Abstract
The aim of this study was to assess the impact of primary Sjögren syndrome (pSS) on sexual life, quality of sleep and chemosensory function of female patients. We conducted a thorough search of electronic bibliographic databases including MEDLINE via PubMed, the Cochrane Library and Google Scholar. The search covered studies published from 15 September 2015 to 30 September 2023, using the terms ‘Sjogren’s syndrome’ combined with other relevant keywords. We selected studies based on the PICO model (Population, Intervention, Control, Outcome) and study design criteria. Fourteen articles met our inclusion criteria. The findings indicate that female patients with pSS experience significant impairments in sexual function, sleep quality and chemosensory abilities. Specifically, their sense of smell and taste is often diminished, and these sensory deficits are related to dryness of mucosal surfaces. Additionally, women with pSS frequently suffer from vaginal dryness and painful intercourse, likely due to inflammation and dryness of the vaginal mucosa. Fatigue, a common extra-glandular symptom of pSS, is associated with sleep disturbances, reduced quality of life and functional impairments. This systematic review highlights that female patients with pSS often experience notable impairments in chemosensory functions (both olfactory and gustatory), sexual function and sleep quality.
Introduction
In the early 1900s, Swedish physician Henrik Sjögren (SHOW-green) first described a group of women whose chronic arthritis was accompanied by dry eyes and dry mouth. Today, rheumatologists know more about the syndrome that is named for Sjögren and—most significantly for patients—can offer advice about how to live with it. 1
Sjögren’s syndrome (SS) is a chronic inflammatory autoimmune disease primarily affecting exocrine glands, such as the salivary and lacrimal glands. It leads to the immune-mediated destruction of these tissues. 2 SS can occur as a primary condition or as a secondary condition alongside other autoimmune diseases, with rheumatoid arthritis being the most common associated condition. Systemic lupus erythematosus and scleroderma are also linked with secondary SS. 3
The syndrome predominantly affects middle-aged adults, with women being nine times more likely to be affected than men, resulting in a male-to-female ratio of about 1:8. The condition is more frequently observed in perimenopausal and postmenopausal women. 4
Over the past decades, the American European Consensus Group (AECG) criteria, developed and endorsed by the American College of Rheumatology (ACR), have been widely used for classification. 5 Two key points in these criteria are: (a) Either a positive salivary gland biopsy or the presence of anti-Ro antibodies must confirm the inflammatory and autoimmune nature of the disease, and (b) The criteria account for the systemic nature of SS, including patients who, despite lacking salivary or ocular symptoms, present with extra-glandular manifestations and B cell activation markers. 6
Typical symptoms of pSS include dry eyes and dry mouth. Patients often experience continuous eye irritation, an unpleasant taste, difficulty eating dry foods and problems with dentures. 7 Chemosensory disturbances such as reduced or distorted taste and smell are also reported. Additionally, patients may suffer from burning sensations in the tongue or other mucosal surfaces, and halitosis, often associated with reduced salivary secretion and chemosensory disorders. 8
Sexual function is crucial to quality of life (QoL), and approximately 50% of women with pSS report sexual dysfunction. Key genital symptoms include vulvar and vaginal dryness, dyspareunia (painful intercourse), itching, genital pain and increased susceptibility to infections. 9 There is limited evidence on the extent to which these symptoms impact sexual function and QoL in pSS patients. Factors influencing sexual function in pSS may include joint pain, age and sex hormones. 10 Musculoskeletal involvement is common in rheumatic diseases, but internal organ involvement can also affect various life aspects, including social, economic, psychological and sexual functions. 11
Fatigue affects about 70% of pSS patients and is a significant cause of dysfunction. 12 Individuals with pSS experience sleep disturbances more frequently than healthy people of similar age and gender. Pain, fatigue and depression are often linked with poor sleep quality. 13 Psycho-cognitive symptoms, such as memory lapses, forgetfulness, mental confusion and diminished concentration, can also occur and negatively impact health-related quality of life (HR-QOL). 14 This will negatively affect the HR-QOL. However, there is limited evidence on the burden of psycho-cognitive symptoms and their impact on the health system. 15
A systematic review has examined the associations between pSS and impacts on smell, taste, sexual function and QoL in female patients. This review assessed the effects of mucosal dryness on these senses and its impact on HR-QOL. A limitation of the study was the lack of primary research, which hindered the exploration of heterogeneity. 16
The relationship between mucosal dryness, chemosensory disturbances, sexual dysfunction and poor sleep quality in pSS is not fully understood. Therefore, this study aims to determine the impact of pSS on sexual life, sleep quality and chemosensory function in female patients.
