Abstract
A cross-jurisdictional pan-Canadian environmental scan was conducted to identify provincial, territorial, and federal financial supports available to families with children living with neurodisabilities. In partnership with the organization Childhood Disability LINK, flowchart-styled pathway documents were developed for each financial support identified, mapping out the processes required to access each support. A critical analysis was completed as it relates to structural barriers, accessibility of program information, and geographic discrepancies. The results revealed that, despite almost universal availability of programs to support families of children living with neurodisabilities, significant barriers and inequity remain. This included considerable variation in access to financial support based on geographic and jurisdictional discrepancies, absence of adequate and accurate information about programs, and minimal support provided to families in the application process. We argue that the barriers and discrepancies identified were an inherent result of the Canadian federalist fragmentation of the delivery of social care and financial support programs for children living with neurodisabilities. A more unified response by Canadian provincial, territorial, and federal governments is clearly needed to take positive steps to address the consequences of federalist fragmentation and respond to the structural barriers and geographic discrepancies identified by this study.
While Canada’s health care system is governed by a set of principles identified in the federal Canada Health Act, R.S.C. 1985, c. C-6, there is currently no federal legislation governing the delivery of social care. This is a product of Canada’s federalist system, whereby governance is constitutionally divided between the federal and provincial governments. Although the provinces have constitutional authority over the delivery of health services, the federal government sets national guidelines for the delivery of funds to the provinces for the management of health care. Due to this division, social care falls into a fragmented constitutional gray area, whereby support for financial costs associated with raising a child living with a neurodisability (ND) is delivered through a combination of provincial, territorial, and federal programs (Prince, 2019). The fragmentation of social care was noted by the United Nations Special Rapporteur on the Rights of Persons With Disabilities, following their first mission to Canada in April 2019 (Devandas-Aguilar, 2019). In their end of mission statement, they wrote that “there is an urgent need for high-level leadership at the federal, provincial and territorial levels to guide and guarantee an effective and coordinated implementation of the rights of persons with disabilities across Canada” (Devandas-Aguilar, 2019, para. 27). The lack of national coordination and gaps in care available to children living with disabilities has only been further exacerbated by the 2019 coronavirus pandemic. As noted by L. Lach and Thomson (2020), the government one-time payments to individuals with disabilities have done little to address what they refer to as a “patchwork jumble of underfunded programs and services.” The failure of supports available to Canadian living with disabilities during the pandemic underscores the importance of the reforms needed for the current social services available.
Our study in 2018 is particularly relevant. After hearing of concerns from parent advocates, researchers at the McGill University Centre for Research on Children and Families partnered with Childhood Disability LINK to initiate and implement the “Pathways Project.” The goal of this project was to create a centralized platform with accurate and up-to-date pathway information on all financial programs available in Canada for children with NDs. These pathways emerged from a cross-jurisdictional, pan-Canadian environmental scan of provincial, territorial, and federal financial support programs available. The project was completed in December 2018 and all of the mapped pathways for the provincial, territorial, and federal programs are publicly available at the Childhood Disability LINK website (
While mapping the pathways, jurisdiction by jurisdiction, it became apparent that there were significant barriers, gaps, and discrepancies. The objective of this article is to examine the nature and scope of these discrepancies—many of which are embedded in the patchwork system of health and social care and are at a higher risk of being under-analyzed and underestimated in times of pandemic and economic crisis. To address this challenge, we combined a critical analysis of existing literature with an environmental scan of financial support programs to compare structural inequities that may account for geographic and jurisdictional availability of and access to financial support programs for children with NDs. As a result, we devised a comprehensive set of pathways that were made publicly available to families. Our aims were (a) to facilitate public access to existing information and available programs as a means of empowering families and (b) to identify areas that require improved coordination, accessibility, accountability, and investment in both existing and future programs. Our hope is that this research will contribute not only to furthering knowledge and reflection but also to foster action and systems’ change in this domain.
Our argument centers on the ways in which the barriers and discrepancies in financial support programs for children living with NDs across jurisdictions are both a structural determinant and a foreseeable consequence of the federalist fragmentation of the delivery of social care. Concerted action on part of the provincial, territorial, and federal governments is needed to proactively address the consequences of that systematic fragmentation and to gradually reduce the socio-geographic discrepancies identified by this study.
