Abstract
Objective.
Although
Methodology.
Our project is a
Results.
The
Conclusions.
Background and Rationale
Simulation includes any process or technology that recreates a contextual background allowing the learner to make decisions, experience success, make mistakes, receive feedback, and gain confidence in an environment that is void of patient risk. Simulation can enhance medical and surgical education by replicating clinical scenarios in an immersive and experiential environment. Research has demonstrated that simulation is superior to conventional educational delivery and a powerful learning tool to achieve higher levels of competence and safer patient care, however time and distance constraints are often the main barriers . Although simulation-based medical education is an invaluable tool in the acquisition and maintenance of knowledge and skills; simulators are often located in urban centers and they are not easily accessible outside these centers due to geographic, cost and time constraints. Unfortunately lack of clinical simulation training is more evident in rural areas with limited teresources that do not have access to costly simulation laboratories, supplies, or trained instructors (Qayumi, 2014).
Telesimulation allows for the education, training, and/or assessment of learners at an off-site location. This simulation delivery method eliminates distance and time barriers to educational content delivery while simultaneously conferring the benefits of simulation beyond the walls of simulation centers (Conde et al., 2010).
Telehealth applications and simulation are increasingly important in many areas of health education and training. They play a vital role in facilitating remote collaborations and providing access to expensive or remote equipment. Telesimulation provides critical value to healthcare educators and learners locally within an institution and globally through collaborations between academic institutions. Training sessions can be conducted at an off-site location, and at time and location convenient for both instructors and trainees. This makes simulation training more feasible within an institution, allows for inter-institutional networking, and more importantly offers a novel educational opportunity to developing or resource limited countries (Conde et al., 2010).
Telesimulation is an innovative educational delivery method with a great academic potential when effectively utilized with advanced technology. Currently, most of the telesimulation tools are held through 2D web conferencing with aid of webcams and screen sharing software. Because telesimulation is a new niche within simulation, creative inventions using advanced digital technology can offer promising solutions for clinical training and education.
Problem
Resources of current traditional means of medical simulation include costly equipment, space, time, faculty, and academic curricula. Those are major challenges and barriers that complicate students’ access to simulation-based clinical training and its implementation within medical education, particularly in rural and resource limited-areas.
Project Goal
Our goal is to transform traditional medical simulation training into a virtual experience to facilitate access through the creative integration of advanced digital technology and telesimulation. Using virtual telesimulation and advanced immersive technology, students located outside urban centers or in resource-limited regions will be granted the ability to access this enhanced form of clinical training.
The utilization of virtual reality (VR) based clinical simulation would allow students the opportunity to: Practice their clinical skills in a risk-free environment. Improve their decision making in life-like scenario Access high quality training at their convenient time, and place. Benefit from academically trained and certified instructors globally.
Materials and Methods
The project proposal was reviewed and approved by faculty committees at McMaster University and Centre for Digital Media in Canada. The product is a result of a collaborative work between the two institutions.
Project Objective
Our objective is to develop a proof-of-concept prototype using virtual reality technology for clinical telesimulation training and global medical education. The project involves the development of an immersive VR environment for trainees and a remote interactive control panel for instructors to control and guide VR clinical sessions in real-time. Through digital telesimulation, access to clinical training is facilitated by overcoming constraints of distance, time, personnel, and equipment.
Project Development
This project entails development of two main components. Student’s VR system for clinical simulation training using Oculus Quest VR headset. Instructor Control Panel (ICP) which is a computer-based application for instructors to control the VR-sessions remotely, in real-time.
Hardware – Oculus Quest
Target Users and Audience
Virtual clinical simulation (VCS) system is aimed at: Medical trainees including under and/or post-graduate students in developing countries and resource-limited rural areas. Faculty members and instructors who would facilitate clinical training sessions.
The user experience and interface for both trainees and instructors were designed to replicate simulation sessions that would be carried out in a traditional simulation center. VCS has taken that simulation experience to the virtual world demonstrating actions, features and functions that are possible to realize in a virtual simulator.
Design Key Features
The main design features unique to this project are Tele-presence Real-time interaction Portability: Oculus Quest is all-in-one VR system. The wireless headset and controllers provide a compact setup, don't require a PC (personal computer), and the 64GB of storage accommodate compatible VR applications. High-fidelity Digitalization User Friendly Multiplayer: compatibility with multiple users for group learning would reduce the amount of time an instructor would have to put into a single trainee training and provide an opportunity for group interaction and learning – similar to real life clinical practice and simulation where training is often carried out in a group. Debriefing: sessions can be video-taped and played back to trainees for feedback.
UX Design (User Experience)
We analyzed the normal steps that the users (instructors and learners) would take to participate in clinical simulation training and created a user journey map (Figure 1). According to the journey map, we decided to focus on designing the essential elements of training session, implementing them in a VR environment and allowing instructors to control the session through PC-based application (Instructor Control Panel). The journey map for simulation session includes briefing, clinical scenario, and debriefing. Furthermore, we outlined the user experience for both students and instructors in algorithmic user flow diagram for better implementation. The user experience included the necessary steps students and instructors would have to do in order to complete the simulation session (Figure 2).
