Abstract
In the current study, mycotoxicoses of ruminants and horses are reviewed, with an emphasis on the occurrence of these diseases in South America. The main mycotoxicoses observed in grazing cattle include intoxications by indole-diterpenoid mycotoxins (Paspalum spp. contaminated by Claviceps paspali, Lolium perenne infected by Neotyphodium lolii, Cynodon dactylon infected by Claviceps cynodontis, and Poa huecu), gangrenous ergotism and dysthermic syndrome (hyperthermia) caused by Festuca arundinacea (syn. Festuca elatior) infected by Neotyphodium coenophialum (syn. Acremonium coenophialum), and photosensitization in pastures contaminated by toxigenic Pithomyces chartarum. Other mycotoxicoses in grazing cattle include slaframine toxicity in clover pastures infected by Rhizoctonia leguminicola and diplodiosis in cattle grazing in corn stubbles. The mycotoxicoses caused by contaminated concentrated food or byproducts in cattle include poisoning by toxins of Aspergillus clavatus, which contaminate barley or sugar beetroot by-products, gangrenous ergotism or dysthermic syndrome caused by wheat bran or wheat screenings contaminated with Claviceps purpurea, and acute respiratory distress caused by damaged sweet potatoes (Ipomoea batatas). The main mycotoxicosis of horses is leukoencephalomalacia caused by the fumonisins B1 and B2 produced by Fusarium spp. Poisoning by C. purpurea and F. elatior infected by N. coenophialum has also been reported as a cause of agalactia and neonatal mortality in mares. Slaframine toxicosis caused by the ingestion of alfalfa hay contaminated by R. leguminicola has also been reported in horses.
Introduction
Mycotoxicoses are important diseases of ruminants and horses. In South America, where pastoral farming systems predominate, there have been a number of studies published regarding mycotoxicoses of ruminants and horses; however, most of this information has been published in Spanish or Portuguese in journals of limited circulation or in meeting proceedings. The current review reports the epidemiology, clinical signs, and pathology of the main mycotoxicoses affecting livestock, mainly in South America, with an emphasis on the information necessary for the diagnosis of poisoning (Tables 1, 2). Comparisons are also made with the occurrence of the same mycotoxicoses on other continents. A description of the details of the laboratory techniques for toxin detection is beyond the scope of this review.
Main features for the diagnosis of mycotoxicosis in grazing livestock in South America.*
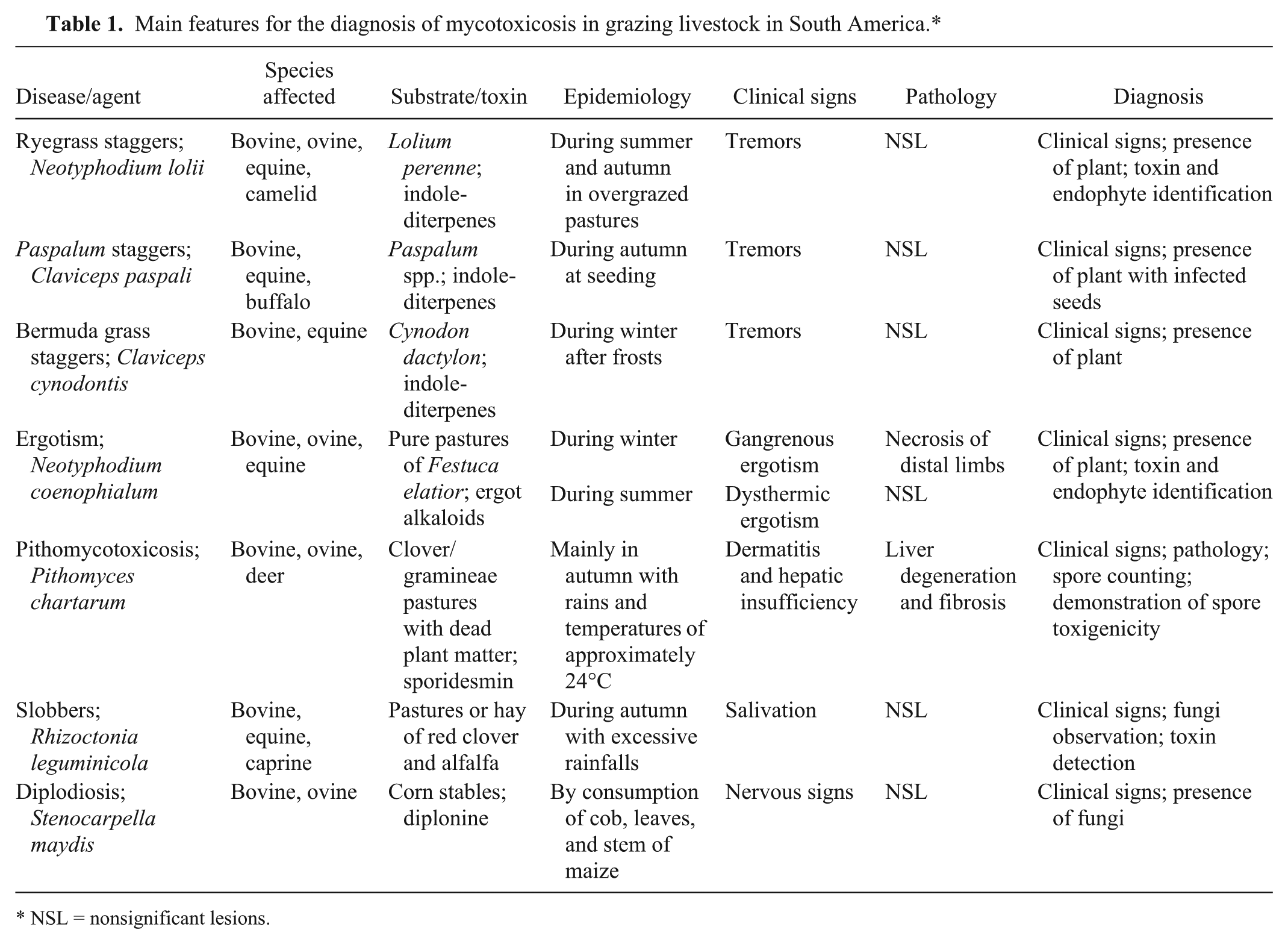
NSL = nonsignificant lesions.
Main features for the diagnosis of mycotoxicosis in livestock ingesting grains or grain by-products in South America.*
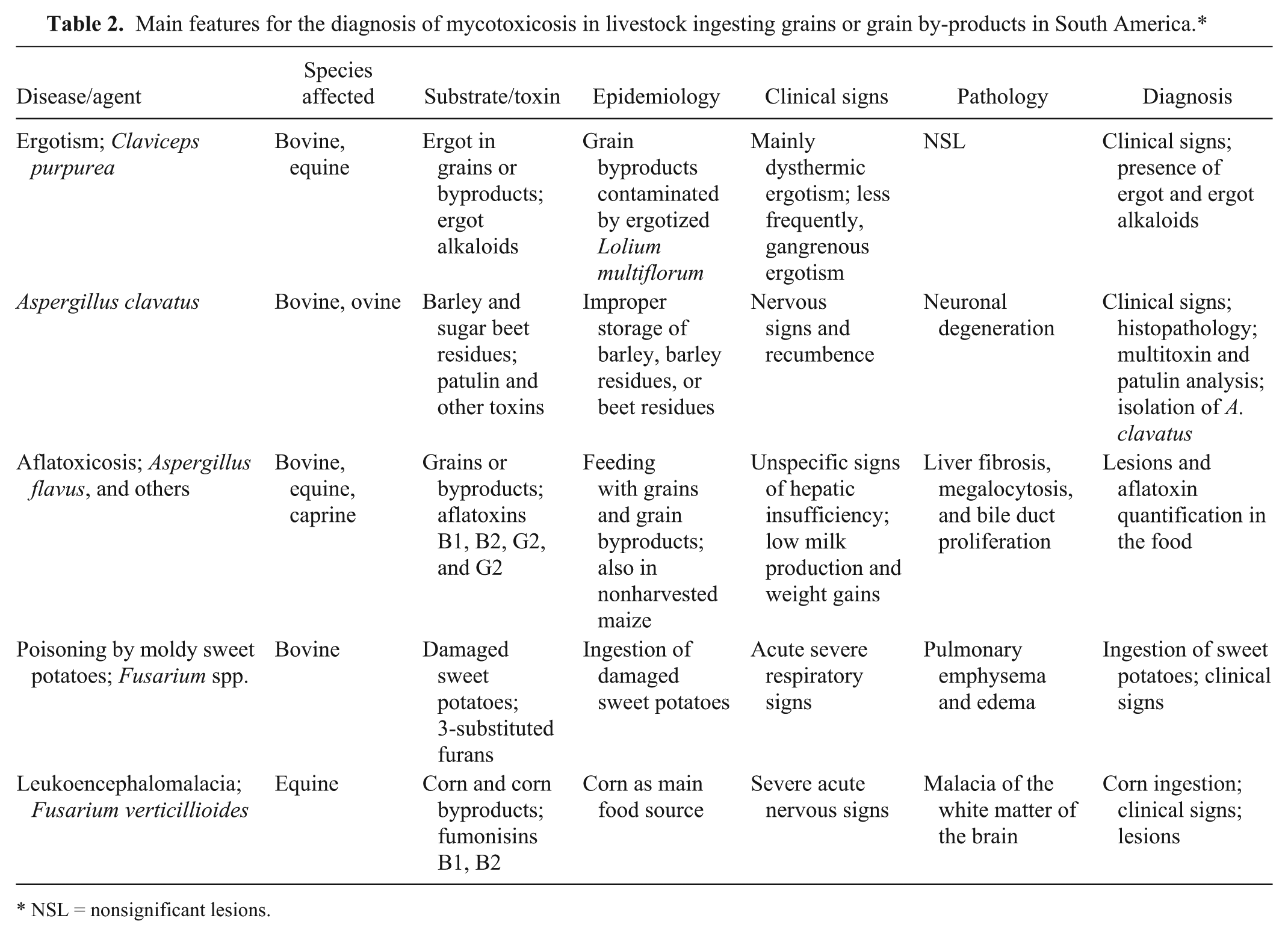
NSL = nonsignificant lesions.
