Abstract
The end of treatment is known to be a particularly challenging time for many cancer survivors as they transition to coping with their condition independently. They may engage in health behaviours, such as implementing drastic dietary changes to manage the side effects of treatment they have undergone or as a way to assuage their anxiety. Understanding cancer survivors’ heightened preoccupation with healthy eating is therefore fundamental to our understanding of the psychological phenomenology of cancer. This study explored how people who have developed a heightened preoccupation with healthy eating after a cancer diagnosis make sense of this change. Eight participants were recruited through social media. They each engaged in a semi-structured interview over Zoom concerning their changed relationship with food following cancer. Their accounts were then analysed using interpretative phenomenological analysis (IPA). The article focuses on four group experiential themes arising from the analysis: Open and Enlightened About Food, Becoming a Better Me?, Developing a New Passion for Nutrition, and Becoming Consumed by Food. The themes that arose from the analysis speak to the experience of becoming a ‘better’ person from having lived through cancer and developed a new relationship with food. Instead of seeing illness as a loss, several of the participants reported a positive shift linked to having developed an interest in healthy eating, something which became central to their identity. However, others experienced their new engagement with healthy eating as a preoccupation that engulfed them. These findings are discussed in light of existing theory and research, and their clinical implications are outlined. Areas for future research are also suggested.
Introduction
Over the last 40 years, cancer survival rates have doubled in the United Kingdom, with half of those diagnosed with cancer surviving for 10 years or more (Cancer Research UK, 2020a, 2020b), spurring a multidisciplinary effort to improve the health-related quality of life for cancer survivors (CS) across medicine, nutrition, and psychology (Montazeri, 2008). To date, most research in this field has investigated the profiles of breast, colorectal, and prostate CS (those with the highest 5-year survival rates; Cancer Research UK, 2020a, 2020b) and the health behaviours they engage in (Beagan & Chapman, 2004).
Throughout the literature, the most ubiquitous behavioural change that is reported among CS is related to dietary habits (Kappauf et al., 2000; Sullivan et al., 2021). Between 45% and 56% of CS make healthy dietary changes, such as increasing their intake of fruits, vegetables, and fibre and reducing their consumption of sugar, alcohol, and fats (Blanchard et al., 2003; Demark-Wahnefried et al., 2000; Maunsell et al., 2002; Shneerson et al., 2015). Research has shown that these changes can help individuals maintain a healthy weight and adequate levels of vitamins, minerals, and phytochemicals, thus reducing the risk of cancer recurrence (Cancer Research UK, 2020a, 2020b). However, a small proportion of CS, particularly women with breast cancer, appear to make more drastic and potentially harmful food choices, guided by the belief that they are increasing their wellbeing and preventing the recurrence of cancer (Beagan & Chapman, 2004). A preoccupation with healthy eating following cancer is therefore an important topic, yet one on which research remains sparse. This is the gap that the present study set out to address.
The article will begin with a concise literature review, followed by a presentation of the study’s aims, methodology, and key findings. It will end with a comprehensive discussion of its clinical implications.
Health behaviours can be defined as the modification of detrimental habits like smoking, inadequate nutrition, and inactivity among CS that may alleviate cancer treatment side effects, potentially lower the risk of recurrence for certain cancer types, and decrease the risk of other prevalent conditions (Pinto et al., 2000). Research has shown that while many CS make no changes in their behaviours following treatment (Beagan & Chapman, 2004), others may view drastic modifications as an essential and immediate response to their illness, a phenomenon known as the ‘teachable moment’ (Demark-Wahnefried et al., 2000). The potential impact of such behavioural changes is manifold. Regan-Smith et al. (2006) argue that self-care behaviours – the actions individuals take daily to maintain their health and wellbeing – help restore a sense of ownership over the illness. Some individuals may even develop a renewed sense of agency and positive self-perception through the process of re-evaluating their identity (Brennan, 2001).
Of particular relevance here is the idea of living with and beyond cancer (LWBC) in that it describes adjusting to and coping with cancer consequences and treatments (Foster & Fenlon, 2011). While the concept is widely used, it lacks clarity and has varying definitions. A conceptual framework was developed by Le Boutillier et al. (2019) to clarify the LWBC process and address CS needs. They did so by engaging in the identification and synthesis of various narratives of LWBC into a “conceptual framework” (Le Boutillier et al., 2019, p. 949). Three themes emerged: adversity, restoration, and compatibility. Adversity refers to the process of dealing with the life-altering effects of being diagnosed with cancer and its ensuing treatments. The researchers found that some CS felt as though they had lost some control due to being unable to participate in their treatment provisions and that they regained agency by being able to “play a part” (Beynon et al., 2015, p. 173). Others, on the other hand, experienced ongoing distress due to the ever-present fear of recurrence. The second theme, restoration, addresses the adjustment process. Finally, compatibility highlights changes in perspective and self-awareness, even amidst suffering. This final theme suggests that individuals have different approaches to cancer and is reminiscent of Tedeschi and Calhoun’s (2004) theory of post-traumatic growth, whereby, following a significant life crisis, individuals may experience ongoing significant and positive shifts around their relationships, their enjoyment of life, and an augmented perception of their individual strength. Le Boutillier’s framework takes the concept of post-traumatic growth further in that it suggests that CS may move back and forth between the stages they identified, rather than moving through a linear process.
The loss of control that is central to the theme of adversity in Le Boutillier’s study had already been explored by Taylor and colleagues (1983). The researchers carried out interviews with 78 women with breast cancer and found that two-thirds of participants perceived that they had some control over a cancer relapse, 37% perceived they had ‘a lot of control’, and the last third believed that although they did not have direct control over their cancer recurrence, doctors could in some way exert some control. They termed this sense of control, mastery, and referred to this process of cognitive restructuring as being “based on illusions, that is, beliefs that have no factual basis or that require looking at known facts in a particular way” (p. 1171). For the authors, these ‘illusions’ were best seen as facilitating positive action. Seeing reality as it truly is, they argued, may sometimes lead CS to feel as though they cannot exert any influence over their situation; this may in turn render them passive and have a negative impact on their mood. By contrast, believing in one’s ability to exert control over the illness could yield important psychological and behavioural benefits.
