Abstract
I investigate whether there is a causal relationship between physical health and entrepreneurship by exploiting the exogenous introduction of the British Clean Air Act (CAA). This legislation generated across-cohort differences in exposure to airborne pollution. A fuzzy regression discontinuity design is used to investigate the causal impact of improved health following the CAA on adult entrepreneurship outcomes. The results carry important implications for scholarship as well as policymakers, with many governments in emerging economies seeking to curb airborne pollution and improve health and economic outcomes for their citizens, while also seeking to promote entrepreneurship.
Introduction
Does improved physical health stimulate entrepreneurship? This question is of considerable scholarly, practical, and policy interest (Gonçalves & Martins, 2021; Hessels et al., 2017; Rietveld et al., 2015). On the one hand, starting and running a venture can entail long hours, stress, and burnout (Lerman et al., 2020; P. C. Patel & Wolfe, 2021)—conditions which may deter those in poor health from pursuing an entrepreneurial career (Pagán, 2009). But on the other hand, by offering greater autonomy and work flexibility, entrepreneurship might be more attractive to workers in poor health (Stephan & Roesler, 2010). These offsetting effects influence the relationship between physical health and entrepreneurship. Both variables in this relationship interest policymakers wanting to promote public health and entrepreneurial activity.
Most empirical studies have investigated the effects of entrepreneurship on health (Ahn, 2020; Gonçalves & Martins, 2021; Nikolova, 2019; Nikolova et al., 2020; Reitveld et al., 2015; Sewdas et al., 2018; Stephan et al., 2020). However, the causal impact of health on entrepreneurship is also of interest. For example, consider a public health policy, which mandates reductions in air pollution. Will improved health outcomes resulting from this policy affect entrepreneurship, and if so, what types of entrepreneurship? Regarding different types of entrepreneurship, for example, employer entrepreneurs tend to be more exposed than solo entrepreneurs to long hours and operational complexities that make poor health a liability in practicing entrepreneurship (Lerman et al., 2020; P. C. Patel & Wolfe, 2021). Thus, could poor health dissuade people from becoming employers—an objective of policymakers interested in job creation (Henley, 2005)? At present, we lack clear answers to these questions. The problem is compounded by the fact that most available evidence is correlational in nature, rather than causal (Fossen & König, 2017; Herber et al., 2020; Rietveld et al., 2015; Rietveld & Patel, 2021; Xiao & Wu, 2021). Correlational methods are vulnerable to problems of reverse causality, confounded treatment and selection effects, and omitted variable bias. These problems limit our knowledge about how physical health influences engagement in entrepreneurship.
One route toward obtaining causal estimates of impacts of poor health on entrepreneurship involves finding a plausible exogenous “instrumental variable” that influences current health but is independent of current engagement in entrepreneurship. Prior research on the health–entrepreneurship relationship has struggled to find a convincing identifying instrument of this kind (Rietveld et al., 2015). Yet an example of plausible instrument might be environmental pollution, to which individuals were exposed in utero or early infancy (Isen et al., 2017). Clinical research has established that airborne pollution has persistent adverse effects on adult health (Bharadwaj et al., 2016). 1 Yet, while a handful of studies discuss the effects of entrepreneurship on the natural environment (York & Venkataraman, 2010), we know little about the effects of adverse environmental conditions on physical health and thereby on entrepreneurship. While there have been studies of the impacts on adult earnings from early exposure to pollutants like total suspended particulates and lead (Grönqvist et al., 2020; Isen et al., 2017), less is known about the impacts of early exposure of pollutants to the decision to be an entrepreneur later in life.
The present article exploits the 1956 British Clean Air Act (CAA) as a natural experiment, yielding an instrumental variable that can provide quasi-causal estimates of the effects of physical health on entrepreneurship. By reducing airborne pollution, it is believed that the CAA improved long-term respiratory health—a prominent aspect of good general physical health. The CAA was the first global effort to introduce a comprehensive set of measures to tackle airborne pollution, with the aim of improving the environment and general public health. Despite its historical nature, the CAA is a relevant and still even a timely reform to analyze in view of the continuing problem of contemporary air pollution. Because impacts of the CAA depend on month-year of birth, they can be identified using a Regression Discontinuity design (RDD; Calonico et al., 2014; D. S. Lee & Lemieux, 2010). Short of random assignment of health, which is neither ethically nor practically feasible, a RDD is probably the closest one can get to estimating causal effects.
This article argues that the exogenous nature and comprehensive impact of the CAA, together with desirable statistical properties of the RDD, make it a strong and plausible instrument for adult respiratory health. However, I will also discuss several important and plausible threats to the identification strategy, including the gradual roll-out of the CAA; the occurrence of intervening events between early pollution exposure and later involvement in entrepreneurship; and survival biases in sample surveys. Overall, although a thorough examination of these and other issues leads us to conclude that the RDD estimates are likely immune to many of these concerns, the article will try to give a balanced account of the drawbacks as well as the advantages of this novel approach to estimating causal impacts of a prominent aspect of physical health on entrepreneurship.
This article makes the following contributions to the entrepreneurship literature. First, it explains how and why poor physical health can facilitate or deter individuals from engaging in entrepreneurship. This complements existing literature that explores the effects of entrepreneurship on health outcomes—a topic which is not addressed here. In fact, as I will go on to argue, this article’s focus on respiratory health conditions (RHCs; rather than health in general) may help us identify the mechanisms underpinning the effects of physical health on entrepreneurship.
A second contribution of this article is to distinguish between two types of entrepreneurship: solo self-employment and employer entrepreneurship. The latter generally places greater physical demands on entrepreneurs, and I theorize that the negative effects of poor respiratory health will be greater for employer than for solo entrepreneurs. While the distinction between solo and employer entrepreneurship has been the focus of some prior research on entrepreneurship as an occupational choice (Fairlie & Miranda, 2017; Lechmann & Wunder, 2017), less is known about the role of physical health in influencing this choice.
Third, the article’s empirical contribution answers recent calls for more causal inference in entrepreneurship (Anderson et al., 2019), as well as a call from the scientific research community for more quasi-experimental evidence on the impact of airborne pollution on human health (Dominici et al., 2014). It also connects and contributes to an adjacent stream of research on the long-term impacts on entrepreneurship of early-life adversity (Cheng et al., 2021; Churchill et al., 2021; Hayward et al., 2022; Yu et al., 2023). While prior work in this stream has explored the effects of political and climate shocks, this article differs by analyzing the impacts of persistent health problems originating in infancy or early childhood. And by identifying respiratory health as another early-life factor that affects adult venturing propensities, the findings carry implications not only for entrepreneurship scholarship but also public policy.
Theory Development
This section investigates how and why physical health influences the decision to engage in entrepreneurship. I first analyze solo entrepreneurs (“self-employed”) before analyzing employer entrepreneurs. I will frame arguments in reference to a specific health condition, namely poor respiratory health, reflecting the context of this study. Respiratory health is strongly correlated with measures of overall health (Wheaton et al., 2013), having knock-on effects on other health conditions (Decramer et al., 2008). For example, respiratory problems regularly show up as a prevalent health condition both in workplace surveys (Goetzel et al., 2003) and general household surveys—including the one used in this study. In addition, chronic obstructive pulmonary disease (COPD) is one of the ten most costly physical health conditions (Goetzel et al., 2003). According to Decramer et al. (2008), systematic consequences of COPD include deconditioning, exercise intolerance, skeletal muscle dysfunction, osteoporosis, metabolic impact, anxiety, depression, and cardiovascular disease. Finally, as we will go on to see later in the paper, focusing on respiratory health carries an additional advantage in terms of justifying the empirical strategy used in this article.
I follow prior research by leveraging the “Job Demand-Resources” (JD-R) model, which has been applied to chronic illness contexts (Brauchli et al., 2015). According to this model, psycho-social work characteristics can be categorized into job demands and resources (Bakker & Demerouti, 2017; Demerouti et al., 2001; Schaufeli & Bakker, 2004). Job demands impose physical, psychological, and organizational pressures, while resources encompass support, job control (e.g. decision authority), flexibility, and benefits. Poor health reduces individuals’ ability to tolerate high demands and increases the value of resources. Jobs differ in terms of their demands and resources, as do broad occupational categories like paid employment, solo self-employment, and employer entrepreneurship. Here, an employer entrepreneur is someone who builds a team or company with employees, whereas a solo entrepreneur typically works alone. I will start by comparing solo entrepreneurship and paid employment through the lens of the JD-R model, before analyzing implications of poor health for employer entrepreneurship.
Health and Solo Entrepreneurship
According to the JD-R model, when demands exceed resources, strain and burnout increase; but when resources balance or exceed demands, work remains attractive. In terms of job demands, physical illness, especially lung disease, reduces stamina, the ability to tolerate long hours, and resilience (Polanco et al., 2024). Self-employment tends to impose high demands, in the form of high levels of risk and uncertainty (Parker, 1996, 1997, 2025), financial anxiety (Sowan et al., 2024), long working hours (Hyytinen & Ruuskanen, 2007; Nordenmark et al., 2019), physically demanding and dangerous working conditions (Mani et al., 2018; Parker, 2018, sec. 5.5), and the need to multi-task across multiple job roles (Lazear, 2005). For example, managing clients, deadlines, marketing, finances, etc., can be mentally and physically taxing. Moreover, health issues may derail momentum without a team to rely on, making solo self-employment less attractive for this reason as well.
