Abstract
Breastfeeding is the only most natural and fundamental part of infant nutrition and early development. It plays a vital role in the optimal nourishment and fostering a myriad of health benefits for newborns. While breastfeeding is a natural process, it may also present challenges. Latching difficulties, maternal perception of inadequate milk supply, maternal medical conditions and her medication use, multiple gestation, congenital abnormalities in the baby, cultural and regional practices of prelacteal feeds, psychosocial factors, and so on can be some of the issues (Charantimath et al. PLoS One. 2020;15(5):e0231755). The problems intensify when these issues present at a rural setting with limited resources and many social factors and myths surrounding breastfeeding. With advancement in the study of breastfeeding techniques and protocols and understanding of the whole physiological process up to molecular level has given us insights as to how these problems can be managed better. An interdepartmental coordination and support are needed for solving these issues and improvise the outcomes in the infant nutrition. We present here a set of 9 mother infant dyads who had a peculiar course of breastfeeding and how they were counseled and managed at a rural medical college setting.
Keywords
Introduction
Breastfeeding forms a vital basis for infant nutrition, providing a complex blend of nutrients and bioactive compounds tailored for the infant’s needs and immunity. It aids maternal recovery, lessening postpartum blood loss, depression, and aiding weight loss, while also reducing risks of breast and ovarian cancers. Beyond nourishment, breastfeeding fosters a strong mother-child bond through skin-to-skin contact. Challenges can arise, demanding expert lactation support due to maternal stress and health conditions affecting milk production and necessitating tailored guidance.1, 2 The under 5 mortality in India is 41.9 per 1000 live births. Major contributors to childhood mortality are diarrhea and respiratory infections, and breastfeeding helps in preventing them.3, 4 This, along with rising deaths from cancers and type II diabetes due to inadequate breastfeeding, may cost the Indian economy $14 billion, equivalent to 0.70% of its gross national income. 5 Presented here are 9 unique cases from a rural medical college in Karnataka, where breastfeeding establishment proved challenging due to maternal or infant factors, requiring specialized counseling and healthcare efforts. This hospital follows a robust breastfeeding policy in line with World Health Organization-Baby Friendly Hospital Initiative (WHO-BFHI) since the beginning.
These cases are unique in themselves and require specific counseling and extra effort from the healthcare workers.
Case 1
A 26-year-old primigravida with paranoid schizophrenia, on Aripiprazole, Escitalopram, and Sertraline, gave birth to a healthy, 3.02-kg male. Immediately exclusive breastfeeding began, following a strategy of daytime direct feeds and nighttime expressed feeds (stored appropriately throughout the day) by the mother herself after taking her medication at night. 6 We utilized the “pump and dump technique” that advocates expressing out of breastmilk at the time where the drug level is at the highest concentration in mother’s blood. These drugs were safe during lactation, and the newborn was monitored closely for the symptoms of toxicity. 7 There was steady weight gain for a week. Maternal relapse on day 5 of life led to the increase in the medication dose in the mother. And the baby developed a breast abscess secondary to squeezing of baby’s breast by caretakers, which needed aspiration and oral antibiotics. This prompted mixed feeding with undiluted cow’s milk via a food feeder called paladai. Lactation support, psychiatric counseling, and medical care were constant. Mother’s stable health, confidence in breastfeeding, and 20 g/day weight gain trend led to discharge in week 2. Knowledge of drug kinetics, medical care, family support, and lactation counseling were key in management.
Case 2
A 29-year-old multigravida with severe preeclampsia and abruption underwent emergency lower segment cesarean section, delivering a 2.1-kg small for gestational age baby with birth asphyxia and grade 3 hypoxic ischemic encephalopathy. Neonatal intensive care unit care lasted 10 days; trophic feeds began on day 3, increasing gradually with medical support. Week 2 saw direct breastfeeding post counseling and support. Baby’s 300-g initial loss turned to gradual gain. However, mother developed postpartum cardiomyopathy on day 20, needing Torsemide, Cilnidipine, Carvedilol, and Sacubitril. Data scarcity rendered them unsafe for breastfeeding. 7 Breastfeeding paused for 3 days; undiluted cow’s milk supplemented. The baby was monitored for occasional side effects such as constipation and occult gastrointestinal bleed and also monitored for urine output during the alternative feed. Motivated for breastfeeding, mother carefully resumed breastfeeding at the high dependency unit, avoiding breastfeeding for 2 feeds after her meds, supplemented by stored milk. 8 Growth of the baby was followed up by regular weight checks which were positive. Mother’s condition improved, drugs tapered, and Carvedilol continued (safe). Discharged on day 30 with direct breastfeeding, 1.795 kg. Maternal motivation, drug knowledge, early breastfeeding, and no formula were vital in management.
