Abstract
Background
Oral cancer is a major type of head and neck cancer that mostly affects the lips, tongue, buccal mucosa, and salivary glands. It is a malignant tumor affecting the oral cavity with an annual incidence of over half a million new cases.
Objectives
The major aim of the current work is to evaluate the anti-cancer potential of marrubiin against oral cancer KB cells.
Materials and Methods
The effect of marrubiin (2.5–160 µg/mL) on KB cell growth was assessed by the MTT assay. The mitochondrial membrane potential (MMP) and apoptosis in the marrubiin-treated and control cells were studied using respective fluorescent staining assays. The angiogenic marker vascular endothelial growth factor (VEGF) and inflammatory cytokines tumor necrosis factor-α (TNF-α) and Interleukin-6 (IL-6) levels were studied using the assay kits.
Results
The MTT assay results prove that the marrubiin treatment effectively decreased KB cell growth dose-dependently. The treatment of marrubiin at an inhibitory concentration (IC50 33.15 µg/mL) effectively induced apoptosis and reduced MMP levels in the KB cells. The VEGF, TNF-α, and IL-6 levels were effectively reduced in the KB cells after treatment with the IC50 concentration of marrubiin.
Conclusion
The present results demonstrate that marrubiin inhibits cell viability and promotes apoptosis in KB cells via decreasing VEGF and inflammatory cytokine levels. Thus, it holds potential as a promising anti-cancer agent for treating oral cancer.
Introduction
Oral cancers are the most prevalent types of malignancies, with approximately 90% of cases being classified as squamous cell carcinomas based on their histological characteristics (Chamoli et al., 2021). Unfortunately, the predicted overall survival percentage for oral squamous cell carcinoma (OSCC) after 5 years is only around 50%. The origin of this cancer is multifaceted, originating from alterations in the mucosa and progressing into tumor lesions and, ultimately metastasis (Ren et al., 2020). The excessive consumption of alcohol and the intake of tobacco are recognized as the primary risk factors for oral cancer due to their pro-inflammatory properties.
Specifically, the act of smoking tobacco results in the production of chemical substances such as benzopyrenes and nitrosamines. These molecules have the effect of reducing the immunological response in the mouth and damaging the deoxyribonucleic acid (DNA) of cells, which in turn promotes the development of cancer (Sarode et al., 2021). As a result, during the initial stages of carcinogenesis, certain abnormalities manifest in the epithelium. It is widely acknowledged that the progression of OSCC is intimately linked to various inflammatory cascades (Siriwardena et al., 2020). Regrettably, OSCC is predominantly detected during an advanced stage, severely decreasing the chances of survival and decreasing the life quality of patients. Hence, the effectiveness of OSCC therapy relies on a timely and suitable method during the initial phase of the tumor (Dumache, 2017).
Treatment methods for oral cancer include surgical intervention, radiotherapy, chemotherapy, or a combination of these techniques. Chemoprevention is a potential approach, as it has been shown that timely therapy of the early stages of tumors can have a positive impact on the cancer-causing pathways (Mohan Shankar et al., 2022). The various drug types, including anti-estrogens, anti-androgens, anti-inflammatories, and vitamins, are employed as chemopreventive agents. However, these approaches are frequently aggressive, leading to a decrease in patients’ quality of life. Additionally, they often do not result in satisfactory survival rates. The 5-year survival rate continues to be lower, even with recent advancements in therapy and diagnosis (Deshmukh & Shekar, 2021). Hence, it is crucial to identify a novel therapeutic approach using organic compounds that have minimal adverse effects, which is essential for inhibiting the rapid growth and metastasis of tumors as well as enhancing the survival rate and life quality of cancer patients.