In terms of job resources, paid employment is more likely than self-employment to offer stable incomes, job security, less financial risk, employer health insurance, paid sick leave, legal protections resulting in human resource (HR) accommodations, and more structured and predictable hours (Boeri et al., 2020; Sowan et al., 2024; Spasova et al., 2017). These protective resources can help offset an individual’s health-related shortfall in capacity. So might other aspects of working in a team in a larger, established organization, in which employees can cover for each other when episodes of ill-health occur (Pauly et al., 2008). This not only weakens linkages between wages and individual productivity but also reduces “sickness presenteeism”—that is, situations where workers continue to go to work despite being ill—leading to even lower long-term productivity (Chambers et al., 2017). Evidence shows that presenteeism is greater among the self-employed than employees (Nordenmark et al., 2019).
These arguments are likely to be especially pronounced for people with poor respiratory health, who tend to be more sensitive to dust, fumes, poor ventilation and air pollution in the environment (Hulin et al., 2012), and need flexibility in case of flare-ups in breathing disorders, fatigue, or hospitalizations. They also tend to have reduced physical stamina, for example, owing to shortness of breath, and greater anxiety about exposure to crowded or poorly ventilated workplaces (Mekwilai, 2022). Here again, paid employment offers several advantages, including organizational health policies, formal accommodations for disease flare-ups, and stable job benefits to cover medical costs. These benefits are usually lacking in the workplaces of the self-employed (Park et al., 2020). JD-R logic therefore suggests that because poor health in general, and poor respiratory health specifically, increases the cost of high job demands, this will predispose those in poor health to take jobs with lower demands but higher institutional resources. Paid employment is thus expected to become more attractive relative to self-employment.
On the other hand, the self-employed tend to enjoy greater control over their working lives than employees do, which serves as a valuable resource (Gonçalves & Martins, 2021; Hessels et al., 2017; Stephan & Roesler, 2010). Solo entrepreneurship offers high levels of autonomy and flexibility (Shepherd & Patzelt, 2015; van der Zwan et al., 2018), control over pace and schedule (Hyytinen & Ruuskanen, 2007), and ability to work from home (N. K. N. Kim & Parker, 2021). These resources are especially valuable for people with fluctuating health conditions, such as those with poor respiratory health, since they facilitate working at one’s own pace, reducing the risks of a flare-up of medical conditions. Also, solo entrepreneurs might have greater control over air quality, mask usage of others, and exposure to pollutants or allergens. And, by working from home, solo entrepreneurs can avoid commuting, which (especially in polluted cities) could aggravate respiratory health symptoms (Giménez-Nadal et al., 2018). In terms of the JD-R model, poor health leads people to avoid extra demands they cannot reliably manage (e.g. employing workers), while still enjoying the autonomy that solo entrepreneurship provides.
While these arguments for and against solo entrepreneurship based on the JD-R model seem fairly evenly balanced, there might be reasons to expect the negative impact to predominate. The longer work hours and physical challenges entailed by entrepreneurship likely reduce the actual autonomy and flexibility that entrepreneurs enjoy in practice (Prottas & Thompson, 2006). Discretion and autonomy can also be eroded by taking external finance (Wasserman, 2008). In addition, the solo self-employed who service a single major client in the “gray area” between dependent and independent employment tend to have limited autonomy in practice (Boeri et al., 2020). At the same time, many corporate workplaces have changed to give workers greater autonomy and flexibility, reflecting a widespread aspiration for these benefits among workers in general (Kalleberg, 2003). This erodes the relative resource-based appeal of solo entrepreneurship for people in poor physical health, without detracting from the other resource advantages of paid employment described above. Hence, I propose:
Health and Employer Entrepreneurship
We saw for that the JD-R framework predicts offsetting effects of physical health on solo self-employment relative to paid employment. On balance, I posited a negative overall effect; but as I argue below, being an employer entrepreneur comes with challenges that can be much more complex than those typically faced by a solo entrepreneur. These imply greater job demands that lead us to expect the negative impact of poor health to be stronger for employer entrepreneurs.
First, running a business with employees entails long and often unpredictable hours, with evidence showing that employers work longer hours on average than solo self-employed do (Ajayi-obe & Parker, 2005; Boeri et al., 2020). Longer work hours reflect employers’ generally larger scale of operations, and the reality that employer entrepreneurs must also recruit, retain, and manage a workforce—all while managing the other aspects of their ventures. Those other aspects can themselves be more complex than those of solo entrepreneurs, including compliance with labor laws, creating and enforcing HR policies, and organizing logistics around payroll, insurance, and benefits. Since workforce management can be challenging, this could be a further deterrent to becoming an employer entrepreneur. Firing workers, especially in response to poor worker performance or work–culture misfit, is emotionally and legally challenging (Molinsky & Margolis, 2006); while keeping the team motivated and engaged is an ongoing challenge for employer entrepreneurs, especially in competitive job markets. The entrepreneur also has to deal with interpersonal issues, team conflict, differing work styles, and sometimes toxic employee behavior. This calls for high levels of resilience and tenacity (Yu et al., 2022), making it especially demanding for those in poor physical health (Stephan & Roesler, 2010). For example, a debilitating health condition like a respiratory illness that restricts the flow of oxygen to the body and reduces stamina, can be expected to reduce the energy available to meet heavy work demands.
Second, employer entrepreneurs also bear a burden of responsibility toward their employees, since the decisions they make directly impact their employees’ financial security. Many employer entrepreneurs operate as sole managers, so they cannot simply take time away from their venture (Gumpert & Boyd, 1984; Yagil & Cohen, 2025). This puts additional pressure on employer entrepreneurs who are in poor health (Hessels et al., 2017; P. C. Patel & Wolfe, 2021), leading to anxiety which could trigger respiratory symptoms. For individuals with chronic illnesses—and especially those with respiratory conditions that involve fatigue, sensitivity to environmental triggers, unpredictable flare-ups, or hospital visits—the job demands noted above can be excessively taxing and difficult to sustain (Polanco et al., 2024). Two aspects of respiratory illnesses appear to be especially salient: the unpredictability of flare-ups make it hard for the employer entrepreneur to sustain leadership and managerial continuity, while sensitivity to environmental conditions mean that workplaces may expose them to dust, fumes, or infections from employees.
At the same time, employer entrepreneurs have limited access to compensatory resources, since they must self-fund health insurance, lack paid sick leave for themselves, and cannot easily pause operations without affecting their employees. Nor can they easily work from home (N. K. N. Kim & Parker, 2021) to reduce exposure to airborne pollution and better control their health condition. The JD-R model, therefore, predicts that the high demands and low health-related resources of employer entrepreneurship make it an especially unattractive option for those in poor physical health. 2
In contrast, both solo self-employment and paid employment provide a more favorable balance of demands and resources. Solo self-employment reduces managerial demands by eliminating responsibility for employees, while offering resources in the form of some autonomy, flexibility, and control over the work environment without the added strain of managing staff—benefits that are particularly valuable for individuals with respiratory conditions seeking to minimize exposure to ill-health triggers. Paid employment combines moderate demands with strong institutional resources, including access to health insurance, paid leave, workplace accommodations, and social support from colleagues and managers (Jolly et al., 2021). These resources help buffer the elevated demands created by chronic illness, enabling individuals to sustain participation in the labor market despite poor health. Taken together, the JD-R framework therefore suggests that employer entrepreneurship will likely be especially unattractive to those with poor health, and poor respiratory health in particular. Specifically, employer entrepreneurship maximizes job demands (responsibility for others, financial risk, constant presence) while offering fewer personal health-related resources. Hence I propose: 3
The Medical and Historical Context
Coal Combustion and Air Pollution
According to a report issued by the World Coal Association, coal provided 36% of global electricity generation in 2022, with the International Energy Agency predicting that coal will continue to generate 22% of the world’s electricity in 2040—retaining its position as the single largest source of electricity worldwide. 4 Much of the ongoing growth in coal-power energy generation capacity is taking place in China and India. Coal is not only burned in power and industrial plants but also in residential homes, where it is principally used for indoor heating and cooking. According to the World Health Organisation, about 2.4 billion people regularly cook and heat their homes with polluting fuels; and each year 3.2 million people die prematurely from household air pollution. 5
The main health-impacting airborne pollutants from burning coal are particulate matter (
Impacts of Early-Life Exposure to Air Pollution on Adult Health
If exposure to treatment by the CAA is to be a powerful instrument for (i.e. an enduring influence on) adult health, it is important to establish that exposure to airborne pollution in infancy influences later health outcomes. Below, I first outline the biological channels by which this linkage works, before discussing the medical evidence.
The main biological channel through which air pollution affects health is by impairing cellular and molecular functioning in early life. These in turn retard lung development, and alter epigenetic regulations and immune responses, causing abnormal respiratory conditions and lung diseases in later life. These adverse effects even predate birth, since maternal exposure to air pollution can directly influence the fetus through the transfer of pollutant chemicals through amniotic fluid and placenta … The maternal exposure and disorders further impact on fetal lung functional and structural development, leading to various late onset respiratory diseases (D. Kim et al., 2018).
This suggests that air pollution, and an intervention like the CAA, has the most pronounced health impacts on the functioning of the respiratory system. Health problems resulting from air pollution start immediately, being associated with a range of birth defects (D. Kim et al., 2018), increased infant mortality (Chay & Greenstone, 2003), and reduced infant respiratory function (Bharadwaj et al., 2016; Neidell, 2004). I am unaware of any prior studies linking the CAA to improvements in infant health in the immediate aftermath of that reform. 6 The earliest British study I could find is Collins et al. (1971), who performed an ecologic study of counties of England and Wales over 1958 to 1964, based on indices of domestic and industrial pollution. Those authors reported statistically significant correlations between air pollution and infant mortality, especially infant respiratory mortality. Subsequent international studies, starting with the famous 1969 Nashville Air Pollution Study, have confirmed these findings. However, according to a literature review by Srám et al. (2005), it was only in the 1990s that more detailed investigations into air pollution and birth outcomes took off. 7 However, since the relationship between airborne pollution and infant health appears to hold across time and space, it is reasonable to suppose that it would have held in the context of the CAA, too.
