Abstract
We aimed to evaluate the expression of amine oxidase-related proteins in metastatic breast cancer tissue and determine its clinical implication. A tissue microarray was constructed from a total of 126 metastatic breast tumors (31 bone metastases (24.6%), 36 brain metastases (28.6%), 11 liver metastases (8.7%), and 48 lung metastases (38.1%)). Immunohistochemical staining for amine oxidase-related proteins (lysyl oxidase, diamine oxidase, and monoamine oxidase A and B) was performed. In metastatic breast cancer tissue, lysyl oxidase (p = 0.001), tumoral diamine oxidase (p = 0.003), stromal diamine oxidase (p = 0.047), and stromal monoamine oxidase B (p = 0.002) were differentially expressed in different metastatic sites. Bone metastases showed low expression of lysyl oxidase, tumoral diamine oxidase, and stromal diamine oxidase. We observed high expression of lysyl oxidase in brain metastases, tumoral diamine oxidase in liver metastases, stromal diamine oxidase in lung metastases, and stromal monoamine oxidase B in bone metastases. Lysyl oxidase positivity was associated with progesterone receptor negativity (p = 0.001), and monoamine oxidase A positivity was associated with human epidermal growth factor receptor-2 negativity (p = 0.003) and the luminal A subtype (p = 0.003). On univariate analysis shorter overall survival was associated with stromal diamine oxidase negativity (p = 0.008), especially in lung metastases (p = 0.025), and stromal monoamine oxidase B positivity (p < 0.001). Stromal monoamine oxidase B positivity was an independent prognostic factor for shorter overall survival in multivariate Cox analysis (hazard ratio, 4.069; 95% confidence interval, 1.649–10.04; p = 0.002). Finally, in metastatic breast cancer, amine oxidase-related proteins were differentially expressed in a manner specific to metastatic site, and stromal monoamine oxidase B expression was correlated with prognosis.
Introduction
Amine oxidases convert alkylamines to aldehydes and ammonia by oxidative cleavage. Amine oxidases are separated into three groups: copper-containing amine oxidases, primary-amine oxidase (AOC2 and AOC3), and diamine oxidase (AOC1); copper-dependent enzyme, lysyl oxidase (LOX) and LOX family (LOX-like (LOXL)2,LOXL3,LOXL4); and flavin-containing amine oxidases, monoamine oxidase A and B (MAOA and MAOB). 1 Amine oxidases are involved in cellular differentiation, cell growth, wound healing, detoxification, and cell signaling via various metabolic pathways. 2 Amine oxidation is also associated with cancer biology. LOX expression has been reported to be associated with both tumor suppression and tumor progression,3,4 and LOX may have various intracellular localization, despite being an extracellular enzyme.5,6 In regard to tumor promoting roles, LOX is associated with the dissemination of colorectal cancer cells to the bone marrow. 7 LOX and other LOX family members are observed in breast cancer and, among them, upregulated LOX was reported to have association with breast cancer invasion and metastasis. 4 High expression of LOX is associated with bone metastasis and tumor relapse in estrogen receptor (ER)-negative breast cancer. 8 Also, LOXL2 expression was associated with poor prognosis in breast cancer. 9 Expression of AOC3 has been reported to correlate with poor prognosis in various tumor types.10–12 Altered MAOA expression is associated with tumorigenesis, metastasis, and poor prognosis in prostate cancer 13 and MAOB is highly expressed rate in glioma. 14
Breast cancer has high morbidity and mortality, mainly caused by the occurrence of distant metastasis. The major metastatic sites of breast cancer are the lung, brain, liver, and bone15,16 and brain and bone metastasis are the most thoroughly investigated.17–22 Tumor metastasis occurs by reciprocal interaction between tumor cells and host tissue, through mechanisms such as adhesion, proteolysis, invasion, and angiogenesis.16,23 Metastatic breast cancer has site-specific characteristics. Brain metastasis is associated with young age, ER negativity, prior lung metastasis, human epidermal growth factor receptor (HER)-2 overexpression, epidermal growth factor receptor overexpression, and basal subtype.19–21 Bone metastasis is associated with lower histologic grade, ER positivity, progesterone receptor (PR) negativity, strand growth pattern, and presence of fibrotic foci in invasive ductal carcinoma.18,24,25 Therefore, the biological traits of metastatic breast cancer may differ according to the metastatic site, and specific metabolic features have been reported for the varying metastatic sites. 26 Hence, differential expression of amine oxidases in different metastatic sites is expected, but has not been investigated thus far. In this study, we aimed to evaluate the expression of amine oxidase-related proteins in metastatic breast cancer and examine whether it has a clinical implication.
