Abstract
Introduction:
Hidradenitis Suppurativa (HS) is a chronic and relapsing acneiform inflammation of the skin, apocrine glands and subcutaneous tissues. It is common among women of the reproductive age group. It is a chronic debilitating condition which may significantly affect the quality of life based on the severity of disease. HS during pregnancy requires additional care and treatment may be challenging in severe or refractory cases.
Case:
We report a case of HS during pregnancy who presented at term with painful skin lesions.
Discussion:
Patients with HS are found to have higher chances of adverse maternofoetal outcomes when compared to general population. In cases where there are worsening symptoms, treatment becomes a challenge. A postpartum flare of symptoms may also be debilitating and affect the quality of life in patients.
Conclusion:
There is a paucity of data for optimal management of HS in pregnancy especially mode of delivery. There is a need for guidelines for the management of skin conditions during pregnancy and its implications.
Introduction
Hidradenitis suppurativa (HS) is a chronic and relapsing acneiform inflammation of the skin, apocrine glands and subcutaneous tissues. It is common among women of the reproductive age group.[1] It is also called Fox den disease/Verneuils’s disease/Ectopic acne/Acne inversa/Pyoderma fistulans sinifica. Intertriginous areas like axilla, groin, breasts are the most commonly affected areas by this condition and are typically characterised by painful inflamed lesions, papules, nodules, abscesses, scars and sinuses which may or may not be foul smelling. Pathogenesis of these lesions is still not clearly understood. Smoking, obesity and presence of metabolic syndrome are a few factors frequently associated with HS.[2,3] The severity of lesions is directly associated with the severity of obesity and quantity of cigarette smoking.[4] Lesions are notoriously difficult to treat and chronic relapsing lesions may sometimes be deep-seated which may significantly affect the quality of life of patients. Patients suffering from HS are also associated with an increased risk of cancer of any kind when compared to general population specific cancers associated with HS are Marjolin’s cancer of chronic lesions of HS over buttocks, hepatocellular cancer, and buccal cancer.[5] HS also has a genetic component where one-third of the cases show an autosomal dominant pattern of Mendelian inheritance.[6] Etiopathogenesis of HS is still unclear however, there is atrophy of the sebaceous gland and inflammation and hyperkeratosis of pilosebaceous unit along with hair follicle destruction and granuloma formation. Hurley staging is used to assess the severity of condition and helps in assessing the treatment.
Case Report
We report a case of a 23-year-old primigravida who presented to us at 37 weeks and for safe confinement. Her pre-pregnancy weight was 65 kgs and her body mass index was 30.9 kg/m2. On general and abdominal examination, she was incidentally found to have multiple deep-seated skin lesions over her groin and axilla [Hurley Stage 1 lesions as shown in Figures 1, 2 (axillary lesions) and 3–5 (groin lesions)]. She had painful nodules of various sizes. The uterus was term-sized and relaxed. Foetal heart rate was 156 beats/min, normal and regular. Admission Non-Stress Test (NST) was reassuring. On probing, she gave a history of similar lesions in the past and this was the third episode. She was conservatively managed with antibiotics and lesions regressed. Dermatology consultation was done at the time of admission and she was diagnosed with HS. She was advised to conservative management for pain with analgesics and antibiotics. High vaginal swab was negative. Patient had premature rupture of membrane (PROM) and underwent Emergency Lower Segment Caesarean Section (LSCS) in view of foetal distress. Liquor was clear and adequate. The baby extracted and cried soon after birth. There were no abnormal intraoperative findings. Post-operative period was uneventful and she was discharged on postoperative day 4. She was followed up 2, 4 and 8 weeks later and her complaints were reduced. Lesions had regressed and she has no pain at present.