Poisoning by indole-diterpenoid mycotoxins
The 3 main grasses that cause tremorgenic syndrome due to the presence of indole-diterpenoid alkaloids are Paspalum spp., Cynodon dactylon, and Lolium perenne. Paspalum staggers occurs when Claviceps paspali invades the unfertilized ovaries of Paspalum spp. during flowering time, replacing them with a mass of fungal tissue named sclerotia (Fig. 1A). 66 The main indole-diterpenoid tremorgens inC. paspali are paspalinine and paspalitrems A–C. 17 This mycotoxicosis occurs in southern Brazil, 66 Uruguay, 56 Argentina, 36 the United States, 17 Australia, 39 New Zealand, 80 Europe,5,44 and South Africa.9,81 Several species of Paspalum can be infected by C. paspali, including Paspalum dilatatum Poiret, Paspalum notatum Flügge, Paspalum distichum L. (syn. Paspalum paspalodes [Michx.] Scribne), Paspalum vaginatum Sw, Paspalum scrobiculatum L., and Paspalum urvillei Steud. In South America and other countries of the southern hemisphere, poisoning occurs from the end of February until early June (i.e., between the end of summer and the start of autumn), when Paspalum spp. is seeding. The disease occurs mainly in rice stubbles 1–2 years after harvest, in cultivated pastures 3–4 years after establishment when the Paspalum spp. substitute the species planted, and in natural pastures with highly fertile soil, such as marshy or irrigated areas.36,56,66 Cattle of various ages and categories, as well as buffalo 5 and horses, 15 can be affected.

Poisoning by consumption of C. dactylon L. has been reported in cattle in Uruguay,57,70 Argentina, 46 the United States, 16 and South Africa 81 and in horses in California. 16 In South Africa, it was determined that the toxicity of this species was due to infection with Claviceps cynodontis, which contains a mixture of indole-diterpenes, of which paspalitrems A and B, as well as paspaline and paspalinine, represented major constituents. 81 In the South American countries, the disease occurs mainly in the winter months (July and August) when the seeding plant is dry due to severe frosts. Cynodon dactylon is a weed of pastures, crops, and degraded areas. Poisoning occurs mainly in pastures severely invaded by C. dactylon, where this plant becomes the only grass available.
Ryegrass staggers is caused by the endophytic fungi Neotyphodium lolii (syn. Acremonium lolii) in perennial ryegrass (Lolium perenne).75,80 The main indole-diterpenoid tremorgens found in L. perenne are paxilline and lolitrems, primarily lolitrem B,23,30,71,80 which are believed to act on γ-aminobutyric acid receptors disrupting neuromuscular control. 43 Neotyphodium lolii also produce ergopeptide alkaloids, which have been associated with reduced milk production due to prolactin depression in cattle and sheep, hyperthermia and heat stress in sheep during the summer, and other signs such as reduction of weight gains and fecal contamination of wool (dags) in lambs (Duringer JM, DeLorme MJM, Lehner A, et al.: 2007, A review of the ergot alkaloids found in endophyte-infected tall fescue and perennial ryegrass and their metabolism after ingestion by livestock. In: Proceedings of the 6th International Symposium on Fungal Endophytes of Grasses: no. 13. Fungal endophytes of grasses, ed. Popay AJ, Thom ER, pp. 377–382. Dunedon New Zealand Grassland Association, New Zealand).23,30,80 Neotyphodium lolii also produces peramine, which confers resistance against insects including the Argentine stem weevil (Listronotus bonariensis).23,71,80 Ryegrass staggers occurs frequently in New Zealand and Australia but has been reported in the United States, Europe, South Africa, and Argentina in sheep, cattle, deer, and horses.47,80 The effects of ryegrass staggers are most serious during the summer and autumn, when the shortage of forage forces livestock to ingest the basal sheath region of the plant, which contains the highest lolitrem concentrations. The poisoning can also be caused by ryegrass hay and ryegrass seed screenings. Neotyphodium lolii is transmitted only through the seeds, so the infection is not spread between plants. However, because the infected plants are more resistant to drought and insect attacks, they produce a greater number of infected seeds, and the infection occurs more frequently in the new plants, increasing the toxicity of the pasture over time.23,39
Another endophyte-related disease associated with tremoring in South America is poisoning by Poa huecu, which has been reported in Argentina. Paxilline has been identified in this type of poisoning, suggesting that the tremors are caused by indole-triterpenoid alkaloids (Towers RN: 1994, Cornezuelo e endofitos como causa de síndromes nerviosos y asoleamento en especies pecuarias [Ergot and endophytes causing nervous diseases and hyperthermia in livestock]. In: Buiatrics Uruguayan XXII Conference. Centro Médico veterinário Paysandú, Uruguay, pp. C1–C10. In Spanish).
Poisoning by indole-diterpenoids contained in Paspalum spp., C. dactylon, and ryegrass cause similar clinical signs, which are characterized initially by fine tremors and discrete head nodding, and can be exacerbated by excitement or movement. Later, the animals display cerebellar ataxia with severe tremors, uncoordinated gait with rigid legs, hypermetria, swaying when standing, and a wide-based stance. When affected animals are driven or startled, they can fall to either side, forward or backward, sometimes into unusual positions, and occasionally paddle violently during vigorous attempts to rise (Fig. 1B). After a period of rest, the animals usually rise unassisted. In the more affected animals, tremors became generalized. Generally, the appetite is maintained, but weight loss occurs. Hypersensitivity to noise or movement is also observed. Severely affected animals may become recumbent, with generalized tremors, opisthotonus, nystagmus, and salivation. When the animals are removed from pastures, full regression of clinical signs occurs in 7–15 days. Some animals have died as a consequence of accidents or while remaining recumbent.36,46,56,57,66,80
No gross lesions are observed following intoxication, but in the case of Paspalum staggers, many Paspalum seeds are observed in the abomasum contents. Most cases have no histological lesions, but some cases with a more prolonged clinical manifestation period have cerebellar lesions, with degeneration and loss of Purkinje cells and the presence of axonal spheroids in the granular layer.38,66
This mycotoxicosis is diagnosed by observation of the characteristic clinical signs and the presence of Paspalum spp. infected by C. paspali, C. dactylon, or L. perenne. The main diseases to be considered during differential diagnosis is poisoning by Ipomoea asarifolia, which causes an identical tremorgenic syndrome in ruminants in northeastern Brazil, and poisoning by Phalaris spp., which also causes tremors in ruminants in South America 62 and other countries. In Phalaris spp., the presence of a characteristic pigmentation of the brain helps in the differential diagnosis of poisoning. Similar signs are observed following the ingestion of crops or their byproducts containing indole-diterpenoid toxins produced by fungi of the genera Aspergillus and Penicillium. 16 Other diseases that should be considered in the differential diagnosis are hypomagnesaemia, poisoning by swainsonine-containing plants, and cerebellar degeneration caused by Solanum spp. 62
Currently, there is no effective treatment for poisoning. The whole herd, or at least animals showing clinical signs, should be gently removed from the infected pastures. In the case of Paspalum staggers, the prevention of intoxication should focus on the suppression of inflorescence. Slashing or mowing may be used to remove seed heads. Paspalum spp. are tolerant of heavy grazing, so high grazing pressure should be maintained during the summer to prevent heavy seeding. High grazing pressure also helps decrease soil contamination by ergot and prevents heavy infection for the next year (Riet-Correa F, Rivero R, Dutra F, et al.: 2007, Micotoxicosis en animales domésticos en pastoreo [Mycotoxicosis in grazing domestic animals] In: Jornadas Uruguayas de Buiatría, Paysandú. Buiatrics Uruguayan XXXV Conference, Paysandú, Uruguay, vol. 35, pp. 116–131). The only way to prevent C. dactylon poisoning is to avoid grazing livestock in severely infected pastures during the winter. Nevertheless, the risk of C. dactylon poisoning is very low, because despite the numerous pastures invaded by this species in South America, poisoning is rare. The prevention of ryegrass staggers is based on the avoidance of heavy grazing during the dry season, thereby forcing livestock to graze the lower part of the pastures. Pastures that are at least 30 cm high can be considered nontoxic. Pastures infected with L. perenne can be replaced by noninfected ryegrass, but this measure is unsuccessful because compared to infected ryegrass, noninfected ryegrass is more susceptible to environmental conditions and less resistant to nematodes and insects. As a consequence, noninfected ryegrass dies and is substituted by endophyte-infected plants, which originate from seeds remaining in the soil. Another possible solution is to replace toxic ryegrass with seeds infected by a strain of N. lolii, which do not produces penitrems. 23 AgResearch Ltd. developed AR6 novel endophyte, which produces peramine and ergovaline to control the Argentine stem weevil and African black beetle (Heteronychus arator), but does not produce lolitrem B; however, lambs on AR6 pasture could be more vulnerable to heat stress due to ergovaline than lambs grazing endophyte-free pastures. 1
Ergotism
Ergot alkaloids produced by Claviceps purpurea and Festuca arundinacea Scribe (syn. Festuca elatior L.; tall fescue) infected with Neotyphodium coenophialum (syn. Acremonium coenophialum) cause diseases in ruminants and horses, including gangrenous ergotism (also known as fescue foot in cases of F. elatior poisoning), dysthermic ergotism (also known as summer toxicosis, hyperthermia, idiopathic bovine hyperthermia, and dysthermic syndrome), and a reproductive form (causing agalactia or hypogalactia).6,10,35,59,65,77,80 Fescue poisoning has also been associated with necrosis of the abdominal fat in cattle. 78 Nervous ergotism caused by C. purpurea, as it is known in human beings, has not been fully documented in domestic animals, and the reported cases were most probably caused by indole-triterpene alkaloids in Claviceps paspali.