Materials and methods
Patient selection and histologic evaluation
During January 2000—December 2012, a total of 126 patients received removal of distant metastasis of breast cancer (liver, lung, brain, or bone) in Severance Hospital in Seoul, South Korea. Only patients with invasive ductal carcinoma of breast as a primary tumor were included. Metastatic carcinoma tissue samples were obtained when metastasis was suspected during follow-up of breast cancer patients. This retrospective study was approved by the Institutional Review Board of Yonsei University College of Medicine. All whole slides of distant metastasis tissues stained with hematoxylin and eosin (H&E) were reviewed again and pathologic diagnoses were approved by two pathologists (J.S.K. and W.H.J.). The histological grade was assessed using the Nottingham grading system. 27
Tissue microarray
A representative area encompassing tumor and tumor stroma was selected from an H&E-stained slide, and a corresponding spot was marked on the surface of the paraffin block. The tissue samples used for tissue microarray (TMA) block construction were collected from distant metastatic sites, and not from primary breast lesions. Only resected metastatic lesions were used. After review of the whole section of H&E-stained slides, representative areas were punched out for TMA construction. Small biopsy samples of metastatic sites were excluded. A puncher punched out 3-mm tissue core from the selected area, which was then transferred to a 6 × 5 recipient block. Two tissue cores of invasive tumor were extracted to minimize extraction bias. Each tissue core was assigned a unique TMA location number that was linked to a database containing other clinicopathologic data.
Immunohistochemistry
The antibodies used for immunohistochemistry in this study are shown in Table 1. A 3-μm-thick tissue section from formalin-fixed, paraffin-embedded tissue was deparaffinized and rehydrated using xylene and alcohol solutions, respectively. 28 Immunohistochemical staining was performed using a Ventana Discovery XT automated stainer (Ventana Medical Systems, Tucson, AZ, USA). Antigen retrieval was performed using CC1 buffer (Cell Conditioning 1; citrate buffer pH 6.0, Ventana Medical Systems). Appropriate positive and negative controls were included.
Source, clone, and dilution of antibodies.

Interpretation of immunohistochemical staining
All immunohistochemical markers were assessed using light microscopy. A cutoff value of 1% or more positively-stained nuclei was used to define ER and PR positivity. 29 HER-2 staining was analyzed according to the American Society of Clinical Oncology/College of American Pathologists guidelines using the following categories: 0 = no immunostaining; 1+ = weak incomplete membranous staining, less than 10% of tumor cells; 2+ = complete membranous staining, either uniform or weak in at least 10% of tumor cells; and 3+ = uniform intense membranous staining in at least 30% of tumor cells. 30 HER-2 immunostaining was considered positive when strong (3+) membranous staining was observed, whereas cases with 0 to 1+ were regarded as negative. Cases showing 2+ HER-2 expression on immunohistochemistry were evaluated for HER-2 amplification using fluorescent in situ hybridization (FISH). Nuclear positivity of Ki-67 was evaluated and the positive tumor cell percentage was reported as the Ki-67 labeling index (LI).
Stained slides were evaluated in a semi-quantitative manner. 31 Tumor and stromal cell staining were scored as follows: 0, negative or weak immunostaining in <1% of the tumor/stroma; 1, focal expression in 1%–10% of tumor/stroma; 2, positive in 11%–50% of tumor/stroma; and 3, positive in 51%–100% of tumor/stroma. Whole included tumor area was evaluated. A score of 0 was considered negative and a score of 1 or more was considered positive.