One documented way CS can assert control in this way is through their food choices, driven by the belief that certain nutritional changes will not only increase their wellbeing but also mitigate the risk of a recurrence. However, while better nutrition can yield beneficial physical and psychological outcomes, a small proportion of CS, particularly women with breast cancer, appear to become preoccupied with strict ‘fad diets’, such as macrobiotics or raw veganism (Bratman & Knight, 2000), which may be harmful and are not founded on scientific knowledge (Huebner et al., 2014). They include foregoing entire food groups that are often unrelated to the prevention of cancer (Maskarinec et al., 2001).
In the context of this study, a heightened preoccupation with healthy eating refers to an intense and often obsessive focus on making dietary choices that are perceived as being beneficial for one’s physical health and wellbeing, and in preventing the recurrence of cancer. This preoccupation typically involves an extreme level of attention to food selection, nutrient content, portion sizes, and the complete avoidance of certain foods or food groups that are deemed unhealthy or harmful. People who experience a heightened preoccupation with healthy eating may engage in behaviours such as meticulously planning meals, strictly adhering to specific diets, and experiencing significant distress or anxiety when faced with food choices that do not align with their perception of ‘healthy’ eating.
Aims
Due to the central importance of nutrition for a large proportion of CS, more specific research into the relationship between cancer and a heightened focus on healthy eating is warranted. Many of the studies currently available have focused on the broader use of complementary and alternative medicine (Molassiotis et al., 2005; Moschèn et al., 2001) or simply on dietary changes (Kassianos et al., 2015). Since traditional medicine often focuses on understanding disease processes at the biological level rather than considering the experience of illness from the perspective of the suffering individual (Little et al., 1998), the present study seeks to move away from a purely medicalised perspective and instead focus on the lived experience of illness from the perspective of the individual. Indeed, understanding how some CS may develop a preoccupation with healthy eating is fundamental to our understanding of the psychological phenomenology of cancer. Moreover, the insights acquired through this research may highlight the potential development of detrimental dietary habits among CS. The aim of this phenomenological study is therefore to explore the experience of CS who have developed a heightened preoccupation with healthy eating.
1
It will address the following questions: 1. How do CS perceive and understand themselves as they become preoccupied with their eating habits following a cancer diagnosis? 2. How do CS experience the change in their lifestyle following a cancer diagnosis, and how do they make sense of it?
Methodology
This research used an interpretative phenomenological analysis (IPA) approach, underpinned by a critical realist epistemology, to foster an in-depth and idiosyncratic understanding of the participants’ experiences (Barker et al., 2002; Bhaskar, 1975). The research question was particularly suited to IPA as this methodology has been applied primarily within the field of health psychology (Brocki & Wearden, 2006). Rather than assuming that illness is predictably experienced in the same way by all, IPA seeks an understanding of individual “patients’ perceptions and interpretation of their bodily experiences, and the meanings which they assign to them” (p. 5). To date, no qualitative study has explored the development of a heightened preoccupation with healthy eating among CS. Attending to the depth and complexity of these experiences, and to the sense-making around them, is therefore crucial in order to lay the foundation for further research and interventions in the fields of psychology and oncology (Smith, 2004).
Demographic Characteristics of the Full Sample of Participants.
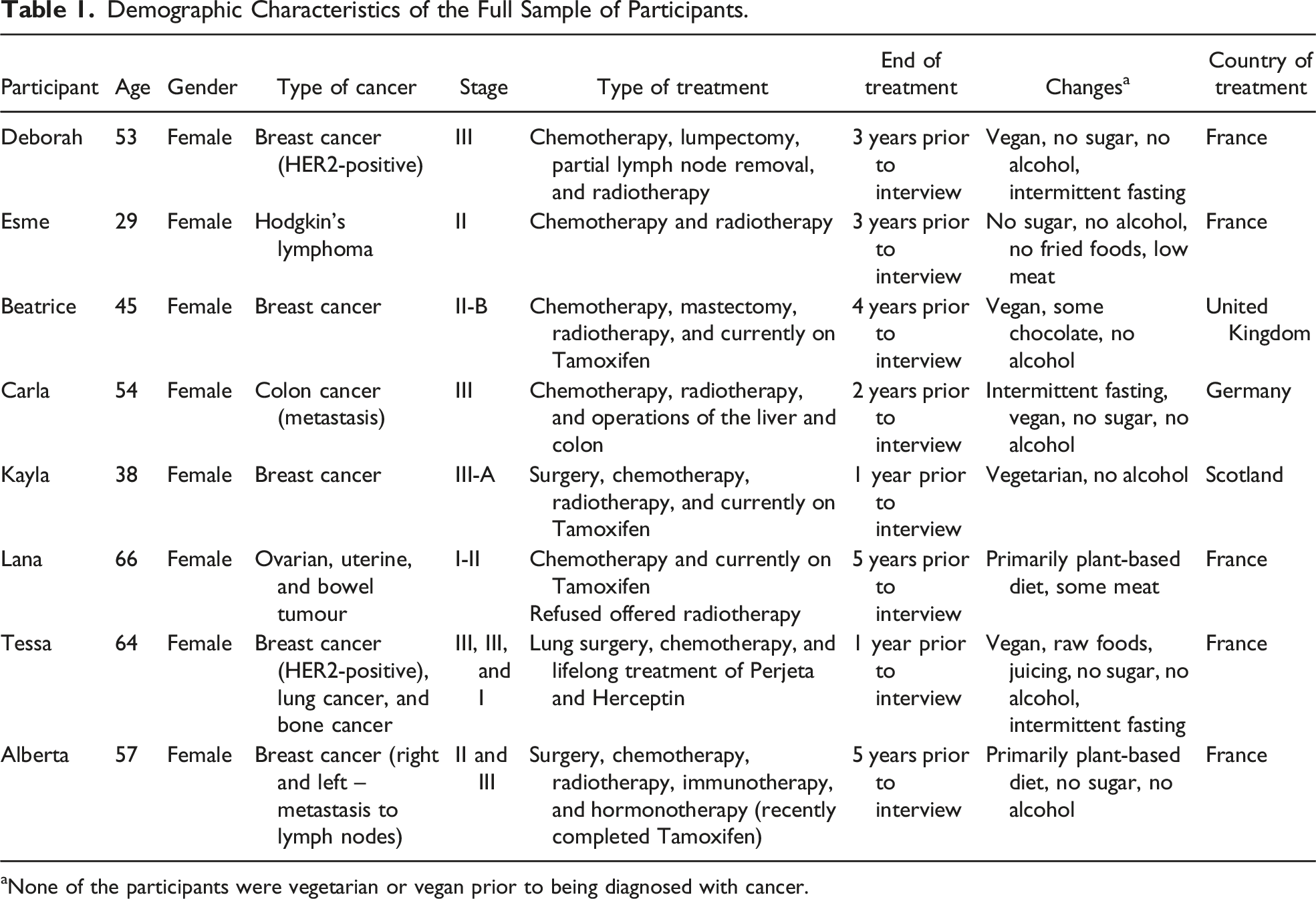
aNone of the participants were vegetarian or vegan prior to being diagnosed with cancer.