The focus in this study is on adult health. Importantly in this regard, D. Kim et al. (2018) reviewed epidemiological evidence of associations between early (prenatal and perinatal) exposure to air pollution and the incidence of respiratory problems later in life and concluded that the linkage was strong. An important mechanism is that COPD originates from environmental exposure at the maternal stage (Martinez, 2009). Independent, non-epidemiological, evidence further confirms that exposure to pollution during early stages of life can cause significant, long-lasting harm that persists beyond adolescence and into adulthood (Almond & Currie, 2011; Barker, 1990). 8 For air pollution specifically, research shows that exposed babies and in utero embryos go on to report health problems as adults (Isen et al., 2017). Other studies have also uncovered linkages between early exposure to air pollutants and abnormal respiratory function in later life, as well as long-term respiratory diseases (Bharadwaj et al., 2016; Sly & Bush, 2016).
The epidemiological and toxicological evidence also indicates the possibility of delayed onset of respiratory diseases caused by prenatal or perinatal exposure to air pollutants (D. Kim et al., 2018). Strikingly, the impacts of air pollution on RHC tend to intensify rather than weaken with age. 9 This explains why it is logical to link adult outcomes (such as entrepreneurship) with changes in early-childhood health conditions brought about by the CAA.
In summary, the scientific evidence suggests that, by reducing airborne pollution, the CAA likely improved respiratory health among adolescents and adults.
The 1956 CAA
In the 1950s, coal combustion was the major energy source in Britain, for both industrial and residential purposes. In December, 1952, the infamous “Great Smog” in London alone killed as many as 12,000 people (Bell & Davis, 2001). It stimulated a political response which culminated in a government inquiry, and ultimately led to the passing of the 1956 CAA.
The CAA was a landmark piece of legislation, which for the first time anywhere in the world introduced a comprehensive set of measures designed to tackle airborne pollution to improve the general living environment and general public health. The Act, which received Royal Assent on July 5, 1956, contained more than 40 clauses relating to chimney heights, smoke control areas (often called smokeless zones) in which only authorized smokeless fuels could be burned, and industrial premises. Generous grants for householders to install smokeless heating appliances were also offered. The CAA reduced emissions from both residential and industrial sources caused primarily by the burning of coal. According to Giussani (1994), air quality improved after the passage of the CAA, mainly because of changes in the industrial sector.
The CAA applied to all parts of the United Kingdom without exception. It might be thought that the CAA had greater impacts in major towns and cities; but, as Brimblecombe (1987) points out, that was not necessarily the case. Residences located near out-of-town coal-burning power stations were also exposed to high local levels of pollution; and winds generally disperse airborne pollution far from their points of origin, making it more appropriate to consider impacts of the CAA across the country rather than in localized places. Hence, this article will analyze impacts of the CAA nationwide. 10
The CAA was not implemented sharply at a single point in time but rather was spread out over time in a fuzzy manner. Data are very limited, but records of British Smoke (denoted by “BS,” measured in units of
Descriptive Statistics.
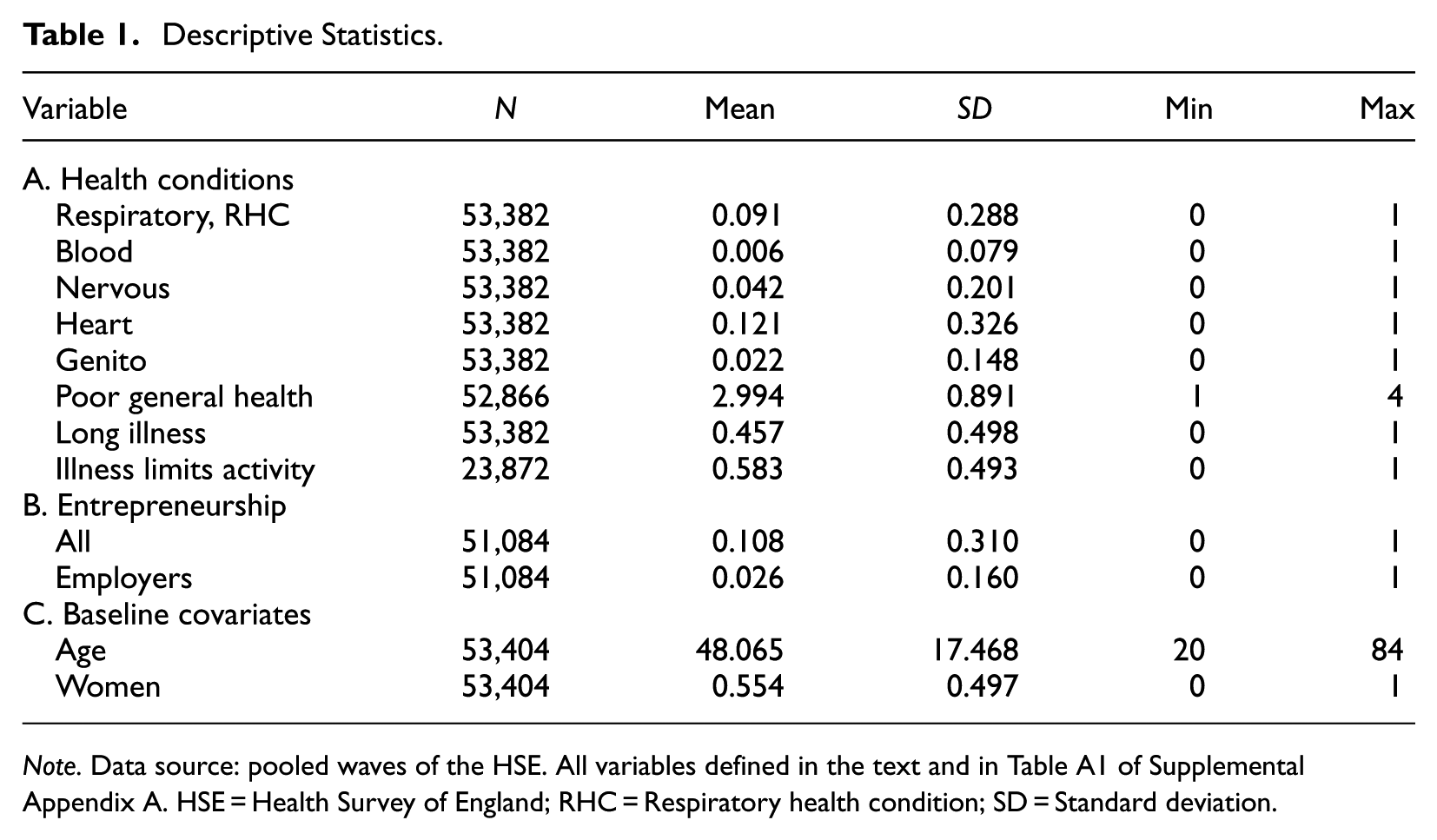
Note. Data source: pooled waves of the HSE. All variables defined in the text and in Table A1 of Supplemental Appendix A. HSE = Health Survey of England; RHC = Respiratory health condition; SD = Standard deviation.
Methods
Methodological Issues in Prior Research
Before outlining the econometric approach used in this article, it is helpful to take stock of common empirical practice. To fix ideas, consider the following regression model relating a variable measuring current health,
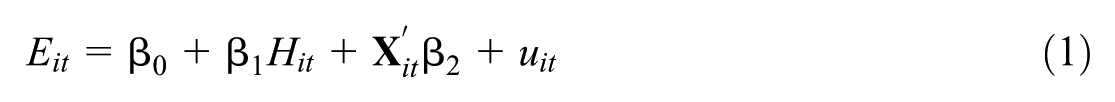
Here,
First, endogeneity arises if the independent variable
Second, it is important to distinguish treatment from selection effects. I argued in section “Theory Development” that poor health might deter people from becoming entrepreneurs; but it is also possible in principle for entrepreneurship to cause poor health. In short, it is unclear whether estimates derived from (1) measure selection into entrepreneurship, an entrepreneurship “treatment” effect on health, or some combination of the two. To distinguish between them, some genuinely exogenous variation in health conditions is needed, such as arises from an unexpected shock. It is important to clarify that not all unexpected events qualify as exogenous shocks. For example, bicycle or horse riding accidents are known to damage physical health; but these occur more frequently among people who cycle or ride regularly, and so are likely in better health to begin with.
Third, OLS is sensitive to the omission of variables that affect both health outcomes and entrepreneurship. Gonçalves and Martins (2021) list several examples, including optimism, resilience, risk aversion, and genetics. To avoid omitted variable bias, the researcher would need to include all relevant covariates in
To overcome these problems, I utilize a RDD, which exploits a truly exogenous source of variation in health outcomes. RDD has several advantages, which are described next.
