Abstract
Objective
Major depressive disorder (MDD) is a highly prevalent debilitating mental health disorder with a lifetime risk of 11–15% in Australia. The most effective treatment for severe depression is electroconvulsive therapy (ECT), but it is associated with high relapse rates. This review aimed to investigate non-ECT interventions for preventing relapse of MDD after an effective acute course of ECT.
Method
The search covered electronic databases, specifically PubMed, PsycINFO and Embase, and clinical trials registered with clinicaltrials.gov and Cochrane Register of controlled trials up to 1 June 2022. Medical Subject Headings and key words used in the search were ‘electroconvulsive therapy’, ‘depressive disorder’, ‘continuation’, ‘maintenance’, ‘prevention’, ‘prophylaxis’, ‘relapse’ and ‘recurrence’.
Results
A total of fifteen articles were included in the review. Interventions investigated by the studies were lithium, lithium + nortriptyline, escitalopram, imipramine, phenelzine, amitriptyline, venlafaxine and cognitive behavioural therapy (CBT).
Conclusions
Lithium was investigated the most, demonstrating good outcomes either as monotherapy or combination therapy with nortriptyline or venlafaxine. Imipramine, phenelzine, amitriptyline and CBT demonstrated encouraging results, while escitalopram failed to show a favourable outcome. Clinicians aiming to reduce the risk of relapse after an effective acute course of ECT could consider lithium, nortriptyline, venlafaxine and CBT.
Introduction
Major depressive disorder (MDD) is a debilitating mental health disorder, with a lifetime risk of 11 to 15% in Australia. 1 MDD remains among the most burdensome disorders worldwide. 2 Approximately 50% patients will experience relapse or recurrence of depression after their recovery from their first episode of MDD. 3 These relapse and recurrence rates would increase with subsequent episodes of MDD. 3 Causes of relapse and recurrence in MDD are multifactorial, including the number of previous episodes, residual symptoms, comorbid conditions, stressful life events, family history, ongoing psychosocial stressors and inadequate treatments. 3 Although ECT is the most effective treatment for severe depression, high relapse rates still exist. Multiple studies have shown that relapse rates within 12 months have been over 50%, with the majority of patients relapsing in the first 6 months despite maintenance treatment after a course of ECT. 4 Maintenance treatment aims to prevent relapse and recurrence and this includes pharmacotherapy, continuation ECT and maintenance ECT. 4 There are already existing recommendations for maintenance and continuation ECT for preventing relapse of MDD.5,6 However, for non-ECT interventions, which are more commonly utilised, the current Royal Australian and New Zealand College of Psychiatrists (RANZCP) guidelines suggest ‘an antidepressant and/or lithium for at least 12 to 24 months’, 7 without a specific guidance as to the choice and comparative efficacy of treatment options. This review aims to investigate the current evidence base for non-ECT interventions in preventing relapse of MDD after an effective acute course of ECT. Due to this area being relatively under-researched, the format of the review was a systematic search strategy with results described in a narrative summary. Through this approach, it aims to provide an understanding of the extent of available evidence, a preliminary guidance to clinicians and importantly, an illumination of the gaps in the current evidence that need to be addressed by future research.
