Abstract
Introduction
Lactation education is an integral part of healthcare. In order to recognise and address the inconsistencies in perceptions, attitudes and delivery of lactation care, we developed the Lactation Aids and Milk Banking (LAMB) survey.
Aim
The purpose of the study was to compare the knowledge, attitude and practices of doctors and nurses about human milk banking and lactation aids and to examine institutional and individual barriers to and facilitators of the delivery of lactation care.
Methods
It was a cross-sectional study, and the survey questionnaire was administered electronically to neonatal physicians and nurses in a tertiary care hospital in India.
Results
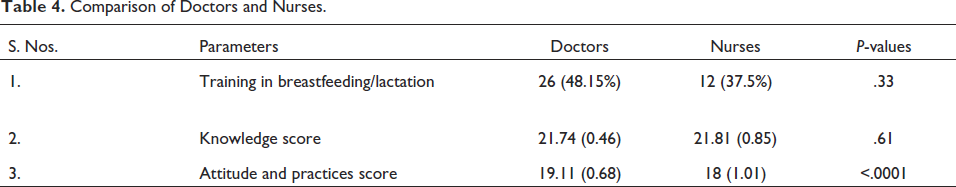
There were 86 participants, including 54 doctors (63%) and 32 (37%) nurses. There was no significant difference in the knowledge score of doctors and nurses (p = .61), although doctors scored significantly higher on the attitude and practices score as compared to nurses (p < .0001). Amongst the doctors, the knowledge score was higher for faculty than residents (p < .0001), though residents scored significantly higher on the attitude and practices score than faculty (p = .0002). This study highlighted five facilitators and two barriers to LAMB and also revealed that physicians and nurses have relatively inadequate knowledge about lactational aids and milk banking.
Conclusion
Lactation education for staff can reinforce support for milk banking and lactation aids, thereby achieving the goal of exclusive breastfeeding. It is also important to mitigate barriers by establishing policies and guidelines in the unit for milk banking and the use of lactation aids.
Keywords
Introduction
When breastfeeding discomfort occurs and infants have difficulty latching on to the breast or gaining weight, interventions might be necessary to correct the cause. The role of medical professionals is to identify the potential cause of the problem and to offer intervention options to remedy the situation. When additional intervention is needed, specific devices and equipment might be helpful to achieve the goal of establishing breastfeeding as soon as possible.
Lactation aids include breast pumps, nipple shields, special needs feeders, nipple everters and supplemental nursing systems. Breast pumps help to maintain milk production when the breastfeeding dyad is separated. 1 A nipple shield is a device that a mother places over her nipple-areolar surface prior to nursing to help the baby latch onto the breast. It is used for sore or cracked nipples, flat nipples, oversupply, and to facilitate the infant’s attachment to the breast2 and is perceived as a short-term solution to help with the initiation of breastfeeding. 3 Supplemental nursing systems are useful for induced lactation and relactation,4-6 whereas special needs feeders are useful for babies with cleft lip and palate. 7
The World Health Organization (WHO) recommends donated human breast milk as the best alternative when a mother’s breast milk is unavailable.8–10 The knowledge of breast milk donation and human milk banking is suboptimal, and there is a need to educate and create awareness in this aspect. 11
Lactation education has not yet been completely integrated into medical and nursing practice, and there are inconsistencies in attitudes towards and delivery of lactation care. Implementing milk banking and lactation aids requires a multidisciplinary, collaborative effort.
The purpose of the study was to learn how caregivers feel about certain situations in which they are involved with milk banking and lactation aids. To examine institutional and individual barriers to and facilitators of the delivery of lactation care, we developed the Lactation Aids and Milk Banking (LAMB) Survey, which was administered to neonatal physicians and nurses in our institution. To our knowledge, this is the first survey to compare the lactation care perceptions of both medical providers and nurses in low- and middle-income countries (LMICs).
Aim
This study was designed to determine the level of knowledge and understanding of the principles of milk banking and lactation aids by medical and nursing staff involved in neonatal care and to describe the current practices in public hospitals caring for neonates.