The RDD
The RDD identifies causal impacts by comparing adult outcomes of people born just before a cutoff date when the CAA took effect with adult outcomes of those born just afterwards. The two variables of interest are health condition
As noted in section “The 1956 CAA,” the CAA was implemented over a rolling window, making an implementation cutoff date “fuzzy” rather than “sharp.” This motivates the use of a “fuzzy” rather than a “sharp” RDD estimator (Cattaneo et al., 2023). There are two stages to a fuzzy RDD. The first stage estimates the impact of the CAA on
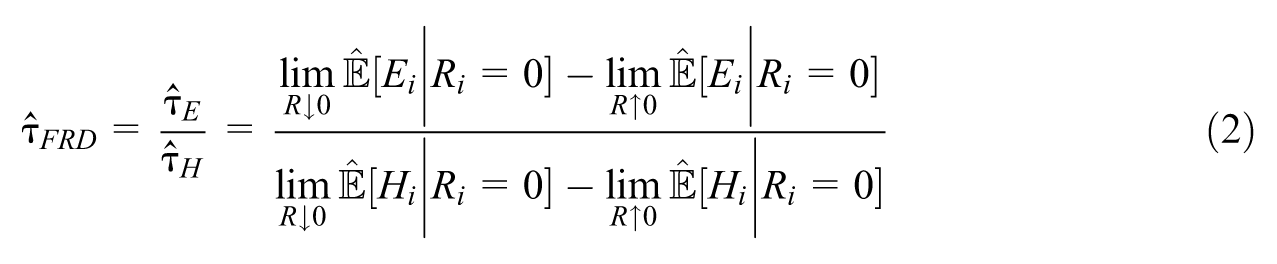
This resembles an “instrumental variables” estimator. Calonico et al. (2014) construct a kernel-based local polynomial non-parametric estimator
The use of limit notation in (2) might give the impression that RDD only estimates treatment effects for the sub-population of individuals exactly at the threshold, and says nothing about treatment effects away from the threshold. As Cattaneo et al. (2023) point out, this is a common misconception. In fact, RDD is an extrapolation-based approach (D. S. Lee & Lemieux, 2010). That is, it uses data away from and not only close to, the cutoff to improve efficiency of the RDD estimator. Thus,
The researcher can choose to condition the expectations
The RDD estimator relies on the minimum of assumptions, requiring only that agents do not have precise control over the running variable,
Using RDD Methods to Analyze the CAA
To start with, one must specify a “cutoff” date, before which the Act did not affect health, and after which it began to do so. In an ideal world, we would know not only when, but also exactly where respondents were born, and the extent of implementation of the CAA at those locations. Since the implementation and impact of the CAA varied across locations, one could then specify more precise cutoff dates that varied across cases. However, while data on date of birth are available, survey information about place of birth and local implementation of the legislation are not. Hence, I apply a common cutoff date to everyone, using month of birth as a common running variable for all cases.
The cutoff date is determined as follows. The CAA received Royal Assent in July 1956. However, the Act took a few months before it began to be implemented by local authorities (Brimblecombe, 1987). Allowing for a 3-month delay suggests a date of October 1956. However, “in utero” health effects from air pollution (D. Kim et al., 2018) mean that embryos gestating in the 9 months after October 1956 were still potentially exposed to high pre-implementation pollution levels. Hence, I extend the October 1956 date by 9 months: making July 1957 the appropriate cutoff date. 13
Two points immediately arise from this discussion. First, it was mentioned that October 1956 is when the CAA “began to be implemented by local authorities.” Implementation rolled out across the country in the months and years that followed, as described in section “The 1956 CAA.” Does this invalidate the use of a RDD? Certainly, a “sharp” design would be inappropriate, as that design assumes a single and precise cutoff date. In contrast, a “fuzzy” design, which models the receipt of treatment as probabilistic rather than binary, is appropriate. In my application, people born after July 1957 had a strictly higher probability of being treated by the legislation than those born before that date. This is sufficient for the fuzzy design to be valid for causal inference, irrespective of the length of the implementation period—provided the local randomization property holds (Lee & Lemieux, 2010, sec. 3.4.1).
Second, it was mentioned that data limitations prevent heterogeneous cutoff dates from being used. How much is lost by using a common cutoff date? On one hand, it might be thought that people born in cities were more affected by the CAA than those born in rural areas, owing to the greater density of pollution sources in cities. However, Britain is a small and densely populated island; and airborne pollution spreads rapidly and over long distances without respecting geographic or regional borders (Burt et al., 2013). Indeed, as Peter Brimblecombe (1987), a leading expert on British air pollution, pointed out in relation to early measurements of sulfur deposits, early researchers were “able to see that most of the sulfur was not deposited within the boundaries of cities, but was transferred into rural areas” (p. 145). And, according to D. Kim et al. (2018), “Exposure to air pollutants mostly occurs in industrial and rural areas due to various manufacturing, traveling, and living activities.”
In any case, while regional data and individual cutoff dates would certainly enable sharper estimates of the causal impact to be obtained, reliance on a common cutoff does not generate biased estimates of the average effect. 14 This means that, to the extent that a causal effect is identified using a common cutoff it will, if anything, understate the statistical significance of that effect. Also, an average estimate understates impacts of the CAA for groups most exposed to pollution, also understating the results for such groups.
Third, it is important to clarify that this empirical design differs from that used in most RDD applications. In my setting, a classical RDD would regard the CAA as the treatment and would seek to measure air pollution as the first-stage outcome variable, whose impact on adult health would be the second-stage outcome. However, such a design cannot be operationalized because we lack data on early-life exposure to pollution and childhood health; and in any case, such a design would not identify impacts on entrepreneurship. 15 Hence, I use RHCs as a proxy for treatment exposure, making the approach more akin to an instrumental variable estimation using a discontinuity-based instrument, rather than a conventional fuzzy design.
Fourth, what of the long temporal gap between the month of birth
Nevertheless, an important caveat with the long temporal gap relates to sample attrition. We only observe treated and untreated individuals who survived to their interview date as adults. So, if respiratory conditions caused by air pollution increased mortality as well as poor adult health, fewer members of the control group survived until the date of interview relative to members of the treatment group. This would understate my estimates of the CAA’s impact—a point that should also be borne in mind when interpreting the empirical findings below.
Data and Variables
I draw data from a large-scale representative national survey: the Health Survey of England (HSE). After describing the HSE dataset, I explain why one specific health measure, namely RHCs, is appropriate both as an outcome of the CAA and as a factor influencing entrepreneurship as theorized in section “Theory Development.” After describing the variables used in the empirical analysis, I present descriptive statistics of the sample.
Data and Variables
The HSE is an annual, ongoing, nationally representative survey of private households in England. Originally commissioned by the U.K.’s Department of Health, the survey commenced in 1991. Over the years, the average annual response rate of households has fluctuated around 75%. Sample sizes of the HSE vary between 12,000 and 20,000 individuals each year. The survey gathers data from face-to-face interviews, self-completion questionnaires, and medical examinations undertaken by a qualified nurse. The HSE contains both self-assessed and objectively assessed data on numerous health conditions. Since data on month of birth, which is needed for the RDD, is only available from 1998 to 2002, these five waves were used in the analysis. The data were downloaded from the U.K. Data Archive via the U.K. Data Service under the End User License. In accordance with the U.K. Data Service terms and conditions, the original or derived microdata cannot be shared publicly; however, the scripts posted by the author at the Harvard Dataverse at https://doi.org/10.7910/DVN/NO0B5Y should enable researchers with authorized access to the original HSE datasets to recreate the dataset used in the analysis and replicate the reported results exactly.
Dependent Variables
Like other studies that utilize large samples of secondary data (Nikolova, 2019; Yu et al., 2023), participation in entrepreneurship is based on a survey question in the HSE asking whether respondents are self-employed. Two measures of entrepreneurship are used to test Hypotheses 1 and 2. The first is a broad measure of entrepreneurship, All, which takes the value 1 if the respondent is a solo (i.e. non-employer) or employer self-employed, and 0 if they are a paid employee. The second is a narrower measure of entrepreneurship, Employers, which takes the value 1 if the respondent is employer self-employed, and 0 if they are solo self-employed or a paid employee. This measure is appropriate given evidence that solo self-employed are more similar to employees in terms of their workloads than employers are (Ajayi-obe & Parker, 2005). Table A1 of Supplemental Appendix A provides detailed definitions of these variables and the others described below, as well as the precise survey questions used in the HSE questionnaires.
Data limitations in the HSE mean that there are insufficient observations to estimate the impacts of health on a different dependent variable, namely, entry into self-employment (or employer-ship). Hence, one might be concerned about reverse causality from entrepreneurship to health, which could confound the econometric estimates. However, there are two reasons to doubt the importance of this concern.
First, prior research has found limited empirical support for a feedback effect from entrepreneurship on physical health. For example, Rietveld et al. (2015) found no evidence of feedback from self-employment to health outcomes. Nikolova (2019) failed to detect significant changes in health among Germans switching into self-employment from unemployment (though positive impacts were observed for those switching from paid employment). Stephan et al. (2020) also failed to detect significant impacts of transitions into self-employment on physical health, while Nikolova et al. (2020) reported that transitioning out of self-employment had little effect on self-reported physical health, either. And using data from a Dutch cohort study, Sewdas et al. (2018) estimated that time spent in self-employment did not affect self-reported health outcomes. In summary, the evidence suggests that being self-employed does not affect physical health outcomes.
Second, according to Shepherd and Patzelt (2015), stress and negative emotions are the main channels through which reverse causality would occur. This would be expected to show up in the form of stress-related illnesses. However, as explained next, my main independent variable is not general health, but rather respiratory health. This is not primarily a stress-related disease, so its presence (based on exposure to a historical event) should be independent of any reverse feedback effect.
Independent Variable
Consistent with the scientific evidence linking coal smoke to respiratory health problems, my principal health measure is a binary variable, RHC, taking the value 1 if the adult respondent reported having a respiratory system health condition, and 0 if not. As with all self-reported health data, one can always ask whether RHC might be prone to reporting error by respondents. There are several reasons to doubt that this is a major problem. Apart from the fact that there is little reason for survey respondents to dissemble about their health, the HSE sends registered nurses to households to gather health data—enhancing the reliability of those data.
