Abstract
Healthcare professionals (HCPs) play a primary role in the delivery of population-based vaccination programs. Their emotional well-being can influence the quality of their relationships with patients and generally the outcome of their consultations. This qualitative study sought to identify the types of emotions that HCPs feel during conversations with vaccine-hesitant patients and their styles of interaction. Semi-structured interviews were conducted between June and November 2022 with 41 HCPs (mainly general practitioners and nurses) responsible for vaccinating patients: 23 in England and 18 in France. Framework analysis showed that participants reported numerous emotions, some associated with connection to patients (such as self-confidence and satisfaction) and others with distance (including anger, frustration, unease, and exhaustion). We identified four clusters of emotions reported together when reflecting on interactions with vaccine-hesitant patients: “self-confidence and emotional empathy” (satisfaction, sadness regarding the patient’s situation); “anxiety and insecurity” (doubts about skills, concern for the patients); “exhaustion and weariness” (feeling of incompetence, nervousness); and “discredit and frustration” (feeling discredited, anger). Three styles of interaction were identified: most HCPs reassured and encouraged patients to get vaccinated (“patient-centered” style), some sought to convince them (“adamant” style), and some to inform them without discussion (“detached” style). In our study, HCPs describing a patient-centered interaction style emphasized emotions of connection more than of distance in their discourse, in contrast to those describing an adamant or detached style. Our results suggest that training programs offered to HCPs involved in vaccination discussions should consider the importance of emotions associated with vaccine discussions.
Introduction
Background
Healthcare professionals (HCPs) play a major role in the vaccination of the populations they serve: they inform, counsel, reassure, and vaccinate patients. They can thus find themselves in sensitive or even difficult situations when, for example, patients are reticent about vaccinations, have questions or fears, or evince a lack of interest (Lip et al., 2023). The HCP’s role is crucial in these situations because of the importance of trust between HCPs and patients (Peretti-Watel et al., 2019). Generally, when difficult situations arise during the care process (e.g., announcement of bad news or recommendation for palliative care), patients may experience negative emotions, including fear and anxiety (Finset, 2012; Weilenmann et al., 2018). HCPs may also experience emotions in such situations, including, for example, empathy or frustration (Martin et al., 2015; Weilenmann et al., 2018). HCPs’ emotions while interacting with patients can influence the course of a consultation and its general outcome, that is, patient adherence to recommendations and treatment (Lip et al., 2023; Scheepers et al., 2015; Weilenmann et al., 2018; Zolnierek & Dimatteo, 2009). Weilenmann’s classification (2021) distinguishes two main types of emotions that HCPs may experience during discussions with patients: those associated with affiliations or connections to patient (self-confidence, empathy, sadness for the patient) and those associated with distance (anger, exasperation, or frustration) (Weilenmann et al., 2021). Emotions linked to connection can foster favorable consultation outcomes by increasing HCPs’ well-being and satisfaction at work (Weilenmann et al., 2018, 2021) and by improving the quality of both patient care and patient trust (Derksen et al., 2015; Scheepers et al., 2015), thereby reinforcing patient adherence to HCPs’ recommendations and prescriptions (DiMatteo et al., 1993; Zolnierek & Dimatteo, 2009).
Because conversations about vaccination are potentially difficult situations for HCPs when their patients are hesitant or reluctant to vaccinate, they may well induce emotions in these professionals. These emotions may affect both the doctor–patient relationship and consultation outcomes, as shown in other fields; it is thus essential to understand their registers. Moreover, as one risk of conversations on this topic is that patients’ hesitancy or reluctance may be reinforced, rather than alleviated, we need to understand how HCPs handle these conversations and specifically if interaction styles (ways HCPs may approach a vaccination conversation) can be distinguished and to what extent they are linked to emotions. Research into HCPs’ emotional experiences during conversations about vaccination is nonetheless limited (Berry et al., 2017; Chou & Budenz, 2020; Loftus et al., 2021), and these potentially essential aspects of vaccination programs have not yet been explored in depth.
HCPs’ emotions can be influenced by the context and conditions of their practices, but also by their personal and professional values. These differ between professions within medicine (Matsumoto & Hwang, 2012; Russell, 1991; Weilenmann et al., 2018). The professional principles of nurses are strongly imbued by “care” (for patients and devotion to others) (Poorchangizi et al., 2019; Rassin, 2008; Sastrawan et al., 2019). For physicians, two important values are common to doctors from different countries: scientific objectivity, which underlies evidence-based medicine (Carretier et al., 2010; Coulehan & Williams, 2003), and a humanist approach that respects patients’ autonomy (Han et al., 2019; Wilson et al., 2013). These values may influence HCPs’ interactional and conversational styles—styles distinguishable partly by the space they leave for patients to voice their opinions (Bouchez et al., 2021) and by each HCP’s degree of cognitive empathy, that is, their ability to understand patients’ emotions while maintaining their clinical detachment. This detachment is defined by its distance from the patient’s emotions, intended to maintain HCPs’ scientific objectivity and protect their emotional balance (Austen, 2016; Decety & Jackson, 2004). Clinical detachment thus limits emotional empathy—the capacity to perceive the emotions of others (Decety & Jackson, 2004).
Understanding the emotions that emerge during consultations with vaccine-hesitant patients, the circumstances in which these emotions appear, and what is likely to influence their nature is important, given their influence on consultation outcomes. We investigated this topic in two different countries (France and England) where differences in organizing vaccination services and strategies for coping with vaccine hesitancy might influence how vaccination is discussed with patients. In France, vaccination of the general population has historically been conducted principally by general practitioners (GPs) (Verger et al., 2015), but the participation of other HCPs (nurses, midwives, and pharmacists) has increased over the past decade (Légifrance, 2022). Patients can choose to have the vaccine administered by their GP or another HCP. In England, various qualified professionals, including physicians, nurses, midwives, and pharmacists (UK Health and Security Agency, 2021), vaccinate the population. Routine vaccinations are provided free of charge through the National Health Service (NHS), usually to individuals registered with a general practice. Faced with marked vaccine hesitancy in the population (Ward et al., 2018), the French authorities extended the number of mandatory childhood vaccines from 3 to 11 in 2018. They also introduced the health pass in June 2021 to improve vaccination coverage against COVID-19 (Ward et al., 2022). The United Kingdom, with vaccine hesitancy levels much lower than in France (Larson et al., 2016; Lazarus et al., 2023), does not have vaccine mandates for the population. England briefly introduced COVID-19 health passes between December 2021 and May 2022 for entry into high-density venues (e.g., football stadiums), but this was not limited to proof of vaccination: a negative lateral flow COVID-19 test was also acceptable (GOV.UK., 2021). COVID-19 vaccination was mandated for care-home workers between November 2021 and March 2022 (GOV.UK., 2022a). It was also proposed for healthcare professionals, but the plan was withdrawn before the scheduled implementation date (GOV.UK., 2022b).
