Abstract
Background
Didactic Lecture (DL) is a teaching method that has been there for a long time in our educational system, but student involvement is minimal. Problem-based Learning (PBL) differs in that it involves students in the learning process. Various skills are learned, such as self-learning, group discussion, communication skills, teamwork and knowledge retention. Critical thinking, analysis and the ability to solve real problems are some benefits of PBL, which can help medical students understand clinical scenarios and analyse, interpret and come up with possible solutions based on sound knowledge. Thus, there is a need to assess the effectiveness of PBL in recall, interpretation and problem-solving skills as compared to the traditional lecture method, as there are very few Indian studies related to PBL in Indian medical students.
Materials and Methods
A non-randomised interventional study was carried out in the Department of Pharmacology at East Point Medical College, Bengaluru. Groups A and B, each with 60 medical students, participated in PBL and DL for either of the two competencies (myocardial infarction and iron deficiency anaemia). After the completion of the DL and PBL sessions, 20 multiple-choice questions (MCQs) were given to the students. The effectiveness of the teaching method was determined by comparing the mean scores of MCQs of both groups.
Results
The group scores were compared using an independent sample t-test and expressed as mean ± standard deviation. The total mean score of PBL for the topic myocardial infarction (11.00 ± 2.64, p value = .001) was statistically significant compared with the total mean score in the DL group (9.38 ± 2.52), and the total mean score of PBL for the topic iron deficiency anaemia (15.28 ± 3.53, p value = .001) was significant compared to the total mean score in the DL group (12.98 ± 3.61), respectively. The mean score for recall and problem-solving for the topic of myocardial infarction was statistically significant in the PBL group compared to the DL group. The mean score for recall, interpretation and problem-solving for the topic of iron deficiency anaemia was statistically significant in the PBL group compared with the DL group.
Conclusion
PBL showed marked improvement in recall, interpretation and problem-solving abilities compared with DL. So, including PBL as a teaching–learning method can promote active and student-centered learning.
Introduction
Medical education has seen a paradigm shift from teacher-centric to student-centric in the past few years. Innovative teaching and learning methods are the need of the hour in all fields. Pharmacology is concept-based and is crucial for a proper understanding of the principles of clinical management and the development of therapeutic guidelines.
1
Traditional lectures enable sharing a large body of knowledge with numerous students but frequently foster passive and superficial learning. In problem-based learning (PBL), a clinical case scenario is used, and the students (as a group) will go about exploring the topic more in a systematic method, mostly by self-learning.
2
This educational approach was pioneered at McMaster University in Canada, and it represents a change wherein the learning is more learner-centric.
3
It is believed that the PBL method is a more dynamic process wherein the student learns and develops a variety of abilities and skills, such as teamwork, information seeking, analyses, exploration of new information and decision-making.
4
Even now, traditional lectures are one of the most popular and economical teaching techniques for transmitting core knowledge and concepts to a larger audience. Evidence from research shows that lectures have some limitations. Important aspects of learning, such as new skill development, application of learned facts in each scenario or critical reasoning, which are required in professional courses, are limited in the traditional lecture method. Positive opinions of PBL in terms of satisfaction, communication abilities, interpersonal relationships, problem-solving and critical reasoning were reported by medical and dentistry students.5–8 However, studies related to PBL in pharmacology are very sparse among Indian medical students. Hence, the current study has been taken up to compare PBL versus didactic lecture (DL) as a teaching–learning method among the undergraduate medical students at East Point College of Medical Sciences and Research Centre, with the following objectives:
To compare the overall effectiveness of PBL and DL as a teaching method among undergraduate medical students. To determine the effectiveness of the PBL method in recall, interpretation and problem-solving skills.
Materials and Methods
This is a non-randomised interventional study conducted by the Department of Pharmacology at East Point College of Medical Sciences and Research Centre, Bangaluru. Approval was obtained from the Institutional Ethics Committee (Ref: EPCMSRC/ADM/IEC/2021-22/09). Second-year medical students were chosen for the study after obtaining their informed consent. Students were divided into two batches, Batch A and Batch B, in the Department of Pharmacology for the practical classes, respectively. We have considered the A batch as Group A and the B batch as Group B.
Group A was exposed to PBL, while a DL was conducted for Group B on the same competency (myocardial infarction) on the same day simultaneously. We ensured that the teaching materials and the facilitators were the same for both groups. We switched the groups in the next session; PBL was conducted for Group B, and Group A was exposed to DL for the competency (pharmacotherapy of iron deficiency anaemia), as shown in Figures 1 and 2, respectively. At the end of PBL and DL sessions, the students were assessed using a questionnaire. There were 20 multiple-choice questions (MCQs), of which eight questions were related to simple recall, six questions were related to interpretation and the remaining six questions were related to problem-solving. The effectiveness of the two teaching–learning methodologies was evaluated by comparing the test scores between the groups.
Schematic Representation of Flow of Study Participants for the Competency Myocardial Infarction.
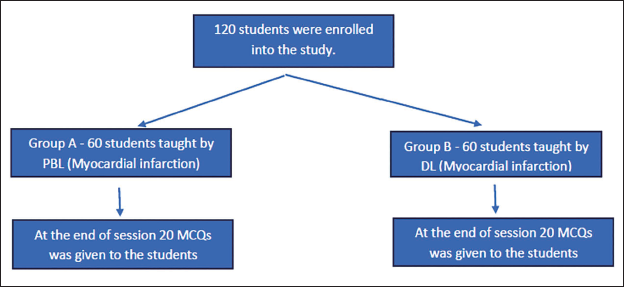
Schematic Representation of Flow of Study Participants for the Competency Iron Deficiency Anaemia.

