Abstract
Our neonatal intensive care unit (NICU) serves an underprivileged population in a resource-restricted environment. The recent COVID-19 pandemic and rapidly changing institutional protocols accentuated the challenges of caring for critically ill newborns. Concurrently, evolving paradigms in neonatal ethics required urgent and high-quality palliative care in a background of racial and socio-economic inequities. Balancing ethical and moral tensions was necessary for compassionate and shared decision-making with families of newborns in high-risk scenarios. Our approach aimed to ensure sustainable online interactions with parents and care providers, virtual education, and, when needed, timely referrals for life-sustaining therapies and palliative care.
The key steps consisted of virtual and in-person family meetings, telehealth for prenatal consultations, traditional in-person teaching, remote educational webinars, and integrating bioethics in providing perinatal and neonatal palliative care.
Case examples representing the gray zones of resuscitation, which were incredibly challenging for family-centered decision-making during the pandemic, are highlighted. NICU providers often experience ethical and moral tensions due to conflicting data on long-term outcomes in many cases, evolving research with contrasting curative care models, and bioethical ambiguity in justifying referrals for regional perinatal centers of care. Ethical stress was addressed by explicating prognostic uncertainty, pathophysiologic heterogeneity, and core concepts in neonatal bioethics. The multilevel allocation of scarce resources, a consistent transdisciplinary approach, and transparent communication with families helped in reducing moral tension.
Tele-advocacy, tele-palliative care, and bioethics education were vital resources for alleviating ethical and moral tensions at our safety-net hospital.
Keywords
Introduction
The COVID-19 pandemic disrupted healthcare systems worldwide, leading to multiple adverse consequences for neonates and their families.1–4 While new challenges in maternal and newborn healthcare unfolded globally during the COVID-19 pandemic, difficulties in managing ever-changing gray zones in neonatology were amplified. In the setting of potential irreversible adverse consequences, including death, the existing literature provides conflicting data for counseling families and navigating these difficult situations. Often, the pathophysiologic heterogeneity and a myriad of confounding variables in each case render uniform recommendations unattainable. Moreover, the impact of persistent racial, ethnic, structural, and process differences on neonatal morbidity and infant mortality adds another layer of complexity.5–7
Safety-net hospitals are essential for providing care to vulnerable populations. Our regional neonatal intensive care unit (NICU) in a safety-net hospital serves an underserved community in a resource-restricted environment. The rapidly changing institutional protocols during the pandemic crisis amplified the challenges faced by the frontline NICU team and disaster service workers. When dealing with challenging scenarios, providing urgent and appropriate counseling to families and high-quality palliative care to patients in restrictive visitation policies and limited healthcare resources at safety-net hospitals became even more difficult. Ethical tension, that is, the tension experienced by healthcare professionals while making decisions complicated by clinical uncertainty and ambiguity regarding the patient’s best interest, 8 and moral tension, defined as an uncomfortable concern, anxiety, indecision, or disputation over the morally right action, are especially challenging. 9 Important causative factors for moral tension in healthcare providers at safety-net hospitals include the worsened social disenfranchisement of patients due to the prevalent inequities in healthcare delivery and poverty. 9
Moral tension and uncertainty in outcomes often lead to hard decisions by healthcare professionals due to their personal beliefs, core human values, and moral reasoning. To add to these challenges, at the onset of the pandemic, there was no evidence that providing counseling and telehealth in high-risk situations addresses the plurality of moral values and divergent approaches in the ethically nuanced gray zones of neonatology. Ethical tension in gray zone scenarios often occurs from decisions complicated by prognostic uncertainty and the absence of clear guidance, if tele-palliative care can help reduce ethical stress among NICU team members confronting irreversible outcomes with limited options.
The NICU providers approached these complex bioethical paradigms through online collaborations, consultations, and tele-advocacy for providing bioethically sound counseling and palliative care when indicated. Here, using clinical case scenarios and diagnosis-based cohort descriptions, we briefly outline the approach that was adopted to deal with difficult neonatal scenarios during the healthcare crisis of an unpredictable pandemic.
