches may be missing crucial aspects of how people actually live with this condition. Participants were equally concerned with managing their social identity, maintaining family relationships, and integrating self-care into their existing life routines. Effective interventions need to address these broader concerns, not just clinical outcomes.
Background
Heart failure is a complex and progressive syndrome resulting from structural or functional abnormalities of the heart, which impair its ability to pump blood effectively and lead to symptoms such as breathlessness, fatigue, and fluid accumulation (Bozkurt et al., 2021; NHFA CSANZ Heart Failure Guidelines Working Group et al., 2018). The global prevalence of the condition continues to rise, driven by population ageing and advances in the treatment of acute events that have improved survival (Groenewegen et al., 2020). It is estimated that more than 64 million people worldwide live with heart failure (Savarese et al., 2023). In Australia, the condition affects approximately 1%–2% of the population, with over 66,000 new cases each year (Parsons et al., 2020; Sahle et al., 2016). The unpredictability of heart failure—the course of which is often punctuated by acute exacerbations that can lead to hospitalization, its incurable nature, and the associated reduction in life expectancy compared to the general population—further demonstrates the impacts of the condition (NHFA CSANZ Heart Failure Guidelines Working Group et al., 2018; Taylor et al., 2017). Beyond the human cost, heart failure also presents a significant economic cost to healthcare systems, primarily due to the high rate of hospitalization associated with the condition (Chan et al., 2016). However, it is thought that over half of heart failure hospitalizations are preventable through community support and individual behavior change (Johnston et al., 2020). In contemporary healthcare practice, it is widely accepted that active engagement and taking responsibility for health and care, herein referred to as self-care, benefits both individuals and the healthcare system (Jaarsma et al., 2020; Narasimhan et al., 2019; Riegel & Jaarsma, 2019).
Thus, the concept of self-care has been integrated into health management guidelines, which recommend a variety of self-care activities, ranging from taking prescribed medications to monitoring symptoms and contacting a healthcare practitioner when required (Heidenreich et al., 2022; Jaarsma et al., 2021; McDonagh et al., 2021; NHFA CSANZ Heart Failure Guidelines Working Group et al., 2018). At the same time, numerous interventions have been introduced to support the adoption of self-care in daily life, but the overall evidence in support of these interventions to improve outcomes for people with heart failure is inconsistent (Jiang et al., 2018; Jonkman et al., 2016; Lee et al., 2022). This, alongside the variation in how self-care is defined and understood across disciplines, has generated confusion and debate concerning the adoption and operationalization of self-care and related interventions (Ausili et al., 2022; Gantz, 1990; Tulu et al., 2021).
What is acknowledged is that developing effective interventions to support self-care requires an understanding of the lived experience, perspectives, and needs of individuals (Butler et al., 2023; Tait et al., 2015). However, people with heart failure are often seen as subjects requiring education as opposed to individuals navigating the complexity of life with a chronic condition (Greenhalgh et al., 2017). A conceptual shift toward recognizing people with heart failure as active participants in their care, and toward exploring what facilitates and constrains self-care, can strengthen the point of departure for developing new interventions and augmenting existing ones. This approach is also timely in contemporary healthcare contexts, where the expanding role of digital health is shaping new interventions that increasingly rely on remote technologies and reduce face-to-face interaction (Whitelaw et al., 2021). This study aimed to understand the self-care experiences of community-dwelling adults with heart failure in Australia while also portraying the context and impact of these experiences. We focused on participants’ accounts of self-care in the context of living with heart failure, irrespective of their alignment with existing definitions or guidelines. In the discussion, we highlight the importance and implications of our findings in relation to the development of self-care interventions, particularly those using digital health.
Methodology
Study Design
This study was part of a larger research program aimed at developing a digital health intervention to support heart failure management in Australia (Maddison et al., 2025). It was proposed that the intervention would include remote patient monitoring via smart devices (e.g., wearables and smart scales), personalized self-care support, and communication with healthcare providers. To contribute toward developing an acceptable intervention, we sought to understand the experiences, perspectives, and needs of people living with heart failure in Australia—with a focus on self-care. To address this aim, this study used a qualitative, experiential design underpinned by a critical realist ontology. This approach enabled the exploration of both individual experiences of self-care and the broader contextual factors shaping those experiences. Data were collected using semi-structured interviews and analyzed using reflexive thematic analysis (Braun & Clarke, 2006, 2019).