Methods
Protocol and Registration
The present systematic review was registered at the National Institute for Health Research PROSPERO International Prospective Register of Systematic Reviews (registration number: CRD42023472493). This study followed the (PRISMA 2020) Preferred Reporting Items for Systematic Review 2020. 17
Data Sources and Search Strategy
The following keywords and Medical Subject Headings (MeSH) terms were used in combination with Boolean operators in the advanced search option. The search was conducted across several electronic bibliographic databases, including MEDLINE via PubMed, Cochrane Library, Embase and Google Scholar. Additionally, related journals, books and bibliographies were screened through electronic searches. Only articles published in English were considered. The search was limited to studies published between September 2015 and August 2023. The keywords used were ‘Sjogren’s Syndrome’, ‘Sexual Dysfunction’, ‘Dyspareunia’, ‘Sjogren’s syndrome and gynaecological issues’, ‘Anosmia’, ‘Hyposmia’, ‘Ageusia’, ‘Hypogeusia’ and
Study Selection
The selection of studies was conducted according to the participants, interventions, comparisons, outcome and study design (PICOS) recommendations.
Eligibility Criteria
Inclusion and Exclusion Criteria of Included Participants, Interventions, Comparators, Outcomes (PICO) and Study Design(S).

Data Extraction
All searched articles were screened by two independent authors for determining whether the inclusion and exclusion criteria were met. The discrepancy was resolved by discussion with the third author. Data on the author, year of publication, country/region where the trial was conducted, sample size, study design, age group of participants, screening/intervention, primary outcome and secondary outcome (if any) were extracted.
Critical Appraisal of Retrieved Studies (Risk of Bias)
Two authors (A and B) independently evaluated the methodological quality and risk of bias for each study using the 11-item checklist developed by the Agency for Healthcare Research and Quality (AHRQ), which is suitable for cross-sectional studies. Each item was marked as ‘YES’, ‘NO’ or ‘UNCLEAR’, with a ‘YES’ response earning 1 point and the other responses receiving 0 points. Based on the total score, studies were categorised as low quality (0–3 points), moderate quality (4–7 points) or high quality (8–11 points). Any disagreements or inconsistencies were resolved by consulting a third author. 18
Synthesis of Results
Literature Search and Study Selection
Final searches were conducted between 23 July and 23 August. Studies published between year September 2015 and August 2023 will be evaluated. An initial search yielded 9,205 articles. Upon screening titles and/or abstracts, no studies were found that investigated the combined impact of dryness on all four aspects—sexual function, sleep and chemosensory function—in patients with SS. As a result, the search strategy was refined to examine the effects of pSS on each of these elements individually, as well as its influence on overall QoL and mental health. A total of 356 studies were identified as potentially relevant; however, 340 were excluded due to reasons such as the absence of female participants or lack of a comparator group. Sixteen studies were selected for full-text review, and ultimately, 14 met the inclusion criteria and were included in the qualitative analysis.
Study Characteristics
The review includes 14 studies. Specifically, five studies examine the impact of pSS on sexual function, another five explore its effects on chemosensory function (both olfactory and gustatory) and four studies assess its impact on sleep quality. Most of these studies are cross-sectional in design. For diagnosing pSS, all studies follow the AECG classification criteria. Participants in these studies range in age from 18 to 70 years, with all studies exclusively including female participants. The subjective assessment of various parameters was performed using the visual analogue scale (VAS), which ranges from 0 to 10. Objective assessments for chemosensory function were conducted using Sniffin’ Sticks for olfactory testing and taste strips for gustatory evaluation. Female sexual function was consistently measured using the Female Sexual Function Index (FSFI) across all relevant studies. Sleep quality was evaluated using the Pittsburgh Sleep Quality Index (PSQI) in the four studies that focused on this aspect. Additionally, the impact of pSS on HRQoL was assessed as a secondary outcome in these studies (Tables 2–4).
Quality Assessment of Included Studies
Assessment was done using Crombie’s item using AHRQ Methodology Checklist for Cross-Sectional and Case–Control Study (Tables 5–7) in which most of these studies showed lower risk of bias. However, studies assessing chemosensory function19–21 showed high-risk category, primarily related to sample representativeness and study design. The studies which assess sexual function24,25 showed higher risk in the adequacy of data description and sample representativeness 28 has area of concern in reporting of response rate, representativeness of the sample and clearly stated aims. The studies which assess sleep function, 32 showed lowest risk of bias; however,29–31 it has at least one high-risk elements in particularly in reporting of response rate and sample representativeness.
Characteristics of the Five Included Studies Assessing Chemosensory Function.