Recruitment was carried out through research advertisements published on Facebook, and participants were selected based on their suitability. Once potential participants had expressed interest in participating in the study, they were sent a participant information sheet. If they confirmed their willingness to participate, they were then sent a consent form to sign and return prior to the interview. To be eligible, participants needed to be over 18, have ended cancer treatment at least a year prior, and have Stage IV (non-terminal) cancer or below (excluding pancreatic and neck–throat cancers) whilst showing no permanent food/digestion impairments from cancer treatment. Moreover, participants would have no history of severe mental health difficulties and no prior eating disorder. A heightened preoccupation with healthy eating was measured by asking possible participants whether they could self-report an increased preoccupation with ‘the quality of food’ that stemmed directly from their experience of being diagnosed with cancer. These criteria were carefully devised to ensure sample consistency while eliminating potential confounding factors, such as the side effects of treatment and pre-existing mental distress and excluding anyone who may not have voluntarily made changes to their eating patterns.
Due to the restrictions imposed by the COVID-19 pandemic, the participants were interviewed over Zoom, using a semi-structured interview schedule. The interviews were carried out by the first author between August and December 2021 and lasted between 70 and 120 minutes, with a mean duration of 90 minutes. The interview questions were designed to capture the nuances of the participants’ experiences in the following domains: • How participants had experienced being diagnosed with cancer. • How they thought that this experience had affected them, and how they managed any negative impacts (physically and psychologically). • How they perceived their relationship with food to have changed since being diagnosed, and what these changes were. • What they perceived to be the main reasons behind making these changes, and whether they intended to make any further changes going forward.
The interviews were audio-recorded and transcribed verbatim. Seven of the interviews were conducted in English. One was conducted in French and translated by a professional translator, who cross-referenced their work with the first author to ensure an accurate understanding of the context and meaning. The transcripts were subsequently analysed following the IPA guidelines outlined by Smith et al. (2022).
Although this study employed an inductive analytic technique to accentuate the participants’ unique and individual experiences (Smith & Eatough, 2007), even a “giving voice” approach “involves carving out unacknowledged pieces of narrative evidence that we select, edit, and deploy to border our arguments” (Fine, 2002, p. 218). The analytical work was primarily carried out by the first author, the second author feeding in at every stage.
The first stage entailed an ‘immersion’ in the data through the transcription of the interviews, as well as an iterative and idiographic reading of the transcripts (Smith et al., 2009). The second stage of the analysis produced more detailed descriptive, linguistic, and conceptual comments about each individual transcript. An iterative process was conducted at this level of analysis by returning to some of the comments and adding a greater depth of interpretation (Tuffour, 2017). The third stage involved a closer analysis of the exploratory notes in order to begin shaping experiential statements (ETs) reflecting both the experiential and the psychological heart (Smith et al., 2022) of the data in a way that was both descriptive and interpretative. These were subsequently organised into personal experiential themes (PETs) capturing each participant’s experience and lifeworld, as well as the meanings that they conveyed about their experience. Once this process had been completed for each individual transcript, “patterns of similarity” (Smith et al., 2022, p. 100) were noted across all the PETs in order to create group experiential themes (GETs) that related to the whole of the sample. Importantly, while the GETs capture the convergences in participants’ accounts of their experiences, they also fundamentally demonstrate “the unique individual way in which different participants are reflecting that shared quality” (p. 101). This was done by noting whether any one case shed light upon another to create a whole, in line with the hermeneutic circle central to IPA. Finally, the titles of the themes were thoughtfully crafted; the authors worked closely together to ensure that they would resonate with the profound emotions, insights, and transformative journeys shared by the participants.
This study adhered to Yardley’s (2000) framework for ensuring the quality of qualitative research. It first demonstrated sensitivity to the relevant contexts by delving deeply into the existing literature. The authors further established their commitment to the research by thoroughly immersing themselves in the data. The research was rigorous: the analysis was thorough, and the data was interpreted carefully by pointing to their unique complexity. The authors ensured that their research was transparent and coherent by continually reflecting upon the data and making sure that it was presented in a clear and meaningful way and in a language accessible to both psychologists and other healthcare professionals. The research questions were focused, and the authors engaged in discussions with the aim of reaching ‘triangulation’ of the results so as to increase the study’s validity (Patton, 1999). The process of triangulation was also strengthened by offering the reader a variety of detailed quotes that were transcribed verbatim and also by presenting contextual information for the study, the participants, and the passages chosen (Larkin & Thompson, 2012).
Ethics
The study was reviewed and granted ethical approval by the Ethics Committee of the Psychology Department at City University. To minimise the possibility of psychological distress, the study solely recruited adults who had completed their treatment over a year prior to the interview and had no history of severe mental health difficulties. The names and phone numbers of helplines and local counselling services were provided in the event that any of the participants experienced distress after the interview.
Results
The analysis produced four group experiential themes: Open and Enlightened About Food, Becoming a Better Me?, Developing a New Passion for Nutrition, and Becoming Consumed by Food. The themes speak to the experience of developing a new relationship with food after cancer (‘Open and enlightened about food’) and becoming a ‘better’ human being in this process (‘Becoming a better me?’). Instead of seeing illness as a loss, several of the participants reported a positive shift linked to having developed an interest in healthy eating, something which became central to their identity (‘Developing a new passion for nutrition’). However, others experienced their new engagement with healthy eating as a preoccupation that engulfed them (‘Becoming consumed by food’). Each of these group experiential themes will be explored below.
Open and Enlightened About Food
Becoming preoccupied with healthy eating following cancer signified a shift in most of the participants’ personal understanding of food, which reportedly led them to experience a sense of enlightenment and openness.
