Abstract
Keywords
Introduction
Global demographic shifts have made aging a major concern for policymakers and practitioners (Bengtson, 2018). By 2050, the population aged 60 and above is expected to reach nearly two billion (World Health Organization [WHO], 2024), necessitating inclusive frameworks that support diverse aging experiences (Sen & Nagaram, 2024; Settersten & Angel, 2011). Equitable aging refers to the ability of older migrants to age with dignity, access to culturally appropriate care, and the opportunity to thrive regardless of their migration history, language, or socioeconomic status (American Association of Retired Persons [AARP] International, 2022). As global migration continues to rise, ensuring equity in aging for diverse migrant populations has become a pressing public health and social concern (Ayón et al., 2020). Migrants often face intersecting barriers including language difficulties, limited health care access, cultural misunderstandings, and systemic discrimination that compromise their ability to age well in host countries (Ayón et al., 2020; De Voogd et al., 2020; Tang et al., 2020). Despite growing attention to health equity and aging, there remains limited conceptual clarity on what equitable aging entails in the context of migration.
In the literature, definitions of equitable aging often emphasize structural determinants of health, fairness in resource allocation, and inclusive health systems, yet they rarely account for the distinct experiences of aging migrants (Carlsson, 2023). Migrants, particularly those with precarious legal status or from marginalized groups, face compounded disadvantages such as limited access to culturally appropriate care, economic insecurity, and social exclusion (Ayón et al., 2020; Siddiq et al., 2023). Equitable aging emphasizes fairness in access to health care, social support, and economic security (AARP International, 2022), particularly for migrants, who face lifelong barriers such as language challenges, legal insecurity, and socioeconomic disadvantages (Ayón et al., 2020; De Voogd et al., 2020; Tang et al., 2020). Migrant aging experiences are shaped by intersecting factors such as legal status and gender. Refugees frequently contend with trauma and health issues linked to forced displacement (Siddiq et al., 2023), while labor migrants often grow older with limited financial security due to prolonged engagement in low-wage employment (Szabó & Goodin, 2024). Undocumented migrants face heightened risks as they age, largely because of restricted access to health care and social services (Ayón et al., 2020). Migrant women, in particular, experience layered vulnerabilities driven by both gender and legal precarity (Carlsson, 2023; Kc et al., 2024).
Understanding equitable aging requires integrating social determinants of health, as older migrants’ outcomes are shaped by lifetime access to education, income, and health care not just individual choices (Hooten et al., 2022). Structural inequities, including language barriers and limited access to culturally responsive services, worsen late-life health outcomes (Lebrun & Shi, 2011; S. Lin, 2024). Multiple social identities including age, ethnicity, gender, and immigration status compound these disparities, calling for tailored policy responses (Hossen et al., 2023; Peckham et al., 2018). Addressing these inequities involves expanding health care access, income support, and culturally competent services (Kobayashi & Khan, 2023; Ro et al., 2022). Translation services, outreach programs, and diverse staffing improve health literacy and care navigation (Siddiq et al., 2023). Community-based solutions, such as faith groups, caregiver support, and senior associations, strengthen social ties and reduce isolation (Jacobsen et al., 2023; Qi et al., 2022). Coordinated policy and advocacy are essential to integrate aging and immigration strategies, enforce anti-discrimination laws, and improve data collection (Georgeou et al., 2023).
Transcultural nursing plays a key role in promoting equitable aging. Nurses must integrate patients’ cultural beliefs, health practices, and language needs into care delivery (Tosun et al., 2021). Tailored interventions such as interpreter use, traditional healing inclusion, and trust-building enhance care accessibility (Henly, 2016; Prosen et al., 2021). Leininger’s framework of culturally congruent care emphasizes cultural preservation, accommodation, and repatterning (Leininger, 2002), aligning with Im and Lee’s (2018) call for evidence-based, culturally competent models to improve migrant health outcomes.
Despite growing research on aging, the concept of equitable aging remains inconsistently defined, especially for migrant populations (AARP International, 2022). Existing theories often overlook intersecting disadvantages such as restrictive legal systems and cultural mismatches in care (Glass & Vander Plaats, 2013; Hossen et al., 2023; S. Lin & Fang, 2023). Achieving equitable aging requires bridging transcultural care, policy, and social determinants. Achieving equitable aging for older migrants require understanding how transcultural health care, policy, accessibility, and social determinants intersect. More consistent terminology is essential to align academic discourse, policy frameworks, and community interventions with older migrants’ health needs. Integrating transcultural health strategies into aging policies can bridge disparities, promote inclusivity, and foster culturally congruent care.
To clarify the conceptual focus of this article, we intentionally use the term “equitable aging among migrants” to position equitable aging as the central concept, with migration serving as the contextual lens through which it is explored. While “equitable aging” broadly refers to the fair distribution of resources, opportunities, and outcomes in later life (AARP International, 2022), its expression among migrants is uniquely shaped by structural inequities, cultural dislocation, and policy-level barriers. Migrant older adults often face intersecting forms of exclusion, including limited access to linguistically and culturally appropriate services, precarious legal status, and social isolation (Hossen et al., 2023; Peckham et al., 2018). By framing the analysis in this way, the concept of equitable aging is situated within a sociopolitical context that recognizes how migration experiences influence individuals’ ability to age with dignity, autonomy, and inclusion.
Despite growing attention to health equity and aging, there remains limited conceptual clarity on what equitable aging entails in the context of migration. This concept analysis seeks to address this gap by exploring the defining attributes, antecedents, and consequences of equitable aging among migrants, providing a clearer foundation for research, policy development, and culturally responsive nursing practice. A careful concept analysis is needed to clarify equitable aging and inform targeted interventions and policy reforms that ensure dignified aging for all migrants. This analysis aims to: (a) conceptually define equitable aging among migrants and (b) develop a preliminary conceptual model to guide academic research and transcultural nursing care.