18
And, even if there is misreporting of health conditions, the RDD estimator
Although it might seem a narrow measure of poor physical health, RHC is a suitable variable to use in this study. First, as explained in section “Impacts of Early-Life Exposure to Air Pollution on Adult Health,” it is the health outcome most directly affected by the CAA. Hence, one would expect a significant negative impact of the CAA on RHC, but not necessarily on other health outcomes. Second, as noted at the start of section “Theory Development,” RHC is a common and serious physical health problem, which is strongly correlated with measures of overall health. Thus, RHC is not as “narrow” a measure of general health as might first appear. Third, and perhaps most important, much of the theory development was framed in terms of RHC, so this measure is congruent with the conceptual arguments above.
To build out this last point, poor respiratory health is a debilitating condition that impairs function, making it harder to do demanding work such as running a business. Evidence shows that people with RHC experience activity impairment and reduced work productivity (Solem et al., 2013). Moreover, respiratory problems such as sleep-related breathing disorders can cause daytime sleepiness and tiredness, which also impairs work performance (Roux et al., 2000). Finally, unlike mental health or measures of general health—which might be prone to feedback effects from being an entrepreneur—RHC is a lifetime liability as explained in section “Impacts of Early-Life Exposure to Air Pollution on Adult Health,” and therefore not obviously affected by reverse causality.
Nevertheless, it is important to recognize that RHC does differ from measures of general health in some respects. This includes its gradual and cumulative onset and persistence, contrasting with other health risks like heart attacks, which tend to be more sudden. This will inform my efforts to connect the findings to the extant literature at the close of the paper.
I also gathered data from the HSE on other health measures to perform validation (placebo) checks. In contemporary Britain and Western Europe in general, air pollution is no longer primarily caused by burning coal. Rather, it comes mainly from vehicle exhaust emissions, exposure to which has been linked to contemporaneous blood and related conditions, the nervous system, the heart and circulatory system, and the genito-urinary system (European Environmental Agency [EEA], 2023). Coding incidences of these conditions as the binary variables Blood, Nervous, Heart, and Genito, respectively, one would expect smaller, and possibly non-significant, effects from the CAA on these variables. I will test this in robustness checks later in the paper. I also estimate the impacts of the CAA on measures of self-assessed general health among adults. Poor General Health is a reverse-coded 4-point ordinal scale (see Table A1 of Supplemental Appendix A). I also code two additional binary variables, Long Illness if the respondent reports they had a longstanding illness of any kind; and Illness Limits Activity if the respondent reports their activities were limited owing to illness. Since these measures reflect numerous factors unrelated to the CAA and are not strongly correlated with RHC (see below), I also expect smaller and imprecise impacts from the CAA on these measures, too.
Descriptive Statistics
Since many self-employed people work into their 80s in Britain (Parker & Rougier, 2007), the sample comprised all workers aged between 20 and 84 years of age. This left a sample size of
Panel B of Table 1 shows that nearly 11% of workers are entrepreneurs, and that about one-quarter of the self-employed are employers. These sample statistics are consistent with nationally-representative estimates from other sources (Moralee, 1998). Table A2 of Supplemental Appendix A presents the correlation matrix of the variables in Table 1. Apart from heart conditions, RHC is the health condition most strongly correlated with self-reported poor general health. However, the inter-correlations of the various health conditions are generally modest.
As noted above, in RDDs, it is essential that any included covariates are exogenous. Unlike regression analysis, there is no need to include covariates (control variables) to deal with omitted variable bias. Crucially, however, potentially endogenous covariates must be excluded, as they can be “bad controls” that undermine causal inference (Frölich & Huber, 2019).
20
In fact, the historical nature of the CAA limits the number of available exogenous “baseline covariates”
Results
Estimates of the Health–Entrepreneurship Relationship
Table 2 presents robust FRD design estimates
Impacts of the CAA on Respiratory Health and Entrepreneurship.
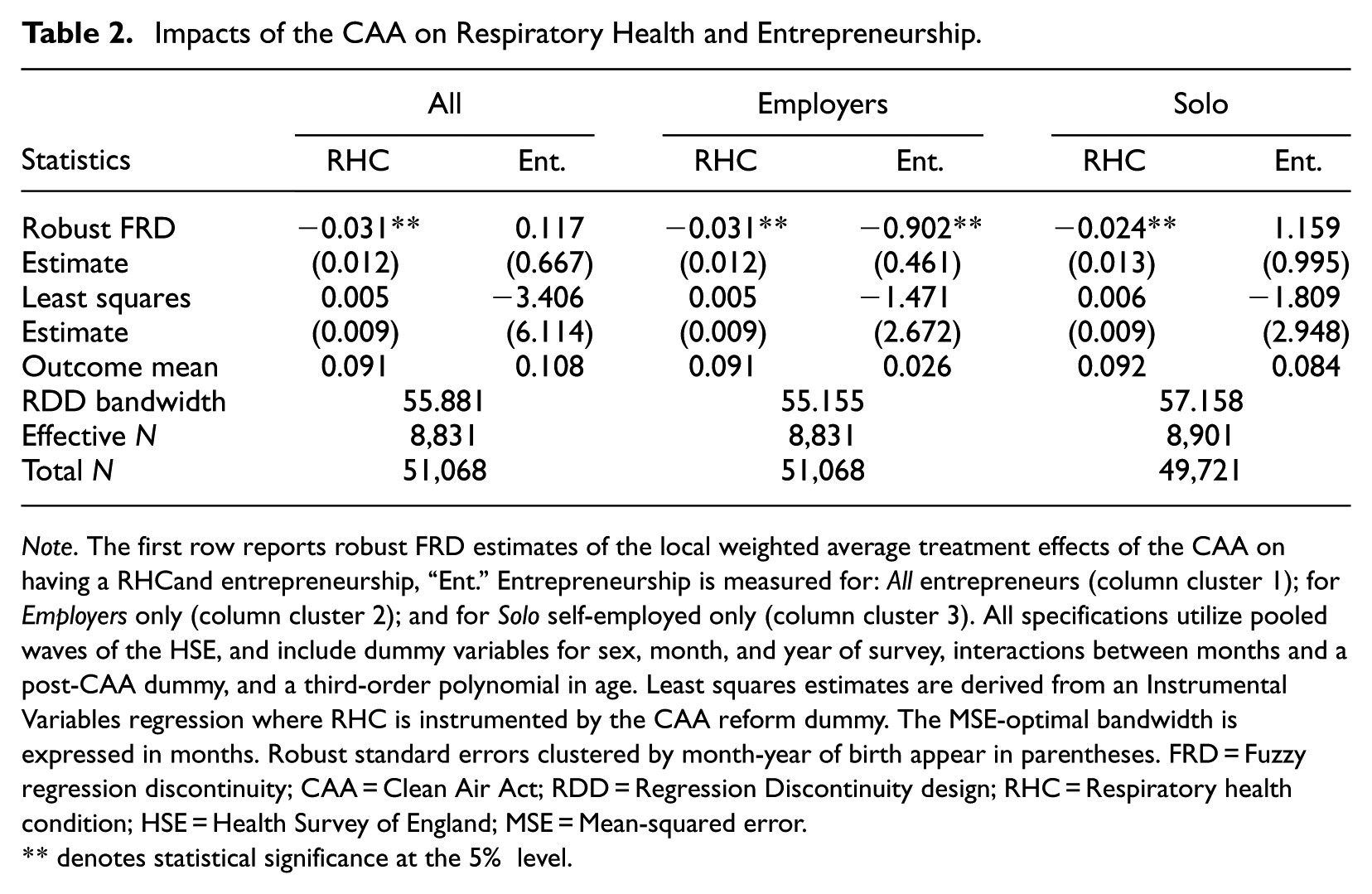
Note. The first row reports robust FRD estimates of the local weighted average treatment effects of the CAA on having a RHCand entrepreneurship, “Ent.” Entrepreneurship is measured for: All entrepreneurs (column cluster 1); for Employers only (column cluster 2); and for Solo self-employed only (column cluster 3). All specifications utilize pooled waves of the HSE, and include dummy variables for sex, month, and year of survey, interactions between months and a post-CAA dummy, and a third-order polynomial in age. Least squares estimates are derived from an Instrumental Variables regression where RHC is instrumented by the CAA reform dummy. The MSE-optimal bandwidth is expressed in months. Robust standard errors clustered by month-year of birth appear in parentheses. FRD = Fuzzy regression discontinuity; CAA = Clean Air Act; RDD = Regression Discontinuity design; RHC = Respiratory health condition; HSE = Health Survey of England; MSE = Mean-squared error.
denotes statistical significance at the 5% level.
Figure 1 graphs the RDD discontinuities in RHC associated with the CAA, based on the estimates presented in the first two column clusters of Table 2. The points in the figure are the mass points, which are noisy monthly averages. The fitted lines in the figure account for the different number of observations corresponding to each mass point in the figure, and therefore portray a clearer discontinuity, consistent with Table 2, whereby the CAA caused a modest, but significant reduction in the incidence of RHCs.