Reflexivity and Positionality
The first author, a digital health researcher from the United Kingdom, with experience in public health and qualitative interviewing, led the study design and analysis. This author was completing a PhD on the potential for digital health to support heart failure self-care in Australia at the time of the data collection and analysis. Two researchers conducted the interviews; the first author conducted seven and a research assistant with experience in research interviews and group facilitation in health settings conducted the other two. The two interviewers met to discuss their experiences after their first interviews and periodically did this throughout the process, forming a platform to challenge and develop interpretations and assumptions. The first author also discussed the research with two further researchers who both have clinical experience, providing further insight and challenge. Moreover, the first author’s work with a dataset of images from wearable cameras worn by people with heart failure informed the interview guide for this study, the images serving as a tool to reflect upon the lived experience and self-care practices of people with heart failure; this work is described further elsewhere (Nourse, Cartledge, et al., 2022). Throughout the research process, the first author engaged in ongoing reflexive practice. This included making informal notes after interviews and during data familiarization. These notes captured reflections on the interviews themselves, thoughts and feelings about the research process, and considerations of how the first author’s professional background may have shaped interactions with participants and interpretations of the data.
Participant Recruitment
This study sought to recruit adults with a self-reported diagnosis of heart failure (over 18 years) who were community-dwelling (living independently as opposed to a hospital, nursing, or other care facility) in Australia. There were no further limits on participant location, as we sought to understand a range of experiences from different locations and healthcare settings within Australia. Additionally, eligibility for the study included the ability to provide informed consent and participate in an interview in English. Exclusion criteria were severe heart failure (persistent New York Heart Association Class IV), recent myocardial infarction, unstable angina, referral to an advanced heart failure transplant unit, severe chronic pulmonary disease (i.e., requiring home oxygen), living in a long-term care establishment (e.g., a care home), or being unable to participate fully in the study for other reasons such as dementia. These criteria reflected the target population for the SmartHeart intervention: community-dwelling adults with heart failure able to engage in self-care with relative independence, without the need for intensive medical care.
The principle of information power, which takes into consideration the amount of information in the dataset and its ability to generate adequate data to tell a rich story about the self-care experiences of people with heart failure, guided the choice of participant group size (Braun & Clarke, 2021; Malterud et al., 2016). Advertisements were placed on social media and website of the university department, and the same advertisement was distributed by two support organizations for people with cardiovascular conditions. This sampling method allowed for targeted outreach and individuals to voluntarily exhibit interest in the study. The advertisement contained contact details for the research team and a web link to information explaining the purpose, procedures, and potential impacts of the study. Interested participants were asked to complete an online form, or contact the research team, to screen for their eligibility and consent to participation. Once written informed consent was received, an interview was scheduled at a convenient time for the participant. At the time of the interview, the interviewer briefly described the research and procedures again and gave each participant time to ask questions before asking them to reconfirm they were willing to take part. All participants were provided with an AUD$20 e-gift card after completing the interview.
Participant Characteristics and Context
Nine participants, comprising three females and six males, aged between 29 and 84 years (average 56 years), participated in the study. Participants were from regional and metropolitan locations across four states in Australia. The time since the participants had been diagnosed with heart failure ranged from 10 months to 16 years, and most participants reported at least one comorbidity, such as type 2 diabetes. Seven participants lived with at least one family member and two lived alone. Three participants were working, and the remaining six participants were retired either for medical reasons or voluntarily. Importantly, as the participants were all recruited through the cardiovascular support organizations, they were engaged with services to support their health and self-care which allowed for an exploration of both the enabling factors and barriers to self-care through the analysis of their experiences.
To provide local context for this research, the Australian healthcare system operates using a hybrid model in which people can purchase private insurance in addition to the mandatory public insurance scheme called Medicare (Dixit & Sambasivan, 2018). Both public and private heart failure services are available. Approximately 80% of people with heart failure in Australia rely upon a general practitioner (GP) for long-term management of their condition (Kalsi et al., 2022; Parsons et al., 2020). Additionally, some people have access to specialist clinics led by multidisciplinary teams that provide services such as education, group exercise programs, and medication review (NHFA CSANZ Heart Failure Guidelines Working Group et al., 2018). However, access to these services is limited in many regional and rural locations (Leach et al., 2022). There are also a range of community programs that coordinate peer support groups and provide access to educational tools and resources (Heart Foundation, n.d.; Heart Support Australia, n.d.).
Dataset Generation
Each participant took part in a single semi-structured interview. The interviews lasted between 40 and 70 minutes (average length, 60 minutes) and were conducted using video conferencing software or over the telephone (per participant preference). The video conferencing software or an audio recorder was used to record the interviews, with brief notes made during each interview, and more extensive notes taken afterward. Before starting the interviews, the interviewers read the interview guide and met to discuss the overall goal of the interview. Aside from a phone call or email exchange to set up the interview time, the interviewers did not have a prior relationship with participants.
