Abstract
Purpose
The primary objective of this study was to determine time to full weight-bearing after the use of a calcium-sulfate-calcium phosphate bone substitute (CaSO4/CaPO4) as a bone void filler in the treatment of primary benign bone tumours following intralesional curettage. The secondary objectives were to determine surgical complications and recurrence rates.
Methods
Retrospective review of patients identified from a surgeon-specific orthopaedic oncology database, who underwent curettage of benign bone tumours and subsequent bone void filling with CaSO4/CaPO4.
Results
A total of 39 patients (20 males, 19 females) met inclusion criteria with an average age of 31 years (range: 13 to 62 years), a median follow-up of 3.7 years, and a maximum follow-up of 11 years. The most common tumour diagnosis was giant cell tumour of bone (GCT) (
Conclusion
This study demonstrates that CaSO4/CaPO4 is a viable option as a bone void filler in the reconstruction of cavitary defects following removal of primary benign bone tumours. CaSO4/CaPO4 provides sufficient bone regeneration early in the post-operative period to allow progression to full weight-bearing within weeks without the need for internal fixation. There were no graft-specific complications noted.
Introduction
Benign bone tumours are typically asymptomatic or minimally symptomatic and are often discovered incidentally.1,2 However, benign aggressive bone tumours, such as giant cell tumour of bone (GCT), chondromyxoid fibroma (CMF), and aneurysmal bone cyst (ABC), can cause local bone destruction and require aggressive intralesional resection.1,2
Intralesional curettage is a surgical technique whereby the tumour mass is removed while surrounding bone is preserved. 3 This leaves a resultant void that must be reconstructed to restore stability.3,4 Various reconstructive options have been described, including autograft, allograft, synthetic bone substitute, or polymethylmethacrylate bone cement.4,5 Autograft is limited in supply and necessitates donor-site morbidity.5,6 Allograft may transmit disease and increase the risk of deep infection and non-union.5,6 Both require a period of immobilization before normal activity can resume, and resorption of both may confound radiographic identification of disease recurrence.5,7–9 Conversely, bone cement may cause thermal damage to nearby joint surfaces and is sufficiently biomechanically dissimilar from bone that normal joint biomechanics are altered.10–12
Synthetic bone substitutes have therefore become a desirable alternative. These new products promise regeneration of normal host bone stock, sufficient mechanical support for early functional rehabilitation, and relatively limitless supply, while eliminating the risk of disease transmission and donor site morbidity. 13 Calcium-sulfate-calcium phosphate bone substitute (CaSO4/CaPO4) is a bone graft substitute composed of a calcium sulfate-calcium phosphate matrix mixed with beta-tricalcium phosphate granules. This product promotes a strong osteogenic response, as the calcium sulfate is rapidly resorbed while the calcium phosphate and beta-tricalcium phosphate granules provide a stable scaffold for osteointegration.14,15 There have been two published case series describing the use of this bone graft substitute in patients following benign bone tumour curettage, with little published data on early functional recovery or longer-term outcomes.15,16
This study aimed to advance current literature on the use of CaSO4/CaPO4 in primary benign bone tumours through a retrospective chart review of patients who underwent intralesional curettage and CaSO4/CaPO4 synthetic bone graft filling of the bone void. The primary objective of this study was to determine the functional (return to weight-bearing) outcomes of a cohort of patients who underwent reconstruction of a cavitary bone defect with CaSO4/CaPO4 following intralesional curettage for a locally aggressive bone tumour. The secondary objectives were to determine the rate of surgical complications and recurrence rates.
Methods
This study received local ethics approval from the Institutional Ethics Board (REB#2023-15,972-C). This is a single-centre retrospective chart review using a surgeon-specific orthopaedic oncology database. The database includes patients operated on by three orthopaedic oncology surgeons at the affiliated hospital institutions between June 2007 to June 2022. Ethics approval was granted to retrospectively review the charts of all patients meeting inclusion criteria.
Patient population
Specifically, the database was used to identify all patients diagnosed with primary benign bone tumours undergoing intralesional curettage and cavitary bone filling with CaSO4/CaPO4 (Pro-DenseTM, Wright Medical Inc. – a subsidiary of Stryker, Memphis, TN). Patients undergoing bone cavitary filling with CaSO4/CaPO4 for reasons other than bone tumours were excluded. Additionally, those receiving further augmentation with internal fixation and/or other bone substitute materials were excluded from the study. Specifically, fixation was not used after the first few cases in which the surgeon used the CaSO4/CaPO4 synthetic bone graft since early regeneration precluding the need for fixation was noted and therefore the surgical approach was changed to exclude fixation. For all patients the planned surgical approach was dependent on the tumour location. Once the neocortex was exposed and debrided, the entire tumour underwent extensive curettage followed by a high-speed burr and copious amounts of normal saline irrigation. CaSO4/CaPO4 was then injected locally into the cavitary defect until it was maximally filled.
