Abstract
This study aimed to co-design a “Deadly Dental Home” for Australian Aboriginal and Torres Strait Islander people (herein referred to as First Nations). Participatory Action Research-Dadirri-Ganma methods utilized respectful listening (Dadirri), self-reflective knowledge sharing (Ganma), and Yarning to design a model of care for the community. Consumers of dental services, community leaders, healthcare providers, and dental service leaders designed a culturally safe and holistic approach to dental care, bringing together First Nations and Western perspectives. A “Deadly Dental Home” is a dental service that arranges continuously available, comprehensive, coordinated, and culturally appropriate dental care. The expression “deadly” carries a sense of empowerment and positivity within First Nations cultures, representing strength, praise, resilience, and excellence. The research emphasized the integration of cultural needs into dental services. Key themes included Reaching Mob, Dental Care Delivery, and Care Across the Life Journey. Continuous and culturally responsive dental care tailored to different life stages from infancy through elderhood included hands-on education and prevention strategies. The need for a culturally competent workforce, a welcoming dental environment, and flexible appointment scheduling was necessary to foster trust and accessibility. The Deadly Dental Home model promotes a comprehensive approach to care extending beyond traditional dental treatment to address broader health determinants. Continued community engagement, partnership with dental services, and research are essential to refining and implementing this model, ensuring it effectively addresses the unique needs of First Nations people.
Introduction
The Australian dental system is funded and governed separately to medical and allied health models of care. Total expenditure on dental services exceeded $9 billion in 2019/20 (Australian Institute of Health and Welfare, 2022). Australia’s dental care system is a mixed healthcare model, where individuals can access care through either public or privately operated services. In the private model, individuals pay on a fee for service basis and can purchase private health insurance to cover part of the expenses (Lam et al., 2012). The public sector is funded by the Commonwealth and State and Territory Governments, and generally low socio-economic groups and children are eligible for subsidized care (Queensland Government, 2019; Queensland Health, 2017). In addition to the public and private dental sectors, a third unique sector for the First Nations community to access dental services is within Aboriginal Community Controlled Health Organisations (ACCHOs) (Campbell et al., 2015). ACCHOs are autonomous, culturally appropriate primary health services run and governed by the local First Nations community (Panaretto et al., 2014).
Following community consultation, we hereafter respectfully respect their wishes to refer to Aboriginal and Torres Strait Islander people as First Nations people. First Nations people have more than double the untreated oral diseases than their aged-matched non-identified counterparts (Australian Research Centre for Population Oral Health, 2019; Do & Spencer, 2016). The National Study of Adult Oral Health found across Australia 73% of older First Nations people had untreated tooth decay, compared to 32% of older non-identified Australians (55–75 years of age) (Australian Research Centre for Population Oral Health, 2019). Moreover, First Nations people have a lower prevalence of tooth fillings than non-identified Australians (Australian Research Centre for Population Oral Health, 2019; Do & Spencer, 2016). The higher burden of disease and lower proportion of treatment, such as tooth fillings, is indicative of untreated disease and less access to prevention and treatment (Australian Research Centre for Population Oral Health, 2019; Do & Spencer, 2016). In the most recent national Child Oral Health study 2012–14, around 3 in 4 of Australian First Nations children aged 5–14 years attended their last dental visit at a public clinic (Do & Spencer, 2016). First Nations children had 31% lower attendance rates to dental services than their non-Indigenous counterparts (Stormon et al., 2022). Eligible children can access $1000 (AUD) of dental treatment over two calendar years in the public, private, or ACCHO sectors under the Child Dental Benefits Schedule (CDBS) (Australian National Audit Office, 2015). Utilization rates of the CDBS were found to be similar in First Nations and non-identified Australians; however, fewer preventive services were claimed in First Nations children (Orr et al., 2021).
Dental services are not listed on Medicare, and many vulnerable and disadvantaged Australians are unaware of their eligibility for subsidized public dental services and face challenges navigating complex triage processes (Australian Institute of Health and Welfare, 2022). Barriers to accessing dental care for First Nations people include fear of dentists, a lack of culturally friendly dental spaces, difficulty finding transport to appointments, and lack of awareness of local dental services (Krichauff et al., 2020). First Nations Australians have differing views on the sector they prefer to receive healthcare (Butten et al., 2019). Individuals want to choose where they receive care (Butten et al., 2019). First Nations mothers from North Brisbane had a safe and beneficial experience in public-school dental services that promoted prevention (Butten et al., 2019). Conversely, some found public dental services irregular and inconvenient to access (Butten et al., 2019). A lack of trust and information about services created barriers for navigating public and private dental services (Butten et al., 2019).