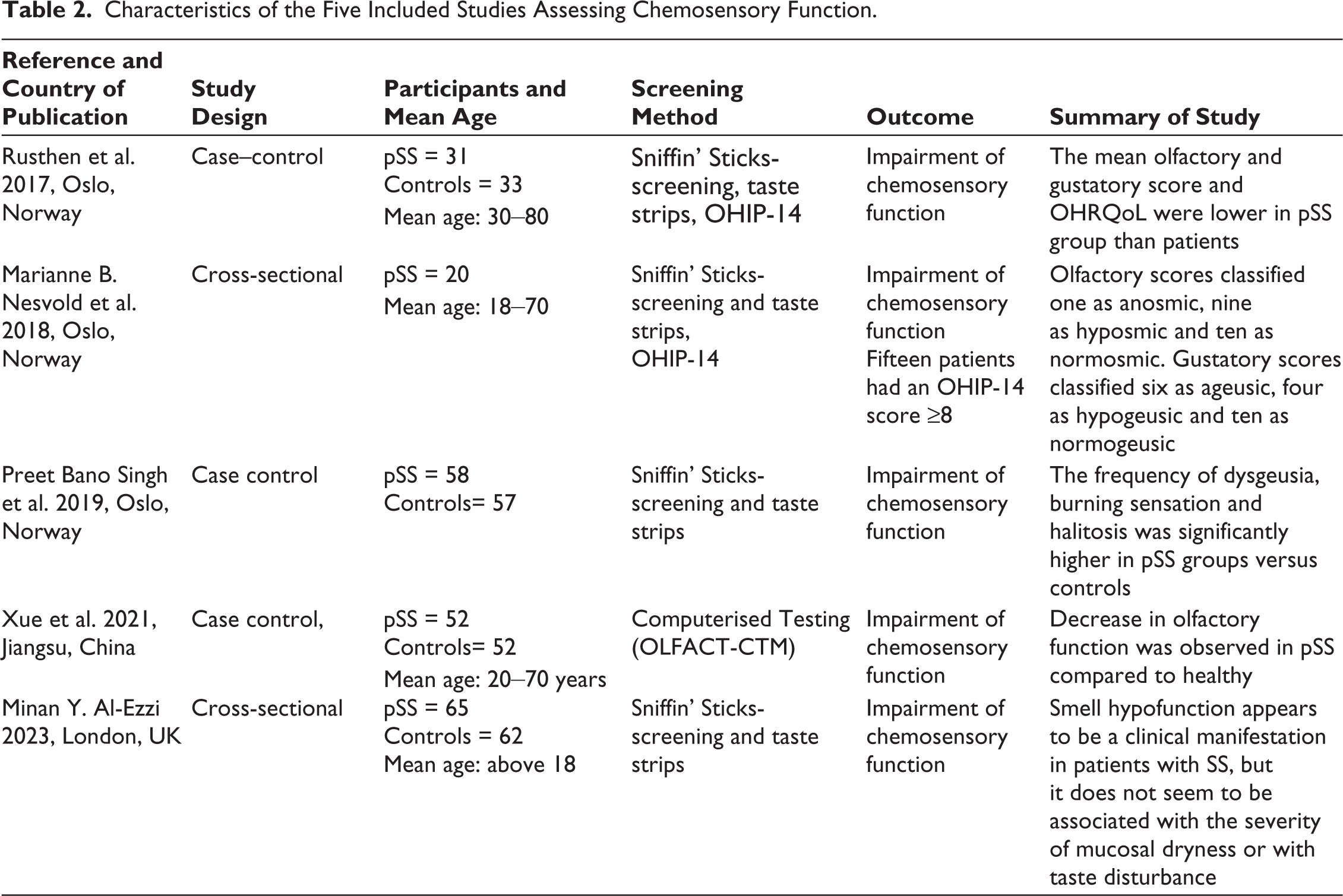
Characteristics of the Five Included Studies Assessing Sexual Function.
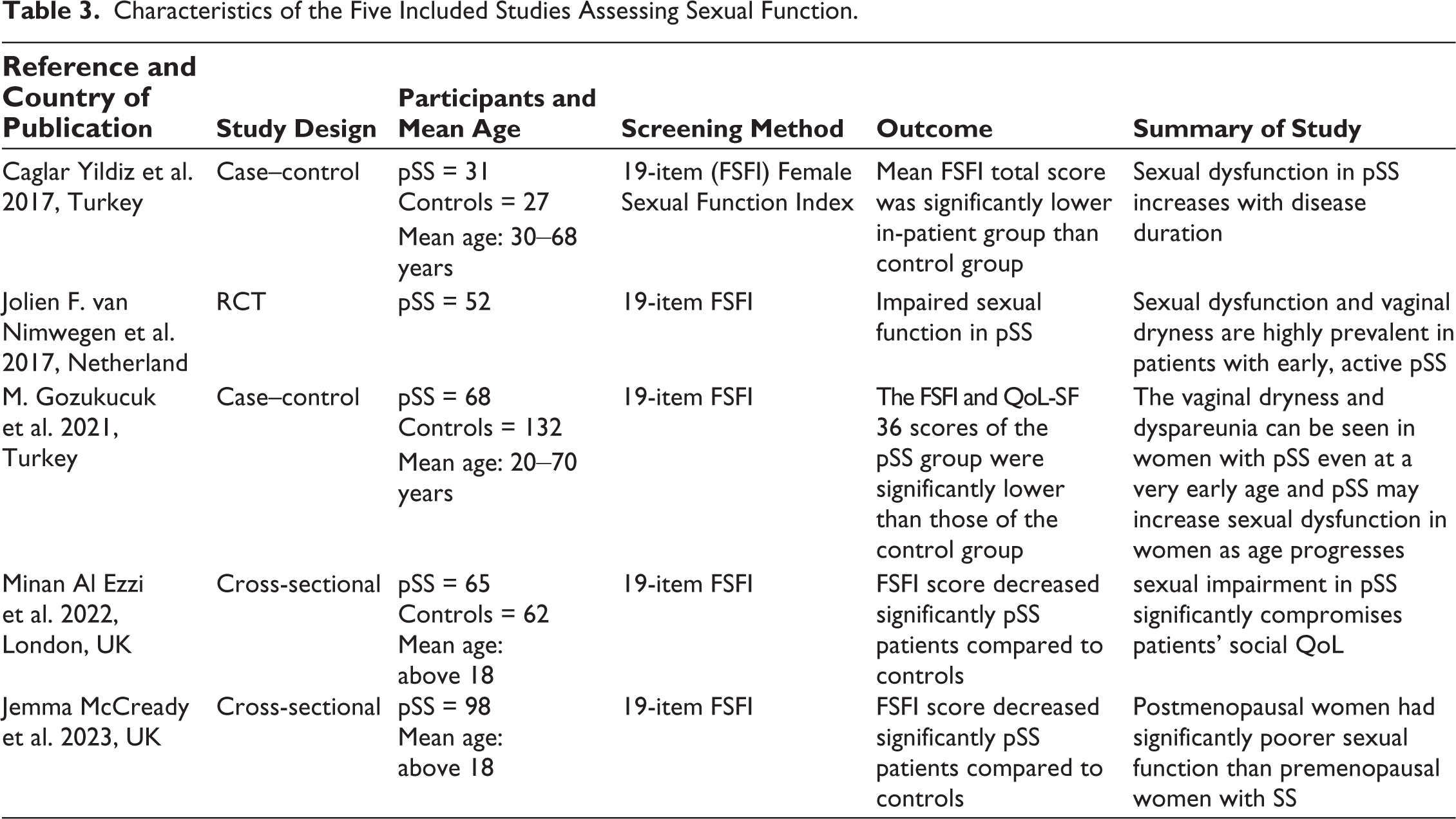
Characteristics of the Four Included Studies Assessing Sleep Quality.
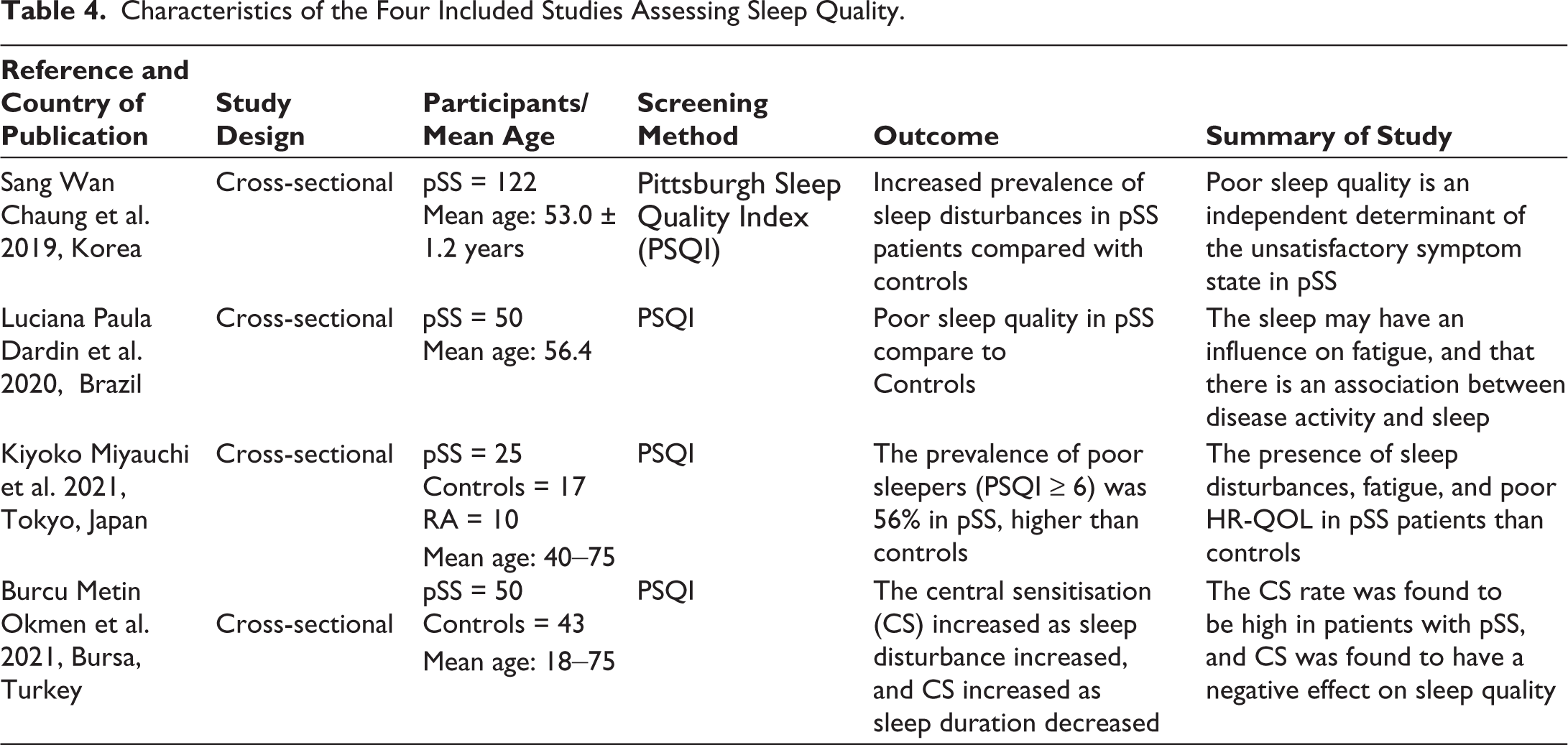
Chemosensory Function
Subjective evaluations of smell and taste functions were conducted in 226 patients with pSS using a 12-odour pen smell identification test and taste strips, and results were compared with those of 204 healthy controls. A significantly higher percentage of pSS patients exhibited ageusia (19% vs. 0%), hypogeusia (32% vs. 12%), anosmia (13% vs. 0%) and hyposmia (29% vs. 9%) compared to controls. However, no significant correlation was found between smell impairment and the severity of dry mouth or taste sensitivity (r = 0.05, P = .6).
