Abstract
Objective
To investigate the clinical efficacy and incidence of complications in the treatment of adult congenital high scapula (Sprengel deformity) using the modified combined Woodward and Green surgical approach.
Methods
From January 2020 to January 2024, 9 adult patients with congenital Sprengel deformity were treated with the modified Woodward and Green combined procedure. There were two males and seven females, aged 18–35 years (mean: 23.5 ± 4.2 years), with 6 cases on the left and 3 on the right. The surgical procedure involved the modified combined Woodward and Green technique. Postoperatively, routine infection prevention, 4-weeks brace fixation, and rehabilitation guidance were performed. Shoulder appearance was evaluated using the Cavendish grading system; bilateral scapular height difference was measured; and shoulder function was assessed using the UCLA Shoulder Function Rating System, including pain, daily activity ability, range of motion, and muscle strength. Paired t-tests were used to analyze pre- and postoperative data with SPSS 22.0 software.
Results
All 9 patients were followed up for 12–36 months (mean: 24.11 ± 6.63 months). Postoperatively, shoulder appearance significantly improved, with marked reduction in scapular position, good correction of elevation and shrugging deformities, and near-normal shoulder contour. Cavendish grading improved significantly (p < 0.05). The scapular height difference decreased from 4.50 ± 0.67 cm preoperatively to 0.89 ± 0.77 cm at the last follow-up, and the UCLA shoulder function score increased from 23.44 ± 1.57 to 30.33 ± 0.67, with statistically significant differences (p < 0.001 for both).
Conclusion
The modified combined Woodward and Green procedure is a safe and effective treatment for adult congenital Sprengel deformity, significantly improving shoulder appearance and joint function. However, due to the small sample size and short follow-up period, future studies with larger samples and longer follow-ups are needed to accurately evaluate the long-term efficacy.
Introduction
Sprengel deformity, also known as Congenital high scapula, is a rare congenital malformation of the shoulder girdle, characterized by fixed elevation of the scapula, abnormal morphology, hypoplasia or atrophy of surrounding muscles, and limited shoulder abduction.1–3 Omovertebral bones are observed in 16%–55% of cases. 4 For pediatric patients, the main surgical approaches are the Woodward and Green procedures. 5 However, adult patients have fully matured skeletal development, often with severe deformities, poor soft tissue elasticity, and severe contractures, making downward relocation surgery less effective and prone to brachial plexus injury. Therefore, most scholars do not advocate treatment. Nevertheless, Sprengel deformity significantly affects appearance and shoulder function, and adult patients also have treatment needs.
To address the severe deformities and soft tissue contractures in adult patients, we modified the traditional Woodward procedure by combining the advantages of the Woodward and Green techniques, aiming to more effectively correct deformities, improve shoulder function, and reduce complications. This retrospective study analyzed the clinical and imaging data of 9 adult patients with Sprengel deformity treated with the modified combined procedure, with the objectives of: (1) evaluating the therapeutic efficacy, (2) assessing safety, and (3) analyzing improvements in quality of life.
Materials and methods
General data
Nine adult patients with congenital Sprengel deformity treated with the modified combined Woodward and Green procedure in our hospital from January 2020 to January 2024 were enrolled. There were 2 males and 7 females, aged 18–35 years (mean: 23.5 ± 4.2 years), with 6 left-sided and 3 right-sided cases. Comorbidities included congenital spinal deformity (7 cases: 3 with vertebral formation defects, 2 with segmentation defects, 2 mixed type), rib deformity (4 cases), and omovertebral bone deformity (2 cases).One patient underwent surgery for congenital scoliosis at another hospital 10 years ago. Because the patient lost the preoperative imaging data, the specific type of their congenital scoliosis cannot be accurately assessed.
All patients presented with varying degrees of abnormal shoulder appearance, elevated scapula, obvious elevation of the affected shoulder compared to the healthy side, and shrugging. Shoulder function was limited in abduction and elevation, affecting daily activities such as dressing and reaching. Six patients had varying degrees of shoulder and back pain.