Metro North Health (MNH) Service is the largest public health service area in Queensland providing care to the community in South-East Queensland. MNH Community and Oral Health provides care to the Jinibara, Kabi Kabi, Turrbal, and Yugara peoples in their home, oral health clinics and vans, community and residential facilities, and bedded services (Queensland Health, 2022). Recognized from an international perspective as the Indigenous population of Australia, in this study we respectfully refer to the local community as First Nations people, respecting these peoples as the first owners and custodians of the lands. Attendance to dental appointments and completion of treatment by First Nations people of MNH oral health were identified as lower than their non-identified counterparts. To investigate attendance to the service, a recent quality improvement initiative was undertaken to evaluate the patterns of attendance and non-attendance to dental appointments over the calendar year of 2022. The quality improvement initiative found the overall proportion of attendance to appointments was higher in non-identified patients, with 74.1 per 100 appointments attended for non-identified and 66.2 per 100 appointments for First Nations (Stormon et al., 2024). The greatest difference in attendance rates was 13.1% lower attendance by First Nations patients in the adult service (16+ years age group) in general appointments (Stormon et al., 2024). The overall rate of completion of courses of care were 68.7 per 100 and 77.9 per 100 for First Nations people and non-identified, respectively (Stormon et al., 2024). Completion of course of care was lowest in general care type among the 16- to 39-year age group, and First Nations provided a voucher for private dental treatment, with a completion of 33.1 per 100 and 41.7 per 100, respectively (Stormon et al., 2024).
Compounding social determinants and inter-generational trauma experienced by First Nations people contribute to distrust in research and poor translation of findings into actual health benefits (Bainbridge et al., 2015). There is an urgent need to undertake meaningful research with measurable benefits defined by the community (Bainbridge et al., 2015). The MNH community health service hosts a monthly gathering of the local First Nations Elders to feedback community needs to the service in a respectful yarning style. The MNH Elders in the Yarning Circle raised their concerns to the health service leaders regarding the community’s unmet oral health needs and voiced the need for improvement. A need to investigate and implement solutions to create an accessible dental service for the First Nations community is warranted given the service and community have identified oral health as a priority. The dental home concept is a model of care which provides anticipatory guidance and an interdisciplinary network of oral health support to facilitate access to care for mothers and their children (Plonka et al., 2012, 2013a; Pukallus et al., 2013). Trials and longitudinal cohort studies in low socio-economic populations have demonstrated the dental homes’ effectiveness in preventing the incidence of dental caries (Plonka et al., 2012, 2013a, 2013b; Pukallus et al., 2013). This study aimed to co-design a “Deadly Dental Home” using respectful listening (Dadirri), self-reflective knowledge sharing (Ganma), and Yarning for First Nations people (Sharmil et al., 2021).
Methods
Framework and Indigenous Methodologies
This study utilized the Generative Co-Design Framework for Healthcare Innovation (Bird et al., 2021). The Generative Co-Design Framework for Healthcare Innovation is a collaborative and iterative process that involves multiple stakeholders, including patients, community leaders, healthcare providers, and policy makers (Bird et al., 2021). The framework aims to create innovative solutions that meet the needs of all stakeholders, while addressing key challenges and opportunities in healthcare.
The Aboriginal co-design methodology, the Participatory Action Research-Dadirri-Ganma, was employed (Sharmil et al., 2021). Four phases of qualitative engagement with the community, researchers, and health service stakeholders were undertaken: (1) Look and Listen, (2) Think and Reflect, (3) Collaborate, Consult, and Plan, and (4) Take Action (Sharmil et al., 2021).
Concepts of Yarning, Ganma, and Dadirri underpinned all interactions, and critical and post-colonial theory shape interpretation and action (Sharmil et al., 2021). The research process begins with consultations in the form of Yarning embodied through free-flowing, uninhibited conversation and deep listening in a safe and respectful environment (Sharmil et al., 2021). Ganma describes each person as being mindful of the other’s individual and combined experiences, and their contribution to the collaboration (Sharmil et al., 2021). Dadirri brings peace, understanding, and increased awareness (Sharmil et al., 2021). This approach brings together the knowledge and experiences of consumers and community leaders to enable an understanding of the realities of health issues and health service responses to create actionable and implementable coordinated care pathways in dental services.
Participants
The Metro North Community Health Elders Yarning Circle and staff members from the health service were invited to participate in the study. Researchers engaging in the Yarning, Ganma, and Dadirri (KP, NS, and DC) brought together Western and First Nations perspectives. KP, a Gumbaynggirr woman, worked as an oral health therapist in the ACCHO and public sectors as a dental practitioner. NS is a non-identified Caucasian academic, also an Oral health therapist, who worked in private and ACCHO sectors. DC is an experienced public dental service leader and non-identified dentist.
Ethical Considerations
Ethical approval was obtained from the Queensland Health Metro North Health Human Research Ethics Committee B (clearance number 100453). This research aligns with the six Aboriginal and Torres Strait Islander ethical research core values specified in National Health and Medical Research Council ethics guidelines and the Australian Institute of Aboriginal and Torres Strait Islander Studies (AIATSIS) Code of Ethics for Aboriginal and Torres Strait Islander Research (National Health and Medical Research Council et al., 2023; The Australian Institute of Aboriginal and Torres Strait Islander Studies, 2020).