Sexual Function
Sexual function was assessed using the FSFI in five of the included studies. In each of these, the mean FSFI scores were significantly lower in the pSS group compared to the control group (P < .05). Furthermore, five of the six FSFI domains—arousal, lubrication, orgasm, satisfaction and pain—were markedly reduced in patients with pSS. Total FSFI scores and all subscale scores, except for pain, showed a negative correlation with the duration of the disease. Sexual dysfunction was consistently associated with reduced QoL and mental well-being in pSS patients, with the most pronounced impact observed on social life quality (β = 0.7, P = .02).
Sleep Function
The subjective assessment was done using PSQI. Included studies showed that 63.5% of pSS patients had PSQI score > 5 indicative of poor sleep quality. There was higher VAS level of overall eye dryness, arthralgia, eyeball pain in Sjogren syndrome Comparison of the PSQI scores of the patients with pSS and the healthy controls revealed a statistically significant difference in favour of the healthy control group in all parameters except duration of sleep and daily function (P < .05).
Discussion
The interplay between mucosal dryness, chemosensory disturbances, sexual dysfunction, poor sleep quality is not fully understood in pSS. The main objective of this review is to systematically evaluate the impact of mucosal dryness on the sensory functions affected by this condition in patients with SS. Thus, we aimed to determine the impact of pSS on sexual life, quality of sleep and chemosensory function of female patients.
Risk of Bias Assessment of Chemosensory Function Using AHRQ’s Methodology.
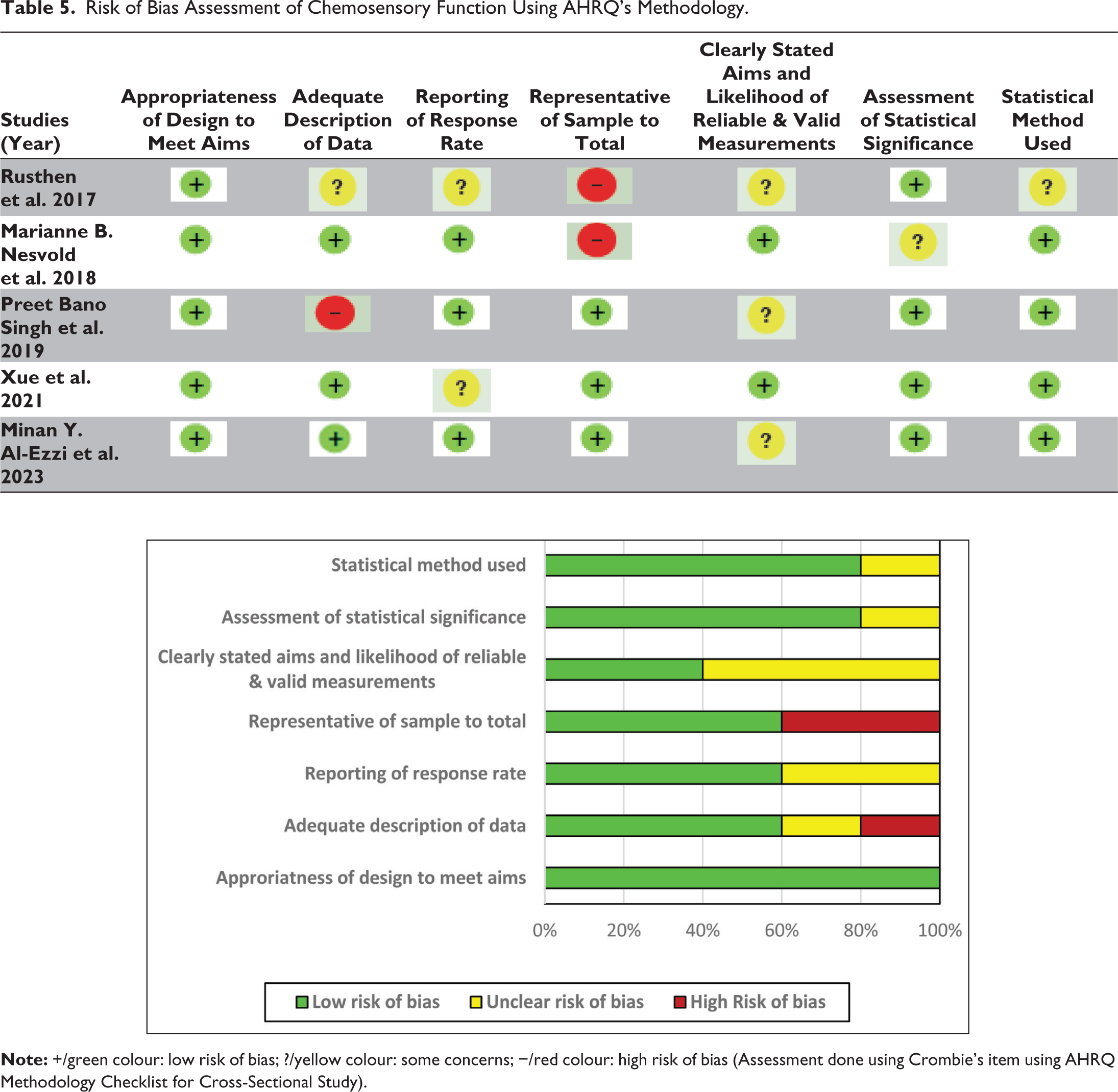
This review included fourteen studies,19–33 of which five assess chemosensory function, other five assess sexual function and remaining four assess sleep quality in pSS patients.