VCS journey map for students and instructors.
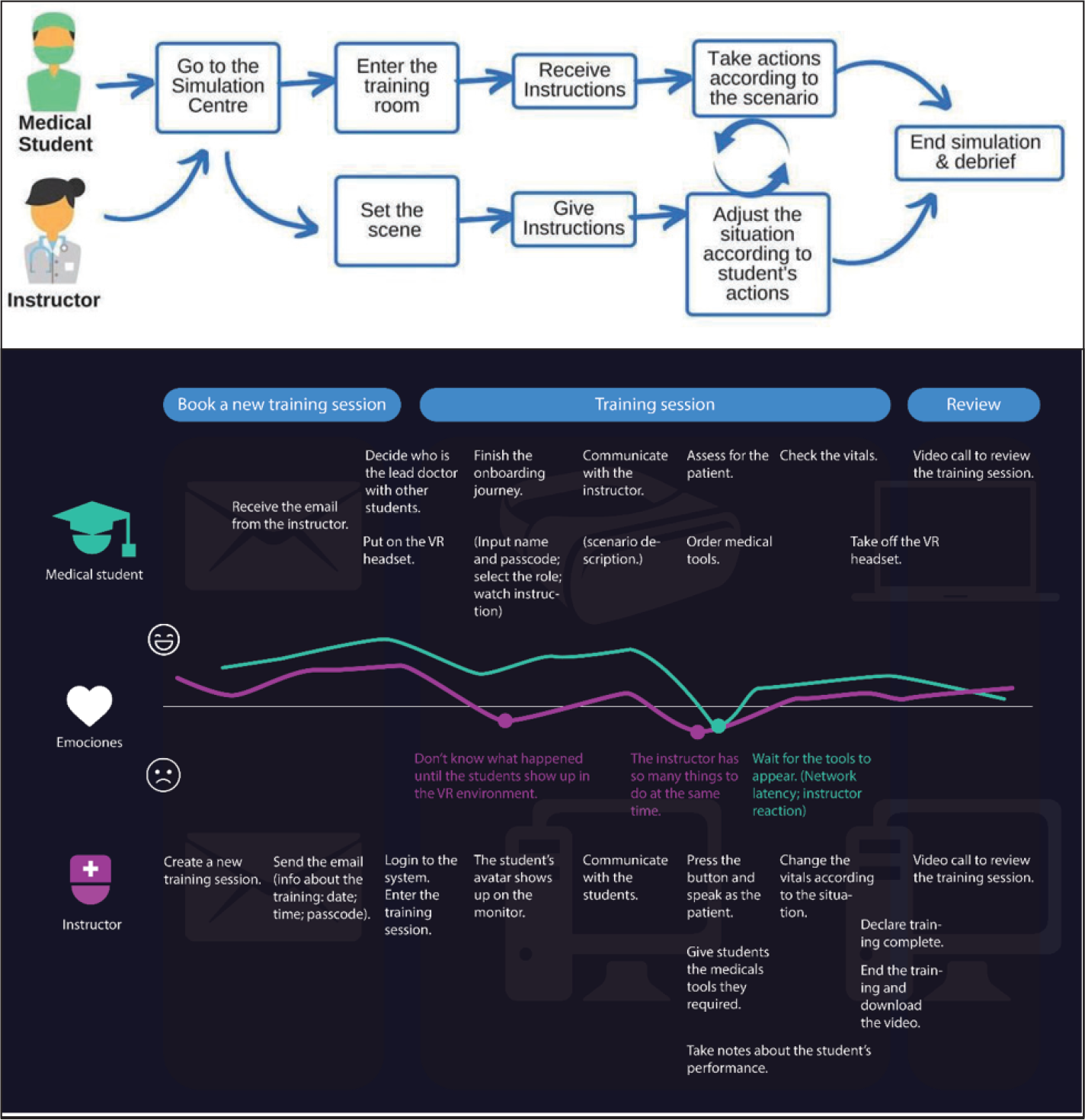
VCS user experience flow diagram for students and instructors.