Due to the participant information sheet, participants were aware that this study would contribute to the development of a digital health intervention, but this was not the primary focus of the interview, and the topic was only specifically raised toward the end. The initial portion of the interview focused on the day-to-day experience of living with heart failure, starting with a question asking the participant to describe a typical day in their life, with subsequent prompts dependent on their responses. Prompts sought to elicit more detail about the self-care practices described by participants and what changes they hoped for. For example, participants were asked about the tools, objects, or services they used, and how these supported their efforts. The latter portion of the interview concentrated on technology use and thoughts about the proposed intervention, and findings from this portion will be reported elsewhere.
The interviews were conducted in August 2021. During this time, several states in Australia were subject to social distancing measures due to the COVID-19 pandemic. Where these restrictions influenced the topics discussed in the interview, the interviewers also encouraged participants to reflect on their experiences before this time.
Interview recordings were transcribed verbatim by a professional transcription company, and transcriptions were checked for accuracy against the original audio recordings by the first author.
Data Analysis
Reflexive thematic analysis was used to support the identification of patterns within the data in relation to patient self-care experiences (Braun & Clarke, 2006, 2019).
The ontological orientation taken to the data in this study was that of critical realism. Hence, as well as capturing the individual experiences of participants, the analysis considers the underlying structures and mechanisms that might generate these experiences (Allana & Clark, 2018; Bhaskar, 2008). Moreover, the critical realist approach embraces the subjective and incomplete nature of human understanding. Likewise, in reflexive thematic analysis, the researcher’s subjectivity also shapes the analysis, meaning that themes were constructed by actively engaging with participants and the data rather than passively waiting for themes to “emerge” (Braun & Clarke, 2022a).
Reflexive thematic analysis involves six phases: familiarization, coding, generating candidate themes, reviewing themes, defining final themes, and writing up (Braun & Clarke, 2006, 2019). Progress through these phases was not linear, with phases revisited as the analysis progressed.
After completing all interviews, each transcript was read and reread alongside the notes made during and immediately after the corresponding interview. During this phase, initial thoughts and ideas were noted in a separate document. After this familiarization phase, the first author coded each interview transcript using both descriptive and interpretative codes to capture the semantic and latent meanings of the data. This approach to coding allowed for the exploration of unexpected findings, as well as building on what is already known about the topic (Thorne et al., 1997). Coding underwent several iterations, with codes being refined and added to along the way. A combination of handwritten notes and qualitative coding software (Atlas.ti) was used to organize and manage data during the analysis process. All coding was conducted manually. The original audio recordings were revisited throughout the analysis to assess participants’ tone and emphasis, and notes were frequently consulted to support interpretation. During the coding phase, a selection of quotes and descriptions of participants and their respective characteristics and