Out of five studies19–23 assessing chemosensory function in pSS, two were case–control and three were cross-sectional, involving a total of 430 participants in the age range of 18–70 years. Subjective assessments of smell and taste were conducted using a VAS, ranging from 0 (no disturbances) to 10 (severe disturbances). For objective smell assessment, researchers used an identification test with 12 odour pens (Sniffin’ Sticks-Screening; Burghart Messtechnik, Wedel, Germany), while gustatory function was evaluated using taste strips. The mean olfactory and gustatory scores were lower in pSS patients, while the Oral Health Impact Profile (OHIP-14) scores were higher, indicating a deterioration in oral health-related quality of life (OHRQoL). Gustatory testing identified significantly more patients with pSS as ageusic (lack of taste) or hypogeusic (reduced taste sensitivity) compared to controls, with fewer patients having a normal sense of taste. Similarly, olfactory testing revealed a higher prevalence of anosmia (loss of smell) and hyposmia (reduced smell) among pSS patients. Additionally, patients with pSS reported a significantly higher frequency of BST (burning sensation in tongue) than did controls (54.8% vs. 6.1%). 21 Notably, pSS patients also showed a higher intake of fat and a lower intake of carbohydrates. This increased fat consumption may serve a lubricating effect in the oral cavity, assisting with mastication and swallowing. 20
The European League Against Rheumatism (EULAR) Sjögren’s Syndrome Patient Reported Index (ESSPRI) and EULAR Sjögren’s Syndrome Disease Activity Index (ESSDAI) showed negative effect on olfactory score. Although dryness of the mucosal membranes was not the key indicative factor for smell impairment.21,22 A strong positive relationship was observed between olfactory and gustatory functions, though the ability to smell did not serve as a reliable indicator of taste sensitivity. 23
Risk of Bias Assessment of Sexual Function Using AHRQ’s Methodology.
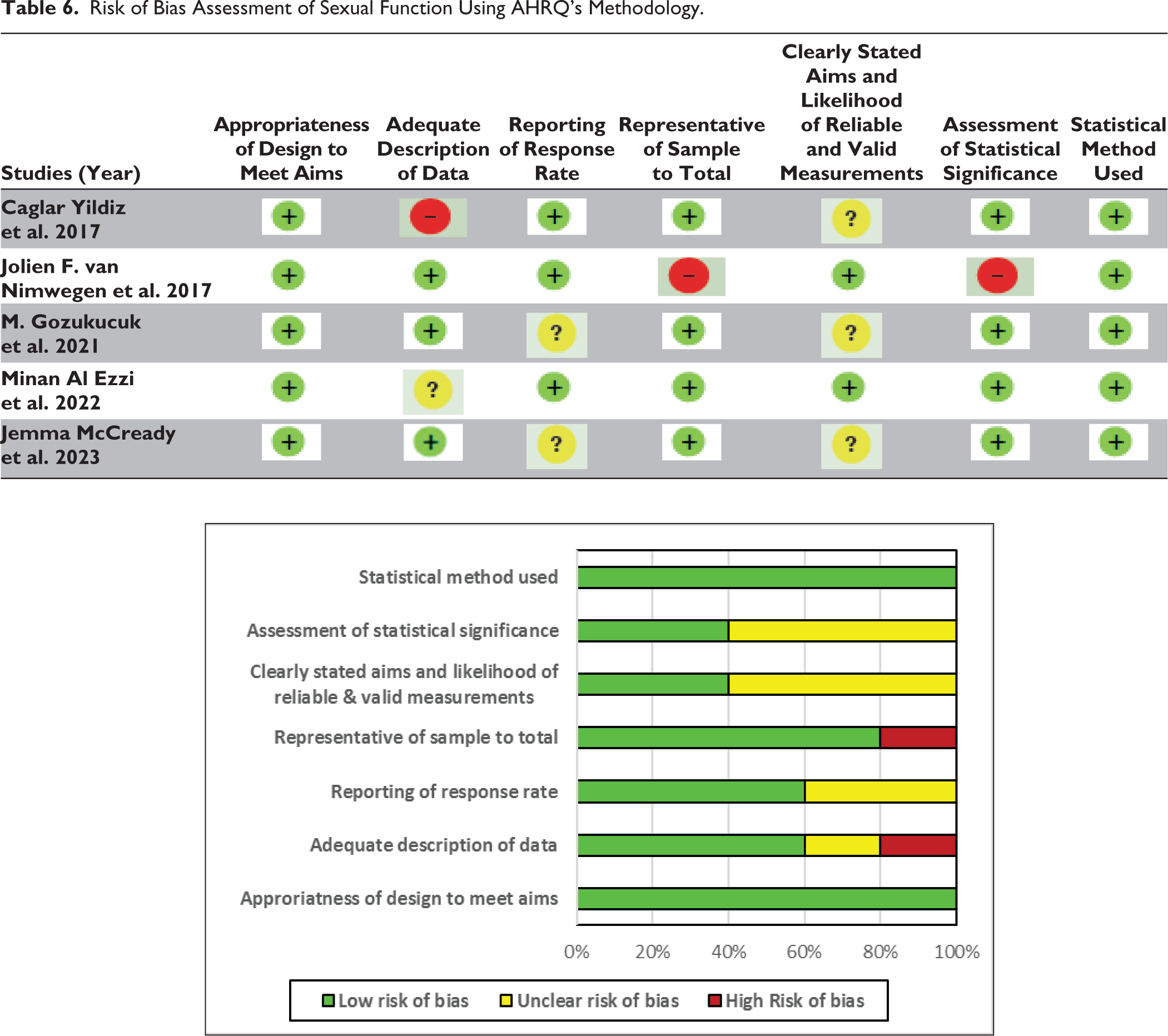