Childhood Neurodisability and Financial Supports: The Canadian Landscape
It is estimated 1 in 11 to 12 Canadian children between the ages of 4 and 11 years (Arim et al., 2015, 2017) live with an ND. ND refers to congenital or acquired long-term conditions that are attributed to neurodevelopmental disorders and/or impairments of the neuromuscular system that vary in severity as well as over time (Morris et al., 2013). These impairments and functional limitations relate to the domains of movement, cognition, hearing, vision, communication, emotion, and/or behavior and encompass a broad group of diagnoses, such as autism spectrum disorder, cerebral palsy, and epilepsy, as well as other rare and genetic conditions (Morris et al., 2013). The term “neurodisability” is consistent with a non-categorical approach that has been recommended since the 1980s (Stein & Jessop, 1982). One of its core tenets is that children with similar impairments and their families will share similar challenges and support needs, regardless of the specific diagnosis received (A. Miller et al., 2016; A. R. Miller & Rosenbaum, 2016). Thus, the need for studies by specific diagnosis are deemed neither efficient nor cost effective. Filipe et al. (2020) argue that this non-categorical definition of ND should be expanded to incorporate eco-social dimensions of disability, which is in line with the United Nations (2006) Convention on the Rights of Persons With Disabilities. This expanded approach to defining childhood ND recognizes the person with a disability as having “a diverse set of needs and rights as well as aspirations and capabilities that warrant a pluralistic and ecological (or eco-social) perspective” (Filipe et al., 2020, p. 2) beyond the medical model of disability.
Children with NDs require various levels of additional support to optimize their development and well-being. Often their families play an instrumental role in managing environmental barriers that inhibit their meaningful participation and inclusion. In recognition of these additional supports and the expenses incurred to overcome barriers and achieve the meaningful participation of children living with NDs, federal, provincial and territorial programs provide additional financial resources to their families. This practice of creating programs aims to “provide additional services and resources for certain disadvantaged groups, without reference to means” to “offset their structural disadvantages” (Prince, 2019, p. 126; Thompson & Hoggett, 1996, p. 23).
One of the most significant challenges that families of children with NDs experience is financial strain. In Canada, the household income trajectories of families of children living with NDs is consistently lower than that of families whose children do not have NDs (Rothwell et al., 2020). Families are affected by a wide range of costs that place an additional burden on their financial resources (Stabile & Allin, 2012). This includes direct and indirect costs and long-term economic impacts (see Note 1). First, direct costs refer to “out-of-pocket” costs that are directly linked to the child’s and family’s disability-related needs, such as child care or respite care that is not covered by provincial health care systems or insurance. Second, indirect costs refer to costs incurred by the family to manage tasks associated with the child’s disability. For example, family members may forego opportunities to advance their education or employment opportunities. Third, long-term economic impacts refer to costs associated with children with NDs’ prolonged dependence and care and barriers they face in accessing education and employed as adults (Stabile & Allin, 2012).
In Canada, up to 30% of families raising children with an ND live at or below the Low-Income Cut-Off (LICO) (Arim et al., 2015). In 2013, it was estimated that the combined direct, indirect, and long-term costs associated with raising a child with a disability in Canada was on average $30,500 a year per family (Dudley & Emery, 2014). Results from a 2016 survey by Employment and Social Development Canada found that approximately 30% of families with a child living with “more severe disabilities” reported financial problems as a result of their child’s disability in the previous year (Roy & Chachin, 2016).
The financial costs associated with supporting children living with NDs also vary greatly between provinces. In 2019, the costs associated with supporting a child living with autism were evaluated in a comparative study of the provinces of New Brunswick and Nova Scotia (Tsiplova et al., 2019). This study examined costs associated with autism care from a multi-payer perspective (Tsiplova et al., 2019). The study determined that the average costs of caring for a child with autism are significantly higher in Nova Scotia ($52,251–$108,816 annual cost) by comparison to New Brunswick ($29,015 annual cost) and that these costs also varied depending on regional location (Tsiplova et al., 2019). A more comprehensive study is required to further evaluate and compare these costs across other Canadian provinces and territories.
In addition to financial difficulties, there has been growing research documenting the negative health outcomes for parents of children living with disabilities (Garner et al., 2013; Rothwell et al., 2019). Caregivers of children with NDs (or a combination of NDs and behavioral problems) exhibited a greater number of health and psychosocial problems than caregivers whose children did not have an ND (L. M. Lach et al., 2009). These caregivers were more likely to report having health problems such as food allergies, high blood pressure, cancer, ulcers, heart disease, and depressive symptoms (Arim et al., 2019), and their families were more likely to be distressed and have lower levels of social support (L. M. Lach et al., 2009). Despite the higher rates of pain and physical health problems reported by parents of children with autism, it has been documented that when these parents access formal and informal supports, they gain psychological and physical benefits (Gouin et al., 2016). Adequacy of services support also plays a role in family well-being (Gardiner et al., 2020). Hence, the availability and accessibility of financial support programs for children living with NDs constitutes a social and structural determinant of their health and well-being as well as that of their parents and caregivers (Filipe et al., 2020).
