Abstract
Background
Proton pump inhibitors (PPIs) are used for various conditions and are generally considered safe drugs; however, there has been a surge in their usage over time, partially related to their safety and overprescription.
Purpose
This study is aimed to assess how much the public of Lahore knows about PPI, and how they use it, and if they follow their physician’s instructions or not.
Methods
A cross-sectional study was planned to attain the objective of the study. Respondents visiting various community pharmacies were inquired about their willingness to participate in this study. Chi-square was used to find the association between sociodemographic parameters and awareness of PPIs. p value less than 0.05 was considered statistically significant.
Results
There were mostly university students (73.7%), with 82.2% having heard of PPIs. Prevalent use (86.85%) is observed, often after a medical condition. Notably, 60.1% use PPIs as needed, but only 52.3% complete the prescribed course. PPIs were taken before meals only by 69.3% of participants. Associations exist between having heard of PPIs, and age with younger participants (p < 0.001) exhibiting less awareness. Females also have heard lesser of PPIs (p = 0.011). Education correlates with unawareness (p < 0.001), and many participants are unaware of PPI side effects (51.04%).
Conclusion
The study contributes valuable insights to the understanding of PPI usage perspectives, offering implications for healthcare practices and public health awareness campaigns. Overall, the public shows signs of awareness but those are not enough to eliminate the misuse of PPIs in Lahore.
Introduction
Omeprazole was the first proton pump inhibitors (PPIs) introduced in 1989. Since then, they have gained widespread global usage owing to their established effectiveness and well-tolerated nature. PPIs are frequently employed in treating conditions such as infections from Helicobacter pylori bacteria, gastroesophageal reflux disease (GERD), ulcers resulting from nonsteroidal anti-inflammatory drugs (NSAID) use, excessive gastric acid production, and indigestion. 1 Recent research indicates that a significant proportion of individuals in the United Arab Emirates (UAE) utilize PPIs and are unaware of the potential adverse events associated with them. 2 Similarly in Saudi Arabia, public lack information about the potential adverse effects of using PPIs. 3 Healthcare providers exert considerable influence on the rates of prescribing PPIs. The usage of PPIs in clinical practice has continuously surged over time. The rise in PPI usage is due to factors like the substitution of H2 receptor antagonists (H2Ras) with acid secretion-controlling medications. 4 Further, the patent for the first PPI, omeprazole, expired in the early 2000s, leading to the availability of generic versions of the medication. This increased competition among pharmaceutical companies, resulting in lower prices for both brand-name and generic PPIs. The availability of generic formulations made PPIs more accessible to a larger population, contributing to their widespread use. 5 Due to inappropriate prescription and overutilization of PPIs, regulatory authorities worldwide are concerned about the increased risk of infections, nutritional deficiencies, rebound acid hypersecretion, masking underlying conditions, that is, GERD, and drug interactions for individuals taking multiple medications. 6 It is observed that healthcare providers thought this was happening a lot because doctors and patients did not fully understand the side effects. People need to follow the PPI schedule their doctor gives them. 7 Often people decide to use PPIs to relieve their symptoms; therefore, it is important to ensure that people use PPIs correctly, and understanding what they feel they need can make a significant difference. 8 Similarly in clinical settings irrational use of PPIs imposes a substantial burden on the healthcare systems across the globe. 9 Nevertheless, a comprehensive evaluation of the perspectives and behaviors of the public concerning the usage of these medications in emerging nations, such as Pakistan, is lacking in the existing literature. 10 Numerous side effects of PPIs are being studied, rational use of PPIs overcomes these, but widespread misuse leads to potential risk increase. 11 Self-evaluation along with self-medication is a prevalent issue in Pakistan. 12 PPIs are being used largely in diseases related to gastrointestinal track (GIT) and their irrational use is very common because people do not have any idea about their side effects. It is very important to create awareness in the general population. Some of the side effects of PPIs that are reported include the interaction of antiplatelet, bone fracture, pneumonia, and enteric infections. PPIs are widely prescribed drugs with many available over-the-counter (OTC). Even if they were not available as OTC, in Pakistan, you can get almost any drug without a prescription except some tightly controlled drugs, such as narcotics in a community pharmacy. 13 Self-evaluation along with self-medication is a prevalent issue in Pakistan. 12 Pakistan is one of the countries where there is widespread misuse of medicines but there seems to be no data on why and how much public is misusing certain medications. Hence, this project was conducted to estimate the awareness of the public regarding PPI usage in Lahore, Punjab, Pakistan.
