Abstract
Background and Aims:
Wasp stings often result in vascular problems and local irritation. Rarely neurological difficulties result from a delayed immune response, which causes acute inflammatory demyelinating polyradiculopathy, stroke and Parkinson’s disease.
Patient’s Concern:
Here we are describing a young male, who presented to us with ascending paralysis a few days after being stung by multiple wasps. The patient did not have any infection or recent vaccination. Nerve conduction velocity (NCV) suggested increased latencies in peripheral nerves. Hence, a temporality between Guillain–Barré syndrome (GBS) and the wasp sting was hypothesised.
Intervention:
After establishing a diagnosis, the patient received standard treatment for acute inflammatory demyelinating polyneuropathy (AIDP). Intravenous immunoglobulins were given over 5 days in divided doses. The patient had gross improvement in the weakness by day 7 and fully recovered in 2 months.
Conclusion:
This case study highlights the possibility of acute demyelinating polyradiculopathy, a serious neurological consequence that can arise from wasp stings. Nevertheless, the pathophysiology of the same is not well recognised in the literature. This emphasises the importance of identifying uncommon causes of GBS and comprehending the mechanism and curative measures.
Introduction
Guillain–Barré syndrome (GBS), also referred to as acute inflammatory demyelinating polyneuropathy (AIDP), is an autoimmune disorder. Two known aetiologies in the literature are vaccinations and infections. According to Yuki and Hartung’s research, these cause the synthesis of autoantibodies through molecular mimicry, which causes peripheral nerve demyelination.[1] Here, we report a young man developing GBS following wasp stings. Although vascular complications are generally reported, neurological complications such as acute polyradiculopathy, myasthenia gravis, optic neuritis and ischaemic or haemorrhagic stroke were occasionally documented with a wasp sting.[2-5]
Case Presentation
A young, 26-year-old male presented to us with weakness in his legs which led to difficulty in walking, inability to hold his slippers with his toes, buckling of his knees and eventually inability to sit up without support. Soon his weakness progressed to bilateral upper limbs. He did not have bladder or bowel involvement, sensory deficit, paraesthesia, backache, limb pains, facial muscle involvement, dysphagia or dysarthria. He did not experience fever, or diarrhoea nor did he undergo recent vaccination. He did not have any comorbidities. On further evaluation, it was found that the patient was stung by multiple (seven to eight) wasps, 10 days ago on his legs. He developed local inflammation for which he took an over-the-counter non-steroidal anti-inflammatory drug.
On day 1, patient was conscious and oriented to time, place and person, with a blood pressure of 118/80 mm Hg, a regular heartbeat of 87 beats/min and a normal respiratory rate of 15/minute There was cranial nerve involvement and no sensory deficit. His motor power was symmetrically decreased with 2/5 and 3/5 in bilateral lower limbs and upper limbs respectively, as per the Medical Research Council (MRC) Power Grading Scale. Biceps, triceps, knee and ankle reflexes were bilaterally absent. The laboratory investigations, including complete blood count and biochemistry, were within normal limits. Human immunodeficiency virus (HIV) was negative by serology. Magnetic resonance imaging (MRI) cervical spine and whole spine screen did not reveal any abnormality to explain such symptoms. Cerebrospinal fluid (CSF) examination revealed no white blood cells and, protein of 56 mg/dL, suggesting albumin-cytological dissociation
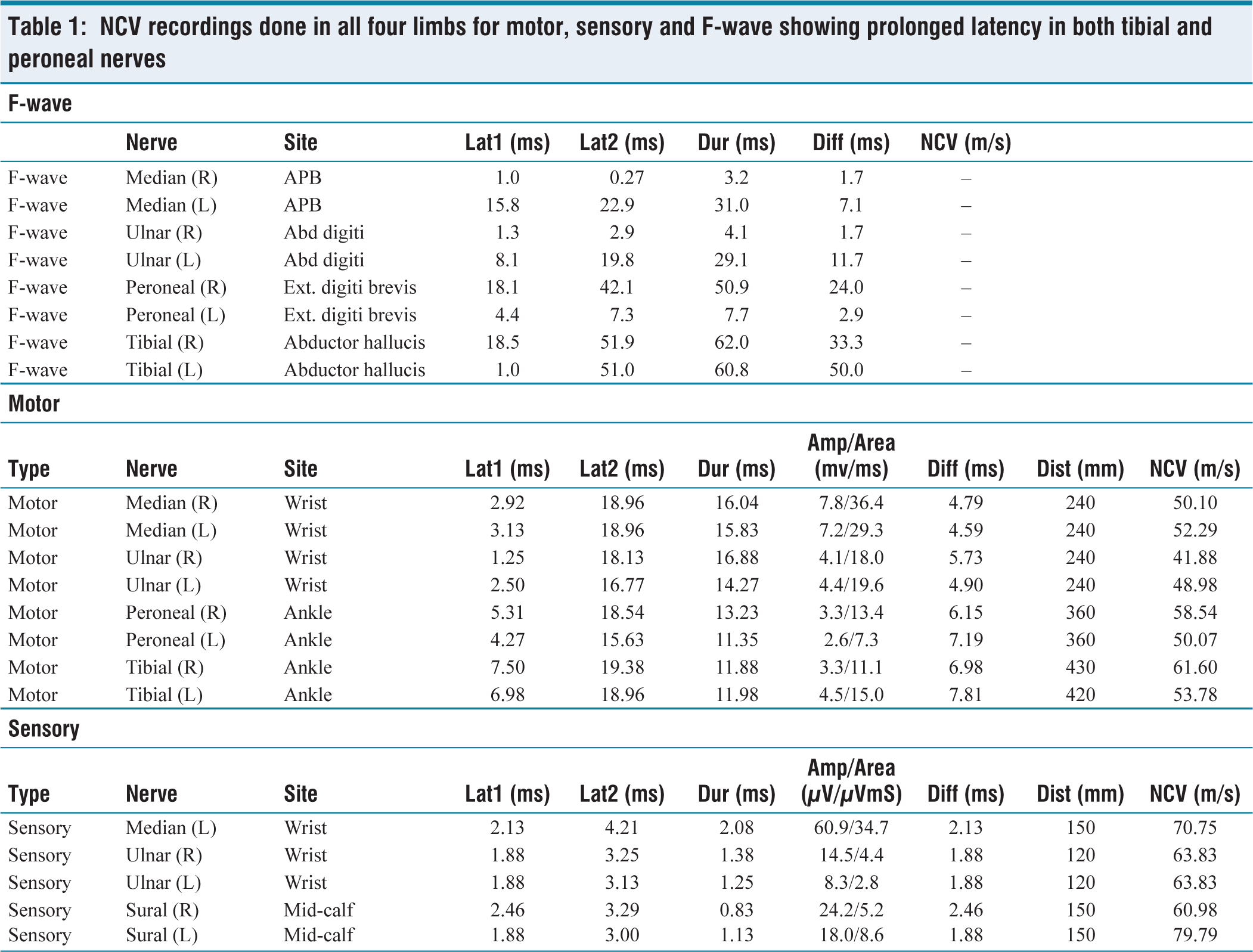
The nerve conduction study suggested prolonged latencies in bilateral tibial and peroneal nerves with normal conduction velocity. It was suggestive of demyelination in both lower limbs. Hence, diagnosis of AIDP was established. The findings of NCV are shown in Table 1.
NCV recordings done in all four limbs for motor, sensory and F-wave showing prolonged latency in both tibial and peroneal nerves