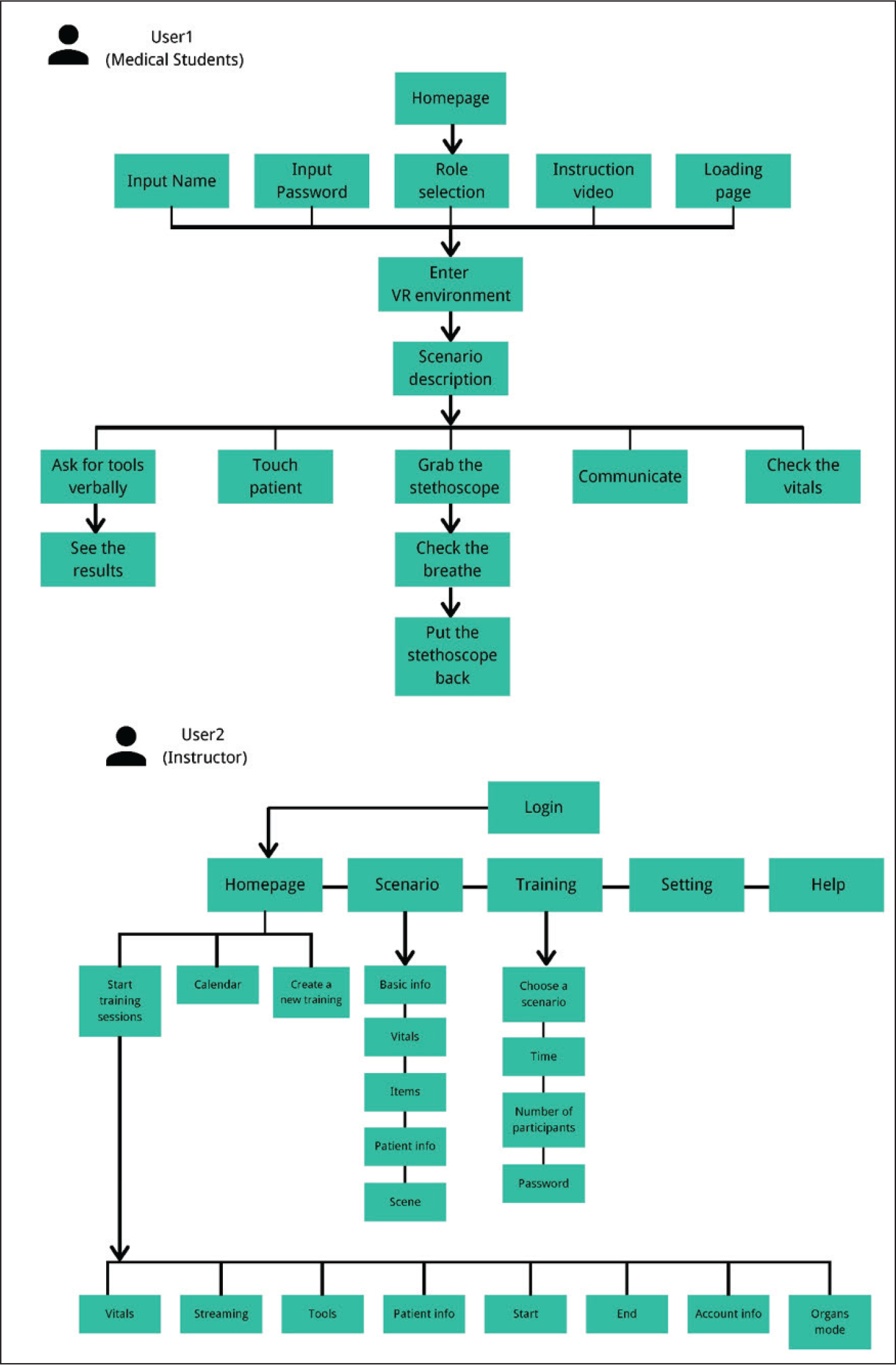
UI Design (User Interface)
After we determined the design content, we started to design the wireframe. We separated them into two parts: instructor’s control panel for instructors, and VR interface for trainees. The goal is to have a simple and clear wireframe that is user friendly and easy to navigate.
Software and 3D Modeling
Software and applications: Autodesk Maya –Version 2019 MGear Auto Rig System (Rigging Plugin for Maya) - Version 2019 NgSkinTools (Weight painting Plugin for Maya) – Version 1.8.2 Autodesk 3D Max Studio –Version 2019 Unity3D –Version 2019.2.19f1 Oculus App Version 15.0.0.200.456 (15.0.0.200.456) Oculus mobile application
Results
User Tests
User tests; objectives, results, and iterations.
