Abstract
Breastfeeding rates in urban Malaysian mothers are below World Health Organization (WHO) targets. Our prospective survey identified breastfeeding prevalences at 3, 6, and 12 months of 85.5%, 77%, and 60%, respectively. Combined (direct and expressed) breastfeeding significantly sustained longer-term breastfeeding. Efforts should be focused on mothers of Indian ethnicity and on expression after one month postpartum.
Keywords
What We Already Know
Following the implementation of the WHO Baby-Friendly Hospital Initiative in Malaysia, the prevalence of exclusive breastfeeding among urban and rural mothers has increased.
However, the rate of exclusive breastfeeding remains below WHO global targets.
More women are working out-of-home, and this may lead to an earlier than intended cessation of breastfeeding. Thus, understanding breastfeeding behavior and practices is crucial.
What This Article Adds
Expression of breastmilk is common among urban working mothers; about one-half of mothers started doing so within one-month post-partum.
Direct breaastfeeding combined with expressed breastmilk at three months is a strong predictor of sustaining breastfeeding at 6 and 12 months compared to either method alone.
Exclusive breastfeeding at 3-months post-partum is a strong predictor of still breastfeeding at 6 and 12 months.
Introduction
The benefits of exclusive breastfeeding last long after its duration for both child and mother. 1 World Health Organization (WHO) recommends exclusive breastfeeding for the first six months of life, with continued breastfeeding up to two years and beyond. 2 The 6-month exclusive breastfeeding prevalence among Malaysian urban mothers was 48.3% in 2016, 3 below the WHO 2030 global target of 70%. 4 Understanding breastfeeding behavior and practices is crucial.
We conducted a prospective survey of postnatal breastfeeding practices among urban mothers to determine the prevalence and factors associated with breastfeeding outcomes at 3, 6, and 12 months.
Methods
We enrolled consecutive mother-infant pairs from the vaccination clinic in University Malaya Medical Centre (UMMC), Malaysia, from July to December 2016. Inclusion criteria were mothers aged above 18 years, without gestational or postnatal complications, and infants aged up to 3 months. The exclusion criteria were preterm or multiple births. Following consent, a face-to-face interview was conducted by trained researchers, using a pre-tested questionnaire. 5 Data obtained at enrolment included socio-demographic variables and infant feeding practices (exclusive/non-exclusive breastfeeding [as per WHO definitions 2 ] and direct, or expressed, or combined breastfeeding [direct and expressed 6 ]). Breastfeeding outcomes at 6 and 12 months were obtained during clinic visits or by telephone. The study was approved by the Medical Research Ethics Committee of UMMC, MREC Number: 20161-2019 and NMRR-17-3535-38512 and carried out in accordance with the Declaration of Helsinki.
All data were coded and analyzed using IBM SPSS Statistics (version 29). Variables were examined for association with still breastfeeding at 3, 6, and 12 months using univariate and multivariate logistic regression analyses. For the multivariate model, variables significant on the univariate analysis were included. Crude odds ratio (OR) adjusted odds ratio (aOR), and their 95% confidence intervals (CIs) are reported. Statistical significance was P < .05.
Results
Altogether, 312 mothers were enrolled, 25 still breastfeeding mothers (8.0%) were lost to follow-up, while the remaining 287 had outcomes recorded at 6 and 12 months (see Figure 1).
