Abstract
Purpose
This study aimed to evaluate the mid–term radiological and clinical results of gradual lengthening of capitate for the treatment of stage IIIA Kienbock’s disease.
Methods
We retrospectively reviewed nine patients (five females, four males) with Lichtman stage IIIA Kienbock’s disease who underwent gradual capitate lengthening at our hospital. Their clinical (range of motion (ROM), grip strength, visual analogue scale (VAS) value for pain, and Mayo wrist score (MWS)) and radiological outcomes (in terms of progression of arthritis and carpal height ratio) at the last follow-up were compared to the preoperative values.
Results
The mean age of the nine patients was 30 years (range: 20–38 years). The mean follow-up period was 73.8 (60–83) months. The average grip strength increased from 14.3 kg preoperatively to 22.3 kg at the last follow-up. The mean MWS increased from 58.8 preoperatively to 79.4 postoperatively. The mean VAS values decreased from the preoperative values: from 1.9 to 0.36 at rest, from 3.75 to 1.6 during mild effort, and from 5.35 to 3 during severe effort. The average carpal height ratio changed from 0.38 preoperatively to 0.53 postoperatively. None of the patients had any arthritic changes in their wrists.
Conclusion
Gradual lengthening of capitate offers satisfactory mid-term results for treating stage IIIA Kienbock’s disease.
Introduction
Kienbock’s disease, first described by Robert Kienbock in 1910, is a clinical and radiological disorder involving avascular necrosis of the lunate bone. 1 Although the disease was identified about a century ago, its aetiology has not been fully elucidated yet; consequently, there is a lack of consensus on its treatment options. 2 The reported prevalence of Kienbock’s disease is seven cases per 100,000 people, 3 and the prognosis worsens with advancing age. 4 Although the exact aetiology is unknown, lunate morphology, negative ulnar variance, and stress syndrome are the causes of Kienbock’s disease. 5
Collapse of the lunate from avascular necrosis causes deformity and disintegration of the central column articulations, proximal row instability, and degeneration of the radial column at the wrist. 5 Lichtman et al. initially classified Kienbock’s disease into four stages (stages I–IV) based on clinical and radiological criteria 6 ; eventually, the classification was modified to include stages IIIA and IIIB depending on the development of carpal instability. Stage IIIB has carpal instability. In stage I, there are no radiographic changes, while the disease is noticeable on magnetic resonance imaging. Stages II and III involve lunate sclerosis and collapse, respectively, and degeneration in the intercarpal joints is observed in stage IV. The treatment is decided based on the radiological stage of the disease. Classically, stage I patients are recommended immobilization and nonsteroidal anti-inflammatory drugs (NSAIDs); for stage II, joint levelling procedures, namely ulnar lengthening or radial shortening, are recommended in patients who have negative ulnar variance. In stage IIIA, scaphotrapeziotrapezoid (STT) fusion or radial wedge osteotomy is done in patients who are ulnar neutral; other procedures for stage IIIA include radial core decompression and revascularization. For stage IIIB, STT fusion or proximal row carpectomy is opted for. In stage IV disease, proximal row carpectomy, wrist fusion, or limited intercarpal fusion may be performed. 7
Apart from these classical management options, several salvage procedures are available for treating stage III Kienbock’s disease, primarily aimed at restoring the wrist architecture and carpal height ratio to improve the patient’s grip strength. Graner et al. described acute capitate lengthening to achieve these purposes. 8 Likewise, Hierner et al. performed gradual capitate lengthening in patients with stage III Kienbock’s disease. 9 This study aimed to report the mid-term clinical and radiologic outcomes of restoring carpal height using external fixator-assisted gradual capitate lengthening in patients with stage IIIA Kienbock’s disease.
