Abstract
Objectives
Eating disorders are serious psychiatric conditions that affect people of all ages. Many psychiatry trainees' first and only experience with eating disorders during training is their Child and Adolescent Psychiatry (CAP) rotation. This study aimed to explore the learning experience of psychiatry trainees working within an Eating Disorder Program (EDP) during their CAP rotation.
Methods
Fifteen trainees who participated in the EDP were recruited to complete an online survey and focus groups; a thematic analysis design was used to identify themes emerging from their responses.
Results
Themes emerged from the trainee learning experience of working in the EDP around what they found they learnt, what aided that process, what was difficult, and recommendations for future improvement.
Conclusions
This study provided insight into the trainee experience in an EDP as one example of how trainees can learn about eating disorders and one way that could inform future workforce and training initiatives.
Keywords
Eating disorders are complex and potentially life-threatening conditions requiring specialised psychiatric treatment that can occur at any age with a peak incidence in adolescence.1,2 A large 10-year longitudinal study reported that children and adolescents had a 6.7% lifetime prevalence of developing an eating disorder. 2 Despite the prevalence and risk of mortality associated with eating disorders, there are no mandatory eating disorder Entrustable Professional Activities (EPAs) that psychiatry trainees are required to undertake as part of the RANZCP Fellowship Program. 3 Eating disorder EPAs are available to be completed as part of elective rotations in a specialist eating disorder service, or in addition to mandatory EPAs during another rotation. This touches on the greater ongoing debate around a specialist versus generalist approach to psychiatry training in Australia and New Zealand, which is outside of the scope of this paper. 4 Regardless, at present it is not possible for all psychiatry trainees to work within a specialist eating disorder service. Therefore, exposure to clients with an eating disorder commonly takes place during the second and third years of training in the Child and Adolescent Psychiatry (CAP) rotations given the peak age of incidence of these disorders. 2
There is limited research into the trainee experience of working with young people with eating disorders and their families. There is also little evidence for how such experiences impact trainees’ perceived learning and comfort in working with clients experiencing an eating disorder following such a rotation and transitioning to fellowship.
Qualitative study designs can be used to explore these questions and have previously been used in examining the trainee experience conducting family therapy within a CAP setting and regarding the trainee experience of supervision.5,6 Therefore, a qualitative design was chosen to examine the psychiatry trainee learning experience working within an Eating Disorder Program (EDP) during their CAP rotation. Trainees participated in the EDP within a tertiary community-based child and youth mental health service (CYMHS). In this program, Stage 2 and 3 trainees take on at least one client with an eating disorder. They are supported by the lead psychiatrist and the two senior EDP coordinators who oversee all clients with an eating disorder attending the service. The coordinators also manage the EDP team, who are available to support all clinicians and trainees within the service. The EDP-specific team consists of a dietician, family peer specialist, youth peer worker, and a rotating roster of the CYMHS nursing staff who are available to conduct physical health monitoring. Once a client is accepted into the EDP they are offered a first family meeting, where the EDP multi-disciplinary team (MDT) attends. Following this, the trainee will continue to see the client and their family with support available from the EDP coordinators and team. On a case-by-case basis, a trainee may also have the opportunity to work alongside an allocated co-clinician from CYMHS.
This paper aims to contribute a greater understanding of the learning experience of the trainees within an EDP and how this process could be improved to support their learning.