Multiple Healed Lesions Over Axilla (Produced After Taking Consent from Patient)
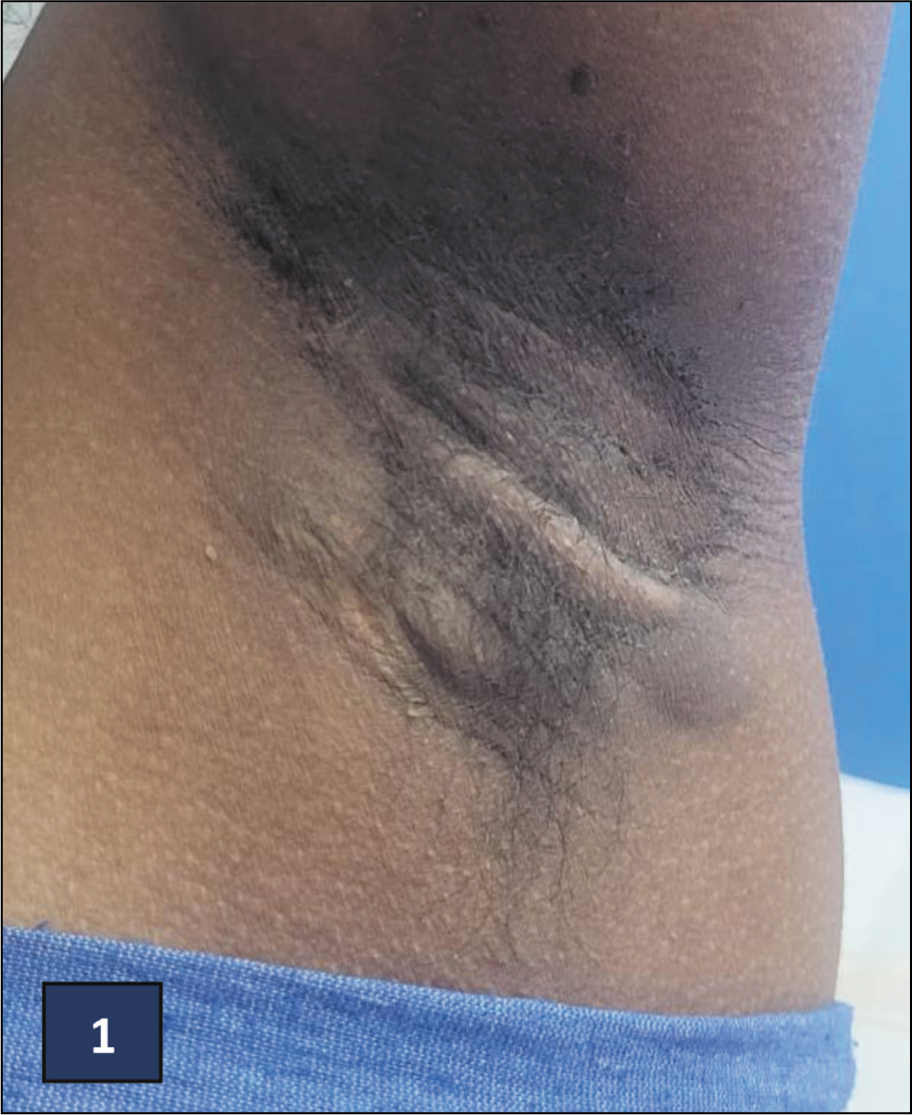
Multiple Healed Lesions Over Axilla (Produced After Taking Consent from Patient)
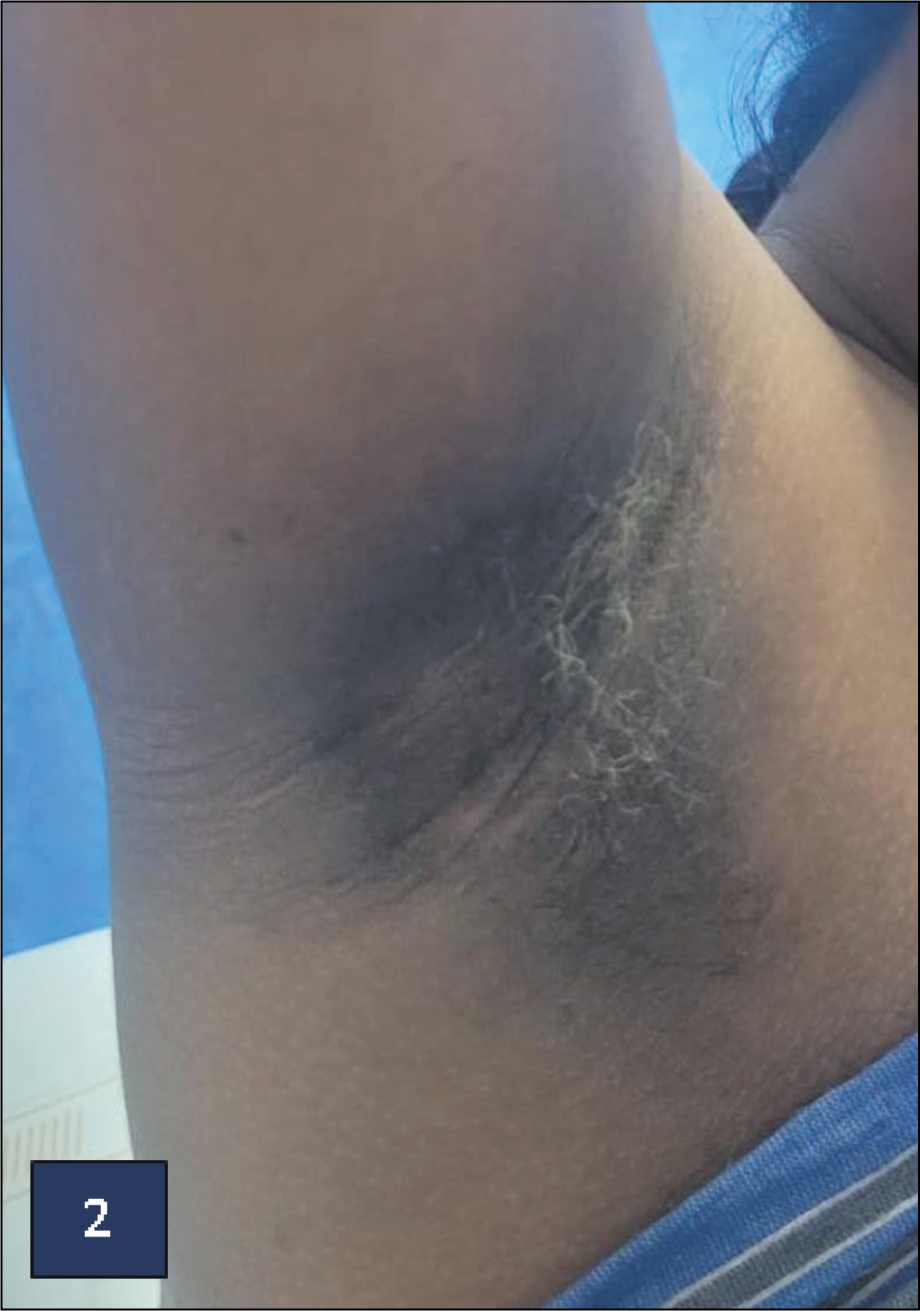
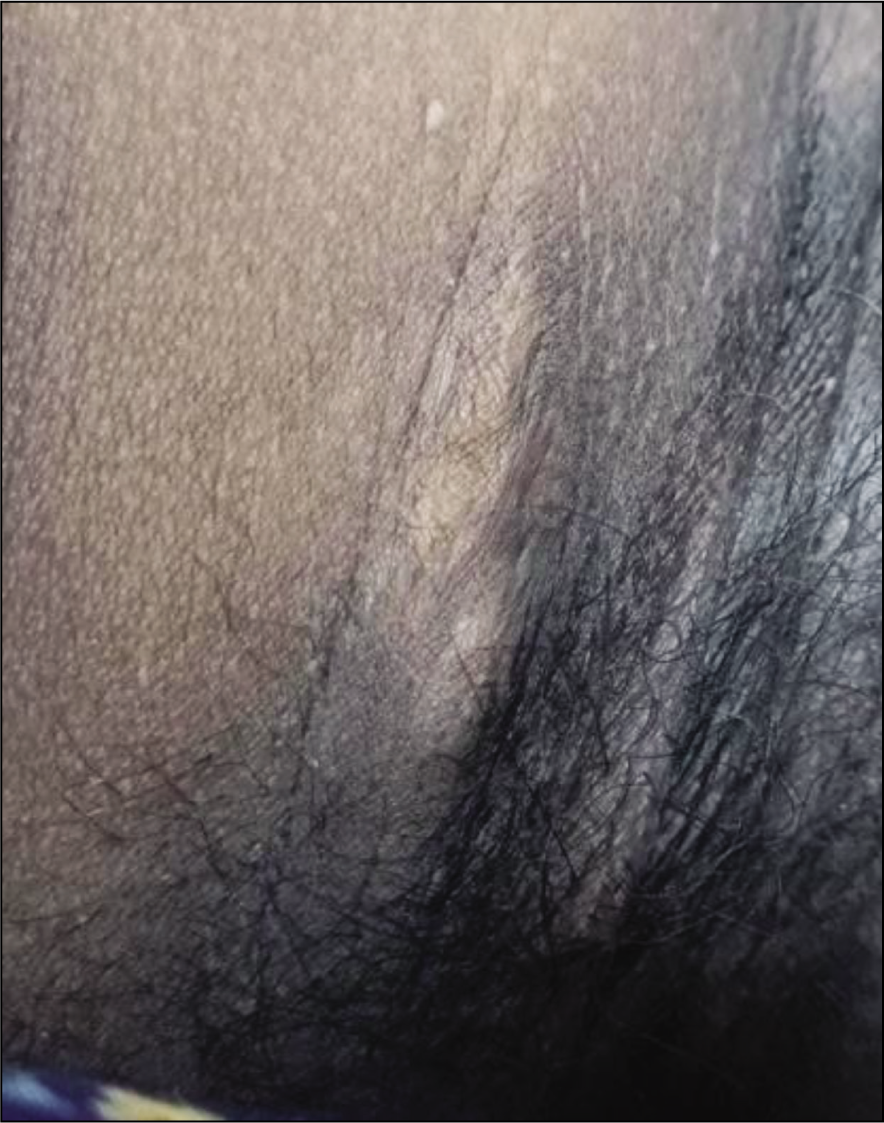
Multiple Deep Seated Skin Lesions Over Her Groin (Produced After Taking Consent from Patient)
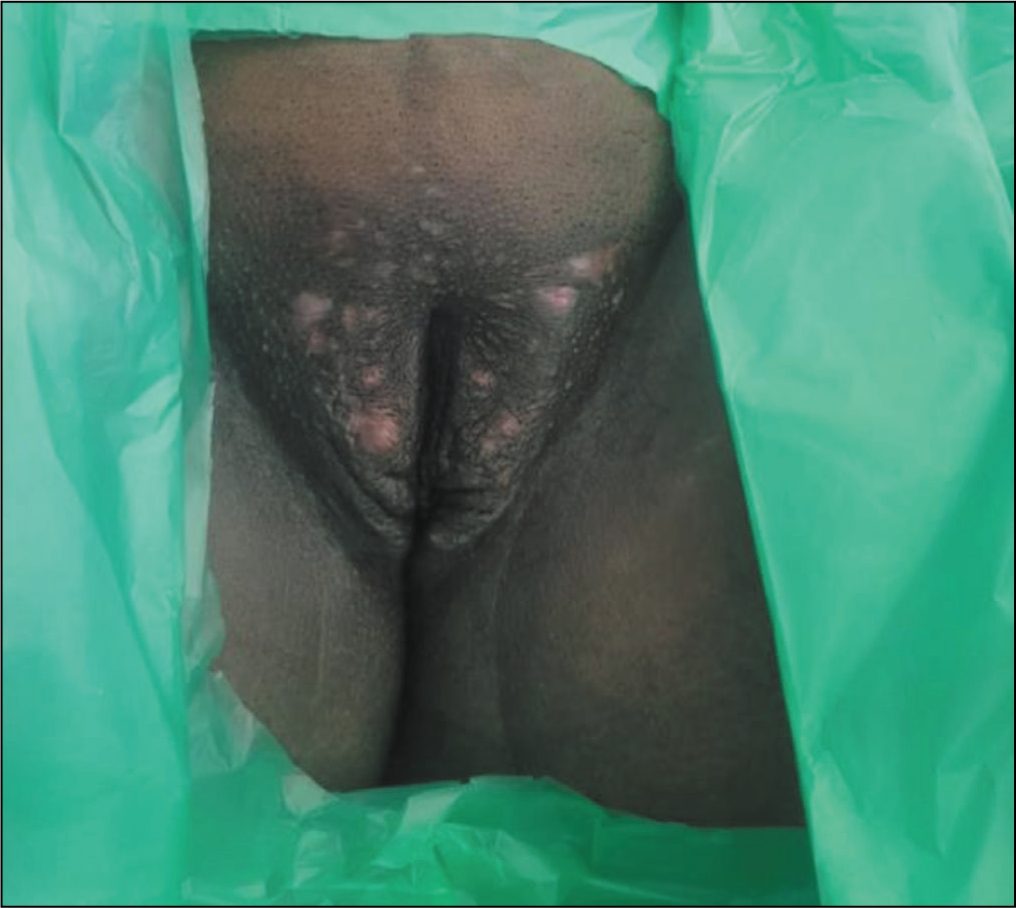
Multiple Deep Seated Skin Lesions Over Her Groin (Produced After Taking Consent from Patient)
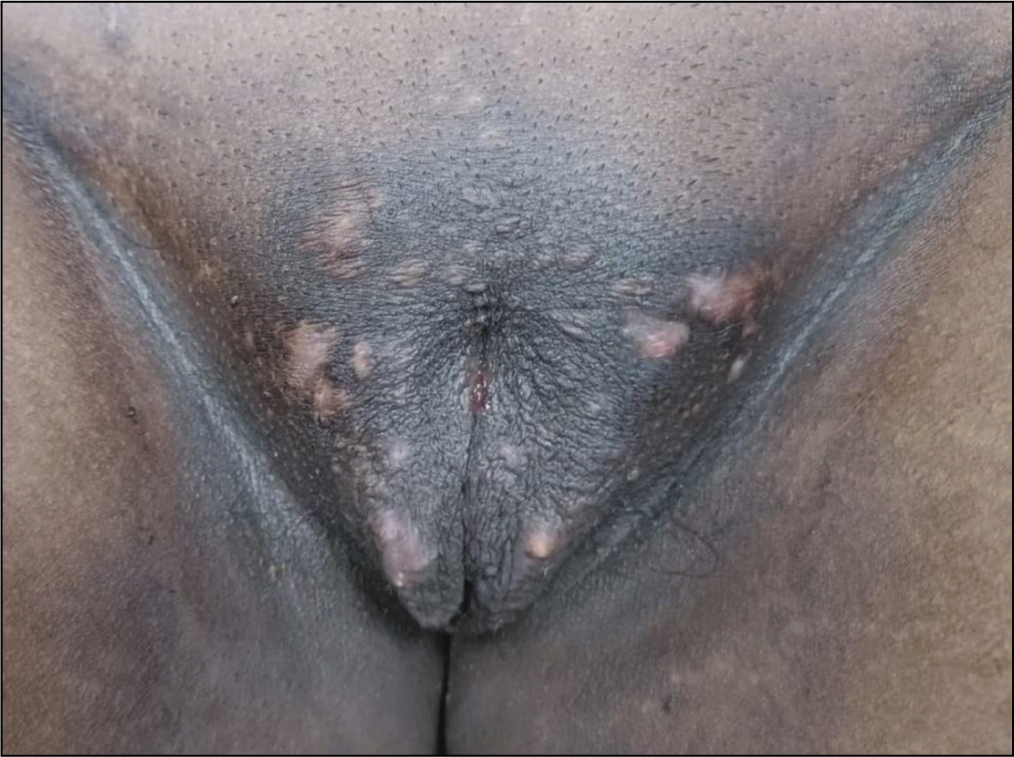
Multiple Deep Seated Skin Lesions Over the Groin (Produced After Taking Consent from the Patient)
Discussion
HS typically is seen among women in their reproductive age group. Not only pregnancy but also post-partum period may remain unchanged or present with aggravation or relief of the symptoms in patients suffering from HS.