Claviceps purpurea is a fungus that infects the ovaries of crops and grass seeds, forming an sclerotium (ergot), which is larger than the seeds, with a black or dark brown color and a hard consistency (Fig. 2A, 2B). In South America, the fungus can affect several species of grasses including Holcus lanatus, Setaria spp., Polypogon chilensis (syn. Chaetotropis chilensis), Poa pratensis, Festuca spp., and Phalaris spp., but most outbreaks in the region have been associated with the ingestion of grains or their byproducts contaminated with Lolium multiflorum L. (annual ryegrass) infected with C. purpurea. 59 Lolium multiflorum is a weed that affects winter cultures, mainly wheat; hence, the main cause of ergotism in cattle in Uruguay is the contamination of wheat bran and wheat screenings contaminated with annual ryegrass seeds infected by C. purpurea (Fig. 2B). Oats harvested from areas severely contaminated by C. purpurea–infected ryegrass have been responsible for outbreaks of agalactia and neonatal mortality in horses. 65 Ergotism has also been reported in animals grazing on ryegrass pastures severely contaminated by C. purpurea. 59

The toxicity of F. elatior is due to infection by the endophyte fungus Neotyphodium coenophialum, which produces ergot alkaloids. 77 This mycotoxicosis is very important in the southwestern United States but has also been reported in several other countries,10,80 including Argentina (Villahoz MD, Moras EV, Barboni AM, et al.: 1984, Reproductive problems of pregnant mares grazing fescue pastures in Argentina. In: Proceedings of 10th Congress on Animal Reproduction and Artificial Insemination, vol. 2, pp. 100–102, June 10–14, Urbana-Champaign, Illinois)35,50 and Uruguay. 61 The endophyte is transmitted only through the seed, but because noninfected plants are less resistant to drought and environmental stress, they die and are replaced by endophyte-infected plants originating from seeds that remain in the soil. 80
Ergot alkaloids are generally classified in 2 main groups: ergoline alkaloids, which include lysergic acid, lysergol, lysergic, acid amide, and ergonovine; and ergopeptine alkaloids, which include ergotamine, ergocristine, ergosine, ergocryptine, ergocornine, and ergovaline. Ergovaline is probably the most active ergot alkaloid produced by N. coenophialum, and the ergopeptine alkaloids ergotamine, ergocristine, ergosine, ergocornine, and ergocryptine are the main toxins in C. purpurea (Duringer JM, et al.: 2007, A review of the ergot alkaloids).24,77
The vasoconstrictive effect of ergot alkaloids through interactions with dopaminergic, adrenergic, and serotonergic receptors cause constriction of the arterioles, resulting in gangrenous ergotism or hyperthermia. 24 In temperate climates, gangrenous ergotism occurs during the winter, and dysthermic ergotism occurs during the summer. In cold climates, vasoconstriction causes ischemia, endothelial degeneration, thrombosis, and ischemic necrosis. 59 At temperatures higher than 25°C, vasoconstriction of peripheral blood vessels causes reduced blood flow to the skin, reducing heat loss when ambient temperatures are high and leading to heat stress and hyperthermia.16,59 In the reproductive form of ergotism in horses, hypogalactia or agalactia occurs as a result of decreased prolactin secretion and inhibition of mammary gland development at the beginning of lactation or as a result of lower milk production during lactation.6,24,77 A 2011 review is available concerning the endocrine disruptive effects of ergopeptine alkaloids on lactogenesis and steroidogenesis on pregnant mares. 24 Fibrosis and thickening of placenta are most likely due to vasoconstriction of the placental vessels.6,65
Gangrenous ergotism and hyperthermia caused by C. purpurea31,59 and F. elation35,61 have been reported frequently in cattle in Uruguay, Argentina, and southern Brazil. The reproductive form of ergotism has been diagnosed in horses that ingested C. purpurea in southern Brazil 65 and Uruguay 59 and in horses that ingested F. elatior in Argentina (Villahoz MD, et al.: 1984, Reproductive problems of pregnant mares grazing fescue pastures). In Uruguay and southern Brazil, morbidity due to hyperthermic ergotism varies from 25% to 70%, and, generally, spontaneous deaths do not occur.31,59 The morbidity of fescue foot can vary from 6% to 80%, depending on the amount of tall fescue grass and the degree of contamination. Fertilization with nitrogen and drought stress can increase the toxicity of the grass. 6 Lower weight gains have also been observed in cattle without clinical signs. 80 Poisoning occurs at different times of the year, with plants at different stages of growth. In cattle in Uruguay and Argentina, the gangrenous form occurs in the winter, and hyperthermic ergotism occurs in the summer. The disease does not occur in paddocks with fescue contents below 50%. 35 The occurrence of ergotism has become rare in Uruguay and Argentina, most likely due to the use of tall fescue mixed with other grasses such as clovers and ryegrass and also to the marketing of controlled seeds with endophyte infection rates of less than 5%. In outbreaks of agalactia due to C. purpurea ingestion, reported morbidity rates are 7–90%, with foal mortality rates of up to 50%. 65
In cattle, gangrenous ergotism is characterized by a dry gangrene of the limb extremities. Initial clinical signs include lameness with swelling and redness of the skin of the coronary band and fetlock, and, in dairy cattle, reduced milk production. Subsequently, the skin becomes gangrenous and shows cracks, sometimes with purulent exudate under the necrotic skin. Gangrenous lesions are separated from normal skin by a clear line. The horn also separates from the underlying tissues, the skin sloughs off, and the rupture of tendons and ligaments may result in loss of the hoof.59,61 The general condition of animals is not greatly affected, although some animals may show skin necrosis at the edge of the ears, the tip of the tail, and the udder.59,61
Dysthermic ergotism in cattle is characterized by heat stress with a high body temperature (40–42°C), rough hair, dyspnea, decreased feed intake and weight gains, reduced milk production, increased water intake, and polyuria. Diarrhea and nasal discharge are occasionally observed. When environmental temperatures increase, affected cattle seek out any shade available, stay in water ponds, and show severe respiratory distress with an extended neck, open mouth, drooling, and tongue exposition. During the hotter hours of the day, the clinical signs are more evident than during the night or on cold days. Some animals may show signs of lameness and gangrenous ergotism in the limbs, ears, and tail 30–60 days after ingestion. Death can occur when infected animals are exposed to ambient temperatures of more than 30°C. With the withdrawal of the contaminated food, the clinical signs disappear slowly over a course of 2–3 weeks. Abortions, agalactia, retained placenta, and reproductive failures such as infertility and anestrus may occur during and after the occurrence of hyperthermic ergotism.31,59,61
In cases of F. elatior poisoning in cattle, adipose tissue necrosis in the abdominal cavity has also been described. This change is detected by rectal palpation as hard masses that range from 1 cm in diameter to large masses that are only partially palpated on the dorsal surface. Such lesions, which may or may not occur simultaneously with dysthermic ergotism, may cause digestive disorders and calving problems. 78
Gangrenous ergotism is a rare disease in sheep, 34 but digestive lesions can be observed in sheep experimentally poisoned by C. purpurea. 22 Poor weight gains and hyperthermia can be observed in sheep grazing tall fescue and in lambs grazing perennial ryegrass contaminated by N. lolii, which also produces ergot alkaloids.59,80 In horses, mainly in mares during the last month of gestation, the main form of ergotism is reproductive and is characterized by a lack of mammary gland development and agalactia. In most cases, agalactia is permanent after birth, but some mares can produce milk after parturition if ergot alkaloids are removed from the food. Premature release of the chorioallantoid also occurs, and the placenta is heavier, thickened, and fibrotic and must be manually broken. Gestation may be prolonged, and some mares have dystocia. Abortion, embryonic death, and anestrus have also been reported.6,65 The foals born to affected mares are weak, without mammary reflex, and neonatal mortality can be higher than 50%. 65 Newborn foals had decreased serum triiodothyronine concentration, hypothyroidism, and signs of dysmaturity, including marked decrease in muscle mass, long fleshy hooves, and delayed eruption of incisor teeth.6,7 After the removal of food contaminated by ergot alkaloids, the frequency of agalactia, other reproductive signs, and neonatal mortality rapidly decreases. 65
Histologically, the lesions of gangrenous ergotism display coagulation necrosis of the skin and subcutaneous tissue, with proliferation of granulation tissue in the deeper layers. The muscular layer of arterioles is hyperplasic, with narrowing of the vessel lumen and of subcutaneous tissue. 59 In the reproductive form in horses, placental lesions are characterized by a thickening of the allantochorion and the degeneration of the chorionic epithelium. In foals, jaundice and enlarged, yellow livers with severe vacuolation of hepatocytes can be observed. 65 No macroscopic lesions have been reported in cases of hyperthermic ergotism in cattle. Histologically, the only lesions observed in the cases described in Brazil were pulmonary emphysema and hypertrophy of the muscular layer of the bronchioles. 31
The diagnosis of ergotism must be established by clinical signs, pathological changes, and the presence of C. purpurea sclerotia in the food or F. elatior contamination by N. coenophialum, which can be confirmed by microscopic observation of leaf sections stained with aniline blue. The determination of the number of infected plants is important for confirmation of the diagnosis and to provide an indication of the toxicity of a pasture of tall fescue. Clinical signs are likely to occur when at least 50% of the plants in a pasture are infected. Infection of 15% of the plants can lead to a reduction in daily weight gains. Milk production may be affected in some animals when the ambient temperature is high and 8% of the plants are infected. 61 However, the percentage of infected plants is not the only factor that determines the toxicity of a pasture. Other factors, such as the botanical constitution, the percentage of fescue, and the nitrogen fertilization of the pasture, as well as the duration and type of grazing animal, can influence the toxicity. The diagnosis of C. purpurea presents difficulties when animals are fed with products or ground-based grains, in which the milled sclerotia cannot be identified. In such cases, laboratory tests are needed to detect the presence of C. purpurea or ergot alkaloids. Ergot alkaloids can be identified in food by thin-layer chromatography, enzyme-linked immunosorbent assays, and high-performance liquid chromatography.10,33 Urinary ergot alkaloids can be determined in animals that are still ingesting the contaminated food. 10
After diagnosis of the disease, grazing animals should be removed from fescue pastures infected by N. coenophialum or ryegrass pastures contaminated by C. purpurea. Contaminated feed should also be removed from penned animals. Treatment should be symptomatic; gangrenous lesions are slowly reversible in milder cases but are not reversible in severe cases. For the prevention of gangrenous ergotism, grains or byproducts should be inspected for the presence of C. purpurea. As a weed in crops, L. multiflorum should be controlled by the use of herbicides, which is difficult due to increasing resistance to herbicides. Crop seeds should be free of ryegrass seeds. In areas invaded by ryegrass, the prevention of seeding will prevent soil contamination by ergot, which can overwinter to infect ryegrass the following year.