Tumor phenotype classification
In this study, we classified breast cancer phenotypes according to the immunohistochemistry results for ER, PR, HER-2, and Ki-67 and FISH results for HER-2 as follows: 32 luminal A, ER and/or PR positive, HER-2 negative, and Ki-67 LI < 14%; luminal B, (HER-2 negative) ER and/or PR positive, HER-2 negative, and Ki-67 LI ≥ 14%; (HER-2 positive) ER and/or PR positive and HER-2 overexpressed and/or amplified; HER-2, ER and PR negative and HER-2 overexpressed and/or amplified; triple negative breast cancer (TNBC): ER, PR, and HER-2 negative.
Statistical analysis
Data were analyzed using SPSS for Windows, Version 23.0 (SPSS Inc., Chicago, IL, USA). Pearson’s chi-square test was used for categorical variables. 33 Fisher’s 34 exact test was used for small sample size analysis. A corrected p value with the application of the Bonferroni 35 multiple comparison procedure was used for analyzing data with multiple comparisons. Statistical significance was set to p < 0.05. Kaplan–Meier survival curves 36 and log-rank statistics 37 were employed to evaluate time of overall survival. Multivariate regression analysis was performed using the Cox proportional hazards model. 38
Results
Clinicopathologic characteristics of metastatic breast cancer
Among the total 126 metastatic breast cancers, there were 31 bone metastases (24.6%), 36 brain metastases (28.6%), 11 liver metastases (8.7%), and 48 lung metastases (38.1%). The status of ER (p < 0.001), PR (p < 0.001), HER-2 (p = 0.032), and Ki-67 LI (p = 0.008) and the distribution of molecular subtype (p < 0.001) were significantly different among the metastatic sites. Brain metastasis was characterized by ER negativity, PR negativity, HER-2 positivity, and high Ki-67 LI. The predominant molecular subtypes were luminal A in bone and liver metastases, HER-2 and TNBC in brain metastases, and TNBC in lung metastases (Table 2). Since all of the patients were stage IV, most of the patients in this study did not receive mastectomy for curative purposes. Therefore, as assessment and correlation of tumor size or lymph node status were not available and appeared inappropriate, these parameters were not included as clinicopathologic factors for analysis.
Basal characteristics of patients with metastatic breast cancer.

ER: estrogen receptor; PR: progesterone receptor; HER-2: human epidermal growth factor receptor-2; LI: labeling index; TNBC: triple negative breast cancer.
Column percentage is used.
p values from Pearson’s chi-square test.
Expression of amine oxidase-related proteins in metastatic breast cancer
LOX (p = 0.001), tumoral AOC3 (p = 0.003), stromal AOC3 (p = 0.047), and stromal MAOB (p = 0.002) were differentially expressed among the metastatic sites (Table 3, Figures 1 and 2). Bone metastases showed the lowest rate of positivity for LOX, tumoral AOC3, and stromal AOC3 among the four metastatic sites. The most highly expressed amine oxidase-related protein in each metastatic site was LOX in brain metastases, AOC3 in liver metastases, stromal AOC3 in lung metastases, and stromal MAOB in bone metastases.
Expression of amine oxidase according to the metastatic site in breast cancer metastases.

LOX: lysyl oxidase; AOC3: diamine oxidase; S: stromal; MAOA: monoamine oxidase A; MAOB: monoamine oxidase B.
Column percentage is used.
p values from Pearson’s chi-square test.

Heat map of amine oxidase-related proteins in metastatic breast cancer.

Expression of amine oxidase-related proteins in metastatic breast cancer. Bone metastases show low expression of LOX, tumoral AOC3, and stromal AOC3. High expression of LOX is observed in brain metastases, AOC3 in liver metastases, stromal AOC3 in lung metastases, and stromal MAOB in bone metastases. Tumor cells and stroma are identified on hematoxylin and eosin staining in the first row, and specific expression of each amine oxidase-related protein in tumor cells or stroma are identified in the below rows.
Association between clinicopathologic factors and expression of amine oxidase-related proteins
LOX positivity was significantly associated with PR negativity (p = 0.001; Figure 3(a)). MAOA positivity showed a significant association with HER-2 negativity (p = 0.003; Figure 3(b)) and the luminal A subtype (p = 0.003; Figure 3(c)).

