Abstract
Introduction
Human milk banking is an essential perinatal service. The present study evaluates the impact of gestational age on the volumes of milk. Further, it also re-evaluates the definition of “Coming to Volume” in pump-based expression of milk.
Methodology
This cohort study was conducted at a tertiary care centre in south India over 10 months from September 2022 to June 2023. The primary objective of the study was to compare the volume of donor milk secreted in relation to postnatal day among mothers delivered at term and preterm gestation. The secondary objective of the study was to compare the definition of “Coming to Volume” (secretion of 500 mL per day by postnatal day 14) with the volumes of milk in the present study. A surrogate marker for “Coming to Volume”, that is, an expression of at least 80 mL in one sitting of the donation was considered.
Results
Of the total 458 mothers, there were 349 (Term) and 109 (preterm) mothers. The average volumes of donor human milk were 142 mL and 122 mL among term and preterm mothers, respectively (p-value .0068). Further, 80% of the term mothers and 75% of the preterm mothers were able to secrete>80 mL per sitting. This volume was attained by postnatal day 7 in 80% (223/280) of term mothers and 65% (53/82) of preterm mothers.
Keywords
Introduction
Human milk banking is an essential perinatal service. There is a rise in the number of human milk banks across India owing to the rising awareness. As the functioning of a milk bank is non-profitable, challenges are not uncommon. Ensuring the availability of donor milk to match the requirements of all the eligible recipients is a big task in itself. Balancing the demand-supply chain has also been observed as one of the three common challenges of human milk banking as reported by a survey conducted in India across 16 milk banks. 1
The donor milk volumes secreted by mothers vary depending on multiple factors that include environmental, maternal, neonatal and social dimensions. 2 There are few studies that have evaluated and concluded that breast-pump-based expression volumes are higher than manually expressed breast milk volumes. 3 Further, the literature on the volumes of milk secreted as a determinant of maternal factors is scarce. We aimed to evaluate gestational age and breast-pump-based expression in relation to the volume of breast milk. The present study evaluates the impact of gestational age on the volumes of milk. Further, it also re-evaluates the definition of “Coming to Volume” (traditionally defined as 500 mL of milk per day by postnatal day 14). 4
Methodology
This cohort study was conducted at a tertiary care unit in south India. The study was conducted over a period of 10 months from September 2022 to June 2023. Institutional Ethical Committee’s approval was obtained for the present study. The demographic characteristics of eligible donors were noted.
Methods
Maternal age, parity, co-morbidities and mode of delivery were recorded. Human milk donation was voluntary in nature. No remuneration was paid to donors and no fees were charged for recipients.
The human milk was collected only after the mother satisfied with all the criteria for donation as per Indian Academy of Pediatrics―Human Milk Banking guidelines. 5 Any mother who was found to be unfit for donation was explained the same, was given adequate medical advice and was also given an acknowledgement letter. Audio-visual aids were used in the postnatal wards to encourage mothers to donate milk. Informed consent was taken from donors before collection of milk and also for the enrolment into the study. Privacy was ensured by providing a separate collection room to express milk.
Donor Milk Collection
Facilities for hand washing and bathing (if required) prior to donating milk were provided to mothers in the milk bank. The lactation consultant counseled the mothers about milk donation and carried out a preliminary examination of the breasts to ensure that there were no local problems (retracted/flat/sore nipple/breast abscess/breast engorgement). The lactation consultant offered practical help if needed and personally supervised the breast milk expression by using hospital-grade electric breast pumps (Medela breast pumps). The milk was collected in sterile bottles as per the milk banking guidelines. The quantity of milk donated by each mother (along with demographic details) was recorded in the donor register as well as in the study proforma. The record of each donation was maintained in the record book of the milk bank. The donated volume of milk was recorded in the study proforma for each sitting. The total volume donated by each mother (one or multiple sittings) was added to calculate the average volume of donations. The presence or absence of breastfeeding was not separately analyzed as this was a highly variable factor not only among different mothers but also in the same mother at different points of the study period.
The donors were divided into two groups: Term mothers and Preterm mothers, based on the gestational age at which their babies were born. All the study variables were compared between the two groups. The amount of milk secreted and the postnatal day on which the donation was done were diligently recorded. The measurement of the volume of milk donated was done using the volume markings written on the collection bottles.