Surgical procedure
All surgeries were performed under general anesthesia. Patients were placed in the prone position on a positioning pad with silicone protection for the face, allowing full exposure of the surgical field and intraoperative comparison with the healthy side. Nerve electrophysiological monitoring was used during the procedure.
The incision was made along the midline of the back from C4 to T9 spinous processes. Skin, subcutaneous tissue, and deep fascia were incised, and muscles (trapezius, rhomboid muscles) were dissected from their spinous process insertions. Dissection proceeded laterally to the scapular spine margin to expose and resect omovertebral bones or fibrous bands attached to the scapular superior angle, followed by release of surrounding restrictive structures. The supraspinous part of the scapula was subperiosteally resected, including the anteflexed and inverted portion. The upper trapezius was transected, and the scapula was pushed downward until the scapular spine was level with the healthy side. The inferior scapular angle was drilled, and a titanium cable fixation system was passed through to secure it to the rib at the same level. The trapezius, rhomboid major, and rhomboid minor muscles were then sutured downward to the lower spinous processes. The free edge of the upper trapezius was sutured, and the deep fascia was shifted downward for suture; redundant lower trapezius was folded and sutured.
After thorough hemostasis and saline irrigation, the wound was closed in layers.
Postoperative management
Postoperatively, antibiotics were administered prophylactically for 24–48 h, and a negative pressure drain was kept for 48–72 h. A protective brace was worn for 4 weeks. During immobilization, patients were instructed to perform finger, wrist, and elbow exercises to promote circulation, prevent muscle atrophy, and maintain limb function for subsequent shoulder rehabilitation.
At 4 weeks, the brace was removed, and a neck-wrist sling was used. Passive shoulder exercises (e.g., small-range pendulum movements) were initiated with therapist or family assistance, gradually transitioning to active exercises (e.g., pendulum exercises). At 6 weeks, wall-climbing, shrugging, and flexion-extension exercises were added, along with resistive training to promote shoulder function recovery.
Outcome measures and evaluation
Shoulder appearance and scapular height difference
• •
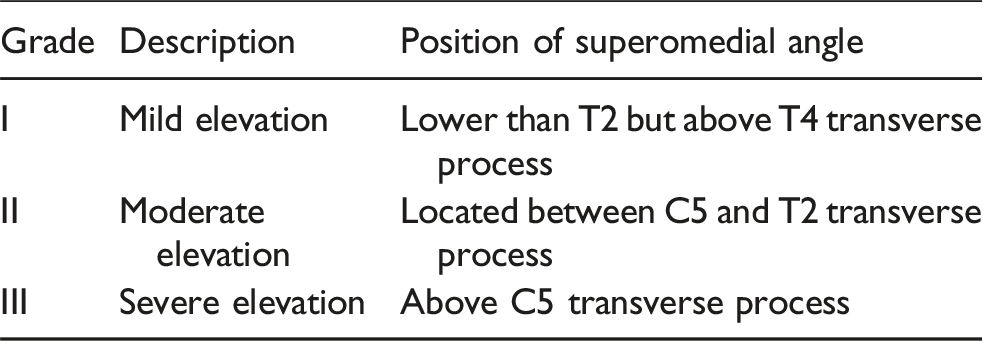
• •
Shoulder function
Shoulder function was evaluated using the UCLA Shoulder Function Rating System, 8 including pain, function, active forward flexion range of motion, flexion muscle strength, and satisfaction (total score 0–35, higher scores indicate better function).
Statistical analysis
Data were analyzed using SPSS 22.0 (SPSS Inc., USA). Rank sum tests were used for categorical variables, and quantitative data were expressed as mean ± standard deviation. Paired t-tests were used for pre- and postoperative comparisons. A p < 0.05 was considered statistically significant.
Results
All 9 patients were successfully followed up for 12–36 months (mean: 24.11 ± 6.63 months).