Association between clinicopathologic factors and expression of amine oxidase-related proteins. (a) LOX positivity is significantly associated with PR negativity (p = 0.002). (b) MAOA positivity significantly correlates with HER-2 negativity (p = 0.004) and (c) luminal A type (p = 0.003)
The impact of expression of amine oxidase-related proteins on overall survival in metastatic breast cancer
The relationship between expression of amine oxidase-related proteins and patient survival was analyzed by univariate log-rank test. Stromal AOC3 negativity and stromal MAOB positivity were associated with shorter overall survival on univariate analysis (p = 0.008 and p < 0.001, respectively, (Figure 4(a) and 4(c)). In lung metastases, stromal AOC3 negativity was associated with shorter overall survival (p = 0.025; Figure 4(d)). In brain metastases, tumoral and stromal MAOB positivity were associated with shorter overall survival (p = 0.009, and p = 0.032, respectively, Figure 4(e) and (f)). Through multivariate Cox analysis, we analyzed the significant parameters in univariate analysis (stromal AOC3 negativity and stromal MAOB positivity) and common prognostic factors of breast (ER, PR, HER-2, and molecular subtype). Stromal MAOB positivity was an independent prognostic factor for shorter overall survival in multivariate Cox analysis (hazard ratio, 4.069; 95% confidence interval, 1.649–10.04; p = 0.002; Table 4). Since the number of deaths in overall and each metastatic site were too small to yield significant statistical results, site-specific Cox analysis could not be performed.
Multivariate Cox analysis of the association between expression levels of amine oxidase in metastatic breast cancers and overall survival.

HR: hazard ratio; CI: confidential interval; ER: estrogen receptor; PR: progesterone receptor; HER-2: human epidermal growth factor-2; TNBC: triple negative breast cancer; AOC3: diamine oxidase; S: stromal; MAOB: monoamine oxidase B.
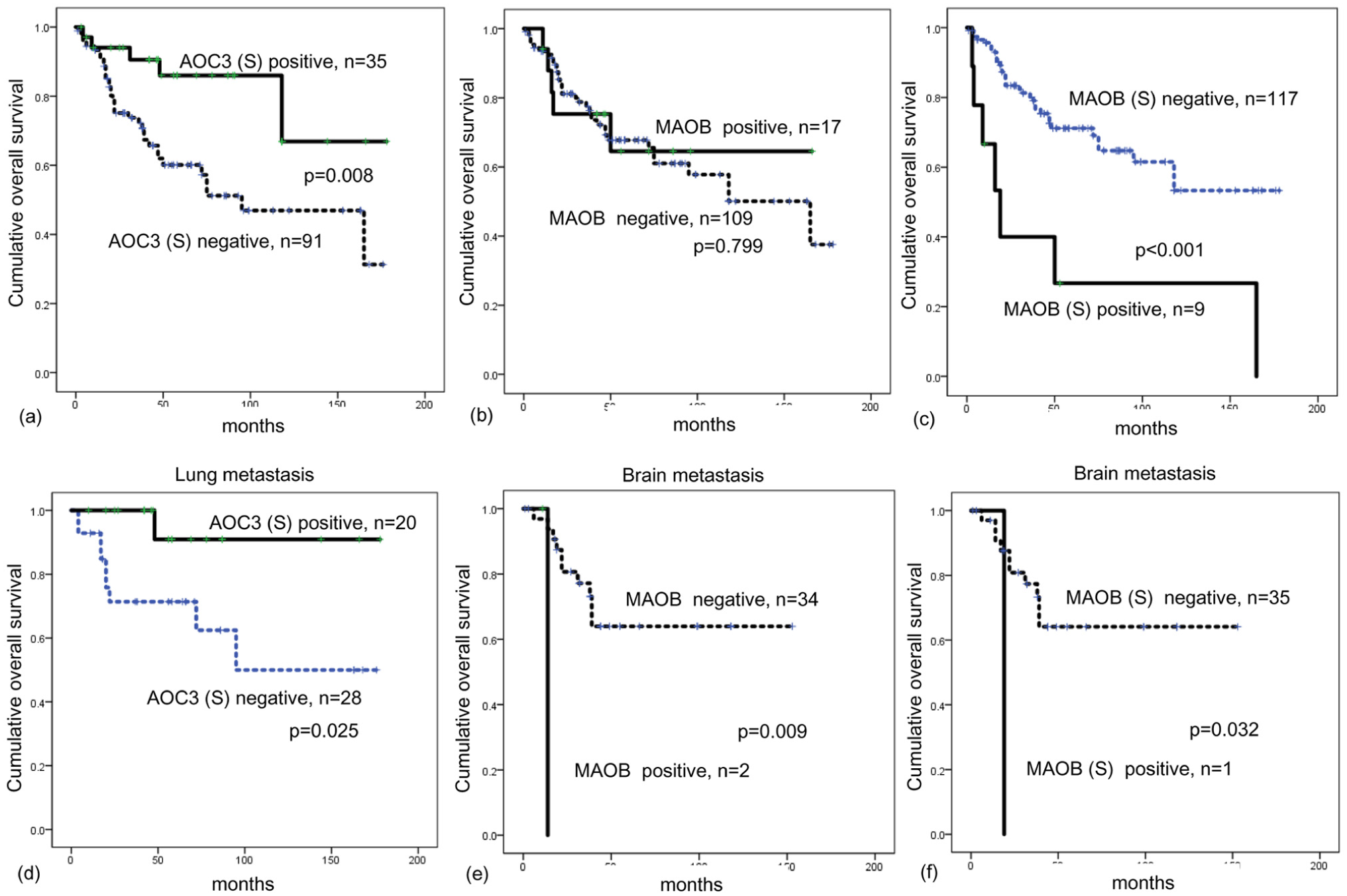
The impact of (a) stromal AOC3, (b) MAOB, and (c) stromal MAOB on prognosis in overall metastatic breast cancer. (d) Stromal AOC3 expression in lung metastasis is associated with shorter overall survival. (e) MAOB and (f) stromal MAOB expression in brain metastasis are associated with shorter overall survival.
Discussion