Objectives
The primary objective of the study was to compare the volume of donor milk secreted in relation to postnatal day among mothers delivered at term and preterm gestation. The milk volume was higher with breast-pump-based expression of milk when compared to manual expression in a parallel study being conducted at the institute. For the sake of the present study, the volume of milk expressed with the help of a breast pump only (under the supervision of a lactation consultant in the milk bank) was considered. The secondary objective of the study was to compare the traditional definition of “Coming to Volume” (secretion of 500 mL per day by postnatal day 14) 4 with the volumes of milk in the present study. As human milk donation is voluntary and is usually done after satisfying the needs of one’s own baby, a surrogate marker for “Coming to Volume”, that is, an expression of at least 80 mL in one sitting of breast-pump-based expression was considered (considering eight expressions in a day―every third hourly) for the present study. The donated milk cannot be equated with secreted milk considering the voluntary nature of donation. The volume of milk donated in each sitting was recorded for every donor, but the maximum volume donated in one sitting per day was highlighted if a mother donated multiple times on multiple days. Such maximal readings per day were considered for the determination of “Coming to Volume”, since the definition deals with the expression of milk in one sitting of donation in the present study. The average volume of milk collected by each mother was used to depict the primary objective, whereas the milk donated in each sitting of the maternal donation was considered for the secondary objective of calculation of “Coming to Volume”.
Data Monitoring
Data were verified by the milk bank in charge and pediatric consultant on a daily basis. Weekly research meetings were held by the first author to ensure consistency and precision of the data. The process of milk banking was supervised by the milk bank managers―the co-authors of the study. The lactation consultant helped mothers with the donation of milk. The pediatric consultant who was assisting residents helped in obtaining consent and collecting and monitoring data. Drafting the manuscript and adding the relevant literature were done under the supervision of first author.
Statistical Analysis
The categorical variables were expressed as proportions. The continuous variables were expressed as mean, SD or median, and centile as applicable. Scatter plots were used to depict the volumes of breast milk secreted as against postnatal day among the two groups studied. Comparison of means and proportions was done using free online MedCalc software (MedCalc Software Ltd., 22 001/May 2023). P-value of less than .05 was considered significant.
Results
A total of 458 eligible human milk donors were enrolled in the study. There were 349 term mothers (Group I) and 109 preterm mothers (Group II). Maternal morbidities (PIH, GDM and antepartum hemorrhage) accounted for 6% in Group I and 15% in Group II. They were higher among preterm mothers. The baseline characteristics of all the donor mothers have been shown in Table 1. Maternal morbidities and rates of LSCS were significantly higher among the mothers in Group II when compared to Group I.
Baseline Characteristics of Donor Mothers.
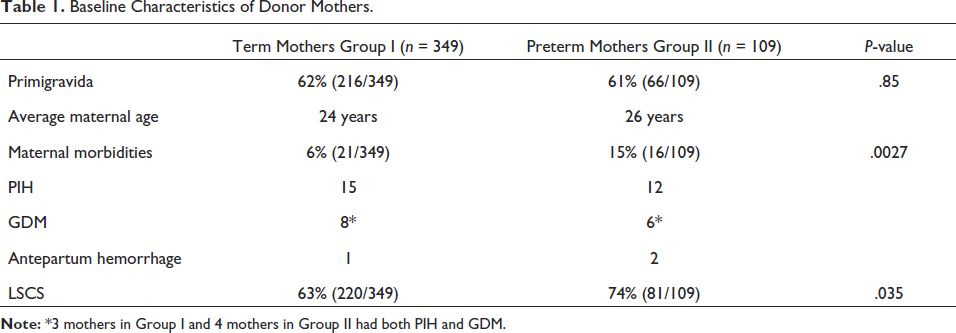
All the mothers used hospital-grade electric breast pumps to express breast milk. The average volume of donor human milk secreted by term mothers was 142 ± 71 mL. Preterm mothers secreted an average of 122 ± 52 mL. The average volume of milk secreted by term mothers was significantly higher than preterm mothers (p-value .0068). The maximal donation occurred on postnatal days 4, 5, and 6 among both the groups. The mothers were encouraged to donate milk as long as possible during the postnatal period. The maximum duration of the donation was up to postnatal days 40 (Preterm) and 90 (Term). Since the donation was voluntary in nature and also after satisfying one’s own baby’s needs, the volumes are not reflective of the actual volume of milk secreted by a mother. The donation of milk continued even after discharge from the hospital during follow-up visits like immunization/ROP screening/hearing screening visits. Table 2 depicts details of the donation of milk.