Objectives
This study had three main objectives, all appropriate for qualitative investigation: - To identify and describe the range of emotions that HCPs reported (and the associated circumstances) during consultations with patients hesitant about or opposed to vaccination, and to classify emotions by their type. - To identify clusters of emotions reported together in descriptions of interactions. - To identify different styles of HCP–patient interactions related to vaccination.
Methods
Ethical Statement
The ethics committees at the authors’ institutions approved this study, which was performed in accordance with the ethical principles stated in the Declaration of Helsinki. All participants gave informed consent before their interviews.
Design
This qualitative study interviewed HCPs involved in delivery of vaccination programs in France and England. The researchers conducted individual semi-structured interviews between June and November 2022.
Recruitment Procedures
We invited practicing HCPs (mainly GPs and nurses) involved in vaccination tasks (i.e., at least one of the following: prescribing, recommending, discussing, and/or delivering vaccination) who agreed to participate in the study. In France, the study took place in the southeast region and randomly selected 50 GPs from the public “Ameli direct” list of about 5300 GPs practicing in this region in 2022 (CartoSanté, 2024). This procedure was supplemented by the snowball method (asking interviewees to recommend other potential participants) due to the difficulty of recruiting among this population for this type of study (Bouchez et al., 2021). Nurses were recruited only through a professional organization: the Union Régionale des Professionnels de Santé Infirmières (the regional union of nursing professionals). Potential participants received an invitation by post or email a week before we telephoned them. Altogether, we were able to reach 30 GPs (from those randomly selected or using the snowball procedure) and 10 nurses to obtain the study sample of 18 participants in France.
HCPs in England were recruited by emailing invitations to a mailing list of 104 HCPs who had agreed to be contacted for an interview after they participated in an earlier quantitative survey as part of a wider research program (Garrison et al., 2023; Holford, Anderson, et al., 2024).
In both countries, we paid particular attention to the HCPs’ diversity (e.g., profession, sex, and age). Recruitment continued until the researchers agreed that the range of HCPs included was adequate and that data were sufficiently saturated to meet the main research objectives, that is, once the thematic analysis of the most recent interviews, separately in each country, no longer revealed any new themes (Nuzhath et al., 2023). Before participating, HCPs received an information sheet about the study, and participants provided written or oral consent before their interviews.
Data Collection
Interviewers were (female) postdoctoral researchers experienced in qualitative methods; they conducted the interviews in French or English, as appropriate, either by telephone or videoconference. All interviews were recorded with the participants’ explicit authorization. Participants were compensated for their time with a gift voucher (£20 in the UK and €50 in France, amounts determined by prior consultation with HCPs in each country). Interviews lasted from 20 to 60 minutes.
Researchers used an interview guide (Appendix—Qualitative interview guide) to conduct semi-structured interviews with open questions. This guide was developed based on the scientific literature on vaccine hesitancy and communication (Berry et al., 2017; Lip et al., 2023; Verger et al., 2022). It included the following topics: (a) HCPs’ experience in discussing vaccination with patients; (b) their confidence in their ability to conduct these conversations; and (c) the obstacles to and factors facilitating communication with patients on this topic. To collect information about each HCP’s emotions during these vaccination-related conversations with patients (especially vaccine-hesitant patients), interviewers encouraged participants to express their feelings (e.g., “How did you feel during this interaction?”), their self-confidence (e.g., “Can you tell me about the last interaction you had with a patient where you felt confident in the communication between you and your patient?”), and how well prepared they felt they are to have these discussions (e.g., “To what extent do you feel informed about vaccination?”). Participants were also asked to describe their role (“What do you consider your role to be in discussing vaccination with patients?”), and to talk about both how they respond to vaccine-hesitant patients (“How did you respond to the patient’s doubts?”) and the obstacles to discussion with their patients (“In general, what stops you from discussing vaccination with patients?”).
Analyses
The audio recordings of all interviews were transcribed verbatim, anonymized, and verified by the researcher who conducted the interview. Interviews conducted in French were transcribed, translated into English, and the translation verified by a second researcher. Analysis of the transcripts was supported by NVivo 1.7.1 software.
Coding Emotions and the Circumstances of Their Onset
Coding Framework for HCPs’ Emotions and Number of HCPs Reporting the Corresponding Emotions (n).

aIndicates emotions added to the initial Weilenmann (2021) categorization during the coding process.
Clusters of Emotions
During the coding process, EB’s observation that HCPs regularly reported some emotions together led us to analyze clusters of emotions. EB then charted the data in a framework matrix (Gale et al., 2013) to identify the clusters, including all the emotions expressed by each HCP. Potential relationships between codes could thus be visualized and emotions that appeared to be commonly experienced together could be identified. Cluster labels were found inductively by consensus: some emotions in each cluster stood out as most frequently reported. We named each cluster by its two main and thus most representative emotions.
Coding of Interaction Styles
Description of the Dimensions and Intensities/Degrees of Interaction Styles, Based on the Terms and Expressions Used by HCPs Describing Their Interactions With Vaccine-Hesitant Patients.