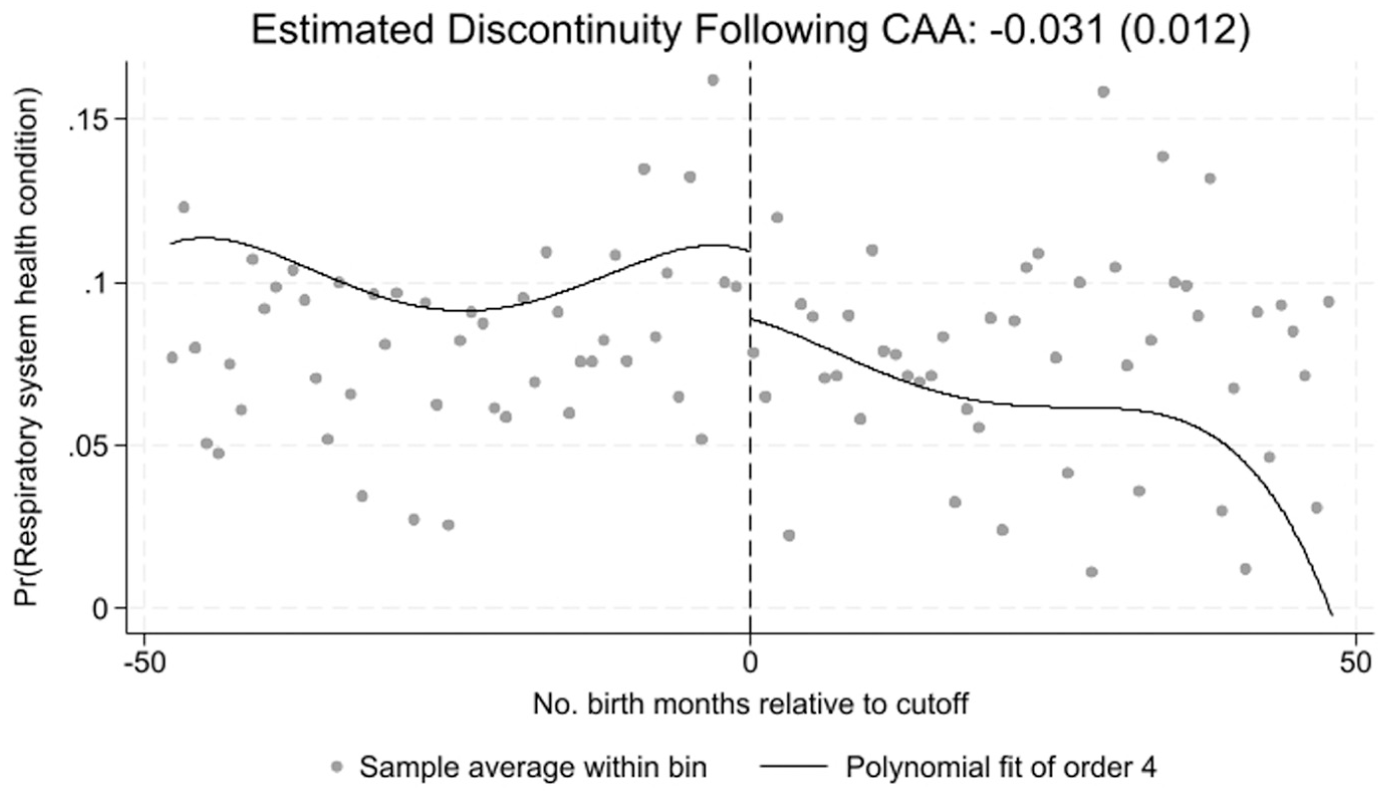
1956 CAA: Impact on adult respiratory health condition.
According to Table 2, the effects of RHC on adult self-employment—both solo and solo grouped with employers—are not statistically significant, in contrast to Hypothesis 1. However, a significant negative impact is detected when the narrower measure of entrepreneurship based on employer status is used, consistent with Hypothesis 2. This might reflect the fact that employer entrepreneurship is more physically demanding than solo entrepreneurship, inducing people with RHCs avoid it. Indeed, although work hours is a crude measure of physical demands of work, evidence from Britain shows that employer entrepreneurs do indeed work longer hours on average than either solo entrepreneurs or paid employees (Ajayi-obe & Parker, 2005). While the magnitude of the FRD coefficient, −0.902, might seem large, it should be borne in mind that the fuzzy RDD estimator is an instrumental variables-type estimator. As such, it measures the impact on the outcome variable only for the sub-population who were most affected by the CAA reform—that is, the local average treatment effect. This is expected to be larger than the average treatment effect, whose value is influenced by those affected less (see S. O. Becker, 2016). Thus, the robust estimates in Table 2 do not describe the average difference in the outcome variable (entrepreneurship in this case) for those with RHCs relative to those without. Hence, it is not comparable to the average employer entrepreneurship rate of 2.6%. 24
Next, I probe the mechanisms underlying these findings. Although I lack data on entrepreneurs’ exertion, I can explore implications of exertion on several variables that are measured in the HSE. First, if poor physical health impedes physically demanding work, as hypothesized, then one would expect a negative association between RHC and the number of days that respondents reported doing heavy manual work in their spare time. Columns (1) and (2) of Table 3 report tobit regressions both without and with covariates to test this idea. The results provide supporting evidence, with RHC being significantly associated with one less day on average that respondents spend doing manual work of 30 min or more per day—the same as the sample mean. Second, I asked whether RHC was negatively associated with working in the manufacturing sector, since traditionally that sector hired many manual workers. Columns (3) and (4) of Table 3 report probit estimates suggesting that it does not. The reason for this finding appears to be that manufacturing work at the turn of the present century did not attract people who choose to perform more manual activities than other sectors, since the correlation coefficient between doing manual work and working in manufacturing was −.008 (p-value: .242).
Manual Work as a Direct Mechanism.
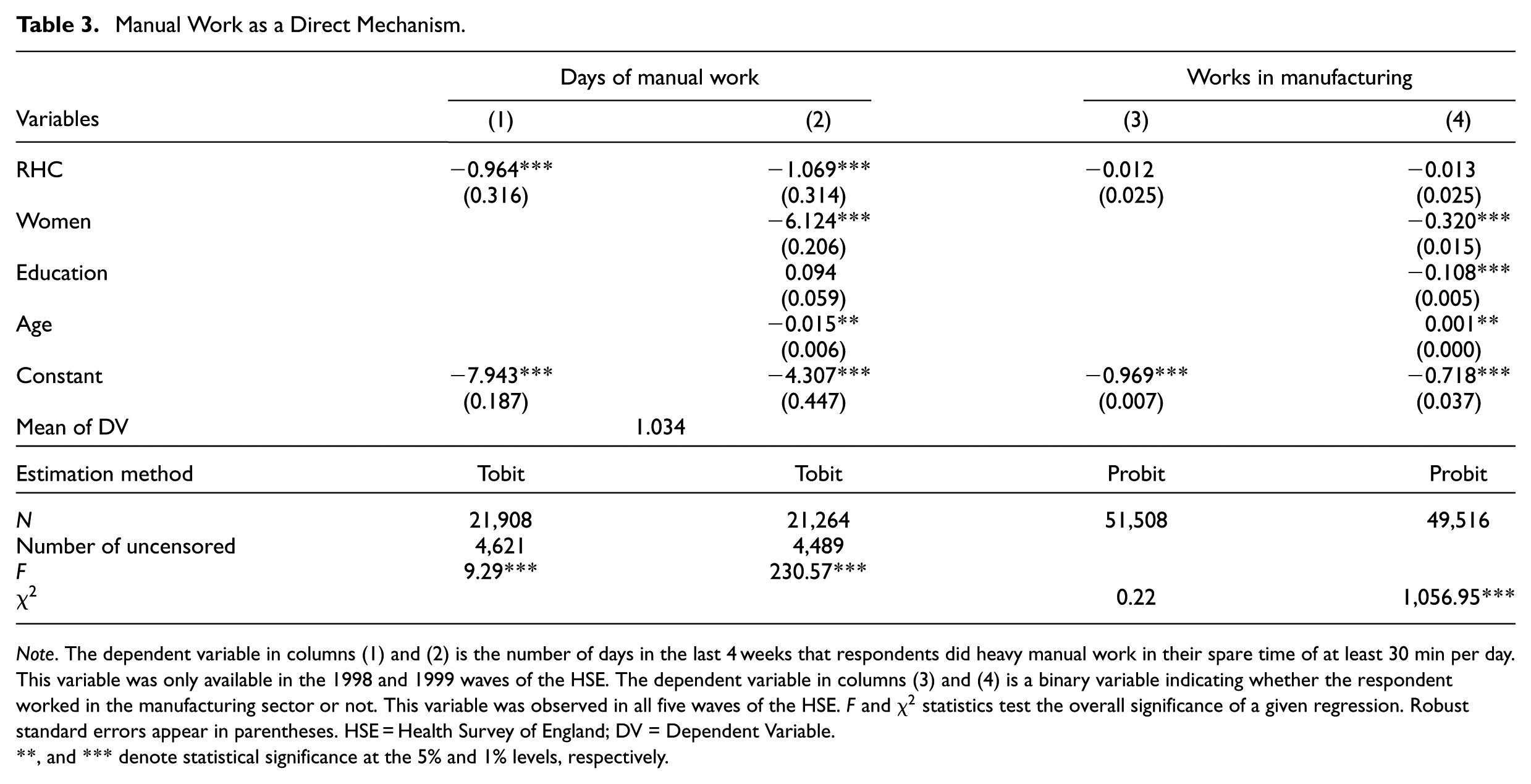
Note. The dependent variable in columns (1) and (2) is the number of days in the last 4 weeks that respondents did heavy manual work in their spare time of at least 30 min per day. This variable was only available in the 1998 and 1999 waves of the HSE. The dependent variable in columns (3) and (4) is a binary variable indicating whether the respondent worked in the manufacturing sector or not. This variable was observed in all five waves of the HSE.
, and *** denote statistical significance at the 5% and 1% levels, respectively.