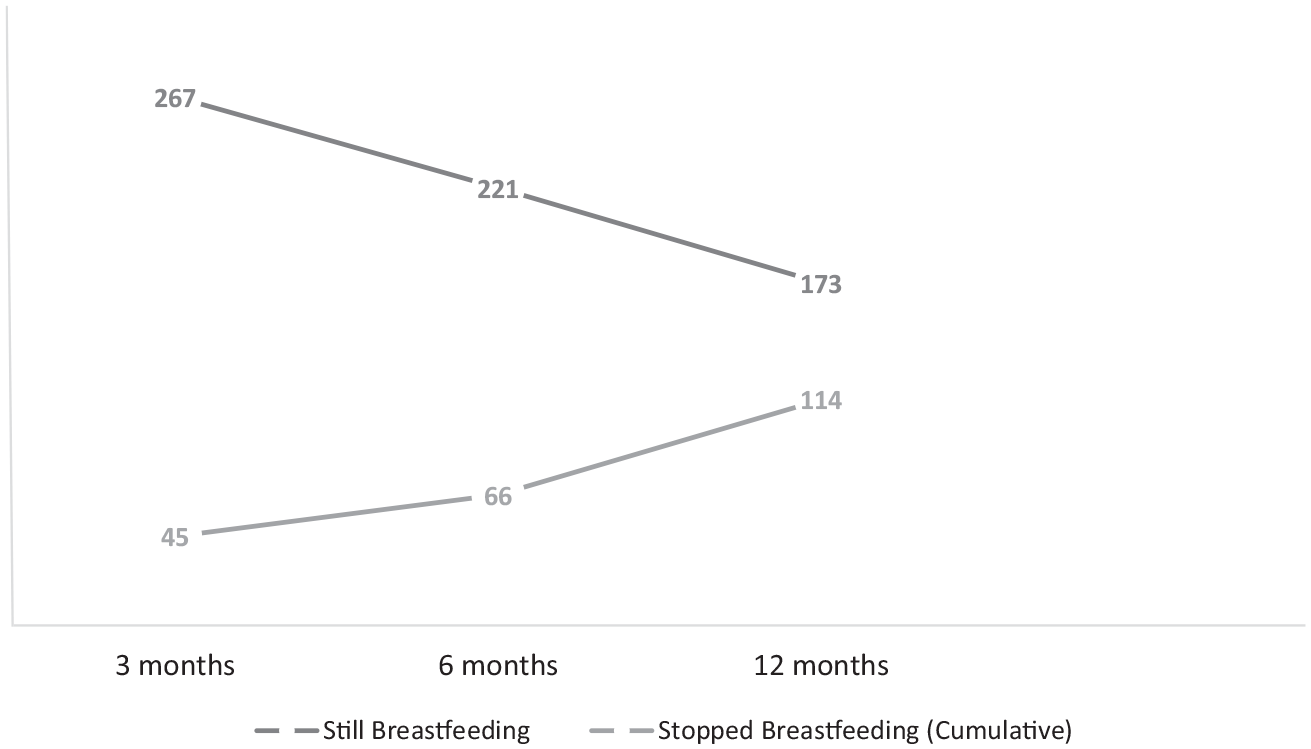
Mothers’ breastfeeding outcomes at 3, 6, and 12 months; total numbers analyzed were 312, 287, and 287, respectively.
Breastfeeding prevalence at 3, 6, and 12 months was 85.6%, 77.0%, and 60.3%, respectively.
Univariate and multivariate analyses results are shown in Tables 1 and 2, respectively. Ethnicity was significantly associated with breastfeeding duration. The odds of a Malay mother still breastfeeding at 3 and 12 months are 4.3 and 7.7 times higher than an Indian mother (aOR = 0.23, 95% CI [0.08, 0.65]; aOR = 0.13, 95% CI [0.05, 0.35], respectively). Other independent factors associated with sustained breastfeeding at 6 and 12 months were tertiary education (aOR = 3.23, 95% CI [1.17, 9.13]; aOR = 2.95, 95% CI [1.37, 6.32], respectively) and prior breastfeeding (aOR = 57.32, 95% CI [5.04, 652.32]; aOR = 1.98, 95% CI [1.02, 3.84], respectively). Expression of breast milk after the first month enabled breastfeeding at 3 months (aOR = 4.75, 95% CI [1.11, 20.35]) compared with those who had not expressed at 3 months. Mothers who expressed within the first month were 5.3 times less likely to continue breastfeeding at 12 months compared with those who did not express by 3 months (aOR = 0.19, 95% CI [0.06, 0.62]). The strongest predictors of breastfeeding at 6 and 12 months were the practices of exclusive breastfeeding at 3 months (aOR = 18.33, 95% CI [6.38, 52.68]; aOR = 9.99, 95% CI [4.69, 21.29], respectively) and combined breastfeeding (aOR = 15.91, 95% CI [5.47, 46.23]; aOR = 2.72, 95% CI [1.17, 6.32], respectively). Bed-sharing showed significance for breastfeeding at 3 months (aOR = 2.58, 95% CI [1.10, 6.05]).