Materials and Methods
A cross-sectional study was planned to attain the objective of the study. Respondents visiting various community pharmacies were inquired about their willingness to participate in this study.
Study Location
The study was conducted in Lahore, Punjab, Pakistan’s general population.
Study Duration
Data were collected over the period of two months, from September 16th to November 16th, 2023.
Study Population
The study was conducted on a general population including both males and females, and the age group was between 18 and 60 years using a self-administered questionnaire.
Sample Size Calculation
The sample size was found using Daniel’s sample size formula, with the settings at a prevalence of 50% for the maximum sample, as the prevalence of usage is unknown. The entire estimation was performed at the confidence interval of 95% with a margin of error of 5%. Using these values, the minimum effective sample size appropriate for this study was found to be 385.
Study Tool
A previously developed and validated tool was used to attain the objectives of this study. Permission of use was granted by the main author and it was adapted as such from their study with only minute changes. 14
Content Validation
Upon incorporating the minute changes the final study tool was piloted among 10 respondents to confirm the appropriateness of the questions and alignment of the study tool with the study objectives.
Structure of the Study Tool
There were three sections in the questionnaire. The first section collected demographics and educational background data of the participants of five items, including age, gender (assigned at birth according to anatomical features), education level, and the participant’s belonging in the medical field, and if they did with which field they belonged to. The second section collected data on the familiarity and awareness with PPIs. It included two multiple options but single-response questions. The third section includes the measurement of participant’s usage and habits regarding PPI intake. This section included eight questions assessing participant’s source of medical information and prescription practices, their usage of PPIs (why, how, when, and completion), and their knowledge of side effects.
Procedure for Data Collection
A self-administered questionnaire was used to collect data from potential respondents. In the case if the candidate needing linguistic support, word-to-word translation was done for them so that they can respond to the study questions appropriately.
Ethical Considerations
People were made aware of our research and given consent to opt out or in. No personal information was collected or retained. Data were kept confidential and only the research team had access to it. There was no benefit or harm to the participants involved. In addition, the study protocol was approved by the department’s human ethics committee.
Statistical Analysis
The statistical package for social sciences was used to perform statistics on the data. Chi-square was used to find the association between sociodemographic parameters and awareness of PPIs. p value less than 0.05 was considered statistically significant.
Results
A total of N = 520 respondents were approached for their participation, of whom n = 388 responded/consented to participate in the interview with a response rate of 74.61%. Among the 388 individuals included in our study pool, females constituted 52.8% of the sample, while males constituted 47.2%. In terms of age distribution, 13.7% of the individuals involved were under the age of 20, 52.8% were between the ages of 21 and 30, 11.3% were between 31 and 40 years, 8.0% were between 41 and 50 years, and 14.2% were above the age of 50. Only 23.2% of the individuals involved worked in the medical sector, that is, students (5.9%), doctors (3.4%), administrators (0.5%), pharmacists (6.44%), nurses (1.54%), technicians (2.6%), and others (3.6%). A major portion of people were university students 73.7%, 13.1% were high school graduates, 3.35% had a diploma, and 1.5% were illiterate. Table 1 shows the sociodemographics of participants.
Sociodemographic Parameters of Participants.