Through her healthy eating journey, Carla began dispelling some of her previously entrenched beliefs around certain foods, like milk and meat. Indeed, through the process of shifting her diet, she began encountering new information that felt intuitive, and this was confirmed to her by her felt sense of physical wellbeing. While shedding old beliefs was an important step in her journey, experiencing the perceived improvement of her wellbeing on a physical level seems to have strengthened her new practices: I also read up on more raw vegan type of food … And I said this is actually quite amazing what it does to your body. Because we’re not really supposed to eat meat and drink the milk. And yeah have all the animal fats and things like that. And that makes so much sense, you know. And you feel … you feel much, much better. (Carla)
Deborah also pointed out that, prior to becoming preoccupied with healthy food, she had held different beliefs. In this passage, she demonstrated her perception of this important shift by juxtaposing her current self and old unknowing self. She also exhibited a sense of becoming better in that she had risen above what everybody traditionally believes about food: I’m gonna call myself probably plant-based rather than a vegan. And it's been a whole re-education … I thought, like everybody else, that we needed calcium from cow’s milk and protein from meat. We don’t. We don’t. There are various plants that are really high in fibre, really high in protein. (Deborah)
In the excerpt below, Lana nearly went as far as to point to the absurdity of some of the beliefs that are generally held by other people, and this seemed to be a way for her to affirm how superior her way of eating is. She further asserted the perceived efficacy of her lifestyle through concrete and measurable evidence: [P]eople say, “Oh, how can you possibly not eat meat?” … They don’t think that anybody can survive without those things. It’s interesting … So people get, kind of, concerned: “Oh, well how are you going to get enough calcium?” Excuse me!? Cows eat the grass. Cows don’t make the calcium, you know. The calcium is in the grass. Calcium is in green stuff. And in fact, interestingly enough, because I have my bloods done obviously regularly … my calcium levels are very high. So … who needs milk? [laughter]. (Lana)
Another way that participants empowered themselves was by creating a distance from their identity as cancer patients. They did so by transcending their illness and preserving the integrity of their ‘healthy’ self through food.
Lana demonstrated her perceived transcendence by comparing her physical resilience to that of her husband: I just want to do things everybody else does. And I don’t want to be labelled as someone who is … got cancer or is sick or anything like that (…) I used to get lots of allergies from stuff out there in the garden. And I don’t get those anymore and I think it’s because my immune system is, is much … much … is topped up every morning by this juice. So I’m convinced that … I’m convinced that I’m, you know, good to go. And even my husband got COVID in December and I didn’t get it [laughter]. And I was living with him. And I didn’t get it! (Lana)
In much the same way, Deborah juxtaposed her dietary choices with those of her family in order to demonstrate their perceived effectiveness. In this passage, she implied that other people noticed how, contrary to normal expectations, she was able not only to transcend her illness but also to gain more energy, even becoming more energetic than them: My husband eats meat, my kids eat meat, they probably they do eat less meat than they did. Because I don’t buy so much and I cook [laughter]. But it’s their choice. And I’m not going to force that onto them. But they do see me and they certainly don’t see a weak umm …, you know, somebody who’s lacking in energy, lacking in vitality from not eating meat and fish and dairy umm … I’m usually the one that’s up last and up first in the morning umm … (Deborah)
Nevertheless, the process of relearning how to eat and nourish the body in ways that feel protective appeared to involve a degree of resentment towards the old unknowing self. Deborah’s repeated use of I didn’t know, as well as her sigh, conveyed a sense of frustration and regret about not having been aware of what she could have done to prevent her illness. She also seemed to be in a conflict about who to hold responsible – herself or the medical community, which had never told her certain information: I didn’t … I didn’t know that Vitamin D was so powerful in reducing our chance to get breast cancer. I didn’t know that turmeric, you know, curcuma, was really effective at reducing inflammation in our bodies. I didn’t know that as a woman erm, certain minerals and vitamins can reduce our chances of being affected by Alzheimer’s. (…) Nobody had ever told me that, and you know information like that is, yeah … [sighs] why are we not telling people this? (Deborah)
The perceived process of becoming enlightened about food appeared to be gradual and required a slow shift in both beliefs and behaviours. For Beatrice, although becoming vegan complicated the process of cooking, it is this challenge that compelled her to find new alternatives. This openness to new ingredients and methods of cooking came across as exciting. As beliefs were shifting, so did old behaviours: [I] finished treatment in June and then, I think the following January, we started “Veganuary,” but I was reducing up until that point already and I didn’t really eat any meat and just learning to be … become more vegan then exploring all of the other options and stuff and then from January it was properly then … before I was, you know, you cook the same things all the time … and stuff and suddenly, most ingredients that make it a nice flavour aren't available to you anymore, you know. No splash of cream, no bacon fat, no bit of chicken or, you know, you can’t just crack an egg on to make it into a meal. So, you have to be so creative and learn and I really enjoyed that. (Beatrice)
Much in the same way, Alberta referred to the gradual process of shifting to a healthy eating pattern that could also have been accelerated by the sense of urgency she felt to protect herself during a time of great vulnerability. In that way, for Alberta, cancer was a turning point that culminated in her preoccupation with healthy eating: [B]efore that, I was just like everybody, you know. I, I ate, um, well, whatever I like. But then, uh, I looked more into … [F]irst, I, I, I switched to buying as much organic [produce] as I could … Um, and then, you know, over the years, I guess getting more and more conscious about the nutrition and food and everything … And I’ve learnt to like vegetables, which I didn’t like before. So, now, I enjoy that. And, uh, of course, when I had the cancer, I’m, ah, it became more acute to … to eat really well. (Alberta)
Some of the participants also experienced a profound heightened state of individual and collective awareness. Beatrice, for example, described the escalation of her preoccupation not only with healthy eating but with the mechanisms underlying the food industry. In this passage, she seemed to be experiencing guilt when reflecting on her previous lack of awareness around the ethics of her food choices: [O]nce you start looking into it, you tune into this animal rights videos and stuff and slaughterhouse videos and suddenly you think: God, right, you know why I have I not really thought about that? And you think about the environment as well. (Beatrice)
Becoming a Better Me?
All of the participants, with the exception of Esme, experienced a fundamental shift in their perception of their wellbeing. They described becoming better, not only through their newfound sense of enlightenment but through experiencing a profound sense of physical wellbeing.