All participants gave verbal consent to participate in this study. As part of this methodology, it was considered inappropriate to request written consent from the Elders and community members involved. Written consent may not be appropriate within the context of the Dadirri, Ganma, and Yarning methodology for several reasons. These cultural practices emphasize the significance of building trust and establishing relationships through personal interactions and dialogue. The act of seeking written consent may be perceived as impersonal and detached, potentially undermining the spirit of mutual understanding and respect fostered by these methodologies.
Aligning with the AIATSIS Code of Ethics principle Indigenous self-determination, research projects involving First Nations communities should be underpinned by a negotiated agreement or protocol. The Elders Yarning circle is led and run by the Elders, who invite selected guests to participate in the Yarning within their safe space of sharing. To maintain the principles of the Elders Yarning circle cultural protocols and the integrity of the Yarning Circle as a safe space, transcription and recording of the discussions was agreed not to be employed.
Dadirri, Ganma, and Yarning Phases
During phase 1 (Look and Listen), researchers KP, NS, and DC were invited to attend the Elders Yarning Circle and respectfully listened to the oral health knowledge and experiences of the Elders. At the Yarning Circle meetings, researchers did not actively contribute to the discussions of the Elders other than to listen and learn about their thoughts and experiences of oral health. NS and DC subsequently attended local First Nations health events to engage with the community one on one. At the events, information about the dental service and dental health was provided by NS and DC and community members shared their experiences where they were comfortable to do so. Critical reflection incorporating both Western and First Nations perspectives was undertaken by researchers in phase 2, Think and Reflect. Researchers drafted the core values and concepts from phases 1 and 2. NS attended a subsequent Elders Yarning circle to report back the Deadly Dental Home values and seek permission from the Elders to subsequently hold a co-design workshop based on the model of care.
A co-design workshop was subsequently held, aligning with phase 3 of the methodology, Collaborate, Consult, and Plan. KP (First Nations), NS (non-identified), and DC (non-identified) shared facilitation of the workshop. The workshop emphasized mutual partnership, where the needs, perceptions, and opinions of each person are considered without hierarchical dominance. The core values and concepts of phase 1 (Look and Listen) and phase 2 (Think and Reflect) were presented to the participants at the beginning of the workshop. Senior Elders, health service consumers, and health service providers collaborated to design the model of care through participation, mutual consultation, collaboration, and collective reflection toward the collaboratively agreed goal. Purposive sampling was used to invite the Elders Yarning Circle, First Nations staff members, and dental staff members to the workshop. Snowball sampling was also employed where the Elders Yarning Circle was invited to extend the workshop invitation to other local First Nations people. The facilitators then held smaller group discussions focusing on the topics identified from the first two phases (Supplemental Table 1). These ideas were then presented back to the entire group by facilitators and discussed as a group specifically in reference to two key groups: (1) mothers and babies, children, and adolescents and (2) adults, Elders, and aged care.
The final phase 4 (Take Action) involved a reflective cycle of consultation and action. Critical reflection on each phase was undertaken and a solution for the Deadly Dental Home drafted. Critical reflection on each phase was undertaken when analyzing data. NS and KP presented the Deadly Dental Home model of care back to the Elders Yarning Circle for final refinement and for confirming the findings reflected their vision for the Deadly Dental Home.
Data Collection
The data collection for the Dental Home Project followed the four-phase approach, integrating the principles of Dadirri, Ganma, and Yarning methodology (Sharmil et al., 2021). Researchers recorded their own thoughts, reflections, and interpretations of the discussions and interactions that occurred during the sessions through reflexive journaling. Reflexive journaling entails the investigators reflecting on their experiences, observations, and insights following each Yarning Circle meeting (Greenwood et al., 2017; Halcomb & Davidson, 2006). This approach allowed the investigators to capture their personal experiences and interpretations while maintaining the privacy and confidentiality of the Yarning Circle participants (Rutakumwa et al., 2020). The use of reflexive journaling is an evidence-based method enabling data collection in a respectful and culturally appropriate manner (Greenwood et al., 2017; Halcomb & Davidson, 2006).
To respect the wishes of the Elders and maintain cultural safety, Yarning Circles were not audio-recorded. Instead, facilitators took detailed notes during the discussions, ensuring that key insights and participant wisdom were accurately documented. Where appropriate, verbatim quotes were recorded in writing to authentically reflect participant contributions. These written records were incorporated into the thematic analysis, ensuring that the voices of participants remained central to the findings.
During co-design workshops, participants recorded ideas and insights on butchers papers and sticky notes, which were collected at the conclusion of each session. Facilitator notes were also taken to document key discussion points. Following the workshops, researchers took reflexive notes to capture their own interpretations, observations, and insights. One week after each workshop, the research team reconvened to collectively analyze the butcher’s papers. Key themes were identified using post-it notes and connections emerging from the discussions using the journaling, notes and butchers paper as the sources of data. This process ensured participant-generated data remained central to the thematic development while allowing for researcher reflection and refinement (Rutakumwa et al., 2020).