In our previous study on primary breast cancer, we showed that amine oxidase-related proteins were differentially expressed in breast cancer according to the molecular subtype. 11 In this study, we found that the expression of amine oxidase-related proteins in metastatic breast cancer differed among the metastatic sites. Among the LOX families, we examined the LOX expression, which have been reported to be upregulated in breast cancer. 39 Brain metastases showed the highest expression rate of LOX. LOX catalyzes cross-linking between collagen and elastin in the extracellular matrix (ECM), and can be detected in the cytoplasm with immunohistochemical staining. In this study, the nuclear localization of LOX was observed in metastatic breast cancer, which has also been reported in previous studies of ovarian and rectal cancers.5,40 Nuclear LOX expression in rectal cancer cells is linked to distant metastasis, and is an independent prognostic factor for poor overall and disease-free survival. 5 Nuclear LOX expression is also an independent prognostic factor for recurrence in advanced high-grade serous ovarian cancer, and appears to be involved in a metastatic cascade by regulating cell proliferation, migration, and anchorage-independent growth. 40 Thus, LOX seems to be associated with tumor metastasis. Also, higher expression of LOX in brain metastases implies that LOX may be involved in tumor progression of metastatic breast cancer in the brain.
Expression of AOC3 has been reported in various tumor types;10,12 however, its specific function in tumors has not thoroughly investigated. Therefore, further studies on the significant role of AOC3 expression in metastatic breast cancer are required. In this study, stromal AOC3 was most highly expressed in lung metastases. AOC3 has been reported as a marker of myofibroblasts, and is thought to be involved in differentiating and activating fibroblasts. 41 A subgroup of cancer-associated fibroblasts that have a myofibroblastic phenotype is reported to promote tumor cell motility 42 and regulate collagen fiber elongation, 43 suggesting that AOC3-expressing stromal cells may affect tumor biology. AOC3 also has an impact on pulmonary fibrosis. It regulates the accumulation of pathogenic leukocytes and induces fibrosis, collagen synthesis, and proliferation of myofibroblasts and CD4+ lymphocytes. 44 Therefore, metastatic breast cancer of the lung may lead to proliferation of AOC3-positive myofibroblasts that serve as a tumor stroma and affect tumor biology, although this requires further study.