Method
Literature search strategy
The search covered electronic databases, specifically PubMed, PsycINFO and Embase, and clinical trials registered with clinicaltrials.gov and Cochrane Register of controlled trials. Medical Subject Headings (MeSH) terms and keywords searched were ‘electroconvulsive therapy’, ‘depressive disorder’, ‘continuation’, ‘maintenance’, ‘prevention’, ‘prophylaxis’, ‘relapse’ and ‘recurrence’. All potential articles published since inception of these databases to 1st June 2022 were searched. Operators used for literature search can be seen in Figure 1. Additionally, a targeted database search of ‘ECT’ and certain interventions, and reference lists of relevant studies were also explored for potential studies to include. Operators for database search.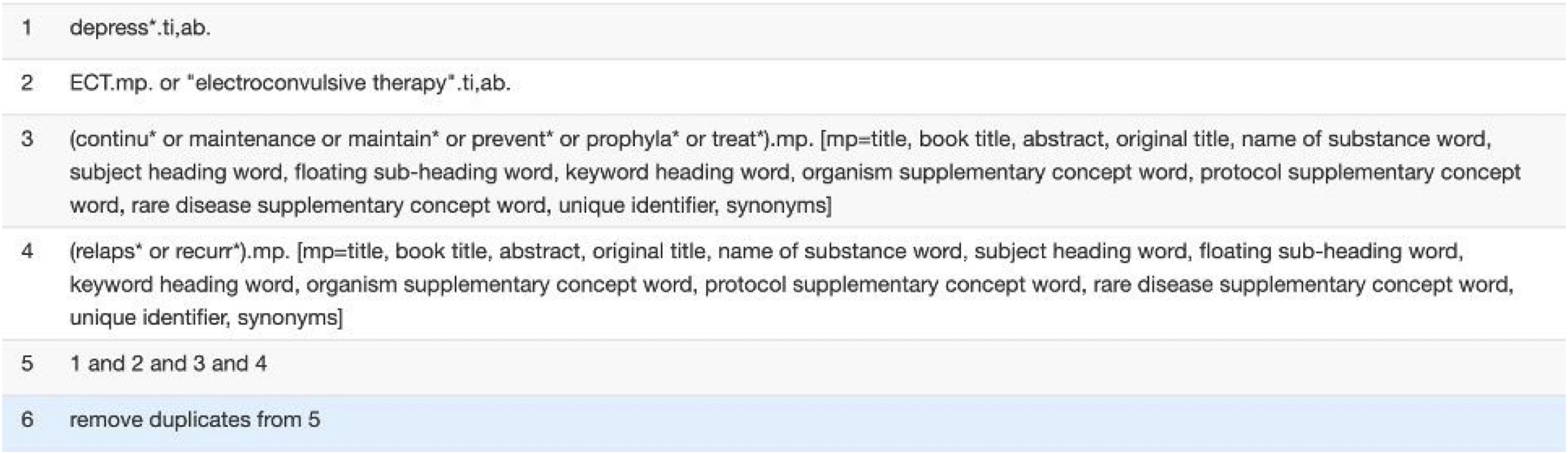
Inclusion criteria
- Original articles. - Published from since inception of databases to 1st June 2022. - English language only. - Studies involving humans of at least 18 years of age. - Diagnosis of MDD, first or subsequent episodes. Any recognised form of diagnostic criteria was accepted. - Remission or response of MDD following an acute course of ECT. - Delusional depression, MDD with psychotic features were also included. Comorbid anxiety disorder, personality disorder and substance abuse/dependence were included due to high frequency of comorbidity with MDD. - Randomised controlled trials (RCTs) and non-randomised observational studies (cohort and case-control studies) exploring non-ECT prophylactic treatments for MDD, including pharmacotherapy, psychotherapy and other types of brain stimulation such as repetitive transcranial magnetic stimulation or a combination of these.
Exclusion criteria
- Bipolar affective disorder, schizoaffective disorder and schizophrenia. Studies of bipolar depression were excluded as management for unipolar and bipolar depression differs significantly and may confound conclusions of this study. For example, lithium may be prescribed for prevention of manic episodes rather than depressive episodes, and antidepressants are typically avoided in bipolar depression due to risks of manic switching. - Dementia or intellectual disability and presence of medical or neurological condition that would affect cognition and treatment response. However, comments on the presence of these conditions were typically not mentioned in the studies. - Review articles, case reports, surveys, presentations, abstract-only publications and studies where the research team could not access the full-text article were excluded. Cross-sectional studies using multivariate analysis to explore potential treatment modalities were also excluded as such studies are more hypothesis generating, rather than hypothesis testing. - ECT interventions were excluded as guidelines and reviews for continuation and maintenance ECT already exist.
Study selection
One author (Song) screened the titles of the publications for the inclusion and exclusion criteria and all potential studies were noted. The titles and abstracts were reviewed to further screen the included studies. Full-text screening was then undertaken according to the stated inclusion and exclusion criteria. Where a decision to include or exclude was unclear, this was resolved by reaching consensus through discussion with two other researchers (Launder and Chong).