Method
This study is informed by Walker and Avant (2019) concept analysis framework, a structured eight-phase methodology designed to systematically define and clarify key concepts. The analysis began by selecting the central concept (Step 1) and articulating the purpose of the analysis to develop a clear, practice-oriented definition that supports nursing theory and culturally responsive care (Step 2). Next, we conducted a targeted review of the literature to explore all known uses and meanings of the concept across disciplines and contexts (Step 3). Through this review, we identified key defining attributes that consistently characterize equitable aging (Step 4). To illustrate these attributes, we developed a model case that embodies all core features, as well as borderline and contrary cases to delineate conceptual boundaries (Step 5). We then analyzed the antecedents (preconditions) and consequences (outcomes) associated with equitable aging (Step 6). Finally, we identified empirical referents including existing tools and indicators used to observe and measure elements of the concept in practice (Step 7) and discussed their relevance to nursing care and policy development (Step 8). This structured process supports the development of a conceptual model that reflects the lived realities of aging migrant populations and enhances nursing practice. To enhance methodological rigor, we followed established literature review procedures, including the development of a comprehensive search strategy, systematic screening and data extraction, and thematic synthesis, while adhering to the PRISMA-ScR reporting guidelines (Page et al., 2021).
Identifying the Concept, Relevant Concepts, and Search Strategy
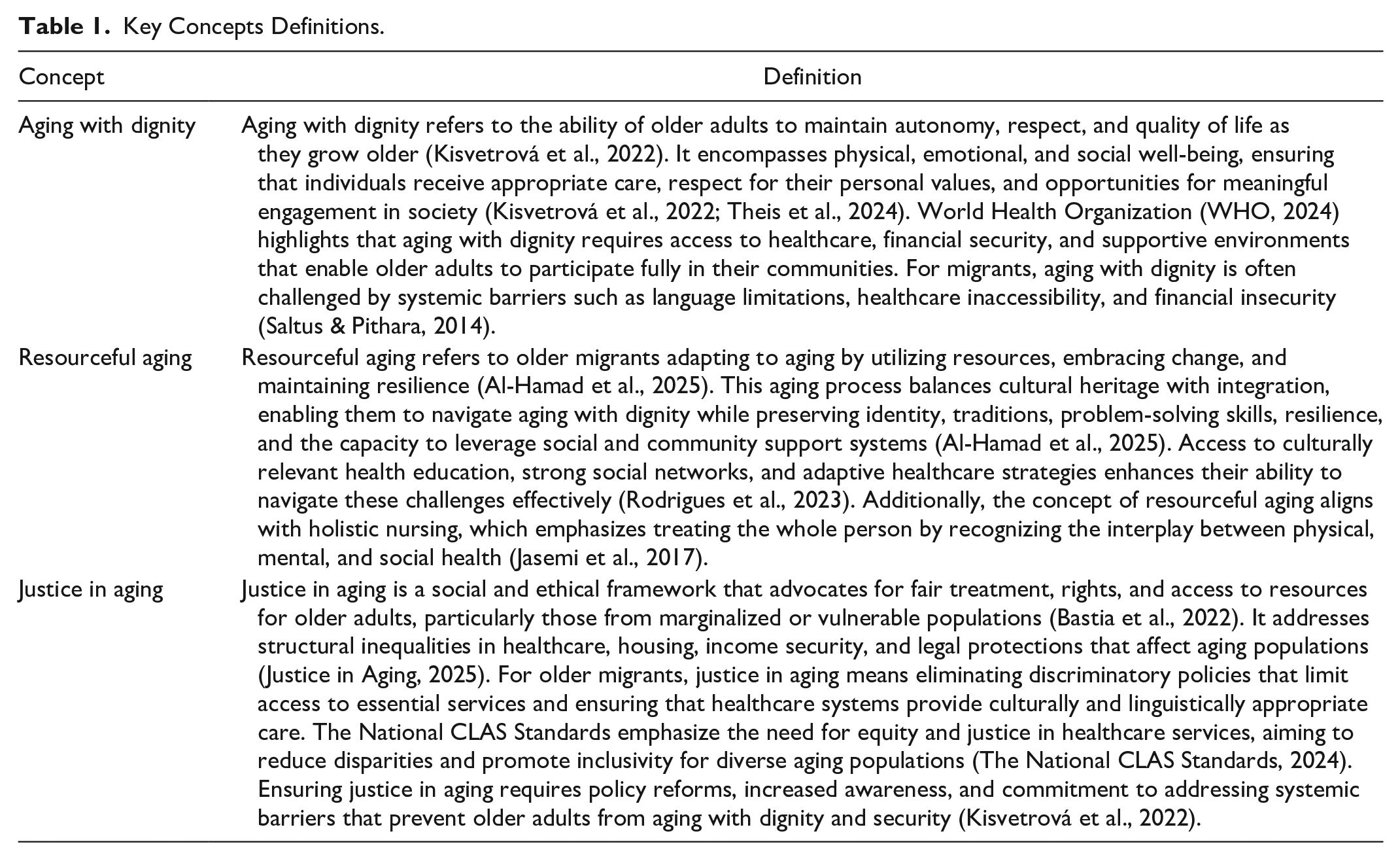
The literature uses various terms to describe similar populations; this analysis adopts the term migrant as an inclusive label for immigrants, refugees, and undocumented individuals, consistent with the IOM definition (International Organization for Migration [IOM], 2019) of those relocating voluntarily or forcibly, permanently or temporarily. Key related concepts include aging with dignity, resourceful aging, and justice in aging also inform this analysis. The following definitions clarify key intersecting concepts—aging with dignity, resourceful aging, and justice in aging—that underpin the analysis of equitable aging among migrant populations. Aging with dignity involves maintaining autonomy, respect, and quality of life in later years, encompassing physical, emotional, and social well-being (Kisvetrová et al., 2022). It requires access to care, respect for personal values, and societal engagement (Kisvetrová et al., 2022; Theis et al., 2024; WHO, 2024). For migrants, this is often hindered by language barriers, limited health care access, and financial insecurity (Saltus & Pithara, 2014). Resourceful aging describes how older migrants adapt by drawing on resilience, cultural heritage, and social support to maintain dignity (Al-Hamad et al., 2025). Access to relevant health education, strong networks, and adaptive care strengthens this capacity (Rodrigues et al., 2023), aligning with holistic nursing’s focus on integrated care (Jasemi et al., 2017). Justice in aging emphasizes equitable treatment and access to resources for older adults, especially those from marginalized groups (Bastia et al., 2022). For migrants, this entails removing discriminatory barriers and ensuring culturally responsive care (Justice in Aging, 2025; The National CLAS Standards, 2024). Achieving justice requires policy reform and addressing systemic inequities (Kisvetrová et al., 2022; see Table 1 for Key Concepts Definition).