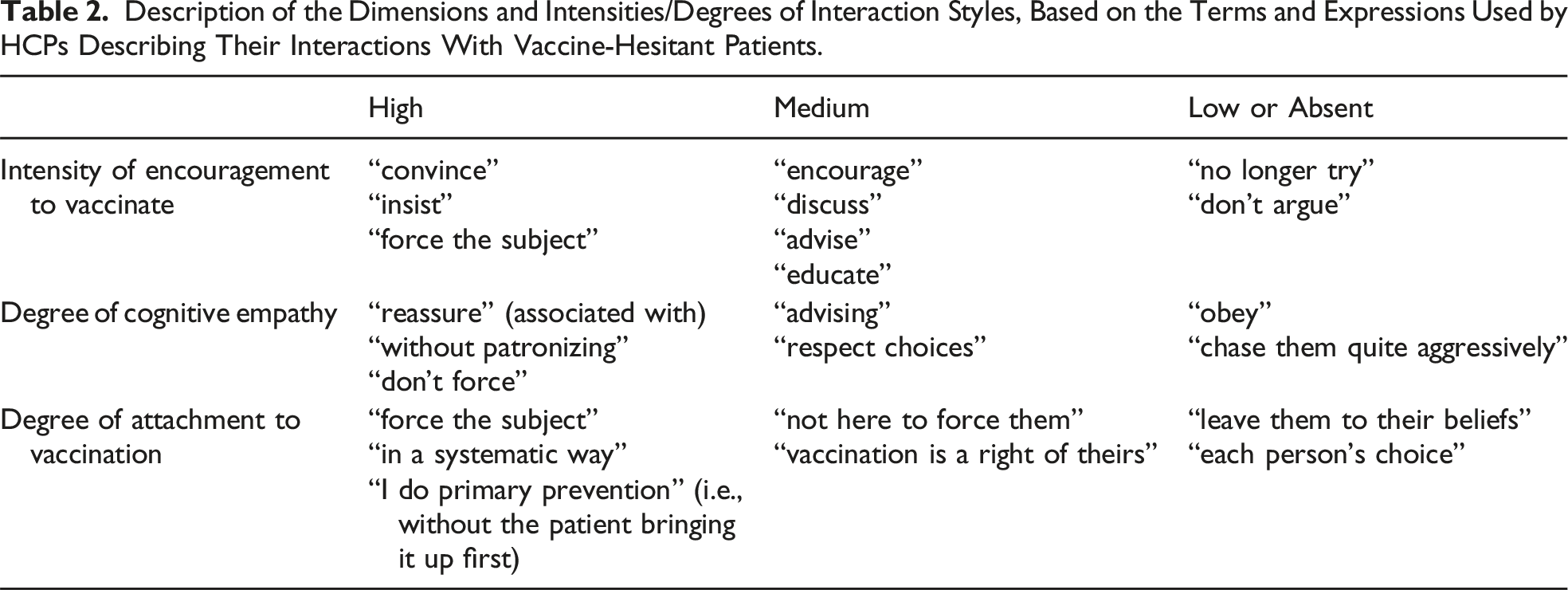
All transcripts were coded with this framework. Exploring relations between codes, that is, linking a given intensity in one dimension to a given intensity in another, enabled us to identify interaction styles.
Rigor
The efforts made during the study to ensure rigor are described in the Appendix, according to the criteria published in Ahmed (2024).
Results
Participants and Their Characteristics
Characteristics of Participants.
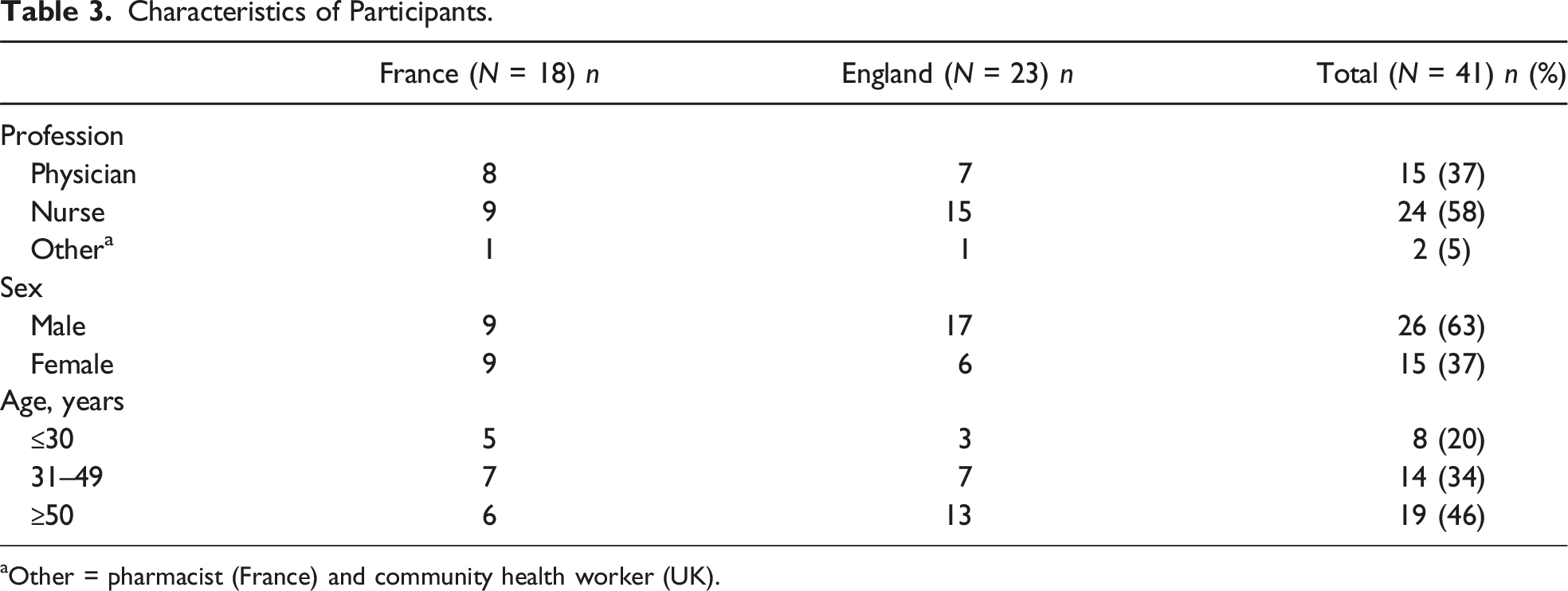
aOther = pharmacist (France) and community health worker (UK).
Emotions, Their Circumstances, and Their Clusters
HCPs reported a range of emotions in dealing with hesitant patients (Table 1). Half the participants mentioned both types of emotion, that is, at least one emotion of connection and at least one related to distance. Some emotions were mentioned more regularly than others in the HCPs’ discourse and are included in the transcript extracts below.