Data extraction
Three researchers (Song, Launder and Chong) developed data extraction categories applied to the included studies, which included authors, trial dates, country of origin, study design, information about participants (sample size, age, gender ratio, type of ECT received and comorbidities mentioned), definition of depression and remission, inclusion and exclusion criteria, intervention, outcomes, key conclusion and limitations. One researcher (Song) extracted information from the included studies.
Outcomes measured
The efficacy of interventions was assessed using the outcome of recurrence or relapse of a depressive episode, defined by any measure of depressive symptom severity if available. This includes duration of depressive episodes, suicide risk, time to hospital readmission, time to relapse and depression rating scores.
Results
As illustrated in the PRISMA flow diagram (Figure 2), the database search yielded a total of 2236 potentially eligible records in the initial retrieval process. From the screening process, eight articles were included, and then seven additional studies were included from a separate targeted search of the database and reference lists, resulting in a total of fifteen studies included in this review.8–22 PRISMA diagram.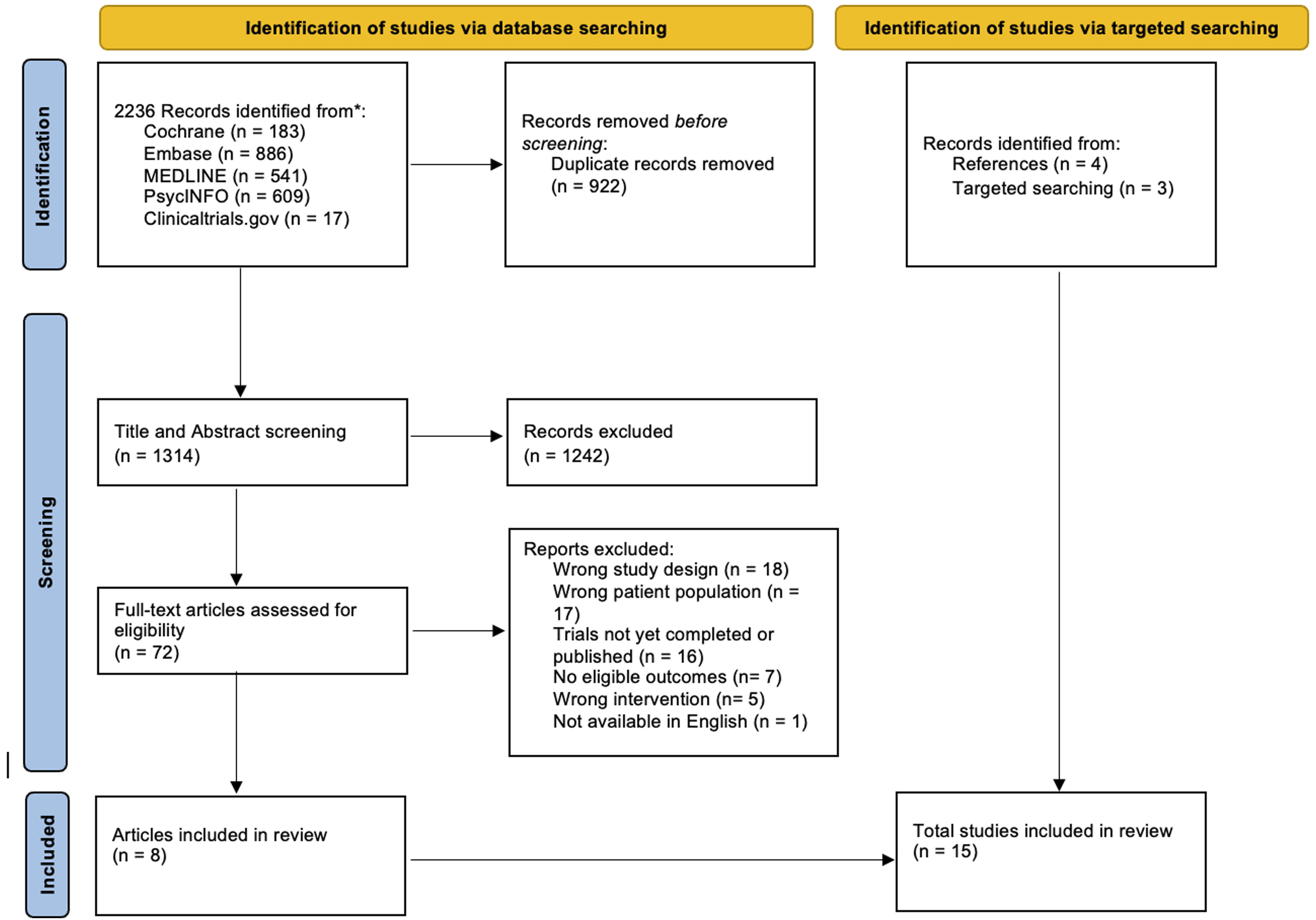
Main characteristics of included trials
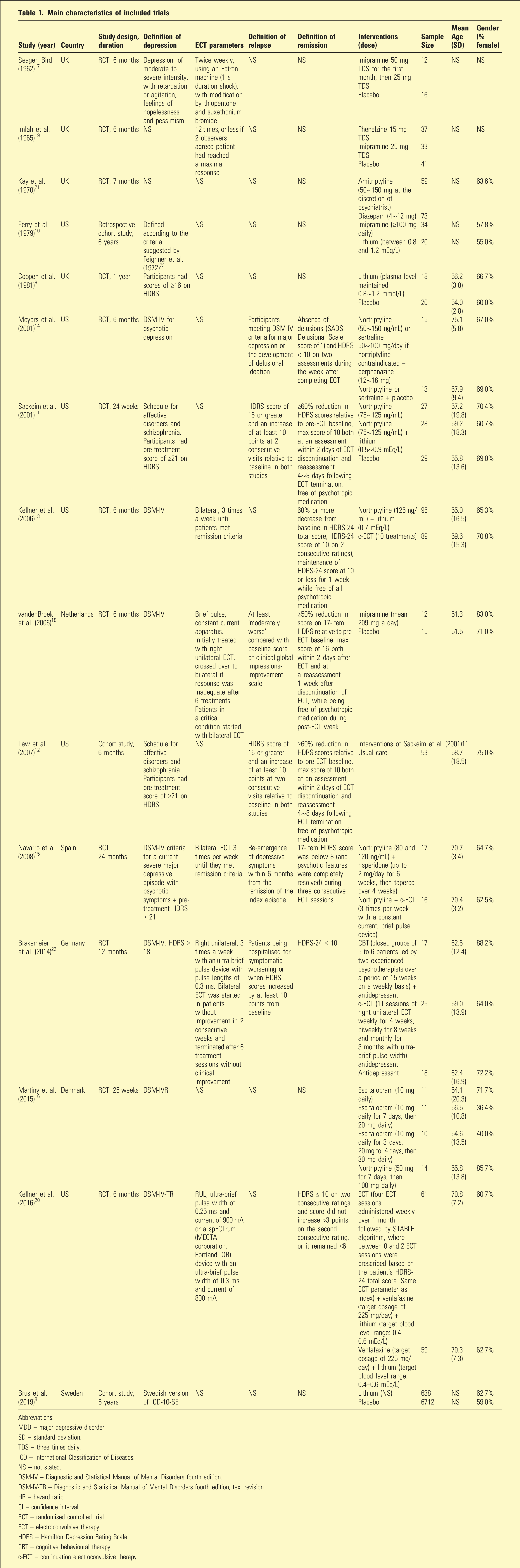
Abbreviations:
MDD – major depressive disorder.
SD – standard deviation.
TDS – three times daily.
ICD – International Classification of Diseases.
NS – not stated.
DSM-IV – Diagnostic and Statistical Manual of Mental Disorders fourth edition.
DSM-IV-TR – Diagnostic and Statistical Manual of Mental Disorders fourth edition, text revision.
HR – hazard ratio.
CI – confidence interval.
RCT – randomised controlled trial.
ECT – electroconvulsive therapy.
HDRS – Hamilton Depression Rating Scale.
CBT – cognitive behavioural therapy.
c-ECT – continuation electroconvulsive therapy.