Depicting Details Related to Donation of Milk.
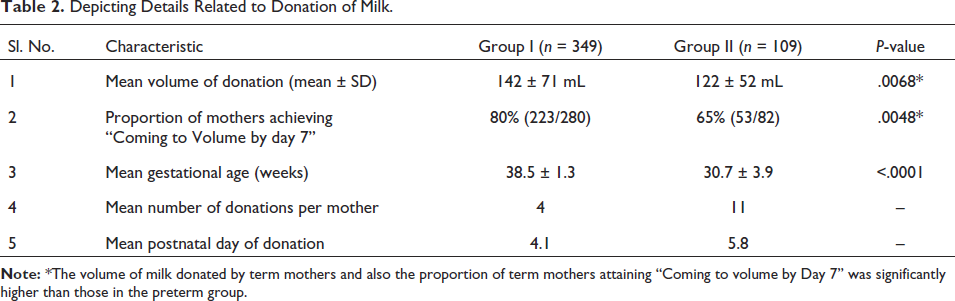
Further, it was noted that 80% (280/349) of the term mothers and 75% (82/109) of the preterm mothers were able to secrete >80 mL per sitting with the help of the hospital-grade breast pump. This volume was attained by postnatal day 7 in 80% (223/280) of term mothers and 65% (53/82) of preterm mothers. It needs to be remembered that these mothers are voluntary donors. Hence, it can be said that a significant number of mothers were able to attain adequate volume (Coming to Volume) during the first postnatal week itself.
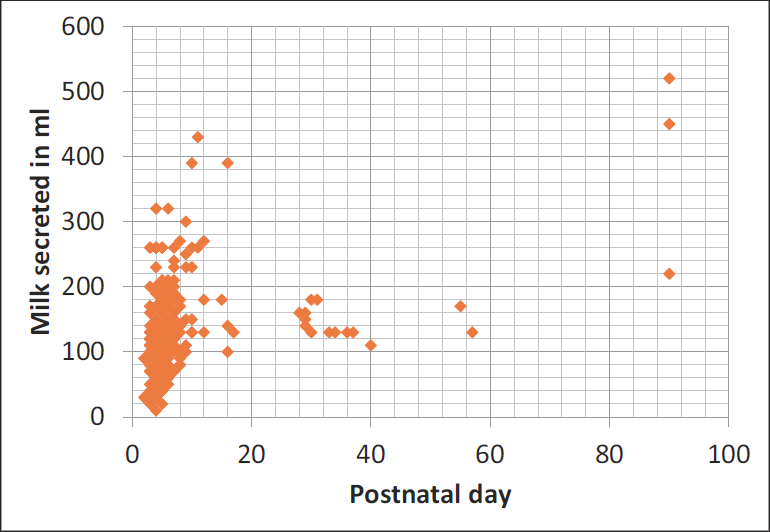
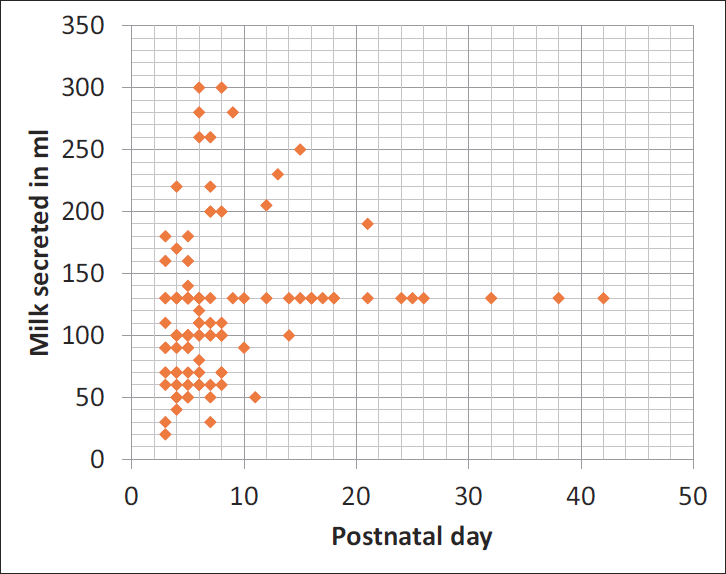
The scatter plots depicting the volume of donor milk against the postnatal day of expression have been shown in Figure 1 (For mothers with term gestation―Group I) and Figure 2 (For mothers with preterm gestation―Group II). The scatter plots depict the amount of milk secretion in a single day per mother.
