Abstract
Objective
There are few studies on the efficacy and acceptability of psychotherapy conducted via telehealth technology for people with personality disorder. This study aims to examine clinician perspectives on virtual psychotherapy.
Method
Twenty multidisciplinary mental health clinicians (85% female, average age 42 years) with at least 2 years of experience in telehealth psychotherapy contributed quantitative and qualitative ratings of acceptability and efficacy of this modality.
Results
Likert scale ratings (1 = not, 5 = very) demonstrated high client acceptability (mean = 4.0), effectiveness (4.0) and high clinician acceptability (4.2) and sustainability (4.2). Three recommendations emerged from qualitative analysis: prioritising frame establishment, ensuring client safety online and maximising alliance-enhancing strategies.
Conclusions
This study, which collected quantitative and qualitative ratings of virtual psychotherapy, found that telehealth psychotherapy can be effective and acceptable for people with personality disorder. Strategies associated with success included strong governance, secure technology and careful attending to relationship management.
Personality disorders are a prevalent mental health disorder, with 7.8% of the global population estimated to meet criteria. 1 Personality disorders are characterised by complex difficulties in both the interpersonal and intrapersonal lived experience. 2 An estimated 40 to 50% of psychiatric patients have a diagnosable personality disorder. 3 Therefore, it is vital that mental health services consider effective, accessible and evidence-based psychotherapy treatment options.
Treatment guidelines for people with personality disorder recommend psychotherapy as a first line of treatment.4,5 The global coronavirus pandemic (Covid-19; declared 11 March 2020-2023) required services to rapidly pivot to virtual platforms to allow continuity of care. Emerging research suggests that people with personality disorder presented to hospital more frequently during this time compared to other groups, 6 demonstrating the need for rapid community-based, accessible and effective interventions for this population.
One example rapid treatment option is the Project Air Strategy (2015) brief intervention clinic. 7 Grenyer and colleagues (2018) have previously reported benefits of this intervention with reduced re-admissions and inpatient bed days. 8 Further, Huxley and colleagues (2019) have reported on improved client outcomes including quality of life and reducing suicidal ideation. 9 Stepped models of care provide therapy options suited to the individuals acuity, presenting concerns, readiness and willingness to engage in treatment. 10 As a first step, brief and rapid follow up psychotherapy provides treatment at the time of acute distress, enabling diversion from emergency and acute services and the commencement of recovery-oriented psychotherapies. 11
