Abstract
Objective
To evaluate and compare pain management, complication patterns, and functional outcomes between cannulated screw and Kirschner wire fixation for treating pediatric medial epicondylar fractures.
Method
A retrospective cohort study was conducted at a tertiary hospital from 2013 to 2023, involving 31 pediatric patients with displaced medial epicondylar fractures (Watson-Jones Types III and IV). Patients were divided into two groups: 16 received cannulated screw fixation, while 15 underwent Kirschner wire fixation. Clinical outcomes, including operation time, fracture healing, pain levels, and complications, were assessed.
Results
Both groups demonstrated similar long-term functional outcomes, with no significant difference in Mayo Elbow Performance Scores (p > 0.05). The cannulated screw group experienced significantly lower pain on the third postoperative day compared to the Kirschner wire group (p < 0.001). The Kirschner wire group had a higher rate of pin-track infections (13.3%) and delayed union (6.7%), whereas the cannulated screw group had fewer complications, with one case of superficial wound infection. Hardware removal occurred significantly earlier in the Kirschner wire group (p < 0.001).
Conclusion
Both fixation methods offer effective treatment for pediatric medial epicondylar fractures, with cannulated screws providing better pain control and fewer complications but requiring longer retention. Kirschner wires allow for earlier removal but carry a higher risk of infection and delayed healing. Treatment decisions should be individualized, considering factors such as pain sensitivity, family preferences, and medical resources.
Introduction
Medial epicondylar fractures represent approximately 20% of pediatric elbow injuries, ranking as the second most common elbow fracture in children after supracondylar fractures.1,2 These injuries predominantly occur in active children aged 9–14 years, often resulting from sports activities or falls. 3 While many cases can be managed conservatively, displaced fractures (Watson-Jones Types III and IV) frequently require surgical intervention to restore elbow stability and prevent long-term complications.4,5 Recent clinical investigations have illuminated that the choice of internal fixation - cannulated screws or Kirschner wire - exerts a tangible influence on surgical outcomes. Cannulated screws provide threaded compression across fracture sites and are increasingly favored for pediatric elbow fractures due to their superior stability, though concerns remain regarding growth plate damage in younger children.6,7 Kirschner wire can provide smooth needle fixation without pressure and is highly regarded for its easy removal and minimal interference to the growth plate.8,9 Although both methods are commonly employed, debates persist regarding the superior approach in terms of efficiency and suitability within the clinical context. The choice of internal fixation method impacts clinical outcomes, particularly for individual treatment experience and prognosis.10,11 Despite widespread use of both techniques, comparative data on pain management and complication patterns remain limited. Pain control is crucial in pediatric patients, as inadequate management can affect rehabilitation compliance and functional recovery.
The aim of this study was to evaluate the advantages and disadvantages of cannulated screw fixation and Kirschner wire fixation for the treatment of medial epicondylar fractures in children, focusing on whether there is a significant difference in pain control outcomes and complication patterns, thus providing an important guide to clinical decision-making.
Materials and methods
This study was designed as a retrospective cohort analysis conducted at a tertiary hospital from 2013 to 2023. A total of 31 patients who underwent open reduction and internal fixation for displaced medial epicondylar fractures of the humerus (type III or type IV according to the Milch classification) were included in the analysis. Patients were categorized into two groups based on the surgical fixation method employed: the cannulated screw group comprised 16 patients (11 males and five females) who received fixation with cannulated screws, while the Kirschner wire group consisted of 15 patients (11 males and four females) who underwent fixation using Kirschner wires. The study was conducted in accordance with the Declaration of Helsinki and reported following the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) guidelines. 12
Inclusion criteria
This study utilizes the Watson-Jones Classification, a widely recognized clinical assessment for humeral epicondyle fractures, which is essential for selecting appropriate treatment options.4,5 Type I and Type II fractures are typically non-displaced or minimally displaced and are suitable for conservative treatment, including closed reduction. Type III and Type IV fractures, often associated with elbow dislocation or bone fragment impaction, require open reduction and internal fixation. The inclusion criteria are as follows: (1) Fresh closed fractures diagnosed as Type III or IV with displacement exceeding 5 mm; (2) Age ranging from 9 to 14 years; (3) Cases subjected to open reduction and internal fixation utilizing either Kirschner wires or cannulated screws;
Exclusion criteria
(1) Congenital deformities of the elbow joint; (2) Open fractures; (3) Incomplete clinical data.