Connection Emotions
Self-Directed
Among the emotions HCPs directed at themselves, the most frequently reported connection emotion was self-confidence. This feeling emerged among HCPs (n = 17) when they felt experienced and competent in answering patients’ questions and in conducting conversations they considered complicated. Frankly, for me, it was very easy [to have conversations about vaccination with patients]. Because in fact, when we know what we are doing, and we are also convinced by what we are doing, we can pass the message on. (FR10, female, 56, nurse)
Patient-Directed
The patient-directed connection emotions most often reported were worry about the patient’s health (eight HCPs) and sadness regarding his or her situation (two HCPs). The first was described most often when the HCP feared that a patient would stop coming for regular medical care after complicated discussions about vaccination, but also when they worried about the fate of children whose parents were not choosing vaccination for them. I find it much more difficult with children to put that [worry] aside in my mind because like I say it’s them making a decision for a vulnerable young person. (UK17, female, 25, nurse)
Context-Directed Specific to COVID-19 Epidemic
Context-directed connection emotions were also reported. One, for example, was satisfaction at fighting against the pandemic by vaccinating patients—a feeling experienced by eight HCPs through their participation in an action (i.e., the COVID-19 vaccination campaign) that made sense for them. The fact I went back into uniform, I was doing my bit for the pandemic, was amazing that nothing was a challenge. I loved going to work every single day and that was that duty of care that I had. (UK13, female, 50, nurse)
Emotions of Distance
Self-Directed
The most reported distancing emotion was a feeling of incompetence; it appeared when HCPs (n = 9) did not know how to respond to a patient’s question or when they felt they lacked knowledge about the COVID-19 vaccine. It is true that sometimes I had some doubts, I mean, I didn’t always know what the best response was to their questions. (FR16, female, 26, physician)
Patient-Directed
Anger at the patients accounted for a considerable proportion of the distancing emotions reported by ten participating HCPs. It included frustration, which participants reported feeling toward patients who did not want to change their position about a vaccine or vaccination in general, and toward repeated arguments critical of vaccination and judged to be fallacious. As a professional, it’s quite frustrating because we’ve had conversations with [vaccine hesitant patients about vaccines in general and the MMR vaccination mentioned as an example]. They have fixed views that we’re not going to change and therefore we’re in this impossible situation where the only way to meet the targets [for vaccinating the population] is to forcibly vaccinate which of course you can’t do. (UK05, male, 52, physician)
Context-Directed, Specific to COVID-19 Epidemic
When the HCPs’ emotions concerned the COVID-19 pandemic, the emotion most frequently reported was concern and fear (eight HCPs) as a reaction to the uncertainties about the course of the pandemic. It was difficult, because we are always stressed that [the pandemic] will rebound and there will be a new variant that is coming. (FR07, male, 57, nurse)
Clusters of Emotions
Clusters of Emotions and Their Principal Associated Emotions.
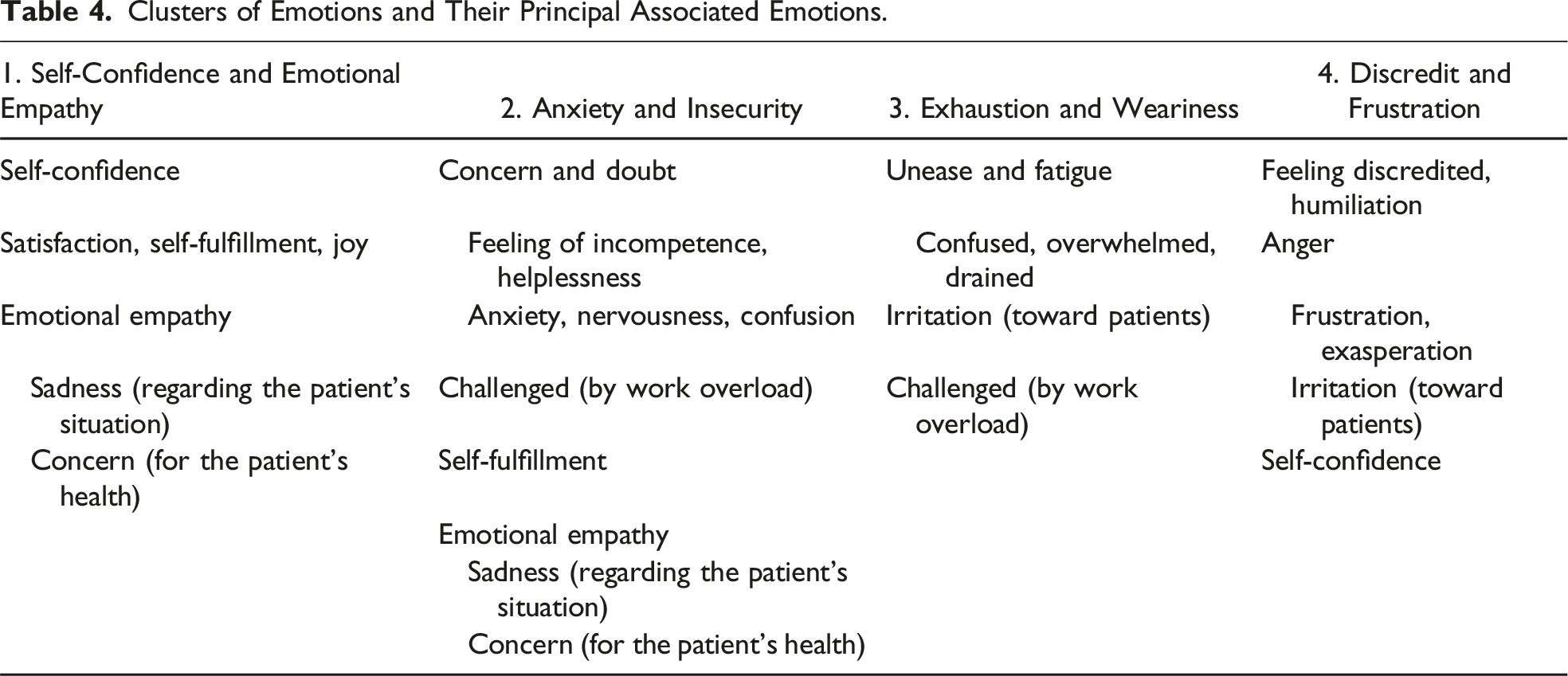
Self-Confidence and Emotional Empathy
In this cluster, connection emotions dominated. Seventeen HCPs often reported self-confidence, described above. Being able to talk about vaccination with their patients and provide them with knowledge brought these HCPs satisfaction. I feel very confident in addressing the topic of vaccination [in general] … I’m more than happy to sit and talk to anybody. (UK08, man, 65, nurse)
HCPs who reported self-confidence sometimes also showed evidence of emotional empathy toward their patients. Some explained that they were concerned about their patients’ health and therefore wanted to maintain a relationship of trust with them to ensure continuity of care. One professional reported that it was difficult for him to face up to his memories of certain patients he had treated in his career, as their situation was sometimes difficult. But sometimes it’s not good to have a lot of memories because we also remember the cases that were very difficult that we had, and it’s difficult to erase them from our memories. (FR12, man, 67, physician)
In all, 20 HCPs emphasized this cluster of emotions in their discourse rather than other kinds of emotions. They were mostly women, nurses, and HCPs practicing in England.