Shoulder appearance and scapular height difference
• • • •
Shoulder function
The UCLA shoulder function score increased from 23.44 ± 1.57 preoperatively to 30.33 ± 0.67 at follow-up (t = 12.218, p < 0.001).Shoulder abduction range of motion increased from 94.44 ± 8.82 preoperatively to 144.44 ± 8.82 at follow-up (t = 22.678, p < 0.001).
Complications
No severe complications such as nerve injury or shoulder function loss occurred. One patient developed superficial wound infection, which healed after antibiotic treatment and dressing changes. No internal fixation cable fractures were observed (Figures 1–4). ① The upper part of the scapula (already cut off); ② The trapezius and rhombus muscles pulled outward; ③ Subscapular angle (will be fixed with cables to the ribs after being pulled down). A patient with left congenital Sprengel deformity (Cavendish Grade Ⅱ) and congenital scoliosis. After the modified combined procedure, shoulder balance was achieved with improvement to Grade 0. A patient with right congenital Sprengel deformity (Cavendish Grade III) and postoperative congenital scoliosis. Postoperatively, bilateral shoulder balance was achieved with improvement to Grade 0. A patient with right congenital Sprengel deformity (Cavendish Grade Ⅲ) and congenital scoliosis. Postoperatively, bilateral shoulder balance was achieved with improvement to Grade 0.



Discussion
Eulenberg first reported 3 cases of congenital scapular elevation in 1863, 9 followed by Willett and Walsham’s anatomical description in 1880. 10 Sprengel and Kolliker reported cases and proposed the etiology in 1891, leading to the term “Sprengel deformity”. 4 The pathogenesis of Sprengel deformity remains unclear but is widely linked to abnormal scapular descent during embryonic development.2,11 Normally, the scapula originates in the cervical region and descends to the posterior thorax; disruption of this process by unknown factors leads to the deformity. Potential causes include neuromuscular developmental abnormalities, genetic regulation disorders, or maternal exposure to adverse factors, but definitive mechanisms require further study.
Key features include significantly elevated scapula with morphological abnormalities, affecting shoulder appearance (elevation, shrugging) and function (limited abduction/elevation), as well as psychological burden from deformity.
The deformity may occur alone or in conjunction with other abnormalities, the most common of which include Klippel-Feil syndrome, congenital scoliosis, rib malformations, tethered cord, or syringomyelia. 12 Among the 9 adult patients with Sprengel deformity reported by us, 7 were complicated with mild congenital scoliosis, and 1 was complicated with congenital scoliosis (having undergone surgery at another hospital without preoperative imaging data). Since all 7 patients had mild scoliosis that had no significant impact on their appearance, we only performed surgery for Sprengel deformity, which severely affected the appearance and shoulder joint function. It is worth mentioning that, in addition to our 9 cases, we have also received a case of congenital high scapula combined with severe congenital scoliosis. The patient has left high scapula, but the left side is a concave side of scoliosis. These two combined deformities have caused her shoulders to reach a relatively balanced state, so we did not perform surgery on her. Four patients were complicated with rib malformations, but this condition did not affect the surgical plan. Since the patients had no neurorelated symptoms preoperatively and the scoliosis in 7 cases was mild, we did not perform MRI for them, so we cannot accurately assess whether the patients have spinal cord abnormalities such as tethered cord or syringomyelia.
The optimal surgical age for Sprengel deformity remains controversial, but most literature favors early intervention at 3–6 years, 13 when skeletal growth allows effective correction. Many scholars recommend surgery for Cavendish Grades III–IV.14,15 However, surgical indications for adults are debated. Adult patients have fully developed skeletons and muscles, with fixed deformities and altered mechanical balance, increasing surgical difficulty. Long-term elevated scapula leads to adaptive changes in muscles (e.g., trapezius, rhomboids, levator scapulae), forming stable abnormal mechanical structures that hinder reduction and increase operative complexity. Most scholars consider downward relocation ineffective in adults and prone to brachial plexus injury, hence non-surgical management is often recommended. Previous reports primarily focus on children,3,16 with only one case of a 19-year-old treated surgically by Khadija Laasri et al. 1 in 2025. In our study, adult patients had low preoperative satisfaction scores (1.67 ± 0.94/10), indicating unmet needs for appearance and function improvement. However, surgical feasibility and optimal techniques for adults remain undetermined, with limited data on outcomes and complications.