Deborah opened her narrative around her shift in wellbeing with the word actually, which put forth the possibility that she herself was surprised by how positive the impact of these changes had been. She highlighted an interesting paradox: feeling better through consequences of the illness. Deborah also asserted this staggering change by contrasting her old and new selves. She did so by outlining changes to both her internal experience, the feeling of having more energy, and her external experience, the difference in her body shape. Her use of the metaphor lean powerhouse to describe her body evoked the strength and energy that she believed she gained through these changes: [A]ctually, I feel amazing. I feel better than I did. I’ve got more energy than I did 10 years ago, my skin’s great. I’m not – my body shape has changed. I’ve not, actually I’ve slightly gained a bit of weight, but I think it’s probably muscle rather than fat. But my body shape has changed umm … It’s really interesting umm … kind of my lower half is much more toned than it was before umm … And I don’t think I had a stomach before before but it’s all the sugar and the fat and all of that is gone. I’m much more of a kind of a lean powerhouse, I’m really fit. We just went walking up the mountains a couple of weeks ago and felt great! (Deborah)
In a similar way, Lana insisted on the unquestionably positive impact of her dietary changes, which is perhaps why she experienced regret around not having made this transition sooner. It is as though she believed that she could have prevented her cancer, seemingly implying that she contributed to it in some way. While her tone was bittersweet, cancer for her seemed to represent a great moment of realisation and enlightenment that helped her change for the better: It’s just positive. Absolutely not at all. It’s just positive things that … I feel better now really than I did 10 years ago … But, you know, it’s a shame that, you know, an illness … you know, it switches you on and it makes you smell the coffee. It’s a shame that, you know, better late than ever, but anyway. (Lana)
Similarly, Deborah insisted on the importance of maintaining these changes as she could truly feel their positive impact. Indeed, both Deborah and Tessa achieved validation for their dietary changes through various scans and from their doctors saying that they had positively contributed to their remission, which is possibly why their commitment to staying a ‘better me’ was so strong. In Deborah’s case, her unwavering conviction in the positive effects of her shift to a different dietary approach led her to take the dramatic step of discontinuing her chemotherapy treatment: Did it (chemotherapy) save my life? I don’t … I don’t know what would have happened if I hadn’t had any chemotherapy. I finished it halfway through when I had a clear MRI against the doctor’s advice. (Deborah)
Moreover, by taking on a new, public persona, Deborah may have become more closely bound to her commitment to her nutritional changes. Here, her description of times before and post cancer showed how stark she perceived her own change to have been: I’d seen through cancer umm … I’d seen the effects of cleaning up my diet. And certainly, post cancer. Yeah, I didn’t, I wasn’t going to change … There’s no point me, working on this … this website and promoting healthy eating if I’m not going to do it myself, so and I wouldn’t not do it myself because that’s what I was doing before I got cancer, I’m not going back there. (Deborah)
The participants reported that they felt these changes profoundly. Such was the case for Tessa, who seemed to have fundamentally shifted her perception of her body and her life through cancer and through having become preoccupied with healthy eating. Tessa admitted that she previously had a more superficial relationship with her body, which then shifted through this experience. She alluded to a disjuncture between a ‘disturbed’ inside and a prettified outside that is superficially wrapped in paper: [I]t is my body, life … It is healthy. I see life as beautiful and long and I see life as bright, sunny. Yes, it is the healthy and clean body. I have had many artificial things … It is as if I was wrapping my body with gift-wrapping paper. But the painting is empty. On the inside, I am disturbed. I put a pretty gift-wrapping paper, gold with a ribbon. But no, when you are in harmony with the body, when you accept that this journey … It is a message to carry on living. (Tessa)
For Esme, that her body’s appearance changed as a result of eating healthy foods was a reflection of its capacity to rise above the illness, as if her restored looks validated her healing: Before being diagnosed, I was very swollen in my face and I have a friend who told me afterwards, after umm … she met me again and said “it’s unbelievable, your face just went back to what it was before umm before you got ill” and I think I associated being swollen with being ill. So for me, seeing my face skinny and my body compact, as well, emmm … gave me the feeling that I was doing the right thing, that I was healthy because I was putting healthy things in me. (Esme)
For Kayla, on the other hand, there seemed to be a fear around the fragility of the ‘better me’ and doubts about her capacity to maintain it. In this passage, she also came across as afraid of being swept back into the ‘old me’ again, a version of herself that she did not seem to like. Kayla’s difficulty in maintaining these changes may have stemmed from the difficulty accessing healthy foods that do not feel solely medical: [M]y savings are almost gone. You see things and back to reality, back to being able to get back to work soon … Yeah. So I thought, I don’t want to go back to normal, I don’t want to go back into bad habits and just undo kind of what’s gone on over the last year … the last six months or so. (Kayla)
For some participants, such as Beatrice and Kayla, there seemed to be a conflict between on the one hand wanting to maintain the changes that were perceived to be beneficial and on the other hand yearning for their past freedom. While Kayla laughed at the end of her description, her tone suggested a deep sense of frustration: On a good day I just kind of accept it: I’m here, I’m alive, I’m doing something to hopefully live a long life so … on a bad day then yeah, my inner toddler comes out and it’s not fair and why do I have to eat this mush? Um, yeah, normally it’s somewhere in between that [laughter]. (Kayla)
Developing a New Passion for Nutrition
Some of the participants found that their experience of cancer not only led them on a personal journey of healing through food but also created a new interest and passion that they began to share with others. The process of learning and sharing their knowledge was therapeutic in itself, and it allowed them to cope with their own experiences.