Univariate Analysis of Breastfeeding Practices at 3 Months and Outcomes at Aged 3, 6, and 12 Months.
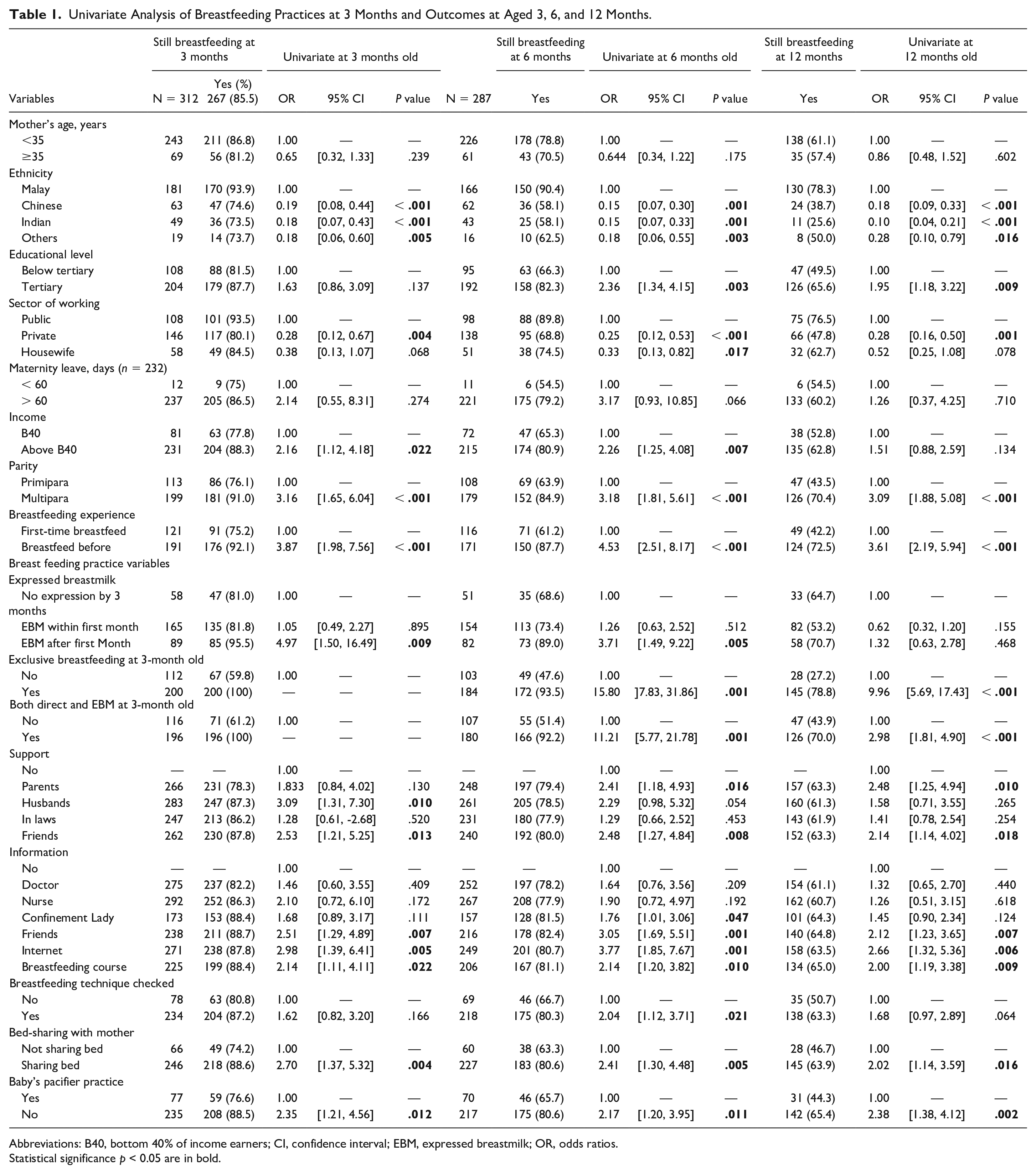
Abbreviations: B40, bottom 40% of income earners; CI, confidence interval; EBM, expressed breastmilk; OR, odds ratios.
