Abstract
Introduction:
Transthoracic echocardiography is a non-invasive diagnostic test used to assess the structure and function of the heart in real-time. An examination of the heart's electrical activity is done non-invasively through electrocardiography (ECG). The ECG is primarily used during an echocardiography procedure to assess the heart's rhythm and to synchronise the cardiac cycles with echocardiographic image acquisition; this enables the echocardiographer to acquire images at specific phases of the cardiac cycle. A handheld echocardiograph is not connected to the electrocardiogram, which is a clinical limitation for the point-of-care ultrasound procedure. The objectives of this review are to highlight the reasons why 3-lead electrocardiography should be incorporated into pocket-sized handheld echocardiographs to support clinicians in conducting and reporting complete cardiac investigations.
Methods:
An in-depth search was made on the PubMed database to find experimental and review studies that assessed the importance of 3-lead ECG in the acquisition of hand-held echocardiographic data. Four related studies were selected for this review.
Results:
The study found that integrating cardiac point-of-care ultrasound into primary healthcare practices such as family medicine or general practitioners’ practices and training clinicians to accurately perform the procedure can expedite cardiovascular disease diagnosis and treatment in critical and non-critical scenarios. Secondly, recent hand-held cardiac ultrasound examination outcomes are as accurate and precise as standard transthoracic echocardiography and cardiac magnetic resonance imaging.
Background
Hand-held transthoracic echocardiography is a non-invasive diagnostic test used to assess the functional anatomy of the heart in real time.[1,2] It uses ultrasound waves to create images of the heart, providing valuable information about its size, and structure. It allows clinicians to visualise the heart’s chambers, valves, and blood flow patterns, enabling them to identify abnormalities or potential issues.[1,2] Through echocardiography, clinicians can diagnose conditions such as valvular disease, congenital heart defects, heart failure, and abnormal heart rhythms.[1] A 3-lead electrocardiogram (ECG) is used to observe the electrical activity of the heart.[3] Three ECG electrodes are used during a comprehensive transthoracic echocardiography, the left arm (LA), the right arm (RA), and the left foot (LL).[1,2] Within the rib cage frame, the RA electrode is positioned beneath the right clavicle’s mid-clavicular line, while the LA electrode is positioned beneath the left clavicle’s mid-clavicular line, and the lower left abdomen is where the LL electrode is positioned close to the rib cage frame.[1,2]
Hand-held echocardiographs are commonly used for focused or point-of-care scanning. However, during hand-held echocardiography, the ECG is not utilised, which is a limitation of the procedure.[4] The objectives of this mini-review are to highlight the reasons why 3-lead ECG should be incorporated into pocket-sized handheld echocardiographs to support cardiologists, internists, emergency medicine specialists, and other clinicians in conducting and reporting complete cardiac investigations.
Method
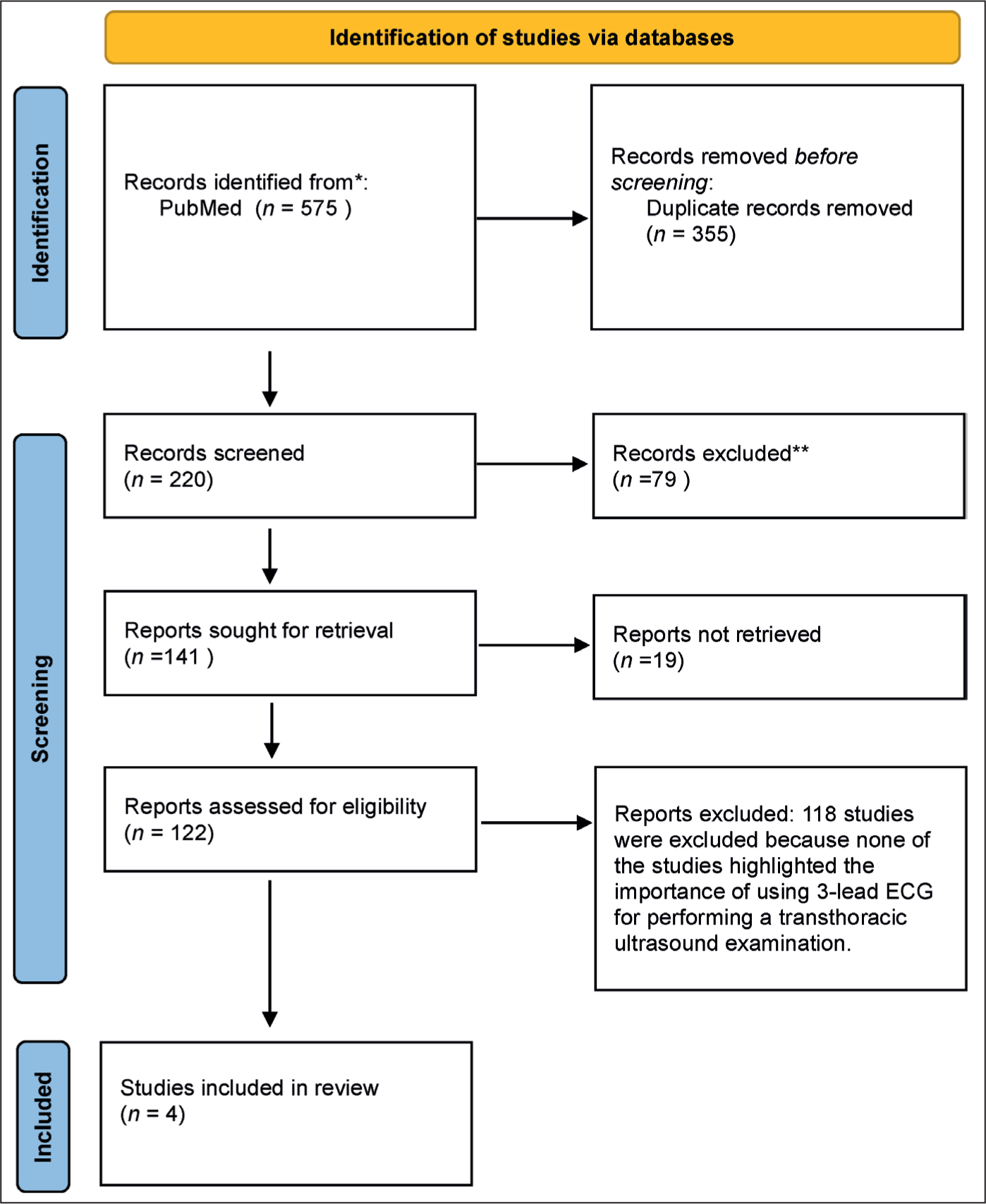