Lana described an almost intense craving for knowledge around nutrition, which translated into her changing career. Her denigration of her past career felt like a way to demonstrate how different her interests had now become, as well as the value she attributed to these new interests. Lana’s laughter intensified the ridiculing of her past interests. In this excerpt, there is a sense that Lana realised how important this newfound passion had been in helping her manage the difficult emotions that arose from cancer. It is perhaps that sense of feeling in control that came through the acquisition of knowledge, and by reassuring herself that she was doing everything in her power to keep herself safe, that allowed her to cope: I’m so thirsty for knowledge about it. I should’ve … I started a PhD myself actually emm at the university of N. But they … in this country they don’t allow you to do a PhD part time … But that’s what I love doing. So I’ve just transferred instead of doing, you know, shitty business stuff which is what I was doing [laughter] I just went down the, you know, the nutrition and fasting and natural remedies and all that, sort of, thing. I just went down that route instead. But I think that’s how I … that’s how I dealt with it actually, I think. When I think about it. (Lana)
Deborah seemed to feel a responsibility to other people to help them avoid her experience of cancer. Her previous suggestion, that she did not have enough information to prevent her own cancer, may have prompted her to share the knowledge she learnt, which thus became a passion in and of itself. Moreover, creating a platform to share her experience may have helped her make peace with her illness, by giving meaning to its occurrence: I think for me, we were talking at the beginning about umm … the project that I’ve started about sharing what I’ve learnt with other people. And for me that is incredibly healing [pause] because it wasn’t for nothing. There was a reason for it. And I’ve been able to share my experience, and … just as a layman really share what I’ve learned with people who either have cancer … have had cancer, or … you know, and prevention has got to be better than cure. (Deborah)
Alberta described this passion as one that required a degree of effort. She spoke of the need to answer questions that were not addressed by medical professionals, which led her to have to take the lead in researching the subject: I studied every single … every single thing to understand, you know, what does that mean? What does that mean? What are the consequences for treatment for a long time now? Side effects, long-term? Uh, or, um, you can do the life expectancy and all that. So … yeah, I, um, I did work a lot. And then I found that other women were asking me because they knew I was doing all this research because the doctors weren’t telling them either, either. And then at first, I starting helping out. (Alberta)
Becoming Consumed by Food
While for some this passion seems to have supported their wellbeing, for others, such as Esme in particular, a heightened preoccupation with healthy food became all-consuming, both of her life and of her sense of self. Although only one participant developed a clinical disorder, they all noted a time of adaptation. Indeed, they initially experienced an all-consuming interest in healthy food, which they slowly needed to adjust.
Deborah described an early period in which she dedicated all her time to thinking about, researching, and preparing foods that she perceived would help her heal. Her commitment was thereafter reinforced by the fact that she was told her efforts had amounted to her being in remission. There is a sense that she felt compelled to continue and not let go: I think initially, it was a big deal. I decided not to eat anything that I shouldn’t eat. So I probably was quite consumed with healing for a period there. And certainly once you know, I was fortunate enough to hear those words, no, no evidence of disease, that then triggers something in you that is kind of I don’t want it back. (Deborah)
This initial period seemed to correlate for most participants with their diagnosis and treatment, which represented a time of great vulnerability. Kayla described a state of being overwhelmed and confused, of fight or flight, in which she found it difficult to think about and decipher what she needed. There is a sense that she felt very much alone and lost in this experience, that it became somewhat consuming and a source of additional anxiety: [I]n hindsight, it would have … would have helped for, you know to have somebody and, you know, you’re, you’re going through so much and your brain is not functioning at its best and things so emmm … that could have helped at the time. Um, just a bit … a bit more advice [around food] and what does and doesn’t help and what’s … what’s harmful and what’s not harmful. (Kayla)
In a similar way, Alberta described the first years as being critical when it came to her relationship with researching nutrition. In this passage, she compared it to an addiction from which she needed to rid herself. Indeed, there was something almost enthralling to her about becoming knowledgeable as it fulfilled her acute need for reassurance, which was constant and overwhelming: I would say, uh, like the, the first two, three years, a lot of time, like almost all my time, I was thinking, uh, about it. And I’m doing so much research. And then, uh, when I stopped, that it was really a slow process stopping. I had to kind of, um, um, disintoxicate [sic] … it becomes like an addiction, I guess. It’s, uh, well, kind of similar. In the beginning, you want to know more. And there’s always more and more and more. (Alberta)
The process of researching various healthy foods was described by Carla as highly engrossing and time-consuming. Indeed, her use of the expression rabbit hole, also used by Deborah in another passage, spoke to its possibly overwhelming nature. Carla pointed out that this process became all the more consuming due to the abundance of information online and the need to be critical of the available resources. It is possible that her disillusionment with the medical community led her to become more sceptical of the information that was available and thus added to the need to cross-reference her sources. Carla seemed to desire to keep a clear mind in order to avoid being manipulated in the way she felt she had previously been: [Y]ou definitely go down the rabbit hole because then you’ll find more information, and you want to look it up, and yeah … yeah … but you have to still keep an open mind and a, yeah, clear mind to not fall into any … uh, yeah, to just leave the option open that maybe what they’re telling you is just the selling thing or … if it is true, so that’s why I also think to read peer reviews or studies, it’s…it’s…it’s quite important as well. (Carla)
The consuming nature of this process became ever more pronounced in the context of a society whose focus was around health and wellbeing. Indeed, Esme referred to the collective focus on health during the COVID-19 pandemic as a factor in increasing her preoccupation with healthy eating. Her listing of the various activities she engaged in around food demonstrated the intensity of this preoccupation and the extent to which she was unable to be present in her life: It used to consume hours … I remember sitting in, in meetings for work and just doing that … just Googling things and preparing things … and … and buying things…and then it didn’t help that COVID happened and … emm … and then there was this focus from everyone on the health … on health … and everything was about that … everything was about exercising at home and … planning meals and … that just tripled the obsession really. (Esme)
Moreover, this all-consuming experience appears to have been isolating for Esme, who created sharp boundaries around her food and conveyed the impression that she may have rebuffed others. Her repetition of the words wanted and everything reinforced the impression of an almost pathological need for control. While she wanted to control her food, it seems that instead she became controlled by it: I wanted to cook everything, everything myself. I wanted to touch everything, I wanted to do everything myself, I didn’t want anyone to … to … to … I wanted to know exactly what was going in there. Umm … yeah. (Esme)
Becoming consumed by food seemed to virtually rob Esme of her identity. She described becoming so consumed by the process of sourcing and eating healthy food that she regressed. Her reference to becoming a child reinforced the idea that, while she desired control over her food as a way to protect herself, she was no longer able to engage with the world as she grew dependent on her food obsession: I feel like I went from being this really independent, vivacious woman to a child and … its … you know, I was obsessed … All I wanted was to find food that felt right, prepare it, buy it, prepare it, consume it and all over again. (Esme)
In this final quote, Esme pointed to the dangerousness of her preoccupation with healthy eating as she became controlled by it. Indeed, she seemed to describe the decline of her interest in other areas of her life, which led her to no longer value the life that she had originally begun this process for. She highlighted the paradox whereby the solution to her desire to live became the problem that would shorten her life: I wanted to live, I wanted to go out, I wanted to see things, I wanted to travel but I had always wanted to live though, I was ready to move to the other end of the world to go on an adventure. I was, you know … I always wanted to live but, but in a way the more I controlled my diet, the more I exercised obsessively, the less I wanted to live ... (Esme)
Discussion
The present study explored how CS perceive and understand themselves as they become preoccupied with their eating habits following a cancer diagnosis. It found that as participants’ approach to eating underwent a fundamental transformation, they felt not only enlightened about nutrition and health but generally ‘better’ as individuals. However, this newfound focus could also engender a sense of being consumed by the process, particularly during the initial stages of this dietary change. This research also sought to understand how CS experience and interpret the change in their lifestyle following a cancer diagnosis. The majority of participants in this study reported a positive transformation in their relationship with food, their physical wellbeing, and their overall sense of health. These results are discussed in greater detail below.