Phytochemicals have been proven to be effective with poor adverse effects and cost-effectiveness (Koh et al., 2020). Marrubiin, an important diterpenoid lactone, is a significant component of various medicinal plants, including Marrubium vulgare and Leonotis nepetifolia. These plants are widely utilized to treat various ailments in various countries. The biological properties of marrubiin as an anti-inflammatory, vasorelaxant, and antioxidant have been well documented (Popoola et al., 2013). Furthermore, several previous studies also highlighted that marrubiin has neuroprotective, anti-atherosclerotic, cardioprotective, and anti-diabetic properties (Nakhlband et al., 2023; Singh et al., 2022). However, the anti-cancer properties of marrubiin have not been discussed yet. Therefore, the main aim of the present work is to study the anti-cancer effects of marrubiin against oral cancer KB cells.
Materials and Methods
Chemicals
Marrubiin, Dulbecco’s modified Eagle medium (DMEM), dimethyl sulfoxide (DMSO), acridine orange/ethidium bromide (AO/EtBr), rhodamine-123 (Rh-123), fetal bovine serum (FBS), and so on, were purchased from Sigma–Aldrich, USA. The ELISA-based assay kits for biochemical assays were purchased from Elabscience, USA.
Collection of KB Cells
The KB cells were purchased from ATCC, USA, and cultivated in a DMEM medium with 10% FBS and a 1% anti-mycotic mixture. The cells were grown at 37°C with 5% carbon dioxide (CO2) in a humidified chamber.
Cytotoxicity Assay
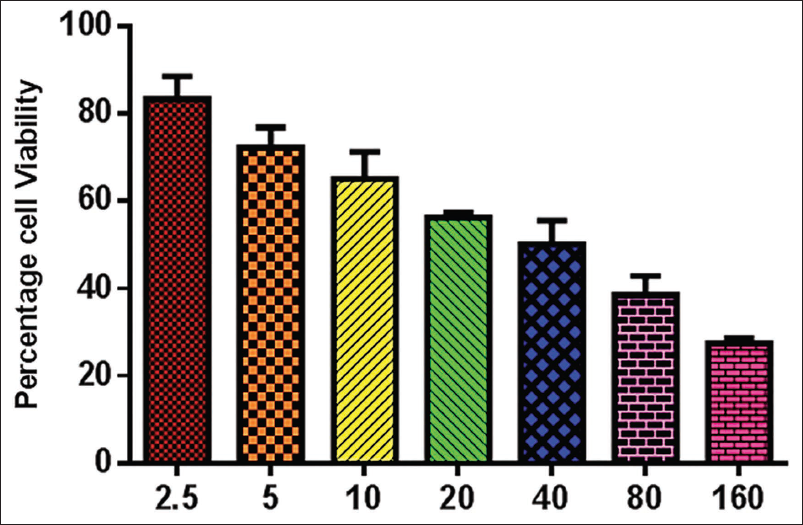
The MTT viability assay was performed to study the cytotoxicity of marrubiin on the KB cells. The KB cells were grown on a 96-well plate for 24 h. Subsequently, cells were exposed to various dosages of marrubiin at 2.5, 5, 10, 20, 40, 80, and 160 µg/mL for 24 h. Subsequently, the MTT reagent was mixed into wells and incubated for an additional 4 h. Subsequently, a 100-µL aliquot of DMSO was mixed into each well to liquefy the formed formazan deposits. The viability was studied by examining the plate at 570 nm.
Dual Staining
The dual staining procedure was conducted to identify the occurrence of both early and late apoptosis in both marrubiin-treated and control cells. In this experiment, cells were treated with marrubiin at an inhibitory concentration (IC50) for 24 h. Then the cells were subjected to staining with AO/EtBr dye (1:1 ratio) at 100 µg/mL concentration for 5 min. Later, the fluorescence microscope was employed to measure the fluorescence intensity.
Mitochondrial Membrane Potential (MMP)
The level of MMP in the marrubiin-treated and control KB cells was studied by the Rh-123 staining assay. The KB cells were cultivated on a 24-well plate for 24 h and then exposed to marrubiin at a concentration of IC50 for 24 h. Later, the cells were stained with a concentration of Rh-123 (10 µg/mL) for 30 min. Finally, the MMP level in the cells was determined using a fluorescent microscope.