Key Concepts Definitions.
A comprehensive database search was conducted with support from a research librarian, using tailored keywords and Boolean strategies. The search was reviewed by another librarian using the PRESS framework (McGowan et al., 2016), with details for search strategy in Supplemental Appendix I. Google Scholar and reference lists were also searched to capture gray literature. The search strategy retrieved 351 records from multiple databases, including Web of Science (n = 109), CINAHL (n = 91), Medline (n = 22), SCOPUS (n = 81), PsycINFO (n = 48), and Google Scholar (n = 20). To maintain a contemporary of the recent waves of migration, only records published from 2010 to 2025 were included, reflecting the evolving migration patterns, aging policies, and support structures developed over the past two decades. The screening process was streamlined using Covidence software, which facilitated efficient record management and reviewer collaboration. After removing 22 duplicates and incomplete records using EndNote, 349 records were screened by two independent reviewers (RR and AZ). Studies were included if published in English and focused on older migrants. Disagreements were resolved through discussion or by a third reviewer (AA).
Following the PRISMA-ScR guidelines (Page et al., 2021), we conducted a systematic data extraction process to ensure consistency and transparency. A data extraction form was developed and piloted to capture relevant information from each included source, including author, year, context, population focus, conceptual definitions, methodological approaches, and key findings related to equitable aging. Two reviewers independently extracted data, and discrepancies were resolved through discussion and consensus. The extracted data were analyzed thematically analyzed (Braun & Clarke, 2023) to identify recurring patterns and refine the conceptual boundaries of equitable aging among migrants. This approach ensured a transparent link between literature and the emergent conceptual structure.
Results
Of the 349 retrieved records, 211 were excluded, and 138 full-text articles were assessed. After further review, 70 were excluded, resulting in 68 studies included in the final analysis. No additional relevant sources were found through reference checks. The PRISMA-ScR diagram (Figure 1) details the screening process.
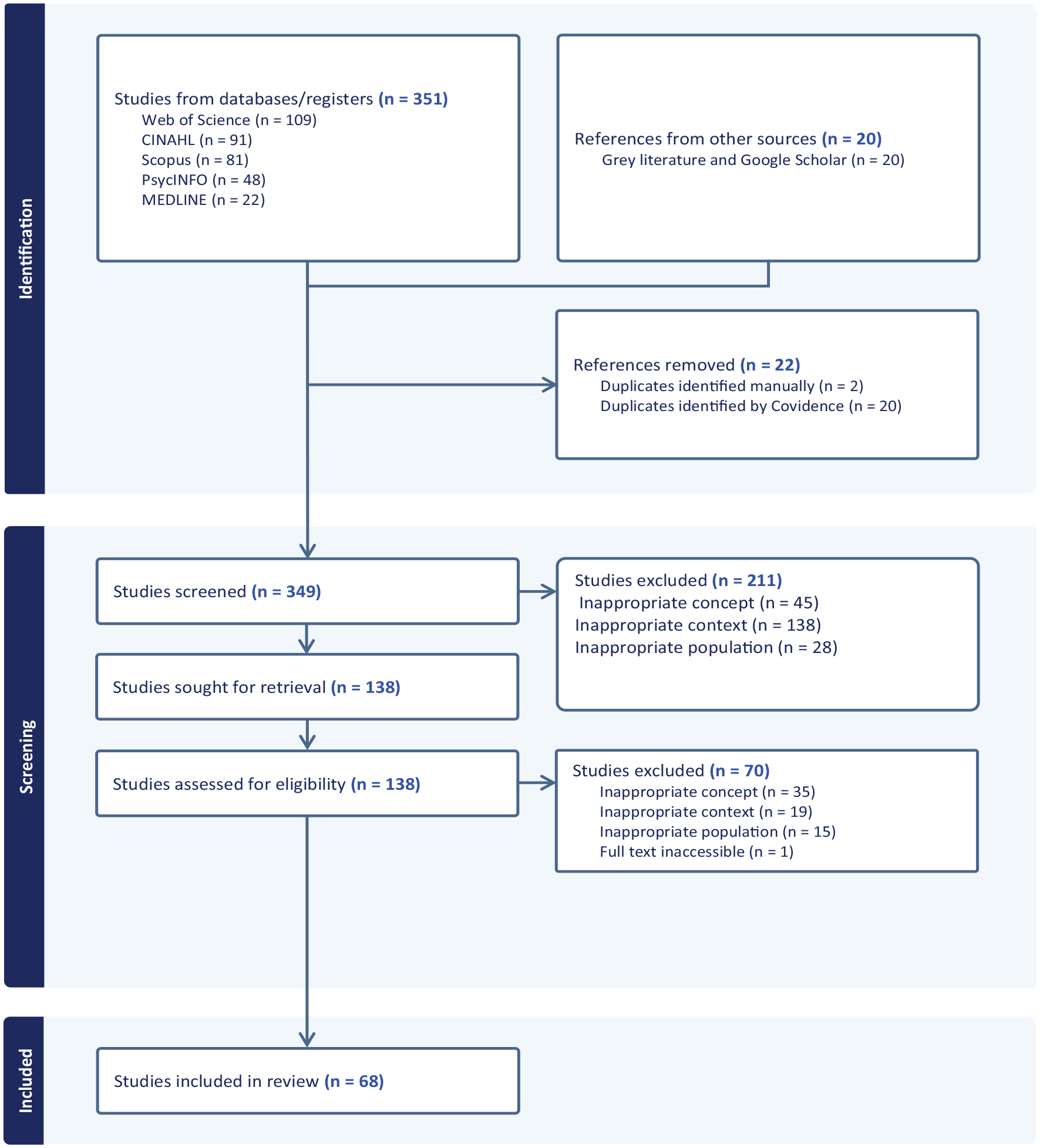
PRISMA Flow Diagram.
Defining Attributes
According to Walker and Avant (2019), attributes represent the defining characteristics of a concept, serving as essential markers that differentiate it from related constructs. These attributes are crucial in determining the concept’s presence and ensuring conceptual clarity (Walker & Avant, 2019). Three fundamental attributes were identified in relation to equitable aging among migrants: (a) fair and just provision of health and social care services; (b) elimination of systemic barriers and disparities; and (c) inclusive and culturally responsive care.