Study Design and Setting
A web-based survey was conducted in the Department of Paediatrics at a tertiary care hospital in India.
Methods
This study was a questionnaire-based prospective cross-sectional study conducted over a period of one month. Institutional Review Board approval was not sought because the study was conducted to understand the lacunae in knowledge, attitude and practices of healthcare professionals so as to improve lactation care delivery in our institution. Furthermore, the survey did not collect personal information from the participants. Participation in the survey was voluntary and anonymous, thus completing the questionnaire indicated consent. The participants were invited to complete the survey by distributing it electronically, with the online version being hosted and stored on Google Forms. The survey was open for a one-month period in January 2023.
Data was collected through a structured and validated questionnaire from 86 participants working with neonates in the paediatrics department, which included 54 doctors and 32 nurses. Doctors included faculty and residents (postgraduate students and senior residents), while nurses comprised nursing staff and nursing students. The questionnaire was framed by the principal investigator of this study, who is a neonatology expert and International Board Certified Lactation Consultant (IBCLC). A pilot study was conducted in the study setting on a test sample of 10 doctors and nurses as a preliminary exercise. Cronbach’s alpha was used to validate the questionnaire. The value of coefficient alpha was 0.75 from the data obtained from the pilot study, which indicates good internal consistency.
Participants’ knowledge of LAMB was scored as 0–29 for the set of 29 questions, with correct answers scored as 1 and incorrect answers marked 0. For attitude and practice, the scoring was based on 13 questions. Answers were categorized as agree (Score = 2), neutral response (Score = 1) and disagree (Score = 0), except question 42, which was scored as agree (Score = 0), neutral response (Score = 1) and disagree (Score = 2). The total score range was thus 0–26.
Inferential statistics included P-values generated from hypothesis testing procedures. Overall responses were compared by the qualification of the respondents in two groups, that is, doctors (n = 54) versus nurses (n = 32). Then, an intragroup analysis was also performed to compare responses across two categories in the doctors’ group (i.e., faculty [n = 9] versus residents [n = 45]).
Various measures were taken to alleviate bias in the survey design and responses. To reduce non-response bias, we made the survey anonymous, sent reminder emails for those who had not responded, and allowed the respondents enough time to complete the survey. To mitigate acquiescence bias, we did not use any leading questions, varied the questions and answers between multiple choice and scale questions, and allowed the respondents enough time to answer the survey. To eliminate primacy bias, recency bias and end aversion, we randomised the order of options and scales presented in the answers. To reduce conformity bias, we made the survey anonymous. The questionnaire was pretested to avoid problems due to flawed questionnaire structure like inappropriate wording, missing data, improper formatting and leading questions.
Statistical Analysis
All data was analysed using the SPSS version 16 statistical package. Continuous variables with a normal distribution were analysed by a two-sample t-test. Categorical data were assessed using the Fischer exact test. A P-value of <.05 was considered statistically significant. A chi-square test was performed to test difference in proportions for question-wise responses in the above independent groups.