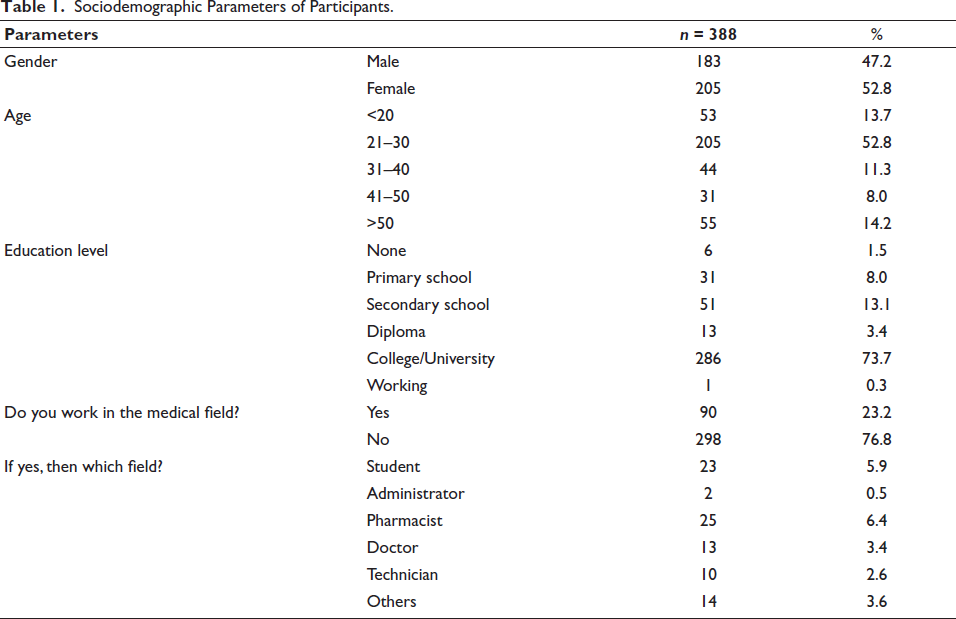
Merely 82.2% of the individuals involved were aware of PPIs beforehand. Concerning their usage, 86.85% with medical consultation had previously taken PPIs, while 13.4% had used them without any visit to the physician. Among all PPIs’ uses, H. pylori infection (14.1%), attribution to peptic ulcer (1.6%), heartburn (4.9%), GERD (0.5%), esophagitis (15.7%), asthma (2.8%), hoarseness (0.5%), gastritis (37.8%), gastroenteritis (11.9%), hiatal hernia (1.2%), and sore throat (5.6%), 18.8% of individuals involved did not know the indication of usage and 2.6% patients were prescribed PPIs to prevent side effects of other medications, shown in Table 2.
Participants’ Knowledge Usage and an Indication of Proton Pump Inhibitors.
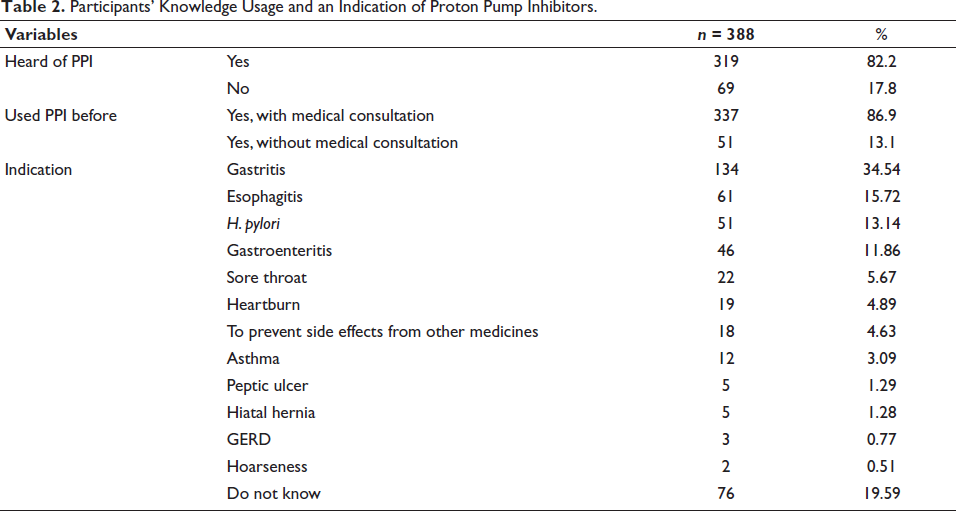
In terms of usage duration, 60.1% (233 individuals) of PPI users utilized them as needed, 12.37% (48 individuals) were irregular in their PPI usage, 11.59% (45 individuals) used them regularly for over four weeks, 11.34% (44 individuals) used regularly for less than four weeks, and 4.6% of users did not adhere to the recommended treatment duration. Among individuals involved, 69.3% suggested taking PPIs before meals, 24% after meals, and 6.7% with meals. Interestingly, only 52.3% of PPI users finished their treatment duration. Of those who did not finish the treatment duration, 66.5% attributed this to symptom relief, 14.05% to concerns about side effects, 10.2% to experiencing side effects, 4.3% to advice from medical acquaintances, 3.2% to cost or availability issues, and 6% to advice from nonmedical acquaintances. The participants seemed to be of the view that medicines are meant to be stopped as soon as they feel relief, and this turns out to show that they have no idea how medicines work. This can be complicated as it poses a concern for healthcare practices not just in terms of PPIs; but for other medications as well such as antibiotics, there is an immense need to make people adhere to regimens for the cause of their safety. Table 3 shows the duration of use of PPIs and course completion.