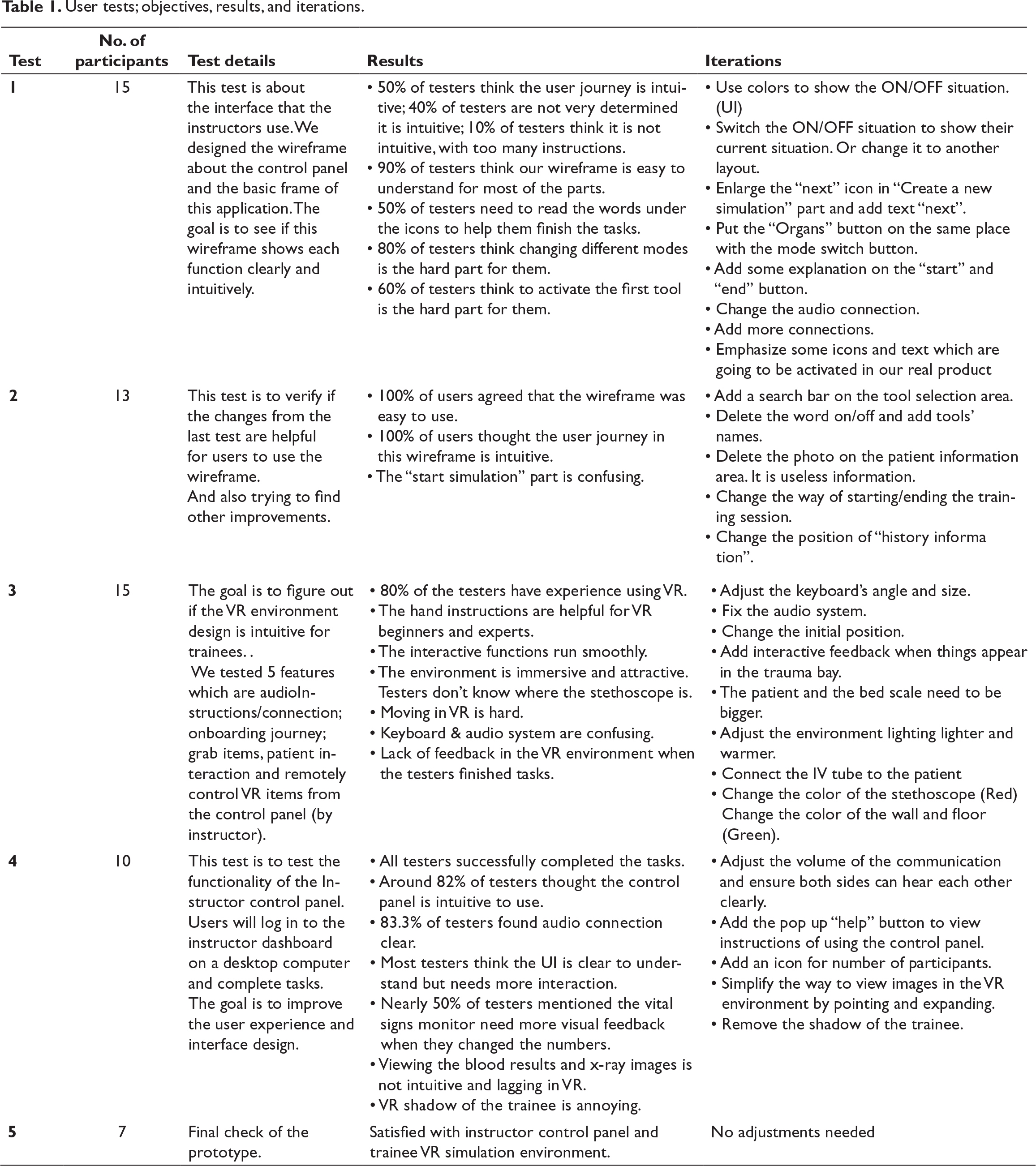
Instructor Control Panel (ICP) – Remote Digital Application
ICP is a computer (desktop or PC) application developed to achieve the following key elements:
Tele-simulaion
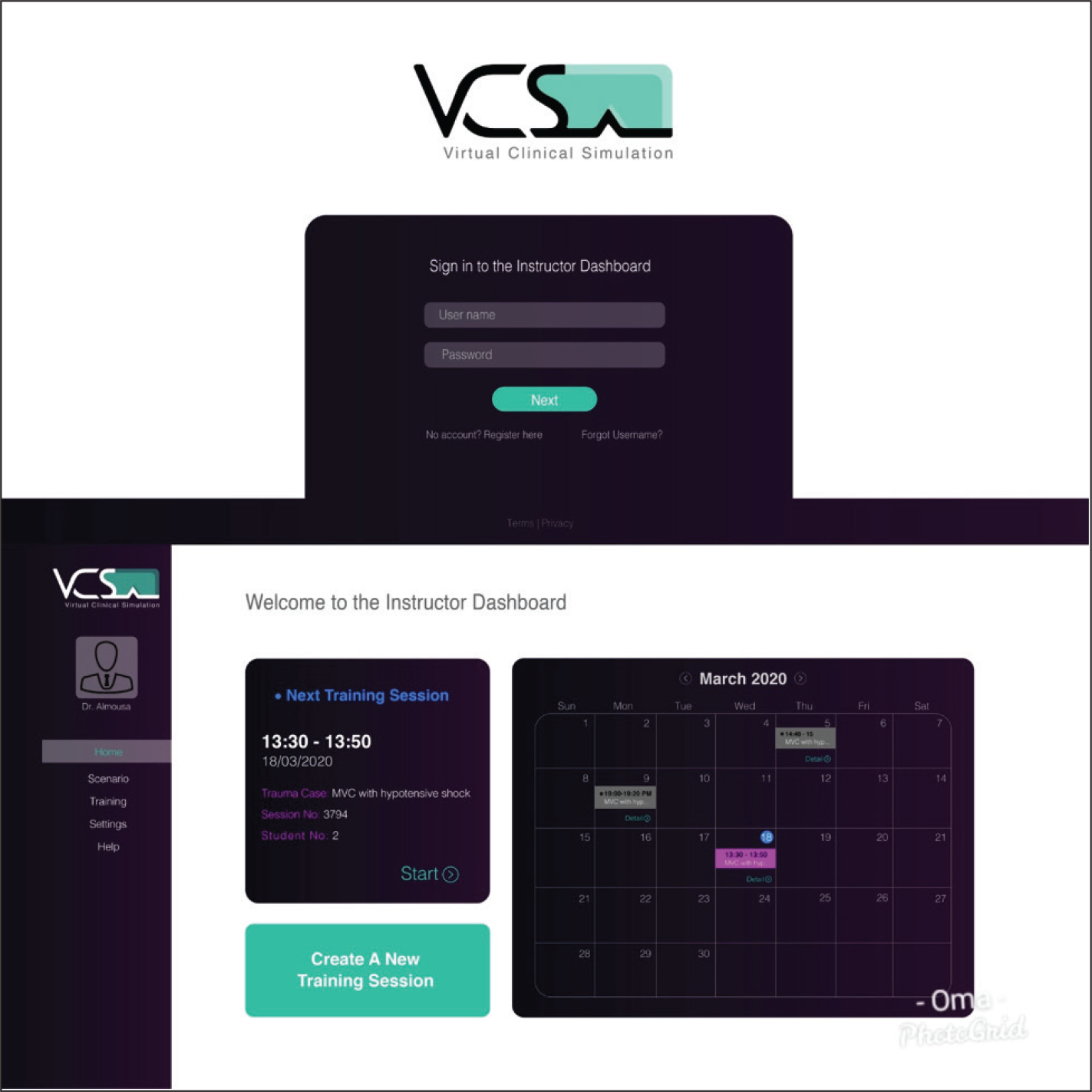
The instructor control panel designed to act as a remote system to provide intructors with full control of the VR training session through a PC-based application. Intructors can login into their personlized accounts which allow them to create, design, moderate, and run clinical training sessions (Figures 3 and 4).