An in-depth search was made on the PubMed database to find experimental and review studies that assessed the importance of 3-lead ECG in the acquisition of hand-held echocardiographic data. Medical Subject Headings terms were used to search the PubMed database. The key terms were echocardiography (AND ECG) AND transthoracic examination. A total of 575 results came out from January 1986 to February 2024 (Figure 1). After utilising Zotero to manage the selection of studies and eliminate duplicates, 220 articles remained. However, none of the studies have evaluated the precise focus of this article, making this the first article to highlight the importance of using 3-lead ECG for performing a hand-held transthoracic echocardiographic examination in a clinical setting. However, four closely related studies[1-4] were selected and summarised.
PRISMA flow diagram for inclusion of studies that highlighted the importance of using 3-lead ECG for performing a transthoracic echocardiographic examination in a clinical setting.[5]
Selection Criteria
The study selection and data extraction were independently performed by the author. Initial evaluation was based on screening of titles and abstracts. The second round of evaluation was based on a full-text review. Studies that evaluated the role of ECG during transthoracic echocardiography or cardiac point-of-care ultrasound procedures on adult patients were included. The study was required to report at least one of the following: the importance of 3-lead electrocardiographs during cardiac point-of-care ultrasound or the benefits of ECG tracing during a routine transthoracic echocardiography examination. Studies that are excluded are case reports, comments, and animal studies.
The Significance of Adding 3-Lead Electrocardiographs to Portable, Handheld Echocardiographs for Point-of-Care Cardiac Evaluation
The ECG should be performed simultaneously with echocardiography to provide synchronisation between the electrical events and the images captured by the echocardiogram.[1,2] This synchronisation helps in interpreting the echocardiographic findings and understanding the relationship between the electrical activity and the structural and functional aspects of the heart. Heart blocks, atrial flutter, ventricular arrhythmias, and atrial fibrillation can be detected by the ECG, which is typically used to assess the heart’s rhythm during an echocardiographic examination.[1,2] The ECG tracing acts as a guide in echo measurements; for example, the ventricular end diastole is noted at the start of the ECG QRS complex, and the ventricular end-systole is characterised at the end of the T-wave.[1] A large pericardial effusion can be confirmed in the ECG because it can be responsible for the electrical alternans on the ECG.[2] In our daily tasks as clinicians, The ECG tracings are essential for the acquisition of appropriately timed loops and for the identification of specific time points within the cardiac cycle during echocardiography, helping to analyse and carry out accurate measurements.[1] The QRS complex on the ECG is used in echocardiography to separate image series into cardiac cycles for playback and storage.[1] The ECG rhythm acts as a guide for left ventricular diastolic function assessment.[1] During tissue Doppler imaging LV diastology assessment, the E wave prime is measured before the P-wave and it corresponds to early rapid filling, the A wave prime is measured after the P-wave and it corresponds to atrial contraction, and the S-wave prime is measured after the QRS interval and it corresponds to left ventricular systolic velocity.[1] Hence, for point-of-care cardiac examination, combining portable handheld echocardiographs with 3-lead electrocardiographs will increase diagnostic efficiency.