Anxiety and Insecurity
This cluster mainly represents distancing emotions, linked to the COVID-19 pandemic: nervousness and anxiety, doubts about the COVID-19 vaccines due to their recency, and doubts about their own professional skills. I was in the lion’s den. Information [about the COVID-19 pandemic and vaccination] came a long time afterward … I didn’t feel very secure in that …. (FR09, women, 57, nurse)
When HCPs’ worries were directed toward patients, however, they were sometimes associated with connection, expressing concerns about their patients’ health and sometimes limiting vaccination discussions with them for fear of losing their trust and to maintain the doctor–patient relationship. You end up in an argument and arguments aren’t good, … and it just doesn’t achieve anything. Because you want them to still trust you for other things as well … So it isn’t just about immunizations it’s about other advice that you may want to give in the future as well and that can be anything health-related. (UK09, women, 52, nurse)
Sometimes HCPs felt that their patients were grateful for their work; this feeling engendered positive emotions, such as self-fulfillment. Because, there are some [patients] who I saw afterwards who said “oh do you remember, I was one of the first ones sick and everything, thank you for everything that you did,” and I mean, that feels good … to see that we could help where we could, help, support, advice, not just health care. (FR07, man, 57, nurse)
Overall, seven HCPs in France and the United Kingdom described emotions in this cluster, fewer than those reporting self-confidence and emotional empathy, but they had similar characteristics: they were nurses (and a community health worker) and mainly women.
Exhaustion and Weariness
In this cluster, distancing emotions were dominant. Irritation and weariness appeared together in the discourse of some HCPs, linked, as they explained, to patients’ repeated use of the same arguments to criticize vaccination. Sometimes it can get a bit tiresome when these discussions come up again and again, repeating the same arguments over and over [against childhood vaccines, vaccination against hepatitis B and COVID-19]. (FR15, man, 35, physician)
These emotions were also linked to the HCPs’ perception that it was impossible to convince these individuals. Some HCPs reported disappointment when patients declined the opportunity to protect themselves and others. Their declarations mainly concerned vaccination against COVID-19, but also vaccination in general. I try to explain to them but I haven’t had any success. To everyone who came saying no to the [COVID-19] vaccine, I never managed to convince any on the contrary. (UK02, man, 46, physician)
Irritation also came from patient demands and the workload that discussions about vaccination involved, particularly during and after the COVID-19 pandemic. They expect you to be able to deliver the moon in a single consultation which clearly isn’t possible, and they, I think, probably are even more unrealistic, some of them, in their expectations. (UK06, women, 47, physician)
For some HCPs, this feeling was coupled with doubts about their ability in the pandemic context, an additional factor of difficulty. It wasn’t that easy, I don’t know if it was difficult, but it was not as easy as that, since ourselves, we didn’t, I mean for us, it was new, and for everyone it was new, this disease, this pandemic … So that was difficult, yes. It is difficult to reassure people. (FR13, female, 48, nurse)
Seven HCPs recounted mainly these emotions. This group included both nurses and physicians, mainly women, and all were older than 30.
Discredit and Frustration
The particular feature of this cluster is the feeling of discredit and humiliation felt by some HCPs when the patients challenged evidence that they considered well-founded and scientifically correct. In this situation, these HCPs felt attacked and devalued. Because they [patients opposing vaccination] reduce your work to participation in a conspiracy. When you try to give scientific arguments … they don’t even consider them so you feel a bit humiliated. (FR01, male, 25, physician)
These emotions also came with frustration, mostly when patients had what HCPs considered a stubborn mindset about vaccines, and scientific evidence had no effect on them. HCPs sometimes used the lexicon of combat. Some HCPs also felt helpless and sometimes tired, even weary of these situations. You’re just not going to win. (FR05, male, 52, physician)
This cluster of emotions was evoked mainly by seven HCPs. Among them, five practiced in France, six were physicians, and four were younger than 30 years.
Styles of Interaction and Clusters of Emotions
Description of HCPs’ Interaction Styles.
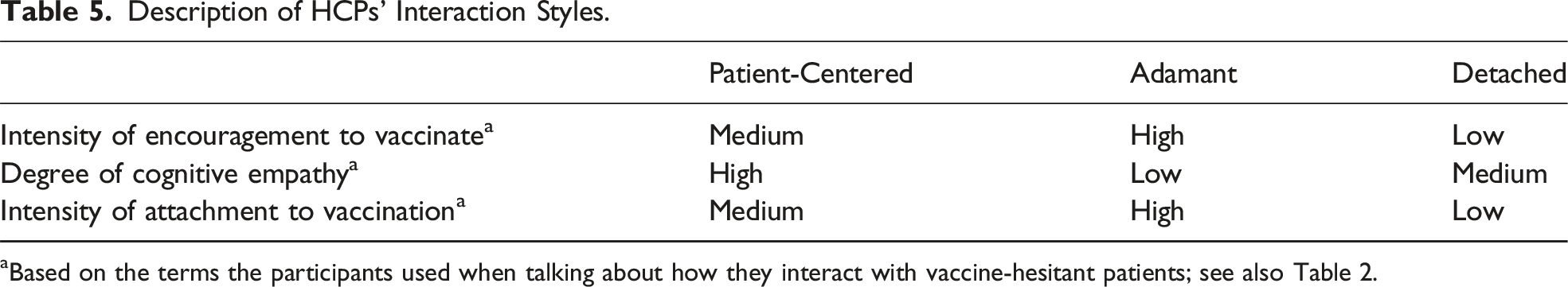
aBased on the terms the participants used when talking about how they interact with vaccine-hesitant patients; see also Table 2.
“Patient-Centered” Interaction Style (n = 26)
A patient-centered interaction style (emerging from the discourse of 26 HCPs) involved reassuring and encouraging vaccine-hesitant patients to lead them to accept vaccination. Participants recounted doing this by listening, discussing, and using cognitive empathy, while remaining attached to this objective. This interaction style was demonstrated by HCPs’ willingness to adopt a strategy of supporting vaccine-hesitant patients as they moved toward acceptance of vaccination in an empathetic, guilt-free, and non-hierarchical relationship, as illustrated respectively in the three citations below. I can spend that time with them to reassure them and most people, we managed to vaccinate .… It’s about getting on their level, and trying to unpick what it is they’re frightened about but also being prepared to … meet them halfway. (UK11, female, 56, nurse) If we explain to them that what they are doing is bad, we upset them even more … We need to have a more pragmatic approach, respect each other’s choices. (FR08, male, 42, nurse) I think sometimes when you’ve been sitting behind a table it looks like you are superior and you are telling them what to do, so I come and chat to them. (UK01, 62, male, nurse)
These HCPs insisted on the need not to push these patients and not to “force the subject on them.” HCPs using this interaction style regularly raised the issue of patient autonomy, underlining that vaccination is above all the patient’s choice. Sometimes, they mentioned that their patients could change their decision later and that it was necessary to give them the time to think about it. I don’t push them on the subject “well ok, it’s ok” I prefer to let them have time to think about it. And…voila. (FR05, female, 27, physician)
The HCPs who described this patient-centered style of interaction mainly emphasized the first cluster of emotions (self-confidence and emotional empathy) in their discourse; they felt satisfied with their work and had a sense of self-confidence.