Endophyte-free fescue seeds are available or can be obtained by treating seeds with fungicides or by using seeds after 12–15 months of storage. In Uruguay, fescue seeds must have infection rates below 5%. 61 Endophyte-free fescue provides excellent livestock performance, but is less resistant to drought and insect attacks. 80 If endophyte-free fescue is planted in an area previously occupied by infected fescue, the culture will rapidly revert to an endophyte-infected pasture as seeds in the soil germinate and the endophyte-free plants die. 80 A better approach is the use of fescue infected by endophytes, called novel endophytes, which produce little or no ergot alkaloids but still produce toxins against insects.3,80 The only way to use toxic pastures is to allow grazing only for short periods, alternating grazing fescue pastures with other species. However, one should consider the possibility of lower weight gains and a drop in production.
Intoxication by Pithomyces chartarum (pithomycotoxicosis)
Pithomyces chartarum is a saprophytic fungus distributed in temperate, subtropical, and tropical regions. It is usually found on dead vegetable matter at the base of the pasture. The spores (Fig. 3) of pathogenic strains of the fungus produce sporidesmins A–H, but sporidesmin A is the most clinically relevant. Sporidesmins B–H are of low biologic significance. Sporidesmin causes cholestasis and pericholangitis, resulting in hepatic photosensitization of sheep, cattle, deer, and camelids. The poisoning, known as facial eczema, is an important disease in New Zealand in perennial ryegrass pastures, but has also been reported in the United States, Canada, England, South Africa, The Netherlands, Uruguay, and Argentina.75,80 In New Zealand, the disease is more common in sheep than in cattle. In contrast, pithomycotoxicosis has only been reported in cattle in Uruguay and Argentina because sheep are rarely grazed in cultivated pastures with high productivity (Riet-Correa F, et al.: 2007, [Mycotoxicosis in grazing domestic animals]).45,54 In Brazil, many outbreaks of hepatogenous photosensitization caused by Brachiaria spp. were misdiagnosed as pithomycotoxicosis, but it is now well known that the toxicity of Brachiaria spp. is caused by steroidal lithogenic saponins, 58 and almost none of the P. chartarum strains from Brazil and Colombia produce sporidesmin.11,18 Analyses carried out in P. chartarum isolated from pastures of Uruguay showed that 60% of the strains were pathogenic (Towers N: 1994, Eczema facial [Facial eczema]. In: Buiatrics Uruguayan XXII Conference, Paysandú, Uruguay. Centro Médico veterinário Paysandú, Uruguay, pp. G1–G9. In Spanish). In contrast, nearly all New Zealand isolates produce sporidesmin. 18

Bovine with severe dermatitis due to pithomy-cotoxicosis. Inset: spore of Pithomyces chartarum. Bar = 30 µm.
Pithomycotoxicosis has been detected since the 1970s in Uruguay and Argentina,45,50,54 where it is the main cause of hepatogenic photosensitization. This disease occurs in cultivated pastures of white, red, or subterranean clover mixed with ryegrass (Lolium rigidum), Festuca arundinacea, Phalaris spp., Avena sativa, or other gramineae. The following 2 epidemiological conditions are necessary for pastures to be toxic: environmental conditions must be favorable for fungal growth, and pathogenic strains of P. chartarum, capable of producing sporidesmin, must be present. For the fungus to multiply, conditions with suitable humidity and temperature are required, as well as a suitable and abundant substrate. The most favorable conditions for fungal growth occur during cloudy days with rain, temperatures above 16°C (optimal temperature is 24°C), and relative humidity of more than 80%. The repetition of these favorable growth conditions significantly increases the number of spores. In South America, outbreaks occur in the late summer and autumn, when climatic conditions and pastures are suitable for fungal growth. 54 Intensive grazing practices facilitate the ingestion of large numbers of spores present in the pasture litter. Pastures with plenty of dead plant material, as in those used for seed production, mixed pastures with wheat or oats, pastures that cannot be baled due to adverse weather conditions, and pastures that have been mowed can become toxic. Hay produced from contaminated pastures or pastures that receive rain may also be toxic, as can round bales that are exposed to rain or high humidity levels. 54
The toxicity of pastures depends on the number of toxic P. chartarum spores in the dead plant material and the toxicity of the individual P. chartarum strains. More than 40,000 spores of pathogenic strains per gram of dead vegetation can cause photosensitivity, leading to a severe drop in milk production, while 100,000 spores/g can lead to death. 54 In Uruguay, the disease was very frequent from 1970 to 2000, but the number of outbreaks has decreased, most likely due to the use of high-quality soils, previously used for pastures, for grain production. Morbidity is variable, with rates of 5–10%, while mortality ranges from 1% to 10%. 54
In cattle, the first clinical signs may be transient diarrhea, depression, anorexia, and severe reductions in milk yields from milking cows. Subsequently, subcutaneous edema can be observed, followed by dermatitis affecting exposed, nonpigmented, uncovered areas of the skin (perineum, external face of the udder, nose and muzzle, lips, ears, and periorbital region; Fig. 3). Jaundice, salivation, and nasal and ocular discharges are frequent. The tongue may be ulcerated on the ventral surface, because of exposure to the sun when the animal licks its nostrils. Some affected animals seek shade, have continuous movements of the head, and exhibit other signs of pain. Sometimes the skin peels from a large area, mainly on the face. More severe cases may be fatal during the acute phase, without presenting photosensitization. Intravascular hemolysis, anemia, hemoglobinuria, and abortions have also been described. 54 In sheep, the most characteristic sign is dermatitis of the face; hence, the disease is called facial eczema. The ears are edematous, and the animals display photophobia and seek out any available shade. Jaundice, subcutaneous edema, and other signs of liver failure are also observed. Acutely affected sheep and cattle can die without presenting photosensitization. In severe cases, edema, hemorrhages, and even necrosis may be observed in the urinary bladder.54,75,80
The serum activities of gamma-glutamyl transferase and aspartate aminotransferase and the serum concentrations of bilirubin are increased in affected animals. Gamma-glutamyl transferase is the best indicator of the disease, and high serum concentrations may persist for periods of 3–6 months. During outbreaks, the analysis of blood enzyme activities may reveal that most animals without clinical signs are suffering liver damage with production losses and increased susceptibility to other diseases. Resistant animals show no increase in serum gamma-glutamyl transferase activities. 80
In acute cases, jaundice occurs, and the liver is yellowish and enlarged. The gallbladder is also enlarged and shows edema of the wall. In cases of longer evolution, the liver may be yellowish or whitish due to periportal fibrous tissue proliferation. These lesions are most marked in the left lobe, which in chronic cases may be atrophic and fibrous.54,80 Histologic changes primarily affect the bile ducts, causing degeneration and necrosis of the epithelium, followed by proliferation of epithelial bile duct cells and periportal fibrosis. The periportal hepatocytes may show diffuse vacuolization or necrosis. In chronic cases, there is severe periportal fibrosis and atrophy of the parenchyma.54,80
Presumptive diagnosis is based on clinical signs and the occurrence of the disease in pastures with dead plant material, especially during the fall. The macroscopic and histological lesions are also suggestive of the diagnosis, but the spores in the pasture must be counted for confirmation. However, because not all strains of P. chartarum produce sporidesmin, at least in regions where the disease has not been previously diagnosed, it is also necessary to know if the strains are sporidesmin producers. Enzyme-linked immunosorbent assays and high-performance liquid chromatography methods can be used to detect sporidesmin in body tissues and grass.18,80 The differential diagnosis should be made with plant poisoning that causes hepatic photosensitization, mainly Brachiaria spp. and Panicum spp., which contain lithogenic steroidal saponins and cause a disease similar to pithomycotoxicosis. Histologically, the liver lesions induced by saponin-containing plants are characterized by the presence of crystals in the bile ducts or within macrophages. The presence of foamy macrophages in the liver is also a characteristic of Brachiaria spp. poisoning. 58 Poisoning by plants such as Lantana spp., Myoporum laetum, Stryphnodendron spp., Enterolobium spp., and Senecio spp. should also be considered in the differential diagnosis. 62
All ruminants must be removed from the infected pastures. Affected animals should be placed in permanent shadow with food and water and treated symptomatically if necessary. These pastures should not be used again until their conditions have changed or until the spore count demonstrates a nontoxic fungal concentration. For prophylaxis, pasture management practices should be used to prevent the accumulation of dead plant matter. When these conditions occur, the pastures can be monitored for toxicity by spore counting. However, in countries where not all P. chartarum strains are toxic, this practice can overestimate the risk of poisoning. 18 Reducing grazing pressure can also reduce toxin intake, as the highest toxin levels are generally in those parts of the pasture closest to the ground. In New Zealand, other practices have been used to prevent facial eczema, including dosing the animals with zinc salts to protect them against the toxic effect of sporidesmin, spraying the pastures with fungicides to reduce spore production, and breeding sheep or cattle with increased resistance to the toxin. 75 The substitution of toxigenic strains of P. chartarum by nontoxigenic strains was proposed in New Zealand as a way to control facial eczema. Unfortunately, nontoxigenic strains, initially representing 80–90% of the isolates, did not persist in the pastures and constituted only 4% of the strains after 4 months. 80 However, survival of nontoxigenic strains may not be a problem in South American countries where P. chartarum constitutes a high percentage of the nontoxigenic strains. 18
Diplodiosis
Diplodiosis is a mycotoxicosis caused by Stenocarpella maydis (syn. Diplodia maydis) in cattle and sheep grazing maize harvested fields. Stenocarpella maydis produce a thick mass of mycelium in the cob, leaves, and stem of maize (Fig. 4A), and after maturation, the fungi forms black,pinhead-sized pycnidia (Fig. 4B).32,48,60 A substituted β-cyclopropylamino acid toxin named diplonine was identified in S. maydis and found to cause nervous signs in guinea pigs, similar to those observed in ruminants. 76

Maize infected by Stenocarpella maydis (syn. Diplodia maydis).