Access to timely and accessible support is an imperative for families of children with NDs. Ritzema (2015) found that adequacy of support moderates the relationship between the complexity of the child’s ND and the child’s well-being. When parents reported that their formal support needs were adequately met, their children’s functional difficulties had a lower impact on their overall well-being (Ritzema, 2015). This moderating effect was further supported by a 2007 Senate of Canada report, Pay Now Pay Later: Autism Families in Crisis, which maintained that “when provided with appropriate support, training and information, families can often ensure that their son or daughter can enjoy a good quality of life” (The Standing Senate Committee on Social Affairs, Science and Technology, 2007, p. 1).
In response to the financial, physical, and psychosocial impacts of raising a child with an ND, provincial, territorial, and federal governments have created multiple financial support programs that vary in format, model, and scale. As noted by Prince (2019), in Canada, there exists a complex realm of social policy for those with a disability. This complex realm consists of a mesh of universal and selective programs to provide disability-needs related funding at the provincial, territorial, and federal levels.
Despite the existence of financial support programs at the provincial, territorial, and federal levels, families of children living with NDs have expressed concerns over accessibility and availability that warrant further investigation. The impetus for this study stemmed from focus groups and interviews with parents of children with NDs living in Montreal, Quebec (Canada) who identified a need for a centralized portal with accurate information on how to access financial support programs in their region (Lach, 2018).
Research Methods
This study was conducted in five phases. First, a list of financial support programs was developed through an environmental scan of provincial, territorial, and federal websites. This list evolved in an iterative manner as outreach with governments and stakeholders occurred.
Second, draft pathways for each support program were created using information from these websites. In some cases, the required information to develop the pathways was not available online and researchers contacted health and social care service providers or program administrators through phone calls and emails to clarify the application process steps.
Third, the draft pathways were validated by at least one stakeholder in each jurisdiction, with a total of 21 stakeholders (see Table 1). This stakeholder consultation phase was a central part of the research process as it enabled draft pathways to be modified based on the feedback from individuals who either navigated the financial support programs themselves, supported others when navigating them, or were directly involved in administering these programs.
Breakdown of Stakeholders Consulted During the Third Phase of the Study.

Note. A “government employee” is someone who either works within a government ministry or department, or works within a program run by government. A “service provider” is someone who works for a community organization or nonprofit that provides services and supports. “Health care professional” includes physicians, nurse practitioners, and social workers.
Fourth, once the consultation phase was completed, the 44 draft pathways were finalized. The final versions of the federal programs and programs in Quebec were then translated into French to ensure they were linguistically accessible and uploaded to the Childhood Disability LINK website (
In the final phase, the mapped programs were classified based on numerous categorizations that included jurisdiction, availability of the program (universal or disability-specific), income caps, the type of funding available (tax credit, stipend, services, etc.), and online accessibility.
Results
Our study identified 44 financial support programs across provincial, territorial, and federal jurisdictions that children living with NDs could be eligible for. The regional breakdown is federal (7), British Columbia (5), Alberta (6), Saskatchewan (1), Manitoba (3), Ontario (3), Quebec (4), New Brunswick (2), Nova Scotia (3), Prince Edward Island (3), Newfoundland and Labrador (3), Yukon (2), Nunavut (1), and Northwest Territories (1).
Four main types of financial support programs were identified: stipends or refundable tax credits (22); non-refundable tax credits (5); services, pharmacare or equipment (full or partial) coverage (12), and support worker funding (5).