VCS instructor application for remote live streaming and real-time control of VR-clinical sessions.
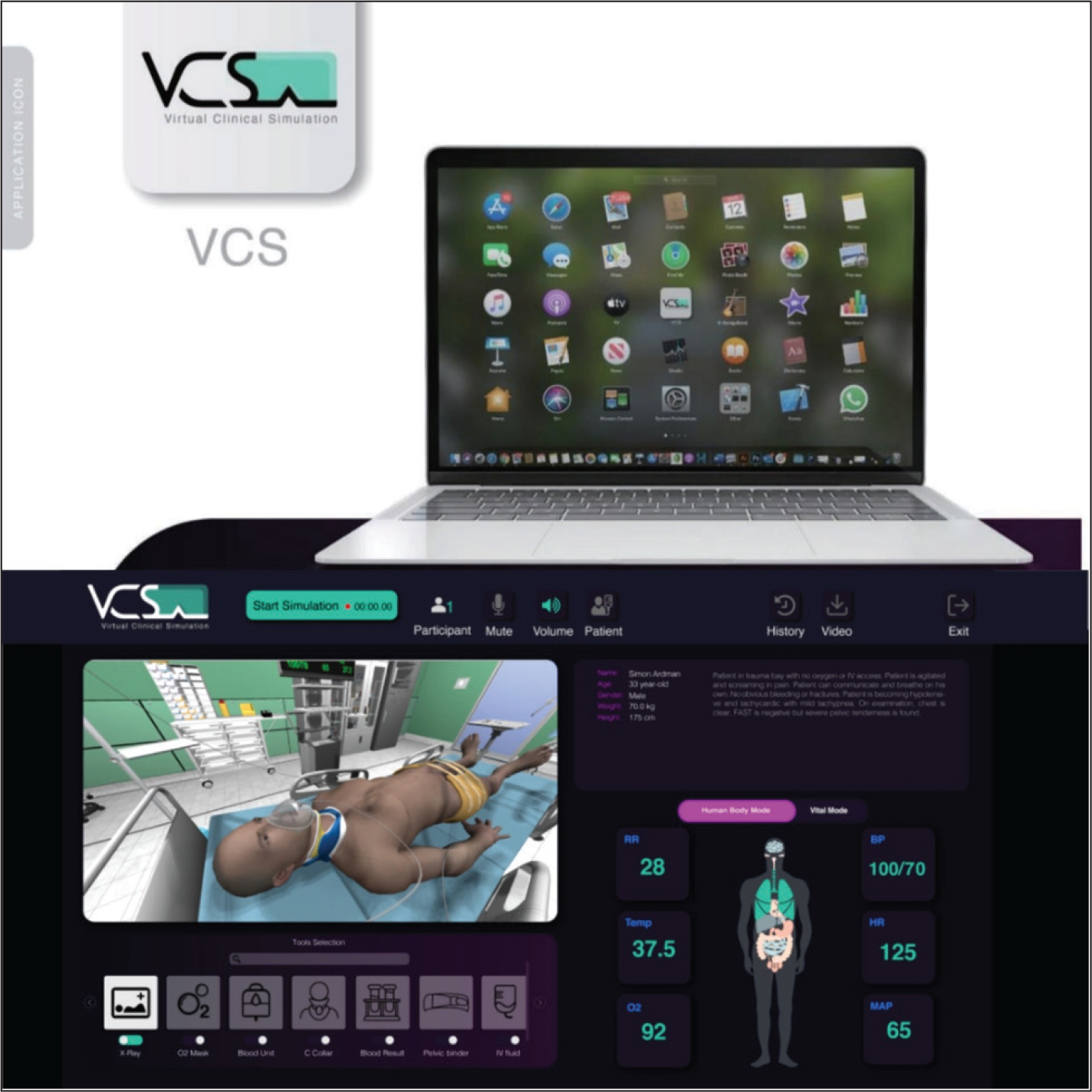
Real-time
Instructors are able to manupulate the progression of VR clinical scenarios and interact with students in real-ime during training sessions. The estalished live connection between the instructor conrtol panel and VR-training system enables dynamic and engaging learning experience.