Relapse, readmission and depression severity outcomes
Summary of results regarding relapse and readmission
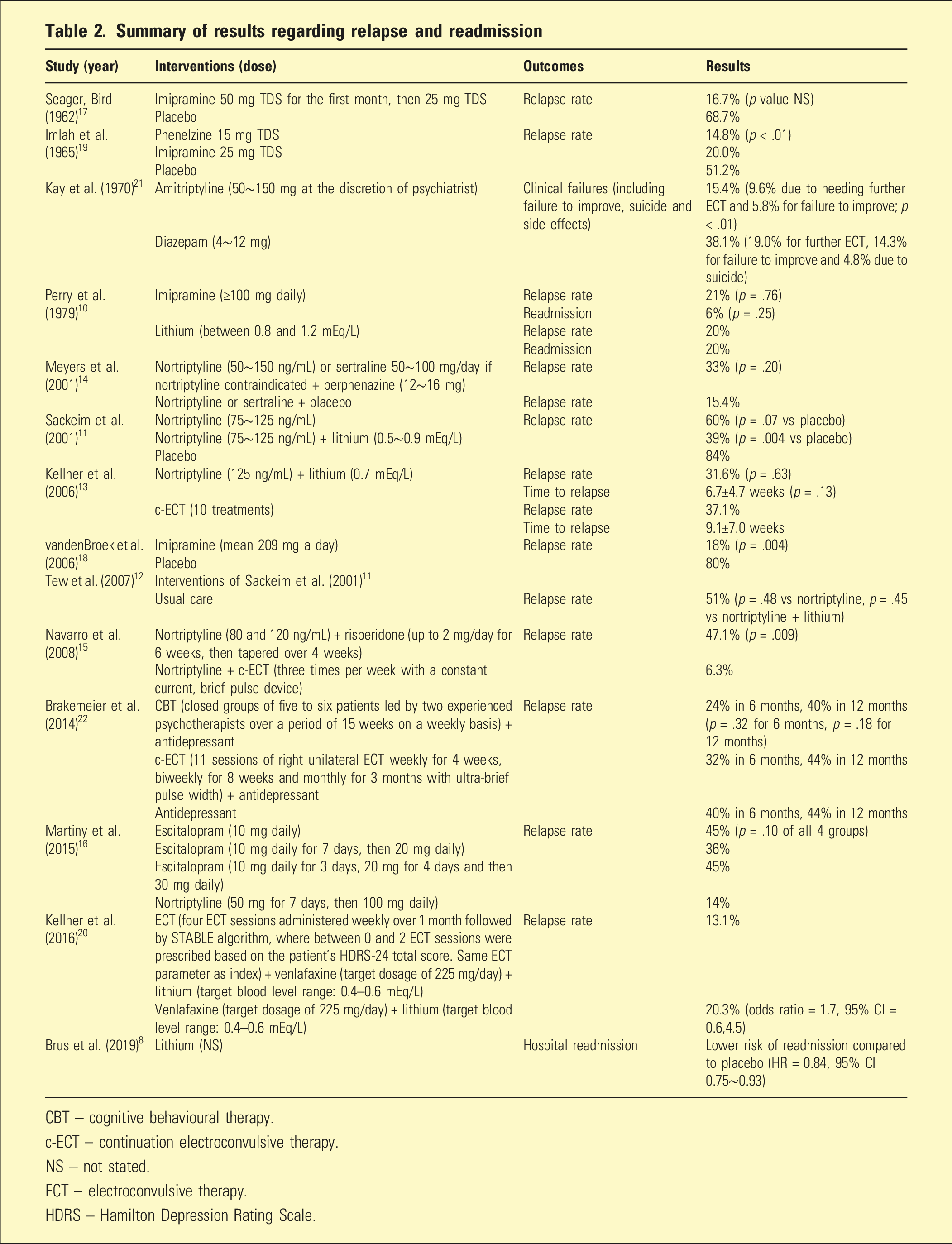
CBT – cognitive behavioural therapy.
c-ECT – continuation electroconvulsive therapy.
NS – not stated.
ECT – electroconvulsive therapy.
HDRS – Hamilton Depression Rating Scale.
Summary of results regarding depression severity

CBT – cognitive behavioural therapy.
c-ECT – continuation electroconvulsive therapy.