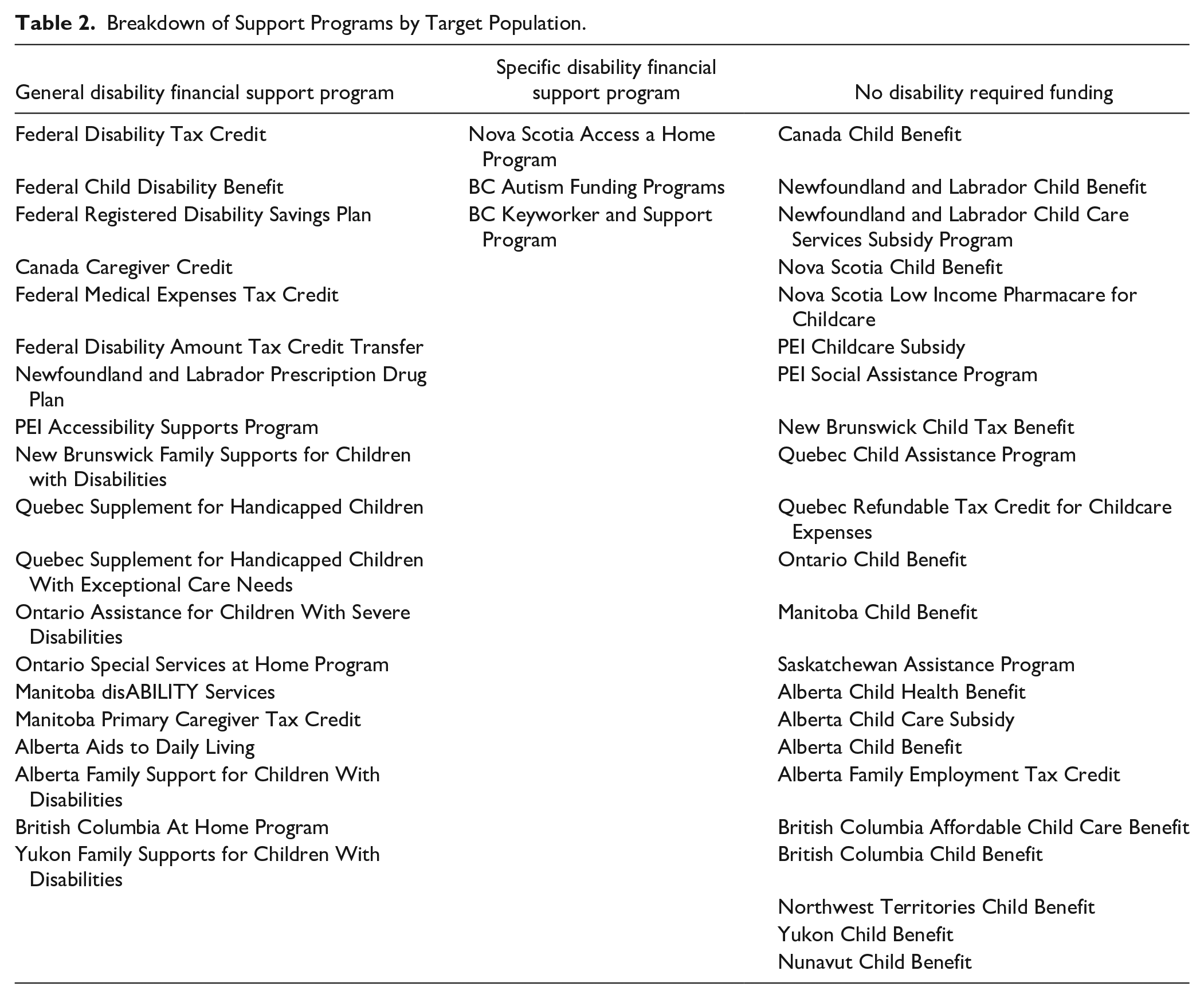
Of the total 44 financial support programs available, 22 of the programs were disability-specific providing targeted funding to individuals living with disabilities and/or their caregivers. Examples of the disability-specific programs include the BC Autism Funding Programs and the Nova Scotia Access a Home Program, which provides funding programs only for individuals who are diagnosed with autism or to those who have physical accessibility needs. The remaining 22 programs were general financial support programs for children and their families that were not limited to children living with disabilities (see Table 2). The majority of examples of general financial support programs are under the child benefit federal and provincial structure. In some instances, provincial, territorial, and federal child benefits can be supplemented if the child has established a disability through the disability tax credit verification.
Breakdown of Support Programs by Target Population.
It was determined that 18 of the 44 programs (40.9%) did not have a sufficient amount of information online to draft the pathways. This included a lack of requisite information on eligibility criteria, disability verification, income caps, and appeal processes if the initial claim is rejected. Of those 18 programs, eight required follow-up with government departments multiple times. Many of the numbers and emails listed had been disconnected and multiple messages were not returned. For Prince Edward Island (PEI), Nunavut, Newfoundland and Labrador, and the Northwest Territories, we experienced additional difficulty connecting with staff in government departments to answer questions about information that was not available online. In some cases, it took almost 4 months to acquire all the information needed to complete the pathways.