Materials and methods
After obtaining approval from the local ethics committee, we retrospectively examined nine patients (four males, five females) undergoing gradual capitate lengthening for stage IIIA Kienbock’s disease between 2015 and 2016. These patients were again assessed at mid-term (5 years of surgery) to assess their current situation, this was then compared to the pre-operative scenarios. All surgical procedures were carried out by two surgeons with advanced experience in hand surgery. Radiological diagnosis was made by plain X-ray of the bilateral wrist. The Mayo wrist score (MWS) and the visual analogue scale (VAS) were used for clinical evaluation. 10 Joint range of motion measurements for all patients were made using the neutral zero method in the pre-op and final follow-up. Pre- and post-operative grip strength evaluations were performed with a handgrip dynamometer. Radiographic evaluation of the preoperative and final follow-up radiographs was done by measuring the carpal height ratio (CHR) which is measured by dividing the carpal height by the length of the 3rd metacarpal with both measurements taken in the long axis of the 3rd metacarpal and arthritis development. 11
Indications and contraindications
This technique is indicated in patients with a diagnosis of Lichtman stage IIIA Kienbock’s disease. Patients with degeneration of the articular surface of capitate and other carpal bones, as well as those with stage IIIB disease with subluxation of the carpal bones, are contraindicated for this technique.
Surgical technique