The treatment with intravenous immunoglobulin (2 gm/ kg over 5 days) was started on day 2 of admission.[6] The weakness ceased to progress and he started to improve gradually. By day 4 of admission the patient was able to grip objects firmly and subsequently roll in bed by day 5. He was able to sit up in his bed by day 7. The upper limb and lower limb power was 4/5 each and he was subsequently discharged. The patient was further followed up in the outpatient department (OPD) as he started walking with support followed by a full recovery achieved after 2 months.
Discussion
Neurological problems from wasp stings are extremely rare and typically associated with a delayed immunological response. Most people experience anaphylactic symptoms only wasp venom contains many allergens, enzymes, bioactive peptides, amino acids and volatile compounds which can produce variety of symptoms. Furthermore, proteinous components of wasp venom can cause tissue damage or serious allergic reactions.[7]
Lee et al reported an elderly female who was taking acupuncture therapy with bee/wasp venom developed AIDP within 10 days of receiving therapy. As all probable etiologies have been ruled out for AIDP in our case with only temporal association left was wasp bite, hence temporal causal connection with wasp bite established as etiology in our case. However, the actual pathophysiological mechanism underpinning this has yet to be determined.[8] Bachman et al. identified a similar association in 1982 when five individuals had a neurological illness three to 10 days after being stung by a Hymenoptera bug. Three patients showed characteristic AIDP (GBS). A fourth patient experienced seizures, while the fifth patient just had cranial nerve involvement and hyperreflexia. The timing of these neurological manifestations after insect bites raises the likelihood of a direct or indirect cause-and-effect relationship.[9]
Similarly, such tendencies have also been reported in children. A 3-year-old male resident of Uttar Pradesh, India, developed ascending paralysis with a diagnostic electrophysiological absence of F-wave in all four limbs. This boy was treated with anti-allergic medications and steroids solely, and he recovered. There, the notion of molecular mimicry was applied to some underlying active wasp venom component, resulting in the generation of autoantibodies.[10]
Conclusion
This case report emphasises the potential for severe neurological complications following bee stings. Healthcare professionals need to be aware of these rare but serious reactions and consider them in the differential diagnosis when such temporal events are present in history. Further research is needed to better understand the underlying mechanisms for developing GBS with wasp venom sting. Also, appropriate management strategies are yet to be established for such cases as database related is very limited.
Footnotes
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
Not applicable.
Informed consent
The authors certify that they have obtained all appropriate patient consent forms. In the form the patient(s) has/have given his/her/their consent for his/her/their images and other clinical information to be reported in the journal. The patients understand that their names and initials will not be published and due efforts will be made to conceal their identity, but anonymity cannot be guaranteed.
Credit author statement
Amandeep Kaur and Anuka Koul contributed to case presentation, data collection, literature search and formatted the original draft for the manuscript.
Monica Gupta and Ishreen Ahuja analysed, read, framed and critically revised the design of the manuscript. All authors read and approved the final manuscript.
Author’s declaration
The manuscript has not been submitted to more than one journal for simultaneous consideration. The submitted work is original and has not been published elsewhere in any form or language. Results have been presented clearly, honestly and without fabrication, falsification or inappropriate data manipulation. Authors have adhered to discipline-specific rules for acquiring, selecting and processing data. No data, text or theories by others are presented as if they were the author’s own (‘plagiarism’). Proper acknowledgements to other works have been given.
Data availability
Data is available upon reasonable request from the corresponding author.
Use of artificial intelligence
Artificial intelligence was not used in this study.