Exploring further the direct “physical” mechanism of demanding work, one might wonder whether the insignificant results for All entrepreneurs in the first columns of Table 2 might simply reflect the inclusion in the sample of people who work part-time. Such people might be able to neutralize the effects of RHC by working a light schedule. If that is the case, removing part-timers from the sample could change the results in Table 2. To check this possibility, I reran the RDD analysis by excluding part-time workers, who are defined in the HSE as working 30 hr per week or fewer. The results are presented in Table 4. They show that the exclusion of part-time workers slightly strengthens the impact of the CAA on RHC. In other respects, however, the results remain qualitatively unchanged.
Impacts of the CAA: Full-Time Workers Only.
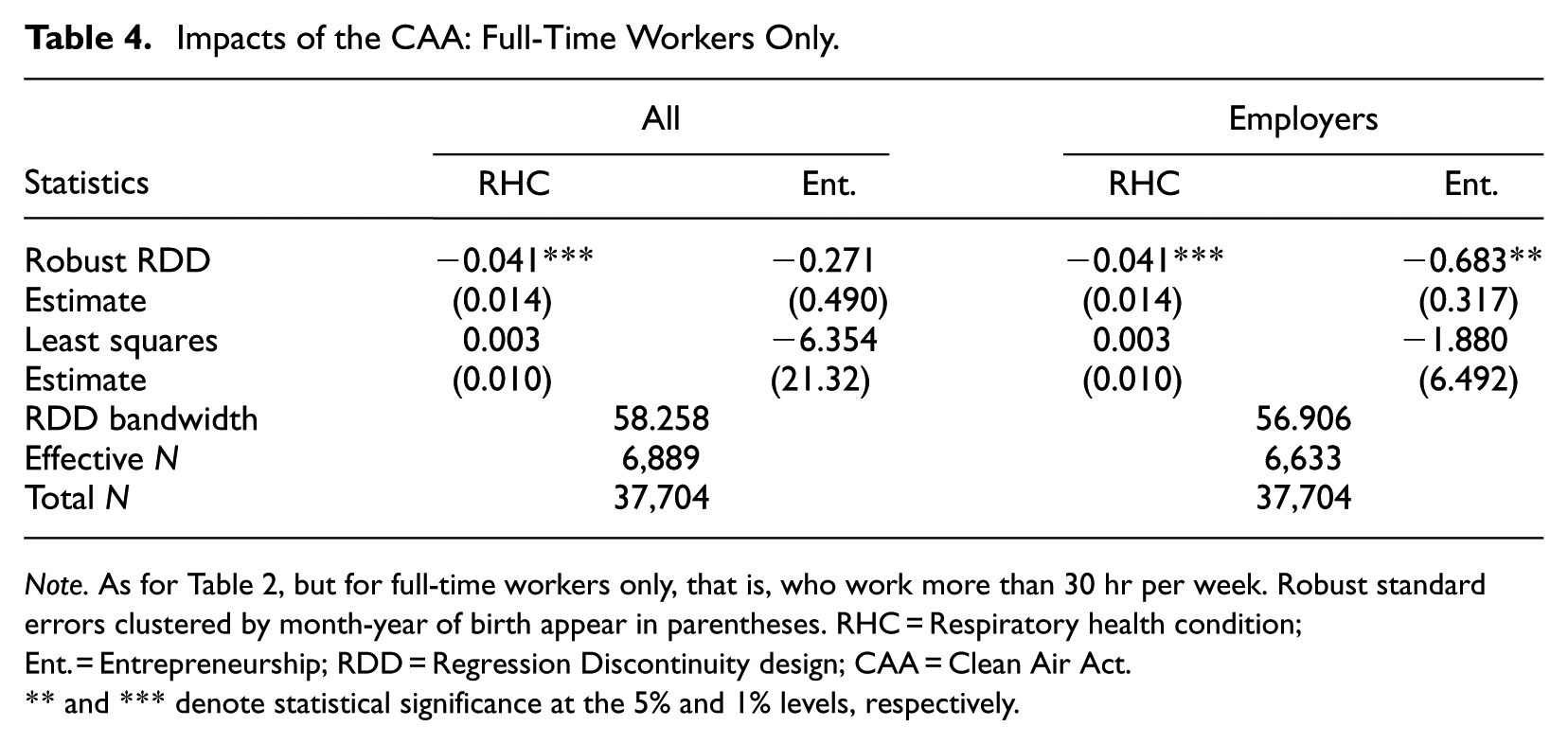
Note. As for Table 2, but for full-time workers only, that is, who work more than 30 hr per week. Robust standard errors clustered by month-year of birth appear in parentheses. RHC = Respiratory health condition; Ent. = Entrepreneurship; RDD = Regression Discontinuity design; CAA = Clean Air Act.
and *** denote statistical significance at the 5% and 1% levels, respectively.
Thus, I have found that while having a respiratory health system condition deters people from becoming employer entrepreneurs, it does not significantly affect solo self-employment. I next investigate whether it affects whether one works at all rather than being economically inactive. Thus, define a binary variable Earner which equals 1 if an individual is earning as an employee or as an entrepreneur of any kind, and 0 if not. Rerunning the RDD analysis but replacing the entrepreneurship measures with Earner, the first-stage estimates are once again statistically significant [
RDD Validity Tests and Sensitivity Checks
Several validation and falsification checks can be performed to check the plausibility of the identifying assumptions underpinning the RDD. These include manipulation tests in the running variable, placebo cutoffs, sensitivity to observations near the cutoff, and covariate balance around the cutoff. Supplemental Appendix B provides details of these tests. In brief, they all uphold the assumptions of the RDD, confirming its validity.
An additional validity test of interest concerns placebo health variables. As noted above, while the CAA is expected to affect RHC, it is not expected to affect the other health conditions listed in Table 1. If the RDD is valid, these placebo checks should not exhibit discontinuities at the time of implementation of the CAA. Table 5 presents the results for these checks. Sure enough, the results bear this out in all cases except one: having a nervous system health condition—whose marginal significance disappears in any case once a Bonferroni correction is applied.
Placebo Health Tests.
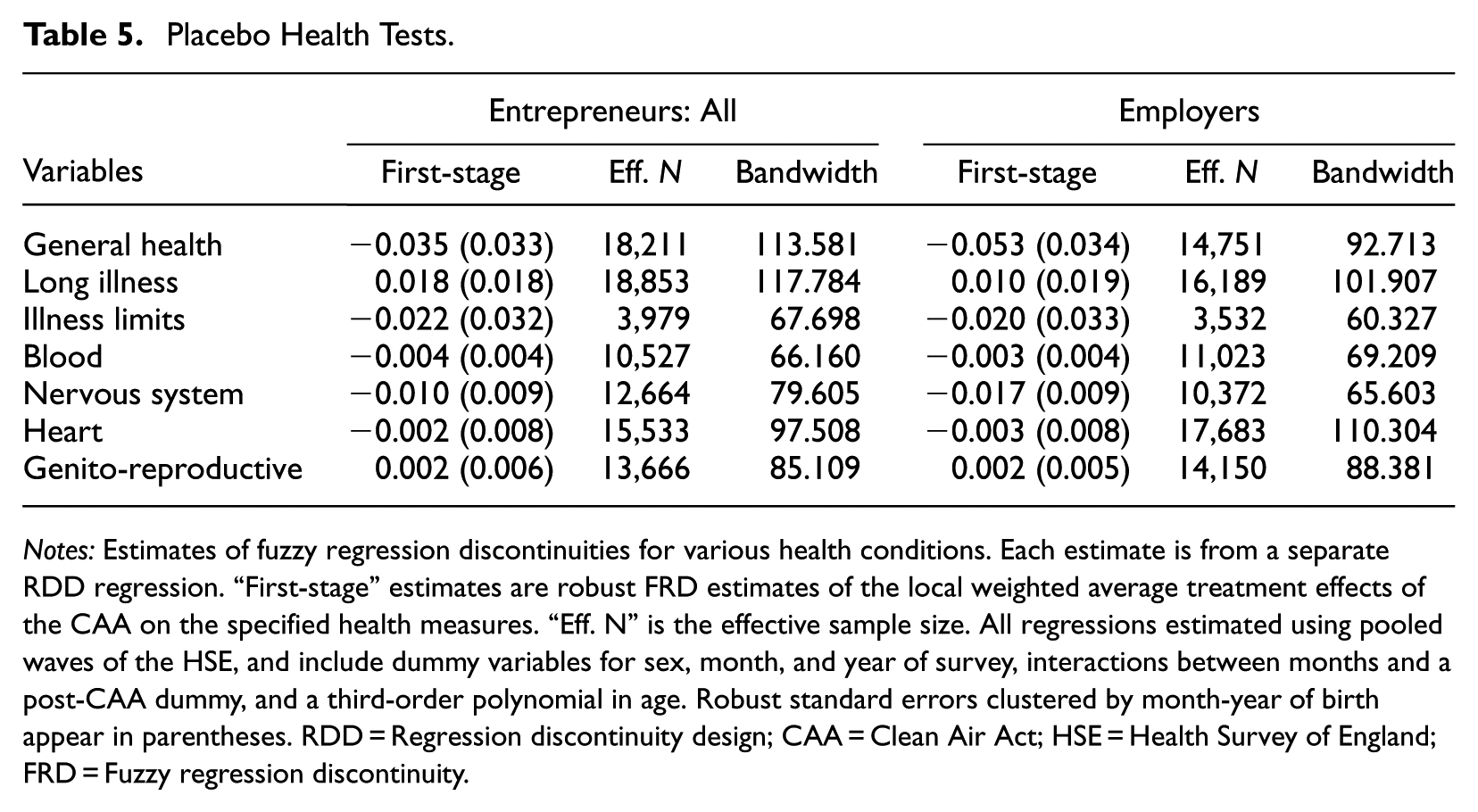
Notes: Estimates of fuzzy regression discontinuities for various health conditions. Each estimate is from a separate RDD regression. “First-stage” estimates are robust FRD estimates of the local weighted average treatment effects of the CAA on the specified health measures. “Eff. N” is the effective sample size. All regressions estimated using pooled waves of the HSE, and include dummy variables for sex, month, and year of survey, interactions between months and a post-CAA dummy, and a third-order polynomial in age. Robust standard errors clustered by month-year of birth appear in parentheses. RDD = Regression discontinuity design; CAA = Clean Air Act; HSE = Health Survey of England; FRD = Fuzzy regression discontinuity.