PBL was conducted with the following steps:
Statistics
We performed statistical analysis using IBM SPSS, version 20. All quantitative variables were checked for normal distribution. Quantitative data are expressed as mean and standard deviation, while categorical data are expressed as frequency and proportion. The mean values were compared between research groups using the independent sample t-test (2 groups). A statistically significant p value was defined as less than .05.
Results
The study had 120 medical students as participants. The participants were of Indian descent. All the students had English as the medium of instruction at school. There were 60 students in each group. Results were expressed as mean ± standard deviation.
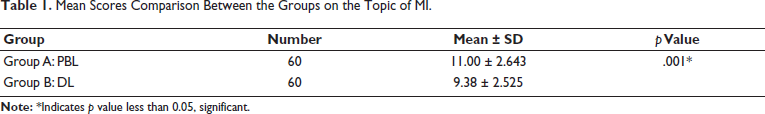
The total mean score of PBL for the topic myocardial infarction (11.00 ± 2.64, p value = .001) was statistically significant compared to the score in the DL group (9.38 ± 2.52), as shown in Table 1. The mean score of the ‘Recall’ aspect for PBL (4.85 ± 1.325, p value = .000) was statistically significant compared to the score in the DL group (3.90 ± 1.23), as shown in Table 2. Table 3 indicates that the mean score of the ‘Interpretation’ aspect for PBL (2.42 ± 0.97, p value = .081) did not differ significantly from the DL group score (2.73 ± 0.98). The mean score of the ‘Problem-solving’ aspect for PBL (3.73 ± 1.42, p value = .000) was statistically significant compared to the score in the DL group (2.75 ± 1.51) as shown in Table 4.
Mean Scores Comparison Between the Groups on the Topic of MI.

Mean Scores Comparison Between the Groups on the Recall Aspect for the Topic of MI.

Mean Scores Comparison Between the Groups on the Interpretation Aspect for the Topic of MI.

Mean Scores Comparison Between the Groups on the Problem-solving Aspect for the Topic of MI.

The total mean score of PBL for the topic of iron deficiency anaemia (15.28 ± 3.53, p value = .001) was statistically significant compared to the score in the DL group (12.98 ± 3.61), as shown in Table 5. The mean score of the ‘Recall’ aspect for PBL (6.37 ± 1.55, p value = .013) was statistically significant compared to the score in the DL group (5.68 ± 1.42), as shown in Table 6. The mean score of the ‘Interpretation’ aspect for PBL (4.5 ± 1.29, p value = .006) was statistically significant compared to the score in the DL group (3.78 ± 1.49), as shown in Table 7. The mean score of the ‘Problem-solving’ aspect for PBL (4.42 ± 1.39, p value = .003) was statistically significant compared to the score in the DL group (3.52 ± 1.81), as shown in Table 8.
Mean Scores Comparison Between the Groups on the Topic of Anaemia.

Mean Scores Comparison Between the Groups on the Recall Aspect for the Topic of Anaemia.

Mean Scores Comparison Between the Groups on the Interpretation Aspect for the Topic of Anaemia.

Mean Scores Comparison Between the Groups on the Problem-solving Aspect for the Topic of Anaemia.