Results
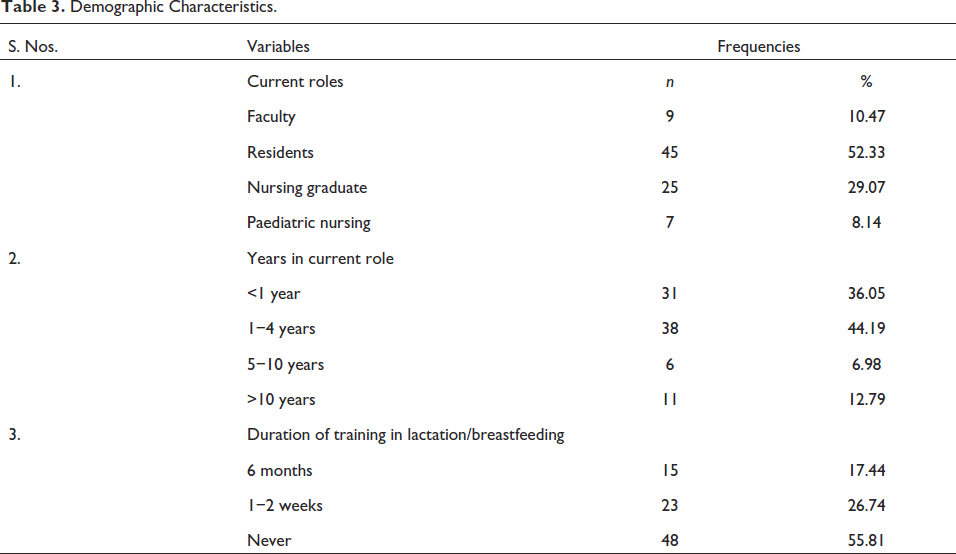
Of the 93 neonatal medical and nursing staff surveyed for this study, 86 completed the questionnaire, resulting in a response rate of 92%. A total of 86 participants took part in the survey, of whom 54 were doctors (63%) and 32 (37%) were nurses. Out of 86 total participants, 45 doctors were undergoing training as junior and senior residents, comprising 52.33% of the study population. The remaining 9 (10.47%) respondents were consultant paediatricians (faculty). Among the nursing staff, 25 (29.07%) were nursing graduates, while 7 (8.14%) had a specialization in paediatric nursing. Around 36.05% had work experience of less than 1 year, 44.19% had experience of 1–4 years, 6.98% had experience of 5–10 years and 12.79% had worked for more than 10 years. Nearly half of respondents had experience of 1–4 years in their current role.
The majority of survey respondents indicated they had experience with breastfeeding or lactation. In our survey population, medical staff (75.93%), compared with nursing staff (68.75%), reported more experience in providing lactation counselling to nursing mothers (p-value = .47). Nearly all respondents agreed that LAMB care was necessary in neonatal nursing and medical education, but less than half of all respondents (38 [44.18%]) had received education or training in the subject, of which 15 (17.44%) had received training for about 6 months and 23 (26.74%) had received training for a duration of 1–2 weeks.
Tables 1 and 2 describe responses to all questions by doctors and nurses. Table 3 shows the demographic characteristics of the participants. Table 4 compares the scores of doctors and nurses.
Intergroup Comparison of Knowledge Between Doctors and Nurses.

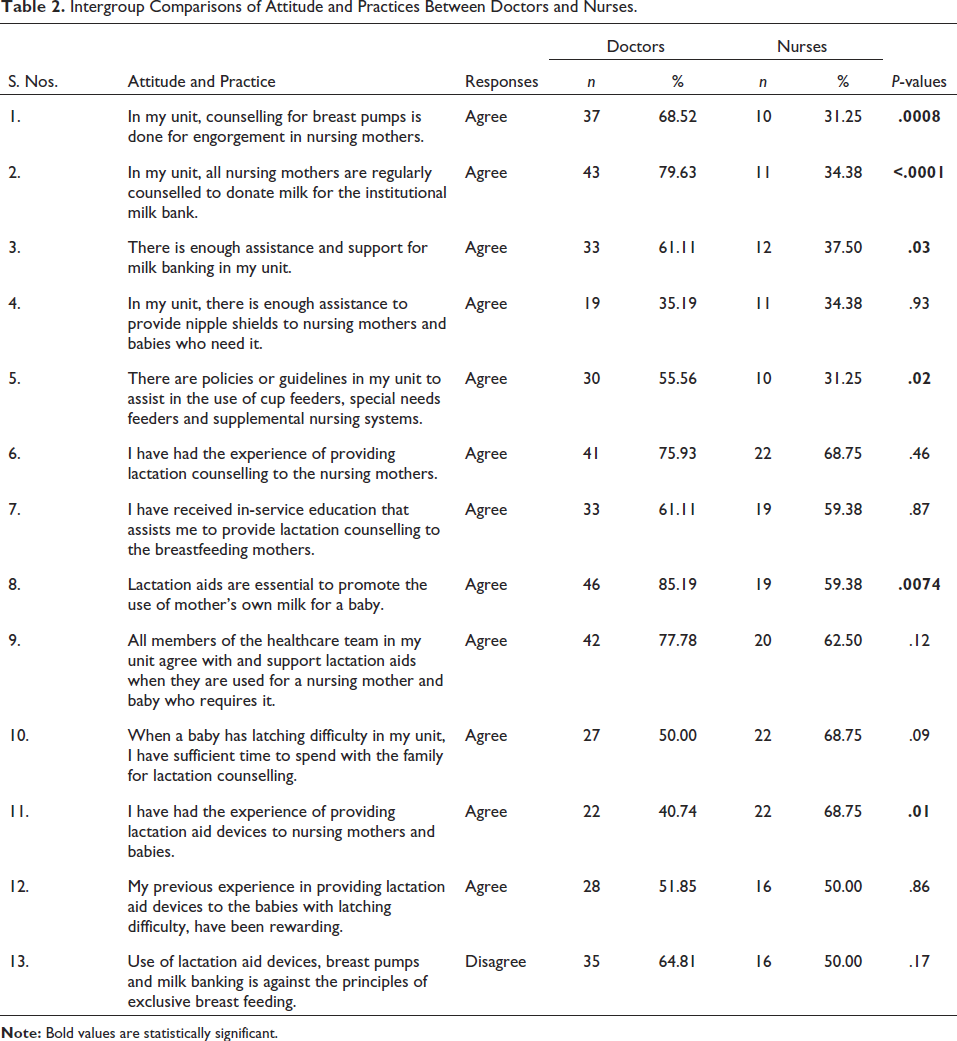