All 22 disability-specific programs required disability verification documents from a health care professional. Although there were slight variations in the provincial and territorial definitions of this authoritative designation, it typically required physicians, nurse practitioners, or other specialists to complete the necessary disability verification forms (Canada Revenue Agency, 2016).
Despite the almost universal requirement of disability verification by a health care professional, this process is only partially centralized in Canada. All of the federal financial support programs (seven identified) are based on the disability verification provided by the Disability Tax Credit (Canada Revenue Agency, 2017). To qualify for any of the other federal financial support programs, such as the Registered Disability Savings Plan (Canada Revenue Agency, 2007), the child living with a disability must first be verified under the Disability Tax Credit. At the federal level, the Disability Tax Credit is the gateway to access all of the other financial programs available to those living with disabilities. At the provincial and territorial levels, disability verification requirements are not centralized—with each program requiring independent documentation from health care professionals to qualify.
The sole exception to this de-centralization of disability verification requirements is the provincial child benefits that are administered in collaboration with the federal Canada Child Benefit. This program, which is primarily administered by the federal government in partnership with the provinces and territories, has the Disability Tax Credit as the centralized disability verification for add-on funding through the Child Disability Benefit.
A final observation was made regarding the financial eligibility criteria for the financial support programs available to families of children living with NDs. Fourteen of the financial support programs available to these families are dependent on financial need regulated through income caps (see Table 3).
Non-Tax Credit-Based Programs Categorized by Inclusion of Income Caps.
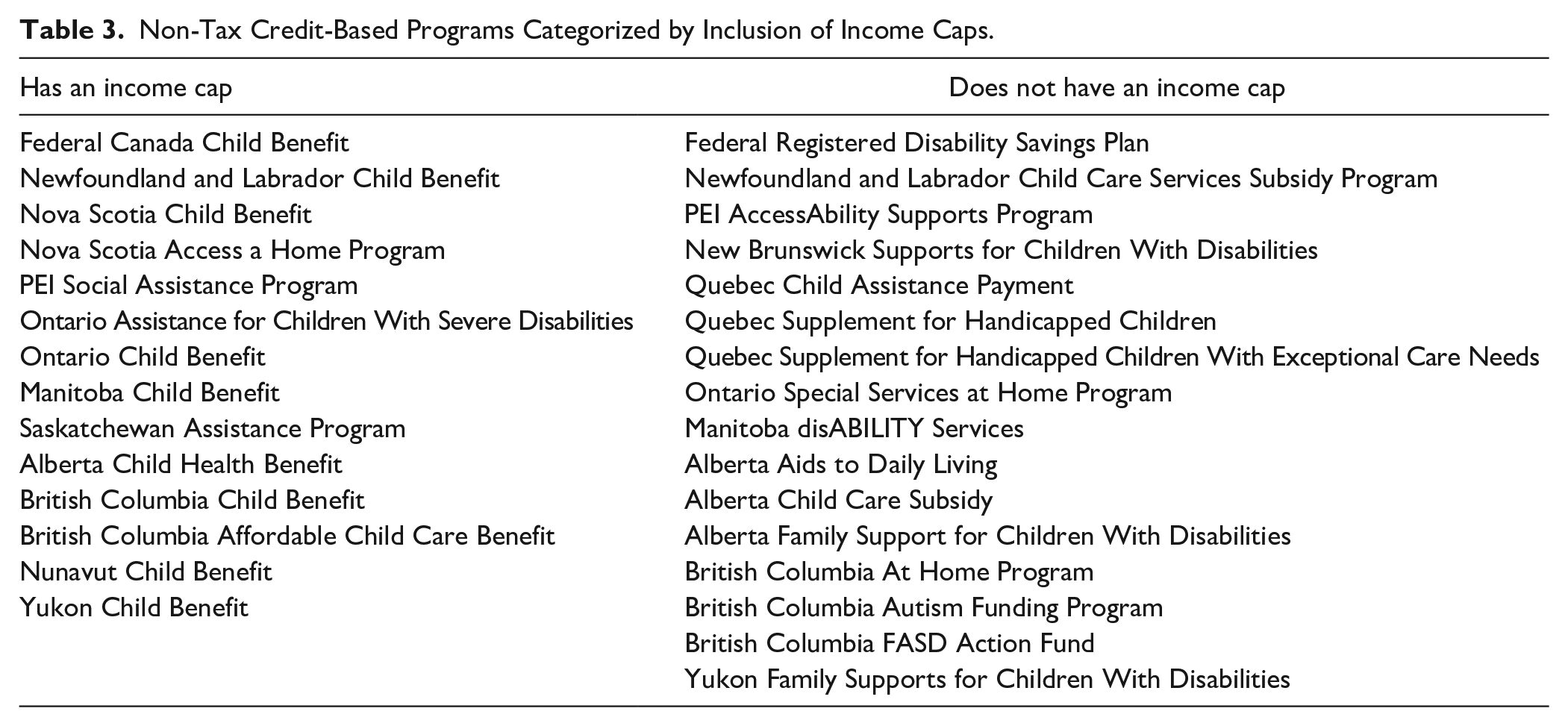

Discussion
There is considerable variation in the number and types of programs offered per jurisdiction, the type and extent of documentation required to access the program, and the online accessibility of the programs. Financial support programs for families of children with NDs impede access to the very support they are intended to provide through structural barriers, limited accessibility of information, and geographic discrepancies.
