Abstract
Background:
Bilateral acute parotitis is commonly associated with conditions like mumps and inflammation. However, its occurrence immediately after caesarean delivery under spinal anesthesia is extremely rare.
Case report:
A 34-year-old primigravida with no significant past medical history developed sudden, painless bilateral parotid gland swelling following a caesarean section performed under spinal anesthesia. She was successfully treated with hydration, steroids, and antihistamines, resulting in complete resolution of symptoms within 24 hours without any complications.
Conclusion:
This case highlights an unusual presentation of bilateral acute parotitis following caesarean section. Although rare, it should be considered a potential complication. Prompt medical management with hydration, steroids, and antihistamines can lead to rapid recovery.
Introduction
Inflammation of the parotid gland, a significant salivary gland, can arise from local or systemic pathology, with infectious or inflammatory conditions being the most common culprits.[1,2] Less common triggers include trauma, surgical procedures such as carotid endarterectomy, oral neoplasms, immunosuppression, sialolithiasis, medication side effects, radiation exposure, osteomyelitis, Lemierre syndrome, sepsis, organ failure, and facial paralysis.[1,2]
Recently, cases of acute parotitis have been reported following general anaesthesia, with factors such as increased positive airway pressure, prone positioning, obesity, prolonged surgical duration, and the use of anticholinergic drugs during mask ventilation being considered potential causes.[3,4] In severe instances, airway obstruction may necessitate emergency intubation or tracheostomy.[5]
The occurrence of acute bilateral painless parotitis after caesarean delivery under spinal anaesthesia is uncommon, and its management remains poorly understood.[6-8] In this context, we present the case of a 34-year-old primigravida with no prior medical history, who developed acute painless bilateral parotitis shortly after undergoing caesarean delivery. This report elucidates the clinical presentation, management strategies, and successful resolution achieved within a remarkably brief timeframe of 24 hours following the initial surgical intervention.
Case Report
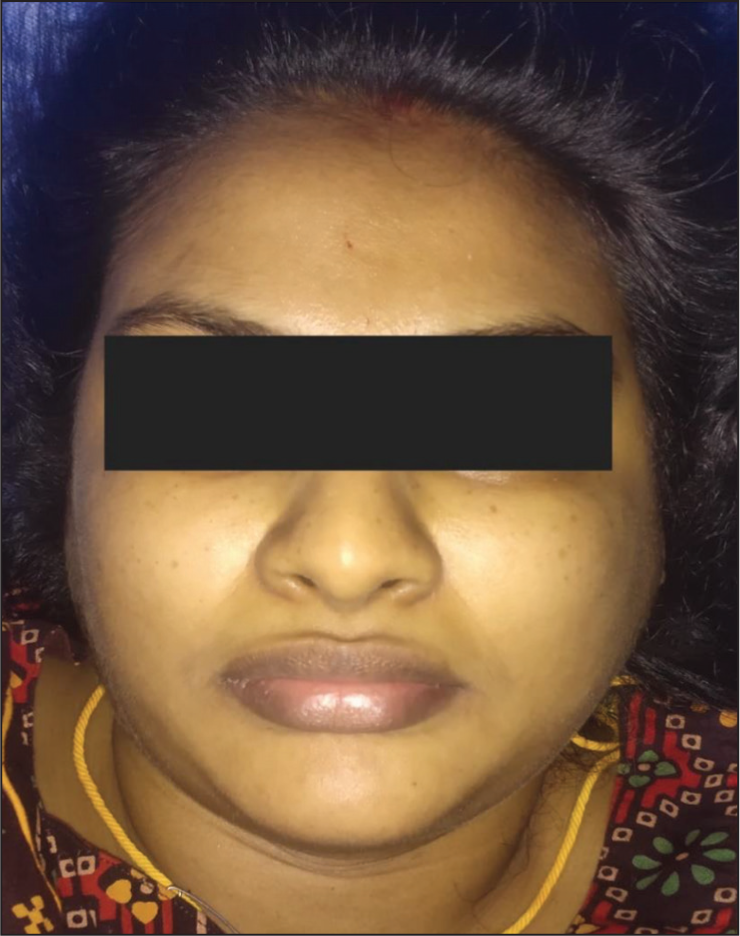
A 34-year-old primigravida, at 36 weeks of pregnancy, experienced painless bilateral cheek swelling five hours post-caesarean delivery under spinal anaesthesia. The caesarean section was performed for severe intrauterine growth restriction of the fetus. Notably, the patient had no history of chronic medical conditions or prior mumps infection. She presented without fever or respiratory symptoms. Clinical examination revealed bilateral painless parotid swelling, with the left side exhibiting greater enlargement than the right (Panel A: frontal view; Panel B: lateral view). Postoperatively, her complete blood count and biochemical parameters, including serum amylase, remained within normal ranges. Additionally, serology for mumps infection showed negative IgM antibody levels, confirming the absence of recent mumps infection.