Methods
The clinical case scenarios representing gray zones, with potentially devastating clinical outcomes and insufficient evidence to support the long-term benefits of the available interventions in this commentary, include: (a) Life-threatening congenital malformations, including chromosomal anomalies; (b) newborns with persistent pulmonary hypertension (PPHN) and shock; (c) prenatal counseling and care for resuscitating extremely low birth infants at the cusp of viability—22 0/7-23 6/7 weeks estimated gestational age (EGA); and (d) preterm infants with fulminant necrotizing enterocolitis (NEC).
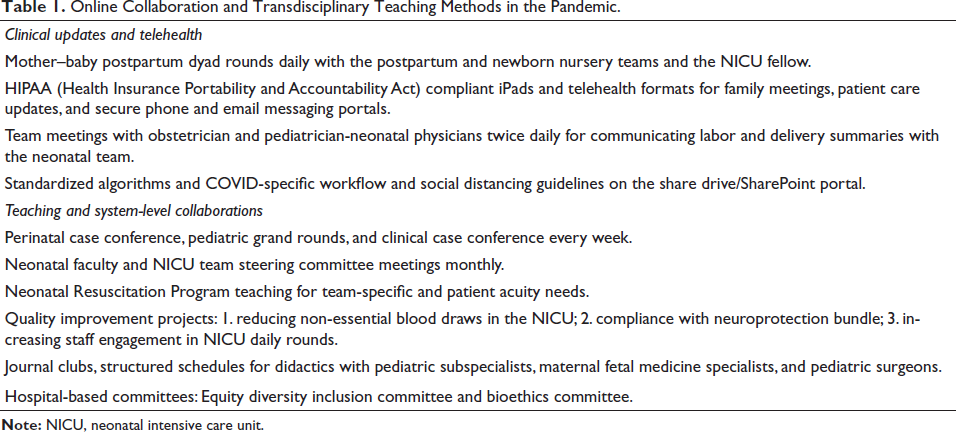
During the pandemic, many essential and even standard NICU resources became scarce due to overwhelming demands on healthcare systems. For this commentary, the measures taken by frontline NICU providers to address ethical and moral tensions in example cases are discussed. We hypothesized that online advocacy, teaching, and collaborations for neonatal palliative care and bioethics could mitigate moral and ethical tensions while providing necessary life-sustaining interventions when needed. Our overarching goals were ensuring that neonates and their families received ethically sound care, timely referrals for extracorporeal life support (ECLS) centers, and specialized palliative care in the strained and uncertain environment of the pandemic, while patient confidentiality and privacy were maintained. The various methods to achieve these goals included (Table 1), and the key steps followed are outlined below:
Structured as well as impromptu online meetings between the neonatal and perinatal care providers and parents.
Virtual platforms for conducting educational webinars, neonatal and perinatal case conferences, and grand rounds.
Consultations using secure electronic communication among various interdisciplinary teams.
Urgently incorporating clinical updates, rapidly changing family visitation guidelines, and pandemic-related regional and hospital protocols.
As feasible, both in-person and virtual bioethics committee consultations.
Online Collaboration and Transdisciplinary Teaching Methods in the Pandemic.

Analysis and Outcomes
Newborns with Postnatally Diagnosed Cardiopulmonary Malformations and PPHN of the Newborn and Shock
Case Example (Figure 1)
Gray Zone: Hemodynamic Instability in a Neonate Diagnosed Postnatally with Life-threatening Pathophysiology.