NS – not stated.
ECT – electroconvulsive therapy.
HDRS – Hamilton Depression Rating Scale.
Lithium
There were three studies that explored the efficacy of lithium in preventing relapse, where two studies were comparing against placebo8,9 and one against imipramine. 10 In two of the studies, there were no suicides in the lithium group and a Fisher’s test demonstrated that patients on lithium were less likely to die by suicide than placebo (p = .014).8,10 In a large-scaled national cohort study, lithium also lowered the risk of hospital readmission compared to placebo (hazard ratios = 0.84, CI 0.75–0.93). 8 Furthermore, a well conducted double blinded RCT reported that the lithium group had lower HDRS scores that became statistically significant by 52 weeks (p < .01), and lower affective morbidity by 26 weeks (p < .01) compared to placebo. 9 This trial recommended maintaining lithium for at least a year after ECT to reach its maximum efficacy. 9 In the study comparing the effect of lithium against imipramine, although relapse rates were similar (20% and 21%, respectively), the patients on lithium had more severe relapse that required rehospitalisation, while participants on imipramine were generally treated with increased doses of the drug on an outpatient basis. 10
Nortriptyline
There were two studies that investigated the combination therapy of lithium + nortriptyline, with one comparing to placebo11,12 and one comparing to c-ECT. 13 The large-scaled RCT compared the combination therapy against c-ECT, and both groups had limited efficacy with more than half of the participants either experiencing relapse or dropping out of the study. Of those who completed the 6 month trial, relapse rates were 44.6% for c-ECT and 40.5% for pharmacotherapy and of those who relapsed, average time to relapse was 9.1 ± 7.0 and 6.7 ± 4.7 weeks, respectively (t61 = −1.53; p = .13). 13
One study compared the combination therapy against nortriptyline monotherapy and placebo.11,12 One of the articles 12 was an extension of the other 11 to further compare the efficacy of protocolised pharmacotherapy against usual care. The trials demonstrated that combined pharmacotherapy was superior to both monotherapy (p = .04) and placebo (p < .001), but not usual care (p = .45) throughout the 24 weeks. Rates of relapse were 39% for combination therapy, 60% for nortriptyline and 84% for placebo. In terms of patients treated with usual care, which was generally some form of pharmacotherapy of selective serotonin reuptake inhibitor (SSRI), TCA or venlafaxine with only one patient receiving c-ECT, the relapse rate was 51%. 12
Two RCTs explored the effect of nortriptyline for psychotic depression. One study compared the combination therapy of nortriptyline of 50 to 150 ng/mL and perphenazine of 12 to 16 mg to nortriptyline monotherapy for 6 months. 14 In this double blinded study, participants were given sertraline 50 to 100 mg per day if nortriptyline was contraindicated. Relapse rates were 33.0% for combination therapy and 15.4% for nortriptyline monotherapy (p = .20). The other study was single blinded, and compared the efficacy of nortriptyline at a dose of 80 to 120 ng/mL combined with risperidone up to 2 mg a day for 6 weeks then tapered over 4 weeks, with nortriptyline and continuation ECT over 2 years. 15 Combination therapy with c-ECT demonstrated significantly lower relapse rates at 6.3%, while that of pharmacotherapy only treatment was 47.1% (p = .009).
Escitalopram
There was one 25-week RCT with small sample size that investigated the effects of three different doses of escitalopram and nortriptyline. 16 The study could not demonstrate a statistically significant difference between all four groups in terms of risk of relapse, defined as HDRS score of 16 or above present for 14 days. It was noted that participants on nortriptyline had a lower risk of relapse than those on escitalopram on an 8% statistical significance level. However, the study portrayed a poor outcome overall as a third of all participants relapsed and treatment was successful only in another third.