Discussion
Lecture is a traditional and didactic teaching method used whenever there is a large audience and core concepts need to be provided. It is more of a one-way method, where the teacher shares the information, but student participation is minimal.
The PBL as an educational tool was first proposed and employed by McMaster University, Canada, in 1969. The focus of this method is on student-centered learning. The concept of PBL enables the learner to understand a given problem by exploring the information available on the problem and finding solutions to it. In contrast to a large audience in the traditional method, here the students learn in small groups (usually around 8–10 students) with a tutor. The tutor or facilitator is not the primary source of imparting facts; he/she only provides guidance. The students are given a clinical case scenario to start with. The students, as a group/team, learn to identify a problem, understand key concepts and develop learning objectives. The tutor provides necessary information as triggers and facilitates the students’ information-seeking and brainstorming activity. This activity helps the team to develop possible solutions and then share this information with others at subsequent sessions. 3
PBL facilitates the retention of knowledge, most of which is self-directed learning, and improves communication skills and teamwork spirit among the students. The students learn to interact better with their peers and the tutor and share a sense of responsibility in the problem-solving and decision-making process.
PBL has been tried as a teaching methodology and found to be effective in undergraduate medical curriculum. According to findings of a meta-analysis conducted in 2019 in China, 8 the PBL teaching model significantly increased theoretical knowledge scores by a mean of 1.16 compared to those of the lecture-based learning method (LBL) teaching model (95% CI, 0.79–1.52; p < .00001). This is consistent with the outcome of the current study.
Studies over the last 10 years have shown that PBL is effective in improving scores. It helps in enhancing attitude and learning skills. Important among them are problem-solving skills and interpretation. 5 A meta-analysis in 2014 of 15 studies 9 shows more increase in students’ theoretical examination scores in PBL (standard mean deviation [SMD] = 0.62, 95% CI = 0.41–0.83) than LBL. The pooled PBL effects were also significant among learning attitude (OR = 3.62, 95% CI = 2.40–5.16) and problem-solving skill (odds ratio [OR] = 4.80, 95% CI = 2.01–11.46). In four systematic reviews and meta-analyses, all from China, it has been revealed that PBL is more effective than LBL.10, 11
A study by Amir et al. 12 has shown that the PBL method resulted in better examination scores and improved problem-solving skills and student satisfaction among first-year MBBS students learning gross anatomy. Similarly, students showed better learning attitudes and examination scores in psychiatry when PBL was introduced than traditional methods of teaching. 13 However, studies looking at the effectiveness of PBL from India are very few. In the current study, we found that knowledge retention scores were higher in the PBL group than in the LBL group.
A questionnaire-based study by Mohan et al., 14 among the fifth-semester medical students at Kasturba Medical College, Manipal, Karnataka, done on 207 students who participated in the study voluntarily, showed that the score for PBL (4.0640 ± 0.05688) was significantly higher than LBL (3.2391 ± 0.05120, p < .05). Similar results were seen in a study conducted in Kerala. 15 In Uttar Pradesh, a study conducted using PBL (17.29 ± 1.87) showed a significantly higher mean score than lecture-based teaching (13.54 ± 5.05, p = .03). 16
The current study on the PBL method had been explored in a paraclinical subject, pharmacology, as compared to clinical subjects in most of the international and Indian studies.
Conclusion
The medical profession is challenging, and aspiring students need to become independent, lifelong learners with an astute ability to identify a problem and provide solutions. Therefore, it is important to employ a teaching–learning method that facilitates students seeking information on a given problem (self-directed learning), analysing and applying the information to a given problem, using critical thinking and interpretation, and providing possible and workable solutions. Following one teaching–learning method cannot impart all the skills to the medical graduate. Compared to traditional lecture-based learning, a combination or hybrid module of interactive small group discussions moderated by a facilitator in a conducive environment will maximise student-centered learning.
Limitations
The study was conducted among only second-year MBBS students, and the sample size was limited to 60 students per group. A comparison of the knowledge retention with pre-test and post-test scores would have been a better outcome parameter.
Footnotes
Abbreviations
Acknowledgments
The authors would like to acknowledge Dr Sudheer and Dr Drishya for their contributions.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
The approval for this study was obtained from the Institutional Ethics Committee (Ref: EPCMSRC/ADM/IEC/2021-22/09).
Funding
The authors received no financial support for the research, authorship, and publication of this article.
Informed Consent
For the study, informed consent was obtained from second-year medical students.