Analysis of Vascular Endothelial Growth Factor (VEGF) Levels
The levels of VEGF in the marrubiin-treated and control cells were analyzed using an assay kit. The assays were performed in triplicates, following the protocols recommended by the manufacturer (Elabscience, USA).
Analysis of Inflammatory Cytokine Levels
The tumor necrosis factor-α (TNF-α) and IL-6 levels in the marrubiin-treated and control cells were analyzed using marker-specific assay kits. The assays were performed in triplicates, following the manufacturer’s instructions (Elabscience, USA).
Statistical Analysis
The data are analyzed using GraphPad Prism, and the results are illustrated as the mean ± SD of triplicates, which are studied by one-way analysis of variance (ANOVA) and Duncan’s multiple range test (DMRT). The significant level was fixed at p < .05.
Results
Effect of Marrubiin on the KB Cell Viability
The marrubiin-treated and control cell viability was investigated by an MTT assay, and the results are presented in Figure 1. Marrubiin treatment at various concentrations (2.5–160 µg/mL) significantly decreased the KB cell viability. The higher dosage of marrubiin treatment on the KB cells leads to a considerable decrease in cell viability. The IC50 dosage of marrubiin was determined to be 33.15 µg/mL, resulting in a 50% inhibition of cell viability. Therefore, the concentration of 33.15 µg/mL of marrubiin was chosen for further assays as the IC50 dosage.
Effect of Marrubiin on the Apoptosis in the KB Cells
The induction of apoptosis in the marrubiin-treated and control KB cells was examined using AO/EtBr dual staining (Figure 2). The KB cells showed a higher rate of apoptotic cell death after treatment with marrubiin than the control. The fluorescence level of yellow/orange fluorescence in the KB cells treated with 33.15 µg/mL of marrubiin demonstrated a drastic elevation than the control (Figure 2). This provides evidence for the enhanced apoptosis in KB cells caused by marrubiin.
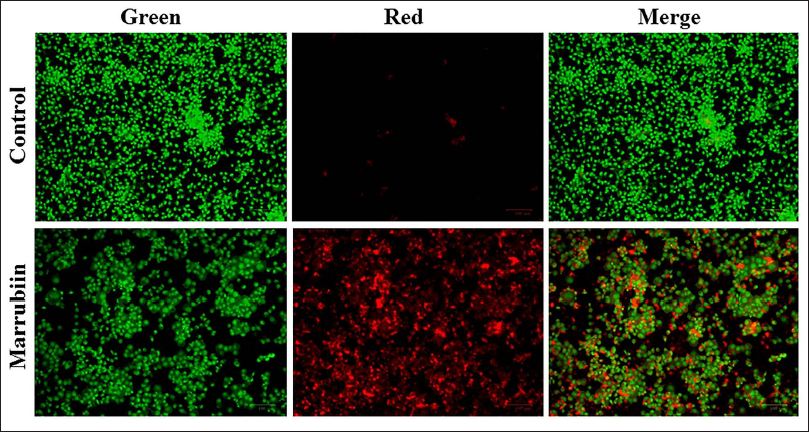
Effect of Marrubiin on the MMP Level in the KB Cells
The impacts of marrubiin on the MMP level in the KB cells were examined using Rh-123 staining. The outcomes are presented in Figure 3. The treatment of marrubiin at a dosage of 33.15 µg/mL significantly reduced the MMP in the KB cells compared to the control. The KB cells, after treatment with 33.15 µg/mL of marrubiin, exhibited reduced green fluorescence than the control, demonstrating a reduction in MMP levels.