Surgical technique
All 31 children with Watson-Jones Type III-IV medial epicondylar fractures without comminution underwent open reduction surgery (Figure 1). All patients received the same anesthesia and antibiotics, and all procedures were performed by the same senior orthopedic surgeon. The choice of K-wire (Figure 2(a)–(f)) or cannulated screw (Figure 3(a)–(f)) depends on the surgeon’s preference as well as the patient’s wishes and financial income. Patients were placed in a supine position for surgical intervention. Brachial plexus block anesthesia, augmented by intravenous anesthesia, was deemed optimal. An incision, approximately 5 cm in length, was performed medial to the distal elbow joint. Should the valgus test prove positive, examination and repair of the medial collateral ligament and capsule were necessitated. Following the surgical incision, the ulnar nerve was isolated at the ulnar nerve groove. Children presenting with preoperative ulnar nerve paralysis or injury were managed with ulnar nerve release or anterior transposition. After complete exposure of the fracture’s distal end, reduction was executed. Open reduction of the humeral medial epicondyle fracture. The location indicated by the arrow is the ulnar nerve. Anteroposterior radiographs showed a humeral medial epicondyle fracture (type IV) in the right elbow (a). A CT scan clearly shows the gap of humeral medial epicondyle fracture (b). The fracture was fixed with two smooth K-wires (c and d). The follow-up radiographs (e and f) showed the union of fracture after removing the K-wires. A displaced humeral medial epicondyle fracture (type IV) in a 14-year-old boy (a) and (b). The fracture was fixed with one cannulated screw (c) and (d). After removing the screw, the radiographs showed good bone healing of fracture (e) and (f).
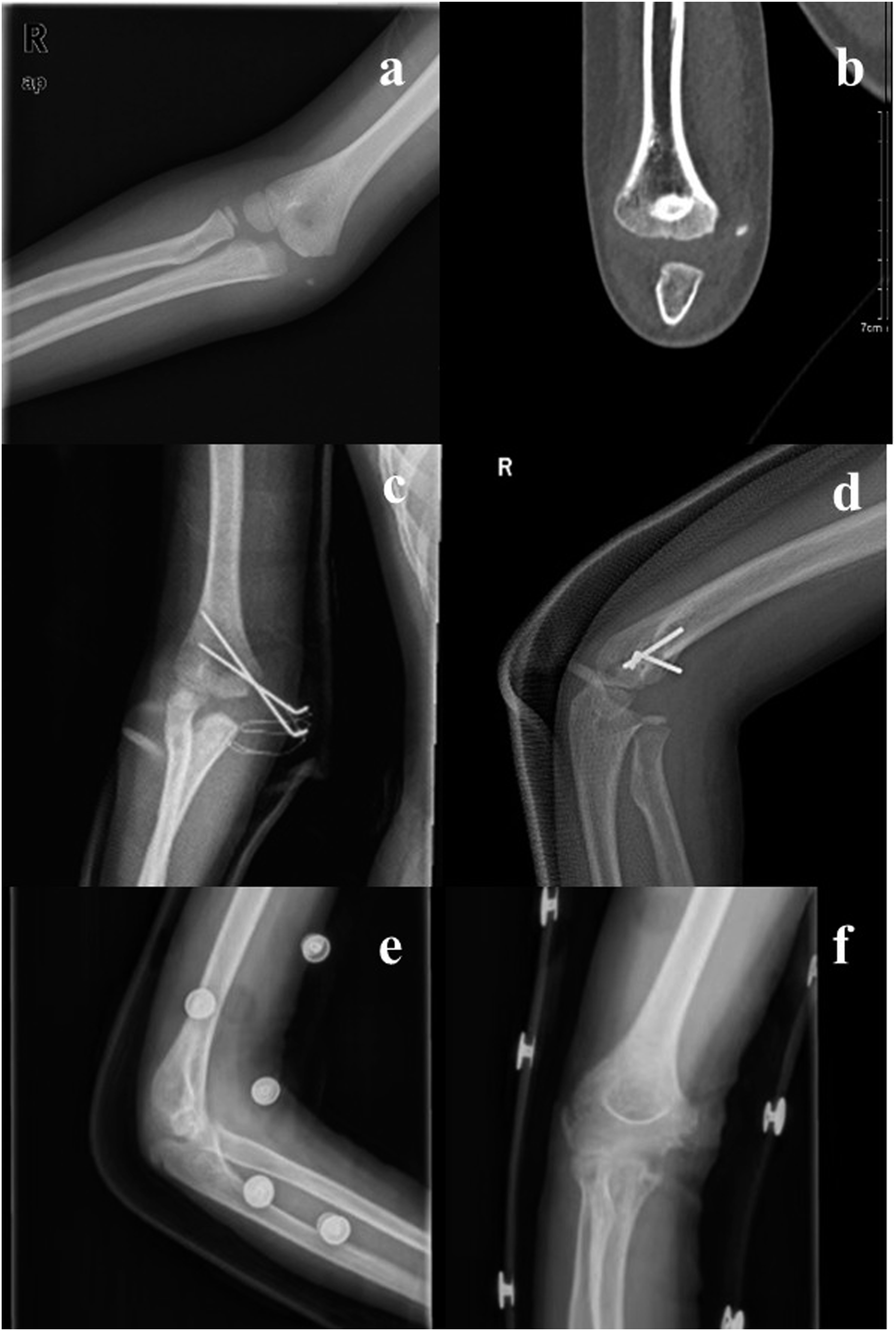

In the K-wire group, 2 or 3 Kirschner wires (1.5–2.0 mm in diameter) were inserted percutaneously and forming a cross to stabilize the humerus fracture. Conversely, patients in the screw group underwent internal fixation with 1 or 2 cannulated screws. Initially, the fracture’s fragmented end was provisionally stabilized, followed by parallel placement of a single hollow guide wire to the fracture line. Upon verification of the guide pin’s satisfactory positioning, a cannulated screw (3.5 mm in diameter) was inserted subsequent to drilling.
C-arm fluoroscopy facilitated insight into the fracture reduction. After cleansing and suturing the incision, a long-arm plaster was applied at an angle of 60° to 90° to the elbow flexion for stabilization. Between four to 6 weeks post-operation, the plaster support was removed, allowing the commencement of functional exercise.
