Abstract
Introduction:
Haemoptysis is uncommon in toddler. Lower respiratory tract infections and foreign body are among the common causes.
Case Presentation:
We are reporting a case of a child presented to emergency department with complaint of mild haemoptysis, whom was later found to have a piece of broken satay skewer at the tonsillar region. The foreign body was removed during the procedure without any complication.
Discussion:
Foreign body ingestion, particularly a piece of broken satay skewer, is difficult to suspect without a proper history and eyewitness. Therefore, parent’s supervision is important. Emergency residents should have a high index of suspicion of foreign body ingestion in a child with vague symptoms.
Conclusion:
Foreign body is among the commonest cause of haemoptysis in an afebrile toddler. Acute haemoptysis in otherwise healthy toddler should alert the emergency residents about foreign body ingestion. History of food intake should be more thorough even if trivial.
Dear editor
Haemoptysis is uncommon in toddler. 1 Lower respiratory tract infection and foreign bodies are among the common causes. 2 However, unsuspected foreign body ingestion creates a diagnostic dilemma in emergency department (ED). Despite being careful, yet there is still a risk of foreign body ingestion by toddlers. We are reporting a case of a child presented to the ED with a complaint of mild haemoptysis, who was later diagnosed as a tonsillar foreign body.
Case
A 20-month-old girl was brought to the ED, complaining of cough with blood-stained sputum. She has no known medical illness or admission except for neonatal jaundice and allergic rhinitis under follow-up. Her symptom was well controlled with medication. Her gross development is appropriate for age. She was otherwise well prior to this current symptom. Around midnight, she had a cough with a streak of blood in her sputum, subsequently in her oral secretions. It was associated with a runny nose. She was otherwise active at home and taking orally well. There was no history of fever. There was no contact with tuberculosis patients. She has no history of other bleeding tendencies. Parents denied any possibilities of foreign body ingestion.
On examination, the child looked well, active and with normal vital signs. Her systemic examination was unremarkable, except for a mildly injected throat. Her blood investigations were normal except for her coagulation profile, whereby her activated partial thromboplastin time (APTT) was slightly prolonged (54 s; normal range: 35–45 s). Her chest x-ray (CXR) revealed no signs of foreign body with normal lung fields bilaterally. She was referred as mild haemoptysis for investigation and planned to be admitted for observation under paediatric team. Otorhinolaryngology (ORL) team was also consulted prior to admission in view of her underlying allergic rhinitis.
During the oral cavity examination by the ORL team, both tonsils were enlarged (grade 2), not inflamed, with no exudate, bleeding point or foreign body is seen. Endoscopy was planned to identify the source of bleeding.
The child was held by her mother, with the help of the accompanying nurse to restrain the child physically. The paediatric flexible scope was inserted through the nose until the area of nasopharynx and oropharynx. At the level of oropharynx, a small piece of satay skewer with a length of roughly 1 cm was found piercing the posterior part of the patient’s left tonsil. It was noted rubbing against the posterior pharyngeal wall causing inflammation of the raw area, possibly causing the per-oral bleed. The enlarged tonsil obscured the foreign body during the oral cavity examination. However, no active bleeding was noted over the injured part. The foreign body was removed immediately during the procedure using the Tilley forceps through the mouth without any complication (Figure 1). Other scope findings were unremarkable. On retrospective clerking, parents claimed to have fed her with satay, and she did complain of throat pain immediately after it but was not given attention. She was discharged on the following day with follow-up under paediatric and ORL clinics.
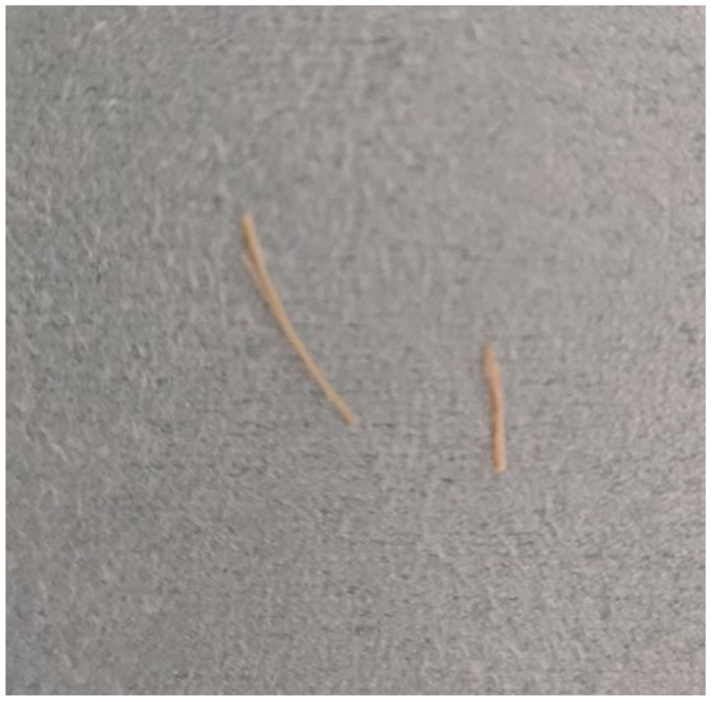
The broken pieces of a satay skewer made of midrib of coconut palm frond found at the tonsil (accidentally broken into two pieces).