This study aimed to explore mental health clinicians’ perspectives on the virtual delivery of psychotherapy to people with personality disorder.
Methods
Participants
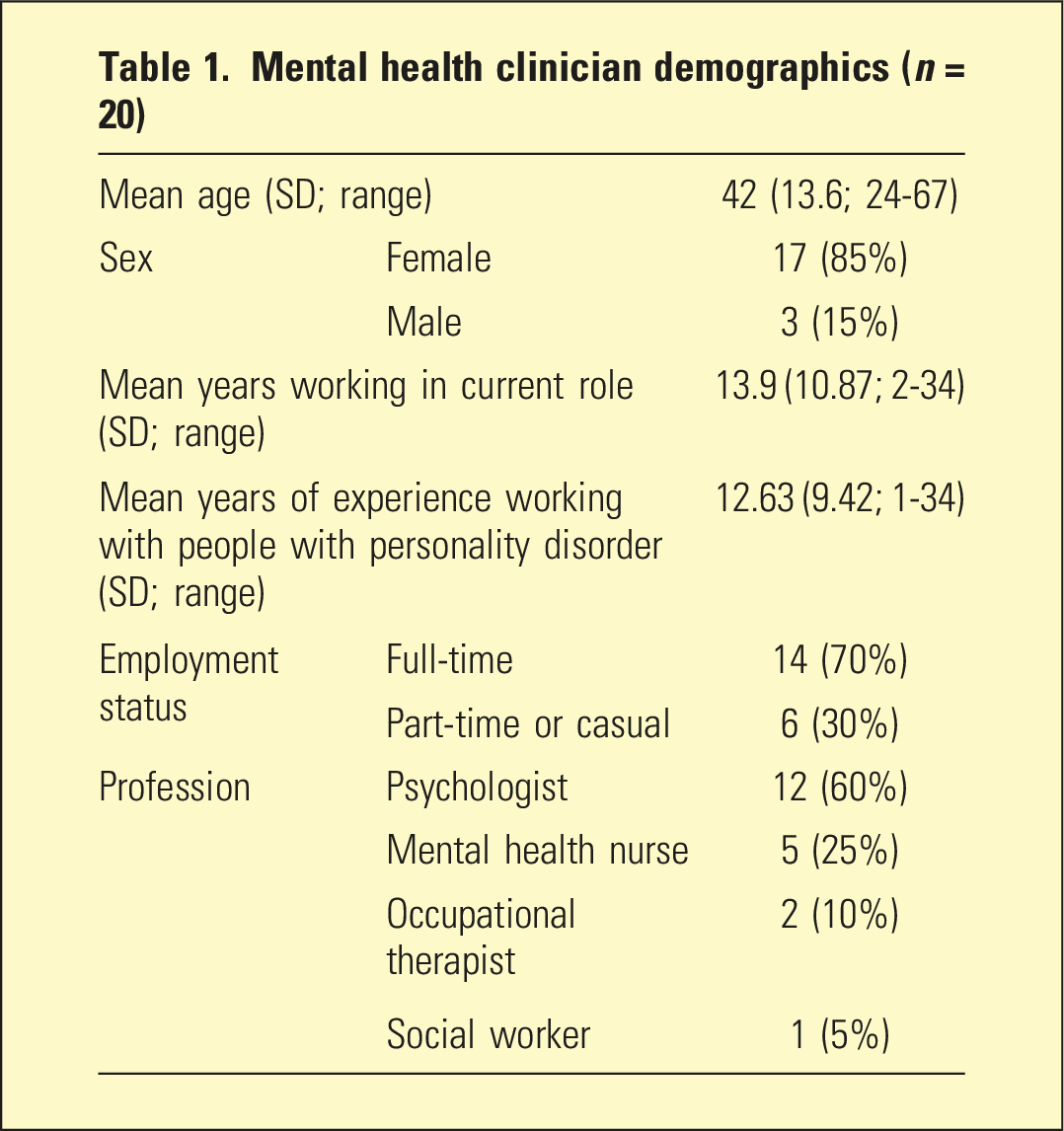
A total of 20 multidisciplinary mental health clinicians (85% female, average age 42 years) were recruited from a snowball sampling call out for volunteers. Participants needed to have at least 2 years experience in telehealth psychotherapy.
Mental health clinician demographics (n = 20)
Psychotherapy
Clinicians provided written informed consent following Institutional Review Board approval. Psychotherapy was a structured one-month brief intervention. The publicly-available Project Air Strategy (2015) manual was utilised. 7
Procedure
Clinicians who consented to the research completed a survey and semi-structured interview. The survey included demographic and service-based questions, and brief ratings as described below. Interviews were conducted between November to December 2022, were audio recorded and transcribed verbatim.
Measures
Acceptability and perceived efficacy
Participants were asked about the acceptability of the virtual brief intervention from the perspective of the client and clinician on a Likert scale from 1 (not) to 5 (very). Participants were also asked how effective the virtual delivery of the brief intervention was from the perspective of the client from 1 (not) to 5 (very). Asking clinicians on their perspective of the clients’ experience has been used previously in the literature as a proxy-measurement of client acceptability. 12 Finally, participants were asked how sustainable they thought telehealth psychotherapy was for the service from 1 (not) to 5 (very).
Semi-structured interview
Participants provided their insights into using telehealth modality for the brief intervention. Participants were asked questions on the acceptability, efficacy, sustainability, challenges and opportunities of telehealth psychotherapy and recommendations. The interviews were an average of 31 min duration (range = 12–54).
Statistical analysis
Quantitative data was analysed using descriptive statistics. Qualitative data was analysed using a Husserlian phenomenological approach. 13 Approximately 20% of the qualitative data was coded by two researchers, and discrepancies were discussed until consensus was reached. Inter-rater reliability was assessed on agreement of theme ratings, with Cohen’s kappa coefficient being K = 0.91, indicating a very strong level of agreement.