Current main surgical methods include the Woodward and Green procedures. 5 The Green procedure involves transecting trapezius, levator scapulae, and rhomboid muscles, fixing the relocated scapula to lower spinous processes with wires, but it has a high trauma profile, risks wire fracture, and requires long wire fixation. The Woodward procedure, now the preferred method for children, involves downward relocation of trapezius and rhomboids, resection of omovertebral bones, and release of levator scapulae, using myofascial flaps for fixation. However, limited soft tissue release in adults often leads to suboptimal correction and postoperative loss of reduction due to muscle tension changes. Excessive traction may cause complications like nerve injury or vascular compromise.
The differences between our surgical approach and the Woodward procedure lie in: (1) Our surgery involves resecting the upper part of the scapular spine — a step not included in the traditional Woodward procedure — which can significantly improve the prominent posture of the neck and nape. (2)We expose the inferior angle of the scapula and approximately 1 cm of the adjacent rib, then fix the inferior angle of the scapula to the rib with a cable. Two months after surgery, when the soft tissues have healed and the scapula is basically stable in position, we will remove the cable to prevent rib cutting and restore the movement between the scapula and the chest wall. Differences between our surgical approach and the Green procedure: We detach the trapezius and rhomboid muscles from the spinous processes, then pull the muscles downward and fix them to the lower spinous processes. We believe that this combined surgical approach can maximize the improvement of the deformity’s appearance and the shoulder joint function.
Some scholars suggest concurrent clavicular osteotomy to prevent brachial plexus injury and improve correction, 5 but its necessity in Woodward procedures is debated. According to reports, 17 intraoperative nerve monitoring (IONM) is effective in preventing potential nerve damage during surgery for Sprengel deformity. According to Lei Feng’s report, 18 IONM during the Woodward procedure for Sprengel deformity is feasible and effective in detecting intraoperative neurologic changes and may be effective in preventing BPI associated with surgery. And according to the description in Lovell and Winter Pediatric Orthopedics, if symptoms of brachial plexus injury occur after surgery, salvage clavicle osteotomy is still effective. In our study, all patients’ intraoperative nerve monitoring showed normal signal, so we did not perform clavicle osteotomy.
Our results showed significant improvements in shoulder appearance, function, and patient satisfaction, with no major complications. However, limitations include: (1) retrospective design without a control group, limiting evidence level; (2) small sample size due to rare disease incidence, potentially introducing bias; (3) short follow-up (mean 12.5 months), with long-term outcomes unconfirmed.
Future studies should enroll larger samples and conduct long-term follow-ups to comprehensively evaluate efficacy, safety, scapular stability, sustained functional improvement, and late complications.
In conclusion, the modified combined Woodward and Green procedure is a safe and effective treatment for adult Sprengel deformity, improving appearance, function, and quality of life. However, further research with larger cohorts and longer follow-ups is needed to refine treatment protocols.
Footnotes
Ethical considerations
This study was approved by the institutional review board of our university (the Ethics Committee of Zhengzhou Orthopaedic Hospital). Informed consent was obtained from each patient and/or their legal guardian (For patients who less than 16 years old). This study were carried out in accordance with the Declaration of Helsinki.
Author contributions
Feng Zhu: Study design, implementation, manuscript writing. Wei Mei and Xiangjian Song: Surgical operation and administrative/technical support.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The datasets used and/or analysed during the current study are not available publically due to privacy, but are available from the corresponding author on reasonable request.