Statistical significance p < 0.05 are in bold.
Breastfeeding Outcomes and Independent Associations From Multivariate Analysis Aged 3, 6, and 12 Months.
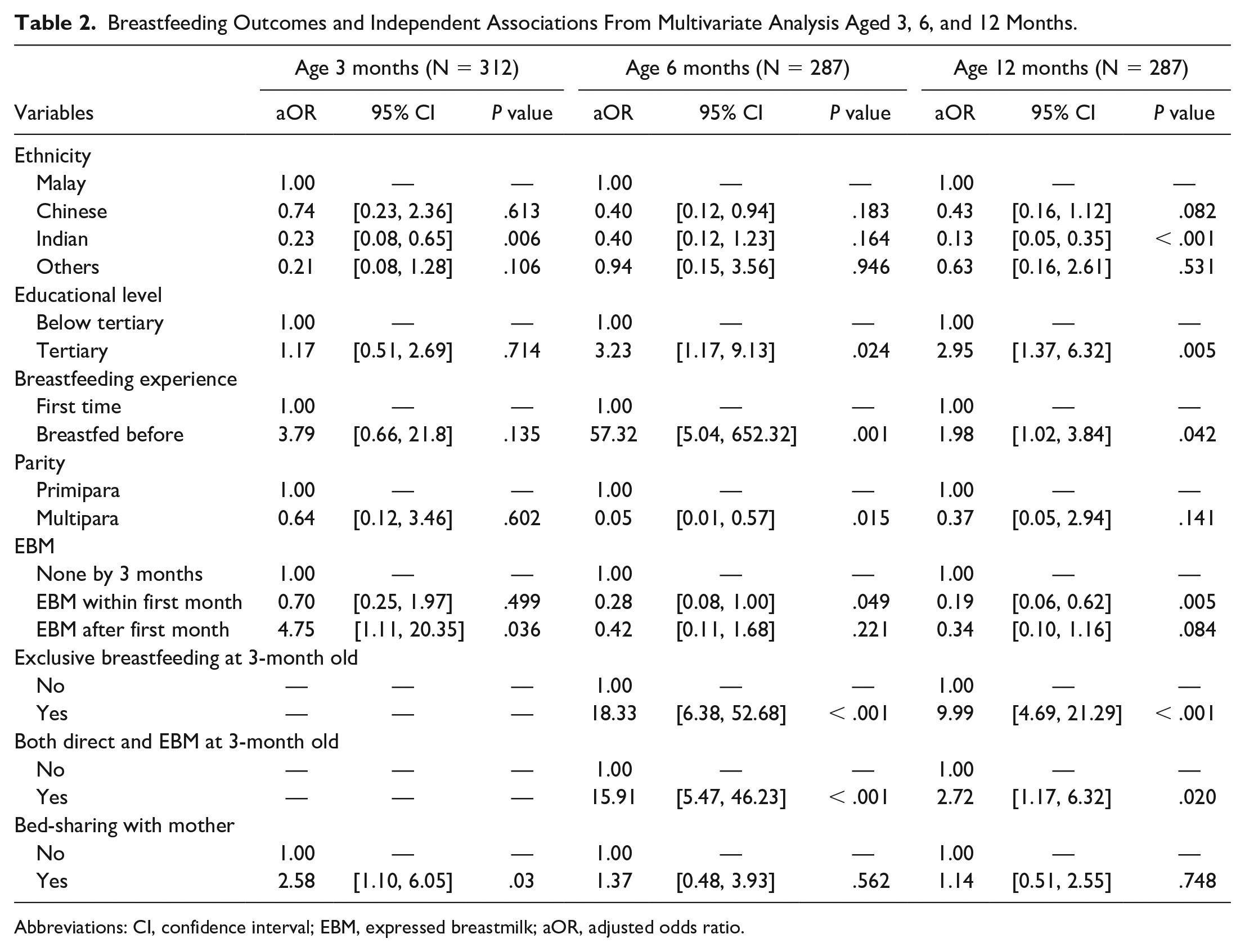
Abbreviations: CI, confidence interval; EBM, expressed breastmilk; aOR, adjusted odds ratio.