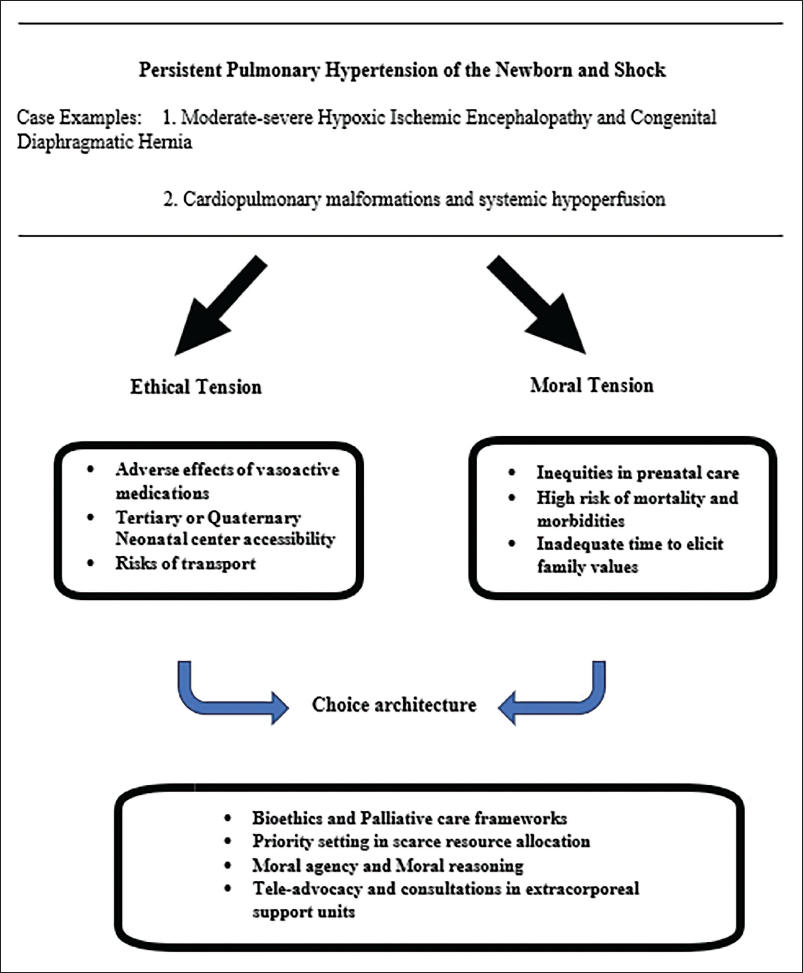
A neonate undergoing therapeutic hypothermia for moderate-severe hypoxic-ischemic encephalopathy (HIE) and a postnatally diagnosed congenital diaphragmatic hernia (CDH). In a case like this, the early NICU course is often complicated by perinatal asphyxia, moderate to severe PPHN, systemic hypotension, and possibly an increased risk of in-hospital mortality if placed on extracorporeal membrane oxygenation (ECMO). 10
Ethical Tension
Conflicting data on the harms and benefits of medical therapies for stabilizing newborns with severe cardiovascular illness make decision-making especially complicated. In the referenced case, the infant required transport to a quaternary pediatric center with ECLS and ECMO capabilities. Comprehensive elicitation of family values before transport proved difficult, as the mother had limited prenatal care due to restricted access to in-person visits at the onset of the pandemic. Prenatal imaging, such as fetal ultrasound and fetal magnetic resonance imaging (MRI), provides critical information about pulmonary hypoplasia and the severity of CDH. However, there is often insufficient time to assess the impact of escalating medical therapies on a rapidly deteriorating clinical condition immediately after birth.