Analysis
The analysis of the reflexive journals is a crucial step in reporting the findings of the Yarning Circle discussions and design of the Deadly Dental Home. The process of analysis involved an examination of the investigators’ journal entries and discussion, identifying key themes, patterns, and insights that emerge from their reflections (Sharmil et al., 2021). A critical aspect of this analysis involved recognizing how researchers’ own biases, assumptions, and perspectives may have influenced data collection and interpretation. Reflexive journaling was not only a means of documentation but also an essential tool for examining the researchers’ roles in shaping meaning within the study. Each researcher engaged in a structured process of self-reflection, analyzing how their positionality influenced the themes that emerged.
The analysis was guided by a qualitative approach, focusing on understanding the depth and nuances of the Yarning and its implications for the development of the Deadly Dental Home concept (Sharmil et al., 2021). The analysis was conducted in stages.
Thematic analysis was then utilized to identify recurring ideas, concepts, and perspectives (Braun & Clarke, 2012; Kyngäs & Kaakinen, 2020). Researchers first reviewed participant materials alongside their own reflexive notes to become familiar with the data. To systematically identify patterns, post-it notes were used to highlight recurring ideas and insights from the butchers papers, which were then coded into preliminary themes. These themes and sub-themes were further refined through discussion among the research team, ensuring that the voices of participants were accurately represented. Finally, the themes were critically examined in relation to the broader context of First Nations oral health and the co-design of the Deadly Dental Home. The final Deadly Dental Home themes were written and shared with the participants. The Elders suggested minor changes to terminology used and subsequently requested a visual representation of the themes, which was created and presented again to the participants. In this final stage, the participants confirmed that their ideas and voices had been captured in the write up and visualization of the Deadly Dental Home.
Results
Phases 1 and 2: Deadly Dental Home Values
A “Deadly Dental Home” is a dental service that arranges continuously available, comprehensive, coordinated, and culturally appropriate dental care. The expression “deadly” carries a sense of empowerment and positivity within First Nations cultures, representing strength, praise, resilience, and excellence. The Deadly Dental Home is a value-based model of care designed by First Nations peoples that leverages the resources within the dental system to embed cultural and social determinants of health. The Deadly Dental Home guiding principles are a dental service that embodies: a. Responsiveness to changing oral health needs across all life stages. b. Connected care joining pediatric and adult oral health services through outreach and intersection into other health services. c. A central point of truth which provides clear information about oral health service choices. d. Safe and trauma informed dental services which embody trust and respect.
Phases 3 and 4: Co-Design Workshop
A total of 23 participated in the co-design workshop, consisting of ten First Nations Elders, seven First Nations staff (including those with social work, nursing, Aboriginal health practitioner, and administration roles), three oral health staff, and three facilitators. Three themes were identified from the Dadirri–Ganma methodology: Dental Care Delivery, Reaching Mob, and Care Across the Life Journey. Each theme and sub-themes are discussed and represented in Figure 1. Visualisation of the co-designed deadly dental home concepts.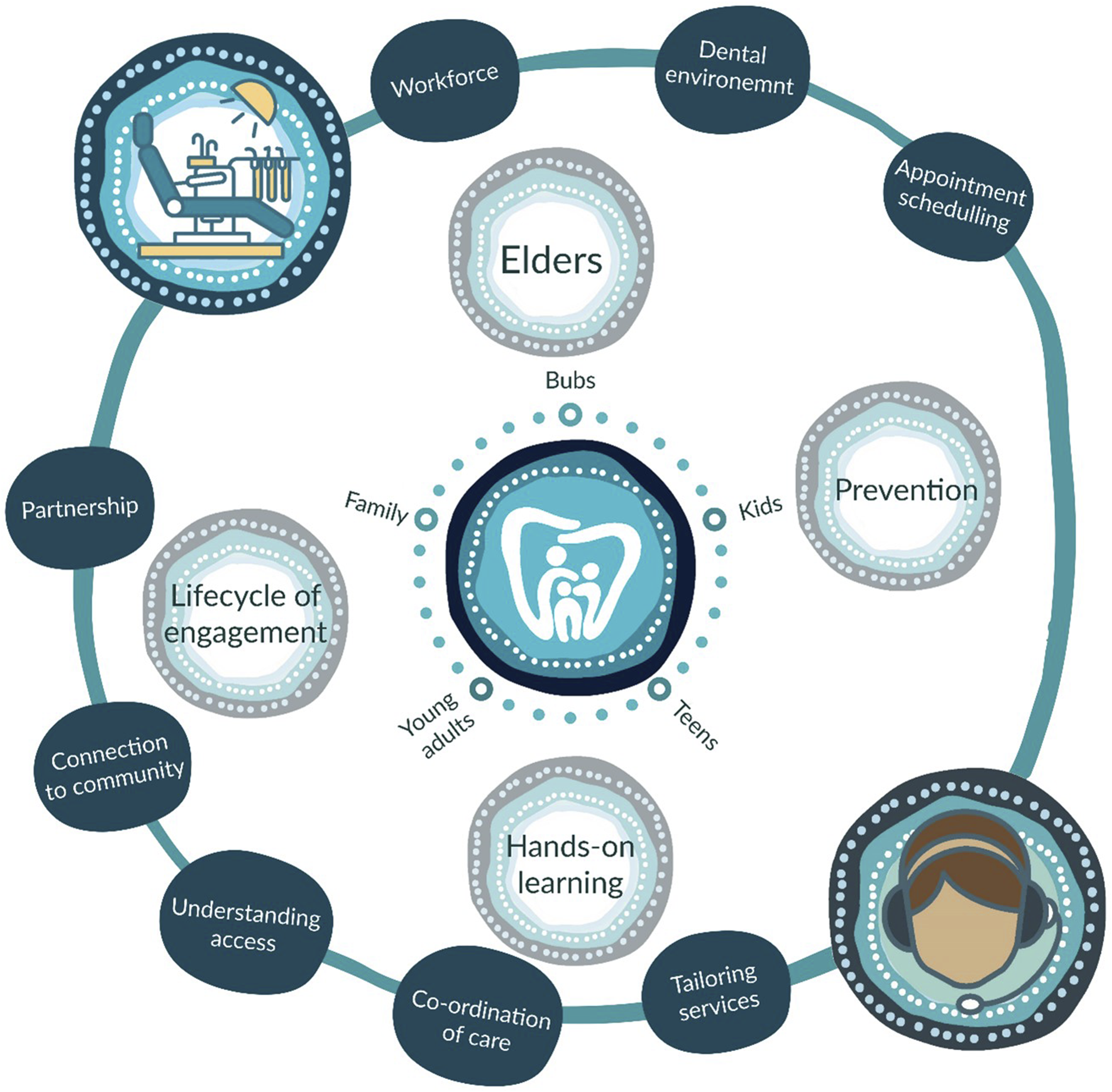
Theme: Reaching Mob