environments were discussed between the authors. These discussions shaped the ongoing coding before moving to the development of candidate themes. To produce themes, the first author grouped codes that captured “patterns of meaning and possible connections, interconnections, and disconnections,” united by a “shared idea” (Braun & Clarke, 2022b). A visual representation (see Figure 1) and a written summary of each theme with illustrative quotes were produced and the transcripts were reviewed once again, this time to ensure the themes reflected the dataset. The analysis continued as the themes were written up, as it was during this process that the boundaries and structure of the final themes were determined. Visual overview of themes.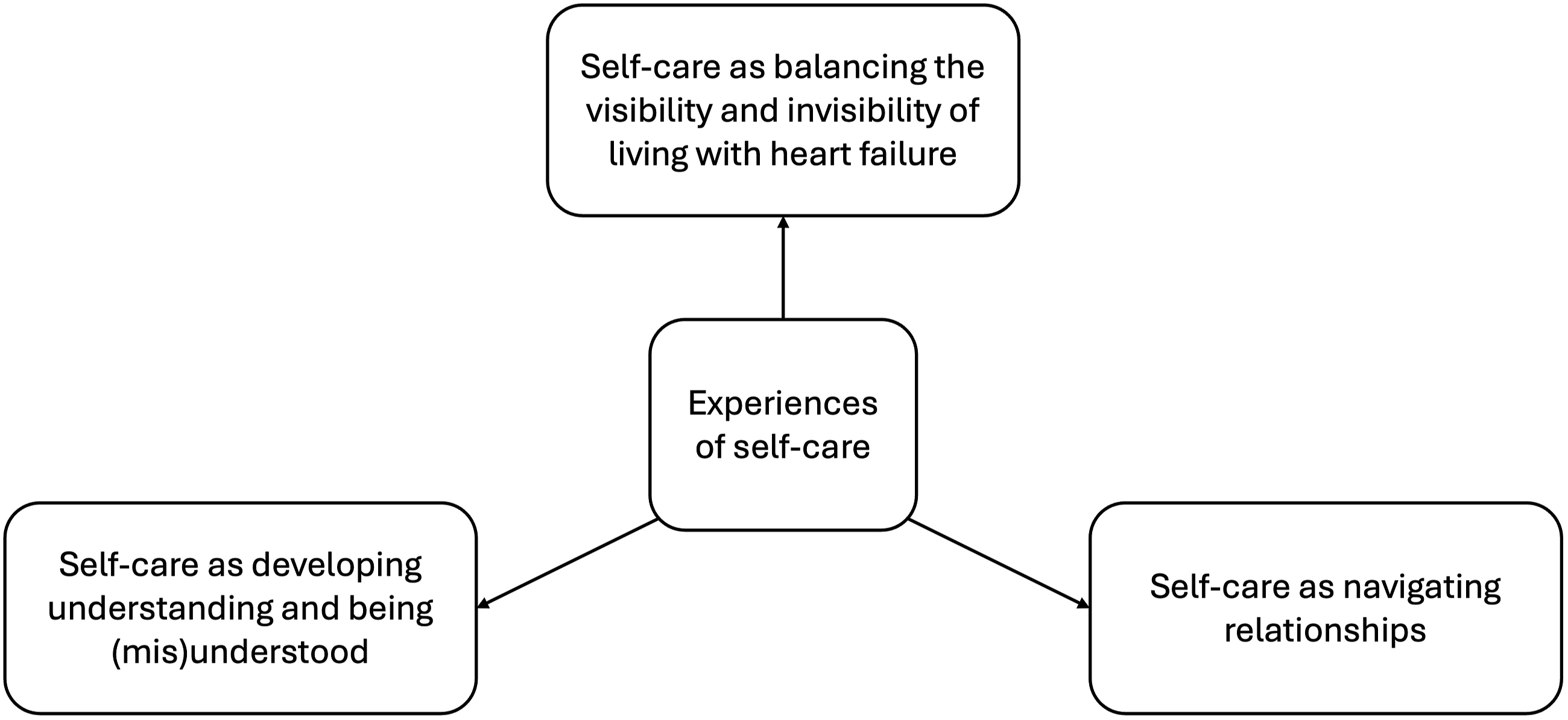
Ethical Considerations
Ethical approval for the study was granted by the Human Ethics Advisory Group at Deakin University (ref. HEAG-H 212_2020). Respectful of the potentially sensitive nature of the interviews, participants were informed that they could skip any question they wished to and end the interview at any time. Participants were also provided with contact details for local counselling services. Identifying information was removed from the transcripts. Pseudonyms and participant IDs are used in the reporting.
Results
Three themes were constructed pertaining to the self-care experiences and influences on these experiences described by participants.
Each theme, along with illustrative data extracts, is presented under its respective heading in the section below. Within participant quotes, clarifying information is presented within square brackets.
Theme 1: Self-Care as Balancing the Visibility and Invisibility of Living With Heart Failure
This theme portrays self-care practices as a means of controlling when and how heart failure was apparent both to participants and to others. Participants navigated a tension between making their condition visible enough to manage it effectively and keeping it invisible enough to maintain daily activities, routines, and social relationships.
Visibility of heart failure comprised aspects that were literally observable, such as the paraphernalia associated with the condition (e.g., medication and monitoring equipment), as well as more abstract aspects that participants themselves experienced or believed others could perceive, such as the consequences of heart failure symptoms and health management tasks. Participants’ self-care adjusted this visibility.
Heart failure being less visible was sometimes perceived as positive, for example, when symptoms were less noticeable (perhaps as a result of self-care practices), or when participants were able to participate in social activities without restrictions. At the same time, heart failure being more visible also had its merits for self-care. Participants described the value of “monitoring,” a term they used to refer to a range of health-tracking activities, including weighing themselves daily, checking their blood pressure, assessing leg swelling, and noticing changes in how they felt. Without these practices, participants felt as if they were in “no man’s land” (P1). These practices made the condition more visible to themselves, enhancing their self-efficacy to take timely corrective action and reassuring them about their health status: I think that gives me a base log of where I am, but it doesn’t tell you how bad you are internally, but you know the numbers are good, so everything must be functioning all right. (P3)
Therefore, the (in)visibility of heart failure was a source of both positive and negative effects on the lives of participants, and self-care was continuously used to strike a careful balance in each participant’s context.