Methods
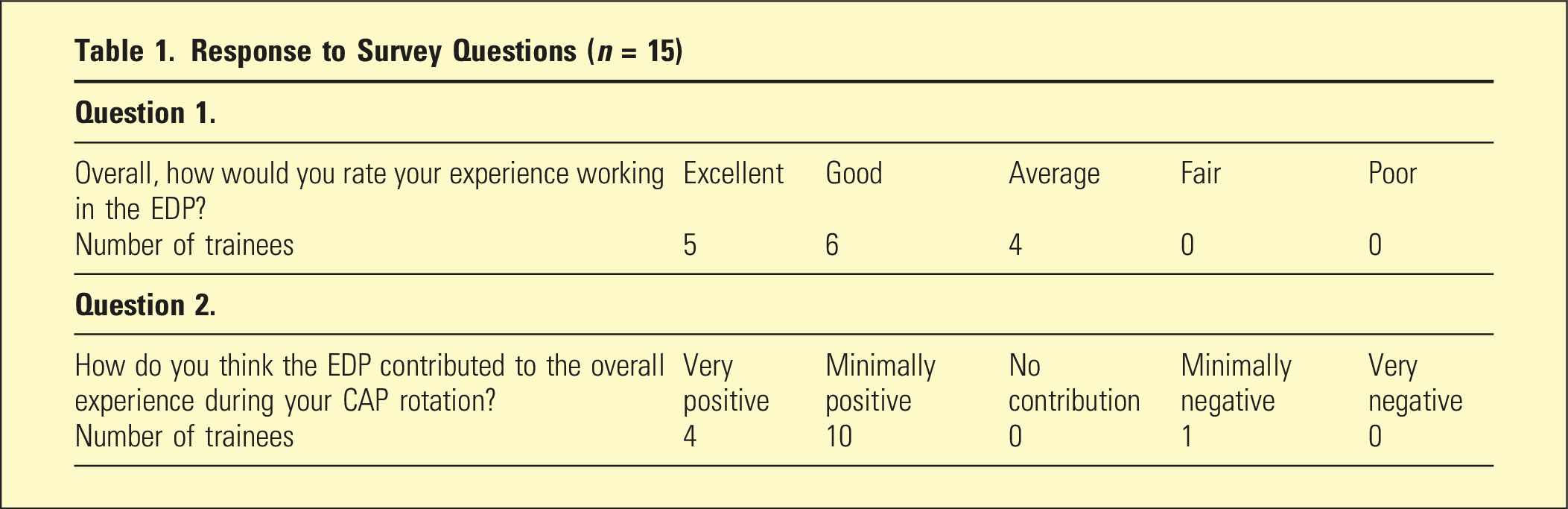
A qualitative study design using thematic analysis was used for this study.7,8 This was further informed by basic quantitative data regarding the trainees experience within the EDP. 9 A total of 15 trainees were identified as having worked in the EDP in the preceding 12 months and were invited to participate in the study via email. All 15 trainees agreed to participate, provided informed consent, and completed the initial online survey based on the survey used by Cheah, Hopkins, and Whitehead. 5 The survey consisted of two Likert rating scale questions, seven yes/no questions regarding their rotation, and seven open-ended questions relating to their experience. Nine trainees also opted-in to participate in one of three focus groups. The focus groups were conducted by the corresponding author in a semi-structured interview format that allowed the participants to expand further on the themes identified within the online survey. The interview questions orientated the trainees to reflect on broad areas of their experience. These included the impact of their experience on their learning, what the program provided to support their learning, difficulties in the process, and what improvements could be suggested. The focus groups were audio-recorded and transcribed verbatim for thematic analysis.
Responses were coded and thematically analysed to uncover the potential benefits and issues of the trainee learning experience working in the EDP. Major themes were identified and elaborated on using an established thematic analysis six-step coding approach. 7
Availability of data and materials
Survey questions, detailed methodology, and data are available from the corresponding author on request.
Results
Response to Survey Questions (
Thematic analysis
Description of Emerging Themes
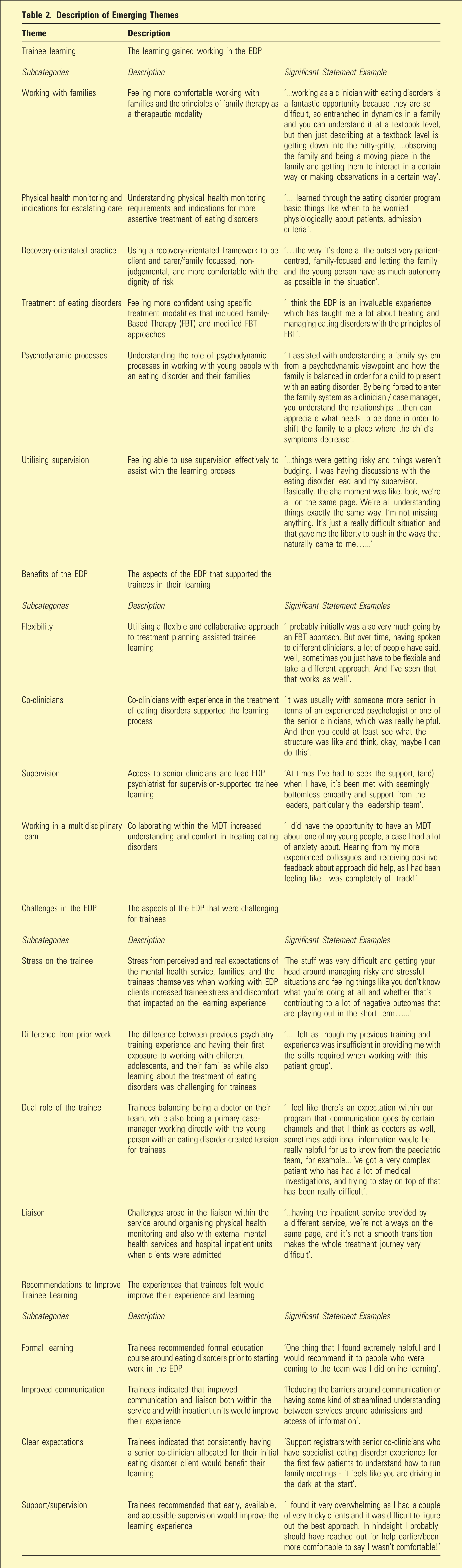

Discussion
The qualitative findings of this study shed light on the learning experience of psychiatry trainees working with the EDP, with themes emerging around what trainees felt they learnt, what aided that process, what hindered their learning, and what they recommended for future trainees. The emerging subcategories within these themes were of interest as they identified areas where trainees felt they learnt the most. These themes indicated trainees had not only learnt the skills specific to treatments of eating disorders but also broader concepts within psychiatry. Themes of learning to work with families, recovery-orientated practice, and working with a psychodynamic focus were areas of learning that emerged from the trainee responses. These findings imply that the EDP was felt to be a way to learn a range of skills required to work with clients with an eating disorder, as well as learn more broadly applicable skills in psychiatry.
Trainees identified specific aspects of the EDP that aided this learning, with themes emerging around the role of supervision, observation of senior clinicians, working with co-clinicians, and working within the MDT. Trainees found benefit from not only working with a lead EDP psychiatrist but also through interdisciplinary supervision with the two EDP coordinators. This extended to trainees describing benefits from working directly alongside their co-clinicians from CYMHS. These concepts could be considered in future training. Utilising interdisciplinary supervision, co-clinicians, and an MDT while within a CAP rotation was felt by trainees to aid the learning experience and this could inform ways of expanding access to training opportunities in the future.