However, some HCPs adopting this style of interaction tended to report anxiety and insecurity (cluster 2): they were keen to encourage patients to be vaccinated, but the context of the COVID-19 pandemic made them doubt their ability to do so. Most of these HCPs were nurses, mainly female, and practicing in England.
“Adamant” Interaction Style (n = 7)
The adamant style (n = 7) was characterized by the aim to convince patients to get vaccinated. HCPs reporting this style explained that they insisted on using scientific evidence to achieve their objective that the patient accept vaccination. Some explained that they did not wait for a patient to raise the subject of vaccination, and they “forced the subject” or “quite aggressively chased them, with phone calls and text messages.” Others used assertive language to describe and explain their interactions with vaccine-hesitant patients. I don’t wait for them to ask me those questions … I force the subject actually. As soon as they are at the key ages, like 25 years, 45 years, 65 years, I talk to them directly. … I have to find arguments. (FR01, male, 25, physician)
Some HCPs reported adopting this style during the COVID-19 pandemic, even though they felt uncertain about anti-COVID vaccines. … During the COVID period, of course, we were, we were overwhelmed with questions, with doubts, for these doubts we had to try to absolutely take them apart. (FR03, female, 28, physician)
The HCPs with an adamant interaction style did not report either cognitive or emotional empathy toward their patients. Instead, they reported discredit and/or frustration (cluster 4) when they failed to achieve the vaccination goal to which they were highly committed. These HCPs were mainly male physicians practicing in France.
“Detached” Interaction Style (n = 8)
Eight HCPs described an interaction style that we called detached, marked by an unwillingness to discuss vaccination with vaccine-hesitant patients; they recommended the vaccines and then did not respond to the patients’ refusals. They explained that in preceding conversations with hesitant patients, they had felt frustrated by their failure to convince these patients to accept vaccination and no longer insisted or even tried to encourage patients, especially those whom they already knew and who had refused, sometimes for years, to be vaccinated. [The patients] say in any case they will not get vaccinated for this or that reason. I admit that I no longer try to convince them. (FR02, female, 52, physician)
This detachment could sometimes take the form of a rather radical position toward vaccine hesitancy—by limiting or making it impossible for these patients to express their concerns. We’re very clear when we take the consent nobody is making you have this. You do not have to have this. You can get up and walk away. I don’t care. It’s your choice … But you get to the point where you kind of like think I’m going to say something that I shouldn’t. You say it after they’ve gone, you know. (UK20, female, 66, nurse)
These HCPs did not clearly report one cluster of emotions more than another. Some said they felt confident talking about vaccination with their hesitant patients (cluster 1), but a low attachment to the goal of vaccination reduced their propensity to engage in discussions with hesitant patients. I don’t mind challenging people nicely because I think I’m fairly skilled at it and there are other times when I shut my mouth because I think it’s not worth the battle. (UK20, female, 66, nurse)
Others felt weary and tired (cluster 3)
These HCPs were mostly women, but shared no other particular characteristics.
Discussion
This study is the first to focus on HCPs’ emotions during conversations with vaccine-hesitant patients and to point out their importance in interaction styles. We identified four clusters melding emotions frequently reported together in descriptions of interactions: self-confidence and emotional empathy (cluster 1); anxiety and insecurity (cluster 2); exhaustion and weariness (cluster 3); and finally discredit and frustration (cluster 4). We also identified three principal interaction styles during HCPs’ discussions with vaccine-hesitant patients, based on the HCPs’ descriptions: some reported a patient-centered style, considering patient concerns and supporting them as they moved toward accepting vaccination, while respecting their choice. Some were adamant, seeking to convince their patients through the force of their arguments, and others were detached, giving their patients information without engaging in a discussion around vaccination. Our results suggest that a patient-centered style may be associated more with emotions of connection than of distance. Conversely, an adamant interaction style may be associated with emotions that distance more than they connect, whereas a detached style may be associated with a greater mixture of emotions.
Clusters of Emotions, Styles of Interaction, and Degree of Cognitive Empathy
By identifying interaction styles, we do not mean to imply that the range of HCPs’ reactions toward patients with vaccine hesitancy is reducible to these styles; these reactions may vary, from one consultation to another, in particular according to the intensity of vaccine hesitancy. However, many of our participants’ descriptions (e.g., of how they used to broach the subject of vaccination) went beyond specific conversations. Interaction styles similar to those found in our study have been observed in qualitative studies in various countries, some conducted during the COVID-19 pandemic (Berry et al., 2017; Bouchez et al., 2021; Cardano et al., 2022; Connors et al., 2017; Nuzhath et al., 2023; Ruijs et al., 2012). The detached style in our study was similar to that of HCPs “adapting to parents’ opinions” in Bouchez et al. (2021); these professionals felt that conversations about vaccination were unnecessary with hesitant patients, and left them to decide themselves. Similarly, the patient-centered style in our study corresponds to that of the “exploring and informing” HCPs in Berry et al. (2017): nurses and doctors who explored the reasons for vaccine hesitancy and suggested answers, while respecting patients’ views.
Many studies have pointed out the value for HCPs of applying a posture of cognitive empathy in their care practices—the capacity to understand patients’ emotions while simultaneously and voluntarily detaching themselves to protect their own well-being and maintain their medical objectivity (Austen, 2016; Derksen et al., 2015; Kerasidou & Horn, 2016). This approach is a powerful means of interindividual communication and one of the key elements in a therapeutic relationship (Decety & Jackson, 2004). During consultations about vaccination, it can help HCPs to have a better understanding of their patients’ reasons for vaccine hesitancy and the emotions it can induce (Berry et al., 2017; Bussink-Voorend et al., 2022)—and to adapt their response accordingly (Derksen et al., 2015). Cognitive empathy is also an effective factor in increasing vaccine acceptance, as demonstrated with motivational interviewing techniques (Gagneur et al., 2019; Verger et al., 2023) or the empathetic refutational interview (ERI), a new approach enabling HCPs to respond objectively to patients’ concerns, while maintaining empathy and a relationship of trust during vaccination consultations (Holford, Schmid, et al., 2024).