All patients were operated on in the supine position on the hand table under general anaesthesia. A nonsterile tourniquet was wrapped around the proximal arm of the patient to maintain systolic pressure above 100 mmHg. A 3 cm long longitudinal incision was made between the 3rd and 4th dorsal compartments to enter the wrist. Tendons were identified and retracted; the capsule was opened towards the ulna in the form of a U-shaped incision. The scapholunate and lunotriquetral ligaments were excised with the help of cut-fragmenting lunate forceps, and the lunate bone was completely excised. Two 2-mm Schanz screws were applied to both proximal and distal parts of the capitate bone. Then, the capitate was osteotomized from the middle with the help of an osteotome, and the capsule and extensor retinaculum were planted. After skin closure, a unilateral external fixator (TASARIMMED, Turkey) was adapted to the Schanz screw (Figure 1). Radiological evolution of capitate lengthening (a). Preoperative (b). Early distraction (c). Consolidation period (d). Radiological aspect after 5 years.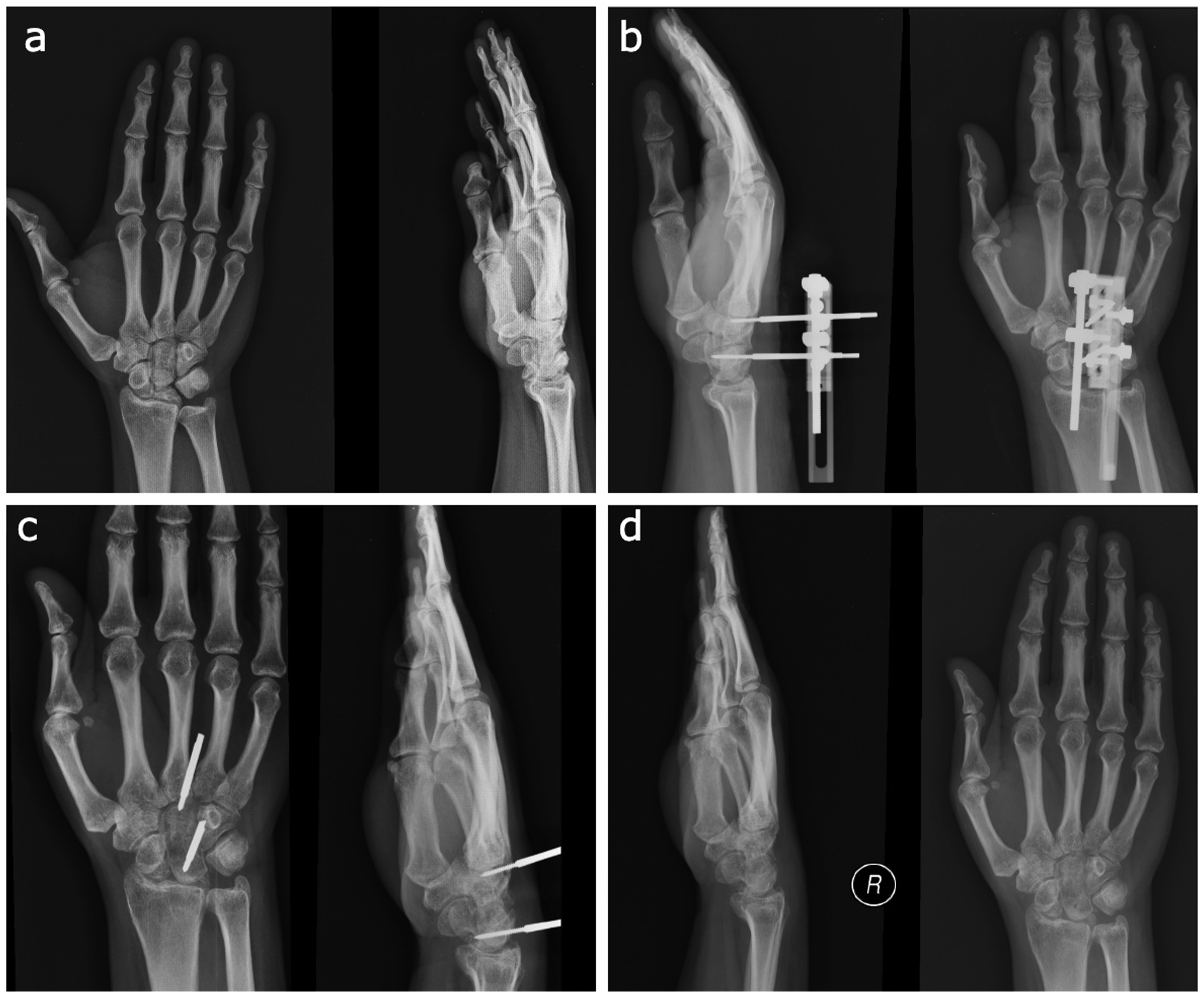
Postoperative course
Wrist range of motion (ROM) exercises were started on the first postoperative day. The patients were encouraged to use their wrists and hands. On postoperative day 5, 0.25 mm distraction was started 4 times a day 6 h apart, and checked with serial radiographs taken every 15 days. Carpal bone height measurements were made on the healthy wrist of the patient; the carpal height of the affected wrist was lengthened to match that of the healthy wrist (Figure 2). After the lengthening period of the patients was completed, monthly control X-rays were performed. After the consolidation period was completed, the external fixator was removed in the intervention room without the use of anaesthesia (Figure 3). Carpal height measurements (a). Carpal height measurement in healthy wrist (b). Carpal height measurement in pathologic wrist (c). Carpal height measurement after capitatum lengthening. Radiological evolution of capitate lengthening (a). Preoperative (b). Early distraction (c). Consolidation period (d). Radiological aspect after 5 years.