Results
Efficacy
Participants rated their client’s experience of virtual care as highly effective (M = 4.0, SD = 0.86; range = 3-5) and acceptable (M = 4.0; SD = 0.86; range = 3-5). Participants also reported that they felt the intervention was acceptable from their perspective as a psychotherapist (M = 4.2; SD = 0.77; range = 3–5). Further, participants reported that the intervention is sustainable (M = 4.2; SD = 0.77; range = 3–5).
Recommendations for delivery of virtual care
Selected examples of significant statements and formulated meanings regarding conducting psychotherapy in an online virtual environment

Recommendations for conducting virtual telehealth psychotherapy

Theme 1: The frame – what makes it work
In addition to the usual frame considerations documented in the Project Air Strategy (2015) brief intervention manual,
7
participants reported that it is essential to orient the client to the specific requirements of psychotherapy delivered via telehealth. It was important to consider the physical location where the client was connecting (e.g. a confidential location free from distractions), where the clinician was connecting, and the shared virtual platform. Practical considerations, including choice of an endorsed platform with sufficient clinical features, enhanced the virtual therapy: ‘there were things we could do online that we might not have done as easily face-to-face, like sharing screens with resources and putting YouTube videos up and emailing resources before and after the session. Particularly the kind of [brief intervention] therapeutic fact sheets and handouts, we were able to do that in the online format, and I think that actually made it more effective for some’.
Theme 2: The holding environment – what makes it safe
Participants commented on the need to carefully consider telehealth risk assessment and management, including ensuring clear risk escalation procedures to support decision making. This also included strong senior endorsement to support the telehealth modality. Participants commented on the need for training in how to use the technology, and how to enhance clinical effectiveness via telehealth: ‘I think for me the biggest things that I think are important considerations in terms of personality disorders and the online space is just the therapeutic relationship and how you keep that attachment and accountability and get that person to really feel held by the clinician and team in the online space. I think finding a way to do that and teach that is really going to be the key to actually getting effective services for people with lived experience of personality disorder to be able to work online… Like, I think if we can do that, I think all the other stuff will fall into place’.
Theme 3 – The therapeutic alliance – what makes it effective
Participants spoke about solutions to overcoming alliance challenges via telehealth, including being more dyadic, focussing on attunement, being creative in enhancing engagement, inviting regular feedback and being mindful of the increased risk of misunderstanding and invalidation. There may be a need to work harder to ensure good communication, and also recognise the possibility of inadvertent disclosure (e.g. potential intrusion of other people). Participants also commented on the importance of maintaining therapeutic boundaries and guiding clients to set up their home-therapy space to maintain the therapeutic value of the intervention. Participants suggested that once engagement and rapport was established, the telehealth psychotherapy could be both effective and acceptable: ‘if we got the relationship and we got the engagement, the efficacy was there. If you had someone who was signed on, who was rearing to go, that was happy to do it, that we’d set it up, did the homework between sessions, then the efficacy was there’.
Discussion
The current study explored the efficacy, acceptability and recommendations of a brief psychotherapy intervention for people with personality disorder delivered via telehealth. Overall, clinicians reported that the virtual intervention was efficacious and acceptable. Qualitative analysis identified core themes centring around The Frame, The Holding Environment and The Therapeutic Alliance. Throughout these three core themes, participants discussed the challenges, opportunities and recommendations (see Table 3) for telehealth psychotherapy.
Our findings are consistent with previous reviews suggesting virtual technologies may be efficacious for people with lived experience of borderline personality disorder (BPD). 14 For example, a recent study found equitable outcomes when comparing telehealth to in-person treatment for BPD patients in a partial hospital setting. 15 Further, studies have found positive outcomes in delivering Dialectical Behaviour Therapy group programs online.16,17 Our study provides further evidence to suggest that telehealth options in the treatment of people with personality disorder are efficacious and acceptable, including for brief community-based intervention during times of crisis.