Traditional self-care activities that feature in heart failure management guidelines were one way of striking this balance. For example, participants described taking medications, exercising, and controlling their fluid intake to alleviate symptoms and improve overall well-being: I’m on blood thinners, so if that gets out of kilter, I try to change my diet to get it back to normal, yeah. Well when I say change it, if it goes too high, I’ll try have a bit more vegetables and salads and stuff. But if it gets too low, if I have a few rice meals it seems to push it up again. Yeah, that’s the only time I’ll change it yeah. (P6)
Yet, when these activities did not fit participants’ unique circumstances, the visibility of heart failure was increased in a negative sense because their attention was drawn to the frustrating aspects of living with the condition. To counter this, participants found ways to adapt and create new self-care practices that better suited their needs. One participant who used a remote monitoring system described turning off the monitoring reminders so that they did not interrupt his morning routine. In making these types of adjustments, participants were able to maintain a sense of control and maintain everyday life activities like work and socializing while managing their heart failure: Because work requires a lot of focus and concentration and yeah. So for that, if I take a higher dose in the morning, that will restrict the blood supply to my mind and therefore I am not as sharp as I would on a half dose. So it’s been a journey with so demanding work and medication titration and the timing and all, so I need to be a hundred percent at work. And then after work I can just take the higher dose and you know that kind of thing. This is kind of just sort of experimentation and trying and testing kind of thing. (P9)
Regardless of whether participants used traditional or adapted self-care practices, they often drew upon objects, tools, and devices for assistance. These included monitoring devices, various types of medication boxes, paper diaries, and smartphones. The visibility of these objects themselves had both advantageous and disadvantageous effects. Strategically positioning these items around the home served as visual reminders, for example, putting medication in a visible spot so as a reminder to take it. Equally, these visual reminders could evoke feelings of unhappiness. Balancing the visibility of these objects became part of self-care, ensuring the line between making heart failure too visible or invisible was maintained: As the numbers grew, I introduced a little weekly clip open thing, so that when I get my meds, go and pick them all up at the end usually—usually once a month, they all seem to run out, some of them run out at the end of the month, I go and get them all at once. I like to get them all at once and then I pop them into their little daily spot. So that I don’t have to—won’t have to think about them. I hate going into the bathroom and getting down all the different boxes and putting each one down in front of me. I absolutely hate it. It depresses me. I do it all at once and put them all in so I’ve got a whole week and I can just clip it open, throw it into my hand and take it. (P5)
Participants also expressed concerns about how visible their heart failure was to others: I sort them all out into containers for morning days and the night days and I do it for two weeks and I keep them in a high cupboard. Now, there’s no children here, but I do have grandchildren that could come sometimes, but I put them in a high cupboard in the kitchen. (P7)
While this specific action reflects practical safety concerns, it also illustrates how self-care oriented not only toward participants’ own health but also toward maintaining the physical and emotional well-being of others.
Theme 2: Self-Care as Developing Understanding and Being (Mis)understood
This theme portrays how participants described understanding as essential for self-care, both in developing their own insight into living with heart failure and in feeling understood by others. Participants highlighted the significance of their personal journey in making sense of heart failure in relation to their own circumstances, as this understanding helped them to initiate, adapt, and sustain self-care. However, this personal understanding was frequently contrasted with the misunderstanding of others, including family and friends, healthcare practitioners, and wider society. Such misunderstanding posed powerful barriers to self-care.
While the interviews centered on participants’ day-to-day experiences, it was noteworthy that many also reflected on the time of their diagnosis as pivotal to their understanding of heart failure and self-care. The days, weeks, and months surrounding their diagnosis were characterized by turbulence, with participants describing that they experienced feelings they had not previously encountered. It was within this context that many participants began the process of understanding their condition and associated self-care needs. Yet, for some, this began even earlier through observing the experiences of others, such as relatives, living with heart failure. Although this prior exposure often carried unsettling preconceptions about prognosis, it also proved to be a source of motivation to invest in self-care: I’ll do anything, and that’s why also I feel like I’m so well supported, because if you get involved and try and improve the stuff, like my old man had the same thing, the exact same thing, cardiomyopathy from alcohol and heart failure, and he wasn’t involved in anything like that and he died within 10 years. With a bit of luck, with all this stuff going on, I won’t die in 10 years. (P1)
Participants’ understanding of their condition was dynamic and sculpted through their self-care practices, which in turn influenced their health, well-being, and motivation. Many described how bodily changes provided feedback, reinforcing the value of recommendations from their healthcare practitioners: You can really feel it though in your body when you do drink too much. It was really surprising. And then, yeah, that has a big flow-on effect. I was quite amazed at how a seemingly little thing had such a big impact. It just took a little bit to really absorb that and realize that, and once I realized it was for my good, I could get my head around it easier. But if you just—at the beginning it feels so tedious and it feels so unimportant, water and salts. It’s like really, what is this going to do? But when you can really see the impact on yourself, then you can make it work. (P8)
However, participants also expressed how the label “heart failure” caused distress, particularly for their family members. While knowledge was empowering for participants themselves, for others, the same information became a source of anxiety: She [participant’s mother] gets a bit confused about the heart situation, and she hears the word—even she doesn’t really get like heart failure, it’s that term, she—it’s like, she—I think it’s a really scary term. She tries to—I don’t know, she doesn’t come to all my appointments anymore because I think it’s too overwhelming for her. Whereas for me, knowledge is power. But for her, it’s more scary. (P8)
Although participants had all experienced challenges in living with heart failure, the message they wanted others to understand was that heart failure is something you can manage and live with. This way of understanding the condition empowered participants to practice self-care. Moreover, most perceived that, compared to other health conditions such as cancer, there was a general lack of awareness and misinformation around the experience and impacts of heart failure. This drove some to “create some awareness” (P2) if they had the chance.