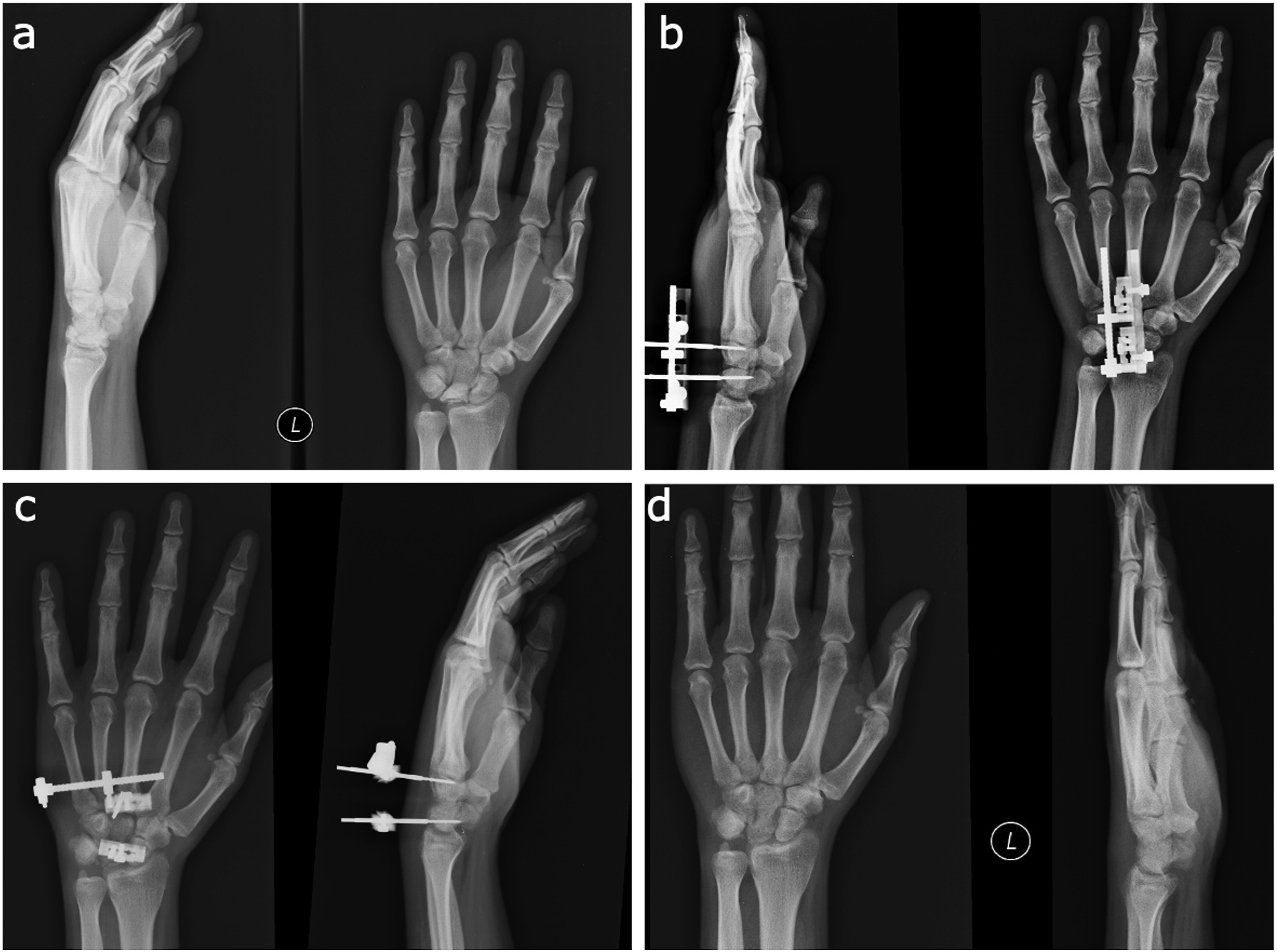
Results
Demographics of patients.

The mean initial MWS of the patients was 58.8 (range: 40–70); at the last follow-up, the average MWS increased to 79.4 (range: 65–85). According to the MWS system, seven patients had good results, and two patients had satisfactory results. The mean VAS was 1.9 at rest, 3.7 at mild effort, and 5.3 at severe effort. At the last follow-up, the mean VAS was 0.3 at rest, 1.6 at mild effort, and 3,1 at severe effort. The mean preoperative ROM was 50°/0°/44.4° for flexion-extension (range: 30–60°/0°/30–50°), 19.4°/0°/31.1° for radial-ulnar deviation (range: 15–20°/0°/20–40°), and 60°/0°/62.2° for supination-pronation (range: 40–80°/0°/40–80°). At the last follow-up, the mean ROM was 47.7°/0°/40° for flexion-extension, 18.3°/0°/28.8° for radial-ulnar deviation, and 55.5°/0°/62.2° for supination-pronation (Figure 4). Active range of motion post operative 6rd year (a). Right hand grip strength (b). Left hand grip strength (c). Flexion (d). Extansion (e). Supination (f). Pronation.
The average carpal height ratio changed from 0.39 preoperatively to 0.48 at the last follow-up. Preoperatively, the average grip strength was 15.4 (range: 13–18) kg, which improved to 22.3 (range: 17–27) kg postoperatively. There were no complaints of pin-site infection or deep infection in any of the patients postoperatively; none of the patients had non-union. In the DTPA-gadolinium-enhanced MRI scanning done at the last follow-up, none of the patients had AVN (Figure 5). At the last follow-up, no patient showed evidence of carpal bone arthrosis on X-rays. DTPA-gadolinium-enhanced MRI study of bone viability in the capitate region 6rd year postoperatively.