Fair and Just Provision of Health and Social Care Services
Fair and just provision of health and social care services refer to the equitable delivery of health and social care services that actively address the cultural, linguistic, and systemic barriers faced by older migrants. Culturally responsive care is foundational to promoting accessibility and equity, particularly as cultural mismatches between migrants and mainstream health care systems often impede service access and utilization (Knipping et al., 2023; Kwan et al., 2016; Lai & Surood, 2013). Inclusive care must incorporate culturally relevant health education (Kwan et al., 2016), linguistically appropriate primary care (Sierra-Heredia et al., 2024), trauma-informed and family-centered supports (Jacobsen et al., 2023), and sensitive approaches to end-of-life care (Barragan-Carrillo et al., 2022). Additional domains such as oral health (Aarabi et al., 2018), mobility support (Newbold et al., 2023), and digital health literacy (Kaihlanen et al., 2022) must also reflect the cultural realities of migrant populations. The availability of culturally competent providers, language-trained professionals (Al Abed et al., 2014; Jacobsen et al., 2023; Nguyen & Reardon, 2013), and accessible health information in native languages (Meade et al., 2020) is essential to ensure that care is fair, just, and tailored to the diverse needs of aging migrant communities.
Elimination of Systemic Barriers and Disparities
Improving health care access for older migrants requires reducing waiting times, offering flexible hours, and ensuring geographic accessibility, particularly in underserved areas (Bolster-Foucault et al., 2024; Ding et al., 2025; Ghanbari-Jahromi et al., 2023; Kwan et al., 2016; Lai & Surood, 2013). Services must reflect the cultural and contextual needs of diverse groups to promote equity (Chowdhury et al., 2021). Migrants often face integration challenges, identity shifts, and exclusion, requiring community-based support (Georgeou et al., 2023; Siddiq et al., 2023). Economic insecurity and limited insurance further increase health risks, highlighting the need for affordable, inclusive services (Choi, 2011; Danso, 2016; Ma et al., 2021; Newbold et al., 2023; Ro et al., 2022).
Culturally trained interpreters and multilingual staff improve communication and care quality (Al Abed et al., 2014; Barragan-Carrillo et al., 2022; Jacobsen et al., 2023; Pot et al., 2020). Low health literacy limits care access and self-management, calling for multimodal education programs (Chen, 2010; Du & Xu, 2016; Ghanbari-Jahromi et al., 2023; Mandal & Pradhan, 2024). Accessible transport and home-based care further reduce barriers (Deckys & Springer, 2013; Lai & Surood, 2013).
Inclusive and Culturally Responsive Care
Inclusive, culturally responsive care requires language-accessible, culturally competent services that respect older migrants’ beliefs, values, and traditions (Balogun et al., 2025; Chui et al., 2020; Parker et al., 2024). Integrating traditional practices into Western care models can enhance accessibility and promote equity (Al Abed et al., 2014). Long-term care settings should adapt activities and food options to residents’ cultural preferences (Thao et al., 2025), while person-centered programs should align with linguistic and cultural needs (Lood et al., 2015). Health providers must also address mental health stigma, which may deter service use, by creating inclusive, non-judgmental environments (Giebel et al., 2015; Hunt et al., 2024; Siddiq et al., 2023). Sensitive topics like dementia, mental health, and end-of-life care require culturally tailored communication (Sayed et al., 2023). Trauma-informed care is essential for migrants with past distressing experiences (Georgeou et al., 2023), and employing providers with shared backgrounds can strengthen trust and engagement (Carlsson, 2023).
Model and Additional Cases
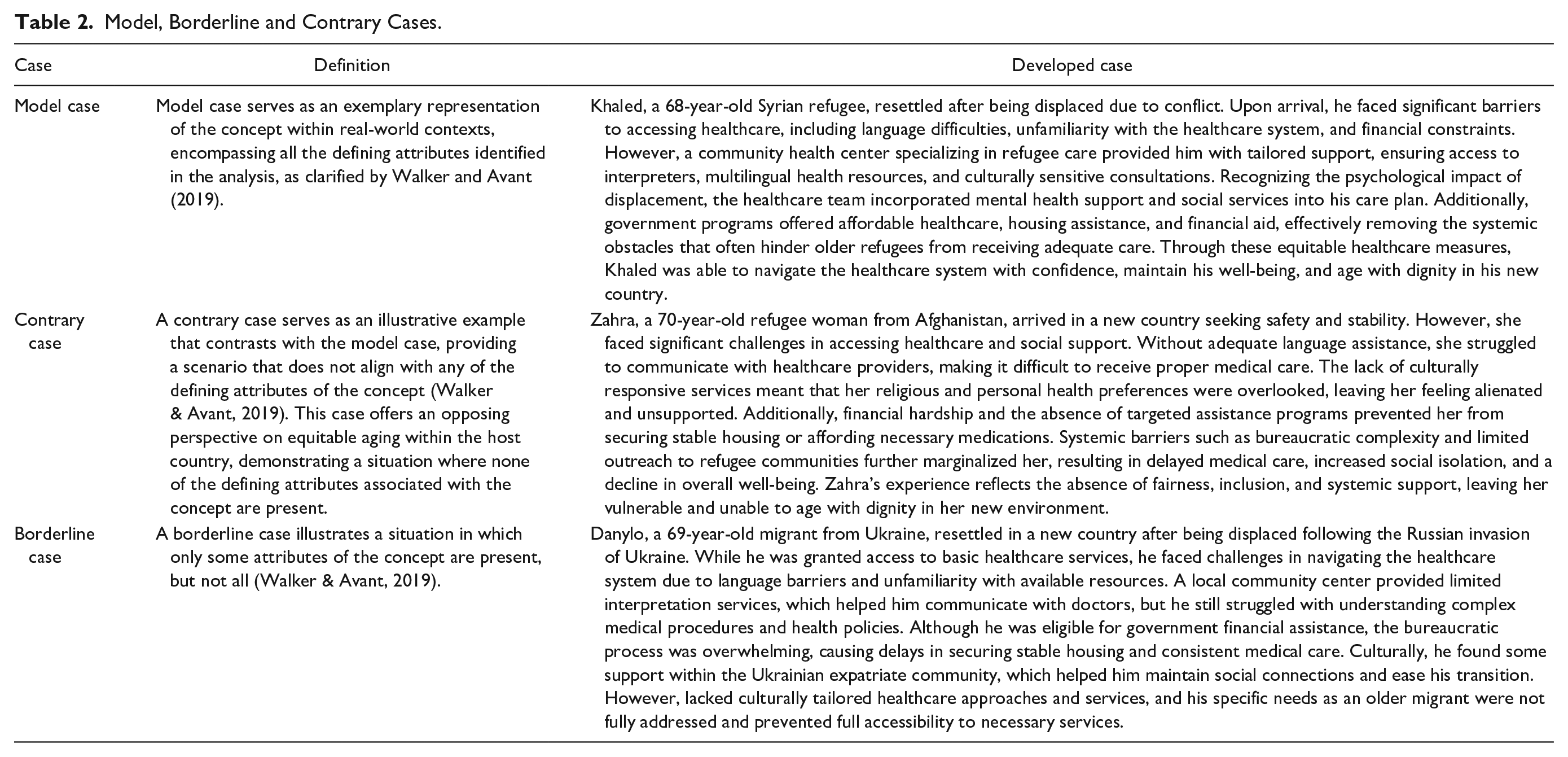
To illustrate equitable aging among aging migrants, model, borderline, and contrary cases were developed (Table 2). A model case includes all defining attributes, while borderline and contrary cases reflect partial or incorrect examples of the concept (Walker & Avant, 2019).