Diplodiosis is the most important mycotoxicosis of sheep and cattle in southern Africa 32 and has also been reported in cattle in Brazil 60 and Argentina 48 in corn stubbles during the autumn and winter (April–September). The morbidity rate is 5–75%, the mortality rate is 2–20%, and animals of different ages are affected. 60
Clinical signs in cattle include weeping, salivation, muscle tremors, ataxia, and dysmetria with exaggerated flexion of the limbs during gait. A wide-based stance and stiff gait are also observed. Some animals become recumbent and may develop opisthotonus and extension of the limbs. The first clinical signs occur 2–10 days after consumption of moldy maize. After being removed from stubble, the animals recover in 7–10 days.48,60 Stillborns and neonatal mortality can occur in pregnant cows and sheep without clinical signs following the ingestion of contaminated corn. 32 There are no significant gross lesions. Histologically, spongiosis (status spongiosus) of the cerebellar and cerebral white matter may be observed in cases of long duration. 32 In Argentina, moderate to severe myelin degeneration has been observed in the white matter of the cerebellum. 48 Spongiosis has also been observed in lambs and calves that die around the time of parturition. 32
The diagnosis of diplodiosis must be established by the observation of nervous signs in cattle grazing in corn stubbles during the winter. The main differential diagnosis is with tremorgenic diseases caused by indole-diterpenoid mycotoxins and with poisoning by Ipomoea asarifolia and Phalaris spp. Poisoning by Aspergillus clavatus shares similar signs with diplodiosis but has a higher mortality rate. A detailed histologic examination of the central nervous system should help in the differential diagnosis, mainly in cases of neonatal mortality when the dams do not show clinical signs.
There is no specific treatment for diplodiosis. After the observation of clinical signs, the herd must be removed from the corn stubbles immediately. Because the pycnidia of the fungus overwinter in the soil, maize residues should be removed from the area (i.e., by deep early plowing or burning) to decrease contamination of the next crop. Alternating maize cultures with other cultures can also help control corn contamination by S. maydis.
Slaframine poisoning
Slaframine is an indolizidine alkaloid produced by the fungus Rhizoctonia leguminicola, which infects leguminous pastures, mainly Trifolium pratense (red clover or rotklee) and Medicago sativa (alfalfa or lucerne). 21 In the liver, slaframine is metabolized to 6-ketoimine, which is similar to acetylcholine. This active metabolite causes excessive salivation and other parasympathomimetic effects. 21 Rhizoctonia leguminicola causes a disease called “blackpatch” in leguminous plants, characterized by dark patches up to 1–3 mm in length on the leaves or stems (Gough FJ, Elliott ES: 1956, Blackpatch of red clover and other legumes caused by Rhizoctonia leguminicola sp. nov. Bulletin 387T, West Virginia University Agricultural Experiment Station, Morgantown, West Virginia. Available at: http://archive.org/stream/blackpatchofredc387goug#page/n1/mode/2up). Rhizoctonia leguminicola also contains swainsonine, which may be responsible for some of the clinical signs observed in the disease. 21
Slaframine poisoning, known as slobbers, has been reported in the United States and other countries and primarily affects cattle and horses, although goats may also be affected.21,82 In Uruguay (Riet-Correa F, et al.: 2007, [Mycotoxicosis in grazing domestic animals]) and Argentina, 50 the disease has been observed in cattle grazing red clover. In the Brazilian state of São Paulo, slobbers was diagnosed in horses that ingested alfalfa hay, which was produced in southern Brazil (state of Paraná) and stored for 4 months before consumption. 8 In Uruguay and Argentina, the disease has been reported to occur during the fall (April–June), apparently as a result of excessive rainfall (Riet-Correa F, et al.: 2007). Poisoning also occurs by the ingestion of alfalfa or red clover hay, in which 5–10% of the original toxicity remains after 10 months. 21
In cattle, clinical signs are decreased milk production, salivation, lacrimation, and piloerection. Some animals may show frequent urination, stiff gait, dyspnea, bloat, and increased frequency of defecation (Riet-Correa F, et al.: 2007, [Mycotoxicosis in grazing domestic animals]). 50 Horses show light to intense drooling accompanied by constant movement of the tongue. 8 Salivation appears 5–6 hr after ingestion of the contaminated food, and the animal recovers 24 hr after removal of the contaminated diet. A presumptive diagnosis can be made by the observation of salivation in animals ingesting leguminous pastures or hay. Rhizoctonia leguminicola poisoning can be confirmed by microscopic observation or fungal isolation from the typical black spots on the plants. To detect slaframine activity, pastures, hay, or their extracts can be administered to guinea pigs to induce salivation. The toxin can be identified by gas chromatography and mass spectrometry. The differential diagnosis includes vesicular stomatitis and salivation in individual horses caused by choking, oral trauma, oral foreign bodies, dental problems, glossitis, and treatment with the drug imidocarb, which causes salivation by reversible inhibition of cholinesterase. 8 In cattle, the main differential diagnosis is with foot and mouth disease and vesicular or ulcerative stomatitis. Affected animals may be treated with atropine to reduce the salivation. 50 There is no practical way to control R. leguminicola in the pastures or hay, but seeds can be treated with fungicides to avoid transmission to fungus-free areas (Gough FJ, Elliott ES: 1956, Blackpatch of red clover and other legumes).
Aflatoxicosis
Aflatoxins are a group of hepatotoxic metabolites (primarily aflatoxins B1, B2, G1, and G2) produced by some strains of Aspergillus, mainly A. flavus and A. parasiticus, at temperatures of 24–35°C and humidity greater than 14%.43,49 Aflatoxin B1 is biotransformed by liver microsomal mixed-function oxidases to form several metabolites, including aflatoxin B1-8,9-epoxide that binds covalently to nucleic acids and proteins and seems to be responsible for cellular necrosis, immune suppression, mutagenesis, and neoplasms.43,49 Aflatoxicosis is a disease that predominantly affects animals that ingest grains or grain byproducts. Pigs and poultry are most often affected, but aflatoxicosis can also occur in other species including cattle (Lafluf O, Termezana A, Rivero R, et al.: 1989, Un caso de aflatoxicosis en bovinos asociado a maíz carbonoso [A case of aflatoxicosis associated with corn infected by Ustilago maydis]. Buiatrics Uruguayan XVII Conference, Paysandú, Uruguay, sección cc8, pp. 1–8).25,40,51 Young animals are more susceptible than adults, and, in cattle, the disease is more common in calves and dairy cows than in adult beef cattle. Aflatoxins only cause clinical signs in calves at high doses (e.g., 0.02–0.08 mg of aflatoxin B1 per kg of body weight daily). 52 However, the effects of aflatoxin poisoning in cattle depend on the aflatoxin concentration in the food, the length of the feeding period, and the age of the animals. In horses, aflatoxicosis is a rare disease, 49 and the few reported cases have been reviewed. 13 As in other species, aflatoxicosis in horses affects mainly the liver causing hepatocellular degeneration, necrosis, and megalocytosis, as well as bile duct proliferation and fibrosis. Hemorrhagic enteritis and pale kidneys with protein precipitate in renal tubules are also observed.13,49 An outbreak of aflatoxicosis was reported in young goats following ingestion of polkudu meal (defatted residue from grated coconut after juice extraction), 73 and decreased milk production has been reported in goats following aflatoxin ingestion. 28 Sheep are resistant to aflatoxins, although high concentrations (2,000 ppb) have been associated with a decrease in weight gain. 25
In Uruguay, an outbreak of aflatoxicosis occurred in cattle that had been grazed for 2 weeks in a corn field in which corn was not harvested due to heavy infection by Ustilago maydis. Out of 81 Holstein dairy cows, 10 became ill and 3 died. Aspergillus flavus was isolated from the corn, which was found to contain 2,700 ppb of aflatoxin B1. The poor condition of this corn, due to U. maydis infection, favored the development of the toxigenic strains of this fungus. High infection by this fungus occurs when rainfall is scarce during the vegetative period of the plant (Lafluf O, et al.: 1989, [A case of aflatoxicosis]). In Uruguay and Brazil, outbreaks of aflatoxicosis were reported in steers that had ingested a ration constituted by 70% sorghum wet grain silage and 27% sorghum silage containing 20 ppb of aflatoxins 25 and in 4-month-old calves that ingested a ration that consisted of alfalfa hay, broken corn, and milk substitute containing 5,136 ppb of aflatoxin B1. 51 The mortality rates varied from 1.6% to 15%.25,51
The most frequent clinical signs of chronic aflatoxicosis, caused by ingestion of aflatoxins for weeks or months, are a decrease in milk production in dairy cattle and lower weight gains in growing animals. Some animals show signs of liver failure, including general unthriftiness, rough coats, anorexia, depression, food refusal, abdominal pain with colic, grinding of the teeth, photosensitivity, severe diarrhea, and rectal tenesmus, sometimes with a prolapsed rectum.20,51 Acute aflatoxicosis is rare, but has been reported to cause anorexia, depression, jaundice, photodermatitis, submandibular edema, diarrhea (sometimes bloody), nervous signs, and abortion (Lafluf O, et al.: 1989, [A case of aflatoxicosis]). 40 Most likely, the most important form of aflatoxicosis is subclinical and nonspecific, causing reduced milk production, lower weight gains, and immune depression associated with an increased frequency of diarrhea, respiratory disease, and mastitis. The increased serum activities of alkaline phosphatase and gamma-glutamyl transpeptidase are good indicators of liver damage due to aflatoxins. 52
Gross lesions include color changes and increased consistency of the liver, gall bladder dilatation with wall edema, and edema of the mesentery and wall of the abomasum (Lafluf O, et al.: 1989, [A case of aflatoxicosis]).20,40 In acute cases, there may be jaundice and bleeding of the subcutaneous tissue, skeletal muscles, lymph nodes, pericardium, and gastrointestinal tract (Lafluf O, et al.: 1989). 40 Histological changes of the liver are characterized by periportal fibrosis, bile duct cell proliferation, megalocytosis, and vacuolization or single-cell necrosis of hepatocytes (Lafluf O, et al.: 1989).20,40,51
The presumptive diagnosis of aflatoxicosis is made through epidemiological data, clinical signs, gross lesions, and primarily by the presence of histological lesions. The definitive diagnosis should rely on the detection of aflatoxins in the food and the characteristic histologic lesions. However, it should be noted that the aflatoxin analysis of the sample is not representative of food consumed during the previous weeks or months and that histologic lesions are not specific. The main differential diagnosis is with poisoning by plants containing pyrrolizidine alkaloids (Senecio spp., Echium plantagineum, Erechtites hieracifolia, and Crotalaria spp. in South America). In feedlots, hay or silage should be observed to detect the possible presence of these plants. Crops can be contaminated by Crotalaria spp. seeds. In the subclinical form, other diseases and management mistakes that cause reduced production and impaired immunity should be considered.