Intergroup Comparisons of Attitude and Practices Between Doctors and Nurses.
Demographic Characteristics.
Comparison of Doctors and Nurses.
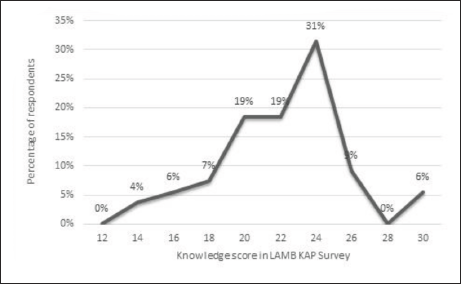
Knowledge of Lactation Aids and Milk Banking
The study included 29 questions on knowledge regarding LAMB. About 85% (n = 46/54) doctors and 87.5% (n = 28/32) nurses were aware of the existence of a milk bank in the hospital. Among the study population, 75.9% of doctors and 84.3% of nurses recognised the role of Feedback Inhibitor of Lactation (FIL) in engorged breasts. A total of 90.74% of doctors (n = 49/54) and 87.5% of nurses (28/32) knew that the minimum prescribed strength for a Comprehensive Lactation Management Centre (CLMC) is a 20-bed Neonatal Intensive Care Unit (NICU). The optimal space requirement for a CLMC was known to 87% of doctors and 90.6% of nurses. A total of 50% of doctors and 87.5% of nurses felt that electric breast pumps should be used in milk banks. Only 51.8% of doctors and 87.5% of nurses were aware that the Low Temperature Low Time (LTLT) method of pasteurisation is used in milk banks, which was a significant difference.
The majority of the study participants agreed that breast milk expression should be done a minimum of eight times during the day. A total of 72% of doctors and 56% of nurses believed that hospital-grade pumps are closed-system pumps.
In the initiation phase of pumping, cycles should be set high and suction should be set low. This question was correctly answered only by 42.6% of doctors and 34.3% of nurses, thereby reflecting inadequate knowledge about the operation of breast pumps. Around 75.9% of doctors and 53.1% of nurses opined that different mothers have a requirement for different flange sizes. Only 64.8% of doctors and 43.7% of nurses were aware that bilateral pumping is more efficacious than unilateral pumping.