Discussion
Very few studies have shown that the incorporation of portable handheld echocardiographic devices with ECG capabilities can significantly improve diagnostic accuracy. Panoulas et al.[6] found that the combination of handheld ultrasound devices with traditional diagnostic methods substantially increased both specificity and sensitivity in diagnosing conditions like left ventricular systolic dysfunction. This suggests that integrating ECG data into handheld devices allows for a more comprehensive assessment of cardiac function, particularly in settings where traditional ECG monitoring may not be feasible. Moreover, the study conducted by Mujtaba et al.[7] emphasises that point-of-care ultrasound combined with 3-lead ECG monitoring enhances the sensitivity of traditional cardiac examinations, which frequently overlook critical signs of cardiac dysfunction. This integration allows clinicians to achieve a holistic view of a patient’s cardiac health, enabling the detection of abnormalities that may not be apparent during physical examinations alone. The European Association of Cardiovascular Imaging[8] recognises the potential of handheld ultrasound devices to improve patient management, particularly when integrated with ECG monitoring. The provision of real-time cardiac data alongside ultrasound imaging enables healthcare providers to make informed decisions regarding patient care. The recommendations emphasise that appropriate training and guidelines are essential for optimising the benefits of this technology. Furthermore, Jeon et al.[9] discussed a novel cardiac data acquisition method that combines ECG with Seismocardiography data. This approach significantly enhances the capability of portable devices to monitor cardiac activities and deliver early warnings for conditions that could lead to sudden cardiac events. The high accuracy of this proposed system demonstrates the viability of integrating ECG monitoring into handheld devices, potentially revolutionising cardiac care by enabling continuous and comprehensive patient monitoring. The use of handheld ECGs for self-monitoring in patients’ post-cardiac surgery highlights the feasibility and acceptability of such technologies.[10] The integration of ECG into handheld ultrasound devices will not only streamline the diagnostic process but also enhance training and competency among healthcare providers.
The standardisation of ultrasound techniques, coupled with ECG monitoring, is crucial for ensuring that all patients receive high-quality cardiac assessments during routine examinations.[11] This training aspect is vital, as it prepares medical students and junior doctors to perform echocardiography with ECG integration, advocating for a paradigm shift in cardiac evaluations. Despite the promising findings, several knowledge gaps remain. For instance, the long-term outcomes of integrating ECG monitoring into handheld devices for various patient populations are yet to be fully explored. Future research should focus on large-scale longitudinal studies to assess the impact of such integrations on patient outcomes across diverse demographics. Additionally, there is a need for research into the cost-effectiveness and practical implementation of these technologies in various healthcare settings. Investigating barriers to adoption, such as technological challenges and training requirements, will also be essential for widespread integration. Moreover, exploring the potential of artificial intelligence in conjunction with integrated ECG and ultrasound data could lead to innovative diagnostic tools that enhance risk stratification and treatment planning in cardiology. The integration of 3-lead ECGs into portable handheld cardiac ultrasound devices holds significant promise for enhancing diagnostic accuracy, improving patient engagement, and streamlining clinical workflows. The current body of literature highlights the advantages of this integration, yet further exploration is necessary to address existing knowledge gaps and optimise the implementation of these technologies in clinical practice. Future studies should aim to elucidate the long-term impacts on patient outcomes and explore innovative applications that leverage the combined capabilities of ECG and ultrasound in cardiac care.