Outcome measures
Operation index and postoperative rehabilitation
The metrics include the duration of operation, and fracture healing time, defined as the interval from the completion of surgery to the manifestation of fracture healing. The diagnostic criteria for fracture healing are based on X-ray diagnosis in the callus shaping stage. 5 Furthermore, the timeframe for the removal of internal fixation is determined from the completion of surgery to the actual removal.
Treatment effect
The Mayo Elbow-Performance Score (MEPS) was utilized in the assessment of therapeutic efficacy.13,14 Scored out of 100 points, evaluations of ≥90,80-89,70-79, and <70 were categorized as excellent, good, fair, and poor, respectively. The combined rate of excellent and good outcomes was computed using the formula: (excellent + good)/total cases ×100%. This evaluation was conducted 1-month post-operation. 15
Degree of pain before and after surgery
Pain levels were assessed at admission and on the third day post-operation using the W-B Facial Expression Pain Scale. 16 The interpretation was as follows: 10 points for very severe pain, 8 for severe pain, 6 for obvious pain, four for mild pain, 2 for slight pain, and 0 for no pain. Lower scores were indicative of reduced pain, as depicted in the subsequent figure 17 .
Incidence of postoperative complications
Those complications such as needle tract infection, superficial wound infection, delayed union, and others were documented after a 3-month postoperative follow-up.
Statistical method
Data analysis was conducted using SPSS 21.0. Categorical data were expressed as frequency and percentage [N (%)]. Shapiro-Wilk test was used to assess normality of continuous variables. For normally distributed data, continuous variables were expressed as mean ± standard deviation; for non-normally distributed data, distributed variables were presented as median (interquartile range). For continuous variables with a normal distribution, an independent t-test is adopted; For continuous variables with non-normal distribution, the Mann-Whitney U test is used; For categorical variables, Fisher’s exact test is used. A p-value of <0.05 was considered indicative of a statistically significant difference.
Results
Baseline characteristics
Comparison of general data of the two groups.

Values are presented as the number (%). Age is presented as the median (interquartile range).
Operation index in the K-wire group and screw group
Clinical outcomes of the children in both groups.

