Abstract

Dear Editor,
We want to report a rare case of an iliopsoas abscess mimicking hip arthritis in a patient with Crohn’s disease, emphasising the importance of differential diagnosis in inflammatory bowel disease (IBD)-related musculoskeletal complaints.
IBD, including Crohn’s disease and ulcerative colitis, is are chronic conditions of unknown aetiology that affect approximately 1 in 250 adults and primarily involves the gastrointestinal system. 1 These disorders are frequently associated with extraintestinal manifestations. Among them, rheumatologic symptoms are particularly common and may include peripheral arthritis, axial involvement, peripheral enthesitis, secondary osteoporosis and secondary hypertrophic osteoarthropathy. 2 Complications of IBD can also result in joint pain, which must be carefully distinguished from sterile inflammatory processes. Bacterial infections of the sacroiliac or peripheral joints may arise secondary to fistula formation or bacteraemia. Furthermore, the adverse effects of IBD therapies, particularly corticosteroids, can contribute to joint damage such as osteonecrosis. 3 Here, we present a case of an iliopsoas abscess mimicking hip arthritis in a patient with Crohn’s disease.
A 22-year-old female with a two-year history of Crohn’s disease, who has been on oral mesalazine (2 g/day) and budesonide (6 mg/day) since diagnosis, with well-controlled disease, was referred from the gastroenterology outpatient clinic with a 10-day history of right hip pain. The patient reported pain radiating to the anterior and posterior regions of the right hip, worsened by movement and persisting throughout the day. She was afebrile and had no axial symptoms. Physical examination revealed pain on movement in all directions without joint redness or warmth.
Laboratory tests showed elevated inflammatory markers (CRP 75.3 mg/L, ESR 50 mm/h), with otherwise unremarkable biochemistry. White blood cell count was 10,240/μL, haemoglobin 10.5 g/dL and platelet count 318,000/μL. Hepatitis and HIV serologies and Brucella testing were negative. Due to acute monoarthritis, magnetic resonance imaging (MRI) of the right hip and sacroiliac joints was performed, along with contrast-enhanced abdominal computed tomography (CT) to evaluate for potential Crohn-related complications.
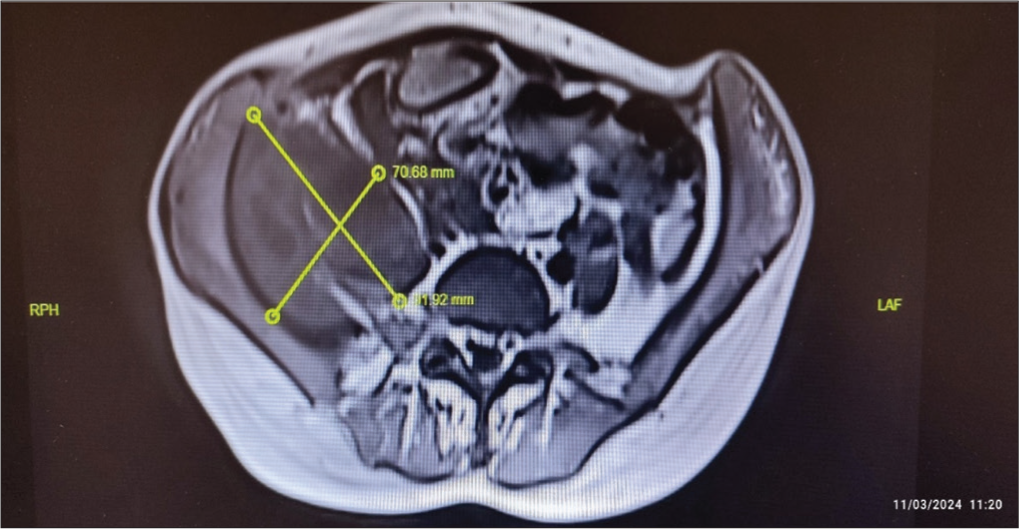
CT imaging revealed a 53 × 92 mm fluid collection within the right iliopsoas muscle, containing air densities and consistent with an abscess. MRI findings supported this, while the sacroiliac MRI was unremarkable. The patient was initiated on nonsteroidal anti-inflammatory therapy and dual antibiotic treatment with sulbactam-ampicillin and ciprofloxacin. Interventional radiology was consulted and percutaneous drainage was performed. Escherichia coli was isolated from the abscess fluid and antibiotic therapy was initiated based on sensitivity results. A second percutaneous drainage was required two weeks later due to persistent findings. Therefore, the duration of intravenous antibiotic treatment was extended to a total of six weeks. The patient was discharged in good condition but was readmitted 20 days later with similar complaints and surgical excision of the recurrent abscess was performed by the general surgery team. The patient was monitored in the general surgery ward for five days postoperatively. She was then discharged with a plan to complete a two week course of oral ciprofloxacin and metronidazole. Following this, azathioprine and infliximab therapy were scheduled to be initiated for fistulising Crohn’s disease.
Crohn’s disease is a recognised cause of secondary iliopsoas abscesses, with an estimated incidence ranging from 0.4% to 4.3%.4–6 While long-term corticosteroid use may increase the risk of abscess formation, this is not typically expected with short-term use.7–9 Iliopsoas abscesses can be diagnostically challenging and delayed diagnosis may lead to sepsis and increased mortality. Hip pain associated with impaired flexion and antalgic gait is are characteristic symptom and may provide diagnostic clues.5,6,10 Although the pain is often localised to the hip, it may also radiate to the flank or thigh.4,5,11–13 Clinicians should consider this differential diagnosis when evaluating hip symptoms in patients with Crohn’s disease. Moreover, patients who develop an initial abscess remain at risk of local recurrence. Management requires both drainage and appropriate antibiotic therapy. In cases of recurrence, as illustrated in our patient, surgical excision may be necessary. 14
Appearance and Dimensions of the Abscess on Magnetic Resonance Imaging T1 Sequence.
We hope this case adds to the awareness of atypical musculoskeletal manifestations of Crohn’s disease and emphasises the need for a multidisciplinary approach in such presentations.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Ethical Approval
Not applicable as this is a single case report with patient anonymity preserved.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
Informed Consent
Written informed consent was obtained from the patient for publication of this case.