Usage Duration of the Drug, Their Appropriate Time, and Whether the Course Is Completed Among the Participants.
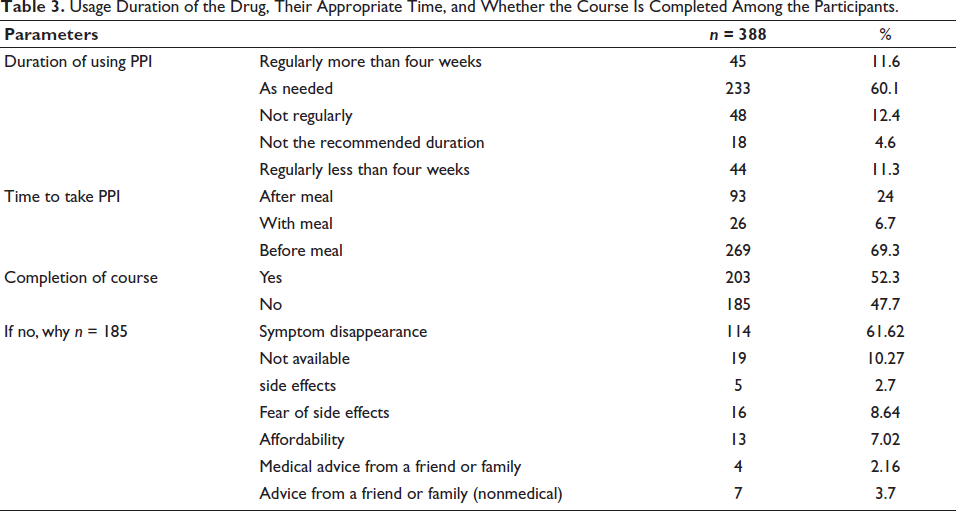
The study findings revealed a significant association between females and males having heard of PPIs (p value = 0.011 of chi-square) and between younger and older individuals (p value < 0.001). Additionally, those individuals who belong to the medical sector have a better understanding regarding PPIs (p value < 0.001). Unexpectedly, there was no notable link found between higher educational attainment and awareness of PPIs (p value = 0.110). Overall, older participants showed a significant awareness of PPI usage compared to younger individuals (p value = 0.029). Moreover, variables such as gender (p value = 0.375), education level (p value = 0.989), and profession in the medical field (p value = 0.515) did not significantly influence PPI utilization, regardless of medical condition (Table 4).
Association Between Participant’s Awareness and Usage of PPIs with Sociodemographic Parameters.
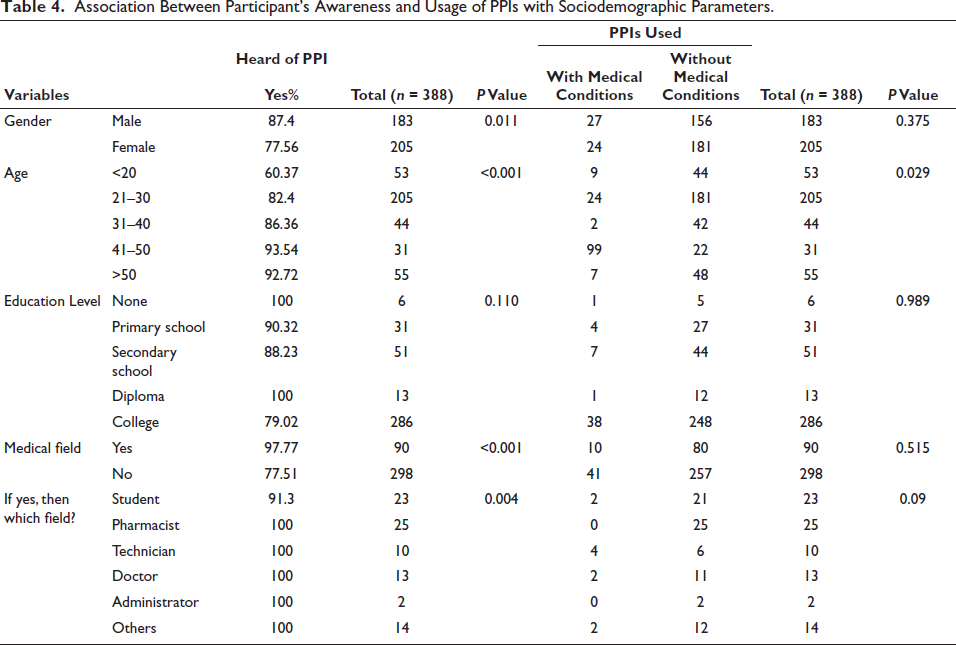
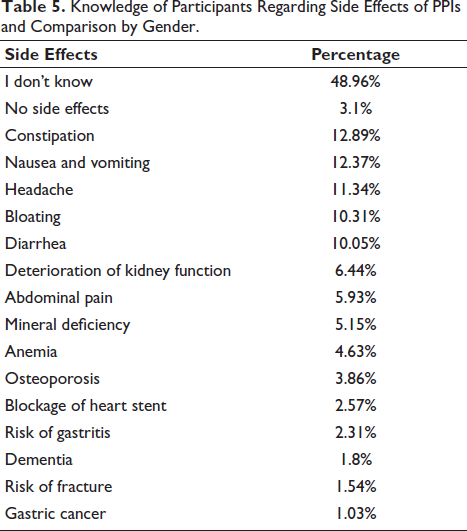
Almost half of the participants reported no knowledge of side effects (51.04%) followed by constipation, nausea and vomiting, headache, bloating, and diarrhea (12.89%, 12.37%, 11.34%, 10.3%, and 10.05%, respectively) as the most common side effects. Others included kidney function deterioration, iron deficiency anemia, blockage of heart stent, and dementia. Table 5 illustrates the side effects of PPIs as acknowledged by participants.
Knowledge of Participants Regarding Side Effects of PPIs and Comparison by Gender.
Discussion
This is perhaps the first study from Pakistan aiming to explore this important topic regarding the use of PPIs. Results have shown that most participants (60.1%) used PPIs as needed, while only 52.3% completed the full course of treatment. This suggests that a significant proportion of patients may not be adhering to their prescribed PPI regimen. 15 Adherence to therapy is one of the main markers of better therapeutic outcomes for any disease, however, 66.5% of those who did not complete the PPI regimen as recommended stated that their symptoms improved with one dose and that is why they stopped using PPIs This is understandable, as PPIs are often used to relieve symptoms of heartburn and acid reflux. However, it is important to note that PPIs are not a cure for these conditions, and stopping them too early may lead to a reoccurrence of symptoms. 16 Further exploration revealed that fear of side effects (14.05%) and actual side effects (10.2%) were identified as significant factors leading to noncompletion.