The mechanisms needed for community to understand and access culturally appropriate dental care were discussed. A responsive and personalized service was captured in five sub-themes relating to the tailoring of services, co-ordination of care, understanding access, outreach, and partnership.
Sub-Theme: Tailoring Services
Emerging across multiple areas of discussion was a “one size fits all” approach would be ineffective as “everyone is different.” The need for a flexible and responsive model of care was described as necessary for meeting the unique social and dental health needs of the community. It was noted that First Nations communities have varying needs, and the Deadly Dental Home concepts could be implemented in the local context (South-East Queensland); however, as the Dental Home expanded and will be scaled to other areas, the local community needs and values must be integrated. Local consultation prior to implementation and a mechanism for feedback ensures the model remains relevant and effective as community needs evolve.
Sub-Theme: Co-ordination of Care
The co-ordination of care was deemed essential for providing effective and continuous dental services. Participants highlighted the importance of having specific roles and mechanisms in place to ensure care is completed and culturally appropriate. There was a notable emphasis on expanding the presence of specific roles, such as liaison officers and Aboriginal health workers (AHWs) as integral members of the frontline health team connecting with the community. Participants highlighted that these professionals were utilized well within other health services to support the community. Their inclusion ensures Aboriginal ways of knowing, being, and doing are understood to enhance the quality of patient care.
The need for an identified “liaison officer” role was described as a crucial bridge between the dental health services and the community. This individual would be responsible for coordinating care, fostering trust, understanding individuals’ cultural needs, and follow-up to facilitate completion of care. The liaison officer would facilitate communication, manage appointments, and link patients with additional health services they needed. Participants described the importance of having the liaison officer not only following up to facilitate subsequent appointments but also checking in on the individual’s experience at their previous appointment. Poor experiences with dental services were described as a deterrent from attending subsequent appointments, and by understanding individuals’ experiences adjustments and support can be provided to facilitate attendance.
The first point of contact at the dental clinic was identified as another critical element for effective care co-ordination. Participants suggested the reception area should be welcoming and, if possible, staffed by First Nations people to enhance comfort and trust. Utilizing existing “Aboriginal and Torres Strait Islander Hub” services and cultural spaces within the system could serve as the cultural liaison and ensure culturally competent care and support upon first entry to the service.
Engagement with the community through AHWs was seen as a vital strategy for initial dental care engagement and ongoing co-ordination. This health practitioner would provide dental screening, education, and prevention in the home or community setting to build trust. AHWs conducting initial screenings will facilitate assessing the complexity of dental diseases and building trust before individuals visit the dental clinic. Participants expressed a preference for in-person contact over telehealth consultations in the home for relationship development and trust building. Transport was identified as a significant barrier, particularly for elders in the community. Providing transportation to and from dental appointments was a suggestion to ensure that elders and others with mobility challenges can access care.