Model, Borderline and Contrary Cases.
Antecedents
Antecedents refer to the necessary conditions that must be in place for a concept to materialize, serving as the foundational elements that give rise to its defining attributes (Walker & Avant, 2019). For equitable aging to be achieved among older migrants, several key factors must be established beforehand. The following discussion illustrates the antecedents.
Availability of Accessible and Inclusive Services
Availability of Accessible and Inclusive Services is a foundational antecedent to equitable aging, as it reflects the structural capacity of systems to deliver fair, culturally responsive, and linguistically appropriate care to diverse aging populations. Accessible and inclusive services ensure fair access to aging support across diverse populations (Lood et al., 2015; Miyawaki et al., 2023). A wide range of affordable, culturally responsive services promotes choice and independence in care (Hurley et al., 2013). Addressing key aging needs such as primary care, cognitive and mental health, oral health, mobility, and cardiovascular care improves outcomes for older migrants (Aarabi et al., 2018; Hunt et al., 2024; Kwan et al., 2016; Newbold et al., 2023; Ogliari et al., 2020; Sadarangani, 2015; Shelley et al., 2011; Sierra-Heredia et al., 2024; Sung, 2014). Involving family caregivers boosts formal care acceptance, while interpreters, translators, and native-language resources support those with limited language skills (G. Kim et al., 2011; Sierra-Heredia et al., 2024; Sung, 2014).
Supportive Aging Policies and Frameworks
Supportive aging policies and frameworks are essential antecedents to equitable aging, as they establish the legal, institutional, and cultural infrastructure that shapes older migrants’ access to care, social inclusion, and financial security. Supportive aging policies and frameworks encompass the existing structural and societal components of systems that allow for equitable aging in older migrants (Salma & Salami, 2020). Universal health care is fundamental for assuring access to services, programs, interventions, and resources for all aging migrants (Abufaraj et al., 2024; Duguet et al., 2016). Cultural norms rooted in filial piety and expectations of intergenerational support foster family involvement in care and strengthen informal social networks (Abufaraj et al., 2024; Carlsson, 2023; Duguet et al., 2016). Legal protections in the form of citizenship status and policies against discrimination can safeguard against the exclusion of aging migrants in service access (Aarabi et al., 2018; S. Lin, 2024). Social security via pensions and benefits provide financial assistance for services and can reduce the financial burden of those in lower income brackets (Aarabi et al., 2018).
Familiarity With the Host Country’s Health Care System
Understanding how to navigate the host country’s health care system is essential for older migrants to access care and resources effectively (Coumans & Wark, 2024). Filial piety can aid in sharing health information within families (Xiao et al., 2024). Information should be offered in multiple formats include oral, audio, visual and reinforced across at least two types to accommodate low literacy, with traditional media often preferred over digital tools (Goodall et al., 2014). Culturally tailored education on disease prevention, such as cardiovascular care for Chinese migrants, is also vital (Kwan et al., 2016). Migrants should be informed about health care navigation and their rights as care recipients (Jang et al., 2020). Navigation programs, such as those for Hispanic patients in end-of-life care, improve service use and treatment outcomes (Barragan-Carrillo et al., 2022). Early mental health screening supports new migrants in accessing care (Siddiq et al., 2023), and outreach in trusted community or religious settings enhances service awareness (Okyerefo & Fiaveh, 2017).
Culturally Inclusive Community Engagement Initiatives
Culturally inclusive community engagement initiatives are vital antecedents to equitable aging, as they facilitate social inclusion, foster belonging, and empower older migrants to actively participate in their communities. Culturally inclusive community initiatives promote migrant participation and strengthen community ties (Runkle et al., 2012). Programs that link migrants with social support networks enhance inclusion and connectedness (Ding et al., 2025; van Hees et al., 2019). Mentorship from community leaders helps newcomers navigate systems and build trust (Cao et al., 2023; Koehn et al., 2022). Volunteering and community contributions foster belonging, while roles like cultural guides enhance older migrants’ self-worth (Kadowaki et al., 2023; Maleku et al., 2022). Incorporating skills like cooking or gardening, along with intergenerational programs, promotes engagement and reduces loneliness (Georgeou et al., 2023).
Consequences
Consequences refer to the outcomes or implications that arise once a concept is fully realized, often leading to further exploration, policy considerations, or areas for future research (Walker & Avant, 2019). The subsequent discussion examines the potential effects and broader impact of equitable aging among migrants including.