A structured bioethics- and palliative-care framework can be utilized for conversations regarding prognostication challenges of life-saving therapies. 11 Online and in-person parental counseling approaches include choice architecture options to restore the mother’s hope and deliberative decision-making, choice recognition, values clarity, and setting an unbiased tone for conversations. 12
Moral Tension
There is often limited time to discuss and provide support from the palliative care team regarding the irreversible outcome of transitioning to exclusive palliative care. Therefore, we suggest that choice architecture and informed permission focus on the availability of ECMO, the risks and benefits of vasoactive therapies, and the feasibility and safety of transport. To address moral tension, the high risk of mortality and morbidity associated with pulmonary hypertension, cardiac dysfunction, and shock are essential considerations for operationalizing urgent life-sustaining interventions. However, our safety-net hospital was located in one of the most adversely impacted regions of the country. We immediately shifted to crisis care, which entailed rationing medical and surgical therapies in the face of a shortage of qualified medical professionals, limited infrastructure, restrictions to perform surgeries, and a shortage of blood products for transfusions. A multilevel approach to allocate scarce resources was instituted within the healthcare system, hospital leadership, and NICU multidisciplinary team committees. Blood products, a very scarce item during the pandemic, were emergently obtained, notwithstanding the time constraints for weighing curative and palliative care options. Additionally, bedside NICU team discussions included a review of curative therapies for CDH, 13 risks of ECLS and transport, and the benefits of reaching a quaternary-level care center.
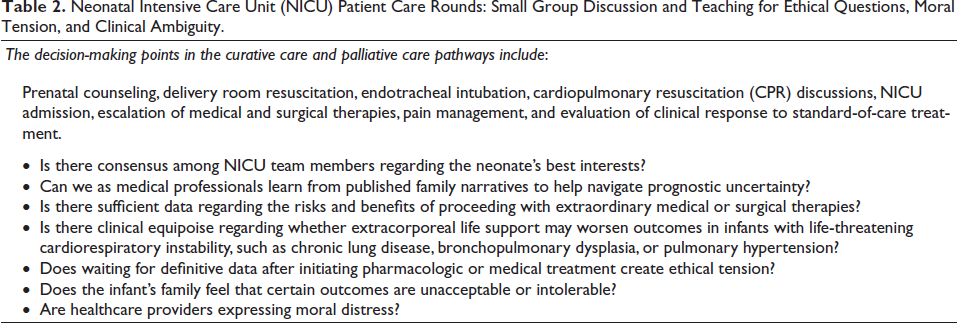
Discussions consisted of proactive assessments based on dynamic supply utilization of the standard resources and post hoc estimates to ensure patients received compassionate, timely, and equitable care. Clinical care providers and disaster service workers had multiple opportunities to express their personal views on how inequities might be impacting outcomes of neonates with significant cardiopulmonary malformations and to reflect on their moral reasoning and ethical awareness (Tables 1 and 2).
Neonatal Intensive Care Unit (NICU) Patient Care Rounds: Small Group Discussion and Teaching for Ethical Questions, Moral Tension, and Clinical Ambiguity.
Health-related Quality of Life (HRQL) and Goals of Care for Infants with Life-threatening Chromosomal Abnormalities
Case Example of Preterm Neonate with Trisomy 18 with Critical Congenital Heart Disease
Healthcare providers often experience ethical tension while caring for babies with Trisomy 18 and 13. Parental interpretations of their infant’s quality of life and the prolonging of life with extraordinary life-sustaining interventions may conflict with the NICU team’s assessments of intractable suffering from a terminal illness and the massive resource utilization in such cases.
Ethical Tension
Improvements in neonatal cardiac surgical care have paved the way for an infant with serious congenital heart disease to live and grow into childhood. Many of these children have significant pre-surgical risk factors at birth, for example, very low birth weight (BW), prematurity, and genetic disorders, that determine their outcome. However, for neonates with Trisomy 13 and 18, there are currently only a limited number of cardiac centers, even in well-developed countries, that offer surgeries to such babies. Many centers have institutional guidelines, possibly with general recommendations on medical and surgical therapies that are deemed futile or non-beneficial. However, there is insufficient literature regarding the detailed ethical underpinnings of cardiac surgical centers that do not offer heart surgery for neonates with life-limiting genetic diseases. Some ethically justifiable considerations for refusing cardiac surgical referrals in such situations might include a high risk of dying during infancy, avoiding harm caused by prolonged pain, and a lifelong dependence on invasive medical technology. Qualitative themes identified by NICU staff in caring for these babies in a recent study included internal conflict, coping with uncertainty, and family experiences, while neonatologists emphasized the variability of presentation and prognosis, rendering the making of intervention choices even harder. 14
In addition to infants with Trisomy 13 and 18, similar ethical issues were encountered while caring for infants with other significant chromosomal abnormalities detected by whole genome sequencing, and/or standard chromosomal and genetic testing. We chose to focus on clarifying the domains/dimensions of HRQL for the purpose of family meetings and on reflecting on advocacy as an integral component of the parents’ voice during goals of care discussions in the NICU (Table 3).