Clinical follow-up, patient, and tumour characteristics
Data extracted from electronic medical records included patient characteristics (i.e., age, sex), tumour characteristics (i.e., location, pathologic and histologic diagnosis, dimensions of defect based on radiographic measurements), volume of CaSO4/CaPO4 used, and functional outcome measures as outlined below. Functional outcome measures were examined for both short-term and long-term follow-up. Generally, patients were followed with a clinical examination and plain radiographs of the surgical site post-operatively at 2 weeks, 4 weeks, 3-6 months, and yearly thereafter. However, no standardized follow-up protocol was adopted and thus these intervals were subjected to some variability among patients.
Radiographic dimensions of the tumours were obtained from preoperative magnetic resonance imaging (MRI) reports. Values reported included the anteroposterior, transverse (medial/lateral), and craniocaudal dimensions. For ease of comparison, these values were converted into volume of tumour (cm3) on Google Sheets 2023 (Google LLC, Mountain View, California, United States). Volume of CaSO4/CaPO4 used was obtained from operative notes and was reported in millilitres (mL). Missing data was notable for these two categories (i.e., radiographic dimensions of the tumour and volume of CaSO4/CaPO4 utilized). Given that a small subset of patients had data missing, these patients were only excluded from the calculations of mean, median, and range for these specific data points.
Primary outcome: Time to full weight-bearing
The primary outcome of the study was time to full weight-bearing. Full weight-bearing was defined as 100% of body weight without restrictions based on clinical examination and radiographic evidence of CaSO4/CaPO4 consolidation. Other functional outcome measures recorded were time to partial weight-bearing, and functional limitations at final follow-up. Partial weight-bearing was defined as clearance for range of motion exercises for the upper extremity bone tumours and 50% of body weight for the lower extremity bone tumours. Clearance for partial and full weight-bearing was determined by the operating surgeon based on radiographic bone regeneration at the periphery of the previous bone void. Return to weight-bearing status was readily obtained from clinical notes as dictated by the operating surgeon at each follow-up.
Secondary outcomes: Surgical complications and tumour recurrence
Other secondary outcomes included frequency of infection requiring antibiotics, infection requiring reoperation, wound breakdown requiring reoperation, tumour recurrence requiring reoperation and thromboembolic complications. No further missing data was noted, beyond what was previously outlined regarding data for tumour volume.
Results
Patient population and tumour characteristics
Patient and tumour characteristics.


Pre and post-operative images following curettage of a UBC of the right distal tibia and bone void filling with CaSO4/CaPO4 in a 13-year-old female.
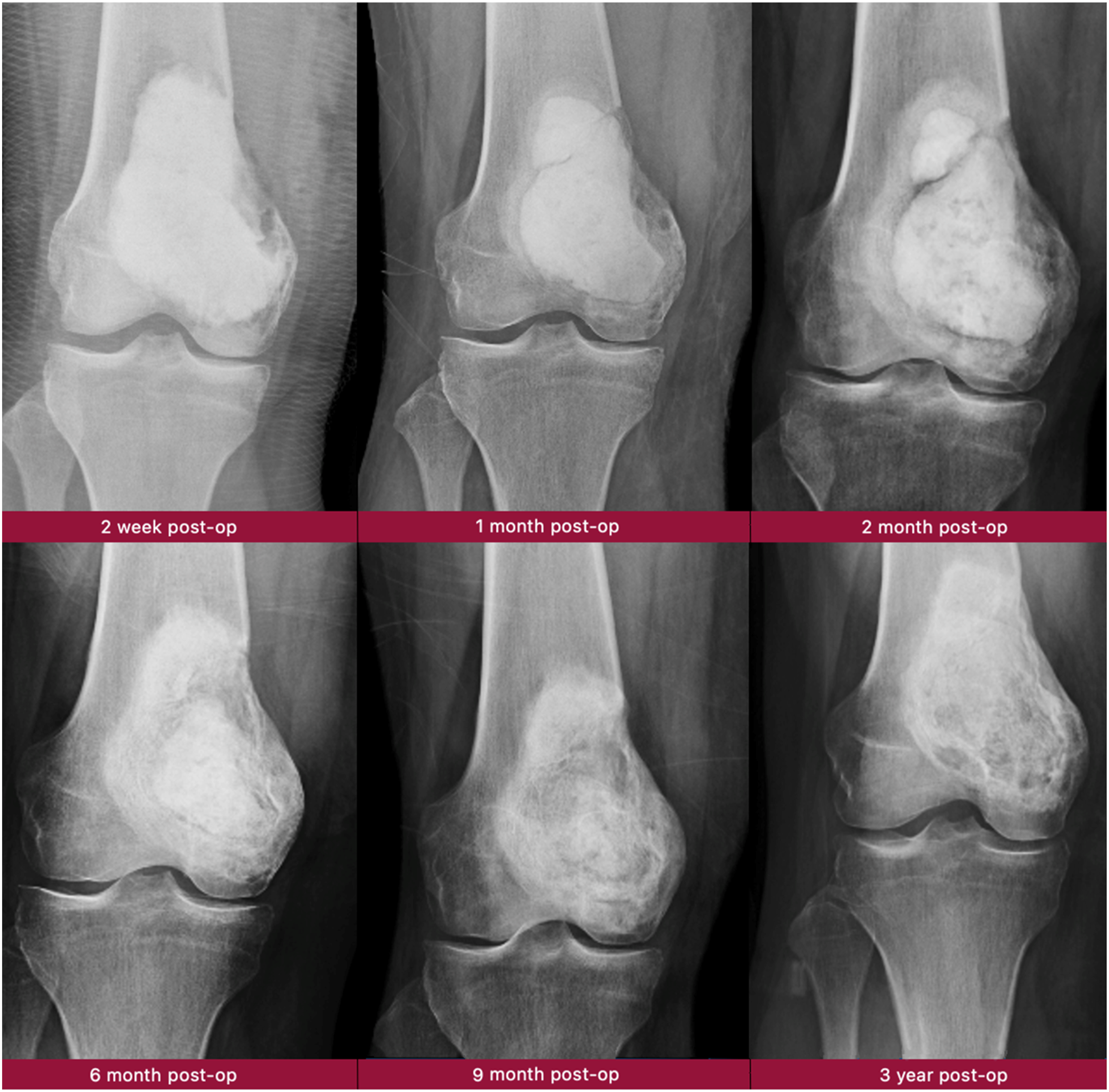
Example of CaSO4/CaPO4 incorporation after intralesional curettage of a large GCT of the distal femur.
Functional outcomes and post-operative complications.