Reduce Health and Social Disparities
Promoting equitable aging helps bridge long-standing health and social gaps for older migrants, fostering a more inclusive and just society. Equitable aging among older migrants significantly reduces health and social disparities, leading to greater inclusion and lower disparities between the older migrants in the host countries (Khoo, 2012; Lahaie et al., 2013; Q. Lin et al., 2022; Shelley et al., 2011). Enhanced access to health and social care not only improves quality of life but also promotes greater social integration and reduces health disparities (Chen, 2010; Duguet et al., 2016). Chowdhury et al. (2021) highlight the need for health care system adaptation to address language and cultural barriers, effectively reducing health and social care inequities for older migrants. Facilitating social networks and addressing structural inequities are crucial, leading to improved health outcomes and reduced social isolation (Johnson et al., 2021). Policies supporting cultural well-being and belonging among aging migrants enhance social participation while preserving cultural identity and facilitating integration (Georgeou et al., 2023).
Promote Health Equity and Service Utilization
Equitable aging facilitates greater health equity and empowers older migrants to access and utilize health and social services that meet their unique cultural and linguistic needs. Improving health equity and service access for older migrants reduces family burden and supports culturally influenced care decisions (Chen, 2010; Duguet et al., 2016; García-Ramírez et al., 2014). Better access leads to earlier diagnoses, timely interventions, and greater engagement in health programs (Duguet et al., 2016), while also fostering trust, autonomy, and dignity (Kisvetrová et al., 2022; Saltus & Pithara, 2014; Theis et al., 2024). Culturally responsive, affordable care with language support and respect for traditions improves quality of life and reduces disparities (Chen, 2010; García-Ramírez et al., 2014). Minority-specific services and providers enhance care acceptance (Carlsson, 2023). Removing service barriers and administrative burdens (Lai & Surood, 2013) and enacting inclusive health legislation (Floyd & Sakellariou, 2017) further promote health literacy and empower decision-making.
Foster Social Inclusion and Cultural Integration
Equitable aging contributes to fostering social inclusion and cultural integration, which are essential for enhancing the sense of belonging, reducing isolation, and promoting community engagement among older migrants. Effective social inclusion and cultural integration reduce isolation and improve community participation among older migrants (Johnson et al., 2021; Qi et al., 2022). Strengthening social networks and addressing structural inequities improve health outcomes and economic well-being (Johnson et al., 2021). Respecting cultural and religious traditions while expanding mental health access can reduce fear and isolation, especially among Middle Eastern/Arab American elders (Sayed et al., 2023). Combating racism, stereotypes, and language barriers enhances health care use and overall well-being (Al Abed et al., 2014). Social connectedness also boosts resilience, improving mental health and life satisfaction (Qi et al., 2022).
Improve Health and Enhance Quality of Life
Equitable aging plays a critical role in improving overall health and enhancing quality of life by ensuring that care is accessible, inclusive, and aligned with the cultural and linguistic needs of older migrants. Improved quality of life is a key outcome of equitable aging, supported by accessible, culturally responsive services (Vang, 2023; Vitman-Schorr & Khalaila, 2022; Zubritsky et al., 2013). Inclusive care reduces disparities, increases service use, and empowers older migrants through information and family support (Duguet et al., 2016). Access to timely care, insurance, and rural services further enhances well-being (Ghanbari-Jahromi et al., 2023). Respecting cultural preferences and eliminating structural racism in care facilities are also essential (Thao et al., 2025). Linguistically accessible services enable informed decision-making and promote autonomy, dignity, and personalized care (Kisvetrová et al., 2022; Nguyen & Reardon, 2013; Saltus & Pithara, 2014; Theis et al., 2024).
Empirical Referents
The final step in concept analysis involves identifying empirical referents—observable indicators or measurement tools that reflect the presence and application of a concept in real-world settings (Walker & Avant, 2019). While no singular, validated instrument directly measures equitable aging among older migrants, several tools assess relevant dimensions that contribute to or constrain equity in aging. Structural determinants of health, such as access to services, language proficiency, and social support, are central to understanding inequities among migrant populations. The Commission of Social Determinants of Health Model (2008) provides a foundational framework for examining the societal and policy-level structures that shape health equity. Nguyen and Reardon (2013), for example, apply this model to highlight how language barriers contribute to systemic health disadvantages in aging migrant communities.
Psychological well-being, a key indicator of equitable aging, is assessed using validated tools such as the Kessler Psychological Distress Scale (K10), which evaluates nonspecific psychological distress (Furukawa et al., 2003), and the Geriatric Anxiety Inventory, which measures anxiety symptoms among older adults (Byrne & Pachana, 2011). Broader health-related quality of life is captured using the SF-12v2 Health Survey (Maruish, 2011), while the Connor-Davidson Resilience Scale (CD-RISC) evaluates psychological resilience, a protective factor in adapting to aging-related challenges (Connor & Davidson, 2003). In addition, the Composite International Diagnostic Interview–Short Form (CIDI-SF) screens for depressive symptoms and has been used in cross-cultural geriatric mental health studies (Gigantesco & Morosini, 2008). Social inclusion and connectedness, which are critical to equitable aging, are often measured by the Social Provisions Scale, capturing dimensions such as guidance, reassurance of worth, and social integration (Russell & Cutrona, 1984), and the De Jong Gierveld Loneliness Scale, which differentiates between emotional and social loneliness (De Jong Gierveld & Van Tilburg, 2010).
To contextualize these measures within diverse aging trajectories, broader frameworks also serve as empirical referents. The quality-of-life domains in long-term care, as outlined by Kane (2001, 2003), and applied by Zubritsky et al. (2013), provide measurable indicators of personal autonomy, dignity, and well-being within institutional settings. Khoo’s (2012) “Third Age” model conceptualizes aging as a phase of active contribution and personal growth, while Carlsson’s (2023) super-diversity framework underscores how multiple identity markers—such as ethnicity, gender, and migration history—intersect to shape older migrants’ access to equitable aging opportunities. Together, these empirical referents offer multidimensional tools and frameworks that, while not comprehensive on their own, collectively provide insight into how equitable aging may be identified, assessed, and promoted among older migrant populations.
Conceptual Definition
Equitable aging among migrants refers to the fair and inclusive process by which older migrants access culturally responsive care and supportive environments that uphold their health, dignity, and social inclusion. This definition recognizes the diverse cultural, linguistic, and socioeconomic backgrounds of aging migrants achieved through supportive policies, community engagement, and culturally responsive services. Equitable aging promotes health equity, service utilization, and cultural integration, enabling aging migrants to experience later life with dignity, fostering their well-being and quality of life within host communities.