Tele-advocacy Toolkit for Consensus on Health-related Quality of Life.

Moral Tension
To address moral tension, it is essential to point out that defining QOL, which is central to many of the discussions regarding the outcome of infants with severe neurocognitive deficits, is conceptually and methodologically challenging. Strategies outlined in Table 2 were adopted in regular bedside teaching for the house staff, and in discussions with NICU care providers and family members to mitigate moral tension, and thus clearly to highlight and differentiate moral tension from the ethical responsibility of advocating for the best interest of the neonate.
The sequential process of transdisciplinary team education and tele-palliative care reframed hope with a careful consideration of a family’s spiritual, cultural, and religious beliefs, and thereby enhanced the team’s moral reasoning for each critical decision-making step (Tables 1–3).
Prenatal Counseling and Care for Resuscitating Extremely Low Birth Infants at the Cusp of Viability—22 0/7-23 6/7 Weeks EGA
Case examples include neonatology consultation to counsel a mother in preterm labor at 22 1/7 weeks gestational age (GA) and the estimated fetal weight of 402 g. With the ever-changing GA of viability, ethical conflicts are central in resuscitating nano-preterm infants, defined as infants born between the GAs of 22 0/7 and 23 6/7 weeks. 15 Interpreting risks of neurocognitive delays at these GAs is challenging, primarily due to the lack of evidence-based and individualized neuroprotection protocols and long-term data. This gap makes it challenging for practitioners in resource-limited settings to reach a consensus on which respiratory and cardiovascular interventions are truly beneficial or life-prolonging, and which may be considered extraordinary, and potentially inappropriate measures, for nano-preterm infants.
Ethical and Moral Tensions
Ethical conflicts and moral distress hinge on the fact that most of the contemporary research is based mainly on experiences from countries routinely providing active resuscitation for babies born at 22 weeks GA and only from a few centers in the USA.15–21 Neonatal Research Network data reported that the overall survival to discharge for 22-week GA infants was only 10.9%, 18 while a systematic review reported overall survival without moderate or severe impairment at 37%. 19 Within the subset of infants with a GA of 22-23 weeks and a BW less than 400 g, only 6 of the 36 actively treated infants survived to discharge. Nano-preterm infants born with a BW of less than 400 g are at the highest risk of mortality, significant morbidities, and neurodevelopmental delays. 20
Although an increasing range of research offers valuable insights into the medical guidance for nano-preterm infants, there is limited evidence on the role of tele-advocacy for dealing with the ethical challenges of prenatal counseling at this ethical gray zone. At the referenced medical center, pregnant mothers at risk for delivering a baby born at 22-23 weeks GA received urgent in-person or telehealth prenatal consultation with a neonatology fellow, obstetrics team, and attending neonatologist. Social services support followed up with the family if they could not participate in the initial consultation. The prenatal discussions included (a) review of current (recent 5 years) local survival and morbidity data for extremely low birth weight infant (ELBWI), including those at the cusp of viability. (b) There is no clear way to predict whether the currently available data on long-term respiratory and neurodevelopmental outcomes could be extrapolated to other locations. (c) Evolving data on the heterogeneity of disabilities and the granular details of neurodevelopmental impairment in population studies. (d) Interdisciplinary conversations and teaching (Tables 1 and 2) focused on heuristics, microethics, and moral values rather than perceived disabilities, ableism, and untreatable suffering. (e) Clear and transparent discussions regarding biases, perceptions, disabilities, institutional culture, and implications of parental attitudes (Table 3). This coordinated and detailed approach ensured the formulation of a unified management strategy for each high-risk infant, helping mitigate the ethical and moral tensions that usually accompany such deliveries.