Sub-Theme: Understanding Access
Word of mouth was described as the strongest mode of disseminating information regarding health services among the community. Positive experiences of health services and staff are often passed on to family and friends, prompting others to access care. Elders described acting as gatekeepers for their community, whereby if they had a positive experience they would arrange and recommend their family to attend the service. Conversely, word of mouth was described as a deterrent to access some health services as “bad news travels faster amongst mob.” Implementing feedback and follow-up mechanisms to understand and overcome negative experiences were needed to overcome this.
Breaking the barriers to having clear information and methods to contact dental services emerged as a theme. Some described that they did not mind calling a generic “hotline” phone number to schedule appointments, but others found calling a hotline difficult to navigate and intimidating to self-identify as First Nations. The solution posed to this was having a call line for First Nations community members to contact where identifying as First Nations was facilitated and preferences for ongoing contact (phone call, SMS, email, letters) and appointment preferences were discussed. Similar to other discussions regarding tailor of services, tailoring the mode of contact for individuals and choosing calls, emails, letters, or text messages were described. Having the option of a “Murri line” with discussions facilitating mob identification to establish trust was suggested as a conversation starter. Opening a trusting connection on the call could then facilitate conversations of cultural, support, transport, and oral health needs.
The use of a website to house information about the Deadly Dental Home was discussed. It was recommended that the site feature information about dental service options in a way community could understand. It was emphasized that the site needed to feature stories and videos of community members who had accessed and used these dental services. The Murri (Indigenous) and Ally (non-Indigenous) dental workforce should also be featured on the site to facilitate an understanding of the practitioner’s community may encounter. Promoting preventive oral health messages like healthy food and drinks and mob pathways into dental careers was recommended to be included. First Nations oral health promotion resources like a children’s storybook on dental visiting were suggested to promote positive experiences early in life. Having a suite of relevant information online was viewed more favorably than “just another brochure” or apps.
Sub-Theme: Connection to Community and Partnership
For the dental home to successfully reach local First Nations, the health service must engage in authentic connection with the community culture and partner outside of health organizations. The Deadly Dental Home practitioners and staff should participate in local cultural and sporting events to promote oral health and connect with community. Endorsement and support from ACCHOs would significantly enhance the sense of belonging and community within the Dental Home. A service operating independently of the community was described as disingenuous. To better integrate care options, partnering with local ACCHOs was recommended to be further explored. It was suggested that the broader public sector health services should be interconnected to facilitate referrals and promote the Dental Home.
Theme: Care Across the Life Journey
For a Dental Home to provide comprehensive and continuous dental care, it was recognized that needs differ throughout the life stages. This theme emerged through the discussions of community involvement, practical and hands-on education, oral health prevention, and the support of Elders.
Sub-Theme: Lifecycle of Engagement
Elders expressed they had missed out on preventive dental opportunities and now face unique challenges with complex needs and challenges with transportation to access appointments. The lifecycle of engagement in dental care was envisioned as a continuous loop that encompasses all stages of life, beginning with a “Lift the Lip” style program within existing First Nations midwifery services, where early oral health education and screening would occur for mothers and their babies. This integration helps link families with multiple children to comprehensive oral health services early.
Delivering dental services through school was described positively, and the need for appreciation of the larger kinship networks of these families when engaging in these appointments. For teenagers, an emphasis was placed on educating around healthy dietary choices and the risks associated with habits like smoking and vaping due to their increasing independence. Keeping teens engaged with dental services into early adulthood is essential to ensure they do not disconnect and only re-engage with dental services years later when their own children require dental care. This continuous support throughout all life stages fosters long-term oral health and well-being for the entire community.
Sub-Theme: Prevention and Hands-On Learning
Prevention and hands-on learning were described as critical components of the Dental Home, ensuring that individuals and families are equipped with practical knowledge and skills. Key prevention opportunities discussed included integrating education into “Mums and Bubs” groups, early childhood programs in prep, and school visits. The importance of making prevention advice practical and implementable was emphasized. Teaching through hands-on activities was described as engaging and makes the information more memorable. This includes educating families about simple and healthy cooking alternatives and raising awareness about hidden sugars in foods. By providing easy-to-implement dietary advice and demonstrating practical steps for maintaining oral health, the Dental Home ensures that preventive measures are accessible and actionable for everyone in the community.
Sub-Theme: Utilizing Elders
Elders play a vital role in promoting health within the community. By engaging these respected individuals to visit schools and collaborate with mothers and families, the Dental Home leverages their wisdom and influence. This inter-generational support fosters a sense of community and shared responsibility, enhancing the effectiveness of the Deadly Dental Home. Elders help bridge the gap between traditional knowledge and modern dental practices, ensuring a culturally sensitive approach to oral health.