VCS Instructor application interface, profile, and dashboard.
Interactive features
Few interactive features have been programed in the protoype. Audio and verbal connection allows interactive communication between students and instructors. Clinical scenario specific features such as patient’s vital signs and exams’ findings (e.g. breathing/heart sounds) can be controlled and changed by intructors according to the scenario. Case-specific tools and interventions such as blood tests, radiology imaging, IV fluid, blood transfusion, oxygen masks and others have been designed and programmed to show up in VR enviroment, when activated by the intructor through the control panel.
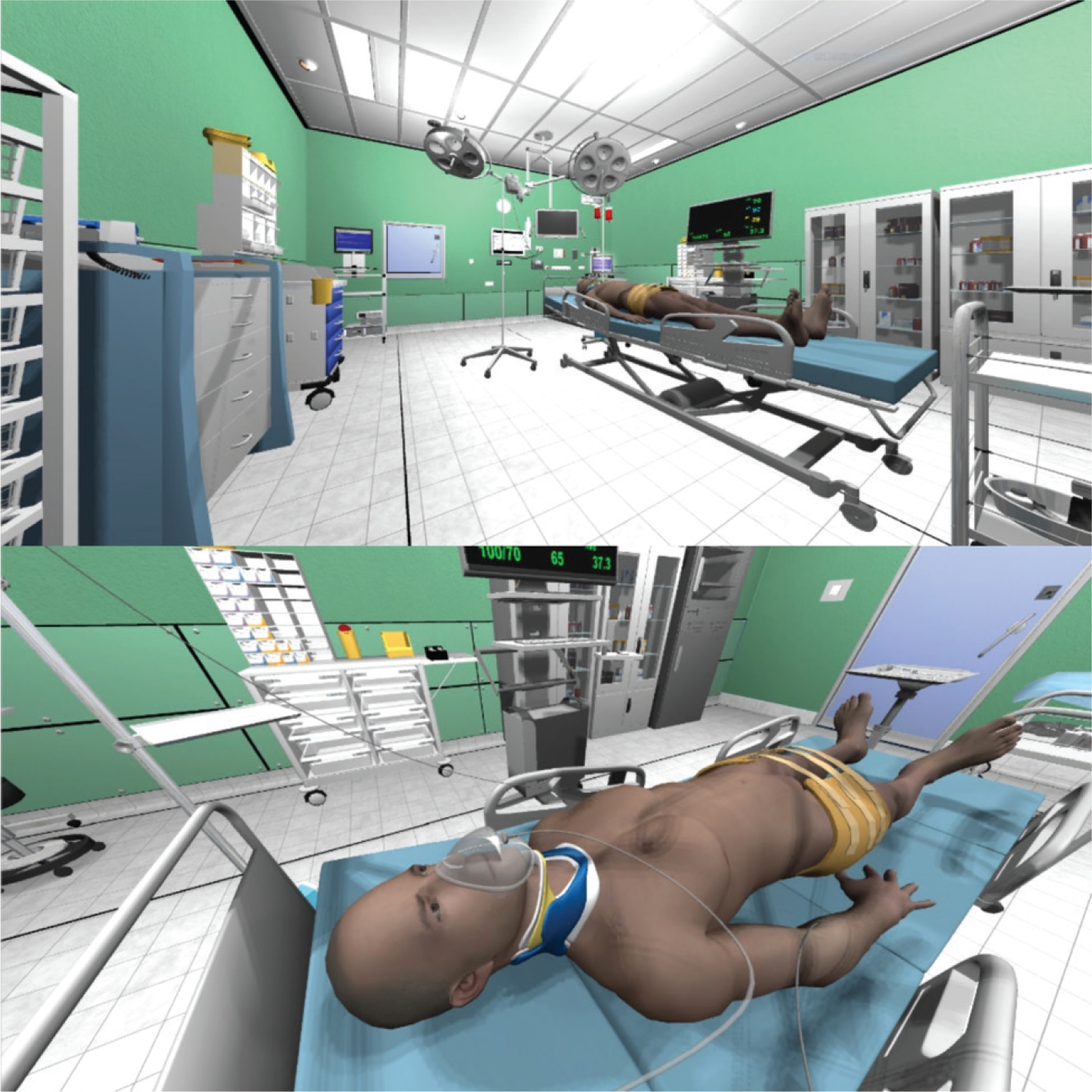
VCS virtual clinical simulation session (trauma bay).