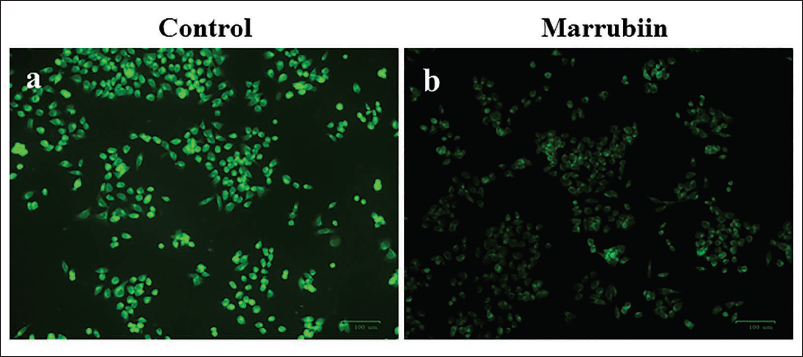
Effect of Marrubiin on the VEGF Level in the KB Cells
The influence of marrubiin on the level of VEGF was examined using an assay kit, and the findings are given in Figure 4. The level of VEGF exhibited a remarkable reduction in KB cells after treatment with 33.15 µg/mL of marrubiin, compared to the control. The findings demonstrated that marrubiin enhanced the reduction of VEGF levels, which may promote the inhibition of angiogenesis in the KB cells.
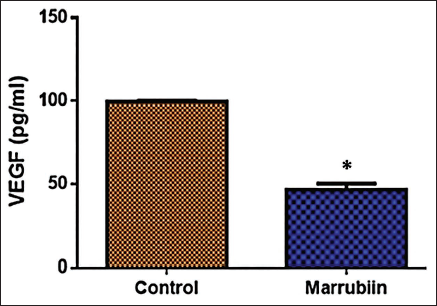
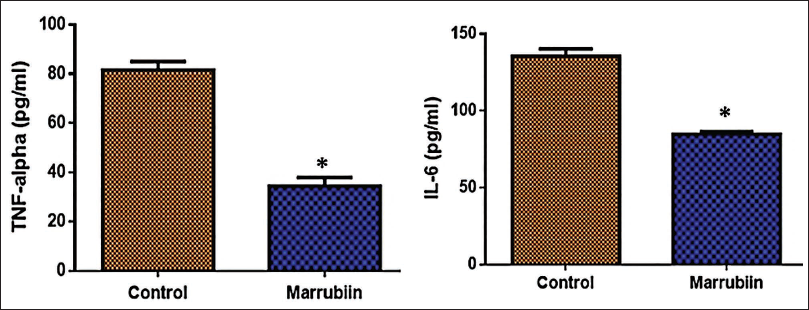
Effect of Marrubiin on the Levels of Inflammatory Cytokines in the KB Cells
The inflammatory cytokine (IL-6 and TNF-α) levels were measured in both marrubiin-treated and control KB cells using estimated assay kits. The results are presented in Figure 5. The treatment with 33.15 µg/mL of marrubiin remarkably reduced the expression of IL-6 and TNF-α in the KB cells. The results demonstrated that marrubiin can stimulate apoptosis in KB cells by controlling inflammatory marker levels (Figure 5).
Discussion
OSCC is the predominant type of cancer that accounts for over 90% of all head and neck cancers. It is the most common type of malignant tumor affecting the oral cavity, with an annual incidence of over half a million new cases. Additionally, OSCC often spreads to nearby lymph nodes (metastasis) (Harada et al., 2023). Because the majority of patients are diagnosed with OSCC when the cancer has already developed at an advanced stage, the 5-year survival rate remains poor. Despite considerable progress in the diagnosis and therapy of tumors, the survival rate remains below 50% and has shown no improvement in recent years (Sung et al., 2021). Despite the significant prevalence of OSCC, it remains essential to discover new bioactive substances and develop innovative strategies to enhance the effectiveness of traditional treatments, reducing their negative side effects and ultimately overcoming their limitations. In this study, the anti-cancer effects of marrubiin were studied against KB cells.