It is very important to have a proper storage container for storing pasteurised milk. Milk containers should be bisphenol A (BPA) free was known to 94.4% of doctors and 90.6% of nurses, while 64.8% of doctors and 71.8% of nurses were aware of the recommendations for stainless steel containers.
Only 40.7% of doctors and 37.5% of nurses knew about the nutrients preserved during pasteurisation. Most of the doctors and nurses agreed that raw milk can be stored for 24 h at room temperature and pasteurised milk can be stored for 6 months at −20°C. Most of the respondents answered correctly regarding post-pasteurisation testing, thawing and dispensing of donor human milk. Most people knew about the role of nipple shields in preterm babies.
Only 27.78% of doctors and 31.25% of nurses felt that the syringe method was a comfortable way to correct inverted nipples. Most respondents felt that the smallest-sized nipple shield, which gives the best result, should be selected. Thin silicone shields were preferred by most as they allow tactile stimulation to the nerves of the nipple and areola. Most professionals warm the nipple shield before application so as to improve adherence, which is a good practice.
Most respondents agreed that cup feeding is better than spoon feeding in terms of pacing the feeds and helps in an easier transition to breastfeeds. The role of the special needs feeder in cleft lip and palate was correctly answered by most. Only 74% of doctors and 62.5% of nurses responded that a supplemental nursing system can be used for induced lactation.
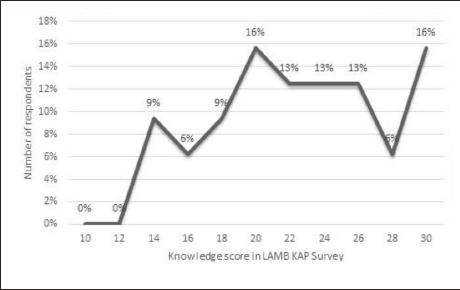
The knowledge score distribution of doctors (Figure 1) revealed that 55% of all doctors had a score between 12 and 22, while 45% had a score above 22, with a mean of 21.74 and a median value of 22 out of 29. The score distribution of nurses revealed that around 40% had a score below 22, while the remaining 60% had a score above 22 (Figure 3).
Knowledge Score of Doctors Regarding Human Milk Banking and Lactation Aids.
Attitude and Practices Score of Doctors Regarding Human Milk Banking and Lactation Aids.
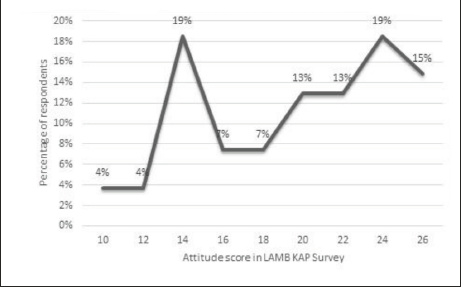
Knowledge Score of Nurses Regarding Human Milk Banking and Lactation Aids.
The intergroup comparison between doctors and nurses (Table 1) on knowledge regarding LAMB showed no significant difference except for the knowledge of the breast pump and its flange size or the method of pasteurisation used (P = .0009). Intragroup comparisons between faculty and resident doctors revealed comparatively higher scores in the faculty group, with faculty showing comparatively higher knowledge regarding milk banking. Significantly more faculty as compared to residents felt that the syringe method was a more comfortable method of breastmilk expression. The intragroup comparison between paediatric nursing and nursing graduates showed no significant difference.
Attitude and Practices Regarding Lactation Aids and Milk Banking
Thirteen questions regarding attitude and practices with possible responses of agree, disagree or neutral were compiled to obtain a score with a range of 0–26. The response recorded is presented graphically (Figures 2 and 4).
Attitude and Practices Score of Nurses Regarding Human Milk Banking and Lactation Aids.