A key identifying assumption of any natural experiment is that no other events occurred at the cutoff date that could have been responsible for the changes attributed to the CAA. Thus, one can ask: Did some other legal reform or societal change occur around the same time, which could potentially explain my findings instead of the CAA? The strongest candidate I could find was the Housing Subsidies Act of 1956, which prioritized the building of new housing to replace slum dwellings. While newer accommodation might be expected to improve health in general, there is no reason to believe that it improved respiratory health specifically. In any case, the number of new homes built as a result of this policy accounted for only a small fraction of the total housing stock, suggesting any impact would be small. Indeed, testing this possibility, using both general health and RHC variables as outcome variables, and placebo cutoff dates for up to 24 months before and after July 1957, failed to uncover any impacts (see Supplemental Appendix B2, for details.)
Other legislative reforms passed in 1956 are even less likely to affect general health, let alone RHC specifically. Thus, the Education Act of 1956 only affected Scotland, which contains just one-tenth of the British population; and even then, it only set regulatory standards for state schools, which are unlikely to have affected health in general, let alone RHC specifically. The same point applies to the introduction of commercial TV and other changes around this time. I also searched for 1957 legislation that might also have affected RHC, but found no plausible candidates. Thus, while one can never rule out the possibility of a confounding alternative change that coincided with the CAA, there is no reason to think it poses a major problem in this study.
While the foregoing evidence bolsters confidence in the validity of the FRD, it is silent about the specific, technical, modeling choices employed in the estimation procedure. These choices include: the polynomial order of the local estimator; the selection of the bandwidth for the localized estimation; the kernel weighting scheme; and the omission of predetermined covariates (Cattaneo et al., 2019). Supplemental Appendix C summarizes details of sensitivity checks of these choices. As is shown there, different specification choices make little or no difference to the results.
In summary, I conclude that the main results reported in the text appear to be both valid and broadly robust to different econometric specification choices.
Discussion
This paper analyzed a natural experiment in the form of a landmark legal change: the 1956 British CAA. This law exogenously reduced airborne pollution across the whole of Britain. Drawing on scientific evidence linking in utero and early childhood exposure to air pollution with the development of RHCs in adulthood, this paper analyzed the CAA using a fuzzy RDD to identify the causal impact of respiratory health on adults’ engagement in entrepreneurship.
The results show that the CAA substantially and significantly improved adult respiratory health—which in turn significantly increased subsequent engagement in employer entrepreneurship. Using the theoretical lens of the JD-R model, this finding can be understood in terms of RHCs hindering individuals’ abilities to undertake an especially demanding type of entrepreneurship associated with running larger firms in which employees must be hired, supervised, and managed. In contrast, RHCs seemed neither to impede people from venturing on their own account, nor from engaging in paid work more generally. To the best of my knowledge, this finding is not only a novel addition to the literature on physical health and entrepreneurship but also confirms the value of distinguishing conceptually between solo and employer entrepreneurs—an insight worth exploring further in future research on entrepreneurship and health.
Although the CAA was passed a long time ago, the findings of this study remain relevant and topical today. Coal combustion continues to be the principal source of energy generation worldwide, as well as a major ongoing global health issue. Thus, despite its historical nature, the lessons of the CAA remain pertinent, especially in countries continuing to suffer from high levels of air pollution, notably India and China (Zhang et al., 2014). Another novelty of the present study is its estimation of long-term impacts of adverse environmental conditions on health and entrepreneurship. This reflects the persistent health impacts of pollution (Bharadwaj et al., 2016). An important contribution of this research is therefore to focus attention on the long-term impacts of environmental damage, which can affect not only human health, but also possibly wealth-creation efforts far into the future.
The findings in this article might also interest policymakers seeking to promote entrepreneurship by job creators specifically. They suggest that cutting air pollution may have an additional long-term benefit over and above promoting better health. In that respect, the present research connects with a growing literature on how background conditions in childhood and adolescence shape future entrepreneurship choices among adults. For example, prior work has explored the influence on adult entrepreneurship of neighborhood segregation during adolescence (Wixe, 2020), the degree of nurturing and stability in families during childhood (Yu et al., 2023)—and childhood adversity caused by exogenous shocks such as the Great Chinese Famine (Cheng et al., 2021) and the Vietnam War (Churchill et al., 2021). Future research could probe the role of other exogenous changes to early-life health outcomes to trace out their influence on later-life choices relating to entrepreneurship, too.
This research is subject to several limitations. First, it focuses on respiratory health, which is only one aspect of human health. Future research could investigate the implications of other specific health conditions for entrepreneurial processes and outcomes. Such a strategy might more clearly identify the precise channels by which physical health impacts entrepreneurship than a broader outcome like general health. I note too that while this article focuses on the impacts of an individual’s physical health on entrepreneurship, it does not speak to the larger literature of entrepreneurship’s impact on health, especially on mental health (Ahn, 2020; Gonçalves & Martins, 2021; Nikolova, 2019; Nikolova et al., 2020; P. C. Patel et al., 2019; Shepherd & Patzelt, 2015; Toivanen et al., 2019; Zhou et al., 2021). The mechanisms at work there are different to those explored here, and conclusions drawn from this study should not be carried over to that forum of inquiry.
A second limitation relates to empirical concerns about causal identification, including non-instantaneous implementation of the CAA and time lags between the CAA and adult outcomes. The historical context is complex, with the CAA being one of several reforms and social changes occurring in the late 1950s. After weighing these concerns, I do not believe that they seriously threaten the identification strategy of the paper; but it is prudent to interpret the results with caution. Also, the fact that the U.K. did not collect accurate national pollution data until the 1970s (Brimblecombe, 1987), while the HSE lacks data about respondents’ places of birth, limits estimates to average treatment effects, reducing their precision, and masking heterogeneity among affected cases. Fortunately, the lack of local data does not induce bias in the FRD estimates; and if anything, it may understate the statistical significance of the findings.
Another challenge to causal inference is that the CAA might have affected entrepreneurship outcomes not only via health but also through some other channel, such as neurological benefits of lower pollution, better education outcomes, and changes to lifestyles and industry structure, among others. If so, the exclusion restriction underpinning the paper’s identification strategy would be violated. Unfortunately, it is not possible to conclusively rule out these threats to identification. While this is true of all instrumental variables applications, it is still worth acknowledging it as a limitation of the present study.
Third, data limitations constrain the empirical work in several respects. For example, ideally one might want to investigate the impact of health, measured at time
Also, the HSE data are not rich enough to investigate what it is about employer entrepreneurship that deters some people with RHCs from choosing it. For example, is it the expected difficulty of managing others, working longer hours, or something else? Future research might not only explore this question, but also whether key aspects of employer heterogeneity (e.g. team strength, delegation practices, nature of the industry, etc.) attenuate the negative impact of poor health on employer status. That would complement a growing body of recent research that seeks to better understand employer entrepreneurship in general (Caliendo et al., 2022; Su et al., 2022). Like us, that research has yet to fully elucidate the managerial processes used by employer entrepreneurs, and how they might be affected by physical health: future research is needed to open this particular “black box.”
The HSE also lacks data on several other outcome variables, such as venture performance, as well as process variables and potential moderators. These include parental socioeconomic status, since exposure to pollution may be affected by parental resources (see Grönqvist et al., 2020, p. 3404). Interestingly, other research has also linked this variable to the decision to engage in solo versus employer entrepreneurship (Su et al., 2022). Moreover, future research might also explore education, risk preferences, cognitive abilities, and social capital formation as pathways through which early-life shocks influence entrepreneurship in later life.
A fourth limitation is that RDDs only analyze historical shocks for which data are available, not shocks that the researcher might ideally like to investigate. Thus, the CAA is for example unsuitable for identifying impacts of adult mental health on entrepreneurship—the subject of considerable recent scholarly attention (Stephan et al., 2020). Subsequent research could search for different historical shocks, and apply quasi-experimental methods to explore how they affect different health conditions and thereby entrepreneurship.
Finally, future work could also use natural experiments to assess impacts on entrepreneurship of public health policies. Building on research linking health insurance coverage and entrepreneurship (Fossen & König, 2017; Wolfe & Patel, 2019), researchers have begun to exploit natural experiments in relation to policies that have increased access to public health insurance, both in the United States (Bailey, 2017) and East Asia (Liu & Zhang, 2018). These studies generally report a positive linkage between access to health insurance and entrepreneurship. Further research along these lines promises to furnish a deeper understanding of how health outcomes, and possibly also public health policies which influence those outcomes, affect entrepreneurship.
Supplemental Material
sj-pdf-1-etp-10.1177_10422587251400220 – Supplemental material for Entrepreneurship and Physical Health: A Natural Experiment Based on the 1956 British Clean Air Act
Supplemental material, sj-pdf-1-etp-10.1177_10422587251400220 for Entrepreneurship and Physical Health: A Natural Experiment Based on the 1956 British Clean Air Act by Simon C. Parker in Entrepreneurship Theory and Practice
Footnotes
Declaration of Conflicting Interests
The author declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author received no financial support for the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
Notes
Author Biography
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