This highlights the importance of educating patients about the potential adverse effects of PPIs and providing reassurance that these side effects are often mild and transient. 17 A smaller percentage of participants discontinued the PPIs because of advice from friends or family (medical: 4.3%, nonmedical: 6%) or affordability/availability issues (3.2%). These factors are of great importance to the healthcare providers so that if any patients are reporting noncompliance to PPI regimen can be educated on these aspects to enhance their compliance to therapy. Some of the other factors reported in the literature led to noncompliance with PPIs. Surprisingly demographic variables were also reported in literature affecting the level of adherence; it was seen that younger, married, and symptomatic patients had lower levels of adherence. 18 Future studies shall explore these factors to identify ways to improve PPI adherence. 19 In addition, another aspect regarding the use of PPIs is the time at which PPIs were consumed; about 30.0% of the respondents were consuming PPIs with a meal or after a meal which might lower their effect; Therefore, the timing of PPI intake varied, with most participants taking them before meals (69.3%), followed by after meals (24%), and with meals (6.7%). It is important to note that the optimal timing of PPI intake may vary depending on the specific medication and the patient’s condition. 20
Further analysis revealed that gender has a significant influence on the awareness about PPIs; it was revealed from the analysis that females were significantly less aware of PPIs in comparison to male respondents. Limited health literacy, lack of exposure to PPIs, and a limited number of episodes of acidity or gut-related complications in comparison to male participants could be some of the main factors resulting in lower awareness about PPIs. In addition, it was also observed that respondents aged 40 and above were found to have awareness about PPIs in comparison to the other age groups or younger individuals. This could be because with age, people become prone to chronic diseases and there is a link between people suffering from chronic diseases and their knowledge and understanding about the drugs and diseases increases. 21 A Danish nationwide drug utilization study also showed that the use of PPIs is increasing rapidly among the elderly. 22 Lack of education is also linked with people being unaware of medicines, also lack of public health literacy is directly linked to inappropriate use of medications. 23 People belonging to the health sciences discipline are more likely to be aware of PPIs than people who do not and that is understood. There is still the factor that students belonging to medical fields could still be unaware of PPIs as they are still learning.