Cancer is the abnormal proliferation of particular cells that have acquired genetic mutations or disrupted the mechanisms of cell division and growth. The specific genetic mutation categorizes normal cells as cancer cells, which are accountable for uncontrolled proliferation, migration, and the spread of cancer to other body parts (metastasis). The cancer cell possesses a remarkable capacity for proliferation and metastasis (Ishida et al., 2017). Uncontrolled and excessive cell division leads to the formation of cancerous tissue and tends to spread to different areas, culminating in the development of metastasis (Fadlullah et al., 2016). The MTT assay is a frequently employed technique to assess the cytotoxicity of sample drugs. It measures the capacity of tetrazolium salt (MTT) to be converted into an insoluble formazan, which is reduced by mitochondrial dehydrogenase present in viable cells. In this work, the MTT assay was employed to study the cytotoxicity of marrubiin on KB cells, and the results demonstrated the dose-dependent toxic effect of marrubiin against KB cells.
Apoptosis is a cell death mechanism that occurs naturally to eliminate old or damaged cells and plays a critical function in maintaining the body’s balance and promoting its growth. Apoptosis is a tightly coordinated mechanism controlled by cellular proteins through several signaling pathways (Abotaleb et al., 2018). It eliminates damaged, infected, or uncontrollably proliferating cells. Apoptosis has a role in the progression of several disorders, including tumors. The majority of anti-tumor therapeutic techniques employ apoptosis and associated cell death networks to overcome malignant tumors. Apoptosis is a well-researched subject in the field of clinical oncology. Tumorous cells can undergo apoptosis with either extrinsic or intrinsic stimulation. The death receptors regulate extrinsic pathways, whereas the mitochondria regulate intrinsic pathways. This process involves membrane blebbing, DNA breakage, and proteolysis of numerous cellular proteins (Sui et al., 2014).
The disruption of apoptosis regulation is a critical factor in tumor development, and therapeutic approaches in clinical cancer treatment aim to target apoptotic pathways specifically. Nevertheless, the absence of apoptosis might lead to drug-off-target effects (Carneiro & El-Deiry, 2020). Hence, a primary objective and keystone of the cancer study in OSCC is to advance targeted therapy to control the process of apoptosis. In this work, the findings demonstrated that marrubiin treatment effectively induced apoptosis in oral cancer KB cells. Therefore, it was clear that marrubiin might have anti-cancer properties against oral cancer KB cells through its apoptotic-inducing effects.
Mitochondria are intracellular organelles that have crucial roles in cellular processes related to both survival and apoptosis. Exposure of cells to apoptotic stimuli leads to considerable changes in mitochondrial structure and activity. A decrease in MMP levels is an early indication of death in tumor cells (Goldar et al., 2015). Cell death occurs when there is a decrease in MMP, leading to the release of pro-apoptotic markers and the stimulation of the mitochondrial apoptotic protease. Apoptosis is initiated by mitochondrial dysfunction, activation of the intrinsic apoptosis pathway, and oxidative damage to vital cellular constituents induced by reactive oxygen species (ROS). Certain anti-cancer drugs cause a decrease in the level of MMP in tumor cells, leading to mitochondria-mediated cell death (Wei et al., 2018). Phytochemicals have demonstrated anti-cancer properties by activating death receptors and causing the loss of MMP in tumor cells. Additionally, anti-cancer drugs can increase the formation of ROS, which is related to apoptosis in cells (Tewari et al., 2022). Consistent with this statement, the outcomes of this work show that marrubiin treatment remarkably decreased the MMP level in KB cells, hence promoting mitochondria-mediated apoptosis.
Although there have been significant advancements in the therapy of OSCC, the overall survival rate has not increased. This may be attributed to the absence of a highly effective cancer biomarker for the early diagnosis of OSCC (Rivera et al., 2017). Angiogenesis, which refers to the development of new blood vessels, facilitates the delivery of oxygen and nutrients and the elimination of metabolic waste. It is also a pivotal factor in tumor development despite the involvement of multiple mechanisms in these processes. Genetic alterations in tumor tissue frequently led to the continuous activation of angiogenesis. The formation of these new blood vessels commonly occurs due to the dysregulation of a certain group of cytokines, particularly through the increased expression of VEGF (Sakata et al., 2019).