aInfection requiring reoperation.
bThromboembolic event occurred many years after the surgery and is likely unrelated.
Primary outcome: Time to full weight-bearing and functional limitations
Among patients with lesions in their upper extremities, the average time to partial weight-bearing/range of motion was 2.6 weeks (range of 2 to 4 weeks) and average time to full weight-bearing/range of motion was 11 weeks (range of 2 to 24 weeks). In comparison, patients with lesions in the lower extremities demonstrated average time to partial and full weight-bearing as 3 weeks (range of 0 to 7 weeks) and 6 weeks (range of 0 to 12 weeks), respectively. At final follow up, two patients reported minor stiffness due to osteoarthritis (2 tibiotalar joints), two had minor range of motion deficits (1 radiocarpal joint, one metacarpal phalangeal joint), one had metatarsalgia, and had a foot drop related to peroneal neuropraxia. All patients had full radiographic incorporation at last follow-up and function as shown in Table 2.
Secondary outcomes: Surgical complication and tumour recurrence
Surgical complications are outlined in Table 2. Four of the study participants experienced superficial wound infections. Two of these patients received a short course of antibiotics (i.e., 7 to 10 days) and achieved complete resolution. One patient required re-operation in the form of irrigation and debridement with primary wound closure. The other patient was diagnosed with sinus tract infection with wound swabs confirming an infection with
One patient experienced a perioperative deep vein thrombosis (DVT) which resolved with anticoagulation therapy, and another patient suffered an immediate fracture of the distal femur when premature anaesthesia reversal prevented limb immobilization prior to active muscle contraction and rapid knee flexion. The latter patient underwent immediate internal fixation, highlighting the importance of immobilization during the process of graft consolidation. Additionally, one patient experienced post-operative transient paraesthesia in the lateral femoral cutaneous nerve which resolved in a few weeks without need for additional investigation or treatment.
Tumour recurrence requiring reoperation occurred in five patients. Four patients experienced recurrence of their GCT requiring
Discussion
Our review of 39 cases of primary benign bone tumours treated surgically with extended curettage and use of CaSO4/CaPO4 bone void filler demonstrated that early weight-bearing was possible without the need for additional internal fixation in all cases in which the limb was successfully immobilized prior to anesthesia reversal (38/39). The mean follow-up was 3.7 years, with a maximum follow-up of 11 years. Most of the patients progressed to partial weight-bearing at 2 to 3 weeks post-operatively regardless of tumour location (i.e., upper extremity vs lower extremity). Additionally, patients demonstrated timely return to full weight-bearing/range of motion at an average of 11 weeks (upper extremity lesions) and 6 weeks (lower extremity lesions). In addition to avoiding complications related to hardware insertion such as implant-related infection and painful hardware, there were also no complications directly related to the use of CaSO4/CaPO4.