Limitations of Current Cardiac Handheld Ultrasound Devices
In recent years, handheld ultrasound devices have emerged as a revolutionary tool in cardiology, enhancing accessibility and facilitating rapid bedside assessments. However, despite their advantages, these devices have notable limitations that affect their diagnostic and clinical utility. One of the primary criticisms of handheld ultrasound devices pertains to imaging quality. While advancements in technology have improved resolution, traditionally, handheld devices cannot achieve the same diagnostic precision as standard echocardiography systems.[12] The limited sample volume and reduced Doppler capabilities can compromise the ability to assess complex cardiac anatomy and haemodynamics effectively.[13,14] Another significant limitation of handheld ultrasound devices is their high degree of operator dependency. The accuracy and interpretation of ultrasound images rely heavily on the user’s skill and experience. Several studies have highlighted that inexperienced operators may misinterpret findings, leading to potential misdiagnosis.[15,16] While training programs aim to improve operator proficiency, the variability in training quality, along with individual differences in skill acquisition, presents ongoing challenges. Most handheld ultrasound devices do not integrate robust protocols and guidelines for cardiac assessment, which can lead to inconsistencies in evaluation and reporting. Established echocardiographic protocols provide a systematic approach to diagnosing various cardiac conditions, and deviations from these can hinder accurate and comprehensive assessments.[16] The absence of standardised approaches in handheld devices may contribute to variability in practice and reduced diagnostic reliability. Handheld ultrasound devices often have limited data storage capabilities and may lack robust data sharing and connectivity features. These limitations complicate the process of archiving, analysing, and retrieving clinical information for longitudinal patient management.[17] Proper documentation and storage of ultrasound findings is critical for follow-up care and research purposes, nevertheless, some hand-held cardiac ultrasound devices do not facilitate adequate documentation due to lesser memory storage capacity compared to standard ultrasound machines.[18-21]
Conclusion
Cardiac point-of-care ultrasound has emerged as a transformative tool in critical settings such as emergency departments and remote healthcare environments such as family medicine practices or general practitioners’ practices. Its applications include rapid assessment of cardiac function, identification of pericardial effusion, assessment of regional wall motion abnormalities, evaluation of heart failure, and guiding procedures like central line placement. Most recent cardiac ultrasound devices have been shown to be comparable to standard transthoracic echocardiography and cardiac magnetic resonance in terms of accuracy and precision.[21] In emergency departments, cardiac point-of-care ultrasound helps in the swift diagnosis of conditions such as cardiac tamponade, myocardial infarction, or shock states, enabling timely interventions that can significantly influence patient outcomes. For example, clinicians can quickly assess left ventricular function in patients with dyspnoea, thereby facilitating appropriate management strategies, be it diuretics for heart failure or initiation of resuscitation protocols for shock. The broader impact of the use of cardiac handheld ultrasound devices in healthcare is substantial. By allowing for expedited diagnosis and treatment in critical scenarios, it enhances patient safety and optimises resource utilisation. It empowers clinicians at all levels of care, fosters interdisciplinary collaboration, and helps bridge the gap in medical accessibility. Integrating cardiac point-of-care ultrasound into primary healthcare practices such as family medicine practices or general practitioners’ practices can lead to improved overall healthcare outcomes, enhance patient satisfaction, and streamline healthcare costs, contributing to a more efficient and responsive healthcare system.
A 3-lead ECG is primarily used during a comprehensive echocardiographic exam to assess the heart’s rhythm because abnormalities such as atrial fibrillation, atrial flutter, ventricular arrhythmias, bundle branch block, and atrioventricular heart blocks can be identified through ECG tracing. Second, a 3-lead ECG is used to synchronise the cardiac cycles with echocardiographic image acquisition. This enables clinicians to acquire images at specific phases of the cardiac cycle. This synchronisation allows for accurate assessment of cardiac dimensions, function, and haemodynamics by ensuring images are captured at the appropriate time loops. Incorporating a 3-lead ECG into hand-held echocardiograms would enhance diagnostic capabilities. Because echocardiograms provide information about the structure and function of the heart, while ECGs provide valuable insights into the electrical activity of the heart, together, these two diagnostic tools provide a more complete picture of a patient’s cardiac condition. Therefore, medical device manufacturers should consider integrating and producing new hand-held echocardiographs with configured 3-lead electrocardiographs that are artificial intelligence-enhanced to assist clinicians in precise point-of-care cardiac assessments.
Footnotes
Declaration of conflicting interests
The author declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The author received no financial support for the research, authorship and/or publication of this article.
Institutional ethical committee approval number
Approval from an Institutional Ethical Committee was not applicable for this article, as it is a review article compiled from various research studies and does not involve direct patient data or interventions.
Informed consent
Informed consent was not applicable for this article, as it is a review article based on previously published research and does not involve direct participation of patients or collection of primary data.
Credit author statement
Conception and design of the work, analysis, and review.
Data availability
Data availability is not applicable for this article, as it is a review article that synthesizes information from existing research and does not involve the generation or analysis of new datasets.
Use of artificial intelligence
The use of artificial intelligence is not relevant to this article, as it does not involve AI technologies or methodologies in its analysis or conclusions.