Operation index, MEPS, W-B scoring and Postoperative complications are presented as the median (interquartile range). *** represents statistically significant differences (P < 0.001).
Cannulated screw fixation has a less painful experience
Functional outcomes were assessed using the Mayo Elbow Performance Score. According to MEPS, the distribution within the screw group was 13 excellent, 2 good, and 1 fair case, comparing with the distribution in the K-wire group of 12 excellent, 2 good, and 1 fair case. The combined excellent and good rates were 93.75% and 93.33% for the screw group and the K-wire group, respectively. Statistical analysis revealed no significant distinction between the two groups (p > 0.05), indicating that both fixation methods yield uniformly satisfactory long-term elbow function.
The most striking difference between groups emerged in postoperative pain management. Evaluation of the W-B pain score at the time of admission demonstrated no statistical divergence between the groups (p > 0.05); however, postoperative day 3 demonstrated a clinically meaningful advantage for cannulated screw fixation. The screw group reported significantly lower pain scores with a median of 4.5 (IQR: 4.0–5.0) compared to 6.0 (IQR: 5.0–6.0) in the K-wire group (p < 0.001). This difference represents a 25% reduction in pain intensity.
Postoperative complications differ between K-wire group and screw group
Postoperative complications demonstrated distinct patterns between fixation methods. A comparative examination of postoperative complications between the two groups is summarized in Table 2. The screw group showed longer hardware retention (p < 0.001), as screws were typically left in place after healing due to their subcutaneous position and minimal interference. In the K-wire group, two patients encountered pin track infections, subsequently alleviated through regular pin track dressing and antibiotic administration. Additionally, one patient from this group experienced delayed union over a 3-month period but achieved fracture healing in the fourth month with long arm tubular cast fixation. Conversely, in the screw group, one patient developed a superficial wound infection that resolved with conservative management, while no cases of pin-track infection or delayed union occurred. No delayed neurological or additional complications were detected at the ultimate follow-up. The K-wire group experienced a higher overall complication rate of 20.0% versus 6.25% in the screw group, though this difference did not reach statistical significance (p > 0.05). All subjects recovered satisfactorily post-treatment, displaying neither elbow pain nor limitations in motion.
Discussion
Medial epicondylar fractures commonly occur in pediatric patients following falls or avulsion injuries, presenting with elbow discomfort, edema, and restricted range of motion, this fracture assumes particular significance in pediatric orthopedics.18,19 While Watson-Jones Types I and II fractures respond favorably to conservative management, displaced Types III and IV fractures necessitate surgical intervention to restore elbow stability and prevent chronic complications.20,21 However, the optimal fixation method remains unclear.
Orthopedic practitioners conventionally employ either cannulated screw or Kirschner wire for intraoperative fixation. Kirschner wire offers practicality with reduced epiphyseal injury risk, and easy extraction. Cannulated screws may increase epiphyseal damage risk in children with open growth plates 22 but provide superior compression and stability. Recent studies demonstrate cannulated screw efficacy in pediatric medial epicondylar fractures of the humerus, 23 with superior stability to Kirschner wire and diminishes risks of nonunion and fracture displacement risks, typically allowing one-time healing. 24 Long-term studies show comparable joint mobility outcomes between both methods at 6 months postoperatively. 25 In clinical practice, the selection of the most effective treatment strategy should be tailored to the specific needs of each child, with a focus on restoring limb functionality after surgery. 26 This investigation addresses the knowledge gap by evaluating pain management and complication patterns between cannulated screw and Kirschner wire fixation, providing evidence for individualized treatment selection.
The most significant finding demonstrates cannulated screw fixation provides superior early postoperative pain control compared to Kirschner wire fixation. This advantage likely results from the subcutaneous positioning of screws, eliminating transcutaneous hardware irritation, and the superior fracture compression achieved through threaded fixation mechanisms. Although all patients experienced a long period of immobilization after surgery, lower pain scores in the screw fixation group indicate improved early comfort and reduced need for analgesics, which can positively affect patient compliance and psychological well-being rather than directly influencing rehabilitation speed.27,28 This finding carries substantial implications for treatment optimization.