For control of aflatoxicosis, the contaminated food should be immediately removed from the diet. For prevention, it is important to avoid feeding animals any crops or byproducts that have been stored improperly. Surveying feed crops for the presence of aflatoxins is the best way to prevent aflatoxicosis, especially the subclinical form. Aluminosilicate products such as hydrated calcium aluminosilicate and sodium bentonite, which are effective in binding aflatoxins and preventing their absorption, have been widely used in the pig and poultry industries to prevent aflatoxicosis.
Poisoning by Aspergillus clavatus
Poisoning by Aspergillus clavatus leads to neuromycotoxicosis of cattle and sheep, characterized by tremors, ataxia, weakness, paresis, and recumbence followed by death. This poisoning occurs primarily in animals that ingest malting residues contaminated with A. clavatus.32,37,55,72,74 In Brazil, this neuromycotoxicosis was reproduced in cattle 19 and sheep 4 fed corn contaminated with A. clavatus, which produces several toxic metabolites, including patulin, tryptoquivalines, cytochalasin E, and glyantripine.55,72 Aspergillus clavatus poisoning has also been reported in animals that have ingested sprouting wheat, sprouting maize, and sorghum beer residues. 32 In Uruguay, the disease was also reported in cattle that ingested sugar beet residues, which were widely used as animal feed in that country until the 1980s. Toxigenic strains of A. clavatus were isolated from toxic sugar beet residues stored under humidity and temperature conditions suitable for fungal growth. 55
The morbidity rates of poisoning by malting residues varied between 17% and 32%, and mortality ranged from 25% to 87%.19,55 In cases of poisoning by sugar beet residues, morbidity rates were 35–93%, and mortality rates were 8.6–34.4%.
Clinical signs include instability, ataxia, weakness or paralysis mainly of the hind limbs, and an inability to rise (Fig. 5A, 5B). Initially, affected cattle appear normal at rest, but manifest clinical signs when stimulated. If the animals are exercised or forced to move, they display muscle tremors, and fall down into a position of sternal recumbence, frequently with the legs extended or in a dog-sitting position. After a short rest, some animals rise and walk normally, but others stay recumbent and may present mild head tremors, salivation, and loss of spinal cord reflexes. Lateral recumbence and paddling are observed in the terminal phase. 37 The clinical course of the disease varies from 2–3 days to 2 weeks. Deaths occur during a period of several weeks. The morbidity rate is 17–32%, and the mortality rate is 25–87%.19,55 A mortality rate of 97% has been reported in sheep. 74
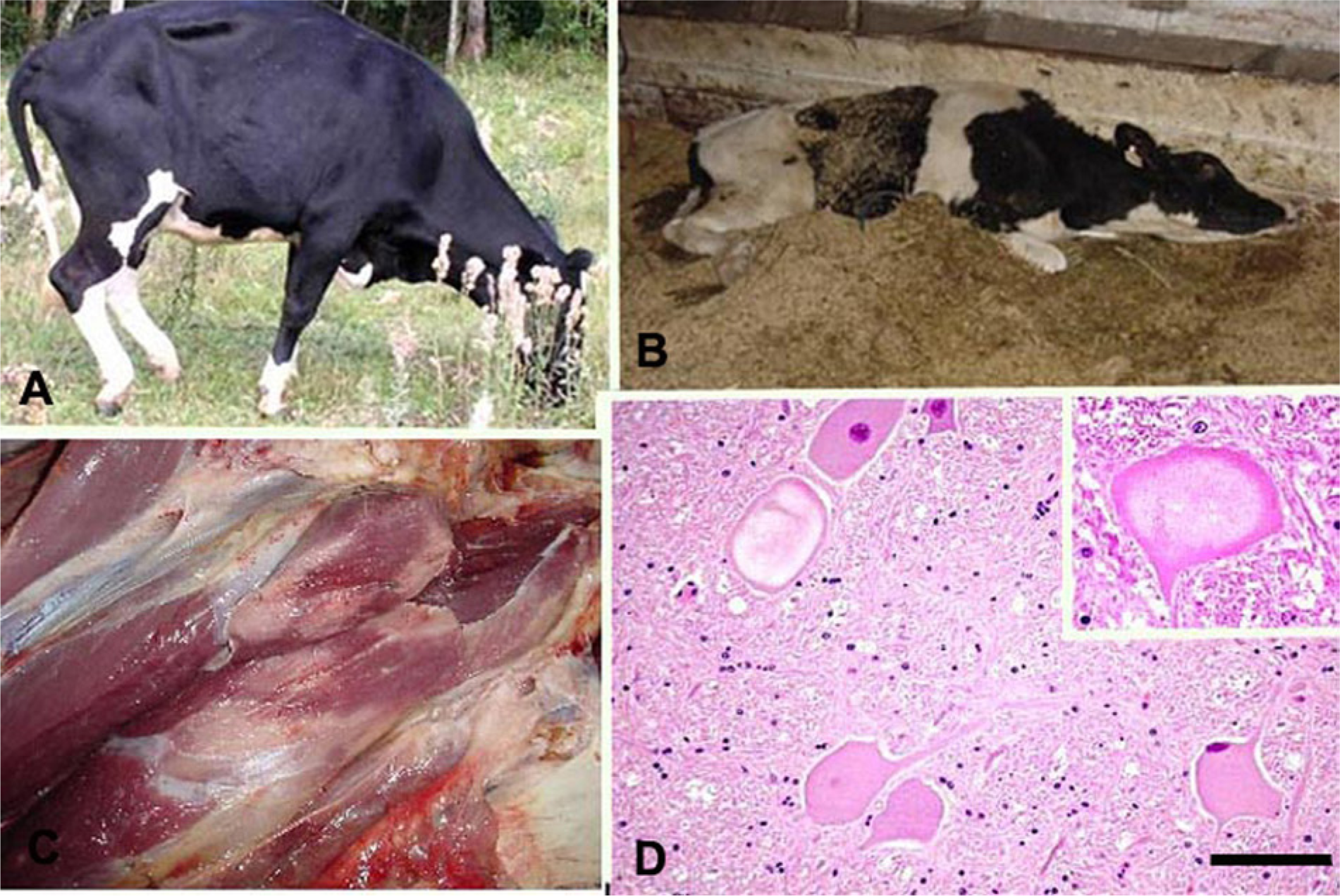
Poisoning by Aspergillus clavatus.
The main gross lesion is a whitish appearance of the large muscles of the fore and hind limbs (Fig. 5C). Histologically, severe chromatolysis, paleness, vacuolation, and margination of the nuclei occur in the neurons of the midbrain, medulla oblongata, and pons and in the ventral horn of the spinal cord (Fig. 5D).37,72 Axonal degeneration is observed in the white matter of the central nervous system and in the peripheral nerves. 72 Focal degeneration and necrosis are present in the skeletal muscles.
The presence of the histologic lesions described above and a history of feeding with barley or sugar beet residues are the most important criteria for the diagnosis of A. clavatus poisoning. Aspergillus clavatus can be isolated from the food, but it is important to consider that not all strains are toxigenic. Multitoxin and patulin analysis of the contaminated food and isolation of A. clavatus should be performed to confirm the diagnosis. The main differential diagnoses are poisoning by indole-diterpenoid mycotoxins and botulism. Indole-diterpenoid poisoning is a tremorgenic disease with much lower mortality rates, and the animals recover in a few days after withdrawal of the contaminated food. Clinically, botulism is very similar to A. clavatus poisoning, but in the latter, neuronal lesions do not occur and muscle lesions are much less common. Analysis for botulism toxin in more than 1 animal is important for diagnosis. In South America, paralytic rabies transmitted by bats causes a similar disease, but with 100% fatality and typical histologic lesions.
In cases of A. clavatus poisoning, the contaminated food should be removed from the diet immediately. To prevent poisoning, barley, barley residues, or beet residues should be stored under appropriate environmental conditions to avoid fungal contamination.