NEC and Surgery
Case Example: Ethical and Moral Tensions (Figure 2)
Gray Zone: Fulminant Necrotizing Enterocolitis in a Preterm Infant with Septic Shock and Disseminated Intravascular Coagulation.
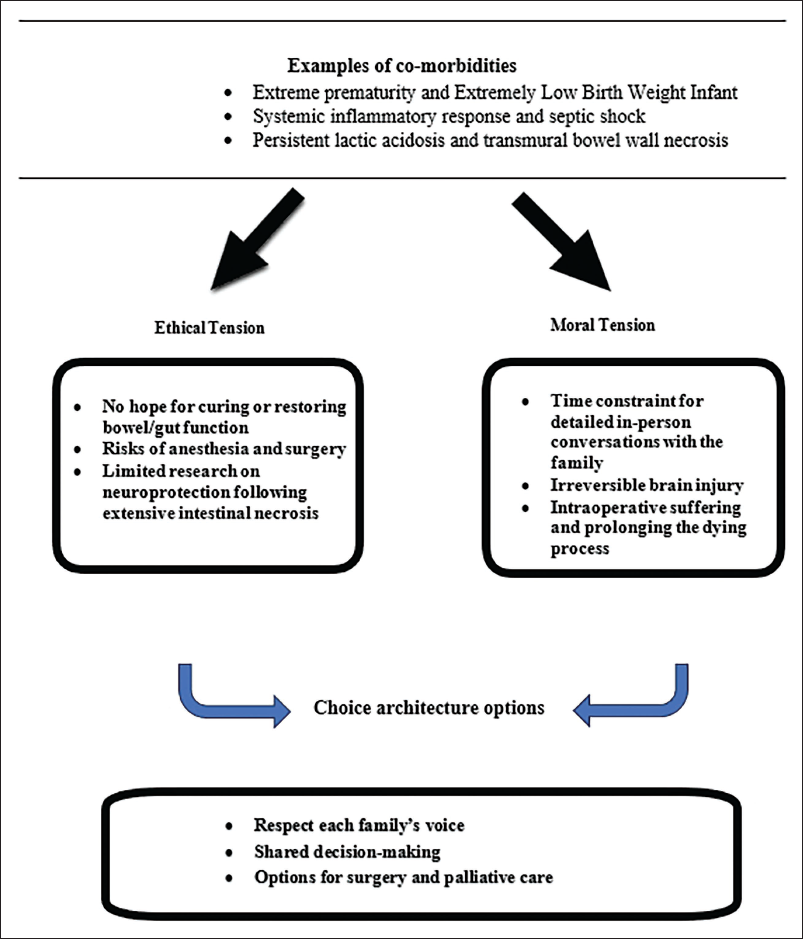
A preterm infant abruptly deteriorated at 4 weeks of age due to fulminant NEC and required emergent endotracheal intubation, cardiopulmonary resuscitation with chest compressions, continuous vasoactive infusions, and multiple blood transfusions. The baby had worsening metabolic acidosis and remained in septic and hypovolemic shock despite escalating medical therapies.