Case 3
A 25-year-old mother with retro viral infection on anti-retro viral therapy (ART) for 6 years, delivered a 2.84-kg term male via vaginal birth. Immediately breastfeeding was started adhering to WHO guidelines. 9 Family hesitated, necessitating counseling with case references. Intensive counseling sessions were done with the whole family and few references of similar cases were given to them and then they were convinced to continue breastfeeding for next 2 years and following the correct ART guidelines of investigating both the mother and the baby at prescribed intervals. Regular ART for mother and baby’s prophylaxis was ensured. After 4 days of weight gain and maternal confidence, discharge followed.
Case 4
A 37-year-old morbidly obese mother (106 kg), with chronic hypertension on beta blockers and preeclampsia, delivered a late preterm SGA girl (1.86 kg) via LSCS. While the baby was stable, the mother’s uncontrolled hypertension led to MICU admission. Day 2 onward, trophic expressed milk fed, gradually increased, sometimes supplemented with donor milk per parents’ consent, aiming for calorie goal. Mother’s recovery enabled breastfeeding, observing weight gain up to day 14. Baby contracted with E. coli, Candida sepsis, aspiration pneumonia, and feed intolerance later. After 2-day partial parenteral nutrition with antibiotics, improvement led to resumed direct breastfeeding. Discharged with exclusive breastfeeding, supplemented expressed milk, and continuous lactation clinic support. She was followed up, and exclusive breastfeeding was ensured and emphasized until 6 months of age. The hospital strictly avoids artificial and ultra-processed feeds, promoting exclusive breastfeeding and discouraging early introduction of other milk sources.
Case 5
A 31-year-old primigravida delivered triplet females at 35 weeks (2 kg, 1.82 kg, and 1.94 kg) via LSCS. Mother was registered at the antenatal clinic and had received prenatal breastfeeding counselling. Babies began direct breastfeeding in high dependency unit, aided by nutritional guidance and hydration for the mother. Hospital stay was stable, leading to discharge with increasing weight gain trend. Regular lactation support addressed her queries time to time. Babies doubled birth weights around 5 months and exclusive breastfeeding was continued until 6 months. After 6 months, mother was advised on breastfeeding plus complementary feeding till 2 years, relying on strong motivation, family aid, breastfeeding technique knowledge, and consistent follow-ups. 10
Case 6
A 25-year-old first-time mother delivered very preterm twin females at 29 weeks (1.18 kg and 1.10 kg) via assisted vaginal delivery. Challenges included prematurity, twin gestation, and maternal inexperience. After counseling on multiple gestation feeding techniques, 11 breastfeeds began via nasogastric tube, gradually upgraded at the NICU. After establishing direct breastfeeding, both the babies were monitored at the high dependency unit in the NICU annex. Initial milk expression was limited; one of the twins had hypoglycemia, moved back to NICU, receiving direct breastfeeding and extra expressed feeds via a food feeder called paladai. Despite the initial decline, weight increased gradually. After 40 days, twins discharged at 1.42 kg and 1.41 kg, exclusively breastfeeding with cross-cradle hold technique.
Case 7
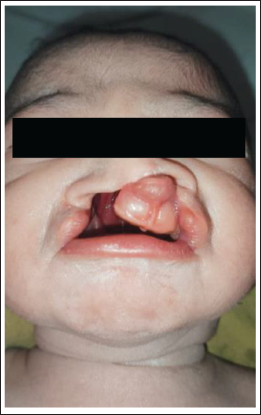
A 23-year-old mother delivered a 3-kg term girl baby with bilateral cleft lip and palate (Figure 1). Proper seal at the nipple was challenging due to the facial clefts. 12 Counseling focused on cross-cradle technique, elevating baby’s head, initially facing seal formation issues. Elevating babies head and queries regarding the nipple and palate seal formation issues were addressed. Overtime, the baby learned to latch, incorporating more areola, and nipple contributed to superior seal at the hard palate. Referral for corrective surgery followed. Mother’s understanding of breastmilk benefits, drawbacks of top feeds, consistent latching assistance, and lactation clinic support were key factors in successful breastfeeding.
Newborn with Bilateral Facial Clefts Given Direct Breastfeeds.
Case 8
This case involves a primiparous mother who was presented with no milk output from her right breast after delivering a term baby weighing 2.62 kg at a different hospital. Breastfeeding began within 2 hours, revealing milk expression only from 1 breast. Past history included an adolescent breast abscess in the mother. Examinations and tests, including blood work and prolactin levels, were conducted. Ultrasonography and sonomammography indicated minimal glandular structure on the affected side. Despite a duct dilation procedure, milk output did not improve. Exclusive breastfeeding on the normal breast increased in frequency, as it can adapt to provide adequate nutrition. 13 As per the advice and motivation, the mother continued exclusive breastfeeding from 1 breast, observing baby’s weight gain for 4 months. Later, 1 or 2 undiluted cow’s milk feeds were introduced. Regular follow-up led to doubling birth weight at 5 months. Unilateral glandular dysfunction, potentially post mastitis,14, 15 was suspected, and biopsy was suggested but not pursued by the mother. Lactation clinic support assisted the mother throughout her breastfeeding journey, extending to complementary feeding after 6 months.