Regarding side effects, most people did not recognize any side effects with usage or believed that PPIs had no side effects at all. PPIs do have prominent side effects with misuse or nonadherence to therapy, but the lack of awareness leads people to think that they may be the result of some other health condition. 24 Patients usually show no concern regarding the adverse effects of chronic use of PPIs and they do not discuss the pros and cons of PPIs with their healthcare providers. 25 An interesting factor was that 13.4% used PPIs without any medical consultation. This could be a dangerous factor because stratification of short-term (<1 year) and long-term (≥1 year) PPI unsupervised use without prescription can lead to fractures which may result in to additional burden to the healthcare system. 26 Therefore, it is vital to educate the patients, most preferably in their mother tongue so that patient literacy about PPIs’ use, their existing health condition, and side effects can be improved. Presenting information in the mother language of patients improves patient knowledge (adults, children, or patients with any other comorbid conditions, e.g., asthma).27, 28 The use of Omeprazole in GERD-related asthma may be beneficial by reducing asthma symptoms and improving pulmonary function. 29 It was also observed that PPIs were being prescribed alongside other medications to patients. The use of NSAIDs, steroids, aldosterone antagonists, and SSRIs can contribute to gastric ulcer and its complications so the use of PPIs along with these drugs reduces the chances of gastric ulceration. 30 Therefore, it is extremely vital to get appropriate consultation from an expert to avoid the unforeseeable circumstances that are associated with the unsupervised or self-directed use of PPIs.
Strength and Limitations
The uniqueness of this research lies in its status as the inaugural research of its kind conducted in Lahore, Pakistan. The findings of this study will help health policymakers assess the usage of PPIs and will contribute to the rational use of PPIs. The limitation is that the participants may provide responses that they perceive as socially desirable rather than reflecting their true awareness and knowledge of PPIs. This could lead to overestimation or underestimation of awareness levels. Since it is a cross-sectional study, covering one-point data collection, it cannot be used to analyze the full complexity of the problem and can lead to biased, incomplete conclusions. The population of study is urban so we cannot implement the same results on rural populations. Addressing these limitations can help improve the generalizability of the findings.
Conclusion
Results of this study have shown that respondent of this study was found to have a moderate level of understanding regarding the use of PPIs, side effects, and other information that is associated with their safe use; hence, the misuse of PPIs is prevalent. Regardless of sociodemographic factors, the respondents use PPIs without medical conditions, discontinue without completing regimens, and have misconceived notions about the efficacy of PPIs. PPIs are safer drugs, but overuse and overprescription lead to potential risks, and there is growing concern about their lack of awareness. This study will contribute to helping health policymakers regarding the misuse of PPIs in Pakistan. Healthcare professionals can get current insights about the percentage of people adhering to regimens and their prescriptions. There should be mandatory education programs for healthcare professionals regarding the prevalence of misuse of PPIs in Pakistan and how they are contributing to it, leading to better use of PPIs.
Recommendations
The current study highlighted that a sizable portion of individuals in the study population lack awareness regarding the potential side effects of PPI usage. Healthcare professionals are advised to explore patients’ beliefs concerning the perceived absence of short-term PPI side effects and counsel them properly regarding the risks and benefits of PPI use. They should also review PPI prescriptions regularly and take measures when there is no indication to reduce the treatment cost. It is recommended that policymakers encourage and organize campaigns promoting the rational use of PPIs and create educational materials such as brochures, posters, and videos that explain what PPIs are, how they work, and what their side effects are. Public health authorities should also provide guidelines to prescribers to ensure rational prescribing.
Abbreviations
Footnotes
Acknowledgments
We would like to acknowledge the community pharmacies in the vicinity of the University of Veterinary and Animal Sciences for their support in data collection.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
The study protocol was approved by the Institutional Review Committee for Biomedical Research University of Veterinary and Animal Sciences, Lahore, Pakistan.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Informed Consent
Written informed consent was taken from the respondents for their participation in this study.