An overarching thread that must be identified and addressed is the role of federalism in contributing to the health and social inequities experienced by families of children living with NDs. We argue that the challenges faced by these children and their families are a foreseeable consequence of the federalist fragmentation of the delivery of social care through a patchwork of programs across jurisdictions. There is a need for proactive actions by federal, provincial, and territorial governments to reduce the siloing of financial support programs for children living with NDs and to ensure equitable and timely access to those programs both over time and across geographic areas.
Structural Barriers Within a Patchwork System
The delivery of financial support programs for children with NDs and their families, as a type of social care, are not designated within the federalist division of powers. As a result, support for financial costs associated with raising a child with an ND falls into a constitutional gray area and is delivered through a combination of provincial, territorial, and federal programs. These financial support programs operate at various jurisdictional levels. This includes universal programs (i.e., programs available to all Canadians regardless of ability, such as the Canada Child Benefit), as well as disability-specific programs (i.e. the Disability Tax Credit and Registered Disability Savings Plan) (Prince, 2019).
There is a lack of centralized information regarding support programs available to families of children living with NDs in Canada. Despite there being 44 financial support programs at the provincial, territorial, and federal levels, there is no government website that consolidates all of this information for ease of access. It should be noted that, almost exclusively, the governments at the various levels consolidated information on the financial support programs for their jurisdiction. However, the siloing of information within jurisdictions creates added barriers for families of children living with NDs.
This siloing of information exists despite there being shared financial support programs between the federal and provincial/territorial governments through the Canada Child Benefit. The Canada Child Benefit, which includes add-on funding for children living with disabilities through the Canada Child Disability Benefit, is a joint program between the various levels of government that is administered by the federal government. This program provides monthly direct payments to families with children who meet the financial and other eligibility criteria requirements. In addition to various factors such as the financial need and number of children, the payment amount from the federal government differs across Canada depending on the location of the resident. This is based on the individual provincial and territorial cost-sharing agreements with the federal government in their administration of the joint program. The joint administration and coordination of the Canada Child Benefit, with the add-on Child Disability Benefit, demonstrates the interconnectedness of these programs and the reliance of families on financial support funding jointly provided by the federal government. The patchwork delivery financial support programs, lacking centralized up to date information, results in additional barriers for families of children living with NDs.
A further finding was the lack of coordination between the various programs and jurisdictions in regard to the verification of a disability. At the federal level, disability verification is centralized within the Disability Tax Credit. This reduces the burden on families by not requiring them to continuously validate the existence of their child’s disability for numerous programs. Upon being validated under the Disability Tax Credit, the individual (or their family) automatically meet the disability verification requirements for the other six federal disability financial support programs. In addition, although there is no defined period of time that the Disability Tax Credit disability verification is valid for, it was communicated to us by families of children living with NDs that they were not required to resubmit documentation on an annual basis, further reducing the added burden of having to repeatedly re-validate the existence of a long-term ND. Although this is outside the scope of the present work, it should also be noted that the Disability Tax Credit eligibility criteria and implementation has been significantly criticized for lack of accessibility and is currently undergoing a government review of these processes (Colbert, 2020). This is relevant in any discussion around centralizing the disability verification for disability-related financial support programs, as the Disability Tax Credit should undergo more critical analysis before being adopted as the universal disability verification standard.