Most participants reported a shift in their personal understanding of food following a cancer diagnosis, which led to an increased preoccupation with healthy eating. This change in perspective was accompanied by a feeling of enlightenment and openness as they began dispelling old beliefs about food. In this way, cancer may be seen as a ‘teachable moment’ (McBride et al., 2008) with deep-reaching consequences: not only was their approach to eating fundamentally altered, their sense of themselves was also affected.
Many of the participants expressed having formed strong personal convictions around nutrition and its contribution to health, and a sense of personal and collective responsibility to adhere to and raise awareness around new principles. This desire to align their actions with their newfound understanding and personal convictions echoes Kucukkaya’s (2010) research, which found that CS tend to develop “an increased self-awareness, acceptance of old and renewed personality, and increased appreciation of personal worth” (Le Boutillier et al., 2019, p. 954) in the later stages following diagnosis. These results are also in line with past research around cancer adaptation. Indeed, Le Boutillier et al. (2019) have highlighted that CS tend to go through a second stage of restoration in which they begin to make sense of their diagnosis by finding meaning in their experience and reasserting their control over their recovery and sense of self; in the third stage, compatibility, they begin developing new meaning around life, a greater self-awareness, and a shift in their priorities (p. 955).
Time and again, the participants’ narratives underscored the significance of agency and choice. When they viewed the pursuit of a healthy lifestyle as a conscious choice and observed themselves taking action in alignment with that choice, a sense of empowerment naturally ensued. The findings thus suggested a newfound confidence in their ability to keep themselves healthy, and their cancer in abeyance, one of them even choosing to discontinue her chemotherapy. Here it is Taylor’s (1983) theory of cognitive adaptation which may resonate, with its focus on the way developing a sense of control over a threatening situation can be adaptive, regardless of whether the cause of that threat is perceived to be within the individual’s control.
The experience of cancer is thought to have long-lasting effects, and as a result, CS may experience profound changes in their views of the world and their own self-concept (Brennan, 2001). Some participants in this study strongly expressed a refusal to go back to their previous selves. Tedeschi and Calhoun’s (2004) theory of post-traumatic growth suggests that following a significant life crisis, individuals may experience ongoing and positive changes in their relationships, enjoyment of life, and perception of their own strength. The majority of participants in the present study appear to have experienced a degree of post-traumatic growth in that they reported a positive shift in their relationship with food, their bodies, and their sense of wellbeing. Indeed, Rasmussen and Elverdam (2007) propose that a diagnosis of illness can be viewed as an ‘epiphany’, or a transformative moment that alters an individual’s life goals, self-concept, and worldview, leading to a new understanding of life (Goud, 1995).
All of the participants in this study, with the exception of Esme, reported experiencing a significant shift in their perception of their own wellbeing. Not only did food allow them to reconnect with their bodies but reconnecting with their bodies also allowed their bodies to guide their food choices. These results echo the findings of a phenomenological study on the experience of individuals living with multiple sclerosis, which revealed that, despite being ill, people may still have a good rapport with their physical self. They argued that ‘the self is no longer (unconsciously) acting upon the body but is taking care of the body’ (van der Meide et al., 2018). One way to comprehend this is through the body affect, which denotes a person’s emotional approach towards their own body. The participants in van der Meide et al.’s (2018) study demonstrated an emotional attitude towards their body that can be described as one of care and dedication to maintaining their health through activities such as exercising and by paying closer attention to their diet. Here also, a phenomenological approach can generate valuable insights: if our body serves as the foundational point of connection to both ourselves and the world (Merleau-Ponty, 1945), then through practices involving our physicality, such as modifying our dietary choices, we actively influence our relationship with ourselves and the world around us. Several participants spoke of the way they had previously been disconnected from their physical needs and self. The encounter with cancer forced upon them a heightened bodily awareness and helped them rediscover their own needs. The modification of their dietary behaviours might therefore be seen as a deliberate endeavour by CS to effectively manage or alleviate their physical and emotional vulnerability, while fostering a re-embodiment that allowed them to re-establish a deeper relationship with themselves and with others.
For some participants, such as Lana, Deborah, and Alberta, an increased focus on healthy eating became a passion, and their dedication to spreading awareness about the positive effects of diet on cancer and overall physical wellbeing became a new identity. Previous research has shown that CS who are able to successfully adapt to a new identity may develop a stronger sense of self and embrace new values and ideals (Mages et al., 1981). The literature has also found that the ability to share experiences and to offer one another ‘peer support’ are common coping mechanisms for CS (Le Boutillier et al., 2019). For the participants in the present study, making meaning out of their cancer experience by supporting others through their passion for food and for the environment helped them find meaning and fulfilment in the face of adversity.
However, findings revealed that while some participants experienced positive outcomes, others experienced negative consequences. Kayla appeared to be fearful of the fragility of her improved self and unsure if she would be able to maintain it. Her struggle to maintain changes viewed as positive may have been due to her isolation, and to the tension between wanting to maintain the perceived benefits of her new diet and longing for her past freedom. This seemed to leave her in an uncomfortable state of dissonance.