Discussion
Hitherto, several surgical techniques have been described for the management of Kienbock’s disease; however, the definitive treatment remains controversial. 2 In this regard, the present study was conducted to elucidate the clinical and radiological results of lunate excision accompanied by gradual capitate lengthening in the treatment of stage IIIA Kienbock’s disease.
The technique of bone lengthening with callotasis was first used in the hand for treating trauma and congenital deformities, and is currently being used widely and safely to restore bone length.12,13 In this study, we used the technique of callotasis to restore the carpal height ratio, which is decreased due to collapse of the AVN of lunate. No bone graft was required, since the capitate bone was gradually lengthened by distracting the callus. Therefore, there were no chances of donor area morbidity compared to the Graner II procedure. 8
It is noteworthy that capitate osteotomy, especially overstretching during one-stage lengthening, may rupture the blood vessels in the capitate region, resulting in deterioration of the blood circulation and AVN in the capitate bone. 14 Therefore, selecting the appropriate osteotomy site and technique can minimise iatrogenic trauma and the resultant circulatory disorder. Considering the intrinsic and extrinsic circulation of capitate, it has been reported that the middle and distal fragments are the least invasive locations. Accordingly, capitate osteotomy in all our patients was performed in the middle 1/3rd of the bone. Consequently, when gradual lengthening was done, the blood vessels were not stretched, and there was no deterioration in vascularity. Alternately, there is an increase in vascularity in the bone, which further reduces the risk of AVN. 14 Furthermore, a short immobilisation time is essential in reducing AVN risk. 15 With capitate callotasis, we required a very short immobilisation time as compared to other available techniques.
Although there are reports that callus formation may decrease with age, there were no secondary fractures during the consolidation or rehabilitation periods in any of our patients, even in the age group of 30 years (range: 20–38 years). Therefore, no patient required bone grafting.
Regarding clinical outcomes, since this technique allows initiating early postoperative rehabilitation compared to the other techniques, the overall increase in ROM was high, and there was a significant improvement in grip strength. 8 In our study, the average grip strength increased from 15.4 kg to 22.3 kg, the mean MWS score increased from 58.8 preoperatively to 79.4 postoperatively, and the mean pain intensity (VAS score) decreased bott at rest and during exertion.
In our study, the mean carpal height ratio changed from 0.39 preoperatively to 0.48 postoperatively. The existing literature suggests a possible relationship between negative ulnar variance and the development of Kienbock’s disease. 16 In our study, negative ulnar variance was detected in seven patients, which may have predisposed them to developing the disease.
Hierner et al. used four K-wires, two proximally and two distally, to perform scaphoid positioning using temporary K-wire fixation during surgery. After the external fixator was removed, they fixed the proximal row bones and the capitate bone percutaneously with the K-wire and started joint ROM exercises. 9 In comparison, we used only two 2 mm schanz screws, one proximally and 1 distally, and did not perform K-wire scaphoid positioning or proximal row fixation with K-wire after removal of the external fixator. We started joint ROM exercises immediately after the operation, and did not encounter any instability in any of the cases.
Notably, malalignment may be observed while lengthening the capitate, which may result in degenerative changes in the radiocarpal joint.