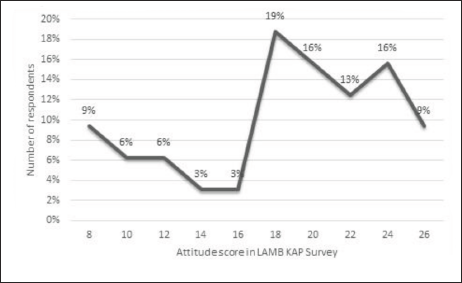
With a mean of 19.1 and a median of 20, 27% of physicians scored <14, 27% had a score between 14 and 20, and 47% had a score of positive attitude of >20 (Figure 2).
A significantly higher number of doctors reported having done counselling for engorgement in nursing mothers (p = .008). Around 68.5% of doctors and 31.2% of nurses said that counselling for engorged mothers is done regularly in the unit (p <.0001).
There was a weak level of agreement among both medical and nursing respondents that the healthcare team supports LAMB. Significantly more doctors than nurses opined that there is enough support for milk banking in the unit (p = .0352). Only one-third of doctors and nurses believed that there was enough assistance for nipple shields for nursing mothers in the unit. A total of 55.5% of doctors and 31.2% of nurses agreed that there are policies or guidelines in their unit to assist in the use of cup feeders, special needs feeders and supplemental nursing systems (p = .0299).
Around 75.9% of doctors and 68.7% of nurses said that they had experience of providing lactation counselling to nursing mothers. A total of 61.1% of doctors and 59.3% of nurses said that they have received in-service education that assists them in providing lactation counselling to breastfeeding mothers. More doctors (85.2%) than nurses (59.38%) believed that lactation aids are essential to promoting the use of a mother’s own milk for a baby (p = .0074).
A total of 77.8% of doctors and 62.5% of nurses felt that they had sufficient time to spend with a family for lactation counselling. Only 40.7% of doctors and 68.7% of nurses said that they had the opportunity to provide lactation aid devices to nursing mothers and babies (p = .0125). Almost half of the doctors and nurses agreed that their previous experience in providing lactation aid devices to babies with latching difficulties had been rewarding. A total of 64.8% of doctors and 50% of nurses disagreed with the view that the use of lactation aid devices, breast pumps and milk banking is against the principles of exclusive breast feeding.
Intragroup analysis was done to compare faculty (consultant paediatricians) (n = 9) versus residents (n = 45) (Tables 3 and 4), and paediatric nursing (n = 7) versus nursing graduates (n = 25). No significant difference was found between the study groups.
There was no significant difference in the knowledge score of doctors and nurses (p = .61), although the score was higher for faculty as compared to residents (p < .0001). Nursing graduates scored significantly higher than paediatric nursing graduates (p = .0001). Doctors scored significantly higher on the attitude and practices score as compared to nurses (p < .0001). Amongst the doctors, residents scored significantly higher on the attitude and practices score than faculty (p = .0002), whereas paediatric nursing graduates and nursing graduates had similar responses.
Discussion
There is a paucity of studies on the perceptions of healthcare professionals towards milk banking and lactation aids, and we believe that ours is the first knowledge, attitude and practice survey in this regard. The survey questionnaire is a novel way of analysing the difficulties in attaining the proper execution of milk banking and lactation aid devices to realise the objective of exclusive breastfeeding. The response rate in the survey was excellent (92%). Our study revealed that physicians and nurses have relatively inadequate knowledge about lactational aids and milk banking. Only 55% of doctors and 87.5% of nurses were aware of the method of pasteurisation used in human milk banks. Hence, creating awareness regarding milk banking and lactation aids amongst treating physicians and nurses is required for the well-being of newborns and nursing mothers.
Only 42.5% of doctors and 34.3% of nurses knew about the settings of breast pumps. The knowledge regarding the preservation of nutrients during pasteurisation was quite poor, with only 40.7% of doctors and 37.5% of nurses being aware of nutrients preserved during pasteurisation. Although knowledge regarding the storage and dispensing of milk was quite adequate, medical staff should be cognisant of the operation and execution of breast pumps in order to provide guidance to mothers regarding their use for expression of milk in situations when a baby is unable to breastfeed or if there is a mother-baby separation.