Unfortunately, the federal centralization of disability verification does not exist at the provincial and territorial levels, all of which require independent verification of the disability for each financial support program. In the present study, there was no observed provincial or territorial centralized disability verification for the programs. This is significant when one considers the fees that can be associated with the filling out of disability verification forms by health care professionals. We received reports of families of children living with NDs, in some instances, being required by health care professionals to pay up to $100 for each disability verification form completed. In provinces with numerous financial support programs for children living with disabilities and their families, ironically, the disability form fees could result in several hundreds of dollars of additional costs for families who are in the process of seeking financial support.
In sum, families of children with NDs face two significant structural barriers in seeking to access financial support programs available to them: the lack of centralization as it relates to information and the disability-related verification process. The current federalist fragmentation that results in a patchwork system of delivery of social supports and services, creates unnecessary barriers and possible additional costs for already financially overburdened families of children with disabilities.
Accessibility to and Accuracy of Information
In addition to a lack of information available online and difficulties in contacting government representatives to gain further information, we also observed that there was significant ambiguity as it relates to information that was provided once getting in contact with government representatives. For example, 18 of the financial support programs available to families of children living with NDs in Canada are dependent on financial need regulated through income caps (see Table 3). For some programs that are income-dependent, we faced significant difficulty in ascertaining the income threshold for eligibility. Many programs specified they were designated for low-income families, but follow-up calls/emails did not provide a threshold or definition for “low-income.”
It is important to highlight that the lack of accessible information, combined with ambiguities inherent in the application process, has led many families of children living with NDs to turn to disability tax agencies to advise them and/or submit the claims on their behalf. These tax agencies often require an up-front fee and are sought out by many families because of the complexities built into the current disability-related funding structure in Canada. Barriers to access the various disability-related financial support programs across jurisdictions are contributing, in that sense, to private market-driven responses and third-party interventions to fill in the gaps left by the fragmented governmental systems. In addition, privately funded services that coordinate and submit disability-related funding applications may not be accessible to low-income families. This results in a paradox of care and social marginalization whereby those who are most in need of additional financial support cannot afford third-party expertise that would facilitate their access to disability tax credit programs.
The lack of accessible information on the financial support programs not only poses a barrier to families accessing the programs themselves, but also a barrier to accessing preliminary information about the programs. It is an added strain on often already overburdened families, whereby they must follow up to acquire critical information required to apply for the financial support programs available to them. This results in many families of children with NDs being required to seek the support of and privately fund disability tax agencies to support them with the complex and vague processes (Rothwell et al., 2020).
Geographic Discrepancies
A key finding of this study was the geographic discrepancies in the number of funding programs, amounts of funding, funding distribution models, and types of funding available based on the province or territory of residence of the child with an ND. First, there was a wide range in the number of funding programs available. It ranged from solely one program in each of the territories and Saskatchewan to five or more programs in British Columbia and Alberta.
Second, many of the provinces and territories have created different funding models and types of funding available to children living with NDs and their families. For example, in Quebec all of the financial programs available were offered as a stipend or refundable tax credit, whereas in Prince Edward Island (PEI), Newfoundland and Labrador, and British Columbia the financial supports are provided through a combination of programs. In PEI, the financial programs were offered through stipends, refundable tax credits, and support worker programs. In Newfoundland and Labrador, the financial supports are provided through stipends, refundable tax credits, services, pharmacare, and equipment coverage. In British Columbia, the financial supports are provided through stipend or refundable tax credits, services, pharmacare, equipment coverage, and support worker programs.
The differences in the number of funding programs and types of funding programs were largely dependent on geographic location. These variations result in considerable geographic discrepancies as it relates to funding for children with NDs and their families. Further research is required into evaluating and contrasting the amounts of financial supports provided to each individual based on the individual funding types and distribution models.
Policy Implications
The structural barriers, limited accessibility of information, and geographic discrepancies we have identified, as it relates to financial support programs for children with NDs, can be addressed through a range of policy reforms. First, governments at the federal, provincial, and territorial level must prioritize having all the necessary information on accessing the financial support programs available online in an easily accessible format. This is one of the most concrete actions that can be taken to reduce barriers to access to government funding for families of children with NDs. Second, the federal government should take a leadership role in centralizing the information on all of the federal, provincial, and territorial financial support programs for children (and individuals) with NDs and their families. The centralized information hub would act as a key accessible resource for parents of children with NDs.