Case 9
This case involves a mother with uncomplicated antenatal period, giving birth to a healthy term girl weighing 3.74 kg. However, her colostrum, starting on day 2, appeared reddish brown (Figure 2). Anxious and uncertain about breastfeeding, she experienced a rare instance of “rusty pipe syndrome.” 16 After counseling and sharing comparable cases from other hospitals, her concerns eased. Rusty pipe syndrome is a benign condition neither calling for panic nor discontinuation of breastfeeding. The reddish hue disappeared within a day, replaced by normal-colored milk. The baby consistently gained weight and was discharged in good health on day 5.
Reddish Brown Colored Colostrum Secreted by Mother on Day 2 of Life.

Discussion
Early initiation of breastfeeding (EIBF) decreases the risk of neonatal mortality. This helps by preventing chances of infection by reducing prelacteal feeds, decreases risk of hypothermia and hypoglycemia in newborn, and helps better breastmilk secretion rates due to suckling early. The recent Indian National Family Health Survey (NFHS-5) data suggest that the rate of EIBF within 1 hour of birth was just 41.8%. 3 The major reasons for this delay could be due to cesarean births, receiving delivery assistance from non–health professionals, maternal medical/surgical complications, baby’s medical/surgical conditions, mother’s hailing from rural areas, social factors, or lack of awareness in mothers. 17 And the key modifiable factors that could facilitate in EIBF were higher maternal educational achievement, mothers who had frequent health service contact, frequent antenatal care visits, and birthing in a health facility. 17 Breastfeeding can present with various complicated scenarios wherein it becomes very necessary to individualize counseling based on the needs and appraising the mother early on regarding the EIBF. After discharge, many mothers tend to start top feeds with other milk sources as they feel or are told that the growing baby’s needs are not met by only with breastmilk. The NFHS-5 data suggest that only 63.7% of mothers continue the exclusive breastfeeding up to 6 months. 3 Getting this cohort of mothers who do not breastfeed into loop and advising them to continue exclusive breastfeeding for 6 months of life becomes the next most important thing in the whole counseling process. The hospital adheres to the baby-friendly hospital initiative, enhancing EIBF rates and exclusive breastfeeding duration. It operates a lactation clinic, strictly following WHO-BFHI guidelines, pursuing accreditation from the Breastfeeding Promotion Network of India (BPNI). This clinic, supervised by BPNI and MIYCN-certified counselors and support staff, offers daily services. Regular capacity-building programs are provided for the staff, with a focus on BPNI lactation provider course training. Mothers receive counseling through breast and baby models, demonstrations, and health spoken tutorial videos in the local language made by IIT Bombay, addressing breastfeeding questions and challenges. Follow-up visits during vaccinations include lactation counseling, and the high-risk mothers are monitored more frequently. The supplementation of undiluted animal milk instead of formula feeds for a brief period when the mothers were unable to directly feed the baby comes with the notion our hospital follows wherein human food should be as unprocessed as possible, and it must be organic and natural. The locally available animal milk, undiluted, directly procured and boiled animal milk or prepacked pasteurized milk (toned, having 3% fat, 3.1% protein, and providing 58 kcal/100 ml) is also advocated by the Nutritional Guidelines for Infants by NACO and the Infant and Young Child Feeding (IYCF) Guidelines of 2010 of Indian Academy of Pediatrics, as it is easily available, economical, and culturally acceptable. 18 These infants can be supplemented by additional nutrient supplements to meet the requirements. The possible complications anticipated with the animal milk are not significantly different from the commercial formula. 19 Hence, unmodified animal milk is preferred over formula as an alternative in rare scenarios of breastmilk nonavailability. The conclusion is to propose targeted and well-coordinated infant feeding policies, and interventions at institution levels, the coordination of public and private sectors, and continued care beyond hospital stay with transition care can improvise the whole breastfeeding experience and outcome in both the mother and the infant.
Consent to Publication Statement
Informed written consent for the publication of clinical photographs/material, from the legal guardian of the patient with an understanding that every effort will be made to conceal the identity of the patient.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Ethical Approval
The Institutional Ethical Committee of CDSIMER, Dayanada Sagar University has approved the case series in the meeting held on August 8, 2023 (the official certificate of approval is in process to be received).
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Human and Animal Welfare Statement
No humans or animals were harmed in this study.
Patient Perspective
Mothers were happy to share the information and were cooperative with the whole counseling and training process.