Imipramine
Overall, there were three RCTs that explored imipramine and two of them investigated the effects of imipramine against placebo. In one study, imipramine markedly reduced the rate of relapse (16.7% in imipramine group and 68.7% in placebo). 17 The other RCT explored the efficacy of imipramine against placebo in patients with antidepressant failure before a successful course of ECT treatment. 18 This study also showed that imipramine reduced the risk of relapse (18% in the imipramine group and 80% in placebo), with Cox regression analysis revealing a significant reduction of relapse risk at 85.6% (p = .007). The efficacy of imipramine was also seen in HDRS scores. For the placebo group, scores increased from mean 5.9 ± 3.81 at baseline to 14.7 ± 9.69 at the endpoint, while for imipramine group, it was from 4.9 ± 2.53 to 8.0 ± 9.21. The final study investigated imipramine, phenelzine and placebo during and 6 months post-ECT. 19 Relapse rates at 6 months were significantly lower in patients with antidepressants: 20.0% for those on imipramine, 14.8% for phenelzine and 51.2% for placebo (p < .01).
Venlafaxine
There was one large-scaled RCT investigating venlafaxine as continuation treatment of depression to prevent relapse. 20 Kellner et al. compared the response of patients receiving ECT, venlafaxine and lithium to those receiving only venlafaxine and lithium. After 24 weeks, mean HDRS for ECT + medication group was 5.5, while that of medication only group was 9.4 (p = .004). Additionally, 20.3% of the medication only group relapsed while the rate was 13.1% for the ECT + medication group, resulting in an odds ratio of 1.7 with a 95% confidence interval of 0.6 to 4.5.
Amitriptyline
There was one RCT exploring the efficacy of amitriptyline against diazepam as the control group. 21 This study measured numerous outcomes. One was clinical failures, which were defined as any reason for the participant to be removed from the trial, including relapse, lack of satisfactory progress and serious side effects. This rate was lower in the amitriptyline group at 15.4%, compared to diazepam being 38.1% (p < .01). Another outcome was depression severity scores of mood rating, HDRS and two additional self-rating scales, Beck Depression Inventory and Lubin’s Depression Adjective Check Lists. Although there were statistically significant differences on all four measures in favour of amitriptyline at 1 month (p < .05 for mood and p < .01 for HDRS, Beck and Lubin), this was not seen at four and 7 months especially perhaps as many participants were withdrawn from the trial for being unwell.
Psychotherapy
There was one RCT that studied the effect of group CBT after a successful course of ECT. 22 There were three intervention groups: one with antidepressant regime according to depression treatment guidelines with group CBT, another with antidepressant treatment and continuation ECT and the other with only antidepressant treatment. Participants in the group receiving CBT and medications demonstrated higher rates of sustained response, defined as neither relapse nor dropout occurring, compared to both the ECT + medications group (p = .02 at 6 and 12 months) and medication only group (p = .05 at 6 months and .06 at 12 months). However, there was no difference between the group in terms of rates of relapse (p = .32 at 6 months and .18 at 12 months).
In this review, five studies were performed in the twentieth century.9,10,17,19,21 Compared to the newer studies, these studies frequently did not clarify the definitions of depression, relapse or remission, or the ECT parameters the participants received. This makes comparing with other studies more difficult and can blur the conclusions. Despite these limitations, strengths in their methodology exist, including a reasonable duration for all studies and most, except one, 19 specifying blinding measures, so the results still contribute important information to draw conclusions.
Discussion
This paper reviewed fifteen studies on MDD relapse prevention after achieving remission from an acute course of ECT. The findings demonstrate that continued pharmacotherapy, with most medications studied, consistently resulted in better outcomes than placebo, although notable relapse rates were still demonstrated. Similar to the discussion in the RANZCP guidelines, which recommended an antidepressant with or without lithium, the interventions explored in the studies were mostly limited to pharmacotherapy with antidepressants and lithium. Lithium was investigated the most, demonstrating good outcomes either as monotherapy or combination therapy with nortriptyline or venlafaxine. Combination of nortriptyline and lithium was more efficacious than monotherapy and resulted in similar outcomes to c-ECT in one RCT. For patients who do not wish to receive c-ECT, this may be a preferable option. However, c-ECT combined with pharmacotherapy of venlafaxine and lithium demonstrated an additional benefit compared to pharmacotherapy alone. The combination of venlafaxine and lithium produced similar effects of preventing relapse to nortriptyline and lithium, and this could be of importance to patients given the potentially more problematic adverse effect profile of nortriptyline. These results support the RANZCP consensus, that venlafaxine should generally be chosen for post-ECT prophylaxis, with consideration of lithium augmentation. 5 Escitalopram failed to show a favourable outcome in reducing the risk of relapse, while amitriptyline and imipramine were successful in lowering both relapse rates and depression severity scores. There was only one study on non-pharmacological treatment, demonstrating that group CBT significantly improved rates of sustained response but not that of relapse.