[7] These lesions typically affect the groin and axilla like in our case. The active lesions are usually multiple, tender and may range from nodules, pustules, and abscess of various sizes and old lesions may be associated with scarring and sinus/fistula formation.
Patients with HS are found to have higher chances of adverse maternofoetal outcomes when compared to general population.[8] It was studied that patients suffering from HS had a higher risk of spontaneous abortions, preterm birth, gestational diabetes, gestational hypertension/pre-eclampsia, and caesarean section. Chronic inflammation may have been one of the causative factors for gestational diabetes.[9] Ascending infection or inflammation/infection of genital lesions may have contributed to higher rates of spontaneous abortions and elective sections.[7,10]
The severity of the condition is usually assessed by Hurley staging and treatment can be planned based on the staging. Stage 3 is the most debilitating and requires a multimodal treatment approach or systemic therapy. In severe, refractory cases, surgery may be required. However, as in our case, Stage 1 can be managed by topical antibiotic clindamycin 1% treatment or intralesional triamcinolone (steroids). There are limited studies on HS management in pregnancy with respect to optimal mode of delivery and complications. It is advisable for clinicians to be aware of safer medications during pregnancy and lactation among HS patients.[11]
Conclusion
HS during pregnancy may usually be unchanged. However, in cases where there are worsening symptoms, treatment becomes a challenge. A postpartum flare of symptoms may also be debilitating and affect the quality of life in patients. There is a paucity of data for optimal management of HS in pregnancy especially mode of delivery. There is a need for guidelines for the management of skin conditions during pregnancy and its implications.
Footnotes
Acknowledgements
We especially thank our patient for her consent for publication.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
Institutional Ethical Committee Approval Number
Ethical permission was not applicable for this article, as this is a case report of a patient who have given written consent for publication.
Informed consent
Informed consent for publication obtained from patient.
Credit author statement
All the authors were involved in conception, literature search, analysis of data and drafting the manuscript.
Concept of the article was given by VS and KG.
Design of the article was by OMJ, SV and KG.
Draft writing by OMJ.
Critical revision and final approval of version to be published was done by SV.
Data availability
This study did not involve the generation, analysis, or use of any data sets, and therefore, data sharing is not applicable.
Use of artificial intelligence
The use of artificial intelligence is not relevant to this article, as it does not involve AI technologies or methodologies in its analysis or conclusions.