Participants suggested that this misunderstanding, both among the public and within healthcare systems, led to services that were inadequate or failed to address obstacles that they experienced: It was hard to try and lose weight with the medications I’m on. Because I’m on Warfarin I have to control how much greens I have. If you’re on greens then most of the diets you can’t go on, because of course they want you to have a lot of greens. So it’s taken a good six, seven months to find food, or a comparative dietician that will allow me to adapt my eating around my medication. (P6)
For many, an essential aspect of coping was feeling understood. A common sentiment among participants was that they felt a lack of such understanding. Friends and family, though well-intentioned, often failed to grasp the lived reality of heart failure, which had practical and emotional consequences: My wife does refuse to go shopping with me because I’m too slow. I do things at my speed. So, there’s two different movements in the ocean, wife goes at 40 miles an hour, I go at four miles an hour. (P3)
Social support played a crucial role in shaping participants’ sense of being understood. However, a perceived lack of understanding, even from healthcare practitioners, meant participants often felt as if nobody understood what they were going through: So I was provided cardiac rehab, and I was given the chance to go to a psychologist, but obviously the psychologist doesn’t understand what I went through, which gets a bit tricky because I can’t explain when I’m explaining [to] somebody and that person is not able to understand what I am saying. And you can judge that they are not on the same page, so usually it’s not very helpful. (P2)
This theme, in essence, emphasizes that developing personal knowledge and receiving understanding from others were seen as essential for self-care. Understanding, in this sense, was not only about grasping information but also about feeling recognized and supported by others.
Theme 3: Self-Care as Navigating Relationships
This theme explores the networks of relationships that participants navigated in the context of self-care, whether with healthcare practitioners, family members, friends, or peers. Participants’ connections and interactions with others shaped their understanding and execution of self-care, as well as their trust in others. In navigating these relationships, participants worked hard to strike a balance between self-reliance and seeking external support.
The interpersonal experiences of self-care offered participants an escape from feelings of uncertainty and loneliness. As described in the previous theme, sometimes participants felt as though support services fell short. Consequently, their search for empathy and shared experiences led many to seek out peer support. However, finding such support was not always easy. The most significant challenge was finding genuine understanding: So I have joined Facebook groups and I usually read people’s stories on Facebook and understand that I’m not alone that I’m going through all this. But yes, sometimes we—like I feel very lonely as well because sometimes you have to share it with somebody that what you are going through, and that disconnect is always there because there’s nobody to understand that. (P2)
This is not to say that people always felt unsupported; many instances of support were described. However, what often transcended the offer of support was an opportunity to talk with others who had shared similar experiences: It’s always good to have someone else that understands what you’re going through. I find a lot of times, no matter who you talk to, your friends or whatever else, they actually don’t understand the restrictions that are on you. And a lot of my friends are still working, so that’s very different for them. So therefore they definitely don’t have time. And of course they don’t then take into consideration that I’m slower to walk somewhere, those sorts of things. (P4)
Building a strong relationship with healthcare practitioners became an essential part of self-care for people with heart failure. Participants described navigating a desire for independence amid the underlying power dynamics in their relationships with healthcare practitioners. They found sharing the outputs and outcomes of their self-directed self-care activities empowering. When this was received well by healthcare practitioners, it reinforced and further guided their self-care practices. However, there were also occasions when participants were left feeling undervalued and uncertain about their self-care as a result of their interactions: And then you’ve got to remember to fit in all the questions at the appointment I write them in my diary. But then even that becomes difficult because it’s just—I don’t know, he just asks specific things and sometimes I’ll just forget. And then it feels a bit like he’ll just say, “How are you going on the medication?” And I don’t know, it just feels sometimes like they’re ticking a box, sort of thing, like there’s not—they’re just checking how low your ejection fraction of your heart is and then not much more. (P8)
Another way in which the power imbalance between participants and their healthcare practitioners was perceived to negatively impact self-care was when participants felt a lack of trust from their healthcare practitioner. This was evident when healthcare practitioners questioned participants’ personal experiences and symptoms. Participants strived to develop mutual trust and put in the work to a point where their healthcare practitioners trusted their accounts, and they, in turn, trusted the advice given: Yeah, once my GP got tuned in to the fact that I knew what was happening to me, once he started to trust me, he didn’t at first, but he has learnt to trust that I’m on the case, right, that I am aware, self-aware. Once he realized I was a self-aware person and that I was spot on with most things he got over the—any distrust. I think they are very distrustful of them side effects. When you tell them, “Look, I don’t think is working. This doesn’t work for me, that side effect, I’m getting a bad side effect.” (P5)