Conceptual Model Development: Equitable Aging and Transcultural Nursing Care
This section introduces a conceptual model linking equitable aging among older migrants with transcultural nursing. It explores how migrants navigate care and community life in host countries, highlighting conditions that support well-being, resilience, and quality of life. These themes align with transcultural nursing’s focus on inclusive, culturally congruent, community-based care (Im & Lee, 2018; Leininger, 2002; Tosun et al., 2021). The model (Figure 2) was developed collaboratively by four researchers (AA, RR, AZ, and YMY), with expert input enhancing its depth. While conceptually strong, it requires future quantitative validation. Rooted in Leininger’s theory that emphasizes cultural preservation, accommodation, and repatterning, the model promotes respectful, patient-centered care for aging migrants (Balogun et al., 2025; Leininger, 2002). See Table 3 for core principles of transcultural care.
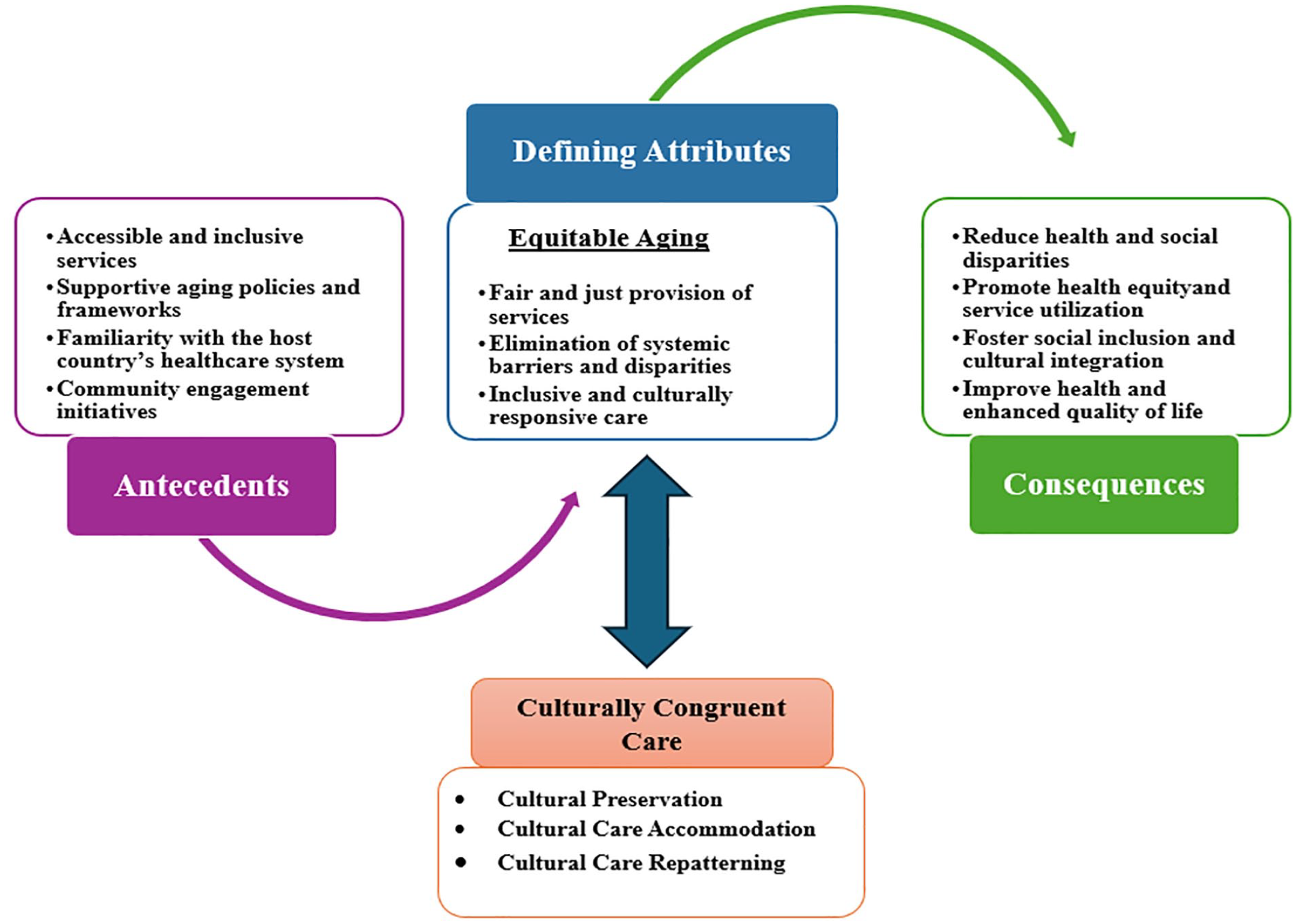
A Conceptual Model on Equitable Aging and Transcultural Nursing Care.
Core Principles of Transcultural Nursing Practice.

Discussion
The landscape of care emphasizes how older migrants navigate formal and informal networks, including culturally specific services (Khoo, 2012), community-based support (Peckham et al., 2018), and transnational health care practices (Metersky et al., 2024) all of which influence their integration into local care systems (S. Lin & Fang, 2023). However, aging migrants often face additional challenges such as mobility limitations (Garcia & Reyes, 2017), past experiences of discrimination (Kisvetrová et al., 2022), and evolving norms of filial piety (J. H. Kim & Silverstein, 2021), which affect their ability to access care. To promote equitable aging, policies should prioritize long-term trust-building with older migrant communities and adopt care landscape mapping to design culturally appropriate, linguistically accessible, and inclusive aged-care services (Hossen et al., 2023).
By shifting the focus from ethnic identity to broader migration-related variables, this approach provides a more nuanced and actionable strategy for improving aged-care accessibility among diverse migrant populations (Rodrigues et al., 2023). Despite the variety of methods to assess specific indicators and circumstances of aging among migrants, there are limited measures to delineate the unique concept of equity in aging migrants (AARP International, 2022; Balogun et al., 2025). The vulnerable positionality of aging migrants in the current socioeconomic and political landscape (Bastia et al., 2022) necessitates further research on appropriate evaluation of equity in the aging process.