Further, although Esme was the only participant in this sample to have been diagnosed with a clinical eating disorder (eating disorder otherwise not specified; EDNOS) following her experience of cancer, other participants echoed some of the same difficulties. Many participants described an initial period following diagnosis during which they had become ‘consumed’ by finding and preparing foods that they believed would support their healing and prevent the recurrence of cancer. This initial period was characterised as a time of vulnerability, pervaded by a sense of loneliness and confusion. It may have been exacerbated by the lack of formal guidance on how to adjust one’s diet following a cancer diagnosis, and by the abundance of conflicting and potentially misleading information online, thought to create a higher risk of engaging in inappropriate eating behaviours (Swire-Thompson & Lazer, 2020). In fact, research has shown that the guidelines offered by primary sources of information, such as Macmillan Cancer Support (2022), are often general and replicate common recommendations for healthy eating (e.g. reducing the consumption of sugar, fat, and red meat, and increasing the consumption of fruit, vegetables, and fibre). Between 30% and 60% of CS therefore feel they lack the necessary knowledge about nutrition and cancer to manage their condition (Kassianos et al., 2015). Moreover, only 63% of CS discuss their use of alternative treatments to their physicians (Bernardi et al., 2003). Between 25% and 90% of cancer patients therefore seek to bridge this gap by engaging in their own search for evidence-based information (Nagler et al., 2010; Zebrack, 2000) but report that they are often confronted with an overwhelming amount of contradictory information. This may lead them to engage in maladaptive eating practices, which can be an antecedent for the development of an eating disorder (Nucci et al., 2022) and highlights the need for improved communication and collaboration between patients and their healthcare providers when it comes to the use of alternative therapies.
Moreover, this preoccupation was compared to an ‘addiction’ by some of the participants, one which they needed to ‘disintoxicate [sic]’ from. Past literature has shown that although orthorexia nervosa is not currently considered an eating disorder, a heightened preoccupation with healthy eating that has an impact on the person’s daily living may be described as a ‘pathological’ shift in behaviour (Chaki et al., 2013). Thus, orthorexia may be considered an obsession with ‘extreme dietary purity’ (Cena et al., 2019), “associated with anxiety to improve health and prevent diseases by means of a proper diet” (Nucci et al., 2022, p. 11). Esme specifically described how her life became centred around managing her diet in a way that appeared pathological and hindered her ability to fully participate in her life. She also reported a decline in interest in other areas of her life that had previously been important to her.
Strengths and Limitations
This research is distinctive in its contribution to the existing body of work, as it sheds light on the somewhat confusing journey of CS who develop a heightened preoccupation with food following their diagnosis. Some of the participants described this heightened focus on food as a beneficial coping strategy amidst the unpredictability of illness and themselves as having grown from the experience. Simultaneously, they spoke of dietary concerns introducing an additional layer of complexity to their overall self-management. Even those fully dedicated to these dietary adjustments initially found the process consuming and needed to establish a balance to prevent becoming overwhelmed.
While having a small and homogeneous sample is a requirement of IPA (Smith & Osborn, 2008), participants’ similarities in terms of gender, age, education, ethnicity, and socio-economic status, as well as the overrepresentation of breast cancer among participants (five out of eight), necessarily limit the transferability of these findings to other populations of CS. Future research drawing on larger, more diverse samples (e.g. by using surveys) is therefore needed. Additionally, a larger study might be able to shed light on the likelihood of some CS but not others developing an eating disorder, thus exploring the potential link between cancer and the onset of eating disorder symptoms.
Finally, while the evidence suggests that lifestyle changes in eating can empower participants during their recovery, this study also reveals that some individuals face substantial challenges. It raises questions about the factors contributing to thriving versus experiencing difficulties when making dietary changes as a CS. The current study primarily focused on participants’ personal accounts of the shifts they went through, and on their perceptions of these changes, but it offers limited insight into the specific contextual conditions that facilitated or hindered these adaptations. These gaps in knowledge represent a few of the avenues for exploration that future researchers could consider.
Clinical Implications
Although this study does not attempt to make universal claims, it provides some insight into the potential risks associated with a heightened preoccupation with healthy eating and identifies areas where support may be needed. This may inform the development of therapeutic interventions or approaches tailored to the unique needs and experiences of CS. Healthcare professionals may need to be attentive to the possibility that some CS appear to be coping well when they are in fact using their diet in ways that may be maladaptive. Therapists may wish to explore how food is used by CS and address any underlying fear of recurrence or anxiety, which may have a negative impact on the person’s quality of life (Johns et al., 2020). Furthermore, those providing support to clients who have both an eating disorder and a life-threatening illness may want to consider the possibility that their eating difficulties are a way of coping with the illness. It may be helpful to investigate this link and incorporate it into their formulation of care.
Moreover, psychoeducation groups could be an effective way to provide CS with information about the role of diet and nutrition in cancer recovery, as well as the opportunity to discuss their concerns and challenges with others with similar experiences. These groups could be facilitated by healthcare professionals, such as registered dietitians or psychologists. Studies have found that psychoeducation groups might offer CS a heightened sense of empowerment regarding their illness and reduce their feelings of despair (Sautier et al., 2014). Thus, by providing CS with access to accurate and reliable information about diet and nutrition, it may be possible to improve their health outcomes, their sense of agency, and overall quality of life, while also mitigating the risks posed by contradictory information.
While food can act as a coping mechanism during significant life changes, and may contribute to a new, transformative relationship with one’s physical and emotional self, it may also develop into a new source of anxiety and guilt. It is therefore important that conversations around food are not overlooked by healthcare professionals, as the timely addressing of any potential concerns could enhance the overall quality of life of CS, while ensuring that no foods are unnecessarily restricted to the detriment of their health.
Conclusion
The present research has provided an in-depth exploration of the experiences of CS who developed a heightened preoccupation with healthy eating. All the participants identified that their preoccupation with food was all-consuming, particularly after diagnosis. While some of the participants in the study perceived that they were able to gradually shift away from their all-consuming preoccupation with food, others found that it grew stronger. In fact, one participant was diagnosed with a clinical eating disorder that required outpatient treatment. This study may offer valuable insights to both counselling and oncology services from the perspective of service users and help healthcare professionals understand the needs and behaviours of individuals who have experienced cancer and how to best support them. Moreover, the study emphasises the potential for disordered eating among CS and suggests that healthcare providers should offer appropriate dietary guidance and support to ensure that patients can play an active role in their recovery without compromising their adherence to conventional treatments and their overall wellbeing. Future research could build upon the findings of this study by conducting both qualitative and quantitative investigations into the prevalence of maladaptive eating behaviours and the anxiety they produce among CS. To make these findings more generalisable, it would be beneficial to conduct studies with larger and more diverse samples.
Footnotes
Author Contributions
Both authors confirm contribution to the paper as follows: study conception and design, data collection, analysis and interpretation of results, and draft manuscript preparation. All authors reviewed the results and approved the final version of the manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical Statement
Informed Consent
Informed consent was obtained from all participants through the signing of consent forms that were emailed by the first author a minimum of a week prior to the interview taking place.