Theme: Dental Care Delivery
The delivery of a culturally safe dental service was conceptualized by participants. A dental service which embodies trust and respect was captured in three sub-themes relating to workforce, the dental environment, and appropriate appointment scheduling.
Sub-Theme: Workforce
During the discussions, participants expressed concerns regarding the level of cultural competency necessary for delivering appropriate healthcare services to First Nations patients and community members. An emphasis was placed by participants on the importance of ongoing learning opportunities on culturally safe healthcare delivery throughout the course of employment and not only as mandatory modules on commencement. The importance for community-led in-person cultural training was described rather than implementing a disingenuous or dated online training. These training opportunities must include consultation with local Elders to ensure authenticity and relevance to the area where the services are being delivered. It was recommended that all external partners and outsourcing service providers adhere to the same standards of cultural competency and training as public service oral health staff, to ensure a consistent level of cultural understanding and safe practices for First Nations patients. Launching a cultural awareness campaign within the healthcare sector was put forward to promote confidence among health staff continuing the cultural safety conversations. The participants said the campaign could increase staff awareness, build competence, and promote inclusivity to translate into respectful and effective patient care for First Nations peoples.
To support the community to work within the health service, participants discussed a need for traineeships, scholarships, and mentorship initiatives. Educating adolescent First Nations communities on dental professional pathways was identified as a method to increase the identified workforce. Traineeships and programs for obtaining qualifications during high school studies were also discussed as important, and it was identified that many of these pathways currently existed. However, it was noted there was a lack of awareness and promotion about these programs within the broader community. Participants continued discussing this theme offering recommendations for health services to set clear targets and actionable strategies for the recruitment and retention of First Nations staff across all levels of the health workforce. Culturally supportive environments that are imbedded in policy and practice are important to ensure current and future employees feel safe, supported, and have a sense of belonging, and suggestions included access to cultural leave and support networks.
Sub-Theme: Environment
Community members highlighted the importance of cultural visibility in health services to foster a sense of belonging, respect, comfort, trust, and empowerment. This supports beliefs of health as a holistic concept of healthy living and being. Displayed artwork and the use of First Nations languages throughout dental clinics were discussed as a method to achieve this in the dental clinical environment. This visibility demonstrates that the health service values and understands First Nations cultures, promoting cultural competence and sensitivity among staff and patients. By doing so, it reduces the sense of alienation and fear that can often be associated with healthcare settings for First Nations people. The Elders expressed a sense of inspiration for the presence of First Nations youth employed within the public health service more broadly. They believe that seeing their culture represented in professional settings can be highly inspiring for other young First Nations people. It conveys that their culture is valued and respected, encouraging them to see their heritage as an integral part of their future careers and identities.
Participants proposed simple and effective gestures to establish a welcoming environment for the First Nations community. One suggestion involved integrating First Nations artwork into the design of all staff uniforms and scrub gowns. This initiative aimed to celebrate culture, enhance visibility, and cultivate cultural pride and awareness among both staff and patients. As dental clinical standards require covering uniforms and scrubs, participants recommended producing and supplying disposable masks adorned with First Nations designs. These masks not only serve a practical purpose but also symbolize cultural representation and inclusivity within healthcare settings. Collaboration with local First Nations artists was a requirement for implementing these recommendations. Engaging these artists in the creation of unique and meaningful designs for healthcare apparel ensures authenticity with the community.
Sub-Theme: Appointment Scheduling
Understanding individual and family preferences for scheduling dental appointments was emphasized to ensure they were attended. This entailed understanding contact, clinic location, and timing preferences. Having a drop-in style clinic was discussed; however, participants felt this would not improve attendance to dental appointments as having a clinic as close as possible to home and transport to the service of more importance. Scheduling appointments for all family members concurrently or one after the other was suggested to engage parents and children.
Discussion
This study utilized Aboriginal co-design methodology to create the concepts of a culturally safe and holistic approach to dental service delivery for First Nations communities. Solutions for improving access to dental service must include leadership by the First Nations community with the health service to create culturally appropriate solutions (Bainbridge et al., 2015; Butten et al., 2020; Sharmil et al., 2021). A strength of this study was the community-driven nature of its inception, where the need for improved oral health services was highlighted by the First Nations communities themselves. This study was not without limitations. Specifically, this study represented First Nations people of South-East Queensland and views and experiences of other First Nations communities may differ to the findings in this research. The decision not to audio-record Yarning Circles made to respect cultural preferences meant that data collection relied on facilitator notes and written records, which may not have fully captured the nuances of discussions. The use of reflexive journaling may introduce subjectivity; however, it also provides valuable researcher reflection.