Relation to previous literature: Return to weight-bearing and surgical complications
The outcomes of CaSO4/CaPO4 bone graft substitutes used in filling of cavitary bone defects following intralesional curettage of primary benign bone tumours have previously been reported. A previous retrospective review of the clinical outcomes of an earlier cohort of 24 patients with benign primary bone tumours who underwent intralesional curettage followed by bone filling with a CaSO4/CaPO4 composite bone substitute showed that the use of a CaSO4/CaPO4 composite was associated with rapid biological integration and an early return to activities of daily living, with no composite-related complications. 15 A later cohort of 56 patients reported a high rate of return to normal functional scores at a mean follow-up of 42 months 16 Notably this study did not report the timing of functional recovery or achievement of early functional recovery. The present study, with overall longer-term follow-up, therefore, represents the largest series of patients treated with CaSO4/CaPO4 following surgical resection of benign bone tumours to report early post-surgical function.
In other studies, calcium sulfate has successfully been used in filling contained bone defects, and results can be comparable to demineralized bone matrix-based allografts, with the advantage of being cost-effective and easy to use. 13 However, a case report showed that progressive osteolysis can occur after the use of synthetic bone graft substitutes, including calcium sulfate, and may require further surgical intervention. 17
The radiographic appearance of graft resorption and new bone incorporation into a post-resection defect of the bone has been characterized and has shown that peripheral new bone regeneration early in the process allows for earlier weight-bearing. 18 In addition, once the calcium sulfate component is resorbed, the mechanical properties of the remaining porous calcium phosphate materials are comparable with cancellous bone. 19 Finally, a comprehensive review of the literature clarified the important balance of calcium sulfate (early resorption and osteoinductive inflammatory response) and calcium phosphate (slow resorption, mechanical stability and osteoconduction) in combination bone graft substitutes. 20
Clinical and research implications
The advantages of synthetic bone graft substitutes for cavitary bone defects include their ability to overcome the limitations of autogenous bone grafts, such as donor site morbidity, limited availability, and increased surgical time. 21 Synthetic bone graft substitutes can also enhance bone healing due to their osteoconductive, and in some cases, osteoinductive, properties. 22 In vitro studies have shown that CaSO4/CaPO4 preferentially binds and stimulates local bone growth factors, and in animal models CaSO4/CaPO4 resulted in new bone formation that was more rapid and stronger than cancellous autograft.14,23,24 Perhaps most interestingly, CaSO4/CaPO4 bone graft substitute combines rapid resorption and robust bone formation with an inherent mechanical stability that allows for early weight-bearing, obviating the need for augmentation with internal fixation.
However, most synthetic bone graft substitutes, especially synthetic ceramics and cements, do not possess any osteoinductive properties. 22 In addition, the cost of synthetic bone graft substitutes can be higher than that of autogenous bone grafts. 13 Therefore, the long-term outcomes of synthetic bone graft substitutes are still being studied, and their safety, efficacy and particularly cost-effectiveness are the subject of ongoing evaluation.
Limitations
The limitations of this study are related to its retrospective design. The retrospective collection of data from medical records is subject to recall bias. In addition, selection bias can be introduced due to the ability of the surgeon in the reported cases to use CaSO4/CaPO4 without the need for internal fixation. More complex cases and larger defects, not included in this series, may require further initial post-operative stability provided by internal fixation. However, several of the cavitary defects in the current study were very large, thus mitigating concern for selection bias. Although the majority of the patients completed follow-up, not all patients returned for all follow-up visits and some were lost to follow-up, introducing the possibility of transfer bias. However, the large number of patients and long-term follow-up in this series are a strength and support the validity of the current findings.
Conclusion
Results of this study indicate that CaSO4/CaPO4, the first and only bone void filler approved for benign bone cysts and tumours for ages six and up in the U.S., is a feasible and reliable choice of bone void filler in the reconstruction of cavitary defects following removal of primary benign bone tumours for pediatric and adult patients. The use of CaSO4/CaPO4 in this series was associated with earlier return to weight-bearing, no major functional impairments at final follow-up, and no complications directly related to the bone graft substitute. Given the low risk for surgical complications related to CaSO4/CaPO4 and the avoidance of the need for internal fixation and prolonged immobilization, the cost-effectiveness of CaSO4/CaPO4 will be an important focus of future research.
Footnotes
Declaration of conflicting interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: M.G is a paid consultant and speaker for Stryker Corporation, which markets CaSO4/CaPO4.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This was funded by a grant from Stryker Corporation.