Preterm infants with surgical NEC are at increased risk for mortality, neurocognitive deficits, and impaired physical growth.22–24 The burden of this life-threatening disease remains high, with almost 30%-50% mortality in surgical NEC cases. 23 In 22-26 weeks GA infants with NEC, gastrointestinal and neurodevelopmental morbidities remain unacceptably high. A retrospective analysis of extremely preterm infants (22-26 weeks) showed moderate-severe neurodevelopmental impairment in 77% of children with short bowel syndrome (SBS) compared with 62% with surgical NEC/spontaneous intestinal perforation without SBS. 24
Advocating for palliative care support in fulminant NEC is essential. A summary of intensive end-of-life counseling for fulminant NEC includes: (a) bowel surgery can potentially increase a preterm infant’s suffering and prolong the dying process. (b) The high risk of intraoperative death is due to concomitant cardiorespiratory failure and coagulopathy. (c) Surgery can be a potentially inappropriate intervention in a dying patient with disseminated intravascular coagulation, shock, and clinical parameters concerning extensive intestinal tissue hypoxia and cell death. (d) Clarifying the limits of resuscitative measures and acknowledgment that a neonate may have untreatable suffering from extensively necrosed bowel. (e) Honest communication that the pharmacologic measures for anesthesia, pain, and agitation may be associated with clinical decompensation in a terminally ill patient. Arrange for the parents to hold their baby in privacy while artificial life support devices were disconnected. (f) Consistent neonatal palliative care support, eliciting the family’s perspective by the suggestions mentioned above regarding nano-preterm infants, if applicable.
Conclusions
Human connection is necessary for moral responsibility and ethically nuanced neonatal-perinatal care. Maintaining patient confidentiality and respecting privacy, concurrently with pandemic-related restrictions, were important components of tele-advocacy and transdisciplinary team-based decision-making with the families of newborns in this report. Though anecdotal, the NICU team involved and the parents of neonates expressed satisfaction regarding the effectiveness of online and in-person collaboration, teaching, and advocacy in dealing with the highly challenging scenarios highlighted in this report. This integrated approach was as effective as the traditional in-person model and, in some cases, better, as it facilitated shared decision-making and complex care coordination in alignment with the family’s increased virtual availability and preferences.
New workflows, including telephone and video conferences, and the shift of family meetings to telehealth, ensured that newborns received timely referrals for life-sustaining therapies in a rapidly evolving pandemic environment. Addressing the associated ethical and moral distress requires substantial time, expertise, and evidence-based mitigation strategies; detailed guidance is beyond the scope of this report. Given the scope of this article as a commentary, its primary limitations are the absence of quantitative outcomes, family-satisfaction metrics, and stress indicators among neonatal providers. We recognize the importance of monitoring these parameters, as well as the need for an in-depth evaluation of the efficacy and long-term sustainability of neonatal telehealth programs.
Barriers to telehealth at our site included internet latency, intermittent disruptions in connectivity, and the lack of a formal policy ensuring that all families of hospitalized neonates had access to a personal mobile phone. These challenges were addressed through coordinated efforts involving hospital administration and informatics specialists. Solutions included innovative educational strategies such as virtual instructional modules for all medical professionals and the integration of community-based resources identified by social services personnel. These interventions were designed to support families, promote mental health advocacy, and enhance parental autonomy during NICU hospitalization.
In summary, the use of tele-advocacy, tele-palliative care, bioethics education, and, when possible, in-person counseling for neonatal palliative care in ethically gray zones proved vital to providing regional perinatal-neonatal care in a resource-limited setting during the evolving pandemic. We believe this approach can be adopted broadly to deliver high-quality perinatal-neonatal care and remains highly relevant in the post-COVID era.
Footnotes
Abbreviations
CDH: Congenital diaphragmatic hernia; ECLS: Extracorporeal life support; ECMO: Extracorporeal membrane oxygenation; EGA: Estimated gestational age; GA: Gestational age; HIE: Hypoxic-ischemic encephalopathy; HRQL: Health-related quality of life; NEC: Necrotizing enterocolitis; NICU: Neonatal intensive care unit; PPHN: Persistent pulmonary hypertension of the newborn; SBS: Short bowel syndrome.
Acknowledgments
Our sincere gratitude to the families of the NICU patients, the NICU team, the Department of Pediatrics, and the Department of Pediatric Surgery at the Harbor-UCLA Medical Center.
Declaration of Conflicting Interests
The authors declared no conflict of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
IRB approval was not required for this review. The content is based on general examples using de-identified cases. The main article describes a commentary on the telehealth and tele-advocacy approaches for education and perinatal-neonatal care, and a bioethical analysis.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Informed Consent
The participant has provided informed consent for the submission of the article to the journal.