The complication analysis reveals distinct risk profiles between fixation methods. The main postoperative complications of Kirschner wire fixation are pin-track infections and delayed union. Pin-track infections, while manageable through conservative measures, represent preventable morbidity affecting patient comfort and healthcare utilization. The inherent inability of the Kirschner wire to exert compression upon the fractured segment may consequently impede fracture healing. Delayed union or nonunion represents a recurrent complication subsequent to a medial epicondyle fracture, particularly discernible within the conservative treatment paradigm for older children. 29 Factors such as premature removal of external plaster fixation removal for rehabilitation could further exacerbate delayed union risk.30–32 The inherent stability advantage of cannulated screws, evidenced by the absence of delayed union cases, supports their efficacy in achieving primary bone healing.
The extended hardware retention requirement for cannulated screws presents both therapeutic benefits and practical challenges, requiring operative removal and increasing costs, particularly relevant in resource-limited healthcare settings or for families with compliance concerns.33,34 However, the absence of healing complications in the screw group suggests that the prolonged retention period reflects no urgency for removal, as the screws are subcutaneously located and cause minimal interference, rather than a biological need for extended fixation. Despite differences in pain management and complication, both fixation methods achieved equivalent functional outcomes at final follow-up, even though MEPS scores demonstrating no significant difference (p > 0.05). This finding reinforces that while fixation method influences the recovery trajectory, ultimate functional restoration remains satisfactory with either technique when appropriately applied.35,36 The comparable outcomes emphasize that treatment selection should prioritize patient-specific factors including pain tolerance, family preferences, and healthcare accessibility rather than functional expectations alone.
These findings support a patient-centered treatment algorithms in pediatric orthopedics. Cannulated screws are optimal for pain-sensitive patients despite longer retention requirements. Conversely, families preferring minimal contact may benefit from K-wires, accepting higher complication risk for earlier removal.37,38 Age-related considerations also merit attention, as younger children with active physes may benefit from K-wire fixation to minimize growth disturbance risk, while adolescents approaching skeletal maturity can safely undergo screw fixation for superior pain management. The clinical significance of this investigation lies in providing quantitative evidence for treatment individualization rather than promoting universal fixation preferences. The systematic analysis of pain trajectories and complication profiles offers clinicians objective data to counsel families regarding treatment options, facilitating shared decision-making processes. Several limitations of this study should be recognized. The relatively small sample size and retrospective design may have limited statistical power and introduced selection bias. Second, the length of pain assessment was not continued after a significant difference was obtained at postoperative day 3, leading to a potential failure to capture the complete recovery trajectory. The 10-year study duration may also contribute to heterogeneity in follow-up time and potential temporal bias. Future prospective investigations with larger patient cohorts could further refine these treatment algorithms and validate the preliminary risk-benefit profiles identified in this study.
Conclusion
Both cannulated screw and Kirschner wire fixation effectively treat medial epicondylar fractures in children with similar long-term outcomes. Cannulated screws offer better early pain control but require longer fixation, while Kirschner wires can be removed sooner, though they carry a higher risk of infection and delayed healing. Treatment decisions should be individualized, considering factors such as pain sensitivity, family preferences, and medical resources. These findings emphasize the value of patient-centered care in guiding shared decision-making.
Footnotes
Author note
We declare that this manuscript has not been published previously and is not currently under consideration by any other journal. We have not used artificial intelligence (AI)-assisted technologies in the production of the submitted work.
Ethical considerations
This study was approved by the Ethics Committee of Chinese People’s Liberation Army General Hospital. Informed consent to undergo treatment with cannulated screw or Kirschner wire fixation was obtained from all patients and their parents or guardians.
Consent to participate
This study has obtained the informed consent of all the legal guardians of the patients.
Consent for publication
All authors have read and approved the final manuscript and have agreed to publish it.
Author contributions
All authors read the proposed manuscript and give their substantial contribution to this study. Conceptualization, F.J.; Methodology, F.J.; Software, F.J.; Data curation, X.D.; Validation, F.J.; Investigation, F.J. and Z.W.; Formal Analysis, Z.W., H.C.; Writing - Original Draft, F.J. and Z.W.; Writing - Review & Editing, H.Z., W.L., H.C., Z.W.; Visualization, Z.W.; Supervision, H.Z. and W.L.; Resources, X.D.; Project Administration, W.L.. All authors approved the final version of the manuscript.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The data set generated during this study is available from the corresponding author upon justified request