Along with choosing the right medication, the next issue is finding the right dose. Medication doses used in the studies, if stated, are all considered to be within the recommended therapeutic ranges (except for two of the older studies which had higher serum lithium level targets than typical contemporary clinical practice9,10) and the most commonly utilised doses were steady-state levels of 125 ng/mL for nortriptyline and 0.7 mEq/L for lithium.11–13 There was one study exploring different doses of a medication. 16 This study failed to demonstrate a difference between the three groups receiving different doses of escitalopram. One reason for this is a small sample size as the groups were comprised of 10 or 11 participants. This also emphasises the importance of patient-tailored dosing based on clinical judgement.
Relevant studies that did not meet the inclusion criteria supported this review’s findings. A retrospective audit that included participants with bipolar affective disorder reported that relapse rates within 6 months were lowest at 16% when managed with lithium + antidepressant compared to other commonly prescribed pharmacotherapy. 24 This class effect of antidepressants in combination with lithium was further portrayed in the RCT by Prudic et al., which included participants with bipolar depressive episodes, and it demonstrated that treatment with either venlafaxine + lithium or nortriptyline + lithium was equally effective in preventing relapse (p = .55). 25 Another pilot study, which also included participants with psychotic features of depression, showed that sertraline was successful in significantly reducing relapse rates (12.5% in those who commenced after four sessions of ECT, 28% in those after 8 sessions and 67% in placebo). 26 A pilot study by Fenton et al. supported the trial conducted by Brakemeier et al. regarding the benefits of CBT as most participants had lower depressive symptoms with CBT combined with c-ECT. 27
Treatment resistant depression is often classified as a failure to achieve a suitable response to two or more adequate courses of pharmacotherapy. Management of treatment resistant depression is complex in that the condition is heterogenous, due to the influences of biopsychosocial factors. This potentially leads to different responsivities to treatment and increases the importance of patient-tailored management and holistic approaches. This aligns with results from the trial of Brakemeier et al., where participants who received psychotherapy and an antidepressant demonstrated significantly higher rates of sustained response, compared to those without psychotherapy. 22
Conclusion
From the findings of this review, some recommendations can be made. Clinicians aiming to reduce the risk of relapse after a successful course of ECT could consider lithium, due to the reasonable amount of supporting evidence. Having shown efficacy in multiple studies, nortriptyline or venlafaxine could be considered, making sure to undertake a risk-benefit analysis to tailor the treatment to each patient. Other options with less supporting evidence include imipramine, phenelzine, amitriptyline and CBT.
Research in the field of non-ECT methods to prevent relapse after ECT remains in its infancy. Given the number of antidepressants available, not many have been studied despite the importance of them in preventing relapse. This can influence the choice of antidepressants, with more considerations of venlafaxine and nortriptyline as first choice. Antidepressants possibly have a class effect with no significant difference in efficacy, as demonstrated in the study of Prudic et al. comparing nortriptyline + lithium to venlafaxine + lithium. Therefore, it is important to tailor the choice of antidepressants individually for patients to tolerate long term, rather than basing it on the limited evidence available. Further exploration is needed for a wider variety of antidepressants, especially comparing the newer ones with better side effect profiles, mood stabilisers other than lithium, antipsychotics, combination therapy and non-medication options, including psychotherapy and brain stimulation treatments other than ECT.
Footnotes
Author contributions
Minji Song: Methodology, formal analysis, investigation, writing – original draft and visualisation. Nathalie Hanna Launder: Methodology, writing – review and editing and supervision. Vivek H. Phutane: Writing – review and editing and supervision. Francine Moss: Supervision. Anne-Marie Keogh: Supervision. Terence W.H. Chong: Conceptualisation, methodology, formal analysis, writing – review and editing and supervision.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