Third, the federal government, working in conjunction with the provincial and territorial governments, should take steps to reduce the burden on families that stems from the disability verification processes. The governments should work collaboratively to jointly reform the existing disability verification processes. There should be a shift toward a singular verification process at the national level that acts as a gateway to accessing all federal, provincial, and territorial financial supports. The singular process that is created should be fully accessible, transparent, and avoid the existing challenges that have been raised regarding the Disability Tax Credit verification processes.
Fourth, the federal government should take on a leadership role by bringing representatives from each province and territory around the table to share knowledges and to strategize together on how to better address inequalities in available financial programs geographically across Canada. This recommendation could be achieved through the creation of a national strategy on disability financial supports. A national strategy, often referred to as a national action plan, differs from a federal strategy in that it encompasses collaboration between the federal, provincial, and territorial governments.
Finally, any steps taken to address the identified shortcomings of financial supports for children with NDs in Canada must account for the unique and complex barriers that Indigenous children face. There must be additional steps taken to understand the experiences of Indigenous children with NDs in trying to access financial supports. Furthermore, any policy reforms must be created and administered in conjunction with Indigenous nations, as has been done with the recent child welfare agreements signed between the federal government, provincial governments, and Indigenous nations (Boisvert, 2021).
Limitations of the Study
There are several identified limitations in this study. First, the provincial, territorial, and federal financial support programs undergo frequent reforms, additions, and removals. The results provided in this study are reflective of their status until December 2018.
Second, it is important to note that due to the research being based out of the McGill University Centre for Research on Children and Families, the researchers were limited to contacting government departments through calls and emails, as opposed to visiting the regional offices. Families who live in the regions where they can access local offices in person, may experience the information-seeking process as less arduous than what was experienced by the researchers who were limited to making telephone calls and sending emails.
Third, to validate the accuracy of the pathways, each draft pathway was reviewed by at least one stakeholder in each jurisdiction. The stakeholders included parents, financial advisors, academics, health care professionals, and government employees. All of the pathways at the federal and provincial levels were validated by identified stakeholders (see Table 1). However, among the pathways created for the territories, we were unable to connect with any of the identified stakeholders in Nunavut and the Northwest Territories.
Fourth, there is a need to identify and analyze the unique gaps in access to services and care that Indigenous children with NDs face. The responsibility of health care and social services for Indigenous communities in Canada is shared by both federal and provincial/territorial governments. This shared responsibility often results in additional administrative confusion, distance from service providers, and funding disparities between provincial and federal programs (Vives et al., 2017). As a result, Indigenous children with NDs face unique challenges in accessing supports that must be analyzed in future research.
Conclusion
In conclusion, we conducted a cross-jurisdictional, pan-Canadian environmental scan to identify provincial, territorial, and federal financial support programs available to families of children living with NDs. In partnership with the organization Childhood Disability LINK, flowchart-styled pathway documents were developed for each financial support, mapping out the processes required to access each support.
A critical analysis revealed structural barriers, limited accessibility of information, and numerous socio-geographic discrepancies. It was argued that some of these challenges could be rooted in the inherent fragmentation of a federalist approach to the delivery of social care and financial support programs for children living with NDs in which a patchwork system prevails. However, without concrete and proactive action by provincial, territorial, and federal governments to reduce the siloing and enhance coordination of financial support programs for children living with NDs, that patchwork system may be a driver of health inequities and socio-economic disparities among Canadians.
The creation of a centralized and in-depth platform on all government financial support programs available to families of children with NDs is a crucial first step to addressing the identified accessibility issues. However, concerted action is required at various levels of the ecosystem (i.e., provincial, territorial and federal governments) to address the fragmentation of a patchwork system that results in barriers and discrepancies in access to disability supports thereby generating inequities among Canadian children and their families. We recommend that coordinated action be accompanied by the systematic collection of data on and multiscale evaluation of existing programs. This approach will determine where the most pressing gaps and needs lie to help establish funding priorities and areas for future policy development in the field of childhood disability and financial support programs.
Footnotes
Acknowledgements
We thank Kids Brain Health Network and Childbright for funding this project. We also thank the countless parents of children living with neurodisabilities who first identified the gap that this study sought to fill and then provided us with countless volunteer hours providing us with feedback. In addition to the parent volunteers, we acknowledge and thank the experts and government officials who provided us with information and feedback on the financial support programs. Finally, we acknowledge the Kanien’kehá:ka Peoples. We recognize that the development and writing of this study was primarily conducted on unceded and unsurrendered Mohawk territory in the Montréal region, and that as settlers we aim to conduct our work in the spirit of reconciliation.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