Live streaming
Instructors can live stream the student VR session in their control panel, which is also equiped with multi-angle and zoom control for maxium viewing.
Debriefing
Instructors can choose recording time and period by simply clicking on record button in the control panel for academic feedack.
Schedule and Library
Instructors are provided with a calendar to book their sessions in advance and library to save and store those sessions for teaching purposes.
Student VR-Training System
Using Oculus Quest headset, VR clinical simulation sessions are programmed to deliver the following:
Onboarding
For VR naive users, this step was designed to guide students on basic functions of VR controllers (e.g. select, grasp, release, exist) and test their physical motion in VR space.
Realism and emersion
Once the clinical session is started, students find themselves fully immersed in a realistic trauma bay that has a lifelike looking patient (blinking, talking, and breathing), tools and equipment (Figure 5). They can freely walk around the room and interact with the environment (VR trauma bay), patient and equipment. The VR controllers appear as student’s/user’s hands in VR space, thus adding more realism to the experience.
Engagement
Students can interact with the patient by taking history and performing examination like auscultating for heart and breathing sounds. They can also grab objects in VR trauma bay and use them for their clinical scenario (e.g. stethoscope). Students can hear and communicate with their instructors in real-time, which allow them to ask for interventions and decide on management options like fluid replacement or blood transfusion. Just like in real life, students can ask for clinical investigations like blood tests or imaging and review them in VR.
VCS project video was created to summarize vision, results, and future directions. [Video 1].
Discussion
Role of Simulation in Healthcare and Medical Education
A major challenge in medical education is the application of theoretical knowledge to clinical setting and management of patients. The acquisition of appropriate clinical skills is key to medical and surgical education, therefore an adjustment in the instructional teaching methods have resulted in innovative medical curricula. The new curricula (e.g., competency-based training) stress the importance of proficiency in several clinical skills. Studies have shown that simulation is a superior educational modality in comparison to passive teaching methods. Simulation-based medical training, when integrated appropriately into learning and competence testing, plays an important role in acquiring critical clinical skills and reflective decision making needed to provide safe patient care (Al-Elq, 2010; Honda, 2020).
Value of VR and Advanced Digital Technologies in Simulation and Medical Education
Unlike traditional means of simulation, VR has a unique power, more than any other technology that has ever existed, to make users believe they are in a completely different environment. This allows leaners to feel experiences and learn as if they would do in real-life. This ability to deliver educational experiences on demand is where the real value of VR lies. VR has the power to enable an immersive, realistic, interactive, adaptive, and dynamic learning environment which is critical for medical education . VR simulation has the potential to reduce time and cost of clinical training, as well as improve and audit quality. VR-simulation has relevance and applicability in both resource-limited and high-income settings (Parham, 2019).
VCS offers realistic clinical scenarios in virtual space that mimics hospital environments such as patients’ wards, trauma bays and clinics. The immersive nature of VCS with high-fidelity lifelike characters designed to deliver interactive learning experience, similar to real-life. The emotional engagement and gamification of VR provides enjoyable learning and encourages active training . VCS scenarios are customizable and repeatable to suit the desired need for clinical training and enables practice and repetition which are keys for knowledge retention and better performance. This is particularly crucial when it comes to rare and critical clinical conditions that mandate prompt recognition and efficient management. The flexibility of access that VCS offers allows active integration of simulation-based training into medical education curricula. On the other hand, access to current simulation centers is restricted by space availability, time and faculty. Simulation centers are costly and require large budgets to build and maintain over time which limit their overall spread and access. VCS delivers simulation sessions at a lower cost and with much fewer resources. VCS simulation system is simple to set up, works in small places (2 X 2 meter), and designed for ease and safety of use. Learners can take part in simulation at their convenient time and place which allows for much broader and flexible access (Figure 6).
VCS system offers a creative telesimulation training platform through an integration of instructor control panel that enables faculty to moderate clinical sessions in real-time for optimal learning and performance. Debriefing has proved to be an essential component of simulation-based learning for clinical performance competency, self-reflection, and satisfaction . VCS software is capable of recording those simulation sessions for academic review and constructive tele-debriefing that follows each clinical scenario to consolidate knowledge and skills.