In a review of five studies24–28 involving 535 adult women (314 cases and 273 controls), sexual function was assessed using the 19-item FSFI. The FSFI assesses six aspects of sexual function—desire, arousal, lubrication, orgasm, satisfaction and pain. A score of ≤26.55 indicates a risk of sexual dysfunction. The pSS group showed notably lower average FSFI scores compared to the control group, with significant reductions observed in five domains: arousal, lubrication, orgasm, satisfaction and pain. Except for the pain domain, FSFI scores demonstrated a negative correlation with the duration of the disease. 24 Sexual dysfunction in pSS was linked to factors such as age, vaginal dryness, low sexual desire, dyspareunia and higher ESSPRI scores. 25 Increased vaginal dryness likely results from the autoimmune nature of pSS and the stress of chronic illness. 11 Notably, sexual function and frequency of intercourse did not correlate with vaginal dryness severity. 26 The postmenopausal women with SS had significantly poorer sexual function (total FSFI score) than premenopausal women with SS. The depression and anxiety scores were seen to be significantly higher in pSS group that did control deteriorating the QoL.27,28
Pertaining sleep disturbances, four cross-sectional studies.29–32 In a review of four cross-sectional studies involving 237 participants (average age 56.4 years, mostly female), sleep disturbances were evaluated using the PSQI. This self-reported questionnaire consists of 19 questions covering seven components: subjective sleep quality, sleep latency, sleep duration, habitual sleep efficiency, sleep disturbances, use of sleep medication and daytime dysfunction. Total scores range from 0 to 21, with a cutoff of 8.5 indicating poor sleep quality. Scores ≥ 5 represent poor sleep quality and scores ≤ 4 represent good sleep quality.29,30 The pSS group had significantly higher PSQI scores than controls, highlighting a clear link between sleep disturbances and SS. The poor sleepers reported greater eye dryness, arthralgia and eyeball pain, as well as increased fatigue and depression. 31 No correlations were found between PSQI scores and ESSDAI or symptom duration. However, actigraphy showed that higher ESSDAI scores were associated with longer periods of nightly awakenings. 32
Risk of Bias Assessment of Sleep Quality Using AHRQ’s Methodology.