Scatter Plot Depicting the Volumes of Donated Milk Against the Postnatal Day Among Group I––Mothers with Term Gestation at Delivery.
Scatter Plot Depicting the Volumes of Donated Milk Against the Postnatal Day Among Group II––Mothers with Preterm Gestation at Delivery.
Discussion
The present study showed that term mothers had significantly higher amounts of breast milk when compared to preterm mothers. The results are similar to the study conducted by Hill et al. 6 The present study has a higher sample size compared to the study by Hill et al. 6 and agrees with the previous results. However, the qualitative analysis of donor milk was not done in the present study.
It is hypothesized that breast-pump-based expressions are relatively painless, less tiring and less time-consuming when compared to manual expression of breast milk and hence contribute to higher volumes of donor milk. An RCT by Lussier et al. 7 showed that expression of milk by electric breast pumps was significantly higher during the first 28 days postpartum when compared to hand expression of breast milk. 7 To maintain uniformity, all the mothers in the study expressed milk using hospital-grade breast pumps.
Hoban 5 defined “Coming-to-Volume” as the expression of 500 mL of milk per day by postnatal day 14. The same definition for “Coming to Volume” has been used in two other studies.8, 9 However, similar literature from India could not be found to the best of our knowledge. Considering the voluntary donation of mothers in the present cohort, a volume of 80 mL per sitting was assumed to define “Coming-to-Volume”. We believe that the enhanced expression of breast milk using a hospital-grade breast pump enabled mothers to attain “Coming-to-Volume” earlier than 15 days of postnatal age in the present cohort. The main reason to quantify the milk output among the human milk donor cohort is to identify mothers who can feed their own babies and have additional volumes to donate for the milk bank. These mothers can be identified as “Champions of Human Milk Donation”, and they can motivate other mothers to successfully breastfeed and also to donate milk at the milk bank. Hence, they can be role models for other mothers in the high-volume perinatal setting.
Adjuvants to successful breastfeeding like counseling and Kangaroo mother care were encouraged among preterm mothers. Kangaroo mother care is a proven method of increasing the rates of exclusive breastfeeding 10 and is carried out systematically at the study center. Mothers are encouraged to give KMC at least 8 hours a day. Quality Improvement initiatives are in place to increase the duration of KMC further.
Majority of the donor milk was collected during the first 10 days of the postnatal period. The donations continued up to 90 days after delivery in the present cohort. A few donors visited the milk bank during postnatal follow-up days and contributed breast milk.
Strength and Limitations
The strength of the present study is the number of donor mothers available for the study and the study also helped us streamline the process of milk banking. The limitations of the study are the lack of qualitative analysis of donor milk and the non-uniformity of the timing of donation due to the voluntary nature of milk donation. The present study has given inputs to frame the fishbone analysis for quality improvement initiatives to increase the quantity of donor milk in human milk banks.
Conclusion
The present study shows that the breast-pump-expressed volumes of milk among term mothers were significantly higher than preterm gestational mothers. Considering a surrogate definition of “Coming to Volume”―80 mL in one sitting of breast-pump-expressed donor milk (considering the voluntary donation and the frequency of eight expressions per day), more than 75% of the mothers in the cohort were able to attain this volume by postnatal day 7. The study helps in identifying the mothers who attain “Coming to Volume” as champions of human milk donation, and the further donation can run on a positive feedback mechanism.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
The present study was assessed and approved by Institutional Ethical Committee.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