Poisoning by moldy sweet potatoes (Ipomoea batatas)
Sweet potatoes (Ipomoea batatas) infected by Fusarium solani (Fig. 6A) may contain 3-substituted furans, including 4-ipomeanol, 1-ipomeanol, 1,4-ipomeadiol, and ipomeanine, which cause acute respiratory distress in cattle. This disease is not technically a mycotoxicosis because the toxins are produced by the tubercle after it has been infected by the fungi. Fusarium solani stimulates host tissues to form ipomeamarone and 4-hydroxymyoporone; the latter is then converted to 4-ipomeanol, 1-ipomeanol, and 1,4-ipomeadiol. 62 Other fungi, including Fusarium oxysporum, have been isolated from sweet potatoes in some outbreaks.26,41 Mechanical injury, chemical treatments, and parasitic infections can also induce the production of 3-substituted furans by sweet potatoes. In some regions, animals are commonly fed tubercles that are visibly moldy (Fig. 6A) or infected by parasites, as these potatoes are considered unfit for human consumption.26,41
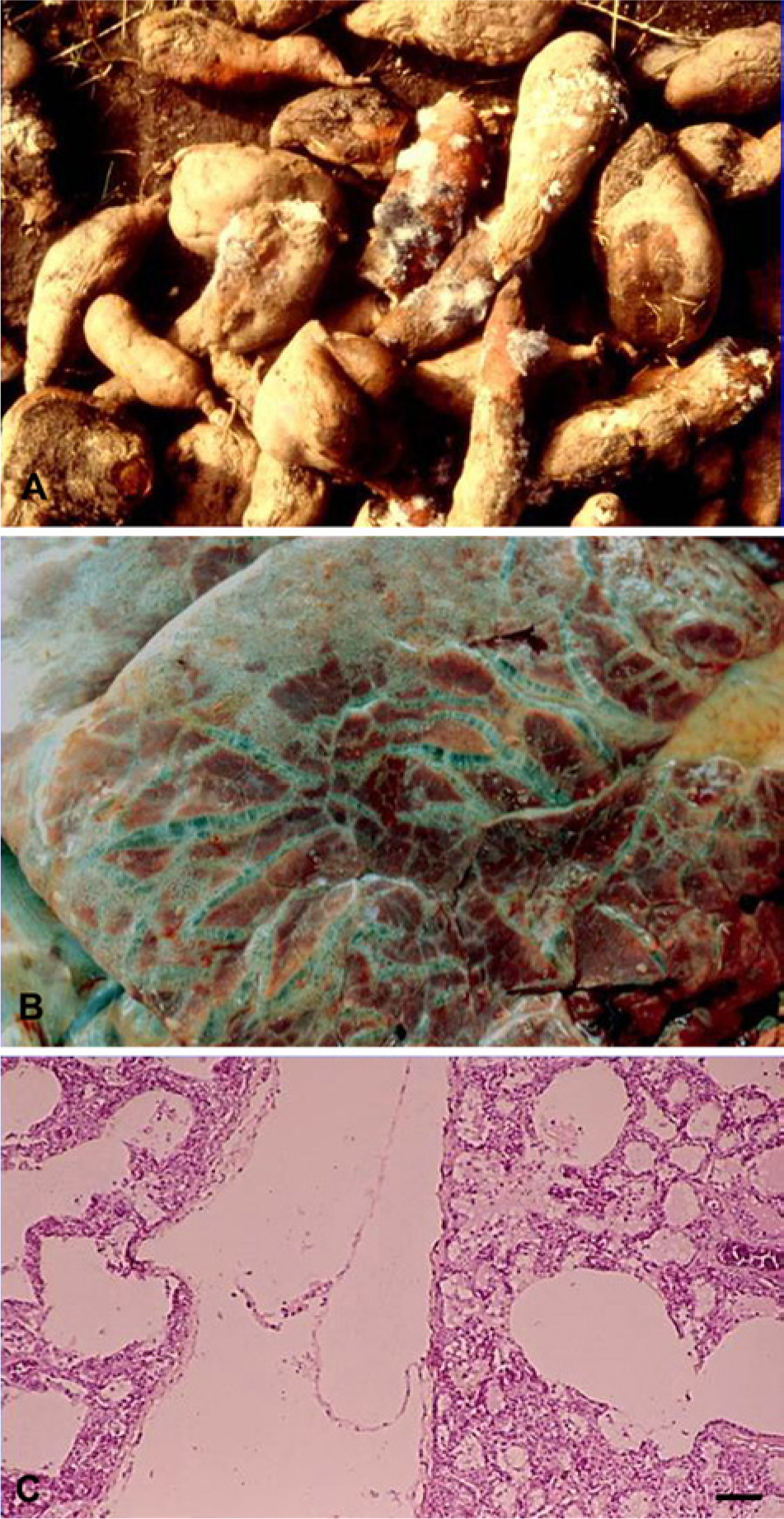
Poisoning by moldy sweet potatoes (Ipomoea batatas).
Poisoning has been reported in Brazil26,41 and Uruguay.
69
The clinical signs include severe respiratory distress with dyspnea, coughing, salivation, and dilated nostrils. Greatly affected animals adopt a position with an extended neck and hanging head. The clinical manifestation period varies from 3–5 days.26,41,69 Necropsy lesions include distended and pale lungs with a rubbery consistency that does not collapse when the thorax is opened. Pulmonary edema and emphysema (Fig. 6B), as well as white foam, can also be observed in the airways. Sweet potato residues can be found in the rumen content. Histologically, the interlobular septa and the subpleural tissues are distended by edema and emphysema (Fig. 6C). Additional lesions are thickening of the alveolar walls by inflammatory cells and edema. The alveoli can be lined by type II pneumocytes, and the pulmonary lymphatic vessels are dilated by air.26,41 The clinical signs and pathology, as well as a history of feeding moldy sweet potatoes, usually allow diagnosis of this type of poisoning, and the macroscopic and histological lesions are characteristic. However, there are several causes of interstitial pneumonia, grouped under the name “atypical interstitial pneumonia,” including poisoning by
Leukoencephalomalacia
Leukoencephalomalacia (LEM) is a disease of equids caused by ingesting moldy corn contaminated by the fungus of the genera Fusarium, including Fusarium verticillioides (syn. F. moniliforme) and Fusarium proliferatum, which produce fumonisin. Many fumonisins have been identified, but only fumonisins B1 and B2 are important as a cause of LEM. Fumonisins alter sphingolipid metabolism by inhibiting ceramide synthase, an important enzyme in the biosynthesis of sphingolipids. High doses of fumonisin B1 may cause hepatotoxicity. In Brazil, F. verticillioides has been isolated consistently from samples of corn that cause LEM.2,29,64,83 Fusarium proliferatum and Fusarium subglutinans are less frequently isolated. Levels of fumonisin B1 ranging from 10 to 500 µg/g were detected in 24 samples of corn that caused LEM. 63 In another 13 samples, fumonisin B1 concentrations ranged from 0.2 mg/g to 38.5 mg/g, and fumonisin B2 concentrations were between 0.1 and 12 µg/g. 79 In Argentina, fumonisin B1 and B2 concentrations were 12.5 and 5.2 µg/g, respectively, in a feed supplement that caused LEM. 27
Leukoencephalomalacia has been diagnosed in horses in all regions of Brazil,2,12,29,53,63,64,67,79,83 in Argentina27,42 and Uruguay, 68 and in mules in the Brazilian states of Pernambuco and Pará.14,67 Outbreaks occur in animals that are fed corn kernels, corn cobs, ground whole corn (a mixture of corn, corn stalks, and corn cobs), corn bran, corn screenings, or other byproducts from the processing of corn for human consumption. Corn that causes LEM may not be visibly moldy. Some outbreaks are caused by apparently normal corn contaminated by F. verticillioides. In the southern and southeastern regions of Brazil, LEM is seasonal, occurring mainly between June and September, although outbreaks have been recorded from March to December.2,63,64 In tropical climates, outbreaks occur in both the dry and rainy seasons.14,67 Fusarium verticillioides infection of maize is more frequent when periods of drought are followed by cool, wet weather during pollination. 43
In corn samples from 21 outbreaks of LEM, the moisture was 16.98 ± 2.30%. In 5 samples, the moisture was below 15%, which is in accordance with Brazilian standards for corn storage. 63 In outbreaks reported in southern Brazil, LEM occurred in horses ingesting more than 1 kg of corn daily or rations containing more than 20% corn. 63 Animals of different ages and both sexes can be affected. Morbidity rates are 4–100%, and case fatality rates are nearly 100%.27,63,68 Partial recovery has been reported in some cases, 27 although this is rare.
Clinical signs of LEM appear abruptly and are characteristic of lesions of the cerebrum and brain stem, including anorexia, dullness, drowsiness, occasional hyperexcitability, muscle tremors, compulsive walking, head pressing, circling, chewing difficulties, unilateral or bilateral blindness, ataxia, decreased eyelid reflex, decreased tone of the tongue and lips, loss of sensitivity of the face, paralysis of the jaw, and recumbence.2,12,27,63,64,67 The clinical manifestation period is 2–72 hr, but most affected animals die within 6–24 hr. Occasionally, the clinical course may last up to 13 days. In some outbreaks, the clinical signs may appear up to 12 days after the corn is withdrawn from the diet.