Discussion
In our cohort of urban Malaysian mothers, the rate of exclusive breastfeeding at 3 months postpartum was 64.1% and of ever breastfeeding at 3, 6, and 12 months was 85.5%, 77%, and 60%, respectively; the 2030 WHO global prevalence target at 12 months is 80%. 4
Among ethnicities, Malay mothers had the highest breastfeeding prevalence at all time points, while Indian mothers were significantly less likely to breastfeed at 3 and 12 months, in agreement with local research.5,7 Prior breastfeeding experience was a positive predictor of breastfeeding at 6 and 12 months; research shows these mothers have more self-efficacy and confidence for breastfeeding. 8
We observed significantly positive relationships between maternal tertiary education and prevalence and duration of breastfeeding, similar to high-income countries. 9 Previous research attributes this to increased awareness of breastmilk benefits, 9 greater intention to breastfeed, 8 and wider availability of milk expression, 10 allowing mothers to be away from home while continuing to feed their infants breastmilk. 6 Expression of breastmilk was high, 81.4% of mothers expressed by three months, compared with 56.6% in Singapore. 6 Compared with no expression at all, milk expression after the first month was an enabler of ever breastfeeding at three months, whereas expression within the first month was significantly associated with breastfeeding cessation by 12 months.
Combined breastfeeding at three months was a strong predictor of sustaining breastfeeding at 6 and 12 months compared with either direct or expressed breastfeeding alone, as seen elsewhere.6,10 Combined breastfeeding may be the most sustainable feeding strategy for working mothers to maintain mother-infant bonding and milk supply through direct feeding. Another strong predictor of still breastfeeding at 6 and 12 months was exclusive breastfeeding at three months postpartum, also found elsewhere. 6 Infant-mother bed-sharing practice was observed in 78.8%, comparable with a previous Malaysian study 5 ; this showed significance with breastfeeding at three months only.
This study is one of a few to describe the prevalence of breastfeeding and associated factors at three time-points up to 12 months among urban mothers in Malaysia. Our small sized, single-center study, limits generalizability. Nevertheless, the ethnic profile was representative of Malaysia. We did not explore the reasons why more than half of mothers expressed within one-month postpartum, long before returning to work.
Conclusion
For urban Malaysian mothers, ever breastfeeding prevalence at 3, 6, and 12 months was 85.5%, 77%, and 60%, respectively. Combined direct and expressed breastmilk helped sustain breastfeeding, though milk expression should only be encouraged after 1 month. To reach global targets, attention must be given to Indian mothers, those without tertiary education, and encouraging combined breastfeeding.
Supplemental Material
sj-docx-1-aph-10.1177_10105395231211978 – Supplemental material for Breastfeeding Prevalence and Factors Affecting Breastfeeding Duration Among Urban Multi-ethnic Malaysian Mothers: A Single-Center University Hospital Study
Supplemental material, sj-docx-1-aph-10.1177_10105395231211978 for Breastfeeding Prevalence and Factors Affecting Breastfeeding Duration Among Urban Multi-ethnic Malaysian Mothers: A Single-Center University Hospital Study by Kai Voon Heng, Lucy Chai See Lum, Emer Breen, Chuan Way Lye, Wai Chee Kuan, Saw Huan Goh, Ling Hang Tan and Kar Mun Yip in Asia Pacific Journal of Public Health
Footnotes
Acknowledgements
The authors acknowledge the contributions of the following individuals who assisted in patient enrollment and data curation: Pheng Hian Tan, Hui Ling Leong, Kai Wei Lim, and Yien Thung Loke.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Data Availability Statement
Data are available upon request and subject to approval by MREC UMMC.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