Despite their valuable lived experience, participants sometimes discredited their own knowledge and skills as they felt comparatively unqualified to understand or manage their heart failure. For instance, they expressed sentiments like “I’m not a nurse” (P1) and “I’m not a doctor” (P8). Some participants doubted their embodied experiences and resorted to seeking validation from other people: So what I did feel one time was the irregularity of the beat when—like I was telling you about the piano. I said to my wife—we were in bed when I—I had felt it before, but I said to her, “You tell me, am I imagining my heart’s not beating right?” And she felt my pulse and said, “No, you’re right. It’s not beating right.” So, see, I wasn’t imagining it. It wasn’t right and I knew that. So I didn’t immediately ring the doctor, but I was off to the doctor the next day saying, “There’s something—I’ve had experience with irregular beating.” (P7)
These examples demonstrate that self-care was not done in isolation but was influenced and supported by others. As alluded to in the first theme, embedded within these relational dynamics was the matter of care—both self-care and care for others. Participants often took steps, not just for their own benefit but for those around them. Such acts, even if perceived as inconvenient or cumbersome, served a dual purpose: looking after oneself while also benefiting others. Participants’ actions often stemmed from a motivation to benefit themselves and to serve the peace of mind of their loved ones: No, I’ve never considered it because [partner] insisted that I get this [shows mobile phone]. And carry the—I had to have my mobile phone, so that if I go out—but most times I hate the thing. I forget to pick it up, and I’d get way down the road and think, “Oh, I forgot the phone.” But I do have a mobile phone, so that if I needed to ring somebody for help for any reason, I’ve got it, but I don’t—I’m not paranoid about anything. I’ve got all these things and I do all these things. If I’m going out, I normally have the phone charged and I carry it with me in a bag, so that I’ve got it with me, but it annoys me. And I don’t make—we’ve got a special phone plan, that our landline on our house and her mobile and mine are all on the same plan, and it’s free from her line and free to the house, so I can ring her on the landline or the mobile or I can ring on the landline to her mobile or—wherever we are, so that there’s a little bit of a contingency plan there, the what if. But I’m not paranoid about it. I try not to be deliberately. (P7)
Discussion
This study explored the self-care experiences of community-dwelling adults with heart failure in Australia, generating three interconnected themes: self-care as balancing the visibility and invisibility of living with heart failure, self-care as developing understanding and being (mis)understood, and self-care as navigating relationships. These themes illustrate the ways in which people with heart failure experience and enact self-care beyond traditional clinical conceptualizations, which raises implications for supporting self-care among people with heart failure.
This study describes self-care as dynamic and context-dependent. Participants described self-care practices not as fixed behaviors aimed solely at improving measurable health outcomes but as strategies that modulate the visibility and invisibility of heart failure. These are used in different contexts to achieve a range of goals, including to preserve normality, reduce the burden on others, and maintain social roles and relationships. This adaptive approach to self-care resonates with Mol’s concept of “care as a matter of tinkering,” which points to the continual adjustments people make in managing chronic conditions, thereby seeing self-care as constantly adapting and difficult to capture in a set of guidelines (Mol et al., 2010). It is also aligned with critiques of overly prescriptive approaches to self-care in heart failure described in the Introduction, which often fail to accommodate the lived complexities of chronic illness management (Greenhalgh et al., 2017).
As interventions are often developed in a way that sees people as passive recipients, rather than active participants, they may themselves constrain self-care practices and people’s ability to adapt to different situations (Hankonen, 2021). Therefore, considering this finding, interventions to support self-care among people with heart failure should facilitate the adaptation of self-care practices based on people’s contexts and goals. Advanced technology can play a role in augmenting the efforts of healthcare practitioners who strive to provide tailored care. To demonstrate, a scoping review of heart failure self-care interventions using smart technology identified several adaptive features such as providing different health advice based on environmental factors, allowing alarms to be scheduled at preferred time, and providing different options for mode of delivery (e.g., a different device based on user preference) (Nourse, Lobo, et al., 2022).
Participants’ accounts depicted a journey from their initial experiences after diagnosis to a point at which they felt empowered to apply their experiential knowledge in their daily lives. Their experience of bodily changes was critical to understanding the importance of self-care, and they often deemed these experiences as more salient than any advice from a healthcare practitioner. This echoes the inclusion of symptom perception in the situation-specific theory of heart failure self-care, which describes how individuals learn to interpret and respond to their bodily experience of symptoms as a source of guidance for managing their heart failure (Riegel et al., 2016). This finding also talks to the complex relationship people have with healthcare practitioners and the potential disconnect between their intuitions and expert advice. Previous research describes that a similar tension between people with heart failure and healthcare practitioners can arise from differences in their respective treatment goals (Karimi & Clark, 2016; Kraai et al., 2018). Navigating these differences is key to forming effective relationships and thus self-care practices. Many existing heart failure self-care interventions are focused on changing patients’ behavior. As a result of this finding, more attention could be placed on supporting healthcare practitioners to recognize, value, incorporate, and communicate about patients’ experiential knowledge. Technologies such as symptom diaries could further facilitate this.