Most of the HCPs adopting a patient-centered interaction style showed cognitive empathy. Previous publications have shown that HCPs may adopt a posture of cognitive empathy during conversations about vaccination (Berry et al., 2017; Loftus et al., 2021). This posture might explain, at least in part, why HCPs in our study who adopted a patient-centered interaction style emphasized emotions associated with connection (cluster 1). Connection emotions, such as self-confidence, have been reported in earlier studies of HCPs’ experiences with caring for patients with COVID-19 (Cui et al., 2021; Ness et al., 2021; Sun et al., 2020).
Nonetheless, some HCPs adopting a patient-centered interaction style noted anxiety and insecurity (cluster 2) together with connection emotions. They reported feelings of incompetence that, consistent with previous studies (Cziraki et al., 2018; Ness et al., 2021; Abu Sharour et al., 2022; Smith et al., 2021; Sun et al., 2020), were related to the COVID-19 pandemic, especially among nurses. In general, the patient-centered interaction style and its potential ability to foster mainly connection emotions and cognitive empathy might be beneficial for the quality of the provider–patient relationship as well as for HCPs’ well-being while simultaneously supporting changes in patients’ attitudes and behaviors (Austen, 2016).
Unlike the patient-centered style, an adamant interaction style was associated mostly with the distanced emotions of cluster 3 (exhaustion and weariness) and/or cluster 4 (discredit and frustration). In our study, HCPs who adopted this style showed attitudes previously observed by Berry et al. (2017): they were eager to preserve their patients’ health and well-being by vaccinating them and were confident in their own medical expertise. Among this group, some reported trying to explore patients’ vaccine hesitancy, but descriptions suggest they did so without adequately respecting the patients’ autonomy. Others, upset by vaccine reluctance, expressed dismay and dissatisfaction. These emotions seem to appear more generally in situations where HCPs are struggling to resolve the tension between their duty to be effective and their patients’ resistance (or other obstacles) (Kempe et al., 2015; Loftus et al., 2021; Wilson et al., 2013). The intensity of the emotions reported sometimes by HCPs describing an adamant interaction style in our study may be a potential obstacle to adopting a posture of cognitive empathy. Some studies suggest that lack of empathy and of respect for patients’ autonomy can reinforce patients’ vaccine hesitancy by a psychological mechanism called reactance, defined as a reaction to feeling that one’s individual autonomy and freedom are threatened (Sprengholz et al., 2022; Cardano et al., 2022). Others suggest that when HCPs are too insistent on vaccination, some vaccine-hesitant patients turn toward complementary and alternative medicine (CAM), which is perceived as more respectful of patients (Deml et al., 2022; Peretti-Watel et al., 2019).
A detached style was associated with a mixture of emotions. Consistent with our results, other work indicates that some HCPs may use strategies of avoidance or delay of sensitive conversations about vaccination, either to preserve their therapeutic relationship with the patient over the long term or because they lack the time necessary for conversations (Berry et al., 2017; Bouchez et al., 2021). HCPs may also lack the skills to handle these conversations, and/or may be vaccine-hesitant themselves, which could affect their willingness and ability to discuss vaccination (Verger et al., 2022). This detached interaction style can result in losing the opportunity to broach the subject of vaccination with vaccine-hesitant patients and failing to explore this hesitation (Cardano et al., 2022).
The Professional Values and Socialization That May Underlie Interaction Styles and Clusters of Emotions
HCPs’ adoption of one style of interaction rather than another may be related in part to their internalization of professional values, through professional socialization. In our study, the HCPs with a patient-centered interaction style and who described mainly emotions from clusters 1 (self-confidence and emotional empathy) and 2 (anxiety and insecurity) were mostly nurses. Nurses’ professional values, which are strongly imbued with the care model of dedication, listening, and empathy, may influence this professional group to feel connection emotions more readily and to adopt a patient-centered style of interaction (Rassin, 2008). Qualitative studies in Ireland and the United Kingdom show that nurses often implement vaccination strategies based on cognitive empathy to help patients manage their emotions and to construct a relationship of trust (Cardano et al., 2022; Loftus et al., 2021). Moreover, nurses may be more inclined than physicians to present the scientific evidence in a manner that supports the patient’s informed decision-making process and facilitates patient autonomy (Rassin, 2008). Our results suggest that some nurses have doubts about their ability to manage conversations with vaccine-reluctant patients, particularly related to COVID-19 vaccination. These doubts may be due to inadequate training, but they may also reflect good self-knowledge, especially in an ever-changing field (as during the COVID-19 pandemic).
HCPs who described an adamant interaction style and highlighted emotions such as discredit and frustration were mostly physicians. They felt that vaccine-reluctant patients challenged their learning and their scientific knowledge, but also, as expressed in several interviews, their integrity. This is consistent with the results of studies of HCPs’ emotions during difficult conversations with their patients in various care situations (Martin et al., 2015) as well as with parents who refuse to vaccinate their children (Berry et al., 2017). In other studies, HCPs also reported frustration dealing with patients who believed media reports over the scientific evidence presented by their HCPs, especially during the COVID-19 pandemic (Loftus et al., 2021; Ness et al., 2021).
In recent decades, medicine has evolved toward a model of shared decision making, which allocates a more important place than before to patients’ involvement in the choice of their treatment and to consideration of their preferences, feelings, and perceptions (Faiman & Tariman, 2019). Some physicians continue to be strongly invested in the model of knower, as expressed by their tendency to push information toward patients without first listening adequately to them (Mjaaland et al., 2011). Medical studies transmit strong professional values, in particular the importance of scientific knowledge, objectivity, and the obligation of means to cure or prevent diseases (Coulehan & Williams, 2003; Wilson et al., 2013). To protect or even guarantee this objectivity in patient consultations, medical students are thus encouraged to show clinical detachment so that they avoid becoming emotionally involved during patient interactions (Weilenmann et al., 2021). Emotional and cognitive empathy have been observed to decrease among these students during this process of professional socialization (Neumann et al., 2011; Phillips & Dalgarno, 2017).
Organizational Setting and Professional Role
Other factors must be considered to explain our observations, especially the organizational setting of vaccination and the roles of the different HCPs. Nurses in England have played an important role in population vaccination for a greater period of time than nurses in France, who at the time of our study were not authorized to prescribe most vaccines independently of physicians. This responsibility of nurses in England and the experience they have accumulated may have led them to develop relational skills in this domain and self-confidence in their relationships with patients (Abu Sharour et al., 2022). Nurses in England are also incentivized to encourage patients to accept vaccination, especially for their children; to do this, some adopt organizational strategies, such as making appointments for vaccination during a consultation (Cardano et al., 2022). Given the current shortage of physicians and other HCPs in Europe (OECD, 2014), health authorities of some countries promote an organization of primary care that enables closer collaboration between physicians and nurses. This could promote recognition of nurses’ skills and improve their autonomy, self-confidence (Bakker et al., 2000; Abu Sharour et al., 2022), and quality of care by enabling the transfer of tasks that demand time (such as health education) from physicians to nurses (Fournier et al., 2018).