Frontal view displaying asymmetrical bilateral parotid swelling, with the left side notably larger than the right
Profile (side) view demonstrating the enlargement of the parotid gland
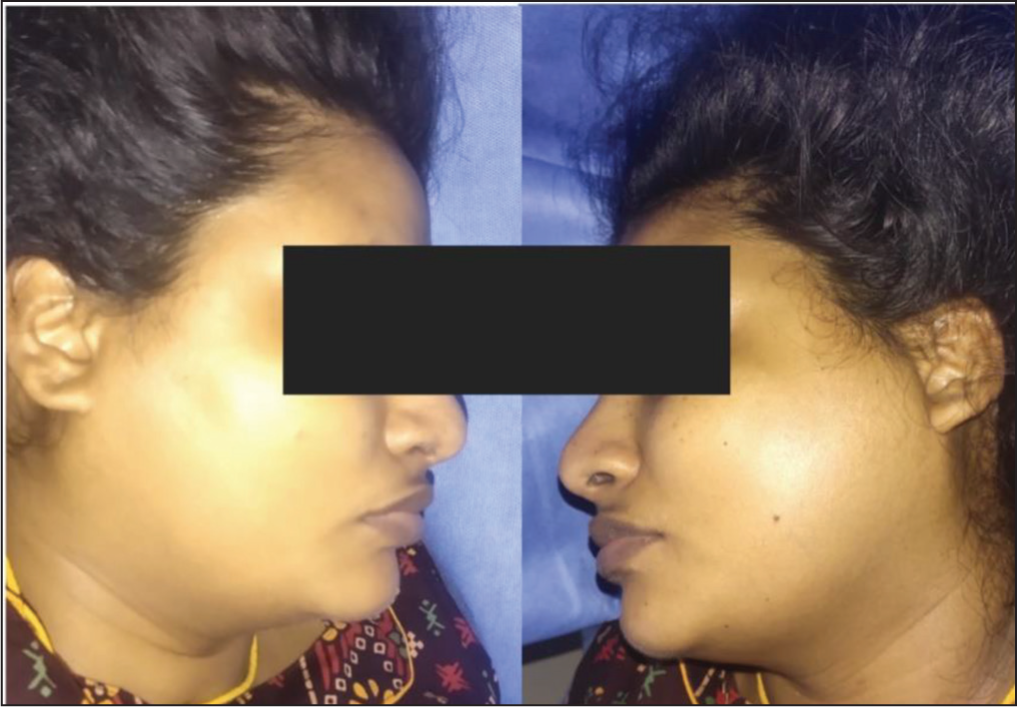
Based on clinical assessment, a diagnosis of acute parotitis was established, with imaging deemed unnecessary due to the absence of pain. Treatment included head elevation and intravenous fluids administered at a rate of 100 ml/hr for hydration. The pharmacological intervention included intravenous dexamethasone (8 mg), paracetamol (1000 mg), and intramuscular pheniramine maleate (45.5 mg). Remarkably, the swelling resolved within 24 hours post-surgery, and the patient was discharged home on the third postoperative day, free from cheek swelling.
Follow-up image taken three weeks later, depicting the absence of parotid swelling, indicating successful resolution of the condition
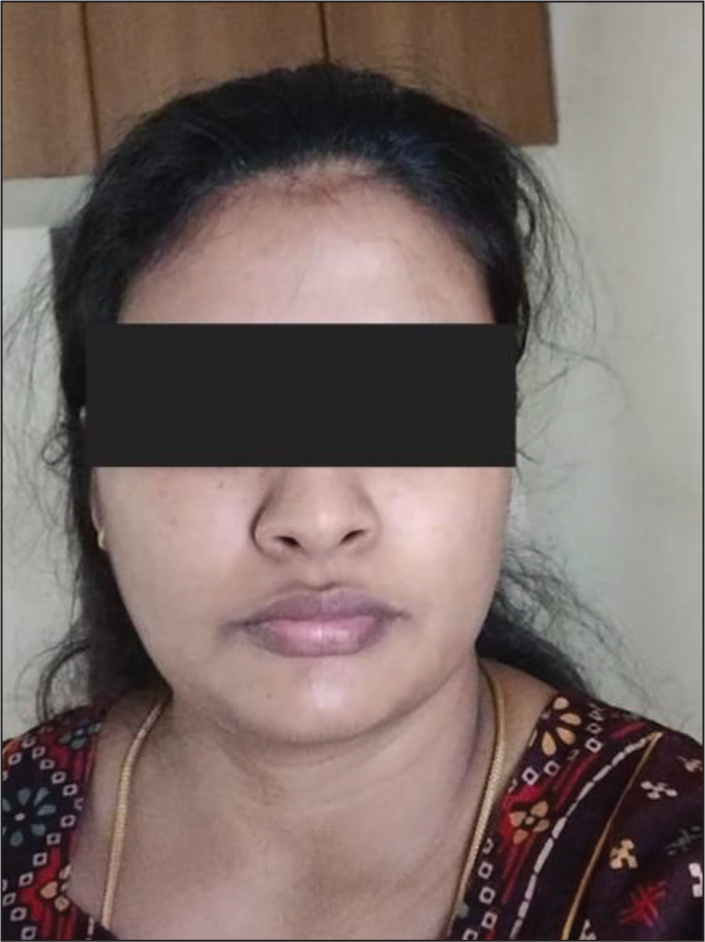
Discussion
Acute parotitis following caesarean delivery under spinal anaesthesia is a rare occurrence. Apart from the common infectious and inflammatory conditions, certain medical treatments, such as L-asparaginase, phenylbutazone, and clozapine, which induce ductal stenosis, may contribute to parotitis. Recently, ephedrine has been implicated in causing bilateral acute parotitis following delivery under spinal anaesthesia, particularly when administered intravenously in larger doses ranging from 48 to 52 mg.[6] However, in our case, only 20 mg of ephedrine was administered to address transient spinal-induced hypotension, and the patient responded well shortly after the injection. The potential mechanism behind the development of bilateral acute parotitis following ephedrine administration involves its beta-stimulating effect on the parotid glands. Sympathetic nerve-mediated glandular stimulation can decrease the secretion of total salivary protein and α-amylase, leading to reduced unstimulated saliva flow from the whole gland or specifically from the parotid gland, thereby resulting in acute bilateral parotitis.[9]
This condition may also manifest with difficulties in swallowing and speaking. Despite the relatively small dose of ephedrine administered, our patient experienced bilateral acute parotitis, which resolved within 24 hours post-surgery without any respiratory complications.
The exact mechanism underlying the occurrence of postoperative acute painless parotitis, a rare complication following Caesarean section under spinal anaesthesia, remains poorly understood. This complication carries the risk of airway obstruction, potentially leading to respiratory distress, despite cases to date reporting successful management with medical support and close monitoring due to its self-limiting nature. It’s important to recognise the possibility of recurrence under similar conditions.