Despite the benefits and ongoing high use of telehealth interventions, 18 this modality presents unique challenges for both the clinician and client. Our results echo previous reports of clinician anxiety in managing risk through telehealth. 19 Whilst the risk is often equitable to an in-person modality, the reduced sense of control in managing the therapeutic environment may heighten the need to support clinicians with clear guidance (see Table 3) and training.12,18,19 Whilst the therapeutic content and best-practice clinical care is transferable across modality, it has been suggested that treatment programs for personality disorders need careful set up to ensure telehealth is successful, 17 and the opportunities of virtual care are maximised. This includes a particular focus on adapting to the unique engagement, privacy, confidentiality and safety needs of telehealth, 17 and the interpersonal challenges inherent in the treatment of personality disorder.
As reported by participants here, a working alliance is paramount in any therapeutic intervention. 20 A systematic review of telehealth modality across a range of mental health conditions suggests that the working alliance may be equitable; however, there is a specific need to consider whether this translates to particular disorders (such as personality disorders) that pose unique challenges to the therapeutic relationship. 21 A recent study surveying psychologists working remotely demonstrated the changed experience of therapy with the loss of some boundaries, impacts on the working alliance and new opportunities for engagement. 19 It was also found that therapists may need to work harder to maintain the therapeutic boundaries of the intervention focused on clinical change, rather than allowing this to be a general ‘check in’ supportive-only approach. These previous findings were extended in the present study, where clinicians provided specific recommendations to enhance the telehealth working alliance for personality disorders and maintain the therapeutic value of the intervention.
Clinician recommendations generated by the current study (outlined in Table 3) detail therapeutic approaches to enhance engagement and efficacy of the telehealth modality. The key qualitative themes parallel the recommendations: the importance of establishing a collaborative frame, the need for a safe holding environment for both client and clinician and a focus on establishing the therapeutic alliance. The success of the modality appears to rest on the client and clinician working together to create a shared virtual space that is engaging and therapeutic. Clinicians may be pivotal in guiding the client to prepare a home-therapy space, both in physical location and psychological readiness. Encouraging the client to take ownership of the session by preparing goals, discussion priorities and desired outcomes enhances engagement in the virtual modality and fosters agency which is a key therapeutic focus in the treatment of people with personality disorders.
This study has a number of limitations. This study focussed on a structured one-month psychotherapy approach, although clinicians had experience in treatments of a longer duration meaning these recommendations are likely also suitable for longer-term therapy. Use of telehealth is often convenient for client and clinician, which may present a bias in inflating ratings of efficacy due to this preference. Whilst the study included a sufficient sample size for qualitative research, future studies may benefit from evaluating the perspectives of a larger sample, including responses from more males. In addition, future research would benefit from seeking direct feedback from clients and measuring comparable outcomes to assess the effectiveness and acceptability of telehealth psychotherapy from multiple perspectives and using a broader range of outcome measures.
Conclusion
The present study investigated the perspective of mental health clinicians delivering a brief virtual intervention to individuals with personality disorder. Psychotherapy delivered via telehealth was found to be both effective and acceptable. This model of care has the potential to increase the scope of practice by offering treatment for those with personality disorder living in remote places, or with other prohibitive barriers to standard face-to-face engagement. To ensure efficacy of this intervention, there is a fundamental need to consider appropriate resourcing, guidelines and senior support. When clinicians feel supported by the service, are provided opportunities to reflect on building rapport virtually, and are provided resources that are therapeutically oriented, they can safely provide accessible and effective psychotherapy via telehealth to people with personality disorder.
Footnotes
Disclosure
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship and/or publication of this article: Project Air Strategy acknowledges the support of the NSW Ministry of Health. The funding body had no role in the study design, collection, data analysis and interpretation or preparation of the manuscript.
Ethical approval
The procedures and measures of this study were reviewed by an Institutional Review Board (the University of Wollongong Social Sciences Human Research Ethics Committee 2022/237) and participants provided informed consent for their data to be used in this evaluation.
Data Availability Statement
Participants gave researchers consent to use the data for this evaluation, but not for further distribution outside of the research team.