VEGF promotes tumor progression by increasing the permeability of blood vessels, allowing the extravasation of molecules with high molecular weight and causing the formation of edema. This process then facilitates the growth of new blood vessels (neovascularization). VEGF is a crucial protein produced by tumors to stimulate angiogenesis. VEGF can enhance blood vessel permeability, stimulate the growth of endothelial cells, and prevent endothelial cell death (Melincovici et al., 2018). Elevated levels of VEGF have been linked to the rapid proliferation and prognosis of various types of cancer (Zhao et al., 2015). VEGF can be a reliable indicator of the diagnosis of oral cancer. Studies have shown that angiogenesis and blood microvessel density are elevated in oral cancer compared to normal epithelium (Essa & Deraz, 2021). The present results highlighted that marrubiin treatment effectively decreased VEGF levels in KB cells. These results proved that marrubiin can inhibit oral cancer development by inhibiting angiogenesis and decreasing VEGF levels in tumor cells.
Approximately 25% of cancers are linked to chronic inflammation (Chai et al., 2015). Inflammation can lead to the loss of cell proliferation inhibition, increased angiogenesis, escape of cell death, conversion of benign cells to cancerous ones, and promotion of metastasis (Murata, 2018). Immune cells release cytokines during tumor metastasis, which promote cell survival and invasion, leading to the conversion of epithelial cells into mesenchymal cells (Hirano, 2021). Hence, understanding the molecular mechanisms underlying the relationship between tumors and inflammation is crucial to preventing and treating cancer.
Chronic inflammation initiates prolonged damage to tissues and plays a substantial role in the development of head and neck tumors. TNF-α is involved in various stages of tumor progression, including inflammation, immunological stress, and distinct stages like initiation, proliferation, angiogenesis, and metastasis (León et al., 2015). It enhances the expression of VEGF through the NF-κB cascade, thereby stimulating the development of lymphatic and blood vessels (Zhang et al., 2019). The upregulation of TNF-α in oral cancer cells is associated with increased proliferation, while its downregulation can diminish this proliferative capacity (Qiu et al., 2018). In this study, the results highlighted that marrubiin remarkably reduced the TNF-α levels in the KB cells. IL-6, a versatile cytokine, participates in immunological and inflammatory reactions. In addition, it has been documented that IL-6 is upregulated in cancer patients, especially in OSCC, and this is correlated with a poor prognosis (Márton et al., 2019). IL-6 can stimulate tumor cell growth, metastasis, and angiogenesis via various pathways (Tanaka et al., 2014). The findings of this work have highlighted that the marrubiin treatment effectively reduced the IL-6 levels in the KB cells.
Conclusion
This study demonstrates that marrubiin inhibits cell growth and induces apoptosis in KB cells. Marrubiin treatment leads to MMP reduction while decreasing VEGF and inflammatory cytokine levels, suggesting its potential role in suppressing angiogenesis and inflammation. These findings highlight marrubiin as a promising anti-cancer agent for oral cancer treatment. However, further research is required to elucidate the precise molecular mechanisms of marrubiin-induced apoptosis, with the ultimate goal of developing it into an effective therapeutic agent for oral cancer.
Footnotes
Abbreviations
AO: Acridine orange; DMRT: Duncan’s multiple range test; DMSO: Dimethyl sulfoxide; EtBr: Ethidium bromide; FBS: Fetal bovine serum; IL-6: Interleukin-6; MMP: Mitochondrial membrane potential; OSCC: Oral squamous cell carcinoma; Rh-123: Rhodamine-123; ROS: Reactive oxygen species; TNF-α: Tumor necrosis factor-α; VEGF: Vascular endothelial growth factor.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
Ethical approval was obtained from the relevant ethics committee or Institutional Review Board (IRB).
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Informed Consent
The participant has provided informed consent for the submission of the article to the journal.