Value of VR Simulation System in Resource Limited Regions
Unfortunately, health care simulation requires substantial human, logistical, and financial investments that preclude their spread in developing countries and resource limited areas. Lack of simulation centers and necessary resources in rural areas make the potential of VR-based simulation tools like VCS even more valuable. Cost, infrastructure, expert faculty, and curriculum are major challenges limiting access to medical simulation training in those regions. The latest generation of VR systems (e.g., Oculus Quest) are more affordable, portable, and fully integrated stand-alone headsets that do not require any additional computers or training (Wang et al., 2017). VCS connects academic experts from around the world to deliver quality training to medical trainees located in remote regions. VR based simulation is not a preference, but rather the clear evolution of medical education that would provide solutions to resource-limited areas through tele-educational platforms. Digitalization of medical simulation is an innovative approach to clinical training and a vital alternative to costly simulation centers and expensive equipment settings . The current VR headsets in the market cost between USD $300-800 and are becoming more affordable as technology evolves. VCS is an application compatible with any VR headset/PC. Moreover, VCS real-time mentoring feature through Instructor control panel and debriefing facilitates access to expert faculties, curricula, and necessary resources globally.
VCS session using Oculus Quest.

Value of VR Simulation System in Developed Countries and Resource Rich Areas
Undergraduate and postgraduate medical education is constantly evolving to ensure quality training and clinical skills acquisition. Competency-based medical education (CBME) has recently emerged as the new educational approach to demonstrate effective learning and safe clinical practice. VR offers educators and leaners a cost effective, accessible, and standardized clinical training on-demand, if implemented properly . VCS allows clinicians to teach, assess, evaluate, and provide feedback to medical trainees in an interactive and lifelike clinical setting at their convenient time and location. VR-based simulation platforms like VCS will transform how we view and deliver education in future to more clinically relevant, problem-based, and practical teaching. This will also facilitate quality inter-professional and inter-institutional education and collaboration, independent of geography (Pottle, 2019).
Limitations
This is a proof-of-concept project and further research studies comparing VR-based simulation using VCS or similar platforms to traditional means of simulation are needed. Haptics (the sense of touch in VR) is still under experimentation which limits the nature of clinical scenarios that could be taught at this stage to non-technical scenarios that aims to improve clinical decision making and leadership skills. Just like any VR application, motion sickness can be problematic for some susceptible individuals which can be hard to predict or quantify. VR novice players and women are found more susceptible to virtual reality sickness. Gender susceptibility may be due to hormonal differences, or it may be because women have a wider field of view than men. Also, kids between the age of 2-12 and adults over the age of 50 are more susceptible. Those who are more sensitive to motion sickness are also more sensitive to virtual reality sickness, especially with games and applications that involve racing and flying. Several techniques have been described to minimize VR-motion sickness such as postural stability or sitting, lowering headset brightness, proper headset-fit, adequate lenses-focus, breathing exercise, and starting slowly while gradually increase time spent in VR (Thompson, 2020) Wi-Fi connection and internet access could be a challenge in some rural and resource limited areas. In pandemic situations, proper sanitization measures such as using alcohol-based disinfectants or using wipeable covers need to be undertaken. Local protocols and center-specific guidelines can vary and therefore should be referred to for users’ safety.
Future Directions
Multiplayer
Multiple trainees can access the same virtual environment simultaneously with a unique access code. Users can collaborate and communicate with one another and do not need to be in the same location to enable multiplayer mode. Students could see each other’s avatars and names in the virtual environment (this function has been programmed in our prototype but needs testing).
Realistic Avatars
Students can have a realistic avatar when they are enrolled in VR training, which can bring them further sense of immersion and engagement.
Mobile-Phone Friendly
The instructor dashboard (control panel) could be programmed to accommodate Android and Apple smartphones. Sessions could be controlled from the instructor’s mobile device in addition to a PC.
Language Subtitles and Translation
Since VCS is made for global academic access, we are planning to include the use of subtitles to accommodate non-English speakers. Scenarios’ descriptions and patients’ phrases could also be translated in real-time.
Conclusions
We believe that our Virtual Clinical Simulation (VCS) system addresses concerns and limitations regarding current means of medical education and simulation training. It provides innovative solutions to major challenges associated with conventional simulation training such as access, cost, personnel, and curriculum. VCS facilitates the delivery of academic and interactive clinical training that is similar to real-life settings. The telesimulation feature combined with the real-time streaming and session control liberate faculty and students from time/place constraints. The realism and immersive nature of VCS are key elements for mental engagement and skills retention. Supervision and mentorship guidance by expert faculty throughout VR simulation sessions, along with constructive debriefing promote educational growth in clinical performance and cognitive skills (e.g., communication skills). Nevertheless, international virtual collaborations between faculties and institutions are essential advancements in healthcare and medical education providing much broader access in developed countries and critical need in resource limited regions. Tele-clinical simulation systems like VCS facilitate necessary academic-community partnerships, as well as global education network between resource-rich and low-income countries.
Footnotes
Declaration of Conflicting Interests
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Supplemental material
Author Biographies
Contact:
Contact:
Contact:
