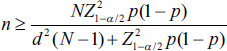Abstract
Background
Mental health issues in children and adolescents are quite significant. Despite their impact, research on psychiatric disorders in these age groups is limited. This study aims to evaluate the prescription patterns of psychiatric medications and the prevalence of psychiatric disorders among children and adolescent age group patients.
Objectives
This study aims to evaluate the prescription pattern of psychiatric medications and the pattern of psychiatric illnesses among child and adolescent age group patients at a tertiary care hospital in India.
Materials and Methods
This hospital-based observational study was conducted over 1.5 years at the Government Hospital for Mental Care in Visakhapatnam, India. A total of 150 patients aged 2–18 years, diagnosed with psychiatric disorders and prescribed at least one psychiatric drug, were included. Data on patient demographics, diagnoses, and prescription details were collected and analyzed using SPSS version 2022, following WHO drug use indicators. Cost analysis compared drug costs within the hospital pharmacy and external pharmacies.
Results
The study population comprised 56% children (2–10 years) and 44% adolescents (11–18 years), with a male predominance in both groups. The average number of medications per prescription was 2–4, with 94% prescribed by generic names and no use of fixed drug combinations or injectable drugs. Mental retardation was the most common disorder, followed by attention deficit hyperactive disorder (ADHD) in children and oppositional defiant disorder (ODD), bipolar disorder, and schizophrenia in adolescents. Risperidone, trihexyphenidyl, carbamazepine, and valproate were the most commonly prescribed medications. Most drugs were available at the hospital pharmacy, minimizing the financial burden on patients. Cost analysis showed significant variations in drug prices outside the hospital.
Conclusion
The study highlights the rational prescription trends among child and adolescent psychiatric patients. There was preference for atypical antipsychotics and newer drug classes over conventional medications. Polypharmacy was up to the mark. The findings emphasize the need for periodic prescription monitoring to ensure safe, effective, and cost-efficient treatment.
Keywords
Introduction
Mental health issues are emerging as a crucial medical aspect in the current world scenario. Mental problems affect 7.3% of children and adolescents in India, which is quite significant. 1 Psychiatric illness management constitutes 4% of the country’s economy. 2 The child age group refers to 2–10 years, and the adolescent age group refers to 11–19 years.3, 4 Children and adolescents differ in many aspects from adults. They vary in their physical maturity, physiological drug handling, along with the duration of treatment needed. The pattern of mental illnesses and the causing factors also vary between children–adolescents and adults. In India, every fifth person is an adolescent between the age group of 11 and 19 years. 5
Exposure to stressful environments can predispose to behavioral problems, anxiety, and depression in adolescents age group people. The number of research studies done on this age group is also considerably less than that of the adult population. Lately, polypharmacy has assumed importance due to a considerable increase in the number of choices of drugs available for prescription for a given condition. Multiple drug consumption can lead to drug–drug interactions, an increase in drug load expenditure, and a decrease in patient compliance. 6 The drug prescribing pattern has wide variations from place to place and time to time depending on various factors such as the prevalence pattern of diseases, availability of drugs, physician’s choice of prescribing, safety, and cost. Studies on the marketing, distribution, prescription, and use of medications in society, taking into account their medical, social, or economic effects, are defined by the “World Health Organization” as drug utilization. 7 For the assessment of the prescribing trend of drugs and for promoting safe and rational utilization of drugs, drug utilization and prescription monitoring studies are very much needed. The current research aims to evaluate the pattern of psychiatric problems and the trends in the prescription of antipsychotics and other psychiatric medications among children and adolescents.
Materials and Methods
The present study was a hospital-based observational study done for 18 months in “Government Hospital for Mental Care,” Visakhapatnam, Andhra Pradesh, after getting due approvals from “Superintendent of the Hospital” and “Institutional Ethics Committee” [IEC number: EC/NEW/INST/2019/397]. The study was done on a total of 150 patients. The prescriptions of subjects between the age group 2 and 18 years of both genders, who were visiting the psychiatric outpatient department on Wednesday when child and adolescent cases were seen, diagnosed with a psychiatric disorder and having at least one psychiatric drug being prescribed and were not requiring hospital admission were taken into consideration. Subjects with pre-existing comorbidities, and need admission were excluded from the study. The consent was taken from the “Legally Authorized Representative” (LAR) of the patient.
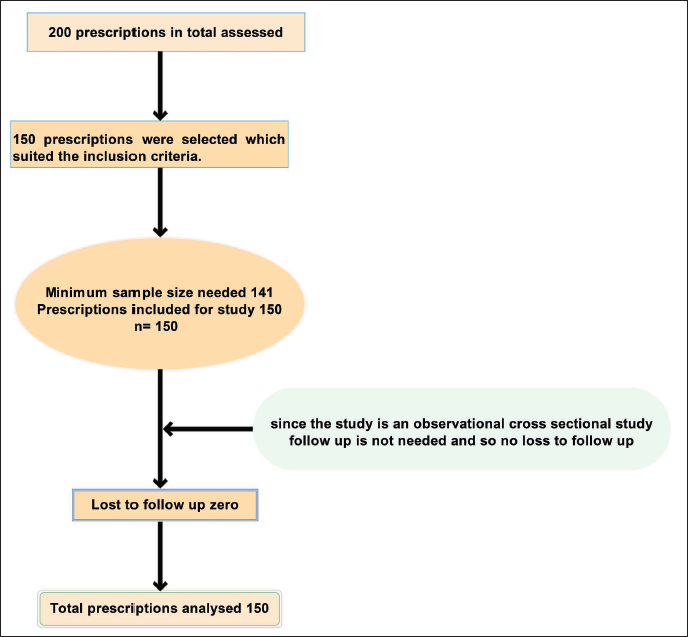
The details were collected according to the predesigned proforma. The following details: patient name, age, gender, guardian’s name, diagnosis, number of drugs prescribed, names of the prescribed drugs, dose, dosage form, dosing schedule, duration of the treatment, any fixed drug combinations or injectable were prescribed or not, and whether they were prescribed in generic or branded names were collected from the prescriptions. The data were fed into Microsoft Excel after cleaning and then exported to SPSS version 2022. The data assessment was done according to WHO drug use indicators. The significance level was fixed at 5% with a 95% confidence interval. Cost analysis was done by comparing the cost of drugs prescribed in the hospital store and from the pharmacies outside the hospital. The cost parameters calculated were: cost per tablet and cost of the drug therapy per month to estimate the financial burden of drug therapy on the patients. The sample size of 150 patients is calculated as below. Figure 1 displays a consort flow diagram to provide readers with clear information about the study.
Sample size: 150 patients.
8
Alpha (α) = 0.05
Estimated proportion (p) = 0.0646
Estimation error (d) = 0.01
Population size (N)
Minimum sample size needed: 141.
Consort Flow Diagram of the Present Study.
Results
A detailed analysis was conducted on the prescriptions of 150 patients who met the inclusion and exclusion criteria, and the following results were observed.
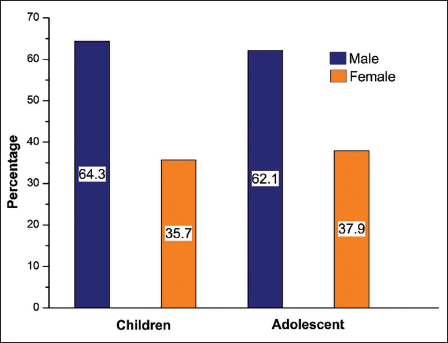
The distribution of the study population can be seen in Figure 2. Males outnumbered females. Child patients constituted 56% of the population, whereas adolescent patients constituted 44% of the total study population. Male patients were more in numbers among both age groups. 64.30% of the child cases and 62.10% of the adolescent cases were males.
Distribution of Study Population as Per Age and Gender.
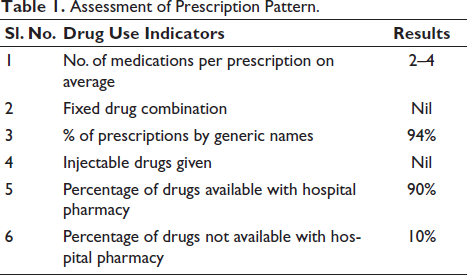
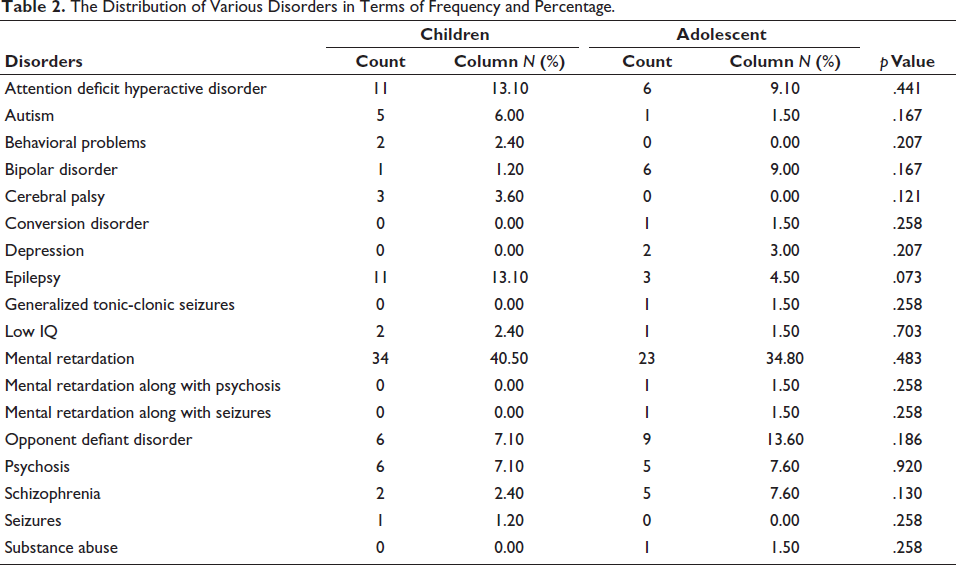
The minimum number of medications encountered per prescription was two, and the maximum was four. The majority of the drugs prescribed were generic drugs. Fixed drug combinations and injectable preparations were not encountered. Almost all the drugs were available in hospital pharmacies except a few, as depicted in Table 1. The pattern of disease distribution is depicted in Table 2.
Assessment of Prescription Pattern.
The Distribution of Various Disorders in Terms of Frequency and Percentage.
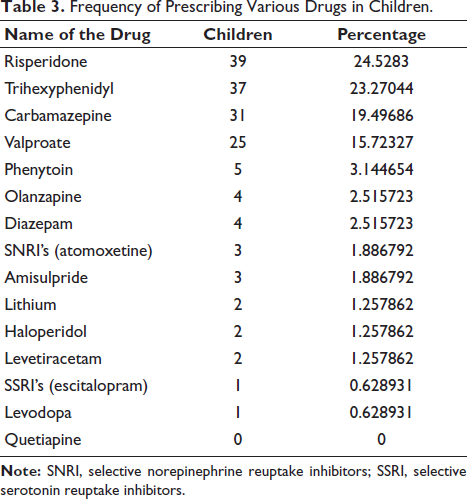
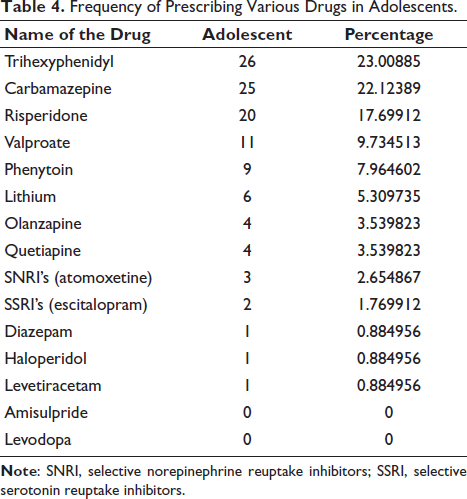
The drugs prescribed among children and adolescent patients are shown in Tables 3 and 4. Risperidone, trihexyphenidyl, carbamazepine, and valproate were some of the most commonly prescribed drugs in both groups. However, there was a variation in the pattern of prescription. Trihexyphenidyl was the most prescribed drug in adolescents, followed by carbamazepine and risperidone (Table 4), whereas in children, risperidone was most frequently prescribed, followed by trihexyphenidyl and carbamazepine (Table 3).
Frequency of Prescribing Various Drugs in Children.
Frequency of Prescribing Various Drugs in Adolescents.
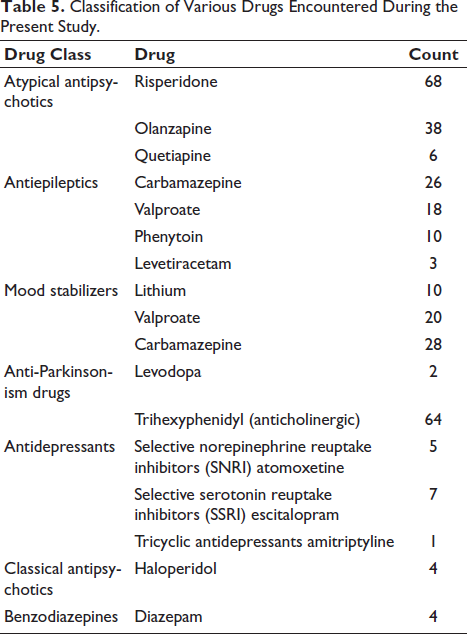
All the drugs encountered during the present study were classified into their respective groups in Table 5. They were classified into antipsychotics, antiepileptics, mood stabilizers, antidepressants, and anti-Parkinsonism drugs. Among antipsychotics, atypical antipsychotics were the most prescribed, and among them, risperidone was more frequently prescribed. Carbamazepine among the antiepileptics, lithium among the mood stabilizers, and SNRIs among the antidepressants were the most commonly prescribed drugs.
Classification of Various Drugs Encountered During the Present Study.
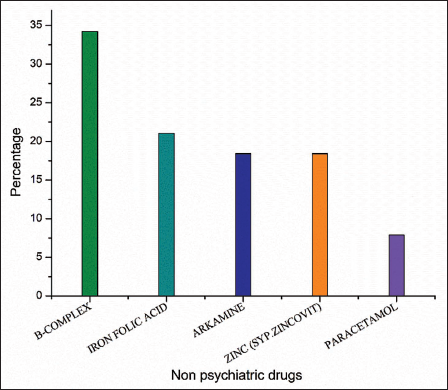
The drugs prescribed other than psychiatric medications can be seen in Figure 3. Iron, folic acid, B-complex, zinc, arkamin, and paracetamol were the drugs encountered.
Nonpsychiatric Drugs Prescribed to Children and Adolescents.
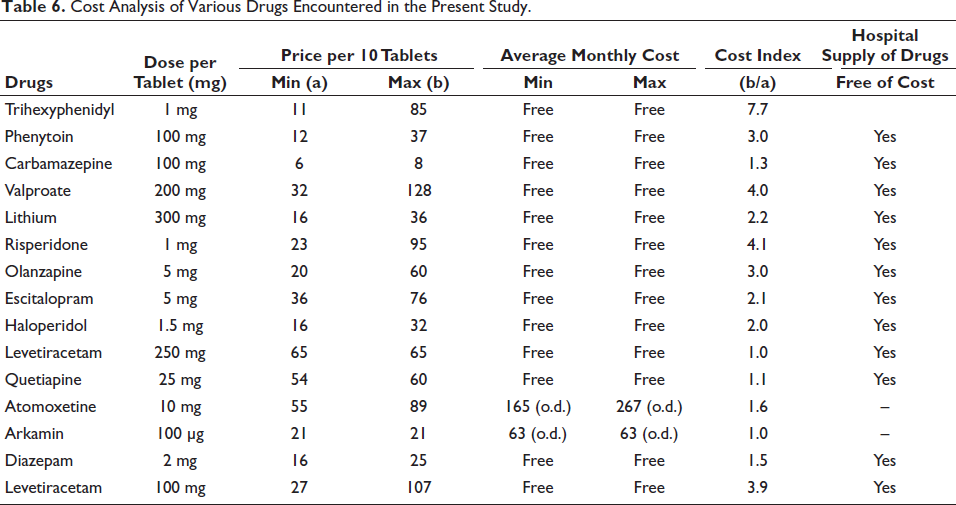
Most of the medications were obtained from the hospital pharmacy. Only the drugs that were unavailable at the hospital pharmacy were bought by the patients from outside pharmacies. Atomoxetine and arkamin were unavailable in the hospital pharmacy, as seen in Table 6.
Cost Analysis of Various Drugs Encountered in the Present Study.
Discussion
Mental illness in children and adolescents often goes unnoticed and lacks the required attention needed. The development of psychiatric illness in children and adolescents can be influenced by a variety of factors, including poverty, changing lifestyles, increased nuclear families, stress and educational competition, solitary parenting, inadequate care, and abusive environments. 9 It is crucial to acknowledge that the inappropriate use of drugs poses a potential risk to patients and also elevates the cost of drug therapy. This requires the periodic evaluation of the pattern of drug utilization. The present study was undertaken at the Government Hospital for Mental Care in Visakhapatnam for a period of 1.5 years after obtaining prior permissions from the “Institutional Ethics Committee.” Studies conducted on the selected age group were comparatively less than those of adult age groups. In the current study, children and adolescents comprised 56% and 44% of the total study population. According to Dörks et al. 10 findings, the age category of “11–19 years” was the most frequently encountered in the current study, whose study showed a preponderance of the adolescent age group “15–19 years.” Male patients outnumbered female patients in both age groups. Males constituted 64.30% and 62.10% among child and adolescent age groups, respectively. There can be several contributing factors behind the lower number of female cases like a preponderance of internalizing disorders among females, the reluctance of parents to bring female children to psychiatry fearing social stigma, the acceptance of mood disorders among females, and so on. 11
The average number of medications per prescription varied from one to four. The average number of medications per prescription was 2.5. This was consistent with the findings of Carmona-Huerta et al., 12 who got a mean value of 4.07. Polypharmacy is defined as the prescription of five or more drugs per prescription. 13 Some patients had more than one diagnosis, which made it necessary to prescribe multiple psychotropic drugs. The pressure to quickly resolve the patient’s complaints can also lead to favor of polypharmacy, which can cause increased side effects, drug costs, and poor compliance with the treatment.
In both child and adolescent cases, mental retardation (MR) was the most commonly encountered disorder. This was followed by attention deficit hyperactive disorder (ADHD) and epilepsy in children. In contrast, in adolescent oppositional defiant disorder (ODD), ADHD, bipolar, and schizophrenia were frequently encountered. MR was often found to be associated with seizures in children. This outcome was comparable to those attained by Lalwani et al., 14 whose studies also showed that MR was the most common disorder observed. The majority of the patients had only one disorder, and only a small proportion of people had two problems like MR associated with behavioral problems, seizures, or psychosis.
In the present study, atypical antipsychotics were more preferred to classical antipsychotics. Risperidone, olanzapine, and quetiapine were the standard atypical antipsychotics prescribed. Classical antipsychotics contributed only 4% of the total antipsychotics prescribed. Out of them, haloperidol was the only drug prescribed. These results were partly in agreement with the results obtained by Dörks et al. 10 and Ghosh et al., 15 in whose studies too atypical antipsychotics were more prescribed. Atypical antipsychotics, because of their lesser side extrapyramidal side effects, were much more preferred than classical ones.
Anticholinergics were the second most frequently prescribed medications in the current study. Of the total number of psychiatric medications prescribed, they accounted for 23.27%. In the present investigation, trihexyphenidyl was the sole anticholinergic that was encountered. It is frequently prescribed in conjunction with antipsychotic medications. Anticholinergics can only be used for a minimal period of time at the lowest dose possible as its extended usage can lead to side effects like angle closure, glaucoma, dryness of mouth, and urine retention. 16
Carbamazepine, followed by valproate, was the most commonly prescribed drug for mood disorders. Lithium is less preferred, constituting approximately 5% of the total psychiatric drugs prescribed. Lower prescribing rate of lithium can be due to various reasons like low therapeutic index, the necessity of periodic monitoring, and the occurrence of multiple side effects. The results obtained were in concurrence with the studies done by Mudhaliar et al. 17 and Kishi et al., 18 in whose studies also, it was observed that carbamazepine was most frequently prescribed with lithium being the second most commonly prescribed drug for mood disorders.
Selective norepinephrine reuptake inhibitors (SNRIs) were the most frequently prescribed drugs in the current study, followed by selective serotonin reuptake inhibitors (SSRIs) for various disorders, including depression and obsessive-compulsive disorder. Among the SSRIs, escitalopram was the most commonly prescribed drug, which was similar to the study done by Mehdi et al., 19 and among SNRIs, atomoxetine was the most frequently prescribed drug. Better tolerability, safety at higher doses, and absence of sedative effects of “SSRIs” and “SNRIs” lead to their preference as compared with tricyclic antidepressants. 20
In children, seizures were often accompanied with MR. Generalized tonic-clonic seizures were mostly observed in the adolescent age group. Epilepsy in childhood needs to be attended to and corrected as soon as possible before the development of chronic adverse effects. Carbamazepine was the most preferred antiepileptic drug, constituting 49% of the total antiepileptics prescribed, followed by valproate, phenytoin, and levetiracetam in children and adolescents; whereas, in studies done by Lee et al., 13 valproate was the most frequently administered medication, followed by clobazam and lamotrigine.
For other disorders like polysubstance abuse, psychosis, MR, and behavioral problems, anxiolytics were most commonly used. Diazepam was the only benzodiazepine encountered in the present study.
The present study was undertaken in a government hospital, so almost all the medications were free of cost. Only a few drugs were not available at the hospital pharmacy during the period of the present study. They include arkamin and atomoxetine, which were to be purchased outside. Table 7 gives the cost calculation chart of drugs not available in hospital pharmacies.
Cost Calculation Chart of Drugs Not Available in Hospital Pharmacy.

The results of this study were in line with various reported data and hold true in terms of the occurrence of psychiatric disorders, their prevalence and polypharmacy, and the types of drugs preferred in such conditions.
During the study, the following limitations and shortcomings were encountered.
Shorter duration of the study period.
Single-centered study.
Smaller sample size.
Reporting bias is an unavoidable limitation as various physicians were prescribed prescriptions during the study period.
Conclusion
Prescription monitoring studies were needed periodically to assess the prescribing trends of physicians and promote the rational utilization of drugs. It is also required to improve patient compliance and decrease the costs and healthcare burden on the patients. MR and ADHD were some of the most commonly occurring disorders in both children and adolescents. Atypical and newer classes of drugs were given more preference than the conventional group of drugs for treating psychiatric disorders. The availability of drugs at the hospital pharmacy was up to the mark. Polypharmacy was within the limits, indicating rational prescribing trends. There was slight overutilization of anticholinergics, especially in combination with antipsychotic drugs, which could lead to the occurrence of side effects like drying of the mouth, blurring of vision, constipation, and so on, and troublesome over the long term.
Footnotes
Abbreviations
Acknowledgments
The authors are thankful to the superintendent of Government Hospital for Mental Care, Visakhapatnam, for allowing us to do the study and are also quite thankful to the head of the Department of Pharmacology and Management of Gayatri Vidya Parishad for their encouragement.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to research, authorship, and/or publication of this article.
Ethical Approval
“Institutional Ethics Committee” approval number (IEC number: EC/NEW/INST/2019/397).
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.