The concept of equitable aging among older migrants emphasizes the need for a multidimensional approach that integrates social, cultural, and health care determinants to ensure fair and inclusive aging experiences (WHO, 2024). The preliminary conceptual model was informed by the principles of transcultural nursing, particularly cultural preservation, accommodation, and repatterning (Leininger, 2002). These principles highlight the necessity of culturally congruent care that respects older migrants’ identities while addressing systemic barriers that limit access to equitable care (Piacentini et al., 2019).
Our analysis revealed that equitable aging is shaped by several interrelated factors, including health care accessibility (Kobayashi & Khan, 2023), social support networks (Hossen et al., 2023), and culturally responsive policies (Sobon Sensor, 2019). Older migrants often face language barriers (Pot et al., 2020), unfamiliarity with health care systems (Rodrigues et al., 2023), and financial constraints (Szabó & Goodin, 2024) all of which affect their ability to receive adequate care. Addressing these challenges requires a transcultural nursing approach that prioritizes culturally and linguistically appropriate care (Piacentini et al., 2019), community engagement (Hossen et al., 2023), and person-centered health and social care delivery (Vakil et al., 2023). In addition, the cultural aspects of aging must be considered when implementing equitable health and social care strategies for older migrants (Stanciu & Vauclair, 2018).
The role of family, religion, and traditional healing practices in shaping health behaviors is critical (Ballout, 2024), and health and social care providers must balance cultural respect with medical best practices (Tosun et al., 2021). The preliminary conceptual model highlights the importance of cultural accommodation (Stanciu & Vauclair, 2018), cultural preservation (De Clercq, 2021) and cultural repatterning (Pacquiao, 2008; Plane & Jurjevich, 2009) to fit the beliefs and values of aging migrants while ensuring optimal health outcomes. By integrating transcultural nursing principles with the concept of equitable aging, the model offers a promising and comprehensive framework for addressing health disparities among aging migrants.
Implications
The findings of this analysis have broad implications for policy, practice, research, and community action. Policymakers must develop inclusive aging policies that address the specific needs of older migrants, including access to health care, social services, and culturally tailored programs (Georgeou et al., 2023; Hossen et al., 2023; Kobayashi & Khan, 2023). Policies should also reduce systemic barriers such as language, finances, and bureaucratic complexity (Pot et al., 2020; Szabó & Goodin, 2024; Theis et al., 2024) and promote social inclusion (S. Lin, 2024).
In practice, transcultural care providers must deliver culturally congruent services through interpreter use, adapted materials, and respect for traditional practices (Ballout, 2024; Balogun et al., 2025; Im & Lee, 2018; Tosun et al., 2021). Interprofessional collaboration is vital for holistic care (Vakil et al., 2023).
The findings hold significant implications for transcultural nursing practice. Nurses play a pivotal role in promoting equitable aging by advocating for culturally responsive care that addresses the unique needs of aging migrant populations. Integrating the identified attributes into nursing assessment, care planning, and health promotion enables nurses to foster inclusion, reduce disparities, and support patient autonomy. Culturally competent nursing interventions, including the use of native-language resources, collaborative care models, and community engagement strategies, can enhance trust and service utilization among older migrants (Bastia et al., 2022; Rodrigues et al., 2023; Szabó & Goodin, 2024). In addition, nurses are well positioned to inform policy development and organizational change by highlighting systemic barriers that hinder equitable aging, thereby advancing the profession’s commitment to social justice and culturally safe care. Future research should explore lived migrant experiences, assess current interventions, and expand beyond English-language sources (Bastia et al., 2022; Rodrigues et al., 2023; Szabó & Goodin, 2024). Community organizations play a key role by providing culturally relevant support and bridging gaps between migrants and health systems (Al-Hamad et al., 2025; Baldassar & Wilding, 2020; Hossen et al., 2023; Qi et al., 2022).
Limitations
This analysis views equitable aging among migrants as a complex, multidimensional concept shaped by socioeconomic, cultural, and policy factors. It focused on conceptual understanding rather than assessing literature quality. Due to its interdisciplinary nature, some aspects may not be fully captured, highlighting the need for further contextual research. The review was limited to English-language sources, potentially missing diverse regional perspectives. A key limitation of this concept analysis is the predominantly health care–focused literature base, which may have excluded relevant insights from disciplines such as sociology, law, and public policy that are integral to understanding equity in aging. In addition, while the proposed model offers a useful framework, it requires future validation and quantitative testing to confirm its relevance to transcultural nursing.
Conclusion
This concept analysis used Walker and Avant’s (2019) method to examine equitable aging among older migrants, identifying key attributes, antecedents, and consequences. Equitable aging involves fair access to services, removal of systemic barriers, and culturally responsive care. Essential antecedents include accessible services, supportive policies, system familiarity, and community engagement. When present, these support well-being, social integration, and health care access. The findings offer a conceptual model to guide transcultural nursing and highlight gaps in policy and practice related to inclusivity and cultural competence. Further research should explore system adaptations across diverse sociocultural contexts to advance equitable aging.
Supplemental Material
sj-docx-1-tcn-10.1177_10436596251359129 – Supplemental material for Equitable Aging Among Migrants: A Concept Analysis and Model Development for Transcultural Nursing Care
Supplemental material, sj-docx-1-tcn-10.1177_10436596251359129 for Equitable Aging Among Migrants: A Concept Analysis and Model Development for Transcultural Nursing Care by Areej Al-Hamad, Yasin M. Yasin, Sepali Guruge, Kateryna Metersky, Lu Wang, Cristina Catallo, Hasina Amanzai, Zhixi Cecilia Zhuang, Rezwana Rahman and Andy Zhang in Journal of Transcultural Nursing
Footnotes
Acknowledgements
The authors would like to thank all contributors and colleagues who supported the development of this study.
Author Contributions
All authors contributed to the study design. AA, YMY, RR, and AZ completed the data analysis. RR and AZ conducted evidence screening and data extraction. AA, YMY, SG, KM, LW, CC, HA, ZCZ, RH, and AZ reviewed the findings. All authors (AA, YMY, SG, KM, LW, CC, HA, ZCZ, RH, and AZ) contributed to the preparation and revision of the manuscript.
Data Availability Statement
All data supporting the findings of this study are included within the article.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was funded by the Bridging Divides that is funded by the Government of Canada through the Canada First Research Excellence Fund (CFREF).
Ethics Approval Statement
The authors have nothing to report, and ethical approval is not required.
Patient Consent Statement
The authors have nothing to report.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