Imaging is typically unnecessary for evaluating parotitis. However, ultrasonography can be beneficial for confirming sialolithiasis, identifying abscesses, distinguishing between solid and cystic masses within the gland, and detecting hypoechoic areas commonly associated with punctate sialectasis. In rare instances, plain radiography or computed tomography (CT), with or without contrast, may confirm sialolithiasis or reveal multiple parotid calcifications in chronic parotitis. Magnetic resonance imaging (MRI) is particularly valuable for distinguishing between chronic parotitis and neoplastic changes within the gland. In our case, imaging was not required as there were no accompanying symptoms, and the swelling resolved following medication administration.
Today, the occurrence of postoperative parotitis is infrequent due to the widespread utilisation of antibiotics, meticulous oral hygiene practices, and adequate perioperative hydration, ensuring a balanced electrolyte status. This rare occurrence typically resolves spontaneously, with supportive measures such as head elevation, hydration, and administration of steroids and anti-inflammatory medications. Given the sensitivity of pregnant patients, close monitoring of hydration status postoperatively is advisable. Remarkably, in our case, this complication self-resolved within 24 hours, a notably shorter duration compared to previously reported cases, highlighting the efficacy of tailored hydration adjustments and anti-inflammatory therapy.
Conclusions
In conclusion, the case of acute painless bilateral parotitis following caesarean delivery under spinal anaesthesia underscores the importance of vigilance and tailored management in the peripartum period. While this complication is rare, its swift resolution within 24 hours, facilitated by meticulous hydration adjustments and anti-inflammatory therapy, highlights the significance of individualised care. Moreover, this case serves as a reminder of the complexities inherent in obstetric anaesthesia and the need for continued research and vigilance to optimise outcomes for both mothers and infants.
Footnotes
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
Ethical approval
Ethical approval is not required because this is a case report.
Patient consent
The patient gave consent to publication of the image for educational purposes.
Institutional ethical committee approval number
Ethical approval from the Ethical Committed Board of OHRC. No 10/2024
Informed consent
The patients and/or their families were informed that data from the research would be submitted for publication, and they consented.
Credit author statement
KT: written, reviewed and analyzed the data.
PR: reviewed the article.
JTJJ: revised the article, concepts and methodology.
Data availability
The data is available on request and from the patient's approval.
Use of artificial intelligence
AI is not used in this article.