In this study, self-care was seen to be highly integrated with family, friends, and healthcare practitioners. The involvement of caregivers in heart failure self-care, as well as the challenges they face, has been explored in the literature (Grant & Graven, 2018). In line with existing literature, participants in this study sought support with their self-care from family members, who helped with tasks such as organizing medications. We also describe that participants’ self-care reduced the concerns of their loved ones as well as ensured their own well-being. Appreciating these motivations could be used as a strategy to engage people in self-care practices, especially in dyadic interventions.
It must also be recognized that other studies have described tensions between the patient and family members who get involved with self-care practices—pointing toward the need for interventions that recognize these roles and help to negotiate them (Riegel et al., 2010). While we describe that people continued to adapt self-care in their daily lives and support systems offered invaluable aid, the nuanced aspects of heart failure often remained incomprehensible to those who have not experienced it. Participants felt this led to services and interventions that failed to meet their needs. To address this, intervention design should dive deeper into individual experiences of self-care and consider how the social, economic, and political contexts can be shaped to inspire more effective support—this might include raising public awareness of heart failure and the needs of people with the condition.
It is reported that people with chronic conditions can experience a “loss of self,” and leading a restricted life can serve as a constant reminder of this (Charmaz, 1983), demonstrated in this study by people adapting their self-care practices to conquer these challenging emotions. Taking a person-centered perspective, in this study, self-care was context- and situation-dependent in order to actively manage one’s health, while not letting the illness define one’s identity (Harkness et al., 2015). Despite the evident importance of emotional resilience, few self-care interventions have provided comprehensive psychosocial support (Lee et al., 2022; Liu et al., 2015).
Strengths, Limitations, and Future Research
This research has provided an in-depth account of the experiences of nine people with heart failure at a single point in time. The application of reflexive thematic analysis allowed us to move beyond descriptive categories to themes that tell a story about the lived experiences of heart failure self-care. The critical realist perspective enabled consideration of both individual experiences and the broader structural contexts that shape these experiences.
However, several limitations should be acknowledged. The participants were all recruited through social media and heart failure support organizations, suggesting they were highly engaged with their condition. This may limit the transferability of the findings to people who are less engaged with heart failure or who have different relationships with the healthcare system. In-depth interviews as a data collection method may have appealed more to participants who were more willing and comfortable discussing their experiences.
The findings suggest directions for future research. First, future research could employ different recruitment strategies and data collection strategies to capture additional experiences. In particular, longitudinal studies could explore how self-care experiences and strategies evolve as the course of heart failure inevitably fluctuates over time. Second, the relational dynamics highlighted in this study warrant further investigation. While participants in this study spoke about the importance of their relationships with others—future research could explore these dynamics from the perspective of others by also involving them in the research through dyadic or family-based designs.
Conclusion
This study shows that people with heart failure use self-care in ways that differ from traditional clinical expectations. Rather than simply following recommendations, participants actively adapted their self-care to manage the social and emotional impact of their condition. They strategically controlled when their heart failure was visible—making it more visible when they needed to monitor their health but hiding it when they wanted to maintain normal relationships and activities. They relied heavily on learning through their own bodily experiences, sometimes trusting these experiences more than healthcare providers’ advice. Importantly, they also made self-care decisions not just for their own health but to manage the impact on family members and maintain their relationships. These findings suggest that current heart failure management approaches may be missing crucial aspects of how people actually live with this condition. Healthcare providers often focus on medication adherence and symptom monitoring, but our participants were equally concerned with managing their social identity, maintaining family relationships, and integrating self-care into their existing life routines. It is likely that addressing broader concerns of patients, not just clinical outcomes, will improve the acceptability and effectiveness of interventions.
Footnotes
Acknowledgements
The authors thank Hannah Thompson for their support with data collection and project administration. The authors thank Heart Support Australia and the Heart Foundation for their support with participant recruitment.
Ethical Statement
Our study was approved by the Human Ethics Advisory Group at Deakin University (ref. HEAG-H 212_2020).
Consent to Participate
All participants provided written informed consent prior to enrolment in the study.
Author Contributions
Rebecca Nourse: Conceptualization, formal analysis, investigation, writing—original draft, and writing—review and editing. Ralph Maddison: Writing—review and editing, supervision, and funding acquisition. Lars Kayser: Writing—review and editing, and supervision.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The SmartHeart project was funded by the National Health and Medical Research Council of Australia (GNT:2004316). RN was supported by a Deakin Postgraduate Research Scholarship.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