This study utilized Aboriginal co-design methodology to develop concepts for a culturally safe and holistic approach to dental service delivery. The authentic partnership and engagement with the community ensured that the research adhered to principles important to First Nations peoples, including respect, reciprocity, and cultural safety (Bainbridge et al., 2015; Butten et al., 2020; Sharmil et al., 2021). This study’s approach underscores the necessity of leadership of the First Nations community with health services to create culturally appropriate solutions. Future research is now required to utilize the concepts of the Deadly Dental Home to implement within the dental service settings and evaluate relevant outcomes. An implementation science approach may be necessary to ensure the concepts can be effectively and appropriately implemented within local and broader dental service settings.
A key theme which emerged from the co-design of the Dental Home was the holistic and integrated views of health, well-being, and community. Well established in previous literature, First Nations communities’ health encompasses physical, emotional, spiritual, and cultural dimensions (Dudgeon & Walker, 2015; Gee et al., 2014). Conceptualized by Gee et al. (2014), the social and emotional well-being framework is a strength-based Aboriginal and Torres Strait Islander health discourse including interconnected domains such as land, culture, spirituality, ancestry, family, and community (Gee et al., 2014). Physical, emotional, and spiritual health and well-being are deeply interconnected in various Aboriginal and Torres Strait Islander concepts (Yap & Yu, 2016). These concepts emphasize the need for cultural activities and engagement to foster strong and resilient individuals and communities. The co-designed concepts of the Deadly Dental Home address these issues by fostering a culturally safe environment that supports the holistic health of First Nations individuals by offering more than “just dental treatment,” including outreach, education, and support services that address broader health determinants, thus promoting a comprehensive approach to care.
Representation of the First Nations community in the delivery of the Deadly Dental Home was a prominent theme. Recent statistics from the Dental Board of Australia (March 2024) reported only 152 dental practitioners were First Nations or 0.6% of the total workforce (Dental Board of Australia, 2024). This significant underrepresentation of First Nations people in the dental profession highlights a critical gap that needs to be addressed to ensure culturally safe and responsive care. Increased representation of Aboriginal and Torres Strait Islander practitioners is essential not only for delivering culturally competent services but also for building trust and engagement within First Nations peoples (Deroy & Schütze, 2019; Lai et al., 2018). Representation matters, as community members often feel more comfortable and supported when receiving care from practitioners who share similar cultural backgrounds (Deroy & Schütze, 2019; Lai et al., 2018). Visible role models in health professions can inspire and encourage younger generations to pursue careers in these fields (Bailey et al., 2020). To bridge this gap, it is crucial to develop and promote training pathways for Aboriginal and Torres Strait Islander individuals, such as targeted scholarships, mentorship programs, and outreach initiatives that make dentistry more accessible and appealing (Bailey et al., 2020). Future research should focus on identifying and overcoming barriers for these communities in becoming dental practitioners, as well as exploring the impact of increased First Nations representation on patient outcomes and community health. By fostering a more inclusive workforce, the Deadly Dental Home model can better support culturally appropriate care and improve oral health outcomes for First Nations people.
The Deadly Dental Home emphasized the critical role of information dissemination that is both relevant and understandable to the community. Effective communication is key to empowering individuals to take charge of their oral health. The model advocates for educational materials and outreach programs tailored to the specific cultural and linguistic needs of First Nations peoples. Ensuring that information is accessible and culturally appropriate is essential for overcoming barriers to care and promoting health literacy.
Conclusion
The Deadly Dental Home is a co-design model of care which aims to deliver culturally safe and holistic oral healthcare for Aboriginal and Torres Strait Islander communities. The Deadly Dental Home creates a holistic approach to oral health that extends beyond traditional dental treatment, incorporating outreach, education, and support services to address broader health determinants. A diverse workforce including First Nations dental practitioners, ally dental practitioners, and supporting professionals were identified as necessary for ensuring the model meets the unique needs of these communities. Continued community engagement, partnership with dental services, and research are essential to refining and implementing this model, ensuring it effectively addresses the unique needs of First Nations people.
Supplemental Material
Supplemental Material - Utilizing Aboriginal Participatory Action Research-Dadirri-Ganma to Co-Design the Deadly Dental Home
Supplemental Material for Utilizing Aboriginal Participatory Action Research-Dadirri-Ganma to Co-Design the Deadly Dental Home by Nicole Stormon, David Carr, Paul Drahm, and Kirrily Phillips in Qualitative Health Research
Footnotes
Acknowledgments
We wish to acknowledge the traditional owners of the land in which this research was conducted, in Brisbane Queensland, the Jinibara, Kabi Kabi, Yuggera, and Turrbal Peoples. We pay our respect to their contribution to global society and dedicate this work to all Aboriginal and Torres Strait Islander communities.
Author Contributions
Nicole Stormon led the design of the study, ethical approvals, acquisition of data, analysis, and write-up of the manuscript. David Carr, Paul Drahm, and Kirrily Phillips made substantial contribution to the study design, acquisition of data, and analysis and revised the manuscript critically for important intellectual content.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research received SWIFT Research Grant funding from Queensland Health Metro North Health (Grant number SWIFT-115-2023).
Ethical Statement
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