Strengths and Limitations
Our international study explored the emotions associated with vaccination consultations among a range of HCPs in two countries with different healthcare systems. It offers a new analysis of emotions: the interviews were conducted to allow the participants to express emotions spontaneously when reflecting on recent interactions with patients about vaccines. HCPs were not asked directly what emotions they felt when dealing with hesitant patients precisely to avoid introducing any influence or suggestions by the interviewer (see Appendix—Qualitative interview guide). Our study provides novel findings on the different clusters of emotions among HCPs in the context of vaccination conversations and their possible association with specific interaction styles. This information is essential to support HCPs’ role in vaccination programs (see the subsection Implications for Policy and Practice).
It is important to acknowledge our study’s limitations. The data were collected through self-reported responses during interviews reflecting on memories of recent conversations with patients. Descriptions may therefore overrepresent what has happened recently rather than what usually happens. However, asking HCPs to talk about a recent interaction is more realistic than asking for an overview, for which respondents may become more hypothetical and less anchored to real events. HCPs might have portrayed their experiences more positively than they are in reality (social desirability bias). Nevertheless, the manifestation of negative emotions and expressions of insecurity among the HCPs provides compelling evidence that the data are reliable and informative. We could not take into account the clinical context of consultations (reasons, patient characteristics) or that of the HCPs’ practice environment (i.e., their typical number and type of patients, staffing levels, stress), which might well affect emotions and interaction styles. We must remain aware that the researchers bring their own conceptions to the interpretation of HCPs’ reports of conversations. While our sample was too small to make definitive statements of associations between professions, interaction styles, and clusters of emotions, the patterns suggested by our results are consistent with the existing literature.
Research Gaps
More research is needed to investigate these results further, especially to reduce the distance between real events and those reported in interview transcripts. Evaluation of communication approaches in real time, for example, using conversation analysis of consultation recordings, could be valuable. For example, video recordings have demonstrated their feasibility and offer the possibility of repeated analyses by different observers, and access to nonverbal manifestations; they can be analyzed in multiple ways, quantitatively and qualitatively (Golembiewski et al., 2023). Studies with larger, more representative samples of more diverse HCP types could also enable further exploration of the associations between interaction styles and emotions in various vaccination contexts that can be associated with different challenges. Specifically, useful research directions could include a robust examination of differences by profession and/or professional context, an assessment of the extent to which interaction styles are stable or vary with vaccination contexts, whether they lead to the emotions involved, or vice versa, and of whether training clinicians to adopt a more patient-centered, empathetic interaction style can lead to a positive shift in the emotions experienced.
Implications for Policy and Practice
Better support should be offered to HCPs in their vaccination roles. It is essential that HCPs undergo initial and continuing training to acquire and update solid scientific knowledge about vaccine-preventable diseases and vaccines. They also require training to acquire core skills in communicating and interacting with patients, as suggested by the potential association between interaction styles and different clusters of emotions. In this regard, techniques for communicating empathetically with vaccine-hesitant patients, such as motivational interviews or empathetic refutational interviews, can be taught (Gagneur et al., 2019; Holford, Schmid, et al., 2024). Additionally, training interventions of HCPs based on mindfulness have proved useful in promoting their emotional awareness, recognition, and regulation (Jiménez-Picón et al., 2021).
Conclusion
Our novel findings suggest that HCPs in both France and the United Kingdom experience a range of clusters of emotions associated with connection or distance during conversations with vaccine-hesitant patients; these clusters are potentially associated with certain interaction styles even though HCPs may have a wider range of reactions. Some of these emotions (distancing) and some styles of interaction (adamant and, to a lesser extent, detached) can be counterproductive in ensuring the well-being of HCPs and patients, as well as for the outcomes of these conversations. Given the central role of HCPs in vaccinating the population, their emotions in the context of vaccine discussions—especially distancing emotions—must be recognized and considered.
Supplemental Material
Supplemental Material - Healthcare Professionals’ Emotions of Distance and Connection When Dealing With Patients’ Vaccine Hesitancy: Interaction Styles, Values, and Implications
Supplemental Material for Healthcare Professionals’ Emotions of Distance and Connection When Dealing With Patients’ Vaccine Hesitancy: Interaction Styles, Values, and Implications by Emeline Brosset, Emma Anderson, Amanda Garrison, Dawn Holford, Harriet Fisher, Patrick Peretti-Watel, Stephan Lewandowsky, and Pierre Verger in Qualitative Health Research
Footnotes
Acknowledgments
All authors thank the participants of the study for their contribution, Jo Ann Cahn for translating the manuscript into English, and Patrick Berthiaume (Les Formations perspective santé Inc., Québec, Canada), Eve Dubé (Laval University, Québec, Canada), and Jeremy Ward (INSERM, Villejuif, France) for their invaluable advice. H.F. and E.A. acknowledge support from the NIHR Health Protection Research Unit in Behavioural Science and Evaluation at University of Bristol. The Health Protection Research Unit (HPRU) in Behavioural Science and Evaluation at University of Bristol is part of the National Institute for Health Research (NIHR) and a partnership between University of Bristol and UK Health Security Agency (UKHSA), in collaboration with the MRC Biostatistics Unit at University of Cambridge and University of the West of England.
Author Contributions
D.H., A.G., E.A., H.F., S.L., and P.V. were involved in the study’s conception and design. D.H., A.G., E.A., H.F., and P.V. were involved in designing the study’s interview guide. D.H., A.G., E.A., and H.F. were involved in data collection and the general coding frame. E.B., P.V., E.A., and P.P.-W. were involved in the conception of the specific coding frame for this manuscript, interpretation of the data, and drafting of the paper. D.H., A.G., E.A., H.F., P.P.-W., S.L., and P.V. were involved in revising the paper critically for intellectual content. All authors approved the manuscript for publication and agree to be accountable for all aspects of the work.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was co-funded by the European Union’s Horizon 2020 research and innovation program (JITSUVAX Project, Grant Number 964728) and by the ICOVAC project (Impact du Covid-19 sur la vaccination en France, Grant Number ANRS0344), which has been funded and labeled as a National Research Priority by the National Orientation Committee for Therapeutic Trials and other research on COVID-19 (CAPNET).
Ethics Statement
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