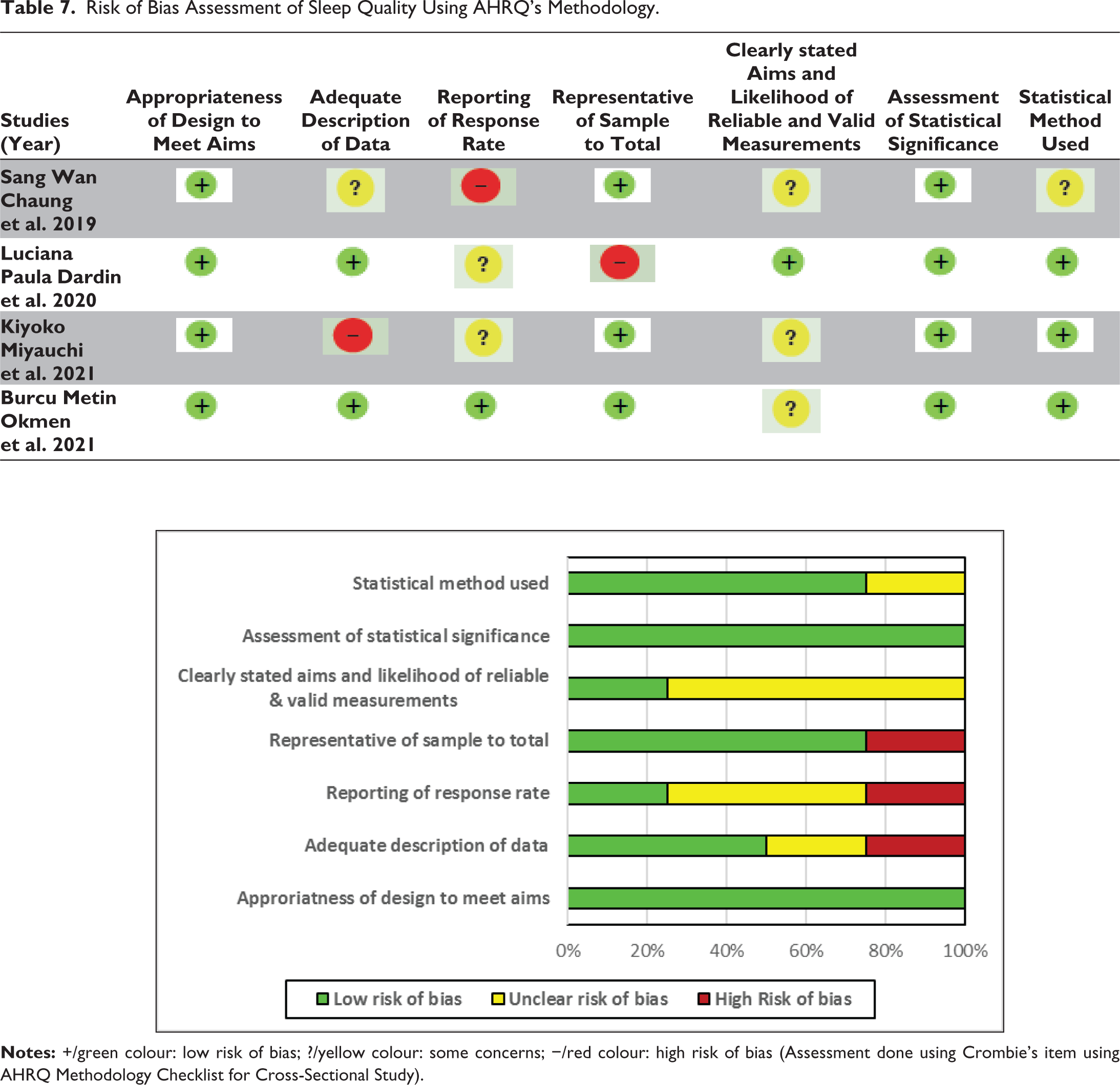
This systematic review highlights that mucosal dryness contributes to diminished taste and smell, vaginal dryness, painful intercourse and poor sleep. Fatigue and sleep disturbances are common in pSS and negatively affect overall well-being and QoL. However, further research is required to identify which specific factors have the greatest impact on patients’ overall well-being.
Future studies should focus on identifying the mechanisms through which mucosal dryness contributes to chemosensory dysfunction, sexual dysfunction and sleep disturbances in pSS patients. Longitudinal research is needed to determine whether early diagnosis and targeted interventions can improve the QoL in these patients.
Limitations
Smaller number of studies with less sample size: The review includes a limited number of studies with relatively small sample sizes, which restrict the generalisability of the findings.
High risk of bias: Some included studies had methodological flaws, such as inadequate sample representation and incomplete data descriptions, leading to a high risk of bias.
Selection bias: Selection bias in recruiting participants may have influenced the outcomes, as the included studies did not always have well-balanced or representative samples.
Heterogeneity: Differences in study designs, assessment methods and participant characteristics contributed to heterogeneity, making it difficult to compare results consistently.
Strength
The strength of the current review lies in its methodology that was conducted in accordance with PRISMA guidelines, to ensure high quality of studies selection and data extraction. The included studies had similarity in screening method, and for this method future meta-analysis of this review will be possible.
Conclusion
In conclusion, this systematic review demonstrated that patients with pSS had impaired chemosensory (olfactory and gustatory), sexual function and sleep quality. Impaired chemosensory function could again adversely affect the OHRQoL. However, the impaired sexual function and sleep disturbances had impact on patients’ well-being. Also, clinical management of female patients with pSS should cover the assessment of their sexual functionality and take the necessary precautions to maintain satisfactory QoL and treatment outcome.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Ethical Statement
Ethical permission was not applicable for this article, as this is a review article drafted from various research articles and not from patients directly.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
Patient Consent
Consent was not applicable, as this is a review article compiled from various research articles and guidelines and not from patients directly.