The lesions are almost bilateral, but asymmetric, with one side much more affected than the other and are located in the cerebrum and/or brain stem. One of the cerebral hemispheres may be enlarged, and malacia of the white matter may be observed on the cut surface, with multifocal to coalescing foci of hemorrhage, brown-yellow discoloration, and softening of the centrum semiovale and corona radiata (Fig. 7A). Cavities containing fluid are often observed in these areas. The internal capsule and thalamus are usually affected, but lesions may be observed also in the mesencephalon (Fig. 7B), cerebellar peduncles, pons, and medulla oblongata. The macroscopic lesions are better evidenced after fixation of the central nervous system in 10–25% formalin, but cavitation, edema (yellow areas), and hemorrhages are easily observed in fresh brain tissue (Fig. 8). In some horses, the liver may be enlarged and yellowish.2,12,63,64,67,83
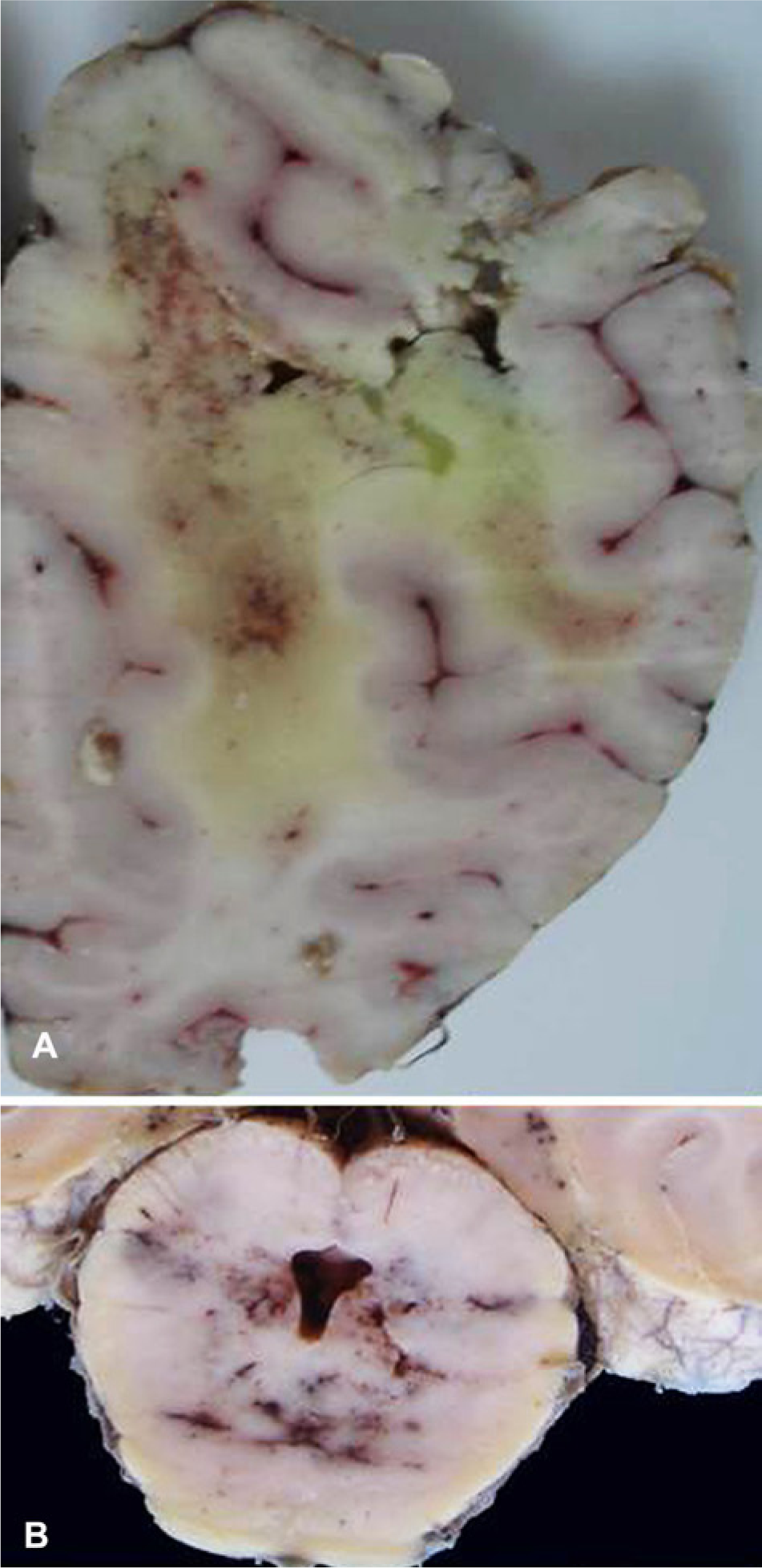
Leukoencephalomalacia in equid.
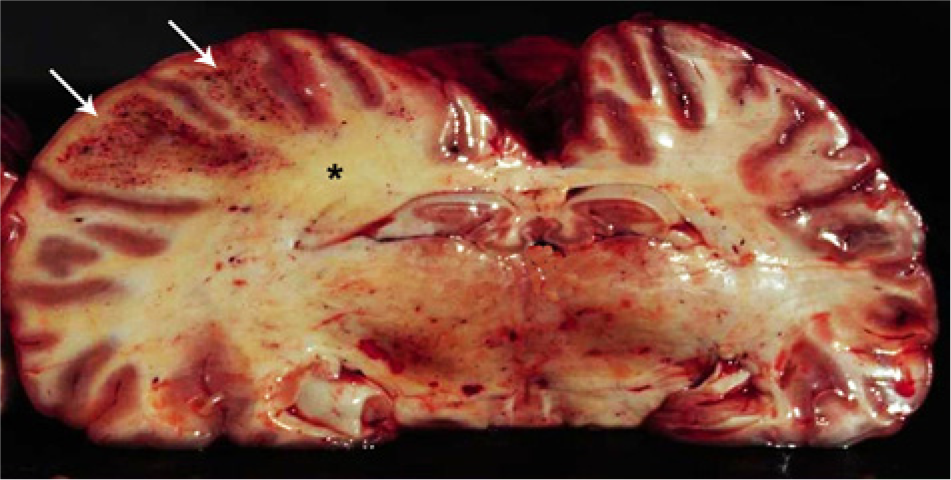
Leukoencephalomalacia in equid. Fresh cerebrum showing enlarged left hemisphere with hemorrhages (arrows) and yellow discoloration of the white matter (*).
Histologically, malacia surrounded by edema and hemorrhage of the neuropil are observed (Fig. 9). An additional characteristic of LEM is the presence of swollen astrocytes or oligodendrocytes, with abundant eosinophilic cytoplasm, deeply eosinophilic intracytoplasmic globules, and eccentric hyperchromatic nuclei (Fig. 9).14,27,63,67 These cells, previously known as clasmatodendritic astroglia, are found in areas of hemorrhage and edema and are swollen because they have imbibed plasma protein. Additional lesions include hypertrophic and degenerative changes in the vascular endothelium and perivascular edema, hemorrhages, and eosinophilic globules. Some vessels have perivascular cuffing of eosinophils, neutrophils, or mononuclear cells.2,12,63,64,67,83 Affected horses may also have hepatic lesions, including vacuolization or necrosis of the hepatocytes.
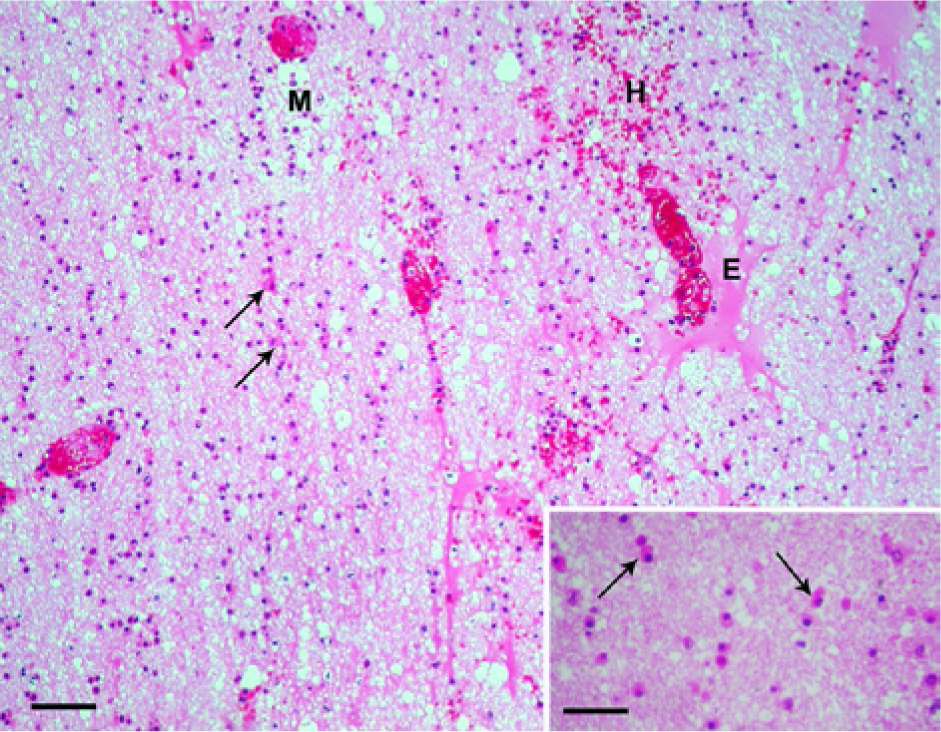
Equine leukoencephalomalacia; cerebral white matter. Malacia (M), perivascular edema (E), and hemorrhages (H) and numerous characteristic reactive glial cells with abundant eosinophilic cytoplasm, sometimes called clasmatodendritic astroglia, are observed (arrows). Hematoxylin and eosin (HE). Bar = 100 µm. Inset: reactive glial cells (arrows). HE. Bar = 30 µm.
The diagnosis of LEM is based on the occurrence of the disease in horses that have ingested diets containing corn or corn byproducts. The main differential diagnosis is with rabies, viral equine encephalitis, and hepatic encephalopathy, which is caused primarily by poisoning with pyrrolizidine alkaloids. Malacia of the white matter, macroscopically similar to that caused by LEM, is observed in equine trypanosomiasis caused by Trypanosoma evansi. In trypanosomiasis, however, the main histologic lesion is severe encephalitis, and the clinical manifestation period is much longer. The only way to prevent LEM is to avoid the ingestion of improperly dried corn. When the corn is properly dried, it should not constitute more than 20% of the dry matter.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by National Institute for Science and Technology for the Control of Plant Poisonings, National Council of Scientific and Technological Development (CNPq; grant 573534/2008-0).