Conversely, there were aspects of working in the EDP that trainees felt detracted from the overall learning experience. One trainee felt that the EDP negatively impacted on their experience during their CAP rotation, as indicated by the quantitative data. This was supported by themes that emerged in the qualitative data around difficulties with the stress felt working with eating disorder clients, the differences from their previous experience in psychiatry, and difficulties in communication and liaison. Themes for improvement to the learning experience evolved from trainees’ proposed solutions to these difficulties. Trainees felt that adding formal training and orientation prior to the EDP would address some anxiety around starting to work with eating disorder clients and provide a theoretical basis for the work. Better utilising the available supervision, having an allocated senior co-clinician, and outlining clear expectations of the trainee role at the outset were also themes that emerged for improvement in response to feeling stressed or uncertain in their role.
Strengths and limitations
A strength of this study was that it was able to use a combination of open-ended survey question design and focus groups to identify themes around trainee learning where future support and training could be directed to better equip trainees with knowledge of eating disorders in the future.
However, there were also several limitations that could limit its generalisability beyond the specific EDP described. The authors and the trainees recruited for the study had personal experience working within this EDP in different capacities. The personal experience of the authors was reflected on during the coding process, and their positions within the service and own experience working with the EDP were used in analysing the themes as they emerged. This knowledge was not only used to limit ‘cherry-picking’ of only positive themes but is also acknowledged as a source of potential bias in thematic analysis.
Another limitation is the potential lack of generalisability to services with a different model of care for the treatment of eating disorders. While the themes and principles may be applicable to other service models, this was not specifically investigated in the current study.
Conclusion
Eating disorders are a complex group of mental health conditions increasing in prevalence in Australia that will require a psychiatric workforce with the skills and confidence to work in this area. The findings of this study demonstrate that working within the EDP as part of their CAP rotation was perceived by trainees as a way to learn skills needed in the treatment of eating disorders. Trainees found this work to be stressful, complex, and different from other experiences in psychiatric training. Providing further opportunities for trainees to work with clients with eating disorders during CAP rotations could help reduce trainee apprehension working in this area and assist with future workforce and training development.
Footnotes
Disclosure
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: The authors were employed by the service where this research was carried out. There is no other conflict of interest.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical statement
This study received ethical approval from the Alfred Health Human Research Ethics Committee.