9
There was no evidence of malalignment in the sagittal plane in any of our patients; no degenerative changes were observed during the 5-year follow-up period on X-rays (Figure 6). Sagittal alignment measurements (a) Sagittal alignment measurement in healthy wrist (b). Sagittal alignment measurement in pathologic wrist.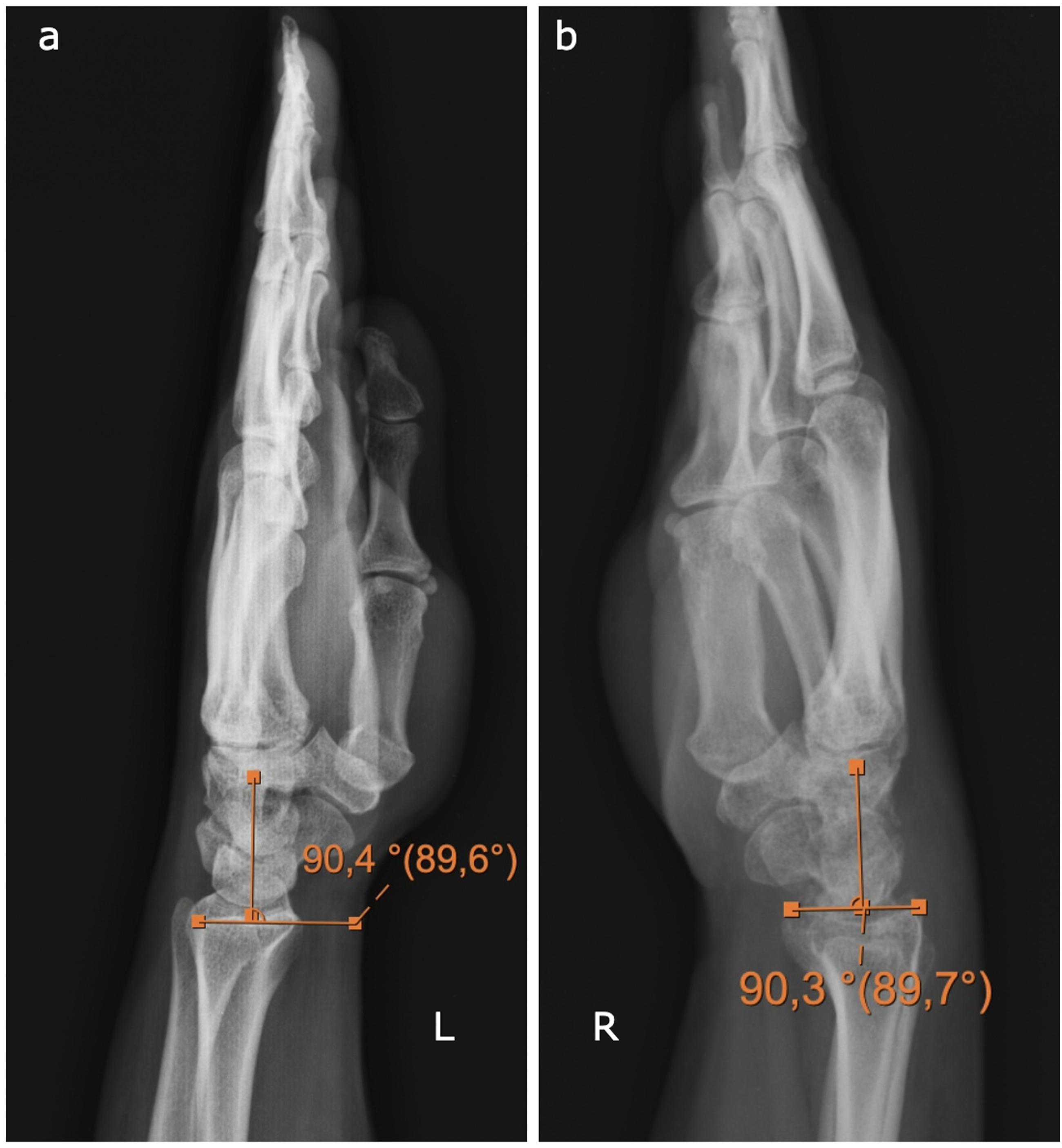
Limitations
This study had several limitations. Follow‐up duration was short and the sample size was small. Therefore, statistical bias was difficult to avoid, which led to the decline in reliability.
Conclusion
Gradual capitate lengthening used in the treatment of stage IIIA Kienbock’s disease has satisfactory mid-term results. Further longitudinal studies with larger sample sizes and longer follow-ups are required to corroborate the efficacy and safety of this technique.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