The bone is one of the preferred metastatic sites of breast cancer, and is characterized by a hypoxic microenvironment that promotes metastatic progression. 45 Under hypoxia, hypoxia-inducible factor 1 alpha (HIF-1α) is activated and promotes a metastatic cascade. 45 LOX is also induced by hypoxia and regulated by HIF-1α, forming positive regulation loop.46,47 In addition, LOXL2 and LOXL4 are upregulated and mediated by HIF-1α.48,49 Moreover, MAOB expression has been reported to be correlated with HIF-1α levels in glioma. 14 The promoters of both HIF1A and MAOB have competitive binding sites for the transcription factors Sp1 and Sp3.14,50 Sp1 and Sp3 play a similar role in HIF-1α activation and expression. 51 However, Sp1 plays a role in the activation of MAOB, whereas Sp3 has a repressive role. 50 A previous study showed that hypoxia-induced downregulation of Sp3. 51 Thus, overexpression of MAOB in the stroma of bone metastases observed in this study may have been induced by the hypoxic microenvironment and consequent Sp3 downregulation.
In this study, a lack of stromal AOC3 expression was associated with shorter overall survival in lung metastasis patients by univariate analysis. As described above, AOC3-positive stromal cells (myofibroblasts) may affect tumor biology, and they may slow down tumor progression in lung metastasis. However, effect of stromal AOC3 expression was not significant when all patients were analyzed by multivariate analysis. Differently regulation of stromal AOC3 according to the different metastatic sites, or too small sample size of this study could be considered as an explanation for stromal AOC3 expression and prognosis. In general, a higher density of stromal myofibroblasts in solid cancer correlates with poor prognosis. 52 However, direct comparison appears to be not appropriate since all of the patients included in this study had already experienced distant metastasis.
Stromal MAOB was the only independent prognostic factor in this study. Although stromal MAOB expression was present in only 7.1% of patients and most frequently observed in bone metastases, both tumoral and stromal MAOB expressions were associated with shorter overall survival in patients with brain metastasis. As described above, stromal MAOB expression appears to be associated with a hypoxic microenvironment, which has been reported to promote distant metastasis leading to poor survival. 45 Moreover, brain metastasis itself is a poor prognostic factor in breast cancer patients. 53 Further extensive studies are required to clarify the prognostic role of stromal MAOB in metastatic breast cancer patients.
There are several limitations in this study. First, the overall sample size is small due to the difficulty of tissue collection, and even smaller when cases are divided according to the metastatic sites. Small sample size may lead to insignificant and unrepresentative statistical results. Second, mRNA levels prior to the proteins were not assessed in this study. Immunohistochemistry is a good method that could effectively identify the protein expression in the specific location among the tissue (tumor or stroma). However, not all expressed proteins that detected by immunohistochemistry are upregulated mRNA status. Since metastatic breast cancer cells may have modified biology compared to the cancer cells residing in primary lesions, further validation study with regard to genetic status is needed.
Our findings suggest that amine oxidase-related proteins could be clinically used as potential therapeutic targets in metastatic breast cancer. LOX inhibitor54–57 and MAOA inhibitor58–60 have been investigated in various types of cancer, including breast cancer, and metastatic breast cancer could also be a therapeutic candidate for these drugs. Further in vivo study to confirm the inhibition of amine oxidase-related proteins subsequent tumor suppression is required.
In conclusion, amine oxidase-related proteins are specifically differentially expressed in metastatic breast cancer according to metastatic site, and stromal MAOB expression status was associated with prognosis.
Footnotes
Acknowledgements
C.Y.J. participated in the design of the study, performed statistical analysis, and carried out the immunoassays. J.W.H. participated in its design. J.S.K. conceived the study, participated in its design and coordination, and helped to draft the manuscript. All the authors read and approved the final manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by a Grant from the National R&D Program for Cancer Control, Ministry of Health & Welfare, and Republic of Korea (1420080). This research was supported by the Basic Science Research Program through the National Research Foundation of Korea (NRF) funded by the Ministry of Science, ICT and Future Planning (2015R1A1A1A05001209).