Discussion
Foreign body ingestion among children is not uncommon. Food and non-food items ingestion have been documented well in various studies. In a study done way back in 1997 in Australia, coin ingestion was the most common non food item ingestion. Fish bone, nuts, carrot, apple, sausage and candy are food-based items commonly ingested by children less than 14 years old. 3 Considering the potential risk of foreign body ingestion in children in this age group, parents and doctors alike must always think of foreign body ingestion in any child presented with unexplained vague symptoms including haemoptysis, as we encountered in our case, which was due to a satay skewer.
Satay or also known as sate is a popular food in Southeast Asia. 4 There are safety issues of the skewers in the satay preparation (Figure 2). With its sharp point, it becomes a dangerous implement that may lead to poking the eaters’ tongue and throat. However, we have never come across foreign body ingestion from the broken pieces of skewers and stuck around the tonsils. Without the initial history of eating satay and unwitnessed foreign body ingestion, it is much more difficult to have thought about satay skewer as the foreign body.

Satay as one of the signature dishes in certain restaurants in Asia.
Parents’ supervision is the most important aspect of care to be given to a child who loves to eat satay. A toddler usually is unable to show obvious signs or symptoms of foreign body ingestion, unlike the older age group. Smaller children usually presented with more vague symptoms, including refusal to eat, crying, vomiting and drooling of saliva. Blood stain saliva may occur in 7% of cases only. 5 Emergency residents should have a high index of suspicion of foreign body ingestion in a child with vague symptoms. Pain may also be the only sign of unwitnessed foreign body ingestion. 6 Rarely, cases of halitosis, chronic sinusitis and recurrent epistaxis have been reported. 7 Tonsil has been the most common anatomical side of impaction.5,8 Thorough and careful examination of the oral cavity should be done in order not to miss any potential foreign body. As in our case, despite multiple oral examinations by emergency residents and ORL doctor, the foreign body was not detected until a proper scope was carried out. Potential limitations include small mouth opening and suboptimal oral examination in an uncooperative child. If needed, examination may be carried out by physically restraining the child with the help of both parents and nurses. Procedural sedation analgesia or conscious sedation may be required in extreme cases. 9 Although anxious parents always brought their unwell child to the hospital immediately after the onset of symptoms, there were cases of ED presentations even after 24 h. 5 In various studies, fish bone and meat have been the most common causes of ingestion causing the symptom.5,8 Satay skewers can also be a cause for those who eat satay.
Conclusion
Foreign body is still among the commonest causes of haemoptysis in an afebrile toddler. Acute onset of haemoptysis in otherwise healthy toddler should alert the emergency residents about foreign body ingestion. History of food intake should be more thorough even it may look trivial. Although satay is delicious, its broken pieces of skewers may be one of the foreign bodies in the oropharynx. ORL team referral may help to uncover this unusual foreign body.
Footnotes
Acknowledgements
The author(s) would like to thank School of Medical Sciences and Hospital Universiti Sains Malaysia, Universiti Sains Malaysia for their continuous support.
Author contributions
N.I.G. and S.M. were the initial doctors who clerk and saw the patient in our emergency department. S.M., M.F.M.S. and K.A.B. were involved in literature review and writing the manuscript. M.F.M.S. and K.A.B. handled the submission process. M.S.A.I. and I.M. were involved in the intervention of the patient, and contributing the scope finding.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship and/or publication of this article.
Availability of data and materials
All patient information is available from her case note in our hospital record unit and cannot be legally or ethically uploaded here.
Informed consent
Written informed consent for publication was taken from the patient’s caretaker using the standardized form given.
Ethical approval
No ethical approval was requested for this case. However, to maintain patient confidentiality, our case report did not include any data or picture that would have enabled identification of the patient.
Human rights
This case report was prepared according to the World Medical Association Declaration of Helsinki.