The syringe method for eversion of inverted nipples is not considered an ideal remedy for inverted or flat nipples because vigorous nipple eversion may lead to nipple trauma, sore nipples and nipples may not remain everted long enough for the infant to achieve a latch. 12 There is also inadequate research on nipple evertors. 12 Only 27.78% of doctors and 31.25% of nurses felt that the syringe method was a comfortable way to correct inverted nipples.
Nursing staff disagreed about the presence of policies or guidelines in the unit, while doctors responded positively (p-value = .0299). Knowledge regarding lactation aids was variable, with most responses averaging 70%−80%, except for the knowledge regarding supplemental nursing systems. This data highlighted the areas with scope for further improvement in the knowledge of medical professionals. The attitude and practices of physicians are guided by their knowledge, which reflects a positive attitude related to the counselling of nursing mothers, milk banking and lactation aids.
The findings from this research highlight five facilitators for LAMB: (1) support by the healthcare team; (2) support by medical and nursing personnel; (3) agreement that a mother’s own milk is as important as curative care; (4) recognition of the importance of lactation education and (5) prioritising breastfeeding.
There were two barriers identified: (1) assistance by medical and nursing personnel and (2) policies and guidelines to assist in the use of lactation aids. Based on this, we advocate ample emphasis on in-service lactation education for medical and nursing personnel involved in neonatal care. We also endorse the establishment of formal guidelines in all units to guide milk banking and the handling of lactation aids.
The strength of this study is that it is the first to utilise a validated survey to compare perceptions about LAMB between medical and nursing staff. Additionally, the response rate was good. The limitations of this study are the small sample size and the limitation to a single centre. The survey instrument in our study was closed-ended, which limited participants’ opportunity to express their opinions that were different from the options we provided.
Differences Between Medical and Nursing Staffs’ Attitudes
Medical staff had statistically significant negative perceptions regarding multiple resource-related items: assistance from peers and the ability to spend time with nursing mothers in need of lactation support.
A study from Iran reported that the knowledge and attitude of healthcare providers were moderately influential in breast milk donation. Healthcare providers can provide education and a positive atmosphere for specialised training for the general public, and their efforts to improve their knowledge and attitudes can contribute to the acceptability of a milk bank in the community and a reduction in the rate of neonatal mortality .13
A systematic review of intervention studies focusing on increasing the breastfeeding knowledge, self-confidence, and supportive behaviours of healthcare professionals reported that breastfeeding education is effective in increasing the knowledge and confidence of nurses .8,14
Another study reported that medical students with more years of training are the most prepared to assist and counsel in newborn feeding. 15 A more supportive workplace provides a greater level of confidence and psychosocial support for healthcare workers. A systematic review from Sub-Saharan Africa identified the facilitators for exclusive breastfeeding, which included positive caregiver and health worker attitudes, knowledge and support during the postpartum period. 16 Improper attitudes can be rectified by guidance and in-service educational programmes.
Conclusion
This study identifies gaps in the knowledge of physicians and nurses about human milk banking and lactation aids. It is essential to create adequate awareness at all levels of the healthcare system through lactation education to reinforce support for exclusive breastfeeding. Several facilitators and barriers to LAMB were identified, implying that facilitators should be strengthened. It is also important to mitigate barriers through the establishment of policies and guidelines in the unit to help in the proper use of milk banking and lactation aids to support the maximum use of mother’s milk in situations where it is not possible to achieve direct breastfeeding.
Abbreviations
BPA: Bisphenol A; CLMC: comprehensive lactation management centre; FIL: Feedback inhibitor of lactation; HTST: High temperature short time; IBCLC: International board certified lactation consultant; LAMB: Lactation aids and milk banking; LMIC: Low and low middle income countries; LTLT: Low temperature long time; NICU: Neonatal intensive care unit; WHO: World Health Organization.
Author Contributions
SS will be the guarantor for this manuscript and will take responsibility for the integrity of this article. All the authors have substantial contributions to each of the following three components: (1) concept and design of study or acquisition of data or analysis and interpretation of data; (2) drafting the article and (3) final approval.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
Not applicable
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
